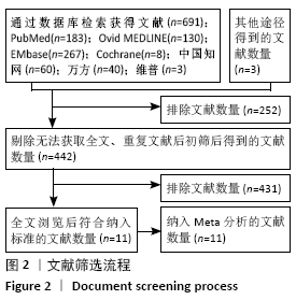
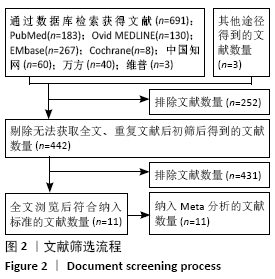
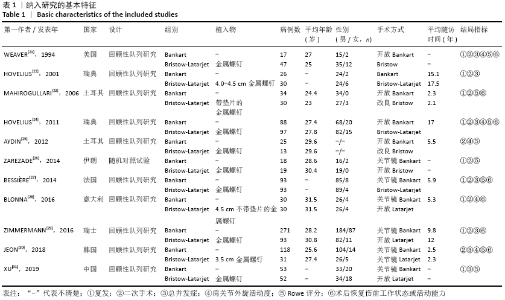
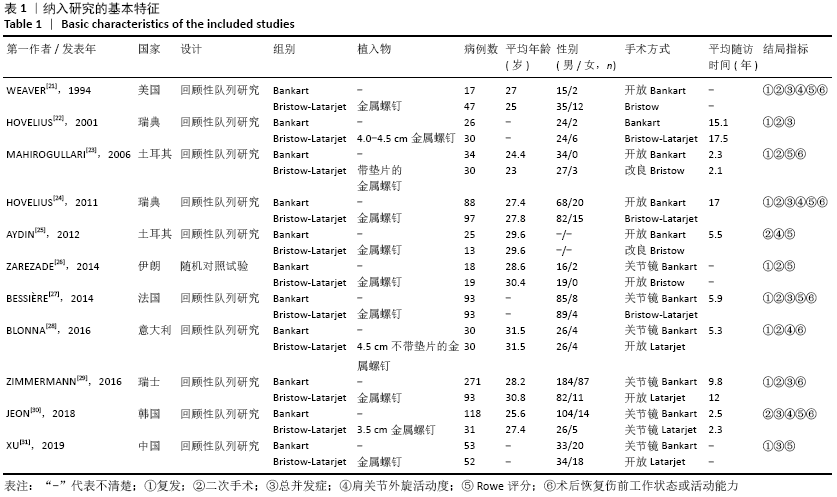
Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (21): 3423-3430.doi: 10.3969/j.issn.2095-4344.3860
Previous Articles Next Articles
Bankart pepair versus Bristow-Latarjet procedure for recurrent anterior instability of the shoulder: a meta-analysis
Wang Yanjiao1, Wang Rui1, Sun Luning2
- 1Graduate Department of Nanjing Sport Institute, Nanjing 210014, Jiangsu Province, China; 2Orthopedic Department of Affiliated Hospital of Nanjing University of Chinese Medicine, Nanjing 210029, Jiangsu Province, China
-
Received:2020-08-18Revised:2020-08-21Accepted:2020-09-15Online:2021-07-28Published:2021-01-25 -
Contact:Sun Luning, MD, Chief physician, Orthopedic Department of Affiliated Hospital of Nanjing University of Chinese Medicine, Nanjing 210029, Jiangsu Province, China -
About author:Wang Yanjiao, Master candidate, Graduate Department of Nanjing Sport Institute, Nanjing 210014, Jiangsu Province, China -
Supported by:the Science and Technology Project of Jiangsu Province, No. BK20191505 (to SLN)
CLC Number:
Cite this article
Wang Yanjiao, Wang Rui, Sun Luning. Bankart pepair versus Bristow-Latarjet procedure for recurrent anterior instability of the shoulder: a meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3423-3430.
share this article
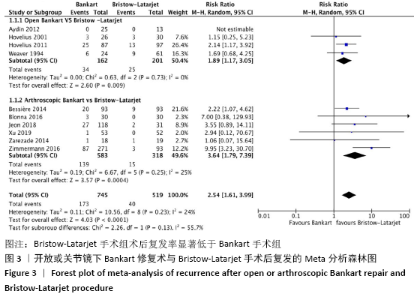
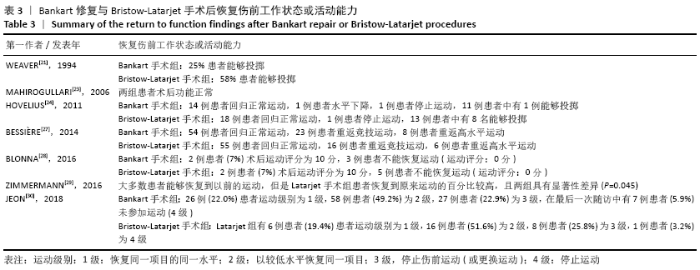
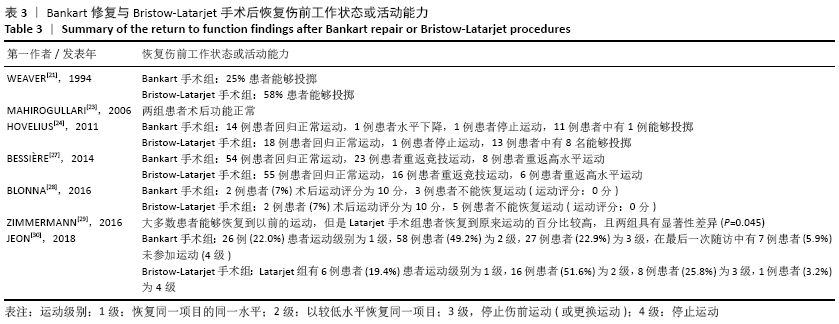
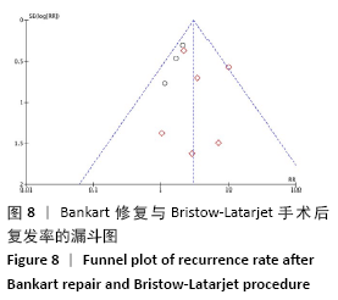
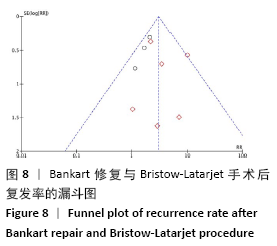
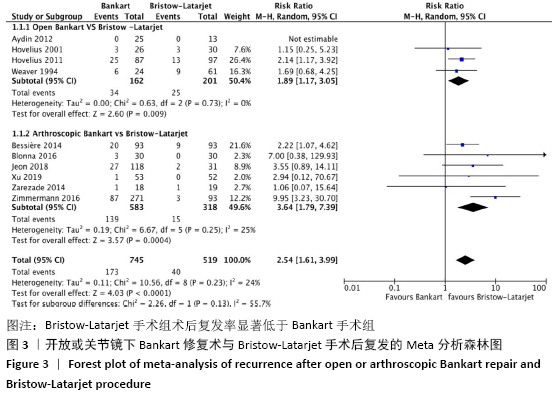
2.4 Meta分析结果 2.4.1 两种方式手术后复发不稳的Meta分析结果 有10项研究报告了两种手术术后复发的结果[21-22,24-31]。在这些研究中,未发现明显的异质性(I2=24%),采用固定效应模型。Bankart手术组有23.3%(n=173)、Bristow-Latarjet手术组有7.7% (n=40)术后出现半脱位或脱位。Bristow-Latarjet手术后复发率更低(RR=2.54,95%CI:1.61-3.99,P < 0.000 1)。 将Bankart修复分为开放治疗和关节镜下治疗2种方式时,Bristow-Latarjet手术组复发率仍显著低于开放Bankart手术组(RR=1.89,95%CI:1.17-3.05,P=0.009)和关节镜下Bankart手术组(RR=3.64,95%CI:1.79-7.39,P= 0.000 4),见图3。 "
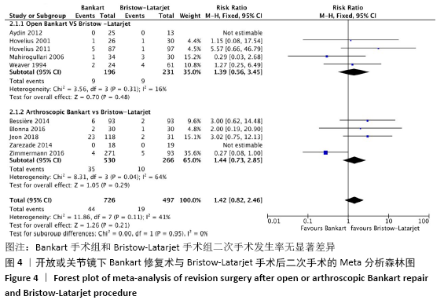
2.4.2 两种方式手术后二次手术的Meta分析结果 有10项研究报告了由于复发不稳而进行二次手术的结果[21-30]。在这些研究中,未发现明显的异质性(I2=41%),采用固定效应模型。Bankart手术组有6.1%(n=44)、Bristow-Latarjet手术组有3.8% (n=19)病例需要进行二次手术。两组二次手术发生率无显著差异(RR=1.42,95%CI:0.82-2.46,P= 0.21)。 将Bankart修复分为开放治疗和关节镜下治疗2种方式时,Bristow-Latarjet手术组二次手术发生率与开放Bankart手术组(RR=1.39,95%CI:0.56- 3.45,P=0.48)和关节镜下Bankart手术组(RR=1.44,95%CI:0.73-2.85,P= 0.29)仍无显著差异,见图4。关节镜下Bankart手术组与Latarjet手术组二次手术发生率异质性较高,异质性文献为ZIMMERMANN等[29]的研究,异质性来源考虑可能与纳入文献的样本量以及随访时间有关。 "
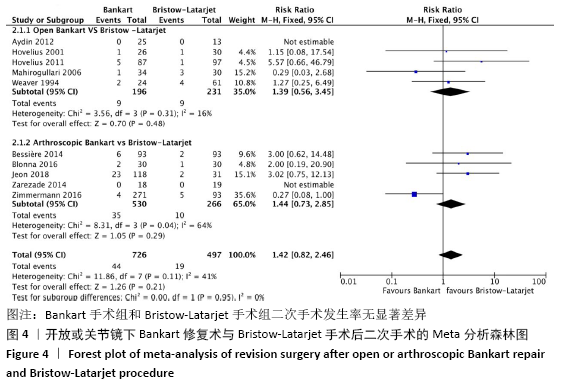
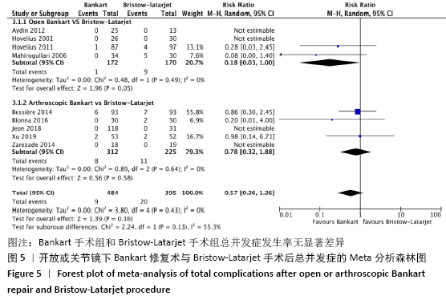
2.4.3 两种方式手术后总并发症发生率的Meta分析结果 有9项研究报告了术后总并发症的结果[22-28,30-31]。在这些研究中,未发现明显的异质性(I2=0%),采用固定效应模型。Bankart手术组有1.9%(n=9)、Bristow-Latarjet手术组有5.1% (n=20)病例出现并发症。两组总并发症发生率无显著差异(RR=0.57,95%CI:0.26-1.26,P=0.16)。 将Bankart修复分为开放治疗和关节镜下治疗2种方式时,Bristow-Latarjet手术组总并发症发生率与开放Bankart手术组(RR=0.18,95%CI:0.03-1.00,P=0.05)和关节镜下Bankart手术组(RR=0.78,95%CI:0.32-1.88,P=0.16)仍无显著差异,见图5。 "
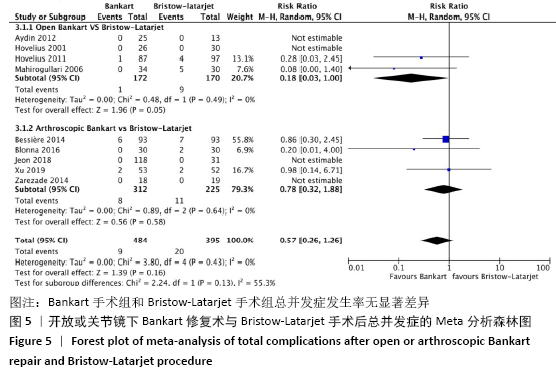
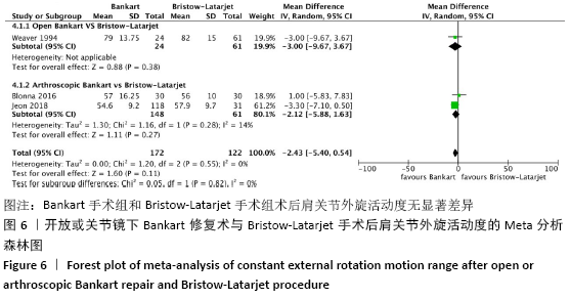
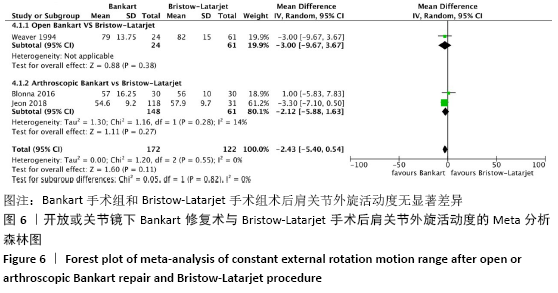
2.4.4 两种方式手术后肩关节外旋活动度的Meta分析结果 所纳入的11篇文献中,部分文献未提供完整的外旋活动度标准差,根据1项研究提供的利用极差来估算标准差的方法[26],从而获得更多的数据在 Meta 分析中被合理利用。经估算后,共有3项研究被纳入研究,未发现明显的异质性(I2=0),采用固定效应模型。Bankart手术组肩关节平均外旋活动度为63.5°,Bristow-Latarjet手术组肩关节平均外旋活动度为65.3°。两组术后肩关节外旋活动度无显著差异(WMD= -2.43,95%CI:-5.40-0.54,P=0.11)。 将Bankart修复分为开放治疗和关节镜下治疗2种方式时,Bristow-Latarjet手术组与开放Bankart 手术组肩关节外旋活动度无显著差异(WMD= -3.00,95%CI:-9.67-3.67,P=0.38),同样,Bristow-Latarjet手术组与关节镜下Bankart手术组的术后肩关节外旋活动度也没有显著差异(WMD=-2.12,95%CI:-5.88-1.63,P=0.27),见图6。"
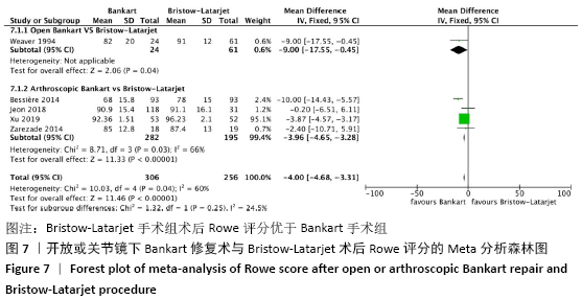
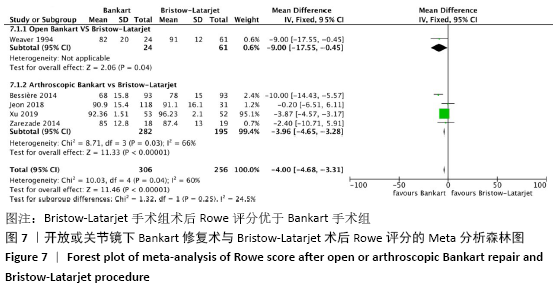
2.4.5 两种方式手术后肩关节Rowe评分的Meta分析结果 采用2.4.4相同的估算方法,共纳入5篇文献,异质性较大(I2 > 50%),异质性文献为Bessière研究,异质性来源可能与原文献未提供完整的研究数据有关,采用随机效应模型。Bankart组Rowe平均得分为83.7,Bristow-Latarjet组Rowe平均得分为88.7分,两组Rowe评分的加权平均差为-4.00,表明Bristow-Latarjet手术组术后Rowe评分优于Bankart手术组(WMD=-4.00,95%CI:-4.68至-3.31,P < 0.000 01)。 将Bankart修复分为开放治疗和关节镜下治疗2种方式时,Bristow-Latarjet手术组的术后Rowe评分仍高于开放Bankart手术组(WMD=-9.00,95%CI:-17.55至-0.45,P=0.04)和关节镜Bankart手术组(WMD=-3.96,95%CI:-4.65至-3.28,P < 0.000 01),见图7。 "
| [1] STREUBEL PN, KRYCH AJ, SIMONE JP, et al. Anterior glenohumeral instability: a pathology-based surgical treatment strategy. J Am Acad Orthop Surg. 2014;22(5):283-294. [2] 朱伟民,王大平,陆伟,等.复发性肩关节前脱位的关节镜下病理分型研究[J].中国内镜杂志, 2010,16(3):237-241. [3] MOURA DL, REIS ARE, FERREIRA J, et al. Modified Bristow-Latarjet procedure for treatment of recurrent traumatic anterior glenohumeral dislocation. Rev Bras Ortop. 2018;53(2):176-183. [4] 朱以明,姜春岩,鲁谊,等.全关节镜下手术治疗骨性Bankart损伤的术后疗效分析[J].中华外科杂志,2011,49(7):603-606. [5] PORCELLINI G, CAMPI F, PALADINI P. Arthroscopic approach to acute bony Bankart lesion. Arthroscopy. 2002;18(7):764-769. [6] BIGLIANI LU, NEWTON PM, STEINMANN SP, et al. Glenoid rim lesions associated with recurrent anterior dislocation of the shoulder. Am J Sports Med. 1998;26(1):41-45. [7] CHUANG TY, ADAMS CR, BURKHART SS. Use of preoperative three-dimensional computed tomography to quantify glenoid bone loss in shoulder instability. Arthroscopy. 2008;24(4):376-382. [8] BOTTONI CR, SMITH EL, BERKOWITZ MJ, et al. Arthroscopic versus open shoulder stabilization for recurrent anterior instability: a prospective randomized clinical trial. Am J Sports Med. 2006;34(11):1730-1737. [9] BROWN L, ROTHERMEL S, JOSHI R, et al. Recurrent instability after arthroscopic bankart reconstruction: a systematic review of surgical technical factors. Arthroscopy. 2017;33(11): 2081-2092. [10] RASHID MS, ARNER JW, MILLETT PJ, et al. The bankart repair: past, present, and future. J Shoulder Elbow Surg. 2020. doi: 10.1016/j.jse.2020.06.012. [11] DEFRODA SF, MEHTA N, OWENS BD. Physical therapy protocols for arthroscopic bankart repair. Sports Health. 2018;10(3):250-258. [12] DONOHUE MA, MAUNTEL TC, DICKENS JF. Recurrent shoulder instability after primary bankart repair. Sports Med Arthrosc Rev. 2017; 25(3):123-130. [13] MIURA K, TSUDA E, TOHYAMA H, et al. Can arthroscopic Bankart repairs using suture anchors restore equivalent stability to open repairs in the management of traumatic anterior shoulder dislocation? A meta-analysis. J Orthop Sci. 2018;23(6):935-941. [14] FREEDMAN KB, SMITH AP, ROMEO AA, et al. Open Bankart repair versus arthroscopic repair with transglenoid sutures or bioabsorbable tacks for Recurrent Anterior instability of the shoulder: a meta-analysis. Am J Sports Med. 2004;32(6):1520-1527. [15] LATARJET M. Treatment of recurrent dislocation of the shoulder. A propos du traitement des luxations récidivantes de l’épaule. Lyon Chir. 1954;49(8):994-997. [16] HELFET AJ. Coracoid transplantation for recurring dislocation of the shoulder. J Bone Joint Surg Br. 1958;40-B(2):198-202. [17] ROLLICK NC, ONO Y, KURJI HM, et al. Long-term outcomes of the Bankart and Latarjet repairs: a systematic review. Open Access J Sports Med. 2017;8:97-105. [18] YANG JS, MEHRAN N, MAZZOCCA AD, et al. Remplissage versus modified latarjet for off-track hill-sachs lesions with subcritical glenoid bone loss. Am J Sports Med. 2018;46(8): 1885-1891. [19] HIGGINS JPT, GREEN S. Cochrane handbook for systematic reviews of interventions version 5.1.0 . The Cochrane collaboration (2011). http://training.cochrane.org/handbook. [20] BAÑARES R, ALBILLOS A, RINCÓN D, et al. Endoscopic treatment versus endoscopic plus pharmacologic treatment for acute variceal bleeding: a meta-analysis. Hepatology. 2002;35(3):609-615. [21] WEAVER JK, DERKASH RS. Don’t forget the Bristow-Latarjet procedure. Clin Orthop Relat Res. 1994;(308):102-110. [22] HOVELIUS LK, SANDSTRÖM BC, RÖSMARK DL, et al. Long-term results with the Bankart and Bristow-Latarjet procedures: recurrent shoulder instability and arthropathy. J Shoulder Elbow Surg. 2001;10(5):445-452. [23] MAHIROGULLARI M, KUSKUCU M, SOLAKOGLU C, et al. Comparison of outcomes of two different surgeries in regarding to complications for chronic anterior shoulder instability. Arch Orthop Trauma Surg. 2006; 126(10):674-679. [24] HOVELIUS L, VIKERFORS O, OLOFSSON A, et al. Bristow-Latarjet and Bankart: a comparative study of shoulder stabilization in 185 shoulders during a seventeen-year follow-up. J Shoulder Elbow Surg. 2011;20(7):1095-1101. [25] AYDIN A, USTA M, TOPAL M, et al. Comparison of Open Bankart Repair versus Modified Bristow Operation for the Treatment of Traumatic Recurrent Anterior Dislocation and Capsular Laxity of the Shoulder. Eurasian J Med. 2012; 44(3):157-162. [26] ZAREZADE A, DEHGHANI M, ROZATI AR, et al. Comparison of Bristow procedure and Bankart arthroscopic method as the treatment of recurrent shoulder instability. Adv Biomed Res. 2014;3:256. [27] BESSIÈRE C, TROJANI C, CARLES M, et al. The open latarjet procedure is more reliable in terms of shoulder stability than arthroscopic bankart repair. Clin Orthop Relat Res. 2014; 472(8):2345-2351. [28] BLONNA D, BELLATO E, CARANZANO F, et al. Arthroscopic bankart repair versus open bristow-latarjet for shoulder instability: a matched-pair multicenter study focused on return to sport. Am J Sports Med. 2016;44(12): 3198-3205. [29] ZIMMERMANN SM, SCHEYERER MJ, FARSHAD M, et al. Long-term restoration of anterior shoulder stability: a retrospective analysis of arthroscopic bankart repair versus open latarjet procedure. J Bone Joint Surg Am. 2016; 98(23):1954-1961. [30] JEON YS, JEONG HY, LEE DK, et al. Borderline glenoid bone defect in anterior shoulder instability: latarjet procedure versus bankart repair. Am J Sports Med. 2018;46(9):2170-2176. [31] XU Y, WU K, MA Q, et al. Comparison of clinical and patient-reported outcomes of three procedures for recurrent anterior shoulder instability: arthroscopic Bankart repair, capsular shift, and open Latarjet. J Orthop Surg Res. 2019;14(1):326. [32] WOODMASS JM, WAGNER ER, SOLBERG M, et al. Latarjet procedure for the treatment of anterior glenohumeral instability. JBJS Essent Surg Tech. 2019;9(3):e31. [33] AN VV, SIVAKUMAR BS, PHAN K, et al. A systematic review and meta-analysis of clinical and patient-reported outcomes following two procedures for recurrent traumatic anterior instability of the shoulder: latarjet procedure vs. Bankart repair. J Shoulder Elbow Surg. 2016; 25(5):853-863. [34] LACHETA L, SIEBENLIST S, IMHOFF AB, et al. Rezidivinstabilität und Instabilitätsarthropathie Recurrent instability and instability arthropathy. Unfallchirurg. 2018;121(2):142-151. [35] BLIVEN KCH, PARR GP. Outcomes of the Latarjet Procedure Compared With Bankart Repair for Recurrent Traumatic Anterior Shoulder Instability. J Athl Train. 2018;53(2):181-183. [36] DOMOS P, CHELLI M, LUNINI E, et al. Clinical and radiographic outcomes of the open Latarjet procedure in skeletally immature patients. J Shoulder Elbow Surg. 2020;29(6):1206-1213. [37] BESSIERE C, TROJANI C, PÉLÉGRI C, et al. Coracoid bone block versus arthroscopic Bankart repair: a comparative paired study with 5-year follow-up. Orthop Traumatol Surg Res. 2013;99(2):123-130. [38] BURKHART SS, DE BEER JF. Traumatic glenohumeral bone defects and their relationship to failure of arthroscopic Bankart repairs: significance of the inverted-pear glenoid and the humeral engaging Hill-Sachs lesion. Arthroscopy. 2000;16(7):677-694. [39] LOCHER J, WILKEN F, BEITZEL K, et al. Hill-Sachs Off-track Lesions as Risk Factor for Recurrence of Instability After Arthroscopic Bankart Repair. Arthroscopy. 2016;32(10):1993-1999. [40] DEFRODA S, BOKSHAN S, STERN E, et al. Arthroscopic Bankart Repair for the Management of Anterior Shoulder Instability: indications and Outcomes. Curr Rev Musculoskelet Med. 2017;10(4):442-451. [41] HOVELIUS L, SANDSTRÖM B, SUNDGREN K, et al. One hundred eighteen Bristow-Latarjet repairs for recurrent anterior dislocation of the shoulder prospectively followed for fifteen years: study I-clinical results. J Shoulder Elbow Surg. 2004;13(5):509-516. [42] HOVELIUS L, SANDSTRÖM B, SAEBÖ M. One hundred eighteen Bristow-Latarjet repairs for recurrent anterior dislocation of the shoulder prospectively followed for fifteen years: study II-the evolution of dislocation arthropathy. J Shoulder Elbow Surg. 2006;15(3):279-289. [43] BURKHART SS, DE BEER JF, BARTH JR, et al. Results of modified Latarjet reconstruction in patients with anteroinferior instability and significant bone loss. J Arthroscopy. 2007;23(10):1033-1041. [44] DOMOS P, LUNINI E, WALCH G. Contraindications and complications of the Latarjet procedure. Shoulder Elbow. 2018;10(1):15-24. [45] BOILEAU P, GENDRE P, BABA M, et al. A guided surgical approach and novel fixation method for arthroscopic Latarjet. J Shoulder Elbow Surg. 2016;25(1):78-89. [46] 许鉴,陆伟.肩关节复发前脱位伴有关节盂骨质缺损的治疗选择[J].中华肩肘外科电子杂志,2019,7(1):5-11. [47] CUNNINGHAM G, BENCHOUK S, KHERAD O, et al. Comparison of arthroscopic and open Latarjet with a learning curve analysis. Knee Surg Sports Traumatol Arthrosc. 2016; 24(2):540-545. [48] HORNER NS, MOROZ PA, BHULLAR R, et al. Open versus arthroscopic Latarjet procedures for the treatment of shoulder instability: a systematic review of comparative studies. BMC Musculoskelet Disord. 2018;19(1):255. [49] HURLEY ET, LIM FAT D, FARRINGTON SK, et al. Open versus arthroscopic latarjet procedure for anterior shoulder instability: a systematic review and meta-analysis. Am J Sports Med. 2019;47(5):1248-1253. [50] WONG SE, FRIEDMAN LGM, GARRIGUES GE. Arthroscopic latarjet: indications, techniques, and results. Arthroscopy. 2020;36(8):2044-2046. [51] TAUBER M, RESCH H, FORSTNER R, et al. Reasons for failure after surgical repair of anterior shoulder instability. J Shoulder Elbow Surg. 2004;13(3):279-285. [52] WARNER JJ, JOHNSON D, MILLER M, et al. Technique for selecting capsular tightness in repair of anterior-inferior shoulder instability. J Shoulder Elbow Surg. 1995;4(5):352-364. [53] RHEE YG, HA JH, CHO NS. Anterior shoulder stabilization in collision athletes: arthroscopic versus open Bankart repair. Am J Sports Med. 2006;34(6):979-985. [54] TAVERNA E, GARAVAGLIA G, PERFETTI C, et al. An arthroscopic bone block procedure is effective in restoring stability, allowing return to sports in cases of glenohumeral instability with glenoid bone deficiency. Knee Surg Sports Traumatol Arthrosc. 2018;26(12):3780-3787. [55] IALENTI MN, MULVIHILL JD, FEINSTEIN M, et al. Return to play following shoulder stabilization: a systematic review and meta-analysis. Orthop J Sports Med. 2017. doi: 10.1177/2325967117726055. |
| [1] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [2] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [3] | Li Dadi, Zhu Liang, Zheng Li, Zhao Fengchao. Correlation of total knee arthroplasty efficacy with satisfaction and personality characteristics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1346-1350. |
| [4] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [5] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [6] | Peng Zhihao, Feng Zongquan, Zou Yonggen, Niu Guoqing, Wu Feng. Relationship of lower limb force line and the progression of lateral compartment arthritis after unicompartmental knee arthroplasty with mobile bearing [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1368-1374. |
| [7] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [8] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [9] | Zhang Shangpu, Ju Xiaodong, Song Hengyi, Dong Zhi, Wang Chen, Sun Guodong. Arthroscopic suture bridge technique with suture anchor in the treatment of acromioclavicular dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1417-1422. |
| [10] | Yuan Jiawei, Zhang Haitao, Jie Ke, Cao Houran, Zeng Yirong. Underlying targets and mechanism of Taohong Siwu Decoction in prosthetic joint infection on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1428-1433. |
| [11] | Wang Debin, Bi Zhenggang. Related problems in anatomy mechanics, injury characteristics, fixed repair and three-dimensional technology application for olecranon fracture-dislocations [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1446-1451. |
| [12] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [13] | Chen Jinping, Li Kui, Chen Qian, Guo Haoran, Zhang Yingbo, Wei Peng. Meta-analysis of the efficacy and safety of tranexamic acid in open spinal surgery [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1458-1464. |
| [14] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [15] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||