Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (5): 796-802.doi: 10.3969/j.issn.2095-4344.2438
Previous Articles Next Articles
Acromioclavicular joint dislocation: how to achieve anatomical reduction, sustained stability and micro-motion
Fang Yi, Zhao Wenzhi, Pan Deyue, Han Xin, Zhang Lu, He Hongtao, Shi Feng, Tian Tingxiao
- the Second Affiliated Hospital of Dalian Medical University, Dalian 116023, Liaoning Province, China
-
Received:2019-06-21Revised:2019-06-26Accepted:2019-07-31Online:2020-02-18Published:2020-01-15 -
Contact:Zhao Wenzhi, MD, Professor, the Second Affiliated Hospital of Dalian Medical University, Dalian 116023, Liaoning Province, China -
About author:Fang Yi, Master candidate, the Second Affiliated Hospital of Dalian Medical University, Dalian 116023, Liaoning Province, China
CLC Number:
Cite this article
Fang Yi, Zhao Wenzhi, Pan Deyue, Han Xin, Zhang Lu, He Hongtao, Shi Feng, Tian Tingxiao. Acromioclavicular joint dislocation: how to achieve anatomical reduction, sustained stability and micro-motion[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(5): 796-802.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
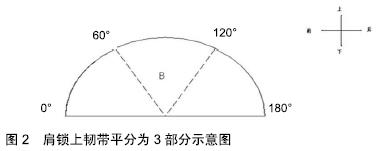
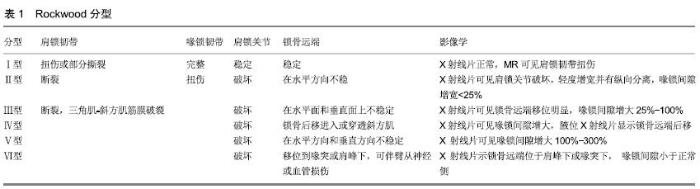
2.1 解剖及生物力学 肩锁关节是由锁骨远端和肩峰外侧缘向内2.0-3.0 cm部分组成的微动关节,是肩胛骨活动的支点。BARTH等[4]通过尸体标本研究锁骨前缘与肩峰的关系得出:肩峰关节面宽度与锁骨远端关节面宽度呈正相关,只有60%(18/30)的标本锁骨前缘与肩峰是真正对齐的,唯一可靠的解剖标志是肩峰和锁骨的关节面。肩锁关节有上下、前后、旋转3种主要运动方式,当上肢上举180°时,锁骨和肩胛骨旋转同时发生,肩锁关节只有5°-8°的活动度,这种“微动”能够缓冲锁骨远端和肩峰之间的应力。肩锁关节的稳定主要依靠动态和静态系统来维持。动态系统由三角肌和斜方肌及两者附着处的联合腱膜组成。静态系统水平方向的稳定性主要靠肩锁韧带及肩锁关节囊,肩锁韧带分布于关节囊的上、下、前、后面,其中肩锁上韧带强度最大[5],并有三角肌和斜方肌加强。MORIKAWA等[6]通过尸体标本研究发现肩锁上韧带不同区域在锁骨远端移位中所起作用不同,将肩锁上韧带平均分为3部分(A区:0°-60°;B区:60°-120°;C区:120°-180°,图2),研究证明:A+B区对抗锁骨远端后移的主要力量,A+C区是对抗锁骨远端旋转的主要力量。垂直方向的稳定性主要依靠喙锁韧带,喙锁韧带包括锥状韧带和斜方韧带两部分,斜方韧带为方形结构,从喙突呈横向走向锁骨外端下方,锥状韧带为圆锥形,从喙突螺旋形上升至锁骨,两者形成一个“V”形结构,接近于相互垂直。RIOS等[7]通过解剖研究发现锁骨远端向内占锁骨全长30%及17%处分别为锥韧带及斜方韧带在锁骨端起点,而在喙突上止点定位,锥状韧带位于喙突基底后内侧,斜方韧带位于前外侧,两者之间的骨桥不小于10 mm。MAZZOCCA等[8]观察到喙锁韧带断裂时总是锥状韧带先断裂,提示锥状韧带在悬吊上肢方面较斜方韧带作用更大,同时发现肩锁韧带在限制水平方向的移动上起主要作用。"
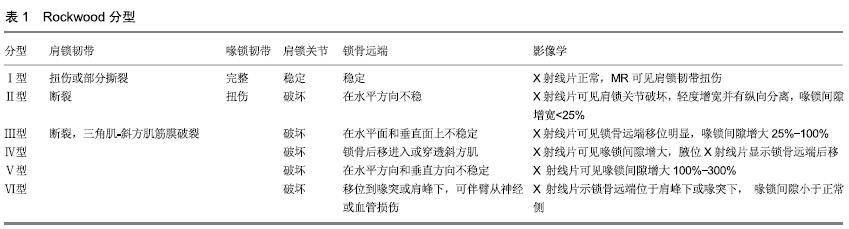
2.2 损伤机制 常见损伤机制为当肩关节处于内收位时肩峰受到外力使其向内、下移位,造成肩锁韧带、喙锁韧带损伤,也可因上肢外展位摔倒,手部着地,外力由上肢传导至肩胛骨,使肩胛骨上移牵拉损伤肩锁韧带、喙锁韧带。 2.3 诊断 2.3.1 X射线诊断 正位X射线检查测量喙锁间距。正常成年人喙锁间平均距离为1.1-1.3 cm,当患侧喙锁间距较健侧相比增大50%时,提示喙锁韧带断裂。Zanca位(X光机球管向头侧倾斜10°-15°)避免肩胛冈重叠,可以清晰地显示肩锁关节。腋位片检查主要用于观察锁骨前后移位情况,适用于RockwoodⅣ型损伤。应力位检查(前臂提拉约4.5 kg的重物),因增加患者痛苦,不建议常规检查。当发现明显肩锁关节脱位而喙锁间距正常时,应考虑喙突骨折的可能。以往对于肩锁关节脱位的影像学诊断依靠Zanca位和腋位片,由于没有关于腋位片拍摄的标准位置的文献发表,也没有确定腋位片病理改变的客观测量,同时急性损伤患者因为疼痛而无法配合导致X射线片质量下降,因此肩锁关节脱位常被漏诊。 2.3.2 超声诊断 HEERS等[9]提出仅根据X射线检查可能低估或高估软组织损伤,为了做出准确的诊断可能需要进行额外的超声检查,提出超声检查对于三角肌和斜方肌的损伤敏感性达80%,特异性达100%,对于两者之间筋膜损伤的敏感性和特异性均达100%。FARUCH BILFELD等[10]同样认为在肩锁关节损伤急性期,超声对于韧带损伤的诊断有很大价值,其中敏感性达88.9%,特异性达90.0%。 2.3.3 CT及MRI诊断 CT检查可以直观地发现有无合并骨折及锁骨远端移位情况。MRI检查对于肩锁关节韧带损伤的诊断有不可替代的作用,正常情况下肩锁韧带、喙锁韧带在T1加权像有更好的对比度,当外伤致局部软组织水肿时,T2加权像显示韧带损伤的高信号影。ALYAS等[11]提出MRI对诊断陈旧性韧带撕裂也有帮助。 作者认为对于肩锁关节脱位的诊断,X射线检查能满足大部分临床需求,但是这种检查方法也有不足,不能对软组织及软骨损伤情况作出诊断,常会出现漏诊及误诊现象。为了明确软组织损伤情况,可能需要进行额外的检查。超声检查对于急性肩锁关节损伤的韧带情况有很大诊断价值且检查费用低廉,但是由于医师经验不足及设备的限制,临床上很少用为常规检查。MRI技术是一种多角度、多参数的诊断方法,对于急性或陈旧性软组织及软骨损伤的诊断具有不可替代的作用,具有较高的临床使用价值。CT检查可清晰显示肩锁关节的对应关系,也可以精确显示喙锁间距及锁骨远端移位情况,3D成像技术更能用于微小骨折的诊断。 2.4 分型 1963年TOSSY等将肩锁关节脱位分为3型,Ⅰ型:X射线显示锁骨轻度移位,提示肩锁韧带不完全断裂,喙锁韧带完整;Ⅱ型:X射线显示锁骨远端直径的一半上翘突起超过肩峰,提示肩锁韧带完全断裂和喙锁韧带牵拉伤;Ⅲ型:X射线显示锁骨远端完全移位,锁骨与喙突之间距离明显增大,提示肩锁韧带及喙锁韧带均完全断裂。1989年ROCKWOOD等在此基础上将肩锁关节脱位的分型扩展到Ⅳ、Ⅴ、Ⅵ型,一直沿用至今,成为目前肩锁关节脱位最常用的分型系统[12],其根据锁骨远端移位程度及方向,将肩锁关节脱位分为6型(表1)。国际关节镜协会(ISAKOS)在Rockwood分型的基础上提议增加RockwoodⅢA型和ⅢB型。ⅢA型定义为稳定的损伤在顶斜位像上不伴有锁骨远端明显向上翘起及肩胛骨明显功能障碍;ⅢB型定义为不稳定的损伤伴肩胛骨难治性功能障碍和顶斜位像上锁骨远端明显向上翘起。作者没有具体说明哪一种损伤分为稳定损伤和不稳定损伤。另外还有一种变异Ⅲ型损伤,即Salter-Harris损伤,包括锁骨远端骺损伤、喙突骨折合并肩锁关节脱位,好发于年轻人。GRANVILLE-CHAPMAN等[13]对于Rockwood分型关于软组织损伤的认识提出了质疑。ESCHLER等[14]同样发现没有任何文献认为Rockwood分型描述的韧带损伤等同于影像学中发现。尽管Rockwood分型具有局限性,但其在影像学评价的作用不应忽视,有必要进一步研究制定一种改进的分类系统。 "
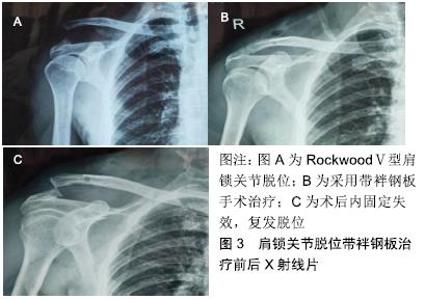
2.5 治疗 ALLEMANN等[15]就肩锁关节脱位的治疗策略问题进行了一项全国性的调查研究,结果显示:大多数医生(98.9%)对Ⅰ型和Ⅱ型肩锁关节脱位倾向于非手术治疗;96.8%的医生对于Ⅳ型、Ⅴ型和Ⅵ型同意手术治疗;对Ⅲ型的治疗,41.6%的医生选择为非手术治疗,58.4%的医生选择手术治疗。非手术治疗以吊带固定为主(63.7%),手术治疗以锁骨钩板为主(41.1%)。Rockwood Ⅰ、Ⅱ型因肩锁关节稳定性尚可,目前多采用保守治疗,如Kenny–Howard夹板、“8”字绷带、三角巾悬吊等,通常将患肢悬吊固定1-3周,对症冰敷、止痛处理,疼痛缓解后开始肩关节功能锻炼,在功能恢复且疼痛消失后可以开始运动。有些学者认为Ⅱ型损伤的治疗应当更加严格,在6-12周内不能参加接触性运动。MURRAY等[16]研究认为,虽然非手术治疗的患者恢复较快,但仍有相当一部分患者在非手术治疗后仍不满意,需要延迟手术重建。孙根文等[17]通过荟萃分析得出:手术治疗和保守治疗均能获得相似而满意的肩关节功能,但保守治疗的康复时间更短,手术治疗能获得更好的美容效果,但喙锁韧带钙化的发生率更高。TANG 等[18]通过Meta分析比较手术和保守治疗RockwoodⅢ型肩锁关节脱位的临床效果,结果显示:手术治疗与保守治疗在疼痛、创伤后关节炎、力量、功能受限、Constant评分等方面无统计学差异,而在韧带骨化、锁骨远端骨溶解等方面提示保守治疗较手术治疗发生率更低,但手术治疗在解剖重建方面优于保守治疗。由于Ⅲ型脱位肩锁韧带、喙锁韧带均断裂,肩锁关节稳定性欠佳,保守治疗无法达到功能复位的要求,因此作者倾向于手术治疗。SCHLIEMANN等[19]认为急性肩锁关节脱位的手术治疗应在3周内完成,3周后韧带残端萎缩,使得残端肌腱愈合的可能性降低。对急性肩锁关节脱位处理不当、保守治疗后失败等原因,易导致陈旧性肩锁关节脱位,FLINT等[20]将陈旧性肩锁关节脱位定义为:伤后6周且有明显脱位症状的肩锁关节脱位。WANG等[21]报道一种治疗陈旧性肩锁关节脱位的术式,将带有喙突骨块的肌肉动力性移植到锁骨上,同时联合使用锁骨钩钢板固定肩锁关节,术后取得良好的功能结果,较低的并发症发生率。祝李霖等[22]提出锁骨钩钢板联合阔筋膜治疗陈旧性肩锁关节脱位可恢复肩关节动力平衡及稳定性,具有固定牢靠、术后关节活动早、并发症少等优点。对于急性Rockwood Ⅲ型及以上肩锁关节脱位的手术方式主要分为以下两类: 2.5.1 肩锁间固定 (1)克氏针固定:以往采用克氏针交叉固定治疗肩锁关节脱位,因固定欠牢靠,克氏针断裂、游走刺破胸膜腔等并发症,临床上很少使用。 (2)锁骨远端截骨:BUSS等[23]报道了关节镜下锁骨远端部分斜切术用于治疗非嵌插RockwoodⅣ型肩锁关节脱位,虽然这种方法不能恢复肩锁关节的解剖结构,但它的好处包括创伤小、可显著减轻疼痛,改善日常生活质量,并能尽早恢复功能。肩锁韧带附着在距关节约1.5 cm的锁骨上,锁骨远端1.5 cm以上的切除可导致肩锁韧带断裂,导致肩锁关节水平不稳定[24]。而且肩锁关节之间的压缩应力能增加关节稳定性,切除锁骨远端不利于肩锁关节稳定性的恢复。 (3)锁骨钩钢板固定:目前,锁骨钩钢板是国内外治疗肩锁关节脱位最常用的方法。约有44%的外科医生使用锁骨钩钢板治疗肩锁节脱位[25]。该方法符合肩锁关节的解剖及生物力学特点,操作简单,将钢板钩插入肩峰下,钢板近端以螺钉固定,依靠杠杆作用复位并维持肩锁关节的稳定,为韧带愈合提供一个稳定的无张力环境。不同钩角的锁骨钩板可诱导锁骨和肩峰产生不同的生物力学效应。LI等[26]通过研究得出锁骨钩钢板的“钩角度”(板钩与水平面夹角)与预后相关,认为15°较0°而言具有术后肩关节疼痛减轻、康复更快等优势。较小的钩角增加锁骨中部1/3的应力,而较大的钩角增加对肩峰的应力[27]。锁骨钩钢板广泛应用于临床的同时,也带来一些不容忽视的并发症,如肩关节疼痛、肩峰撞击综合征、肩袖损伤、再脱位、骨侵蚀和磨损等[28-30]。单纯使用锁骨钩钢板固定肩锁关节而不修复重建喙锁韧带,取出内固定物后复发脱位的发生率3%-12%[28]。部分学者认为从血供方面考虑,认为无需显露、修补喙锁韧带。但断裂的喙锁韧带均有不同程度挛缩、排列紊乱,即使部分韧带瘢痕愈合,也是在松弛状态下愈合,不能发挥正常韧带应有的作用。LEE等[31]证实瘢痕愈合的喙锁韧带只有正常韧带张力强度的35%。作者认为使用锁骨钩钢板治疗肩锁关节脱位的同时应修补重建喙锁韧带。 2.5.2 喙锁间固定重建 喙锁间固定重建的代表:Bosworth法、喙突带肌肉动力性移位、Weaver-dunn术、缝合锚钉、肌腱移植及袢钢板技术等。 (1)Bosworth法:即喙锁间加压螺钉内固定术,由于螺钉断裂、松动等问题,临床很少使用。 (2)喙突带肌肉动力性移位:又称Rewar术。该术式治疗肩锁关节脱位虽取得较好效果,但需要切除锁骨远端及凿取部分喙突移位,手术创伤较大,对解剖结构破坏亦明显,临床上少用。 (3)Weaver-dunn术:包括锁骨远端切除,同时将喙肩韧带从肩峰转移到锁骨远端残端,以恢复肩锁的稳定性,该手术已被广泛研究,其失败率高达30%,生物力学强度仅为正常喙锁韧带的25%[32],改良的术式是通过直接的喙锁间固定或钩钢板来结合韧带转移,有少数研究报道与自体半腱肌移植的解剖性喙锁韧带重建技术相比,改良手术的效果较差[33]。 (4)缝合锚:生物力学研究显示,缝合锚的生物力学特性与喙锁韧带类似[34]。韩冰等[35]通过尸体研究得出:喙锁韧带断裂载荷(413.0±123.48) N,1枚锚钉失效载荷(345.1±111.23) N,2枚锚钉失效载荷(465.3±100.64) N。提示2枚锚钉较1枚锚钉重建喙锁韧带,应力得到了分散,更符合生物学特点。 (5)肌腱移植:GAROFALO等[36]报道一种采用自体腘绳肌腱移植联合三股编织缝线治疗V型肩锁关节脱位的术式,这项新技术可以在没有任何植入内固定装置、仅需部分缝线情况下实现移植肌腱的固定,取得良好效果。 (6)带袢钢板技术:近年来,带袢钢板技术逐渐兴起并被大家接受,通过在锁骨和喙突间建立骨道,以袢钢板及环袢代替喙锁韧带治疗肩锁关节脱位。袢钢板材质为钛合金,袢环为聚对苯二甲酸乙二醇酯,直径2 mm,平均强度为1 345 N,生理性喙锁韧带强度为580 N[37],理论上能够提供足够强度。该内固定装置具有固定稳定,创伤小,患者易于接受,更好地恢复关节功能,不损伤关节面,无肩峰撞击弊端,无需二次手术等优点。张黎明等[38]采用关节镜辅助下TightRope装置修复重建喙锁韧带治疗12例Ⅲ-Ⅵ型肩锁关节脱位患者,治疗效果满意。尽管应用带袢钢板重建喙锁韧带的短期疗效满意,但需获得更长时间的临床效果评价。因为此类重建方法只是暂时维持复位,需靠愈合的喙锁韧带最后维持复位,否则人工韧带终究会在反复的负荷下失效(图3)。对于术后喙锁韧带能否修复愈合并恢复受伤前的强度,目前尚缺乏相关证据。 "
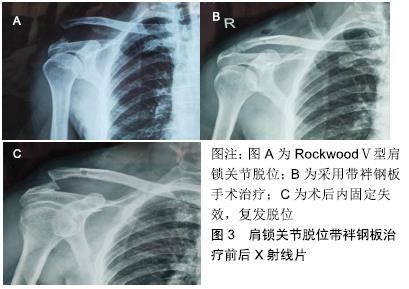
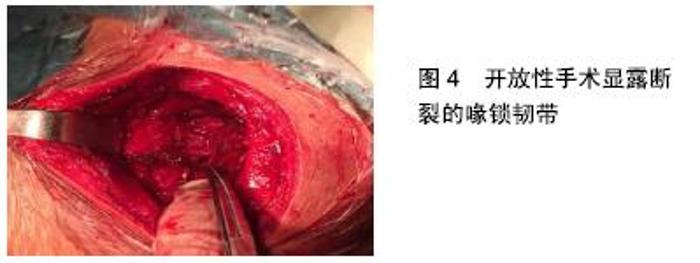
以下问题成为学者们研究的重点和难点。 (1)开放VS微创手术:在现有的文献中,开放手术和关节镜微创手术治疗肩锁关节脱位在复位的丢失率、并发症的发生率以及返修率上没有统计学差异,开放手术较关节镜手术有更高的骨折(锁骨或喙突)发生率(图4)。FAHMY等[39]通过研究表明关节镜辅助下使用带袢钢板治疗高程度肩锁关节脱位是安全的,微创手术具有良好的至优性、短期的功能康复和低发病率,但应该由受过良好肩关节镜训练的外科医生来完成。关节镜技术具有小切口、更少的软组织损伤、便于直视下寻找解剖标志、关节内微小损伤的评估及治疗等优势,与此同时,微创手术增加了肌皮神经、肩胛上神经、肩胛上动脉损伤,联合肌腱分离的风险[40]。 "
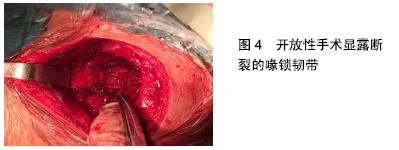
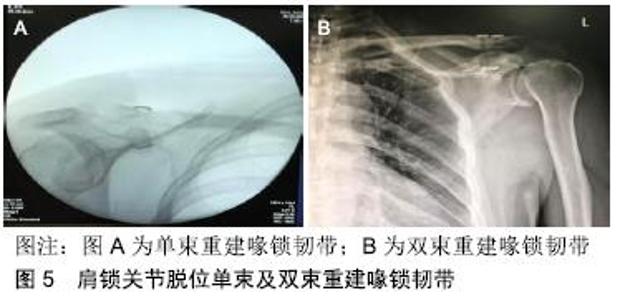
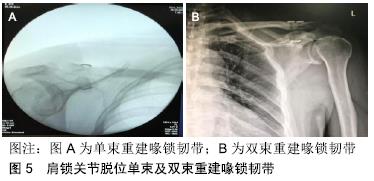
(2)单束重建 vs. 双束重建(图5):单束重建安全性较高,但忽略了锥状韧带和斜方韧带的生物力学功能,如果双束解剖重建,恢复了韧带的生物力学功能,但锁骨上需要2个骨道,增加了对锁骨骨皮质突破率,造成锁骨的最大承载力下降,存在锁骨骨折的风险。XU等[41]通过比较在关节镜辅助下单束与双束重建喙锁韧带治疗急性肩锁关节脱位的疗效,得出:双束重建喙锁韧带较单束重建相比,可获得更好的临床效果,更低的并发症(再脱位、纽扣滑脱、骨磨损、肩锁关节不稳等)发生率。LU等[42]通过比较双带袢钢板和三带袢钢板治疗肩锁关节脱位的疗效,认为两者在切口长度、失血量、手术时间、住院天数、术后Constant评分及从事以往工作的能力方面无明显差异,并且后者比前者需要花费更多的费用,同时指出,不管用双或三带袢钢板,复位的丢失仍是最普遍的并发症,导致复位丢失的主要原因是手术技术而不是带袢钢板的数量。PARK等[43]通过新鲜尸体样本研究得出双束重建喙锁韧带(锥状韧带垂直骨道,斜方韧带后外侧骨道)可以提供更好的前后方向稳定性。"

(3)重建喙锁韧带的同时是否修复肩锁韧带:SCHEIBEL等[44]通过研究得出在单独重建的喙锁韧带后,41%的病例出现持续的水平方向不稳定。部分学者证实喙锁韧带重建联合肩锁韧带加强较单纯重建喙锁韧带而言能提供更好的水平方向的稳定性[45-46]。因此,重建喙锁韧带的同时应修补肩锁韧带。 (4)钻孔的方向、位置:KOCADAL等[47]研究喙锁韧带重建技术中锁骨隧道位置对内植物负荷的影响,得出:中位隧道(隧道靠近锁骨前后缘中点)会增加了内植物的负荷,而侧向隧道(隧道远离锁骨前后缘中点)会降低了内植物的负荷,并提出术前准备时测定TR值可提高重建成功率。TR值(tunnel ratio)是由锁骨远端外侧边到每个锁骨隧道中心的距离除以锁骨总长度计算出来的[7]。EMMANUEL等[48]研究得出锥状韧带隧道TR值为0.20- 0.25,斜方韧带隧道TR值为0.13-0.16,并认为位于这些比率之外的隧道位置是造成喙锁韧带重建失败的因素之一。YU等[49]通过研究喙突纽扣钢板位置和肩锁关节脱位术后复位丢失之间的关系,得出:纽扣钢板位于喙突中心区域能获得更大的荷载及有效地减少术后复位丢失。 ZHU等[50]通过实验研究确认肩锁关节脱位解剖重建中喙锁韧带的位置和方向,实验对象是20具尸体标本的40个肩关节,分别沿着锥状韧带和斜方韧带走行插入克氏针,测量锥状韧带、斜方韧带中心到锁骨远端的距离和两枚克氏针的角度。结果显示:斜方韧带的中心距锁骨外侧端和锁骨的前缘的长度为(21.7±1.1)mm和(6.4±0.5)mm;斜方韧带的外翻角和后倾角度分别为(39.3±0.9)°和(6.0±0.6)°。锥状韧带的中心距锁骨外侧端和锁骨的后缘的距离分别为(36.6±0.9)mm和(5.5± 0.4)mm;锥状韧带外翻角和后倾角度分别为(6.6±0.7)°和(11.0±0.9)°。薛骋等[51]通过三维模型和尸体模型上施行喙锁韧带完全解剖重建技术并测量相应的钻孔参数,得出在喙突钻孔过程中,锥状韧带钻头须前倾10°-15°(平均12.4°)、外倾5°-10° (平均6.8°),斜方韧带钻头须前倾20°-30°(平均25.2°)。这些发现对于肩锁关节脱位的解剖重建具有重要意义,可以准确地确定钻孔的位置和方向。 (5)骨折的风险:肩锁关节脱位喙锁韧带重建术后喙突骨折发生率在1.7%-20%[52]。DUNN等[53]总结喙突骨折的危险因素,喙突宽度较小、手术暴露不足、钻头较粗导致骨量丢失,过早恢复活动可能增加喙突骨折的风险,此外,偏心的喙突骨隧道能增加二次骨折的风险。GONZALEZ等[54]主张钻一个直径小的骨隧道来降低骨折的风险。另外,THEOPOLD等[55]报道了一项减少术中辐射暴露的安全技术,即关节镜下可控无氟导航喙突锁骨上钻孔修复肩锁关节脱位。这种方法能够精确定位,避免重复钻孔从而减弱骨量。与传统的钻孔导轨定位相比,具有较高精确度,可降低医源性喙突骨折和固定装置移位的危险。 总之,需要明确的一点是无论何种固定方法重建喙锁韧带都无法达到解剖重建,因喙锁韧带在锁骨上的附着点是一个“面”而不是一个“点”。 2.6 术后康复锻炼 令人满意的治疗效果,不仅靠精细的手术操作,还需要正确、科学的康复锻炼。康复计划因治疗方式的不同而不同,一般情况下,在术后6周,予以吊带固定患肢,并在术后早期开始渐进式运动练习。在这一初始阶段之后,运动范围和加强练习逐渐增加,非接触式项目可于3个月后恢复,一般接触式运动可于术后6个月后进行[12]。"

| [1] PALLIS M, CAMERON KL, SVOBODA SJ,et al.Epidemiology of acromioclavicular joint injury in young athletes.Am J Sports Med. 2012; 40(9):2072-2077. [2] MARKEL J, SCHWARTING T, MALCHERCZYK D, et al. Concomitant glenohumeral pathologies in high-grade acromioclavicular separation (type III - V).BMC Musculoskelet Disord. 2017;18(1):439. [3] BEITZEL K, COTE MP, APOSTOLAKOS J,et al.Current concepts in the treatment of acromioclavicular joint dislocations.Arthroscopy. 2013 Feb;29(2):387-397. [4] BARTH J, BOUTSIADIS A, NARBONA P, et al.The anterior borders of the clavicle and the acromion are not always aligned in the intact acromioclavicular joint: a cadaveric study.J Shoulder Elbow Surg. 2017; 26(7):1121-1127. [5] MAZZOCCA AD, ARCIERO RA, BICOS J.Evaluation and treatment of acromioclavicular joint injuries.Am J Sports Med.2007;35(2):316-329. [6] MORIKAWA D, DYRNA F, COTE MP, et al.Repair of the entire superior acromioclavicular ligament complex best restores posterior translation and rotational stability.Knee Surg Sports Traumatol Arthrosc. 2018 Oct 10. [7] RIOS CG, ARCIERO RA, MAZZOCCA AD.Anatomy of the clavicle and coracoid process for reconstruction of the coracoclavicular ligaments. Am J Sports Med. 2007;35(5):811-817. [8] MAZZOCCA AD, SPANG JT, RODRIGUEZ RR, et al.Biomechanical and radiographic analysis of partial coracoclavicular ligament injuries.Am J Sports Med.Am J Sports Med. 2008;36(7):1397-1402. [9] HEERS G, HEDTMANN A.Correlation of ultrasonographic findings to Tossy's and Rockwood's classification of acromioclavicular joint injuries. Ultrasound Med Biol. 2005;31(6):725-732. [10] FARUCH BILFELD M, LAPÈGUE F, CHIAVASSA GANDOIS H, et al. Ultrasound of the coracoclavicular ligaments in the acute phase of an acromioclavicular disjonction: Comparison of radiographic, ultrasound and MRI findings.Eur Radiol. 2017;27(2):483-490. [11] ALYAS F, CURTIS M, SPEED C,et al.MR Imaging appearances of acromioclavicular joint dislocation. Radiographics. 2008;28(2):463-479. [12] VAN BERGEN CJA, VAN BEMMEL AF, ALTA TDW,et al.van Noort, New insights in the treatment of acromioclavicular separation.World J Orthop.2017;8(12):861-873. [13] GRANVILLE-CHAPMAN J, TORRANCE E, RASHID A, et al.The Rockwood classification in acute acromioclavicular joint injury does not correlate with symptoms.J Orthop Surg (Hong Kong). 2018;26(2): 2309499018777886. [14] ESCHLER A,RÖSLER K, ROTTER R, et al.Acromioclavicular joint dislocations: radiological correlation between Rockwood classification system and injury patterns in human cadaver species.Arch Orthop Trauma Surg. 2014;134(9):1193-1198. [15] ALLEMANN F, HALVACHIZADEH S, WALDBURGER M, et al. Different treatment strategies for acromioclavicular dislocation injuries: a nationwide survey on open/minimally invasive and arthroscopic concepts. Eur J Med Res. 2019;24(1):18. [16] MURRAY IR, ROBINSON PG, GOUDIE EB, et al.Robinson, Open Reduction and Tunneled Suspensory Device Fixation Compared with Nonoperative Treatment for Type-III and Type-IV Acromioclavicular Joint Dislocations: The ACORN Prospective, Randomized Controlled Trial.J Bone Joint Surg Am. 2018;100(22):1912-1918. [17] 孙根文,帕拉提•阿巴伯艾力, 李涛,等. 植入物内固定与保守疗法修复Rockwood Ⅲ型肩锁关节脱位的系统评价[J].中国组织工程研究,2016, 20(13):1946-1953. [18] TANG G, ZHANG Y, LIU Y, et al.Comparison of surgical and conservative treatment of Rockwood type-III acromioclavicular dislocation: A meta-analysis.Medicine (Baltimore). 2018;97(4):e9690. [19] SCHLIEMANN B, ROßLENBROICH SB, SCHNEIDER KN, et al. Weimann, Why does minimally invasive coracoclavicular ligament reconstruction using a flip button repair technique fail? An analysis of risk factors and complications.Knee Surg Sports Traumatol Arthrosc. 2015;23(5):1419-1425. [20] FLINT JH, WADE AM, GIULIANI J, et al. Defining the terms acute and chronic in orthopaedic sports injuries: a systematic review.Am J Sports Med.2014;42(1):235-241. [21] WANG Y, ZHANG J.Acromioclavicular joint reconstruction by coracoid process transfer augmented with hook plate.Injury. 2014;45(6):949-954. [22] 祝李霖,黄东,吴伟炽,等.锁骨钩钢板联合阔筋膜治疗陈旧性肩锁关节脱位[J].中华创伤骨科杂志,2016, 18(6):542-544. [23] BUSS DD, ANDERSON K, TERVOLA N, et al.Giveans, Posterior Distal Clavicle Beveling for Chronic Nonincarcerated Type IV Acromioclavicular Separations: Surgical Technique and Early Clinical Outcomes, Arthroscopy. 2017;33(1):84-89. [24] PONCE BA, MILLETT PJ, WARNER JJ. Acromioclavicular joint instability-reconstruction indications and techniques, Operative Techniques in Sports Medicine.2004;12(1):35-42. [25] THOMAS K, LITSKY A, JONES G,et al.Biomechanical comparison of coracoclavicular reconstructive techniques.Am J Sports Med. 2011; 39(4):804-810. [26] LI G, LIU T, SHAO X, et al.Fifteen-degree clavicular hook plate achieves better clinical outcomes in the treatment of acromioclavicular joint dislocation.J Int Med Res.J Int Med Res. 2018;46(11):4547-4559. [27] HUNG LK, SU KC, LU WH, et al. Biomechanical analysis of clavicle hook plate implantation with different hook angles in the acromioclavicular joint.Int Orthop. 2017;41(8):1663-1669. [28] KIENAST B, THIETJE R, QUEITSCH C, et al. Mid-term results after operative treatment of rockwood grade III-V Acromioclavicular joint dislocations with an AC-hook-plate.Eur J Med Res. 2011;16(2):52-56. [29] LIN HY, WONG PK, HO WP, et al.Clavicular hook plate may induce subacromial shoulder impingement and rotator cuff lesion - dynamic sonographic evaluation.J Orthop Surg Res. 2014;9:6. [30] KIM E, LEE S, JEONG HJ, et al.Three-dimensional scapular dyskinesis in hook-plated acromioclavicular dislocation including hook motion.J Shoulder Elbow Surg. 2018;27(6):1117-1124. [31] LEE YS, LAU MJ, TSENG YC, et al.Comparison of the efficacy of hook plate versus tension band wire in the treatment of unstable fractures of the distal clavicle.Int Orthop. 2009;33(5):1401-1405. [32] LEE S, BEDI A.Shoulder acromioclavicular joint reconstruction options and outcomes, Curr Rev Musculoskelet Med.2016; 9(4):368-377. [33] BEITZEL K, OBOPILWE E, CHOWANIEC DM, et al. Biomechanical properties of repairs for dislocated AC joints using suture button systems with integrated tendon augmentation, Knee Surg Sports Traumatol Arthrosc.2012;20(10):1931-1938. [34] WELLMANN M, ZANTOP T, WEIMANN A, et al. Biomechanical evaluation of minimally invasive repairs for complete acromioclavicular joint dislocation.Am J Sports Med. 2007;35(6):955-961. [35] 韩冰,冯晖,陈烁,等.修复Ⅲ度肩锁关节脱位:带线锚钉重建喙锁韧带的生物力学变化[J].中国组织工程研究,2015,19(4):568-572. [36] GAROFALO R, CECCARELLI E, CASTAGNA A, et al.Open capsular and ligament reconstruction with semitendinosus hamstring autograft successfully controls superior and posterior translation for type V acromioclavicular joint dislocation.Knee Surg Sports Traumatol Arthrosc. 2017;25(7):1989-1994. [37] WELLMANN M, KEMPKA JP, SCHANZ S, et al.Coracoclavicular ligament reconstruction: biomechanical comparison of tendon graft repairs to a synthetic double bundle augmentation.Knee Surg Sports Traumatol Arthrosc. 2009;17(5):521-528. [38] 张黎明,汪志芳,施海伟.关节镜辅助锁扣带袢双钛板TightRope置入修复肩锁关节脱位:早期即可坚强固定[J].中国组织工程研究,2015,19(9): 1441-1446. [39] FAHMY FS, FATHI H, ELATTAR M.Clinical outcomes of arthroscopic assissted fixation of acute high grade acromioclavicular joint disruption. J Orthop. 2019;16(2):133-136. [40] MARSALLI M, MORAN N, LASO JI.Arthroscopic Acromioclavicular Joint Reconstruction With TightRope and FiberTape Loop.Arthrosc Tech. 2018;7(11):e1103-e1108. [41] XU J, LIU H, LU W, et al.A retrospective comparative study of arthroscopic fixation in acute Rockwood type IV acromioclavicular joint dislocation: single versus double paired Endobutton technique.BMC Musculoskelet Disord. 2018;19(1):170. [42] LU D, WANG T, CHEN H, et al.A comparison of double Endobutton and triple Endobutton techniques for acute acromioclavicular joint dislocation.Orthop Traumatol Surg Res. 2016;102(7):891-895. [43] PARK I, ITAMI Y, HEDAYATI B, et al.Biomechanical Analysis of Single-, Double-, and Triple-Bundle Configurations for Coracoclavicular Ligament Reconstruction Using Cortical Fixation Buttons With Suture Tapes: A Cadaveric Study.Arthroscopy. 2018;34(11):2983-2991. [44] SCHEIBEL M, DRÖSCHEL S, GERHARDT C, et al. Arthroscopically assisted stabilization of acute high-grade acromioclavicular joint separations.Am J Sports Med. 2011;39(7):1507-1516. [45] JORDAN RW, MALIK S, BENTICK K, et al.Acromioclavicular joint augmentation at the time of coracoclavicular ligament reconstruction fails to improve functional outcomes despite significantly improved horizontal stability, Knee Surg Sports Traumatol Arthrosc. 2018 Sep 28 [46] SAIER T, VENJAKOB AJ, MINZLAFF P, et al.Value of additional acromioclavicular cerclage for horizontal stability in complete acromioclavicular separation: a biomechanical study.Knee Surg Sports Traumatol Arthrosc. 2015;23(5):1498-1505. [47] KOCADAL O, YÜKSEL K, GÜVEN M.Evaluation of the clavicular tunnel placement on coracoclavicular ligament reconstruction for acromioclavicular dislocations: a finite element analysis.Int Orthop. 2018;42(8):1891-1896. [48] EISENSTEIN ED, LANZI JT, WATERMAN BR, et al. Medialized Clavicular Bone Tunnel Position Predicts Failure After Anatomic Coracoclavicular Ligament Reconstruction in Young, Active Male Patients.Am J Sports Med. 2016;44(10):2682-2689. [49] YU XB, LI T, HU W, et al.Position of Coracoid Button Predicts Loss of Reduction in Acromioclavicular Joint Dislocation Patients Treated With the Suture-Button.J Invest Surg. 2019:1-6. [50] ZHU NF, RUI BY, ZHANG YL,et al.Anatomic study of coracoclavicular ligaments for reconstruction of acromioclavicular joint dislocations.J Orthop Sci. 2016;21(6):749-752. [51] 薛骋,徐海波,宋李军,等.喙锁韧带完全解剖重建的钻孔技术研究[J].中华创伤骨科杂志, 2015,17(4):337-341. [52] MARTETSCHLÄGER F, HORAN MP, WARTH RJ, et al. Complications after anatomic fixation and reconstruction of the coracoclavicular ligaments. Am J Sports Med. 2013;41(12):2896-903. [53] DUNN JC, WATERMAN BR.Successful nonoperative management of coracoid fracture associated with suture-button fixation of acromioclavicular separation.Mil Med. 2015;180(1):e138-41. [54] GONZALEZ R, DAMACEN H, NYLAND J,et al. Acromioclavicular joint reconstruction using peroneus brevis tendon allograft.Arthroscopy. 2007;23(7):788.e1-4. [55] THEOPOLD J, MARQUASS B, VON DERCKS N, et al. Arthroscopically guided navigation for repair of acromioclavicular joint dislocations: a safe technique with reduced intraoperative radiation exposure. Patient Saf Surg. 2015;9:41. |
| [1] | Zhang Shangpu, Ju Xiaodong, Song Hengyi, Dong Zhi, Wang Chen, Sun Guodong. Arthroscopic suture bridge technique with suture anchor in the treatment of acromioclavicular dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1417-1422. |
| [2] | Zhang Chao, Lü Xin. Heterotopic ossification after acetabular fracture fixation: risk factors, prevention and treatment progress [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1434-1439. |
| [3] | Wang Debin, Bi Zhenggang. Related problems in anatomy mechanics, injury characteristics, fixed repair and three-dimensional technology application for olecranon fracture-dislocations [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1446-1451. |
| [4] | Zhang Lei, Ma Li, Fu Shijie, Zhou Xin, Yu Lin, Guo Xiaoguang. Arthroscopic treatment of greater tuberosity avulsion fractures with anterior shoulder dislocation using the double-row suture anchor technique [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 895-900. |
| [5] | Song Shan, Hu Fangyuan, Qiao Jun, Wang Jia, Zhang Shengxiao, Li Xiaofeng. An insight into biomarkers of osteoarthritis synovium based on bioinformatics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 785-790. |
| [6] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [7] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Comparison of the advantages and disadvantages of multiple implants in treatment of traumatic dislocation of sternoclavicular joint [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 443-448. |
| [8] | Li Yang, Zhang Mingyong. Meta-analysis of the effect of double Endobutton and clavicular hook plate on the treatment of acromioclavicular dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 463-470. |
| [9] | Cheng Chongjie, Yan Yan, Zhang Qidong, Guo Wanshou. Diagnostic value and accuracy of D-dimer in periprosthetic joint infection: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3921-3928. |
| [10] | Huang Maomao, Hu Yue, Wang Binchuan, Zhang Chi, Xie Yujie, Wang Jianxiong, Wang Li, Xu Fangyuan. Bibliometric and visual analysis of international literature addressing ischemic stroke rehabilitation in recent 10 years [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3725-3733. |
| [11] | Liu Zhiwei, Xie Rui, Sun Kai, Li Kaiming, Wang Xiongwei, Zhan Jiawen, Zhu Liguo. Interpretation of diagnostic criteria for cervicogenic headache: challenges and understandings in diagnosis and differential diagnosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3746-3751. |
| [12] | Jiang Xiaoyan, Zhu Haifei, Lin Haiqi, Lin Wentao. Cold therapy promotes self-limited recovery of delayed-onset muscle soreness [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3609-3613. |
| [13] | Zuo Zhenkui, Han Jiarui, Ji Shuling, He Lulu. Pretreatment with ginkgo biloba extract 50 alleviates radiation-induced acute intestinal injury in mice [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3666-3671. |
| [14] | Lin Tianye, Yang Peng, Xiong Binglang, He Xiaoming, Yan Xinhao, Zhang Jin, He Wei, Wei Qiushi . Comparison of preoperative three-dimensional reconstruction simulation and intraoperative drawing of femoral osteotomy to measure rotation angle in vitro [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3349-3353. |
| [15] | Wang Yanjiao, Wang Rui, Sun Luning. Bankart pepair versus Bristow-Latarjet procedure for recurrent anterior instability of the shoulder: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3423-3430. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||