Chinese Journal of Tissue Engineering Research ›› 2026, Vol. 30 ›› Issue (21): 5605-5613.doi: 10.12307/2026.769
Previous Articles Next Articles
Dynamic evolution of evaluation standards for effectiveness and safety after anterior cruciate ligament reconstruction in the knee
Li Chengke1, Gao Miaomiao1, Lei Lei1, Ma Rongxing2, Zhang Jingyu1, Hu Yongcheng1
- 1Tianjin Hospital of Tianjin University, Tianjin 300211, China; 2Tianjin Medical University, Tianjin 300211, China
-
Online:2026-07-28Published:2026-03-06 -
Contact:Hu Yongcheng, MD, Chief physician, Tianjin Hospital of Tianjin University, Tianjin 300211, China -
About author:Li Chengke, MS candidate, Tianjin Hospital of Tianjin University, Tianjin 300211, China -
Supported by:Beijing-Tianjin-Hebei Basic Research Cooperation Special Fund, No. 22JCZXJC00130 (to ZJY); Science and Technology Project of Tianjin Metrology Bureau, No. 2024TJMT039 (to ZJY); Tianjin Hospital Science and Technology Fund, No. TJYY2401 (to ZJY); Science and Technology Project of Tianjin Health Commission, No. TJWJ2024MS027 (to ZJY)
CLC Number:
Cite this article
Li Chengke, Gao Miaomiao, Lei Lei, Ma Rongxing, Zhang Jingyu, Hu Yongcheng. Dynamic evolution of evaluation standards for effectiveness and safety after anterior cruciate ligament reconstruction in the knee[J]. Chinese Journal of Tissue Engineering Research, 2026, 30(21): 5605-5613.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
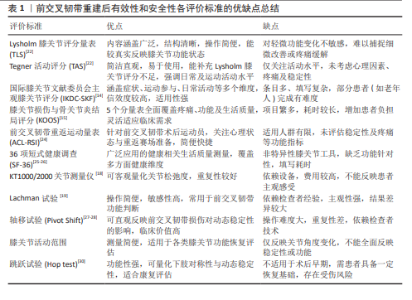
2.1 文献检索结果与评价标准纳入 最终纳入文献136篇,根据记录在Excel表格中的数据,分别确定自1990年1月至2023年8月主观及客观评价标准使用次数排名前6位的评价标准: 主观评分:Lysholm膝关节评分量表(The Lysholm Knee Scoring Scale,TLS)为71/136(在所纳入的136篇文献中有71篇文献采用了Lysholm膝关节评分量表);Tegner活动评分(Tegner Activity Scale,TAS)为65/136;国际膝关节文献委员会主观膝关节评分为38/136;膝关节损伤和骨关节炎结局评分(Knee Injury and Osteoarthritis Outcome Score,KOOS)为32/136;前交叉韧带受伤后恢复运动量表(ACL Return to Sport after Injury scale,ACL-RSI)为25/136;36项短式健康调查量表(The MOS 36-item short-form health survey,SF-36)为18/136。 客观评价标准:KT 1000/2000关节测量仪为60/136;Lachman试验(Lachman test)为53/136;轴移试验(Pivot Shift test)为47/136;国际膝关节文献委员会客观膝关节评分为40/136;膝关节活动范围为37/136;跳跃试验(Hop test)为34/136。 由于其他评价标准的使用频率较低且随年份变化趋势不明显,因此未对它们进行动态性分析。 2.2 纳入评价标准介绍 Lysholm膝关节评分量表:于1982年首次发布[21],并在1985年进行了修订[22],主要用于评估膝关节韧带手术后的效果,尤其是与膝关节不稳定相关的症状。修订后的Lysholm膝关节评分量表包含8个项目,分别是:①跛行(5分);②支撑(5分);③锁定(15分);④不稳定(25分);⑤疼痛(25分);⑥肿胀(10分);⑦爬楼梯(10分);⑧下蹲(5分),总分为100分。各项得分累计后得到总分,得分范围在0-100分之间,其中100分代表完全无症状或功能障碍。评分标准分为优秀(95-100分)、良好(84-94分)、一般(65-83分)和差(≤64分)13。该量表内容涵盖广泛,结构清晰,使用简单,可以较为真实地反映患者膝关节的功能状态。但它对细微或不明显的膝关节功能变化敏感度不高,可能无法充分反映膝关节功能的轻微改善或疼痛缓解。 Tegner活动评分:于1985年发布。考虑到Lysholm膝关节评分量表可能会因活动水平下降而不能准确反映患者实际情况,因此开发了该量表以补充Lysholm膝关节评分。Tegner活动评分是基于患者日常生活、娱乐活动和竞技体育参与的分级系统,共分为0-10的11个等级,患者需选择最能描述其当前活动水平的等级。在该评分中,活动水平6-10级只有在参与娱乐或竞技体育活动时才适用[22]。该量表简洁、直观并且易于患者使用,但其主要集中于评估患者活动水平,未充分考虑患者的恐惧感、受伤后的自信心等心理因素,也未涵盖膝关节的疼痛、稳定性等功能性评估。 国际膝关节文献委员会主观膝关节评分:国际膝关节文献委员会于1987年成立,并在1993年出版了国际膝关节文献委员会客观膝关节评价表[23],随后于1994年进行了修订,最终在2001年推出了国际膝关节文献委员会主观膝关节评分,适用于各种膝关节问题的功能评估。国际膝关节文献委员会主观膝关节评分量表一共包含18个项目,涵盖3个领域:症状(7项)、运动参与(1项)和日常活动能力(9项),以及当前膝关节功能(1项)。评分方式因项目而异,包括是/否(第6项)、5分Likert量表(第1,4,5,7,8和9项)及11分数字评分量表(第2,3和10项)等。最后将各项得分(不含10a项)累加后,通过公式:(总分/87)×100计算得出总评分,满分为100分,表示完全无活动或症状限制[14]。国际膝关节文献委员会主观膝关节评分在评估前交叉韧带重建术后膝关节功能方面表现出良好的有效性和安全性,但由于其项目较多、填写过程较复杂,老年人或教育程度较低的患者理解和完成该量表可能需要更多时间与指导。 膝关节损伤和骨关节炎结局评分:该量表于1998年出版,适用于评估因创伤引发的骨关节炎以及可能导致此类疾病的膝关节损伤(如前交叉韧带损伤、踝关节损伤和软骨损伤)所带来的膝关节功能问题。膝关节损伤和骨关节炎结局评分量表包含5个单独评分的分量表:①疼痛;②其他症状;③日常生活功能;④运动和娱乐功能(Sport/Rec);⑤膝关节相关的生活质量,总计42个项目,每个项目均采用Likert量表进行评分。所有项目的得分按分量表维度进行累加,再换算成0-100的等级评分,其中0分代表严重的膝关节问题,100分则表示完全没有问题。该量表不设定总分数,分别分析每一维度对临床判断更有参考价值[15]。膝关节损伤和骨关节炎结局评分量表能较为全面地评估患者膝关节功能,且可根据不同临床需求灵活调整,便于针对不同患者关注的功能方面进行评估,但其涵盖内容较多,评估过程可能会花费患者较长时间。 前交叉韧带受伤后恢复运动量表:发布于2008年,一共包括12个问题,从风险评估、情绪反应以及信心3个方面评估患者的心理状态。评分方式可采用0-100的视觉模拟量表或0-10的数字评分量表,最终得分为各题项得分的平均值,得分越高,说明患者心理准备越充分[24]。该量表专为前交叉韧带重建术后的运动员设计,主要用于评估其心理状态及是否具备重返赛场的心理条件,量表简便、适用于快速筛查,但对于非运动员或以日常活动为主的人群适用性较弱。另外该量表未纳入膝关节稳定性、疼痛等实际功能评估,其结果并不能全面反映膝关节的整体功能恢复情况。 36项短式健康调查(SF-36量表):该量表发布于1992年,涵盖了8个健康相关领域:生理机能、生理职能、躯体疼痛、一般健康状况、活力、社会功能、情感职能和精神健康,一共包括36个条目。每个领域的得分反映了患者在该方面的健康状况,得分越高,表示其健康状况越好[25-26]。SF-36量表在整体健康评估中虽然被广泛应用,但它在针对膝关节功能的精确测量上略显不足,而且其项目较多,填写过程相对耗时,可能会增加患者的负担。 KT 1000/2000关节测量仪:是一种用于评估膝关节前后稳定性的仪器,通过测量胫骨相对于股骨的位移距离,来客观量化膝关节的松弛程度,常用于前交叉韧带损伤后的评估[18]。 Lachman试验:是一种临床常用的评估前交叉韧带功能的测试,医生在患者肌肉放松的情况下施力,以检测胫骨向前的过度活动,从而判断前交叉韧带的完整性,阳性结果提示前交叉韧带损伤[19]。 轴移试验:是一种临床常用的判断前交叉韧带断裂的测试。医生在检查过程中将患者的膝关节从伸直到逐渐屈曲的过程中,施加轴向负荷和外翻力。当测试呈阳性时,常提示前交叉韧带受损[27-28]。 膝关节活动范围:膝关节活动度是指膝关节运动时所通过的运动弧,常以度数表示。适用于所有膝关节功能评估,尤其是术后膝关节功能恢复情况的评估。 跳跃试验:用于测量腿部的爆发力和力量,既具有功能性又具有定量性,适用于前交叉韧带重建、踝关节扭伤和应力性骨折等受伤后患者的膝关节稳定性评估。NOYES等[29]最初描述的4种不同跳跃测试的组合可能特别适合作为前交叉韧带重建术后正在接受康复治疗患者膝关节功能的结局指标,包括单跳测试、三跳测试、交叉跳测试、6 m定时跳测试[30]。在2个肢体上获得测量数据,结果以手术肢体的测量数据表示为对侧肢体测量数据的百分比,称为肢体对称指数。基于这4项跳跃测试的表现,肢体对称指数被用于量化膝关节动态稳定性[29,31-32]。 各评价标准的优缺点总结见表1。"
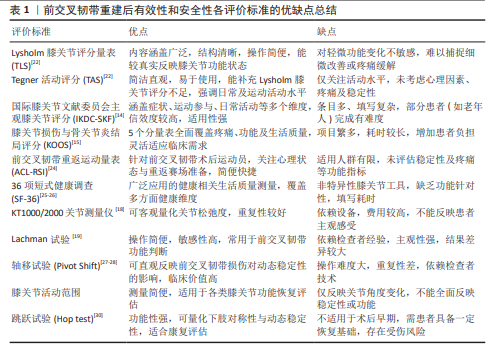
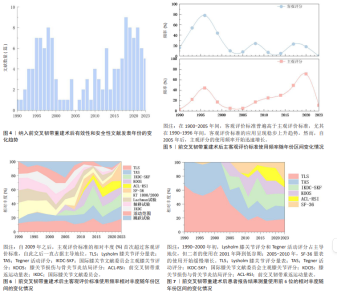
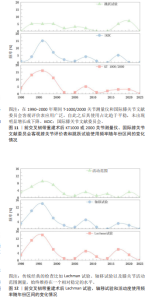
2.3 主客观评价标准应用趋势的动态演变 通过对纳入文献的逐年分析,发现前交叉韧带重建术后有效性和安全性评估量表的使用经历了时代的巨大变迁。图4展示了从1990-2023年间文献数量的变化趋势,整体呈现相对增长趋势。 如图5所示,在1900-2005年间,客观评价标准普遍高于主观评价标准,尤其在1990-1996年间,客观评价标准的应用呈现稳步上升趋势。然而,自2005年后,主观评分的使用频率开始迅速增长。虽然2002-2008年期间,主、客观评价标准的使用频率逐渐缩小,但自2009年之后,主观评价标准的相对丰度(%)首次超过客观评价标准,自此之后一直占据主导地位,见图6。为了验证这一趋势的统计学显著性,作者将数据每5年分为1组,并采用Cochran-Armitage趋势检验进行统计。结果显示,随时间推移使用主观评价表的比例呈现显著上升趋势(Z=6.32,P < 0.000 01),具有统计学意义,强有力地证实了从客观主导到主观主导的演变并非随机现象。"
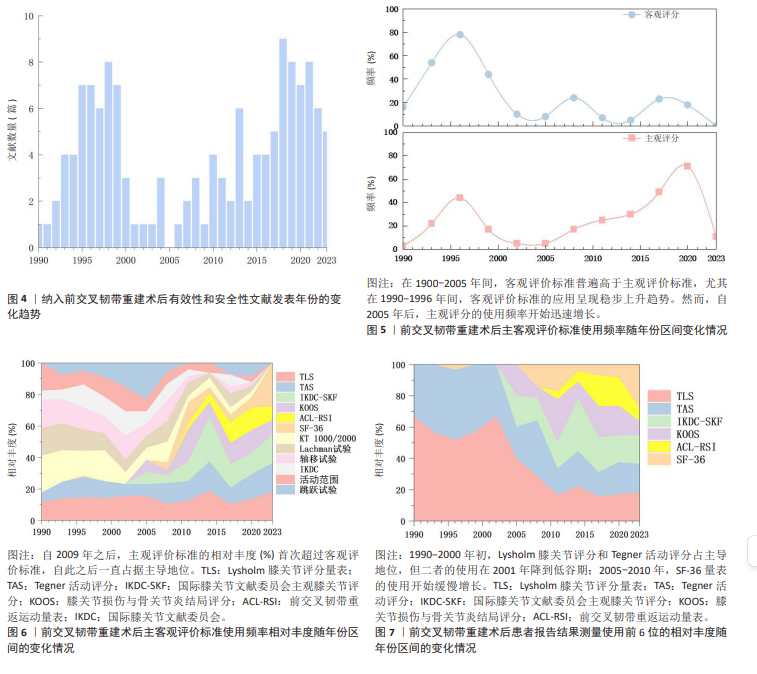

2.4 主观评价标准使用的动态演变 如图7所示,不同的主观评价标准的使用也发生了翻天覆地的变化,在早期阶段(1990-2000年初),Lysholm膝关节评分和Tegner活动评分占主导地位,但二者的使用在2001年降到低谷期;其次,在过渡时期(2005-2010年),由于患者开始对术后生活质量的关注,导致SF-36量表的使用开始缓慢增长。 人民生活水平进一步发展后(2010年后),评价格局又一次发生巨大的变化。如图8所示,Lysholm膝关节评分和Tegner活动评分的使用占比略有所回缓。除此之外,图9显示出国际膝关节文献委员会主观膝关节评分和膝关节损伤和骨关节炎结局评分的使用频率呈现出迅猛式增长,迅速成为新的主流。在此之间,前交叉韧带受伤后恢复运动量表自2008年首次出现后,其应用也逐步上升,真切反映出临床患者迫切重返运动的心理状态。综上所述,主观评估的重心从单一的膝关节功能评分导向到了更个性化、更全面的膝关节功能与心理状态评估。"
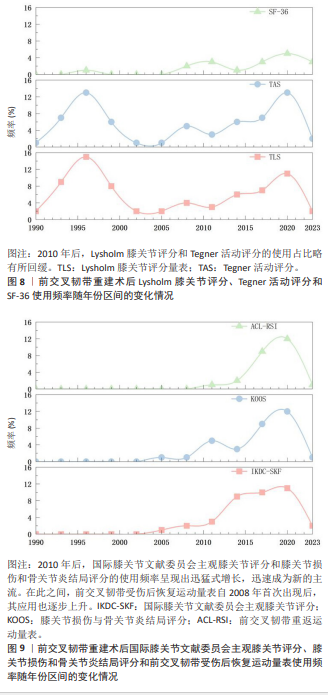
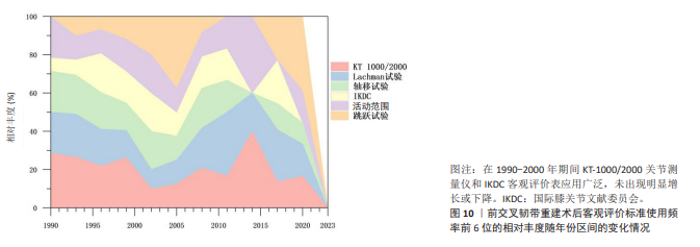
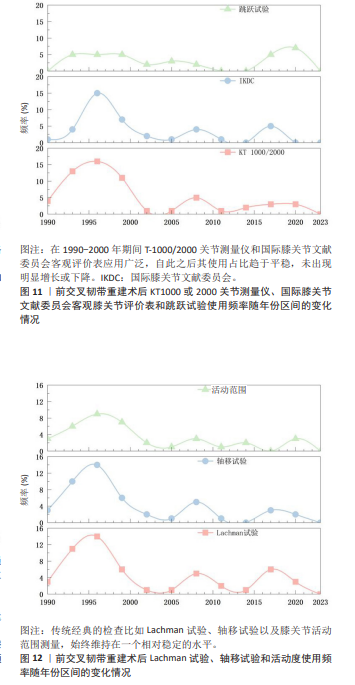
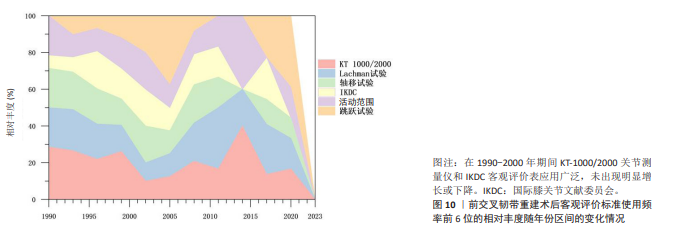
2.5 客观评价使用工具的动态演变 相比于主观评价标准的剧烈演变,客观评价标准的使用趋势显示出高度的稳定性和延续性。如图10,11所示,在1990-2000年期间KT-1000/2000关节测量仪和国际膝关节文献委员会客观评价表应用广泛,自此之后其使用占比趋于平稳,未出现明显增长或下降。除此之外,传统经典的检查比如Lachman试验、轴移试验以及膝关节活动范围测量,因其操作的简便性和临床的不可替代性,始终维持在一个相对稳定的水平,成为客观评估的“基石”,见图12。同时跳跃试验作为功能性测试的代表,其应用同样保持稳定,这体现了临床医生和患者对回归运动动态功能评估持续的最终的需求。综上所述,客观评价从未被主观评估所淘汰,而是从其早期的主导地位转变为与主观评估相辅相成的稳定角色。"
| [1] BOGUNOVIC L, MATAVA MJ. Operative and nonoperative treatment options for ACL tears in the adult patient: a conceptual review. Phys Sportsmed. 2013;41(4):33-40. [2] DODSON CC, SECRIST ES, BHAT SB, et al. Anterior Cruciate Ligament Injuries in National Football League Athletes From 2010 to 2013: A Descriptive Epidemiology Study. Orthop J Sports Med. 2016;4(3):2325967116631949. [3] GRIFFIN LY, AGEL J, ALBOHM MJ, et al. Noncontact anterior cruciate ligament injuries: risk factors and prevention strategies. J Am Acad Orthop Surg. 2000; 8(3):141-150. [4] 吴登科, 田朝奇, 周志广, 等. 不同时机膝关节镜下前交叉韧带重建术的效果及对患者Lysholm评分、骨隧道宽度的影响[J]. 临床医学,2024,44(11): 39-41. [5] FILBAY SR, ACKERMAN IN, RUSSELL TG, et al. Health-related quality of life after anterior cruciate ligament reconstruction: a systematic review. Am J Sports Med. 2014;42(5):1247-1255. [6] MATHER RC 3RD, KOENIG L, KOCHER MS, et al. Societal and economic impact of anterior cruciate ligament tears. J Bone Joint Surg Am. 2013;95(19):1751-1759. [7] 卢海燕, 赵达锋, 陈剑, 等. 自制等长测试工具在关节镜下前交叉韧带重建术中应用的效果观察 [J]. 中国骨与关节损伤杂志,2025,40(2):145-150. [8] 匡萃琳, 黄文娟, 胡建华, 等. 三种手术时机下行关节镜下前交叉韧带重建术后膝关节功能和稳定性的对比研究[J]. 中国医学创新,2023,20(22):19-22. [9] MYKLEBUST G, BAHR R. Return to play guidelines after anterior cruciate ligament surgery. Br J Sports Med. 2005;39(3):127-131. [10] 张磊, 周鑫, 祁冀, 等. 取自体同侧1/2腓骨长肌肌腱重建膝关节前交叉韧带 [J]. 中国组织工程研究,2017,21(24):3815-3820. [11] LANGFORD JL, WEBSTER KE, FELLER JA. A prospective longitudinal study to assess psychological changes following anterior cruciate ligament reconstruction surgery. Br J Sports Med. 2009;43(5):377-381. [12] ARDERN CL, TAYLOR NF, FELLER JA, et al. Return-to-sport outcomes at 2 to 7 years after anterior cruciate ligament reconstruction surgery. Am J Sports Med. 2012;40(1):41-48. [13] JOHNSON DS, SMITH RB. Outcome measurement in the ACL deficient knee--what’s the score? Knee. 2001;8(1):51-57. [14] IRRGANG JJ, ANDERSON AF, BOLAND AL, et al. Development and validation of the international knee documentation committee subjective knee form. Am J Sports Med. 2001;29(5):600-613. [15] ROOS EM, ROOS HP, LOHMANDER LS, et al. Knee Injury and Osteoarthritis Outcome Score (KOOS)--development of a self-administered outcome measure. J Orthop Sports Phys Ther. 1998;28(2):88-96. [16] DAVIS JC, BRYAN S. Patient Reported Outcome Measures (PROMs) have arrived in sports and exercise medicine: Why do they matter? Br J Sports Med. 2015;49(24):1545-1546. [17] PEER MA, LANE J. The Knee Injury and Osteoarthritis Outcome Score (KOOS): a review of its psychometric properties in people undergoing total knee arthroplasty. J Orthop Sports Phys Ther. 2013;43(1):20-28. [18] 周敬滨, 王予彬, 李国平. KT2000/KT1000对膝稳定性定量分析的研究进展 [J]. 中国运动医学杂志,2003,22(3):307-309,313. [19] GURTLER RA, STINE R, TORG JS. Lachman test evaluated. Quantification of a clinical observation. Clin Orthop Relat Res. 1987; 216:141-150. [20] KOCHER MS, STEADMAN JR, BRIGGS K, et al. Determinants of patient satisfaction with outcome after anterior cruciate ligament reconstruction. J Bone Joint Surg Am. 2002; 84(9):1560-1572. [21] LYSHOLM J, GILLQUIST J. Evaluation of knee ligament surgery results with special emphasis on use of a scoring scale. Am J Sports Med. 1982;10(3):150-154. [22] TEGNER Y, LYSHOLM J. Rating systems in the evaluation of knee ligament injuries. Clin Orthop Relat Res. 1985;198:43-49. [23] HEFTI F, MÜLLER W, JAKOB RP, et al. Evaluation of knee ligament injuries with the IKDC form. Knee Surg Sports Traumatol Arthrosc. 1993;1(3-4):226-234. [24] WEBSTER KE, FELLER JA, LAMBROS C. Development and preliminary validation of a scale to measure the psychological impact of returning to sport following anterior cruciate ligament reconstruction surgery. Phys Ther Sport. 2008;9(1):9-15. [25] WARE JE JR. SF-36 health survey update. Spine (Phila Pa 1976). 2000;25(24): 3130-3139. [26] WARE JE JR, SHERBOURNE CD. The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care. 1992;30(6):473-483. [27] JAKOB RP, STÄUBLI HU, DELAND JT. Grading the pivot shift. Objective tests with implications for treatment. J Bone Joint Surg Br. 1987;69(2):294-299. [28] MUSAHL V, CITAK M, O’LOUGHLIN PF, et al. The effect of medial versus lateral meniscectomy on the stability of the anterior cruciate ligament-deficient knee. Am J Sports Med. 2010;38(8):1591-1597. [29] NOYES FR, BARBER SD, MANGINE RE. Abnormal lower limb symmetry determined by function hop tests after anterior cruciate ligament rupture. Am J Sports Med. 1991; 19(5):513-518. [30] REID A, BIRMINGHAM TB, STRATFORD PW, et al. Hop testing provides a reliable and valid outcome measure during rehabilitation after anterior cruciate ligament reconstruction. Phys Ther. 2007;87(3):337-349. [31] RUDOLPH KS, AXE MJ, SNYDER-MACKLER L. Dynamic stability after ACL injury: who can hop? Knee Surg Sports Traumatol Arthrosc. 2000;8(5):262-269. [32] RUDOLPH KS, AXE MJ, BUCHANAN TS, et al. Dynamic stability in the anterior cruciate ligament deficient knee. Knee Surg Sports Traumatol Arthrosc. 2001;9(2):62-71. [33] VAN MELICK N, SENORSKI EH, KRÓLIKOWSKA A, et al. Anterior cruciate ligament reconstruction rehabilitation: Decades of change. Knee Surg Sports Traumatol Arthrosc. 2025;33(4):1178-1182. [34] 王雪飞, 刘强, 钟海珍, 等. 基于中风病患者报告的结局评价量表的第一轮临床验证[J]. 中华中医药杂志,2012,27(3): 603-606. [35] 童健, 孟嘉, 包倪荣, 等. 前交叉韧带重建后的满意度调查[J]. 中国组织工程研究,2017,21(24):3821-3826. [36] BERK AN, PIASECKI DP, FLEISCHLI JE, et al. Trends in Patient-Reported Outcomes After Anterior Cruciate Ligament Reconstruction: A Systematic Review. Orthop J Sports Med. 2023;11(5):23259671231174472. [37] LOUREIRO-NUNO SM, ROMERO-MORALES C, LÓPEZ-LÓPEZ D, et al. Assessing the Predictive Value of Preoperative Knee Function Tests and Self-Report Scores in Anterior Cruciate Ligament Injury Recovery. Sports Health. 2025;19417381251326602. [38] AL-GBURI M, KRISTIANSEN JB, CHRISTENSEN KB, et al. Functional performance tests, clinical measurements, and patient-reported outcome measures do not correlate as outcomes 1 year after anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc. 2023;31(12):5905-5912. [39] KILINC BE, KARA A, CELIK H, et al. Evaluation of the accuracy of Lachman and Anterior Drawer Tests with KT1000 ın the follow-up of anterior cruciate ligament surgery. J Exerc Rehabil. 2016;12(4):363-367. [40] HORVATH A, MEREDITH SJ, NISHIDA K, et al. Objectifying the Pivot Shift Test. Sports Med Arthrosc Rev. 2020;28(2):36-40. [41] BRIGGS KK, LYSHOLM J, TEGNER Y, et al. The reliability, validity, and responsiveness of the Lysholm score and Tegner activity scale for anterior cruciate ligament injuries of the knee: 25 years later. Am J Sports Med. 2009;37(5):890-897. [42] KOCHER MS, STEADMAN JR, BRIGGS KK, et al. Reliability, validity, and responsiveness of the Lysholm knee scale for various chondral disorders of the knee. J Bone Joint Surg Am. 2004;86(6):1139-1145. [43] OHJI S, AIZAWA J, HIROHATA K, et al. Changes in subjective knee function and psychological status from preoperation to 6 months post anterior cruciate ligament reconstruction. J Exp Orthop. 2022;9(1):114. [44] URHAUSEN AP, GRINDEM H, L HI, et al. Patient Acceptable Symptom State Thresholds for IKDC-SKF and KOOS at the 10-Year Follow-up After Anterior Cruciate Ligament Injury: A Study From the Delaware-Oslo ACL Cohort. Orthop J Sports Med. 2024;12(5):23259671241250025. [45] PETUSHEK EJ, DIEKFUSS JA, LAMPLOT JD, et al. Usefulness of Current Patient-Reported Outcome Scales for ACL Injury: A Mixed-Methods Evaluation of Stakeholder-Perceived Utility of Specific Constructs and Items Across the Rehabilitation Timeline. Orthop J Sports Med. 2024;12(3): 23259671231218964. [46] ARDERN CL, GLASGOW P, SCHNEIDERS A, et al. 2016 Consensus statement on return to sport from the First World Congress in Sports Physical Therapy, Bern. Br J Sports Med. 2016;50(14):853-864. [47] ZHANG Y, XI X, HUANG Y. The anchor design of anchor-based method to determine the minimal clinically important difference: a systematic review. Health Qual Life Outcomes. 2023;21(1):74. [48] SEDAGHAT AR. Understanding the Minimal Clinically Important Difference (MCID) of Patient-Reported Outcome Measures. Otolaryngol Head Neck Surg. 2019;161(4):551-560. [49] ANTUNES R, JACOB P, MEYER A, et al. Accuracy of Measuring Knee Flexion after TKA through Wearable IMU Sensors. J Funct Morphol Kinesiol. 2021;6(3):60. [50] ADLOU B, WILBURN C, WEIMAR W. Motion Capture Technologies for Athletic Performance Enhancement and Injury Risk Assessment: A Review for Multi-Sport Organizations. Sensors (Basel). 2025; 25(14):4384. [51] KLÖPFER-KRÄMER I, BRAND A, WACKERLE H, et al. Gait analysis - Available platforms for outcome assessment. Injury. 2020;51 Suppl 2:S90-S96. [52] YANG T, LI Y, YANG L, LIU Q. Magnetic resonance imaging of cruciate ligament disorders: current updates. EFORT Open Rev. 2025;10(7):475-486. [53] BOUSSON V, BENOIST N, GUETAT P, et al. Application of artificial intelligence to imaging interpretations in the musculoskeletal area: Where are we? Where are we going? Joint Bone Spine. 2023;90(1):105493. [54] SCHMIDT S, KRAHL D, PODSZUN J, et al. Combining a digital health application with standard care significantly enhances rehabilitation outcomes for ACL surgery patients. Knee Surg Sports Traumatol Arthrosc. 2025;33(4):1241-1251. |
| [1] | Li Zhifei, Han Bin, Liu Qiuli, Zhang Zhanming, Wei Haokai, Zuo Kuangshi, Zhang Yisheng. Cervical motion characteristics in patients with cervical spondylotic radiculopathy based on motion capture technology [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2286-2293. |
| [2] | Wang Nan, Chen Shuang, Xi Zhipeng, Qian Yuzhang, Zhang Xiaoyu, Gu Jun, Kang Ran, Xie Lin. MRI evaluation of nerve root subsidence sign affecting efficacy of percutaneous endoscopic decompression in lumbar spinal stenosis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2262-2268. |
| [3] | Zhu Xiaolong, Zhang Wei, Yang Yang. Visualization analysis of research hotspots and cutting-edge information in the field of intervertebral disc regeneration and repair [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2391-2402. |
| [4] | Wen Fayan, Li Yan, Qiang Tianming, Yang Chen, Shen Linming, Li Yadong, Liu Yongming. Unilateral biportal endoscopic technology for treatment of lumbar degenerative diseases: global research status and changing trends [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2380-2390. |
| [5] | Xinjiang Branch of China Trauma Rescue & Treatment Association. Expert consensus on diagnosis and treatment of brucellar osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2403-2412. |
| [6] | Li Qingbin, Lin Jianhui, Huang Wenjie, Wang Mingshuang, Du Jiankai, Lao Yongqiang. Bone cement filling after enlarged curettage of giant cell tumor around the knee joint: a comparison of subchondral bone grafting and non-grafting [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 1896-1902. |
| [7] | Jiang Xinghai, Song Yulin, Li Dejin, Shao Jianmin, Xu Junzhi, Liu Huakai, Wu Yingguo, Shen Yuehui, Feng Sicheng. Vascular endothelial growth factor 165 genes transfected into bone marrow mesenchymal stem cells to construct a vascularized amphiphilic peptide gel module [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 1903-1911. |
| [8] | Sun Lei, Zhang Qi, Zhang Yu. Pro-osteoblastic effect of chlorogenic acid protein microsphere/polycaprolactone electrospinning membrane [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 1877-1884. |
| [9] | Wu Yanting, Li Yu, Liao Jinfeng. Magnesium oxide nanoparticles regulate osteogenesis- and angiogenesis-related gene expressions to promote bone defect healing [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 1885-1895. |
| [10] | Chen Haojie, Wang Dai, Shen Shan. Immune inflammatory microenvironment mechanisms in peri-implantitis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2054-2062. |
| [11] | Yang Qiongqiong, Liu Wei. Comparison of performance and clinical effects of zirconia and titanium implants [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2063-2071. |
| [12] | Liu Yang, Liu Donghui , Xu Lei, Zhan Xu, Sun Haobo, Kang Kai. Role and trend of stimuli-responsive injectable hydrogels in precise myocardial infarction therapy [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2072-2080. |
| [13] | Wang Zheng, Cheng Ji, Yu Jinlong, Liu Wenhong, Wang Zhaohong, Zhou Luxing. Progress and future perspectives on the application of hydrogel materials in stroke therapy [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2081-2090. |
| [14] | Guo Yuchao, Ni Qianwei, Yin Chen, Jigeer·Saiyilihan, Gao Zhan . Quaternized chitosan hemostatic materials: synthesis, mechanism, and application [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2091-2100. |
| [15] | Liu Dawei, Cui Yingying, Wang Fanghui, Wang Zixuan, Chen Yuhan, Li Yourui, Zhang Ronghe. Epigallocatechin gallate-mediated bidirectional regulation of reactive oxygen species and its application in nanomaterials [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2101-2112. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||