Chinese Journal of Tissue Engineering Research ›› 2017, Vol. 21 ›› Issue (9): 1334-1339.doi: 10.3969/j.issn.2095-4344.2017.09.005
Previous Articles Next Articles
Ectopic osteogenesis of bone marrow stromal stem cells under bone morphogenetic protein 2/vascular endothelial growth factor 165 co-transfections
Zhou Hang-yu, Xia De-lin, Gan Sheng-yuan, Shao Xue-lei
- Department of Oral and Maxllofacial Surgery, Hospital of Stomatology, Southwest Medical University, Luzhou 646000, Sichuan Province, China
-
Online:2017-03-28Published:2017-03-31 -
Contact:Xia De-lin, M.D., Professor, Department of Oral and Maxllofacial Surgery, Hospital of Stomatology, Southwest Medical University, Luzhou 646000, Sichuan Province, China -
About author:Zhou Hang-yu, Master, Physician, Department of Oral and Maxllofacial Surgery, Hospital of Stomatology, Southwest Medical University, Luzhou 646000, Sichuan Province, China -
Supported by:the Applied Basic Research Fund of Sichuan Provincial Science and Technology Department, No. 2008jy0014
CLC Number:
Cite this article
Zhou Hang-yu, Xia De-lin, Gan Sheng-yuan, Shao Xue-lei. Ectopic osteogenesis of bone marrow stromal stem cells under bone morphogenetic protein 2/vascular endothelial growth factor 165 co-transfections[J]. Chinese Journal of Tissue Engineering Research, 2017, 21(9): 1334-1339.
share this article
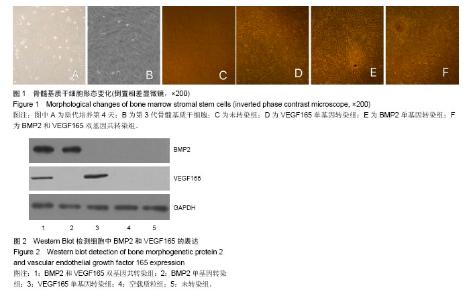
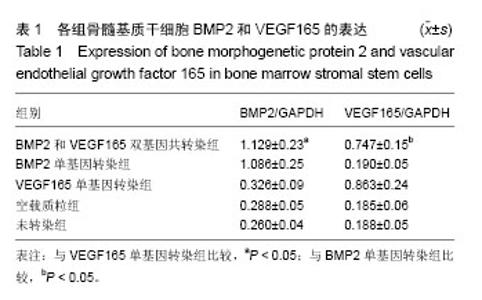
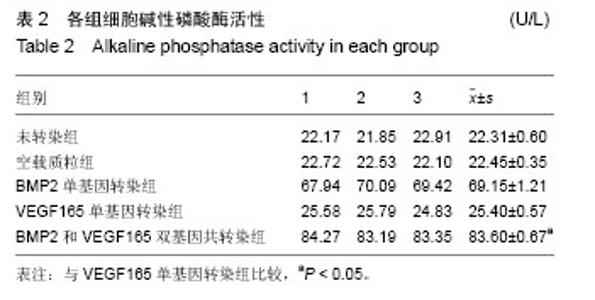
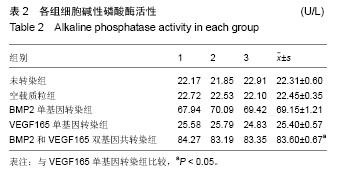
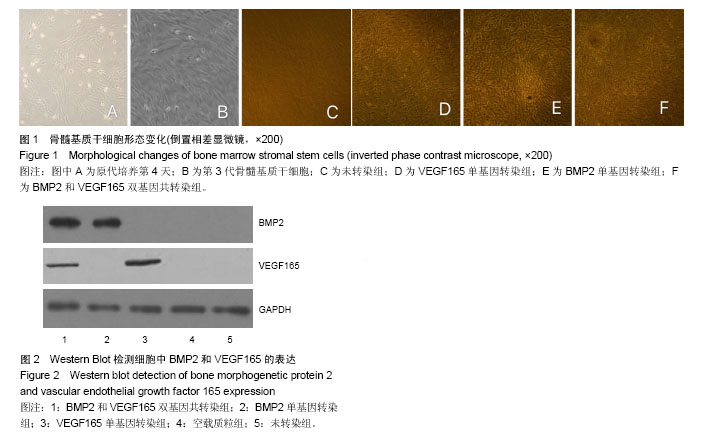
2.1 骨髓基质干细胞形态 原代培养第4天就可以观察到细胞附壁,呈梭形,数量较多,局部呈多个散在分布的细胞集落(图1A)。第4-6天开始形成典型的均匀分布的簇状增殖灶,细胞数量增多,细胞呈长梭形,细胞紧密排列。第6天后细胞数量迅速扩增,细胞簇状增生灶数量增加,范围扩大。第7-9天细胞生长即可以达80%-90%融合,呈长梭形,紧密排列类似漩涡状。 传代细胞接种4 h后开始附壁铺伸,12 h活细胞基本完成贴壁,第3天迅速增殖,第7天即可达到80%-90%融合,呈现比原代更均匀的长梭形(图1B)。经成骨诱导7 d后,细胞逐渐汇合,呈现铺路石状。随着诱导时间的延长,局部细胞呈重叠生长,间充质逐渐堆积,间充质中矿盐沉积,形成多个结节,并逐渐融合。培养14 d后,可见褐色点状矿化结节中心。 组间差异:未转染组、空载质粒组、VEGF165单基因转染组,在培养期间一直观察不到成骨细胞特征(图1C,D)。BMP2单基因转染组、BMP2和VEGF165双基因共转染组,均能观察到骨髓基质干细胞向成骨细胞分化,且BMP2和VEGF165双基因共同转染组(图1F)的骨髓基质干细胞分化速度和强度均大于BMP2单基因转染组(图1E)。 2.2 Western Blot检测细胞中BMP2和VEGF165的表达 在BMP2和VEGF165双基因共转染组和BMP2单基因转染组中有大量的BMP2分泌位于上清中,见图2。在未转染组、VEGF165单基因转染组和空载质粒组中则只有很少。在BMP2和VEGF165双基因共转染组和VEGF165单基因转染组中有大量的VEGF165分泌于上清中,在未转染组、BMP2单基因转染组和空载质粒组中VEGF165分泌量很少。统计结果显示双基因共转染组和单基因转染组差异有显著性意义(P < 0.05),见表1。"
| [1] Langer R, Vacanti J. Advances in tissue engineering. J Pediatr Surg. 2016;51(1):8-12.[2] Kumar V, Khare T, Sharma M, et al. Engineering Crops for Future: A Phosphoproteomics Approach. Curr Protein Pept Sci. 2017 Feb 9. [Epub ahead of print] [3] Ansari T, Lange P, Southgate A, et al. Stem Cell-Based Tissue-Engineered Laryngeal Replacement. Stem Cells Transl Med. 2017;6(2):677-687. [4] Sánchez P, Pedraz JL, Orive G. Biologically active and biomimetic dual gelatin scaffolds for tissue engineering. Int J Biol Macromol. 2017;98:486-494. [5] Paschos NK, Brown WE, Eswaramoorthy R, et al. Advances in tissue engineering through stem cell-based co-culture. J Tissue Eng Regen Med. 2015;9(5):488-503.[6] Ehnert S, Aspera-Werz RH, Freude T, et al. Distinct Gene Expression Patterns Defining Human Osteoblasts' Response to BMP2 Treatment: Is the Therapeutic Success All a Matter of Timing. Eur Surg Res. 2016;57(3-4): 197-210.[7] McBride-Gagyi SH, McKenzie JA, Buettmann EG, et al. Bmp2 conditional knockout in osteoblasts and endothelial cells does not impair bone formation after injury or mechanical loading in adult mice. Bone. 2015;81:533-543. [8] Rogers MB, Shah TA, Shaikh NN. Turning Bone Morphogenetic Protein 2 (BMP2) on and off in Mesenchymal Cells. J Cell Biochem. 2015;116(10):2127-2138. [9] Jang CH, Choi CH, Cho YB. Effect of BMP2-Platelet-rich Plasma-Biphasic Calcium Phosphate Scaffold on Accelerated Osteogenesis in Mastoid Obliteration. In Vivo. 2016;30(6): 835-839.[10] Kawakami Y, Takayama K, Matsumoto T, et al. Anterior Cruciate Ligament-Derived Stem Cells Transduced With BMP2 Accelerate Graft-Bone Integration After ACL Reconstruction. Am J Sports Med. 2016 Nov 30. [Epub ahead of print] [11] Liu K, Jing Y, Zhang W, et al. Silencing miR-106b accelerates osteogenesis of mesenchymal stem cells and rescues against glucocorticoid-induced osteoporosis by targeting BMP2. Bone. 2017;97:130-138.[12] Schliephake H, Rublack J, Förster A, et al. Functionalization of titanium implants using a modular system for binding and release of VEGF enhances bone-implant contact in a rodent model. J Clin Periodontol. 2015;42(3):302-310.[13] Liu HJ, Hu RY, Dai WJ, et al. Culture and Identification of Bone Marrow Mesenchymal Stem Cells from Enhanced Green Fluorescent Protein-transgenic Rats. Zhongguo Yi Xue Ke Xue Yuan Xue Bao.2016;38(1):9-15.[14] Nagasawa M, Cooper LF, Ogino Y, et al. Topography Influences Adherent Cell Regulation of Osteoclastogenesis. J Dent Res. 2016;95(3):319-326. [15] Liu HJ, Hu RY, Dai WJ, et al. Culture and Identification of Bone Marrow Mesenchymal Stem Cells from Enhanced Green Fluorescent Protein-transgenic Rats. Zhongguo Yi Xue Ke Xue Yuan Xue Bao. 2016;38(1):9-15. [16] Xiang J, Zheng X, Zhu X, et al. Optimization of the protocols for in vitro culture and induction of hepatic differentiation of rat mesenchymal stem cells. Nan Fang Yi Ke Da Xue Xue Bao. 2015;35(8):1090-1096. [17] Zhang W, Zhang F, Shi H, et al. Comparisons of rabbit bone marrow mesenchymal stem cell isolation and culture methods in vitro. PLoS One. 2014;9(2):e88794.[18] 杨俊丽,韩霞,孙明启,等.兔骨髓间充质干细胞的生物学特征及原代培养[J].中国组织工程研究,2015,19(50):8043-8047.[19] 刘伟,陈剑,宋佳,等.兔骨髓间充质干细胞的分离、培养及鉴定[J].中国实验诊断学,2013,17(8):1366-1369.[20] Hopkins CR. Inhibitors of the bone morphogenetic protein (BMP) signaling pathway: a patent review (2008-2015). Expert Opin Ther Pat. 2016 Aug 4. [Epub ahead of print] [21] Abdallah BM. Marrow adipocytes inhibit the differentiation of mesenchymal stem cells into osteoblasts via suppressing BMP-signaling. J Biomed Sci. 2017;24(1):11.[22] Chen Z, Ni S, Han S, et al. Nanoporous microstructures mediate osteogenesis by modulating the osteo-immune response of macrophages. Nanoscale. 2017;9(2):706-718. [23] Salazar VS, Gamer LW, Rosen V. BMP signalling in skeletal development, disease and repair. Nat Rev Endocrinol. 2016; 12(4):203-221. [24] Itoi T, Harada Y, Irie H, et al. Escherichia coli-derived recombinant human bone morphogenetic protein-2 combined with bone marrow-derived mesenchymal stromal cells improves bone regeneration in canine segmental ulnar defects. BMC Vet Res. 2016;12:201. [25] Sharma S, Sapkota D, Xue Y, et al. Adenoviral Mediated Expression of BMP2 by Bone Marrow Stromal Cells Cultured in 3D Copolymer Scaffolds Enhances Bone Formation. PLoS One. 2016;11(1):e0147507. [26] Hu T, Abbah SA, Toh SY, et al. Bone marrow-derived mesenchymal stem cells assembled with low-dose BMP-2 in a three-dimensional hybrid construct enhances posterolateral spinal fusion in syngeneic rats. Spine J. 2015;15(12):2552- 2563.[27] Jin IG, Kim JH, Wu HG, et al. Effect of bone marrow-derived stem cells and bone morphogenetic protein-2 on treatment of osteoradionecrosis in a rat model. J Craniomaxillofac Surg. 2015;43(8):1478-1486.[28] Yin C, Chen J, Chen Z, et al. hBMP-2 and hTGF-β1 expressed in implanted BMSCs synergistically promote the repairing of segmental bone defects. J Orthop Sci. 2015; 20(4):717-727. [29] Wang X, Li Y, Han R, et al. Demineralized bone matrix combined bone marrow mesenchymal stem cells, bone morphogenetic protein-2 and transforming growth factor-β3 gene promoted pig cartilage defect repair. PLoS One. 2014; 9(12):e116061.[30] Wang T, Liao TA, Zhong SB. Transfection of bone marrow mesenchymal stem cells using green fluorescence protein labeled hVEGF165 recombinant plasmid mediated by liposome. Asian Pac J Trop Med. 2013;6(9):739-742. [31] Liang W, Cai Q, Liu Y. Transfection of human vascular endothelial growth factor 165 gene into rat bone marrow mesenchymal stem cells in vitro. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2011;25(11):1383-1388. [32] Hang D, Wang Q, Guo C, et al. Treatment of osteonecrosis of the femoral head with VEGF165 transgenic bone marrow mesenchymal stem cells in mongrel dogs. Cells Tissues Organs. 2012;195(6):495-506.[33] Zhang C, Ma Q, Qiang H, et al. Study on effect of recombinant adeno-associated virus vector co-expressing human vascular endothelial growth factor 165 and human bone morphogenetic protein 7 genes on bone regeneration and angiopoiesis in vivo. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2010 ;24(12):1449-1454. [34] Zhang M, Wang D, Yin R. Histocompatibility of nano-hydroxyapatite/poly-co-glycolic acid tissue engineering bone modified by mesenchymal stem cells with vascular endothelial frowth factor. Zhonghua Yi Xue Za Zhi. 2015; 95(37):3061-3065. [35] Liu S, Jin D, Wu JQ, et al. Neuropeptide Y stimulates osteoblastic differentiation and VEGF expression of bone marrow mesenchymal stem cells related to canonical Wnt signaling activating in vitro. Neuropeptides. 2016;56:105-113.[36] Yadin D, Knaus P, Mueller TD. Structural insights into BMP receptors: Specificity, activation and inhibition. Cytokine Growth Factor Rev. 2016;27:13-34.[37] Yadlapati M, Biguetti C, Cavalla F, et al. Characterization of a Vascular Endothelial Growth Factor-loaded Bioresorbable Delivery System for Pulp Regeneration. J Endod. 2017;43(1): 77-83.[38] Payne SL, Peacock HM, Vickaryous MK. Blood vessel formation during tail regeneration in the leopard gecko (Eublepharis macularius): The blastema is not avascular. J Morphol. 2017;278(3):380-389.[39] Liu Y, Olsen BR. Distinct VEGF functions during bone development and homeostasis. Arch Immunol Ther Exp (Warsz). 2014;62(5):363-368.[40] Whitehouse MR, Howells NR, Parry MC, et al. Repair of Torn Avascular Meniscal Cartilage Using Undifferentiated Autologous Mesenchymal Stem Cells: From In Vitro Optimization to a First-in-Human Study. Stem Cells Transl Med. 2016 Dec 15. [Epub ahead of print].[41] Chen K, Zhang C, Wang L, et al. Progress on strategies to promote vascularization in bone tissue engineering. Zhongguo Gu Shang. 2015;28(4):383-388.[42] Li JJ, Zhao Q, Wang H, et al. Reconstruction of segmental bone defect by gene modified tissue engineering bone combined with vascularized periosteum. Zhonghua Zheng Xing Wai Ke Za Zhi. 2007;23(6):502-506.[43] Han TY, Liu XW, Liang N, et al. In vitro effects of recombinant adenovirus-mediated bone morphogenetic protein 2/vascular endothelial growth factor 165 on osteogenic differentiation of bone marrow mesenchymal stem cells. Artif Cells Nanomed Biotechnol. 2017;45(1):108-114.[44] Zhang C, Liu HM, Li QW, et al. Construction of recombinant adenovirus vector containing hBMP2 and hVEGF165 genes and its expression in rabbit Bone marrow mesenchymal stem cells. Tissue Cell. 2014;46(5):311-317.[45] Lin Z, Wang JS, Lin L, et al. Effects of BMP2 and VEGF165 on the osteogenic differentiation of rat bone marrow-derived mesenchymal stem cells. Exp Ther Med. 2014;7(3):625-629.[46] 管大凡,陈月芹,刘洪美,等. hBMP2/hVEGF165双基因腺病毒修饰BMSCs复合n-HA/PA66修复骨缺损影像学观察[J].中国矫形外科杂志,2015,23(20):1881-1887.[47] 张聪,刘洪美,李庆伟,等.腺病毒载体介导人BMP-2与VEGF-165对骨髓间充质干细胞形态特征及增殖能力影响的实验研究[J].中国实验诊断学,2015,19(11):1813-1817.[48] Silva E, Vasconcellos LM, Rodrigues BV, et al. PDLLA honeycomb-like scaffolds with a high loading of superhydrophilic graphene/multi-walled carbon nanotubes promote osteoblast in vitro functions and guided in vivo bone regeneration.Mater Sci Eng C Mater Biol Appl. 2017;73: 31-39.[49] Liu DD, Zhang JC, Zhang Q, et al. TGF-β/BMP signaling pathway is involved in cerium-promoted osteogenic differentiation of mesenchymal stem cells. J Cell Biochem. 2013;114(5):1105-1114.[50] 曹建华.年龄和性别与血清肝功能相关酶的关系探讨[J].检验医学与临床,2010,7(4):325-327.[51] Hou L, Liu Y, Gao Q, et al. Spiroplasma eriocheiris Adhesin-Like Protein (ALP) Interacts with Epidermal Growth Factor (EGF) Domain Proteins to Facilitate Infection. Front Cell Infect Microbiol. 2017;7:13. [52] 罗小娟.健康未成年人群干化学法血清酶水平分析[J].循证医学, 2015,15(4):232-236. |
| [1] | Yao Xiaoling, Peng Jiancheng, Xu Yuerong, Yang Zhidong, Zhang Shuncong. Variable-angle zero-notch anterior interbody fusion system in the treatment of cervical spondylotic myelopathy: 30-month follow-up [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1377-1382. |
| [2] | Wang Jing, Xiong Shan, Cao Jin, Feng Linwei, Wang Xin. Role and mechanism of interleukin-3 in bone metabolism [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1260-1265. |
| [3] | Xiao Hao, Liu Jing, Zhou Jun. Research progress of pulsed electromagnetic field in the treatment of postmenopausal osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1266-1271. |
| [4] | Hui Xiaoshan, Bai Jing, Zhou Siyuan, Wang Jie, Zhang Jinsheng, He Qingyong, Meng Peipei. Theoretical mechanism of traditional Chinese medicine theory on stem cell induced differentiation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1125-1129. |
| [5] | An Weizheng, He Xiao, Ren Shuai, Liu Jianyu. Potential of muscle-derived stem cells in peripheral nerve regeneration [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1130-1136. |
| [6] | Fan Yiming, Liu Fangyu, Zhang Hongyu, Li Shuai, Wang Yansong. Serial questions about endogenous neural stem cell response in the ependymal zone after spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1137-1142. |
| [7] | Wen Dandan, Li Qiang, Shen Caiqi, Ji Zhe, Jin Peisheng. Nocardia rubra cell wall skeleton for extemal use improves the viability of adipogenic mesenchymal stem cells and promotes diabetes wound repair [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1038-1044. |
| [8] | Zhu Bingbing, Deng Jianghua, Chen Jingjing, Mu Xiaoling. Interleukin-8 receptor enhances the migration and adhesion of umbilical cord mesenchymal stem cells to injured endothelium [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1045-1050. |
| [9] | Luo Xiaoling, Zhang Li, Yang Maohua, Xu Jie, Xu Xiaomei. Effect of naringenin on osteogenic differentiation of human periodontal ligament stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1051-1056. |
| [10] | Cui Xing, Sun Xiaoqi, Zheng Wei, Ma Dexin. Huangqin Decoction regulates autophagy to intervene with intestinal acute graft-versus-host disease in mice [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1057-1062. |
| [11] | Wang Xinmin, Liu Fei, Xu Jie, Bai Yuxi, Lü Jian. Core decompression combined with dental pulp stem cells in the treatment of steroid-associated femoral head necrosis in rabbits [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1074-1079. |
| [12] | Fang Xiaolei, Leng Jun, Zhang Chen, Liu Huimin, Guo Wen. Systematic evaluation of different therapeutic effects of mesenchymal stem cell transplantation in the treatment of ischemic stroke [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1085-1092. |
| [13] | Guo Jia, Ding Qionghua, Liu Ze, Lü Siyi, Zhou Quancheng, Gao Yuhua, Bai Chunyu. Biological characteristics and immunoregulation of exosomes derived from mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1093-1101. |
| [14] | Zhang Jinglin, Leng Min, Zhu Boheng, Wang Hong. Mechanism and application of stem cell-derived exosomes in promoting diabetic wound healing [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1113-1118. |
| [15] | Huang Chenwei, Fei Yankang, Zhu Mengmei, Li Penghao, Yu Bing. Important role of glutathione in stemness and regulation of stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1119-1124. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||