Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (30): 4863-4869.doi: 10.12307/2021.275
Previous Articles Next Articles
Long-term survival rate and reoperation of Wallis interspinous dynamic stabilization system for treatment of lumbar degenerative disc disease
Gu Honglin, Zheng Xiaoqing, Liang Changxiang, Zeng Shixing, Zhan Shiqiang, Chang Yunbing
- Department of Spine Surgery, Guangdong Provincial People’s Hospital, Guangdong Academy of Medical Sciences, Guangzhou 510080, Guangdong Province, China
-
Received:2021-02-09Revised:2021-02-19Accepted:2021-03-18Online:2021-10-28Published:2021-07-29 -
Contact:Chang Yunbing, MD, Chief physician, Department of Spine Surgery, Guangdong Provincial People’s Hospital, Guangdong Academy of Medical Sciences, Guangzhou 510080, Guangdong Province, China -
About author:Gu Honglin, MD, Attending physician, Department of Spine Surgery, Guangdong Provincial People’s Hospital, Guangdong Academy of Medical Sciences, Guangzhou 510080, Guangdong Province, China -
Supported by:Guangdong Science and Technology Plan Project, No. 2011B061300036 (to ZSQ); Guangdong Provincial Traditional Chinese Medicine Bureau Scientific Research Project, No. 20212001 (to GHL)
CLC Number:
Cite this article
Gu Honglin, Zheng Xiaoqing, Liang Changxiang, Zeng Shixing, Zhan Shiqiang, Chang Yunbing. Long-term survival rate and reoperation of Wallis interspinous dynamic stabilization system for treatment of lumbar degenerative disc disease[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(30): 4863-4869.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
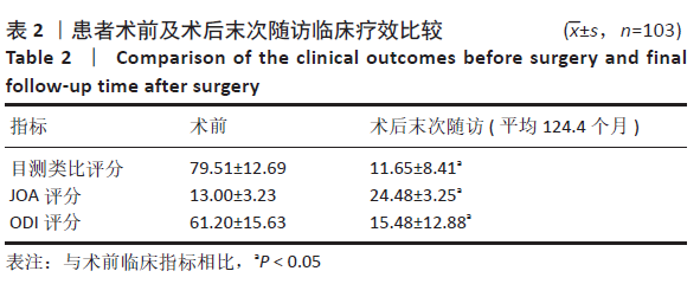
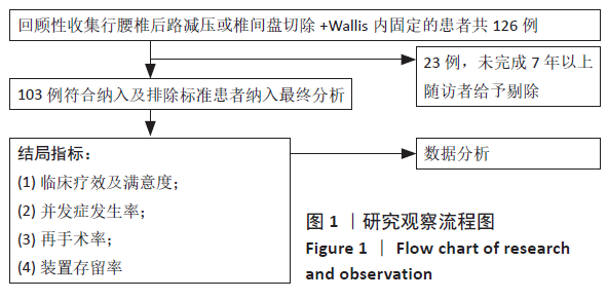
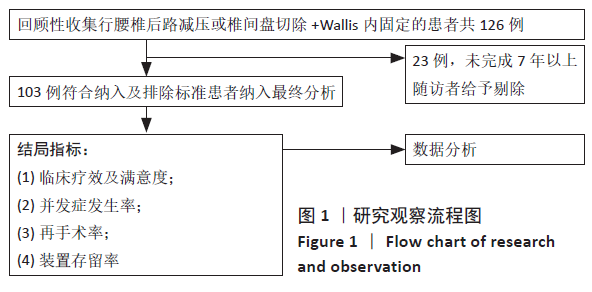
2.2 患者基线资料及一般手术指标分析 103患者例随访92-144个月,平均随访(124.43±11.44)个月;共包括男62例,女41例;年龄19-77岁,平均年龄(43.12±11.51)岁;术前诊断腰椎管狭窄症9例,腰椎间盘突出症46例,腰椎管狭窄症合并腰椎间盘突出症41例,腰椎滑脱症7例。在103例患者中腰椎间盘切除伴/不伴椎管减压者87例(术前诊断为腰椎间盘突出症或腰椎管狭窄症合并腰椎间盘突出症),未行腰椎间盘切除者16例(术前诊断腰椎管狭窄症者或腰椎滑脱症),其中行椎管减压者12例,仅行Wallis植入撑开者4例。共植入Wallis装置107枚,其中单节段植入89例,双节段植入4例,置于融合相邻节段作为Topping-off 10例。手术固定节段:L2/3节段2例,L3/4节段9例,L4/5节段94例,L5/S1节段(均为骶椎腰化)2例。单节段手术时间60-95 min,平均手术时间(73.61±12.07) min;双节段手术时间90-100 min,平均手术时间(94.85±4.81) min;出血量50- 200 mL,平均出血量(70.89±15.30) mL。 2.3 患者临床指标及满意度情况分析 所有患者术后末次随访时目测类比评分、JOA评分及ODI评分均较术前明显改善 (P < 0.05),见表2。"
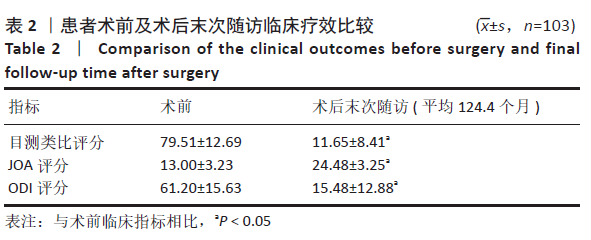
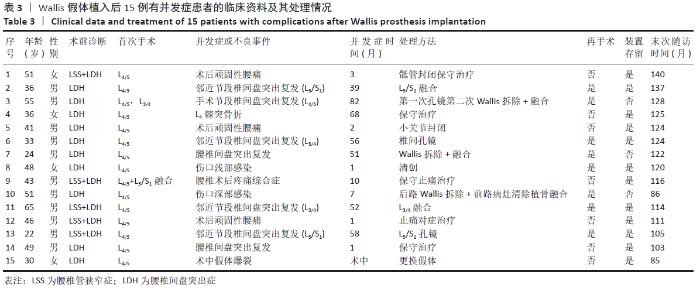
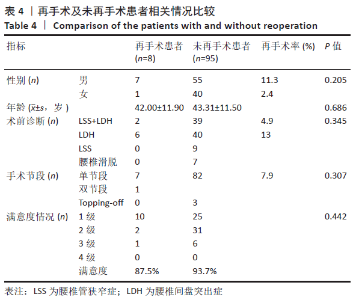
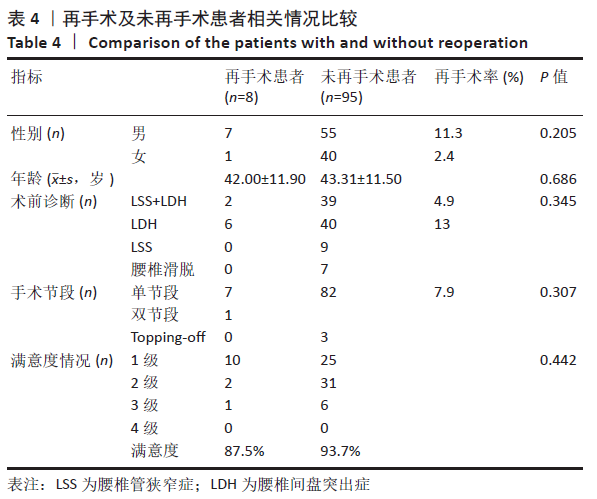
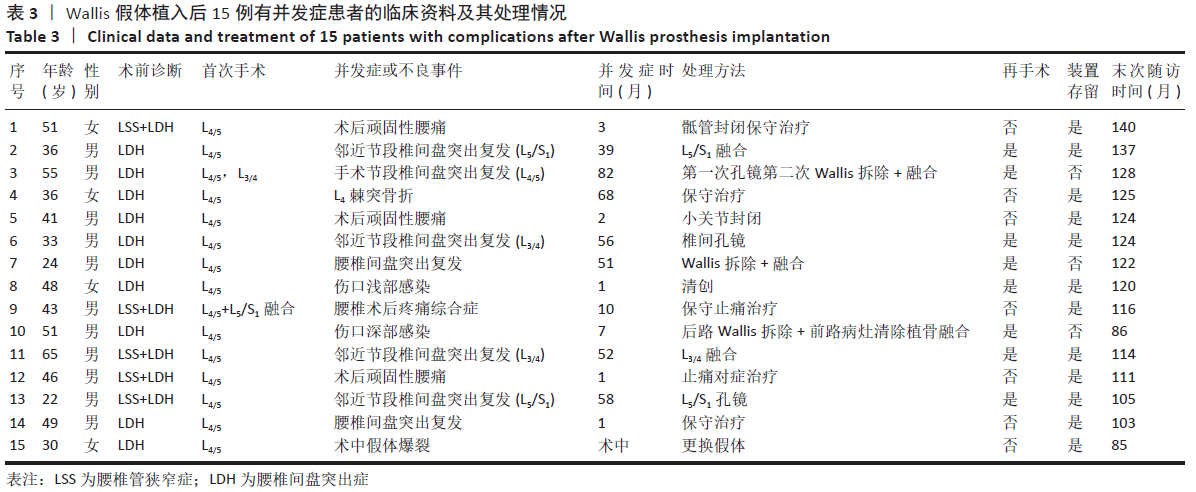
患者末次随访时总体满意度为93.2%。 2.4 患者术后并发症情况分析 共15例患者出现术中及术后并发症,见表3。并发症发生率为14.5%(15/103),术后并发症发生的平均时间为1-82个月,平均时间(30.79±29.83)个月。15例患者均行腰椎间盘切除术伴/不伴椎管减压,行椎间盘切除患者并发症发生率为17.2%(15/87),而未行椎间盘切除的16例患者均无并发症情况。 根据是否与Wallis装置相关分为内固定相关并发症及非内固定相关并发症。其中内固定相关并发症(9例):3例为Wallis手术节段椎间盘突出复发,均为L4/5节段,其中1例24岁男性术后51个月后出现,行Wallis取出+L4/5减压椎间融合内固定术;1例49岁男性术后1个月后出现,经保守治疗后症状好转,未行手术;另外1例L3/4,L4/5双节段Wallis植入,术后6年再次出现右下肢疼痛,经腰椎磁共振确认为L4/5椎间盘突出复发,使用椎间孔镜摘除突出椎间盘后症状缓解,但2个月后再发右下肢疼痛,行磁共振及椎间盘造影确定为L4/5椎间盘突出再次复发,保守治疗无效,行L3/4,L4/5 Wallis取出,L4/5椎间融合;4例为手术邻近节段椎间盘突出复发或再发狭窄:其中2例行椎间孔镜下椎间盘髓核摘除,2例行减压融合;1例36岁女性患者于术后68个月复查X射线片时发现棘突骨折,未行手术,佩戴腰围制动后骨折愈合;1例术中植入过程中假体爆裂,予更换假体。非内固定相关并发症(6例):1例术后1个月出现伤口浅部感染,经清创及抗感染治疗后治愈;1例术后7个月出现伤口深部感染,经腰椎MRI检查及穿刺活检明确为椎间盘炎,予深部清创、Wallis取出及自体髂骨植入椎间融合,术后继续抗感染治疗后症状好转,随访7年患者无不适症状;4例出现术后不明原因腰痛,经实验室检查及影像学检查排除感染、假体及椎管内因素,最终经骶管、小关节封闭或止痛治疗后好转。 根据术后并发症出现的时间,可分为术后早期并发症及术后中远期并发症。其中术后早期并发症(7例):出现在1年内,包括1例手术节段腰椎间盘突出复发,2例手术部位感染,4例术后不明原因腰痛,发生时间为1-10个月,平均发生时间为(3.57±3.55)个月。术后中远期并发症(7例):出现在术后3年以上,包括2例手术节段腰椎间盘突出复发,4例手术邻近节段腰椎间盘突出或再狭窄,1例棘突骨折,发生时间为39-82个月,平均发生时间(58.00±13.70)个月。 2.5 患者术后再手术情况分析 15例患者出现并发症,有8例患者行二次手术,再手术率为7.8%(8/103),其中装置相关并发症的再手术率为5.8%(6/103)。二次手术距首次手术时间为1-82个月,平均时间(43.25±27.09)个月。有3例行装置移除,装置移除的时间为7-82个月,(46.67±37.69)个月,其中2例为腰椎间盘突出复发,均行内固定拆除+融合手术,1例为伤口深部感染。有5例未移除装置:包括1例伤口浅部感染行伤口清创、4例手术邻近节段椎间盘突出复发或再发狭窄行椎间孔镜或融合手术。患者男7例,女1例,男性再手术率为11.3%,女性再手术率为2.4%,男性患者再手术率略高于女性,但无显著差异(P=0.205);再手术患者平均年龄为(42.00±11.90)岁,未再手术患者平均年龄为(43.31±11.50)岁,两者之间无显著差异(P=0.686)。 "
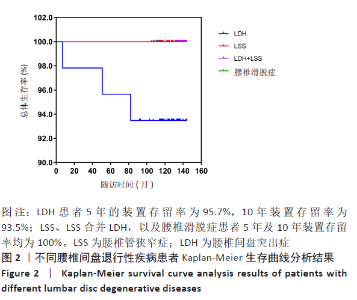
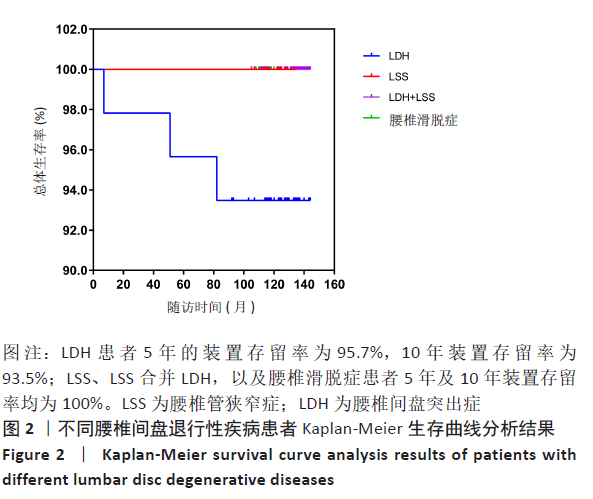
2.6 患者装置存留率情况 103例患者的Wallis总体5年装置存留率为98.1%(101/103),10年存留率为97.1%(100/103)。装置移除的3例患者术前均诊断为腰椎间盘突出症,腰椎间盘突出症患者5年的装置存留率为95.7%(44/46),10年装置存留率为93.5%(43/46)。腰椎管狭窄症、腰椎管狭窄症合并腰椎间盘突出症,以及腰椎滑脱症患者5年及10年装置存留率均为100%(Log Rank,P > 0.05),见图2。而对于不同手术方式,行椎间盘切除术患者5年及10年的装置存留率分别为97.7%(85/87)及96.6%(84/87),未行椎间盘切除术患者5年及10年装置存留率均为100%(Log Rank P > 0.05)。经Cox回归分析,患者年龄、性别、手术节段、手术方式及术前诊断均非影响装置存留率的危险因素(P=0.496,0.965,0.176,0.983,0.952)。"
| [1] MO Z, LI D, ZHANG R, et al. Comparative effectiveness and safety of posterior lumbar interbody fusion, Coflex, Wallis, and X-stop for lumbar degenerative diseases: a systematic review and network meta-analysis. Clin Neurol Neurosurg. 2018;172:74-81. [2] ZINI C, BELLINI M, MASALA S, et al. Percutaneous interspinous spacer in spinal-canal-stenosis treatment: pros and cons. Medicina (Kaunas). 2019;55(7):381. [3] 芦俊峰,王宝东,曹杨.腰椎棘突间撑开系统的分类特点及临床应用[J].中国组织工程研究,2018,22(11):1774-1780. [4] BLOCK J, LAVELLE W, NUNLEY P. Toward a cure for lumbar spinal stenosis: The potential of interspinous process decompression. Med Hypotheses. 2019;132:109357. [5] KOROVESSIS P, REPANTIS T, ZACHARATOS S, et al. Does Wallis implant reduce adjacent segment degeneration above lumbosacral instrumented fusion? Eur Spine J. 2009;18(6):830-840. [6] 赵赫,俞兴,唐向盛,等. Wallis与Coflex两种棘突间动态稳定系统修复腰椎退行性疾病的Meta分析[J].中国组织工程研究,2017, 21(11):1798-1804. [7] SENEGAS J, VITAL JM, POINTILLART V, et al. Long-term actuarial survivorship analysis of an interspinous stabilization system. Eur Spine J. 2007;16(8):1279-1287. [8] NICHOLSON JA, SCOTT C, DUCKWORTH AD, et al. Survival analysis of the Wallis interspinous spacer used as an augment to lumbar decompression. Br J Neurosurg. 2017;31(6):688-694. [9] SVENSSON I, SJOSTROM B, HALJAMAE H. Assessment of pain experiences after elective surgery. J Pain Symptom Manage. 2000; 20(3):193-201. [10] FUKUI M, CHIBA K, KAWAKAMI M, et al. Japanese Orthopaedic Association Back Pain Evaluation Questionnaire. Part 2. Verification of its reliability: the Subcommittee on Low Back Pain and Cervical Myelopathy Evaluation of the Clinical Outcome Committee of the Japanese Orthopaedic Association. J Orthop Sci. 2007;12(6):526-532. [11] FAIRBANK JC, PYNSENT PB. The Oswestry Disability Index. Spine (Phila Pa 1976). 2000;25(22):2940-2952 . [12] SLOSAR PJ, REYNOLDS JB, SCHOFFERMAN J, et al. Patient satisfaction after circumferential lumbar fusion. Spine (Phila Pa 1976). 2000;25(6): 722-726. [13] KIM H, WU P, RAORANE H, et al. Generation change of practice in spinal surgery: can endoscopic spine surgery expand its indications to fill in the role of conventional open spine surgery in most of degenerative spinal diseases and disc herniations: a study of 616 spinal cases 3 years. Neurol India. 2020;68(5):1157-1165. [14] WANG M, ALGHAMDI M. Editorial. Interspinous spacers for lumbar stenosis: time for obsolescence? J Neurosurg. Spine. 2021. doi:10.3171/ 2020.8.SPINE201205. [15] 昌耘冰,王义生,柯雨洪,等.Wallis棘突间动态稳定系统的初步临床应用[J].中国临床解剖学杂志,2009,27(4):487-489. [16] 顾宏林,詹世强,昌耘冰,等.Wallis棘突间动态稳定系统治疗腰椎退行性疾病的中期疗效及并发症分析[J].中国骨科临床与基础研究杂志,2014,6(4):203-209. [17] SENEGAS J, VITAL JM, POINTILLART V, et al. Clinical evaluation of a lumbar interspinous dynamic stabilization device (the Wallis system) with a 13-year mean follow-up. Neurosurg Rev. 2009;32(3): 335-342. [18] 李宗阳,简磊,来佳辉,等.Dynesys与Wallis系统治疗单节段腰椎间盘突出症的长期疗效及安全性[J].中华实用诊断与治疗杂志, 2020,34(3):268-273. [19] 王东杰,杨彬,李宗阳,等.Wallis棘突间动态稳定系统治疗腰椎间盘突出症的长期疗效[J].中国矫形外科杂志,2018,26(13): 1170-1176. [20] 孙浩林,李淳德,刘宪义,等.棘突间动态稳定系统治疗腰椎退变性疾病的并发症分析[J].中华外科杂志,2013,51(1):35-39. [21] EPSTEIN NE. A review of interspinous fusion devices: high complication, reoperation rates, and costs with poor outcomes. Surg Neurol Int. 2012;3:7. [22] PINTAURO M, DUFFY A, VAHEDI P, et al. Interspinous implants: are the new implants better than the last generation? A review. Curr Rev Musculoskelet Med. 2017;10(2):189-198. [23] TRAM J, SRINIVAS S, WALI A, et al. Decompression surgery versus interspinous devices for lumbar spinal stenosis: a systematic review of the literature. Asian Spine J. 2020;14(4):526-542. [24] FORSTH P, OLAFSSON G, CARLSSON T, et al. A randomized, controlled trial of fusion surgery for lumbar spinal stenosis. N Engl J Med. 2016; 374(15):1413-1423. [25] GHOGAWALA Z, DZIURA J, BUTLER WE, et al. Laminectomy plus fusion versus laminectomy alone for lumbar spondylolisthesis. N Engl J Med. 2016;374(15):1424-1434. [26] GOEL S, MODI H. Reoperations following lumbar spinal canal stenosis. Indian J Orthop. 2018;52(6):578-583. [27] RAVINDRA VM, GHOGAWALA Z. Is There still a role for interspinous spacers in the management of neurogenic claudication? Neurosurg Clin N Am. 2017;28(3):321-330. [28] TAMBURRELLI FC, PROIETTI L, LOGROSCINO CA. Critical analysis of lumbar interspinous devices failures: a retrospective study. Eur Spine J. 2011;20(Suppl 1):S27-S35. [29] 朱震奇,刘海鹰,刘辰君,等.棘突间弹性固定翻修术的原因分析[J].中国矫形外科杂志,2018,26(7):582-588. [30] SENEGAS J. Mechanical supplementation by non-rigid fixation in degenerative intervertebral lumbar segments: the Wallis system. Eur Spine J. 2002;11(Suppl 2):S164-S169. [31] SANDU N, SCHALLER B, ARASHO B, et al. Wallis interspinous implantation to treat degenerative spinal disease: description of the method and case series. Expert Rev Neurother. 2011;11(6):799-807. [32] FLOMAN Y, MILLGRAM MA, SMORGICK Y, et al. Failure of the Wallis interspinous implant to lower the incidence of recurrent lumbar disc herniations in patients undergoing primary disc excision. J Spinal Disord Tech. 2007;20(5):337-341. [33] 金新蒙,刘杰,吕枫,等. Wallis棘突间动态稳定系统治疗单纯腰椎间盘突出症的中长期疗效分析[J].中国矫形外科杂志,2016,24(21): 1943-1948. [34] ZHOU Z, JIN X, WANG C, et al. Wallis interspinous device versus discectomy for lumbar disc herniation: a comparative study. Orthopade. 2019;48(2):165-169. [35] ZHOU Z, XIONG W, LI L, et al. Adjacent segmental degeneration following Wallis interspinous stabilization implantation: biomechanical explanations and the value of magnetic resonance imaging. Medicine (Baltimore). 2017;96(22):e7056. [36] OSTER B, KIKANLOO S, LEVINE N, et al. Systematic review of outcomes following 10-year mark of spine patient outcomes research trial for intervertebral disc herniation. Spine. 2020;45(12):825-831. [37] ATLAS SJ, KELLER RB, WU YA, et al. Long-term outcomes of surgical and nonsurgical management of sciatica secondary to a lumbar disc herniation: 10 year results from the maine lumbar spine study. Spine (Phila Pa 1976). 2005;30(8):927-935. [38] GU H, CHANG Y, ZENG S, et al. Wallis interspinous spacer for treatment of primary lumbar disc herniation: three-year results of a randomized controlled trial. World Neurosurg. 2018;120:e1331-e1336. [39] SOBOTTKE R, SCHLUTER-BRUST K, KAULHAUSEN T, et al. Interspinous implants (X Stop, Wallis, Diam) for the treatment of LSS: is there a correlation between radiological parameters and clinical outcome? Eur Spine J. 2009;18(10):1494-1503. [40] ASGARZADIE F, KHOO LT. Minimally invasive operative management for lumbar spinal stenosis: overview of early and long-term outcomes. Orthop Clin North Am. 2007;38(3):387-399. [41] 孙英飞,张启栋,石东平,等.Wallis棘突间动态稳定系统治疗腰椎管狭窄患者的疗效[J].中国现代手术学杂志,2019,23(1):45-49. [42] MARSH GD, MAHIR S, LEYTE A. A prospective randomised controlled trial to assess the efficacy of dynamic stabilisation of the lumbar spine with the Wallis ligament. Eur Spine J. 2014;23(10):2156-2160. |
| [1] | He Xinyu, Zhou Honghai, Jiang Hong, Ma Zhijia, Su Shaoting, Lin Zehong, Tian Junming, Chen Longhao, Liu Baijie. Changes in lumbosacral sagittal plane parameters of L5/S1 disc herniation reabsorption [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1330-1335. |
| [2] | Yu Weijie, Liu Aifeng, Chen Jixin, Guo Tianci, Jia Yizhen, Feng Huichuan, Yang Jialin. Advantages and application strategies of machine learning in diagnosis and treatment of lumbar disc herniation [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1426-1435. |
| [3] | Ma Shuwei, He Sheng, Han Bing, Zhang Liaoyun. Exosomes derived from mesenchymal stem cells in treatment of animals with acute liver failure: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1137-1142. |
| [4] | Zhang Rui, Wang Kun, Shen Zicong, Mao Lu, Wu Xiaotao. Effects of endoscopic foraminoplasty and laminoplasty on biomechanical properties of intervertebral disc and isthmus [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 833-839. |
| [5] | Liu Changzhen, Liu Xin, Li Yuefei, Wang Jianye, Feng Zhimeng, Sun Zhaozhong. Imaging landmarks of one-hole split endoscope in the treatment of upper lumbar intervertebral disc herniation under the guidance of three-dimensional reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 939-944. |
| [6] | Wang Jiani, Chen Junyu. Angiogenesis mechanism of metal ions and their application in bone tissue engineering [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(5): 804-812. |
| [7] | Xu Gang, Zhang Changchun, Zhu Kun, Ye Yuchen, Zhou Pinghui. Effects of miR-141-3p on dorsal root ganglion inflammation and lower limb pain in rats with lumbar disc herniation [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(16): 2593-2598. |
| [8] | Liang Hairui, Cai Zhencun, Zhang He, Duan Siyu, Chen Beibei. Application of pulsed electromagnetic fields in the treatment of orthopedic diseases [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(12): 1944-1949. |
| [9] | Wang Mei, Suo Na, Yu Huan, Yang Jianbo. Mechanism of miR-206 on inflammation, analgesia and autophagy related proteins in nucleus pulposus of rats with lumbar disc herniation [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(11): 1712-1718. |
| [10] | . Changes in Lumbosacral Sagittal Plane Parameters of L5/S1 Disc Herniation [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(在线): 1-6. |
| [11] | You Zhengqiu, Zhang Zhongzu, Wang Qunbo. Early symptomatic intervertebral disc pseudocysts after discectomy detected on MRI [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1403-1409. |
| [12] | Yuan Haibo, Li Dongya, Pan Bin, Guan Kai, Chen Feng, Yuan Feng, Wu Jibin. Sagittal related factors of upper lumbar disc herniation [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(31): 4984-4989. |
| [13] | Wang Chunyu, Chen Zhigang, Zhang Jianli. Effects of mecobalamin on neuropathic pain and acid-sensing ion channels in a rat model of lumbar disc herniation [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(17): 2658-2663. |
| [14] | Li Xin, Luo Mingran, Li Gen, Cheng Lin, Pan Bin, Yuan Feng. Establishment and validation of a prognostic model for the recurrence risk after percutaneous endoscopic lumbar discectomy [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(13): 2087-2092. |
| [15] | Lu Yu, Xiang Junyi, Yin Benjing, Bi Heng, Li Jizheng, Wei Jiajia, Jia Tao, Li Pengfei, Li Jubao. Finite element comparative analysis on treatment of lumbar disc herniation by the oblique wrench method and the combination of traction, pressing, and oblique pulling [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(13): 2011-2015. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||