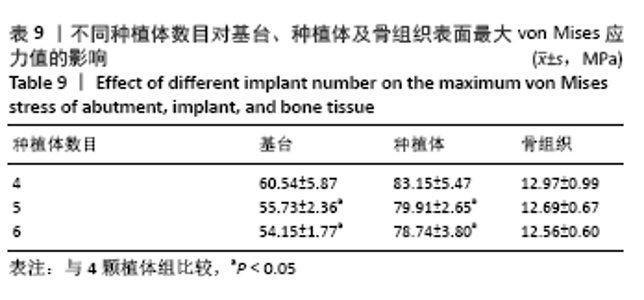
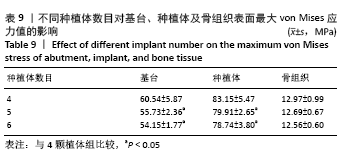
Chinese Journal of Tissue Engineering Research ›› 2022, Vol. 26 ›› Issue (4): 573-578.doi: 10.12307/2022.094
Previous Articles Next Articles
Finite element analysis of the influence of different implant designs on the stress of mandibular edentulous jaw
Wang Can1, 2, Gu Weiping1, 2, Jiang Yubin3, Zhu Lin1, 2, Chen Gang1, 2
- 1Jiangsu Key Laboratory of Oral Diseases, Nanjing Medical University, Nanjing 210029, Jiangsu Province, China; 2Department of Polyclinics, Affiliated Hospital of Stomatology, Nanjing Medical University, Nanjing 210029, Jiangsu Province, China; 3Department of Stomatology, Jiangyin People’s Hospital, Jiangyin 214400, Jiangsu Province, China
-
Received:2020-09-12Revised:2020-09-15Accepted:2020-10-24Online:2022-02-08Published:2021-11-03 -
Contact:Gu Weiping, Master’s supervisor, Chief physician, Jiangsu Key Laboratory of Oral Diseases, Nanjing Medical University, Nanjing 210029, Jiangsu Province, China; Department of Polyclinics, Affiliated Hospital of Stomatology, Nanjing Medical University, Nanjing 210029, Jiangsu Province, China -
About author:Wang Can, Master candidate, Jiangsu Key Laboratory of Oral Diseases, Nanjing Medical University, Nanjing 210029, Jiangsu Province, China; Department of Polyclinics, Affiliated Hospital of Stomatology, Nanjing Medical University, Nanjing 210029, Jiangsu Province, China -
Supported by:the Advantage Discipline Construction Project in Jiangsu Universities, No. 2018-87
CLC Number:
Cite this article
Wang Can, Gu Weiping, Jiang Yubin, Zhu Lin, Chen Gang. Finite element analysis of the influence of different implant designs on the stress of mandibular edentulous jaw[J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 573-578.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
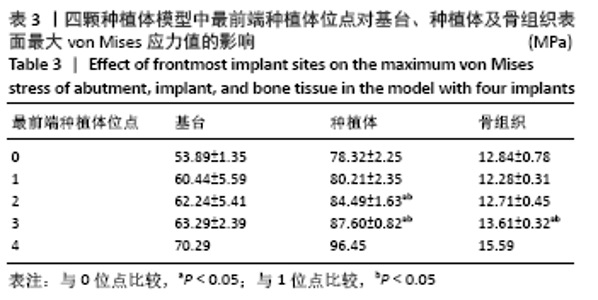
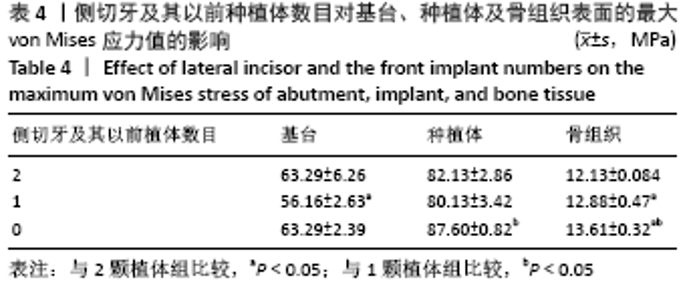
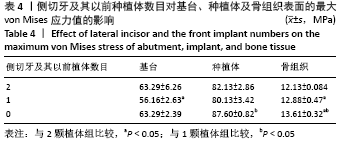
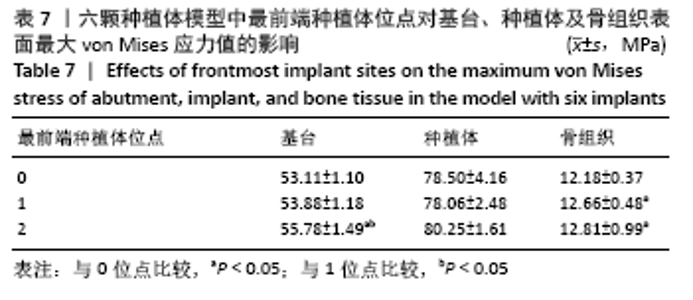
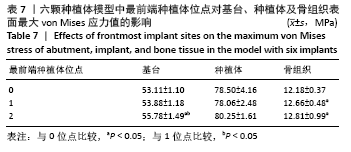
2.1.1 骨组织表面的von Mises应力值 当种植体分布为 C5-C1-D1-D5时,骨组织表面von Mises应力值最小,为12.04 MPa;当种植体分布为C5-C4-D4-D5时,骨组织表面von Mises应力值最大,为15.59 MPa。 2.1.2 最前端种植体位点对基台、种植体、骨组织表面von Mises应力值的影响 不同最前端种植体位点模型间基台表面的von Mises应力值比较差异无显著性意义(P > 0.05);最前端种植体位于0,1位点模型种植体表面von Mises应力值小于最前端种植体位于2,3位点模型(P < 0.05);最前端种植体位于1位点模型的骨组织表面von Mises应力值小于最前端种植体位于3位点模型(P < 0.05),见表3。"

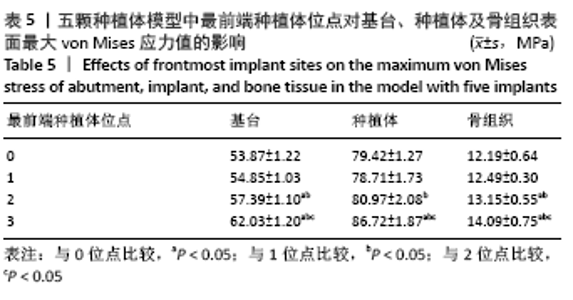
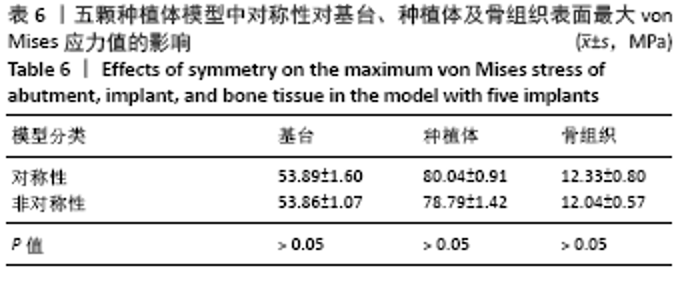
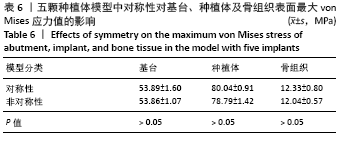
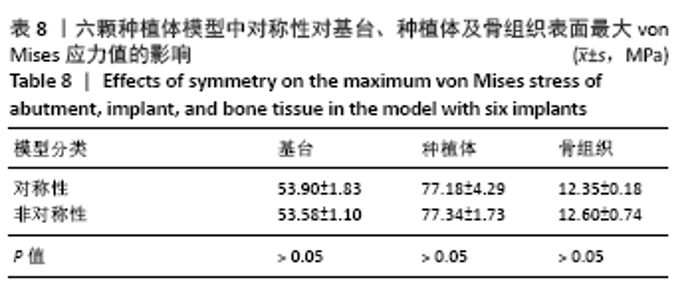
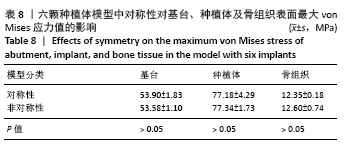
2.1.4 对称性对基台、种植体、骨组织表面von Mises应力值的影响 当最前端种植体位点相同时,对称模型骨组织表面的von Mises应力值较非对称模型小,基台及种植体表面的von Mises应力值较大。最前端植体位于1位点时,模型C5-C1-D1-D5骨组织表面的von Mises应力值最小,为 12.04 MPa;最前端植体位于2位点时,模型C5-C2-D2-D5骨组织表面的von Mises应力值最小,为12.20 MPa;最前端植体位于3位点时,模型C5-C3-D3-D5骨组织表面的von Mises应力值最小,为13.38 MPa。 2.2 五颗种植体模型间基台、种植体、骨组织表面von Mises应力值的比较 2.2.1 骨组织表面von Mises应力值 当种植体分布为 C5-C4-0-D2-D5时,骨组织表面的von Mises应力值最小,为11.61 MPa;当种植体分布为C5-C4-D3-D4-D5时,骨组织表面的von Mises应力值最大,为14.62 MPa。 2.2.2 最前端种植体位点对基台、种植体、骨组织表面von Mises应力值的影响 最前端种植体位于0,1位点模型间的基台、种植体及骨组织表面von Mises应力值比较差异无显著性意义(P > 0.05),其余各组间基台、种植体及骨组织表面von Mises应力值差异有显著性意义(P < 0.05),见表5。"

| [1] OH SH, KIM Y, PARK JY, et al. Comparison of fixed implant-supported prostheses, removable implant supported prostheses, and complete dentures: patient satisfaction and oral health-related quality of life. Clin Oral Implants Res. 2016;27(2):e31-e37. [2] YAO CJ, CAO C, BORNSTEIN MM, et al. Patient-reported outcome measures of edentulous patients restored with implant-supported removable and fixed prostheses: A systematic review. Clin Oral Implants Res. 2018;29 Suppl 16:241-254. [3] REISSMANN DR, DARD M, LAMPRECHT R, et al. Oral health-related quality of life in subjects with implant-supported prostheses: A systematic review. J Dent. 2017;65:22-40. [4] ELSYAD MA, ELGAMAL M, MOHAMMED ASKAR O, et al. Patient satisfaction and oral health-related quality of life (OHRQoL) of conventional denture, fixed prosthesis and milled bar overdenture for All-on-4 implant rehabilitation. A crossover study. Clin Oral Implants Res. 2019;30(11):1107-1117. [5] DURKAN R, OYAR P, DESTE G. Maxillary and mandibular all-on-four implant designs: A review. Niger J Clin Pract. 2019;22(8):1033-1040. [6] LIMA LB, DE FREITAS NR, NOVAIS VR, et al. Impact of Implant Number on Mandibular Implant-Supported Profile Prostheses: A Systematic Review. Int J Oral Maxillofac Implants. 2018;33(4):795-807. [7] DE LUNA GOMES JM, LEMOS CAA, SANTIAGO JUNIOR JF, et al. Optimal number of implants for complete-arch implant-supported prostheses with a follow-up of at least 5 years: A systematic review and meta-analysis. J Prosthet Dent. 2019;121(5):766-774. [8] NIEDERMAIER R, STELZLE F, RIEMANN M, et al. Implant-supported immediately loaded fixed full-arch dentures: evaluation of implant survival rates in a case cohort of up to 7 years. Clin Implant Dent Relat Res. 2017;19(1):4-19. [9] SOTO-PENALOZA D, ZARAGOZI-ALONSO R, PENARROCHA-DIAGO M, et al. The all-on-four treatment concept: Systematic review. J Clin Exp Dent. 2017;9(3): e474-e488. [10] WINDAEL S, VERVAEKE S, WIJNEN L, et al. Ten-year follow-up of dental implants used for immediate loading in the edentulous mandible: A prospective clinical study. Clin Implant Dent Relat Res. 2018;20(4):515-521. [11] ISHIGAKI S, NAKANO T, YAMADA S, et al. Biomechanical stress in bone surrounding an implant under simulated chewing. Clin Oral Implants Res. 2003;14(1):97-102. [12] EMAMI E, MICHAUD PL, SALLALEH I, et al. Implant-assisted Complete Prostheses. Periodontol 2000. 2014;66(1):119-131. [13] GOIATO MC, DE MEDEIROS RA, DA SILVA EV, et al. Biomechanical evaluation of spring system for implant-supported prosthesis: analysis by photoelasticity and extensometry. J Med Eng Technol. 2017;41(4):309-313. [14] FRASER D, FUNKENBUSCH P, ERCOLI C, et al. Biomechanical analysis of the osseointegration of porous tantalum implants. J Prosthet Dent. 2020;123(6):811-820. [15] LI H, SHI M, LIU X, et al. Uncertainty optimization of dental implant based on finite element method, global sensitivity analysis and support vector regression. Proc Inst Mech Eng H. 2019;233(2):232-243. [16] BAHADIRLI G, YILMAZ S, JONES T, et al. Influences of Implant and Framework Materials on Stress Distribution: A Three-Dimensional Finite Element Analysis Study. Int J Oral Maxillofac Implants. 2018;33(5):e117-e126. [17] MORIWAKI H, YAMAGUCHI S, NAKANO T, et al. Influence of Implant Length and Diameter, Bicortical Anchorage, and Sinus Augmentation on Bone Stress Distribution: Three-Dimensional Finite Element Analysis. Int J Oral Maxillofac Implants. 2016;31(4): e84-91. [18] SAHIN SC. Static and Dynamic Stress Analysis of Standard- and Narrow-Diameter Implants: A 3D Finite Element Analysis. Int J Oral Maxillofac Implants. 2020;35(4): e58-e68. [19] CIDADE CP, PIMENTEL MJ, AMARAL RC,et al. Photoelastic analysis of all-on-four concept using different implants angulations for maxilla. Braz Oral Res. 2014;28:S1806-8324. [20] LI X, CAO Z, QIU X, et al. Does matching relation exist between the length and the tilting angle of terminal implants in the all-on-four protocol? stress distributions by 3D finite element analysis. J Adv Prosthodont. 2015;7(3):240-248. [21] GONDA T, YASUDA D, IKEBE K, et al. Biomechanical Factors Associated With Mandibular Cantilevers: Analysis With Three-Dimensional Finite Element Models. Int J Oral Maxillofac Implants. 2014;29(6):e275-282. [22] LV J, LIU C, LAN J, et al. Three-dimensional finite element analysis of the effect of the location and diameter of implants on the stress distribution in three-unit implant-supported posterior cantilever fixed partial dentures under dynamic loads. Hua Xi Kou Qiang Yi Xue Za Zhi. 2013;31(6):552-556. [23] TAKAHASHI T, SHIMAMURA I, SAKURAI K. Influence of number and inclination angle of implants on stress distribution in mandibular cortical bone with All-on-4 Concept. J Prosthodont Res. 2010;54(4):179-184. [24] OZAN O, KURTULMUS-YILMAZ S. Biomechanical Comparison of Different Implant Inclinations and Cantilever Lengths in All-on-4 Treatment Concept by Three-Dimensional Finite Element Analysis. Int J Oral Maxillofac Implants. 2018;33(1):64-71. [25] GENG JP, TAN KB, LIU GR. Application of finite element analysis in implant dentistry: A review of the literature. J Prosthet Dent. 2001;85(6):585-598. [26] 宋少云,尹芳.有限元网格划分中的圣维南原理及其应用[J].机械设计与制造,2012(8):63-65. [27] RISMANCHIAN M, BAJOGHLI F, MOSTAJERAN Z, et al. Effect of implants on maximum bite force in edentulous patients. J Oral Implantol. 2009;35(4):196-200. [28] AYALI A, ALTAGAR M, OZAN O, et al. Biomechanical comparison of the All-on-4, M-4, and V-4 techniques in an atrophic maxilla: A 3D finite element analysis. Comput Biol Med. 2020;123:103880. [29] LIU T, MU Z, YU T, et al. Biomechanical comparison of implant inclinations and load times with the all-on-4 treatment concept: a three-dimensional finite element analysis. Comput Methods Biomech Biomed Engin. 2019;22(6):585-594. [30] HSU YT, LIN GH, WANG HI. Effects of Platform-Switching on Peri-implant Soft and Hard Tissue Outcomes: A Systematic Review and Meta-analysis. Int J Oral Maxillofac Implants. 2017;32(1):e9-e24. [31] DEL FABBRO M,BIANCHESSI C,DEL LUPO R,et al.Platform switching vs standard implants in partially edentulous patients using the Dental Tech Implant System: clinical and radiological results from a prospective multicenter study.Clin Oral Investig. 2015;19(9):2233-2244. [32] SHACKLETON JL, CARR L, SLABBERT JC, et al. Survival of fixed implant-supported prostheses related to cantilever lengths. J Prosthet Dent. 1994;71(1):23-26. [33] CORREA S, IVANCIK J, ISAZA JF, et al. Evaluation of the structural behavior of three and four implant-supported fixed prosthetic restorations by finite element analysis. J Prosthodont Res. 2012;56(2):110-119. [34] MCALARNEY ME, STAVROPOULOS DN. Determination of cantilever length-anterior-posterior spread ratio assuming failure criteria to be the compromise of the prosthesis retaining screw-prosthesis joint. Int J Oral Maxillofac Implants. 1996;11(3):331-339. [35] MCALARNEY ME, STAVROPOULOS DN. Theoretical cantilever lengths versus clinical variables in fifty-five clinical cases. J Prosthet Dent. 2000;83(3):332-343. [36] DRAGO C. Ratios of Cantilever Lengths and Anterior-Posterior Spreads of Definitive Hybrid Full-Arch, Screw-Retained Prostheses: Results of a Clinical Study. J Prosthodont. 2018;27(5):402-408. [37] BALKAYA MC. Investigation of influence of different implant size and placement on stress distribution with 3-dimensional finite element analysis. Implant Dent. 2014;23(6):716-722. [38] OGAWA T, DHALIWAL S, NAERT I, et al. Impact of implant number, distribution and prosthesis material on loading on implants supporting fixed prostheses. J Oral Rehabil. 2010;37(7):525-531. [39] SOUSA RM, SIMAMOTO-JUNIOR PC, FERNANDES-NETO AJ, et al. Influence of Connection Types and Implant Number on the Biomechanical Behavior of Mandibular Full-Arch Rehabilitation. Int J Oral Maxillofac Implants. 2016;31(4): 750-760. [40] BRANEMARK PI, SVENSSON B, VAN STEENBERGHE D. Ten-year survival rates of fixed prostheses on four or six implants ad modum Brånemark in full edentulism. Clin Oral Implants Res. 1995;6(4):227-231. |
| [1] | Wei Guoqiang, Li Yunfeng, Wang Yi, Niu Xiaofen, Che Lifang, Wang Haiyan, Li Zhijun, Shi Guopeng, Bai Ling, Mo Kai, Zhang Chenchen, Xu Yangyang, Li Xiaohe. Biomechanical analysis of non-uniform material femur under different loads [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1318-1322. |
| [2] | Zhang Yufang, Lü Meng, Mei Zhao. Construction and verification of a full spine biomechanical model of adolescent scoliosis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1351-1356. |
| [3] | Zhang Jichao, Dong Yuefu, Mou Zhifang, Zhang Zhen, Li Bingyan, Xu Xiangjun, Li Jiayi, Ren Meng, Dong Wanpeng. Finite element analysis of biomechanical changes in the osteoarthritis knee joint in different gait flexion angles [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1357-1361. |
| [4] | Li Guijun, Fang Xiaohui, Kong Weifeng, Yuan Xiaoqing, Jin Rongzhong, Yang Jun. Finite element analysis of the treatment of hallux valgus deformity by microplate combined with super strong suture elastic fixation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 938-942. |
| [5] | Wen Mingtao, Liang Xuezhen, Li Jiacheng, Xu Bo, Li Gang. Mechanical stability of Sanders II type calcaneal fractures fixed by two internal fixation methods [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 838-842. |
| [6] | Wang Hailong, Li Long, Maihemuti·Yakufu, Chen Hongtao, Liu Xu, Yilihamu·Tuoheti. Finite element analysis of stress distribution of acetabular prosthesis in the Lewinnek safety zone [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 843-847. |
| [7] | Li Shuo, Su Peng, Zhang Li, Wu Qiulong, Hu Xiangyu, Lai Yuliang. Positive effect of supracondylar femoral osteotomy on the correction of knee varus based on three-dimensional reconstruction and finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 858-863. |
| [8] | Wei Bing, Chang Shan. Finite element analysis of different angles of nail placement in sagittal plane of spinal fracture [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 864-869. |
| [9] | Liu Yuhang, Zhou Jianqiang, Xu Xuebin, Qu Xingyue, Li Ziyu, Li Kun, Wang Xing, Li Zhijun, Li Xiaohe, Zhang Shaojie. Establishment and validation of finite element model of lower cervical spine in 6-year-old children [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 870-874. |
| [10] | Guo Xiaohui, Song Xizheng, Xiang Hanrui, Kang Zhaorong, Li Daming, Kang Yu, Hu Jun, Sheng Kai. External spinal fixation elastic stress in the treatment of jumping spinal fracture [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 919-923. |
| [11] | Yang Feng, Zhao Qian, Zhang Shixuan, Zhao Tienan, Feng Bo. Effectiveness and safety of rapamycin combined with CD133 antibody stent in preventing vascular restenosis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 579-584. |
| [12] | Zhang Jianguo, Chen Chen, Hu Fengling, Huang Daoyu, Song Liang. Design and biomechanical properties of dental implant pore structure based on three-dimensional finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 585-590. |
| [13] | Chen Xiaoxu, Luo Yaxin, Bi Haoran, Yang Kun. Preparation and application of acellular scaffold in tissue engineering and regenerative medicine [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 591-596. |
| [14] | Kang Kunlong, Wang Xintao. Research hotspot of biological scaffold materials promoting osteogenic differentiation of bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 597-603. |
| [15] | Shen Jiahua, Fu Yong. Application of graphene-based nanomaterials in stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 604-609. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||