Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (4): 632-639.doi: 10.12307/2022.988
Previous Articles Next Articles
Medial open-wedge tibial osteotomy versus lateral closed-wedge tibial osteotomy for unicompartmental knee osteoarthritis: a meta-analysis
Yu Jiaan, Liu Xinwei, Lian Hongyu, Liu Kexin, Li Zitao
- Second Department of Orthopedics, Hongqi Hospital Affiliated to Mudanjiang Medical College, Mudanjiang 157011, Heilongjiang Province, China
-
Received:2022-01-08Accepted:2022-02-12Online:2023-02-08Published:2022-06-23 -
Contact:Li Zitao, Master, Chief physician, Professor, Master’s supervisor, Second Department of Orthopedics, Hongqi Hospital Affiliated to Mudanjiang Medical College, Mudanjiang 157011, Heilongjiang Province, China -
About author:Yu Jiaan, Master candidate, Second Department of Orthopedics, Hongqi Hospital Affiliated to Mudanjiang Medical College, Mudanjiang 157011, Heilongjiang Province, China -
Supported by:Fundamental Research Project of Heilongjiang Provincial Colleges and Universities, No. 2017-KYYWFMY-0864 (to LZT)
CLC Number:
Cite this article
Yu Jiaan, Liu Xinwei, Lian Hongyu, Liu Kexin, Li Zitao. Medial open-wedge tibial osteotomy versus lateral closed-wedge tibial osteotomy for unicompartmental knee osteoarthritis: a meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 632-639.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
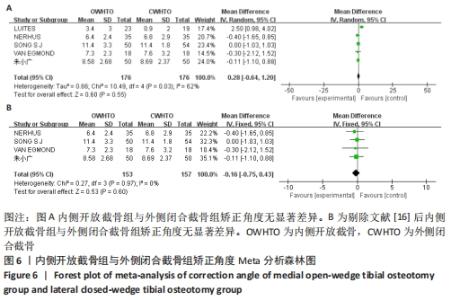
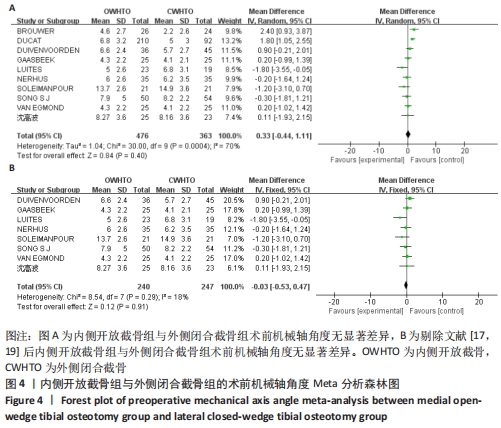
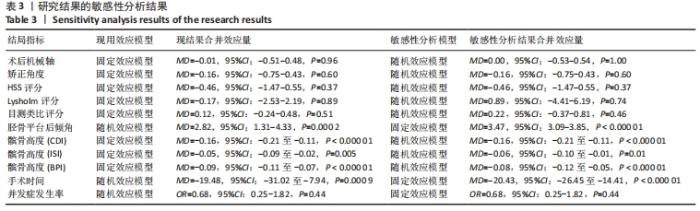
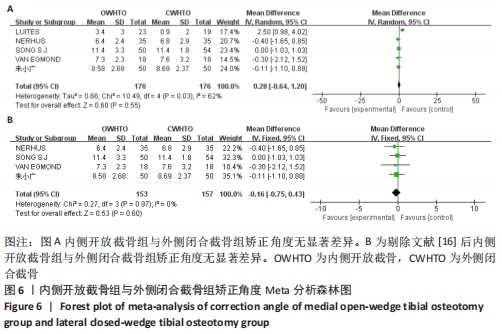
2.3.2 各组矫正角度的差异 有5项研究报道了两组的矫正角度[11,14,16,18,20],异质性分析结果显示:P=0.03,I2=62%,各研究间异质性明显(MD=0.28,95%CI:-0.64-1.20,P=0.55)。敏感性分析显示,异质性来源可能与LUITES等[16]患者术后角度测量方法不规范有关,剔除文献后异质性明显下降(P=0.97,I2=0%),使用固定效应模型进行分析,结果显示两组间术后矫正角度无显著差异(MD=-0.16,95%CI:-0.75-0.43,P=0.60),见图6。将固定效应模型更换为随机效应模型,结果无变化(MD=-0.16,95%CI:-0.75-0.43,P=0.60),说明结果稳定佳。"
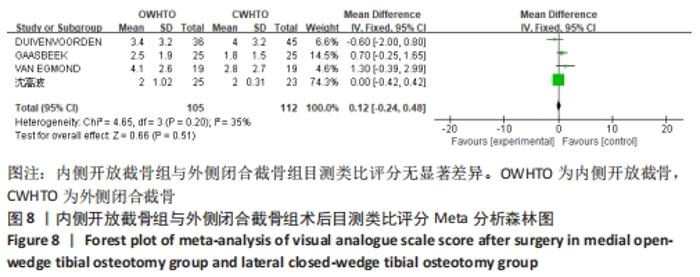
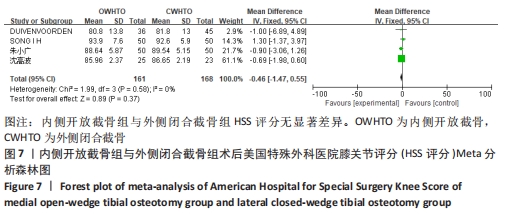
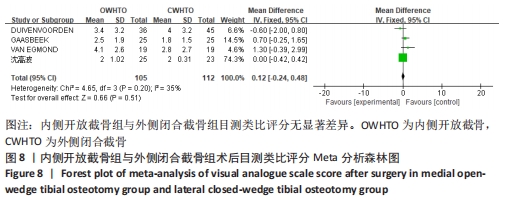
有2项研究报道了两组术后膝关节Lysholm评分[16,18],各研究结果间无统计学异质性(P=0.21,I2=37%),使用固定效应模型分析,结果显示术后Lysholm评分两组间无显著差异(MD=-0.17,95%CI:-2.53-2.19,P=0.89)。将固定效应模型更换为随机效应模型,结果无显著差异(MD=0.89,95%CI:-4.41-6.19,P=0.74),说明结果有良好稳定性。 2.3.4 各组疼痛评分的差异 有4项研究报道了两组术后目测类比评分[12-14,23],各研究结果间无统计学异质性(P=0.20,I2=35%),使用固定效应模型分析,结果显示术后目测类比评分两组间无显著差异(MD=0.12,95%CI:-0.24-0.48,P=0.51),见图8。将固定效应模型更换为随机效应模型,结果无显著差异(MD=0.22,95%CI:-0.37-0.81,P=0.46),说明结果有良好稳定性。 "
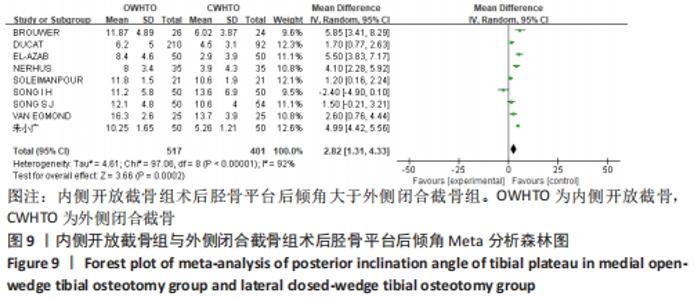
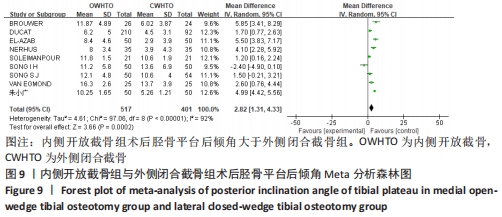
2.3.5 胫骨平台后倾角的差异 有9项研究报道了两组术后胫骨平台后倾角[11,14-15,17-22],各研究结果间具有明显统计学异质性(P < 0.000 01,I2=92%),敏感性分析认为各研究间年龄、性别无显著差异,并逐一去除研究,异质性无显著差异。分析认为不同研究者对于影像学阅片的主观差异以及不同医生手术技术的差别是异质性来源,遂使用随机效应模型分析,结果显示术后胫骨平台后倾角两组间有显著差异(MD=2.82,95%CI:1.31-4.33,P=0.000 2),内侧开放截骨组术后胫骨平台后倾角更大,见图9。将随机效应模型更换为固定效应模型,结果无显著差异 (MD=3.47,95%CI:3.09-3.85,P < 0.000 01),说明结果有良好稳定性。 "
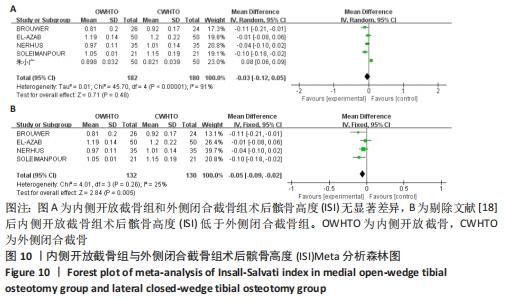
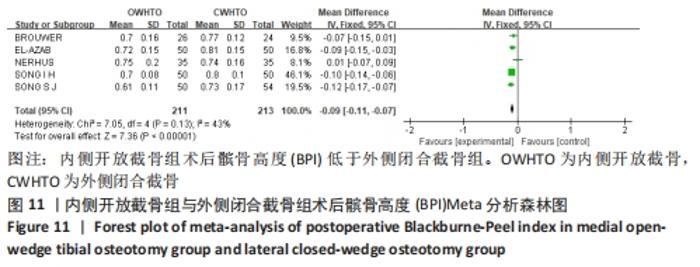
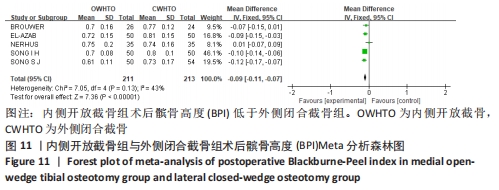
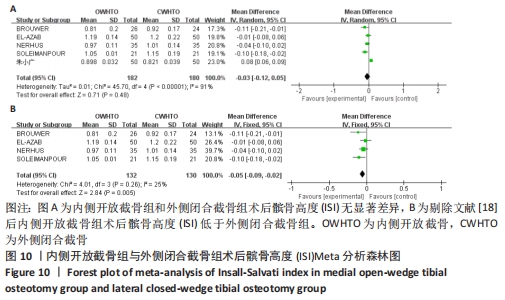
2.3.6 各组髌骨高度变化的差异 有2项研究报道了两组术后髌骨高度的Caton-Deschamps指数(CDI) [12,21],各研究结果间无统计学异质性(P=0.31,I2=2%),选择固定效应模型分析,结果显示两组术后髌骨高度CDI有较大差异(MD=-0.16,95%CI:-0.21至-0.11,P < 0.000 01),内侧开放截骨术后髌骨高度较低。将固定效应模型更换为随机效应模型,结果无变化,说明结果稳定。 有5项研究报道了两组术后髌骨高度的Insall-Salvati指数(ISI) [11,15,17-18,21],异质性分析:P < 0.000 01,I2=91%,各研究间异质性较大(MD=-0.03,95%CI:-0.12-0.05,P=0.48)。敏感性分析认为异质性可能来源于人种差异,并剔除文献。剔除文献[18]后异质性明显下降(P=0.26,I2=25%),使用固定效应模型进行分析,结果显示两组间术后ISI有显著差异(MD=-0.05,95%CI:-0.09至-0.02,P=0.005),内侧开放截骨术后髌骨位置较低,见图10。将固定效应模型更换为随机效应模型,结果无显著差异(MD=-0.06,95%CI:-0.10至-0.01,P=0.01),说明结果较稳定。 "
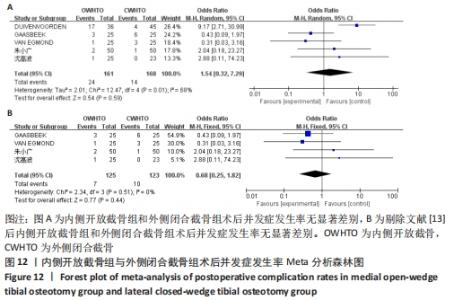
2.3.7 各组手术时间差异 有2项研究报道了两组手术时间[12,15],各研究结果间有统计学异质性(P=0.06,I2=71%),选择随机效应模型分析,结果显示两组手术时间有显著差异(MD=-19.48,95%CI:-31.02至-7.94,P=0.000 9)。内侧开放截骨相比外侧闭合截骨手术时间更短。将随机效应模型更换为固定效应模型,结果无显著差异(MD=-20.43,95%CI:-26.45至-14.41,P < 0.000 01),说明结果较稳定。 2.3.8 各组术后并发症差异 有5项研究报道了两组术后并发症[12-14,18,23],异质性分析:P=0.01,I2=68%,各研究间异质性较大(OR=1.54,95%CI:0.32-7.29,P=0.59)。进行敏感性分析后,发现年龄、性别等均不是异质性来源,可能与医生的手术操作有关。剔除文献[13]后异质性明显下降(P=0.51,I2=0%),使用固定效应模型进行分析,结果显示两组间术后并发症发生率没有显著差异(OR=0.68,95%CI:0.25-1.82,P=0.44),见图12。"
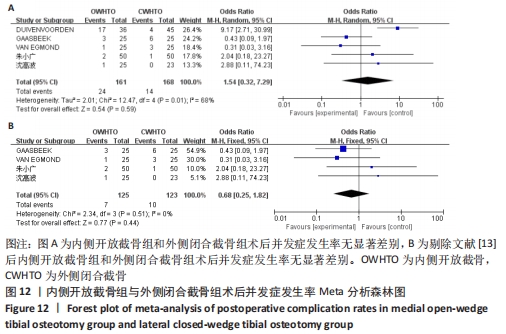
| [1] 中国医院协会临床新技术应用专业委员会,中华医学会骨科学分会关节外科学组,中国医师协会骨科医师分会骨关节炎学组.中国膝关节周围截骨下肢力线矫正术治疗膝关节骨关节炎临床指南[J].中华骨科杂志, 2021,41(23):1655-1672. [2] ENGH GA, AMMEEN D. Is an intact anterior cruciate ligament needed in order to have a well-functioning unicondylar knee replacement? Clin Orthop Relat Res. 2004; (428):170-173. [3] KIM JH, KIM HJ, LEE DH. Survival of opening versus closing wedge high tibial osteotomy: a meta-analysis. Sci Rep. 2017;7(1):7296. [4] KUNZE KN, BELETSKY A, HANNON CP, et al. Return to work and sport after proximal tibial osteotomy and the effects of opening versus closing wedge techniques on adverse outcomes: a systematic review and meta-analysis. Am J Sports Med. 2020;48(9):2295-2304. [5] 黄野.坚持膝关节骨关节炎的阶梯化治疗[J].实用骨科杂志,2020,26(12):1057-1058. [6] 黄野,柳剑,王兴山,等.胫骨高位截骨术适应证解析[J].中华外科杂志,2020,58(6): 420-424. [7] BERRUTO M, MAIONE A, TRADATI D, et al. Closing-wedge high tibial osteotomy, a reliable procedure for osteoarthritic varus knee. Knee Surg Sports Traumatol Arthrosc. 2020;28(12):3955-3961. [8] 王兴山,柳剑,顾建明,等.改良闭合楔形胫骨高位截骨术治疗膝内翻畸形的疗效观察[J].中华关节外科杂志(电子版),2016, 10(5):474-480. [9] 李静,李幼平.不断完善与发展的Cochrane系统评价[J].中国循证医学杂志,2008,8(9): 742-743. [10] CLAUDIO L, BRENDON S, MARCO S, et al. Assessing the quality of studies in meta-analyses: advantages and limitations of the Newcastle Ottawa Scale. World J Meta Anal. 2017;5(4):80-84. [11] NERHUS TK, EKELAND A, SOLBERG G, et al. Radiological outcomes in a randomized trial comparing opening wedge and closing wedge techniques of high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc. 2017;25(3):910-917. [12] GAASBEEK RD, NICOLAAS L, RIJNBERG WJ, et al. Correction accuracy and collateral laxity in open versus closed wedge high tibial osteotomy. A one-year randomised controlled study. Int Orthop. 2010;34(2):201-207. [13] DUIVENVOORDEN T, BROUWER RW, BAAN A, et al. Comparison of closing-wedge and opening-wedge high tibial osteotomy for medial compartment osteoarthritis of the knee: a randomized controlled trial with a six-year follow-up. J Bone Joint Surg Am. 2014; 96(17):1425-1432. [14] VAN EGMOND N, VAN GRINSVEN S, VAN LOON CJ, et al. Better clinical results after closed- compared to open-wedge high tibial osteotomy in patients with medial knee osteoarthritis and varus leg alignment. Knee Surg Sports Traumatol Arthrosc. 2016; 24(1):34-41. [15] SOLEIMANPOUR J, ELMI A, JAFARI MA, et al. Comparison of genu varum treating results using open and closed wedge high tibial osteotomy. Pak J Biol Sci. 2013;16(14):686-691. [16] LUITES JW, BRINKMAN JM, WYMENGA AB, et al. Fixation stability of opening- versus closing-wedge high tibial osteotomy: a randomised clinical trial using radiostereometry. J Bone Joint Surg Br. 2009;91(11):1459-1465. [17] BROUWER RW, BIERMA-ZEINSTRA SM, VAN KOEVERINGE AJ, et al. Patellar height and the inclination of the tibial plateau after high tibial osteotomy. The open versus the closed-wedge technique. J Bone Joint Surg Br. 2005;87(9):1227-1232. [18] 朱小广,彭庆州,王大鹏.开放与闭合胫骨高位截骨治疗膝骨性关节炎临床对比研究[J].中华老年医学杂志,2021,40(4):491-495. [19] DUCAT A, SARIALI E, LEBEL B, et al. Posterior tibial slope changes after opening- and closing-wedge high tibial osteotomy: a comparative prospective multicenter study. Orthop Traumatol Surg Res. 2012;98(1):68-74. [20] SONG SJ, YOON KH, PARK CH. Patellofemoral cartilage degeneration after closed- and open-wedge high tibial osteotomy with large alignment correction. Am J Sports Med. 2020; 48(11):2718-2725. [21] EL-AZAB H, GLABGLY P, PAUL J, et al. Patellar height and posterior tibial slope after open- and closed-wedge high tibial osteotomy: a radiological study on 100 patients. Am J Sports Med. 2010;38(2):323-329. [22] SONG IH, SONG EK, SEO HY, et al. Patellofemoral alignment and anterior knee pain after closing- and opening-wedge valgus high tibial osteotomy. Arthroscopy. 2012; 28(8):1087-1093. [23] 沈高波,崔龙慷,方源,等.内侧开放与外侧闭合胫骨高位截骨治疗内侧间室膝骨性关节炎的早期疗效对比[J].实用医学杂志, 2021,37(8):1031-1036. [24] BROUWER RW, HUIZINGA MR, DUIVENVOORDEN T, et al. Osteotomy for treating knee osteoarthritis. Cochrane Database Syst Rev. 2014;(12):D4019. [25] SCHROTER S, ATESCHRANG A, LOWE W, et al. Early full weight-bearing versus 6-week partial weight-bearing after open wedge high tibial osteotomy leads to earlier improvement of the clinical results: a prospective, randomised evaluation. Knee Surg Sports Traumatol Arthrosc. 2017;25(1):325-332. [26] ZIQI Z, YUFENG M, LEI Z, et al. Therapeutic effects comparison and revision case analysis of unicompartmental knee arthroplasty and open wedge high tibial osteotomy in treating medial knee osteoarthritis in patients under 60 years: a 2-6-year follow-up study[J]. Orthop Surg. 2020;12(6):1635-1643. [27] 郭保逢,秦泗河,黄野.膝关节骨关节炎的保膝治疗进展[J].中国修复重建外科杂志, 2018,32(10):1292-1296. [28] JONES GG, JAERE M, CLARKE S, et al. 3D printing and high tibial osteotomy. EFORT Open Rev. 2018;3(5):254-259. [29] NOYES FR, GOEBEL SX, WEST J. Opening wedge tibial osteotomy: the 3-triangle method to correct axial alignment and tibial slope. Am J Sports Med. 2005;33(3):378-387. [30] KIM GB, KIM KI, SONG SJ, et al. Increased posterior tibial slope after medial open-wedge high tibial osteotomy may result in degenerative changes in anterior cruciate ligament. J Arthroplasty. 2019;34(9):1922-1928. [31] AMIS AA. Biomechanics of high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc. 2013;21(1):197-205. [32] SCHUSTER P, GESSLEIN M, SCHLUMBERGER M, et al. Ten-year results of medial open-wedge high tibial osteotomy and chondral resurfacing in severe medial osteoarthritis and varus malalignment. Am J Sports Med. 2018;46(6):1362-1370. [33] BITO H, TAKEUCHI R, KUMAGAI K, et al. Opening wedge high tibial osteotomy affects both the lateral patellar tilt and patellar height. Knee Surg Sports Traumatol Arthrosc. 2010;18(7):955-960. [34] ELMALI N, ESENKAYA I, CAN M, et al. Monoplanar versus biplanar medial open-wedge proximal tibial osteotomy for varus gonarthrosis: a comparison of clinical and radiological outcomes. Knee Surg Sports Traumatol Arthrosc. 2013;21(12):2689-2695. [35] NUTE DW, BOTTONI CR. Editorial commentary: uniplane high tibial osteotomy just below the metaphyseal flare is preferable to biplane opening wedge high tibial osteotomy distal to the tuberosity: a cut below our expectations. Arthroscopy. 2021;37(8):2579-2581. [36] KIM JS, LEE JI, CHOI HG, et al. Retro-tubercle biplanar opening wedge high tibial osteotomy is favorable for the patellofemoral joint but not for the osteotomized tubercle itself compared with supra-tubercle osteotomy. Arthroscopy. 2021;37(8):2567-2578. [37] IACONO V, DE FRANCO C, AULETTA N, et al. New plates with polyaxial locking system and PSI technique in medial open wedge high tibial osteotomy: preliminary results. J Biol Regul Homeost Agents. 2020;34(3 Suppl 2):111-113. |
| [1] | Xu Xiangjun, Wang Chao, Song Qunshan, Li Bingyan, Zhang Jichao, Wang Guodong, Dong Yuefu. Optimal angle for prosthesis implantation in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 612-618. |
| [2] | Li Shihao, Li Qi, Li Zhen, Zhang Yuanyuan, Liu Miaomiao, Ouyang Yi, Xu Weiguo. Plantar pressure and gait analysis in patients with anterior cruciate ligament injury and reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 626-631. |
| [3] | Xu Yangyang, He Peiliang, Meng Qingqi, Li Siming. A meta-analysis of the effects of continuous adductor canal block and continuous femoral nerve block on early activity after knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 640-645. |
| [4] | Chai Hao, Yang Deyong, Zhang Lei, Shu Li. 3D printing personalized osteotomy guide technology versus conventional total knee arthroplasty on the accuracy of lower limb force alignment: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 646-654. |
| [5] | Li Yaping, Liu Hong, Gao Zhen, Chen Xiaolin, Huang Wujie, Jiang Zheng. Three-dimensional motion analysis of lower limb biomechanical performance in Tai Chi practitioners accompanied by knee joint pain [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 520-526. |
| [6] | Wang Jianye, Liu Xin, Tian Lin, Sun Ning, Li Yuefei, Bi Jingwei, Liu Changzhen, Sun Zhaozhong . Measuring the position relation between nerve tissue and bony structure in lumbar spinal canal decompression area by constructing a three-dimensional model of the lumbar spine [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 539-546. |
| [7] | Wei Bo, Yao Qingqiang, Tang Cheng, Li Xuxiang, Xu Yan, Wang Liming. Advantage of medial pivot prosthesis in total knee arthroplasty via medial subvastus approach [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 552-557. |
| [8] | Wan Guoli, Shi Chenhui, Wang Weishan, Li Ang, Shi Xunda, Cai Yi. Retrospective analysis of the influencing factors of chronic pain after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 558-564. |
| [9] | Gu Mingxi, Wang Bo, Tian Fengde, An Ning, Hao Ruihu, Wang Changcheng, Guo Lin. Comparison of early efficacy and safety of simultaneous and staged bilateral total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 565-571. |
| [10] | Zhang Jinbiao, Li Xiaoming, Xing Wanlin, Ma Fei, Yu Qiaoya, Dai Rongqin. Early warning efficacy of thrombus molecular markers after total knee arthroplasty in patients complicated with venous thromboembolism [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 572-577. |
| [11] | Chen Lei, Jia Yanfei, Lyu Huicheng, Zhang Lifeng. Application of T-shaped plate for fractures involving the quadrilateral region of acetabulum [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 578-582. |
| [12] | Yu He, Zheng Jiafa, Song Xiufeng, Guan Shengyi. Tibiotalocalcaneal arthrodesis with blood supplied fibular flap combined with hollow screw in the treatment of end-stage ankle osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 588-593. |
| [13] | Guo Yingqi, Gong Xianxu, Zhang Yan, Xiao Han, Wang Ye, Gu Wenguang. Meniscus extrusion and patellofemoral joint cartilage injury and bone marrow lesions: MRI semi-quantitative score [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 600-605. |
| [14] | Lu Hui, Wu Qimei, Liu Rong. Finite element analysis and application of unilateral and bilateral bone-filling mesh container in treatment of osteoporotic vertebral compression fracture [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 391-397. |
| [15] | You Aijia, Li Wenjie, Zhou Junli, Li Chun. Systematic evaluation of six dressings on wound safety following total hip and knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 486-492. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||