Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (4): 565-571.doi: 10.12307/2022.792
Previous Articles Next Articles
Comparison of early efficacy and safety of simultaneous and staged bilateral total knee arthroplasty
Gu Mingxi, Wang Bo, Tian Fengde, An Ning, Hao Ruihu, Wang Changcheng, Guo Lin
- Second Department of Orthopedics, Zhongshan Hospital Affiliated to Dalian University, Dalian 116001, Liaoning Province, China
-
Received:2021-11-25Accepted:2021-12-31Online:2023-02-08Published:2022-06-22 -
Contact:Guo Lin, MD, Chief physician, Professor, Master’s supervisor, Second Department of Orthopedics, Zhongshan Hospital Affiliated to Dalian University, Dalian 116001, Liaoning Province, China -
About author:Gu Mingxi, Master candidate, Second Department of Orthopedics, Zhongshan Hospital Affiliated to Dalian University, Dalian 116001, Liaoning Province, China
CLC Number:
Cite this article
Gu Mingxi, Wang Bo, Tian Fengde, An Ning, Hao Ruihu, Wang Changcheng, Guo Lin. Comparison of early efficacy and safety of simultaneous and staged bilateral total knee arthroplasty[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 565-571.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
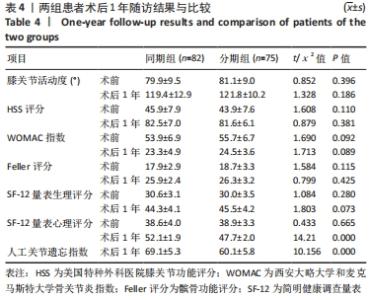
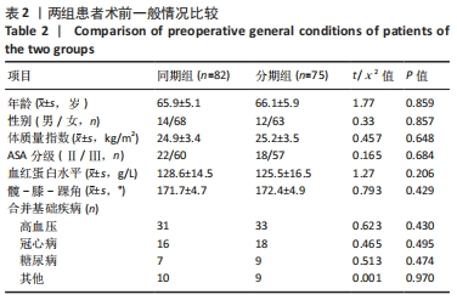
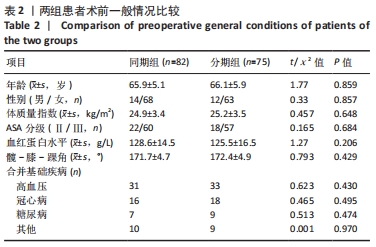
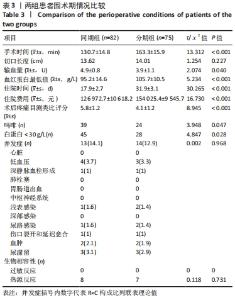
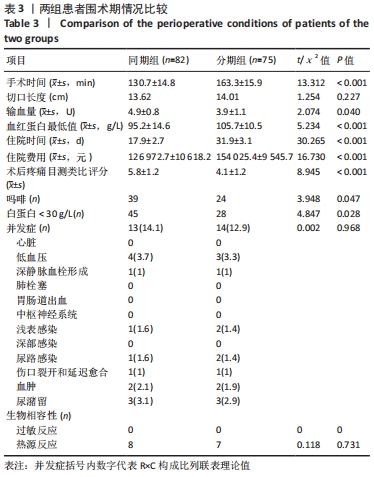
2.4 两组患者住院时间及住院费用比较 分期组的住院时间是2次单独住院累积的结果,与分期全膝关节置换相比,同期全膝关节置换将住院时间缩短了近50%(P=0.000),且成本降低约20%(P=0.000),见表3。 2.5 两组患者围术期疼痛程度比较 相较于分期组,同期组患者围术期内的疼痛程度更高,见表3。 2.6 两组患者围术期血红蛋白水平和输血量的比较 两组患者术前平均血红蛋白水平差异无显著性意义(P=0.206),见表2。与分期组相比,同期组患者围术期内血红蛋白水平显著降低(P=0.000),平均输血量也更高(P=0.000),表明同期组患者术后用血需求更大,见表3, 2.7 两组患者围术期营养状况的比较 用白蛋白比较了同期组与分期组患者术后的营养状况,同期组围术期内出现低白蛋白血症的风险更高(P=0.028),见表3。 2.8 两组患者围术期并发症的比较 同期组和分期组分别有13例和14例发生贫血、尿路感染、伤口延迟愈合等轻微并发症,通过口服抗生素、放置导尿管、膀胱冲洗及关节穿刺等对症治疗后痊愈,未见其他并发症。两组之间并发症发生差异无显著性意义,见表3。 2.9 两组患者早期临床功能结局的比较 两组患者之间术前与术后膝关节活动度、HSS评分及WOMAC指数的差异无显著性意义(P > 0.05);术后1年随访时,两组术后平均膝关节活动度显著改善,HSS评分也显著改善,WOMAC指数评分明显降低。两组患者术后Feller评分的差异无显著性意义,表明两组患者髌骨关节功能无明显差异(P=0.425),见表4。"
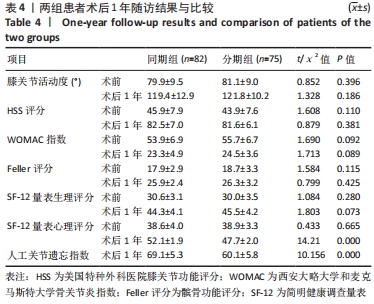
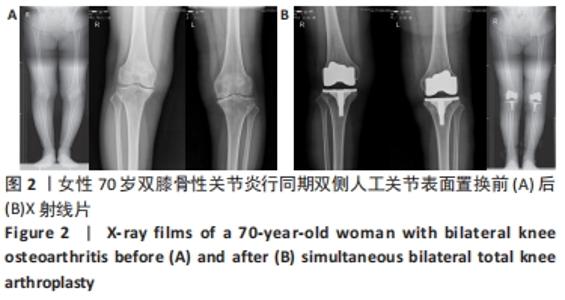
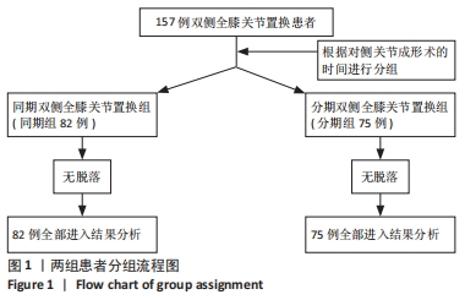
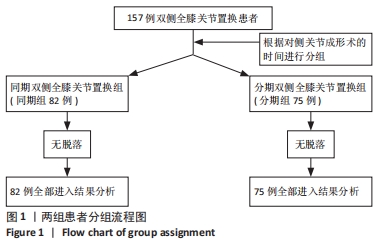
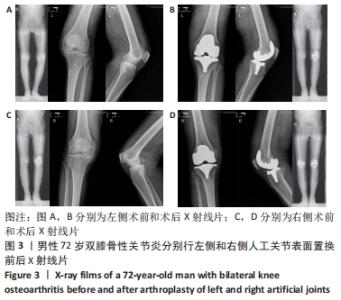
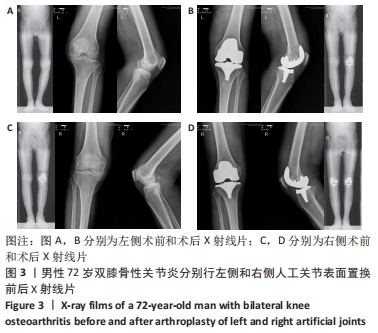
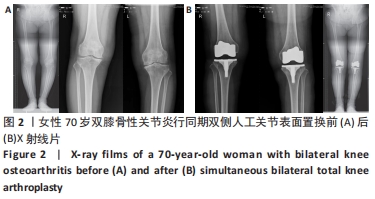
2.10 两组患者早期生活质量的比较 结果显示两组在术后早期随访时生理评分的差异无显著性意义(P=0.073);术后6个月随访时,相较于分期组,同期组患者的心理评分更高(P=0.000),人工关节被遗忘指数(FJS)评分更高,表明选择同期双侧置换的患者能够获得更好本体感觉,见表4。 2.11 生物相容性 两组患者术后均未发生严重不良过敏反应,未出现不明原因的皮肤红斑、湿疹等过敏反应。少数患者术后半年内出现膝关节局部发热反应,部分患者表现出滑膜炎的症状,在排除其他反应热源以后,考虑为金属吸收热,两组之间的局部反应热发生率无明显差异(P > 0.05),经局部激素注射和改善循环治疗后,症状好转,术后1年金属反应热基本消失。 2.12 典型病例图片 同期双侧全膝关节置换前后X射线片见图2;分期双侧全膝关节置换前后X射线见图3。"
| [1] CUBUKCU D, SARSAN A, ALKAN H. Relationships between pain, function and radiographic findings in osteoarthritis of the knee: a cross-sectional study. Arthritis. 2012;2012:984060. [2] SOBH AH, SILJANDER MP, MELLS AJ, et al. Cost Analysis, Complications, and Discharge Disposition Associated With Simultaneous vs Staged Bilateral Total Knee Arthroplasty. J Arthroplasty. 2018;33(2):320-323. [3] WAIMANN CA, FERNANDEZ-MAZARAMBROZ RJ, CANTOR SB, et al. Cost-effectiveness of total knee replacement: a prospective cohort study. Arthritis Care Res. 2014;66(4):592. [4] KURTZ S,ONG K, LAU E, et al. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Br. 2007;89(4):780-785. [5] MARDANI-KIVI M, LEILI EK, TORFEH N, et al. Bilateral total knee arthroplasty: Simultaneous versus staging in the same or in twice hospitalization. J Clin Orthop Trauma. 2020;14:59-64. [6] HUANG L, XU T, LI P, et al. Comparison of mortality and complications between bilateral simultaneous and staged total hip arthroplasty: A systematic review and meta-analysis. Medicine (Baltimore). 2019; 98(39):e16774. [7] YONG TM, YOUNG EC, MOLLOY IB, et al. Long-Term Implant Survivorship and Modes of Failure in Simultaneous Concurrent Bilateral Total Knee Arthroplasty. J Arthroplasty. 2020;35(1):139-144. [8] ODUM SM, TROYER JL, KELLY MP, et al. A cost-utility analysis comparing the cost-effectiveness of simultaneous and staged bilateral total knee arthroplasty. J Bone Joint Surg Am.2013;95:1441-1449. [9] HUSSAIN N, CHIEN T, HUSSAIN F, et al.Simultaneous versus staged bilateral total knee arthroplasty: a meta-analysis evaluating mortality, peri-operative complications and infection rates.HSS J. 2013;9(1): 50-59. [10] YOON HS, HAN CD, YANG IH. Comparison of simultaneous bilateral and staged bilateral total knee arthroplasty in terms of perioperative complications. J Arthroplasty. 2010;25(2):179-185. [11] SHETH DS, CAFRI G, PAXTON EW, et al. Bilateral simultaneous vs staged total knee arthroplasty: a comparison of complications and mortality. J Arthrop. 2016;31:212-216. [12] MEEHAN JP, DANIELSEN B, TANCREDI DJ, et al. A population-based comparison of the incidence of adverse outcomes after simultaneous-bilateral and staged-bilateral total knee arthroplasty. J Bone Joint Surg Am Vol.2011;93:2203-2213. [13] ZHANG Z, CHAI W, ZHAO G, et al. Association of HSS score and mechanical alignment after primary TKA of patients suffering from constitutional varus knee that caused by combined deformities: a retrospective study. Sci Rep. 2021;11(1):3130. [14] JAIN S, WASNIK S, MITTAL A, et al. Simultaneous bilateral total knee replacement: a prospective study of 150 patients. J Orthop Surg (Hong Kong). 2013;21(1):19. [15] PARK HJ, CHANG MJ, KIM TW, et al. Subchondral Bone Condition and Intraoperative Grading of Cartilage Degeneration Underneath Patella Unrelated to the Clinical Outcome after TKA with Unresurfaced Patella. J Knee Surg. 2021 Feb 19. doi: 10.1055/s-0041-1723980. [16] 王海棠,寿涓,任利民,等.SF-12量表评价上海市社区老年人生命质量的信效度研究[J].中国全科医学,2019,22(9):1057-1061. [17] 王家伟,尹宗生,马广文,等.单髁置换术与全膝关节置换术后人工关节遗忘程度的比较[J].实用骨科杂志,2018,24(5):464-467. [18] RIPOLLÉS-MELCHOR J, ABAD-MOTOS A, DÍEZ-REMESAL Y, et al. Postoperative Outcomes Within Enhanced Recovery After Surgery Protocol in Elective Total Hip and Knee Arthroplasty (POWER2) Study Investigators Group for the Spanish Perioperative Audit and Research Network (REDGERM). Association Between Use of Enhanced Recovery After Surgery Protocol and Postoperative Complications in Total Hip and Knee Arthroplasty in the Postoperative Outcomes Within Enhanced Recovery After Surgery Protocol in Elective Total Hip and Knee Arthroplasty Study (POWER2). JAMA Surg. 2020;155(4):e196024. [19] MEMTSOUDIS SG, MA Y, CHIU YL, et al. Bilateral total knee arthroplasty: risk factors for major morbidity and mortality. Anesth Analg. 2011;113:784-790. [20] WILKIE W, MOHAMED N, REMILY E, et al. Same Day versus Staged Total Knee Arthroplasty: Do Cost Savings Justify the Risk? J Knee Surg. 2020 Jul 13. doi: 10.1055/s-0040-1713734. [21] Agarwala S, Butani M, D’Mello J, et al. Decreasing hospital length of stay and enhancing recovery in Total Knee Arthroplasty. J Clin Orthop Trauma. 2020;11(1):122-128. [22] Fu D, Li G, Chen K, et al. Comparison of clinical outcome between simultaneous-bilateral and staged-bilateral total knee arthroplasty: a systematic review of retrospective studies. J Arthroplasty. 2013;28(7): 1141-1147. [23] LIU L, LIU H, ZHANG H, et al. Bilateral total knee arthroplasty: Simultaneous or staged? A systematic review and meta-analysis. Medicine (Baltimore). 2019;98(22):e15931. [24] KEATING EM, MEDING JB, FARIA PM, et al. Predictors of transfusion risk in elective knee surgery. Clin Orthop Relat Res. 1998;357:50-59. [25] PATIL N, WAKANKAR H. Pros and cons of simultaneous bilateral total knee arthroplasty including morbidity and mortality rates. Orthopedics. 2008;31:780-789. [26] TRASOLINI NA, MCKNIGHT BM, DORR LD. The opioid crisis and the orthopedic surgeon. J Arthroplasty. 2018;33:3379e3382.e1 [27] JENSEN JE, JENSEN TG, SMITH TK, et al. Nutrition in orthopaedic surgery. J Bone Joint Surg Am. 1982;64(9):1263-1272. [28] MAN SL, CHAU WW, CHUNG KY, et al. Hypoalbuminemia and obesity class II are reliable predictors of peri-prosthetic joint infection in patient undergoing elective total knee arthroplasty. Knee Surg Relat Res. 2020;32(1):21. [29] ANOUSHIRAVANI AA, SAYEED Z, CHAMBERS MC, et al. Assessing in-hospital outcomes and resource utilization after primary total joint arthroplasty among underweight patients. J Arthroplast. 2016;31(7): 1407-1412. [30] MALAHIAS MA, GU A, ADRIANI M, et al. Comparing the Safety and Outcome of Simultaneous and Staged Bilateral Total Knee Arthroplasty in Contemporary Practice: A Systematic Review of the Literature. J Arthroplasty. 2019;34(7):1531-1537. [31] HU J, LIU Y, LV Z, LI X, et al. Mortality and morbidity associated with simultaneous bilateral or staged bilateral total knee arthroplasty: a meta-analysis. Arch Orthop Trauma Surg. 2011;131:1291-1298. [32] RESTREPO C, PARVIZI J, DIETRICH T, et al. Safety of simultaneous bilateral total knee arthroplasty: a meta-analysis. J Bone Joint Surg Am. 2007;89:1220-1226. [33] SPICER E, THOMAS GR, RUMBLE EJ. Comparison of the major intraoperative and postoperative complications between unilateral and sequential bilateral total knee arthroplasty in a high-volume community hospital. Can J Surg. 2013;56(5):311-317. [34] MARCH LM, CROSS M, TRIBE KL, et al. Two knees or not two knees? Patient costs and outcomes following bilateral and unilateral total knee joint replacement surgery for OA. Osteoarthr Cartil. 2004;12(5):400. |
| [1] | Xu Xiangjun, Wang Chao, Song Qunshan, Li Bingyan, Zhang Jichao, Wang Guodong, Dong Yuefu. Optimal angle for prosthesis implantation in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 612-618. |
| [2] | Li Shihao, Li Qi, Li Zhen, Zhang Yuanyuan, Liu Miaomiao, Ouyang Yi, Xu Weiguo. Plantar pressure and gait analysis in patients with anterior cruciate ligament injury and reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 626-631. |
| [3] | Yu Jiaan, Liu Xinwei, Lian Hongyu, Liu Kexin, Li Zitao. Medial open-wedge tibial osteotomy versus lateral closed-wedge tibial osteotomy for unicompartmental knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 632-639. |
| [4] | Xu Yangyang, He Peiliang, Meng Qingqi, Li Siming. A meta-analysis of the effects of continuous adductor canal block and continuous femoral nerve block on early activity after knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 640-645. |
| [5] | Chai Hao, Yang Deyong, Zhang Lei, Shu Li. 3D printing personalized osteotomy guide technology versus conventional total knee arthroplasty on the accuracy of lower limb force alignment: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 646-654. |
| [6] | Li Yaping, Liu Hong, Gao Zhen, Chen Xiaolin, Huang Wujie, Jiang Zheng. Three-dimensional motion analysis of lower limb biomechanical performance in Tai Chi practitioners accompanied by knee joint pain [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 520-526. |
| [7] | Wei Bo, Yao Qingqiang, Tang Cheng, Li Xuxiang, Xu Yan, Wang Liming. Advantage of medial pivot prosthesis in total knee arthroplasty via medial subvastus approach [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 552-557. |
| [8] | Wan Guoli, Shi Chenhui, Wang Weishan, Li Ang, Shi Xunda, Cai Yi. Retrospective analysis of the influencing factors of chronic pain after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 558-564. |
| [9] | Zhang Jinbiao, Li Xiaoming, Xing Wanlin, Ma Fei, Yu Qiaoya, Dai Rongqin. Early warning efficacy of thrombus molecular markers after total knee arthroplasty in patients complicated with venous thromboembolism [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 572-577. |
| [10] | Yu He, Zheng Jiafa, Song Xiufeng, Guan Shengyi. Tibiotalocalcaneal arthrodesis with blood supplied fibular flap combined with hollow screw in the treatment of end-stage ankle osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 588-593. |
| [11] | Guo Yingqi, Gong Xianxu, Zhang Yan, Xiao Han, Wang Ye, Gu Wenguang. Meniscus extrusion and patellofemoral joint cartilage injury and bone marrow lesions: MRI semi-quantitative score [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 600-605. |
| [12] | Lu Hui, Wu Qimei, Liu Rong. Finite element analysis and application of unilateral and bilateral bone-filling mesh container in treatment of osteoporotic vertebral compression fracture [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 391-397. |
| [13] | You Aijia, Li Wenjie, Zhou Junli, Li Chun. Systematic evaluation of six dressings on wound safety following total hip and knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 486-492. |
| [14] | Li Mingxiu, Wang Xuan, Yang Jie, Li Yi. An osteoarthritis model in vitro: characteristics and new design idea [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(2): 300-306. |
| [15] | Liu Yinghong, Yi Yating. Mechanism and implication of angiogenesis in osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(2): 307-313. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||