[1] HASHIMOTO K, AIZAWA T, KANNO H, et al. Adjacent segment degeneration after fusion spinal surgery—a systematic review. Int Orthop. 2018;43(4):987-993.
[2] KANG T, PARK SY, KANG CH, et al. Is biportal technique/endoscopic spinal surgery satisfactory for lumbar spinal stenosis patients? Medicine. 2019;98(18):e15451.
[3] MAZAS S, BENZAKOUR A, CASTELAIN JE, et al. Cervical disc herniation: which surgery? Int Orthop. 2018;43(4):761-766.
[4] HOUTEN JK, WEINSTEIN GR, COLLINS M. Long-term fate of C3-7 arthrodesis: 4-level ACDF versus Cervical Laminectomy and Fusion. J Neurosurg Sci. 2021;65(4):402-407.
[5] ALPERT JN. Review of the Diagnosis and Management of Lumbar Spinal Stenosis. JAMA. 2022;328(8):779-780.
[6] FU S, ZHANG C, YAN X, et al. Volumetric Changes in Cervical Disc Herniation. Spine. 2022;47(7):E296-E303.
[7] ZHANG C, FU S, YAN X, et al. Cervical microendoscopic laminoplasty-induced clinical resolution of disc herniation in patients with single- to three-level myelopathy. Sci Rep. 2022;12(1):18854.
[8] CANALE ST, BEATY JH. Campbell’s Operative Orthopaedics. 11th ed. Philadephia: Mosby, 2011.
[9] TEICHTAHL AJ, URQUHART DM, WANG Y, et al. A Dose–response relationship between severity of disc degeneration and intervertebral disc height in the lumbosacral spine. Arthritis Res Ther. 2015;17:297.
[10] ABDOLLAH V, PARENT EC, SU A, et al. The effects of axial loading on the morphometric and T2 characteristics of lumbar discs in relation to disc degeneration. Clin Biomech. 2021;83:105291.
[11] HUSSAIN M, NATARAJAN RN, AN HS, et al. Patterns of height changes in anterior and posterior cervical disc regions affects the contact loading at posterior facets during moderate and severe disc degeneration: a poroelastic C5-C6 finite element model study. Spine (Phila Pa 1976). 2010;35(18):E873-E881.
[12] MAQUER G, SCHWIEDRZIK J, HUBER G, et al. Compressive strength of elderly vertebrae is reduced by disc degeneration and additional flexion. J Mech Behav Biomed Mater. 2015;42:54-66.
[13] LUOMA K, VEHMAS T, RIIHIMÄKI H, et al. Disc Height and Signal Intensity of the Nucleus Pulposus on Magnetic Resonance Imaging as Indicators of Lumbar Disc Degeneration. Spine. 2001;26(6):680-686.
[14] BROOKS M, DOWER A, ABDUL JALIL MF, et al. Radiological predictors of recurrent lumbar disc herniation: a systematic review and meta-analysis. J Neurosurg Spine. 2021;34(3):481-491.
[15] O’CONNELL GD, JOHANNESSEN W, VRESILOVIC EJ, et al. Human internal disc strains in axial compression measured noninvasively using magnetic resonance imaging. Spine (Phila Pa 1976). 2007;32(25): 2860-2868.
[16] DOLAN P, ADAMS MA. Recent advances in lumbar spinal mechanics and their significance for modelling. Clin Biomech. 2001;16:S8-S16.
[17] TAO Y, GALBUSERA F, NIEMEYER F, et al. The impact of age, sex, disc height loss and T1 slope on the upper and lower cervical lordosis: a large-scale radiologic study. Eur Spine J. 2021;30(9):2434-2442.
[18] DALY CD, GHOSH P, BADAL T, et al. A Comparison of Two Ovine Lumbar Intervertebral Disc Injury Models for the Evaluation and Development of Novel Regenerative Therapies. Global Spine J. 2018;8(8):847-859.
[19] SUZUKI A, DAUBS MD, HAYASHI T, et al. Patterns of Cervical Disc Degeneration: Analysis of Magnetic Resonance Imaging of Over 1000 Symptomatic Subjects. Global Spine J. 2018;8(3):254-259.
[20] 蒋欣, MORISHITA Y, HENRY H, 等. 腰痛患者MRI上各节段腰椎间盘退变形式与年龄的相关性分析[J]. 中国脊柱脊髓杂志,2009, 19(11):845-849.
[21] ZHANG C, LI D, WANG C, et al. Cervical Endoscopic Laminoplasty for Cervical Myelopathy. Spine (Phila Pa 1976). 2016;41 Suppl 19:B44-B51.
[22] 牛策号, 张春霖, 严旭, 等. 椎体后方结构及对突出椎间盘体积测量的影响[J]. 中国组织工程研究,2023,27(18):2897-2902.
[23] YANG B, O’CONNELL GD. Intervertebral disc swelling maintains strain homeostasis throughout the annulus fibrosus: A finite element analysis of healthy and degenerated discs. Acta Biomater. 2019;100:61-74.
[24] JEONG JG, KANG S, JUNG GH, et al. Biomechanical Effect of Disc Height on the Components of the Lumbar Column at the Same Axial Load: A Finite-Element Study. J Healthc Eng. 2022;2022(23):1-13.
[25] ZHANG F, ZHANG K, TIAN HJ, et al. Correlation between lumbar intervertebral disc height and lumbar spine sagittal alignment among asymptomatic Asian young adults. J Orthop Surg Res. 2018;13(1):34.
[26] 龚克, 胡学昱, 凃志鹏, 等. 影像学正常人群腰椎椎间高度指数、椎间角度及腰椎前凸角度的研究分析[J]. 生物骨科材料与临床研究,2018,15(2):19-24.
[27] MCDONALD CL, ALSOOF D, GLUECK J, et al. Adjacent Segment Disease After Spinal Fusion. JBJS Rev. 2023;11(6). doi: 10.2106/JBJS.RVW.23.00028.
[28] AHLGREN BD, LUI W, HERKOWITZ HN, et al. Effect of Anular Repair on the Healing Strength of the Intervertebral Disc. Spine. 2000;25(17): 2165-2170.
[29] TANAKA N, AN HS, LIM TH, et al. The relationship between disc degeneration and flexibility of the lumbar spine. Spine J. 2001;1(1): 47-56.
[30] O’CONNELL GD, SEN S, ELLIOTT DM. Human annulus fibrosus material properties from biaxial testing and constitutive modeling are altered with degeneration. Biomech Model Mechanobiol. 2011;11(3-4): 493-503.
[31] YANG H, JEKIR MG, DAVIS MW, et al. Effective modulus of the human intervertebral disc and its effect on vertebral bone stress. J Biomech. 2016;49(7):1134-1140.
[32] ALLEN MJ, SCHOONMAKER JE, BAUER TW, et al. Preclinical Evaluation of a Poly (Vinyl Alcohol) Hydrogel Implant as a Replacement for the Nucleus Pulposus. Spine. 2004;29(5):515-523.
[33] KIRNAZ S, CAPADONA C, WONG T, et al. Fundamentals of Intervertebral Disc Degeneration. World Neurosurg. 2022;157(2):264-273.
[34] LIU ZS, FANG M, YANG L, et al. Correlation between the height reduced and the degeneration of lumbar intervertebral disc. Chin J Med Imaging Technol. 2011;27(2):388-391.
[35] MACKI M, HERNANDEZ-HERMANN M, BYDON M, et al. Spontaneous regression of sequestrated lumbar disc herniations: Literature review. Clin Neurol Neurosurg. 2014;120:136-141.
[36] KIRKALDY-WILLIS WH, WEDGE JH, YONG-HING K, et al. Pathology and Pathogenesis of Lumbar Spondylosis and Stenosis. Spine. 1978; 3(4):319-328.
[37] JIANFA Z, SHANGLI L, SHIZHEN Z. Experimental study on stiffness and strength of lumbar intervertebral disc. J Appl Biomech. 1996;(3): 160-162+189.
[38] STOUSTRUP P, RESNICK CM, ABRAMOWICZ S, et al. Management of Orofacial Manifestations of Juvenile Idiopathic Arthritis: Interdisciplinary Consensus‐Based Recommendations. Arthritis Rheumatol. 2022;75(1):4-14.
[39] POOTHERI S, ELLAM D, GRÜBL T, et al. A Two-Stage Automatic Color Thresholding Technique. Sensors (Basel). 2023;23(6):3361.
[40] 刘盼. 关于DR测距误差的分析[J]. 中国辐射卫生,2020,29(2): 153-156.
[41] Н.И.МУСХЕЛИШВИЛИ. Курсаналитической теометрии. 2016.
[42] GUELLIL N, ARGAWAL N, KRIEGHOFF M, et al. Novel Methods to Measure Height and Volume in Healthy and Degenerated Lumbar Discs in MRIs: A Reliability Assessment Study. Diagnostics. 2022;12(6):1437.
|
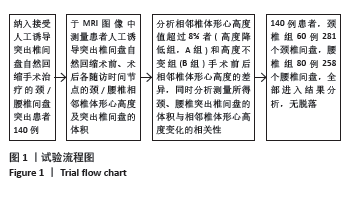
 此次研究iRHNP诱导突出椎间盘自然回缩后椎间盘的生物强度尚有待更为长期(> 5年及以上)的随访观察。
此次研究iRHNP诱导突出椎间盘自然回缩后椎间盘的生物强度尚有待更为长期(> 5年及以上)的随访观察。