Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (21): 3401-3408.doi: 10.3969/j.issn.2095-4344.3854
Previous Articles Next Articles
Local infiltration anesthesia versus femoral nerve block for pain control and safety after total knee arthroplasty: a meta-analysis
Deng Zhibo, Li Zhi, Wu Yahong, Mu Yuan, Mu Yuexi, Yin Liangjun
- Department of Orthopedics, Second Affiliated Hospital of Chongqing Medical University, Chongqing 400010, China
-
Received:2020-08-31Revised:2020-09-04Accepted:2020-09-21Online:2021-07-28Published:2021-01-25 -
Contact:Yin Liangjun, MD, Chief physician, Master’s supervisor, Department of Orthopedics, Second Affiliated Hospital of Chongqing Medical University, Chongqing 400010, China -
About author:Deng Zhibo, Master candidate, Department of Orthopedics, Second Affiliated Hospital of Chongqing Medical University, Chongqing 400010, China -
Supported by:the Livelihood Project of Chongqing Science and Technology Commission, No. cstc2017shmsA130049 (to YLJ); the Chongqing Science and Technology Plan Project, No. cstc2018jscx-msybX0088 (to YLJ)
CLC Number:
Cite this article
Deng Zhibo, Li Zhi, Wu Yahong, Mu Yuan, Mu Yuexi, Yin Liangjun. Local infiltration anesthesia versus femoral nerve block for pain control and safety after total knee arthroplasty: a meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3401-3408.
share this article
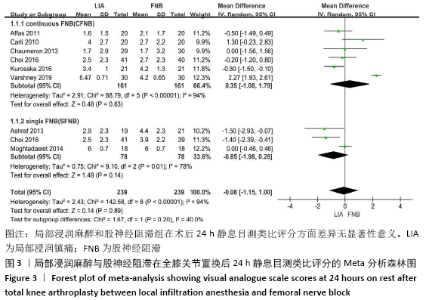
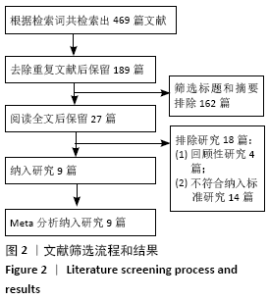
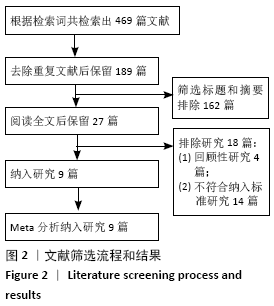
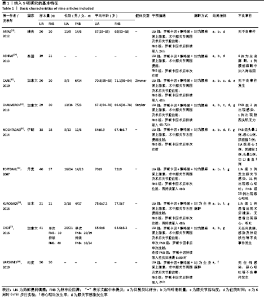
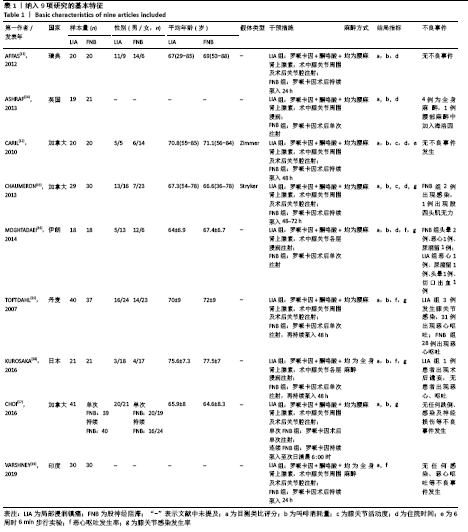
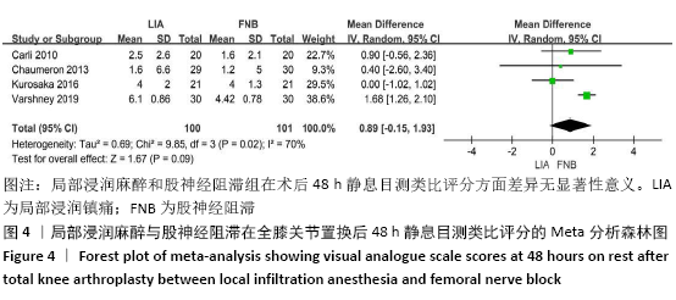
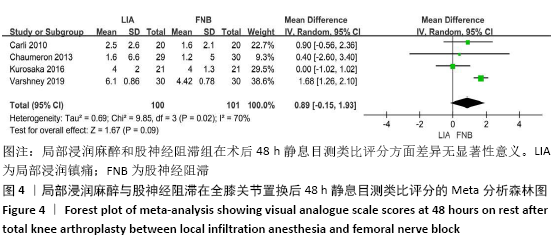
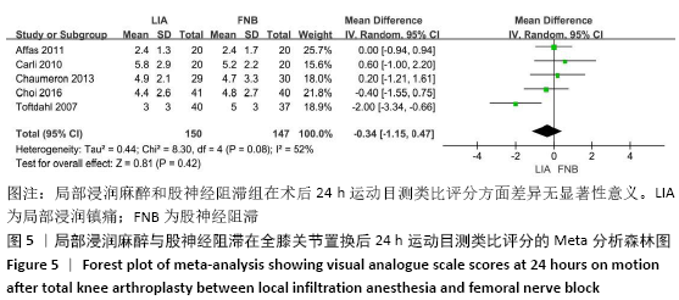
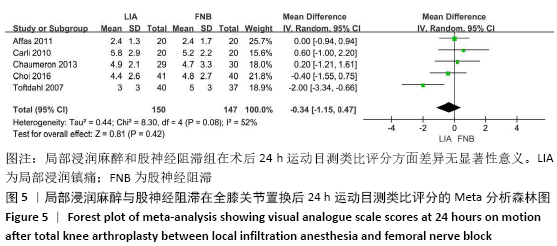
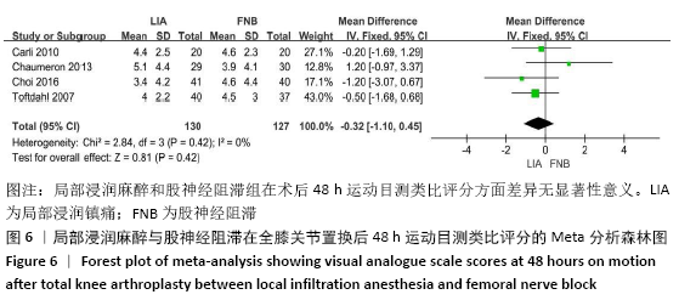
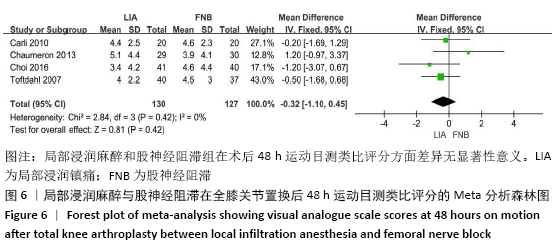
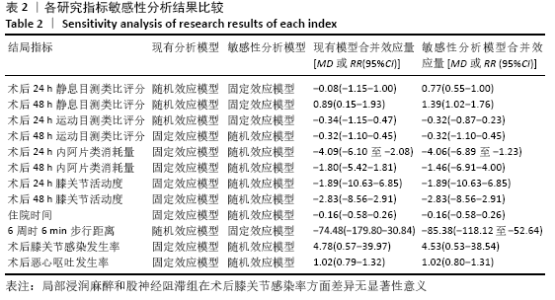
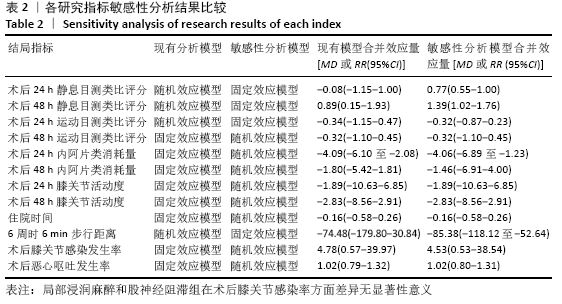
2.2 文献质量评估结果 文章采用Cochrane协作工具评估随机对照试验的偏倚风险评价。有7篇文献详细介绍了随机分配方法[12-18],包括随机数字表、随机化表和随机数发生器;有7篇文献记录了通过密封信封来隐藏分配信息[11-15,17,19],有4篇文献报道了对参与者和实施者的双盲法[15-17,19],有6篇研究对所有结果评估均采用了盲法[12,14-17,19],有1篇文献可能有不完整数据报告[13],所有文献均无选择性报告或其他偏倚。因此总体分析纳入文献的偏倚呈低风险。 2.3 Meta分析结果 2.3.1 各组镇痛相关指标比较 术后目测类比评分:有9项研究报道了全膝关节置换后24 h和48 h的静息及运动目测类比评分[11-19]。对于在全膝关节置换后24 h静息及运动时和48 h的静息目测类比评分,异质性结果显示各研究间有异质性(I2 24 h静息=94%;I224 h运动=52%;I248 h静息=70%),通过敏感性分析,考虑为文献质量相对较低的2篇文献所致[12,19],且其围术期口服镇痛药物与其他文献不完全一致,故采用随机效应模型;而术后48 h的运动目测类比评分无异质性(I2=0%),采用固定效应模型。结果显示两组患者术后目测类比评分比较均无显著性差异(MD24 h静息= -0.08,95%CI:-1.15-1.00,P=0.89;MD24 h运动=-0.34,95%CI:-1.15-0.47,P=0.42;MD48 h静息=0.89,95%CI:-0.15-1.93,P=0.09;MD48 h运动=-0.32,95%CI: -1.10-0.45),术后24 h静息亚组分析也显示单次FNB组或持续FNB组与LIA组比差异无显著性意义(MD=0.35,95%CI:-1.08-1.79,P=0.63;MD=-0.85,95%CI:?1.98-0.28,P=0.14),见图3-6。"
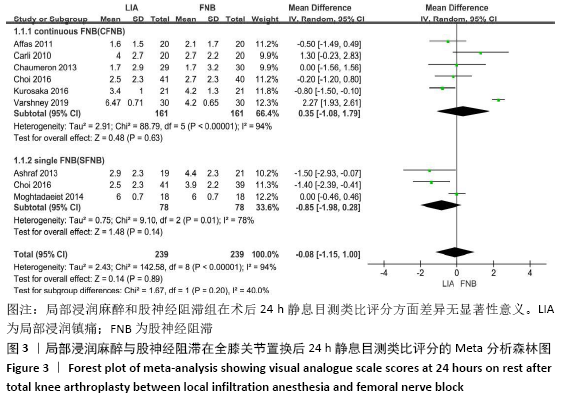
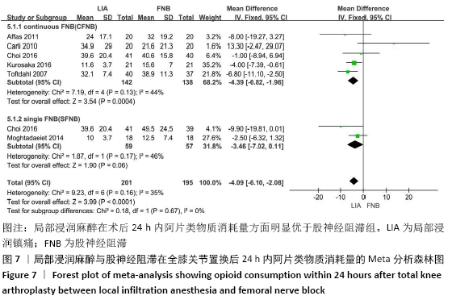
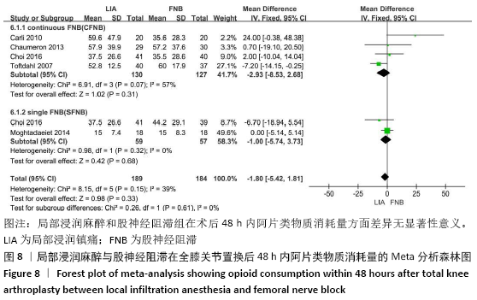
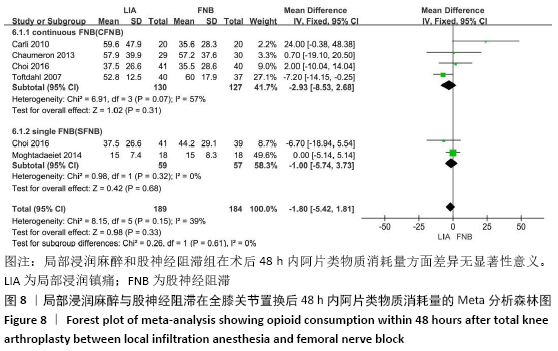
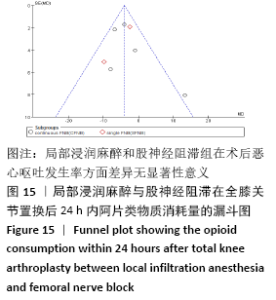
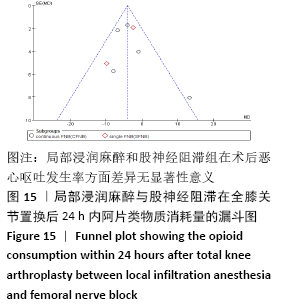
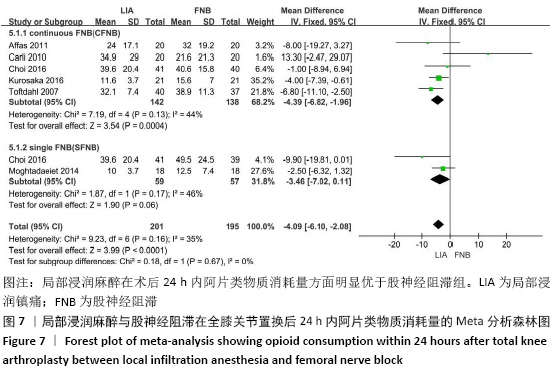
阿片类物质消耗量:有8项研究报道了全膝关节置换后0-24 h和 0-48 h的阿片类物质消耗量[11-13,15-19]。异质性结果显示均无显著异质性(I224 h= 35%,I248 h=39%),采用固定效应模型。分析结果显示两组患者在48 h内无显著性差异(MD=-1.80,95%Cl:-5.42-1.81,P=0.33),但24 h内LIA组明显优于FNB组(MD=-4.09,95%CI:-6.10至-2.08,P < 0.000 1)。在亚组分析中,24 h内LIA组阿片类药物消耗量也明显低于持续FNB组(MD=-4.39,95%CI: -6.82至-1.96,P=0.000 4),虽然与单次FNB组对比未达到显著性差异(MD= -3.46,95%CI:-7.02-0.11,P=0.06),但P值非常接近0.05,所以文章认为在术后早期LIA消耗阿片类量明显比FNB组少,见图7,8。 "
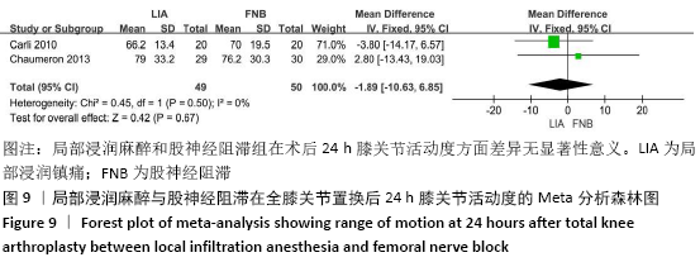
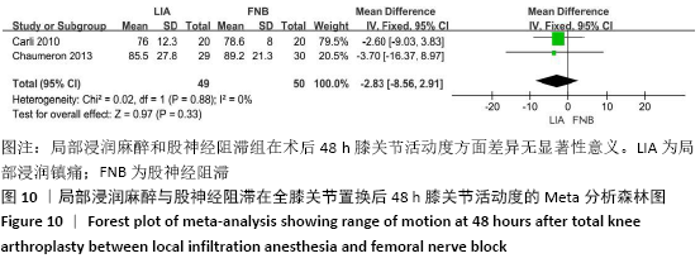
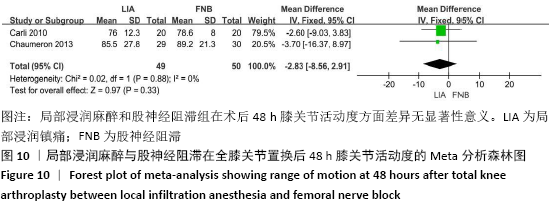
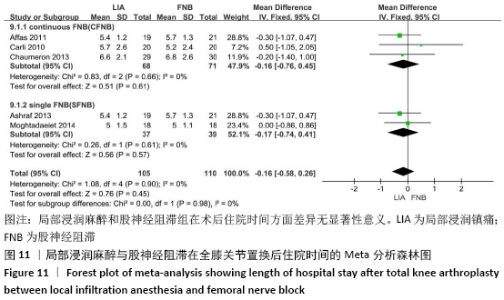
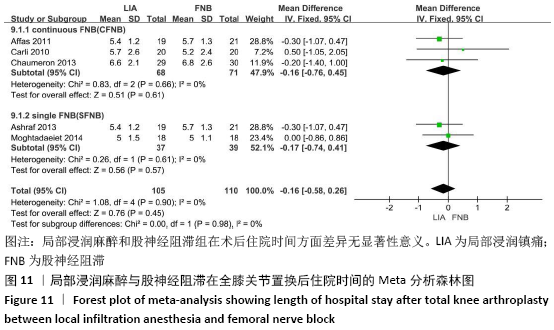
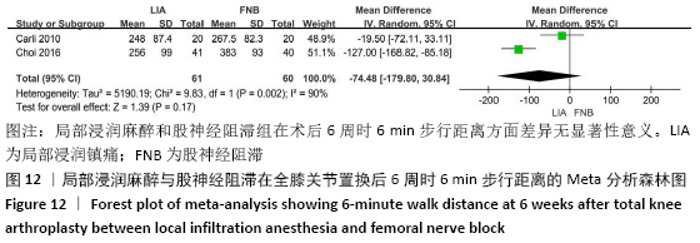
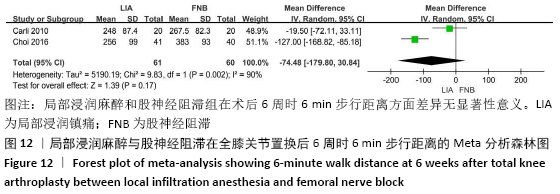
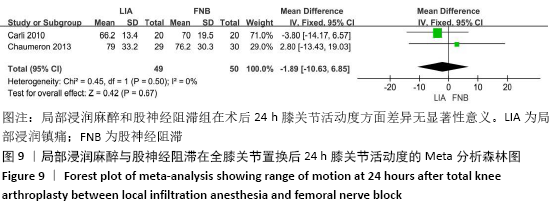
2.3.2 各组膝关节功能恢复相关结果比较 有6项研究记录了全膝关节置换后的膝关节功能恢复相关指标[11-13,15-17]。对于术后24 h和48 h内的膝关节活动度、住院时间,异质性结果显示均无显著异质性(I2=0%),采用固定效应模型;而术后6周的6 min步行距离(6MWT-6W),存在显著异质性(I2=90%),采用随机效应模型。分析结果显示两组在术后膝关节活动度(MD24 h=-1.89,95%CI:-10.63-6.85,P=0.67;MD48 h= -2.83,95%CI:-8.56-2.91,P=0.33)、住院时间(MD=-0.16,95%CI:-0.58-0.26,P=0.45)、6周6 min步行距离 (MD=-74.48,95%CI:-179.80-30.84,P=0.17)差异无显著性意义,同时住院时间亚组分析也表现了相同的结果(MD单次FNB= -0.17,95%CI:-0.74,0.41,P=0.57;MD持续FNB=-0.16,95%CI:-0.76,0.45,P=0.61),见图9-12。"
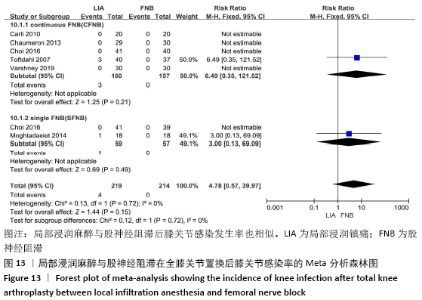
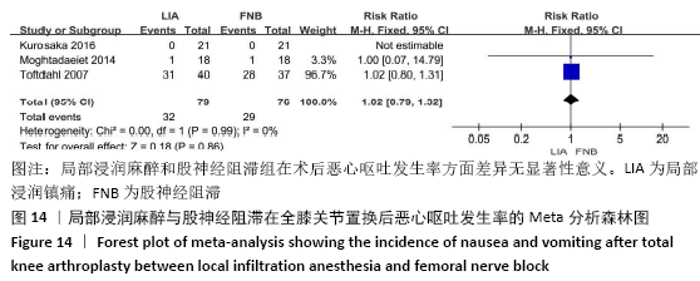
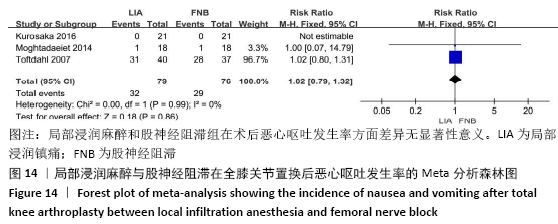
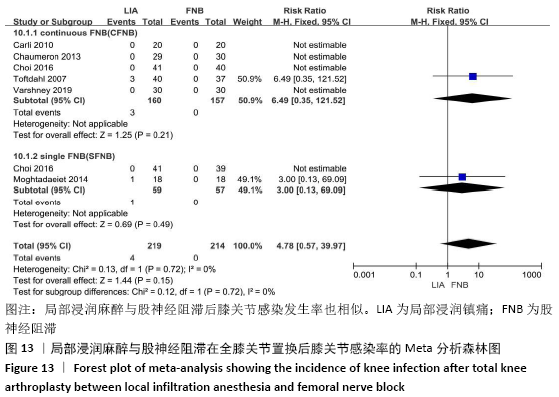
2.3.3 各组并发症比较 有4项研究共392膝记录了置换后感染的发生 率[11-12,15,17]。因为检测结果无显著异质性(I2=0%),采用固定效应模型。Meta分析发现两组患者在膝关节感染方面无显著性差异(RR=4.78,95%CI:0.57-39.97,P=0.15),同时亚组分析显示LIA组与持续FNB组或单次FNB组膝关节感染发生率也相似(RR持续FNB=6.49,95%CI:0.35-121.52,P=0.21;RR单次FNB= 3.00,95%CI:0.13-69.09,P=0.49),见图13。有3项随机对照试验共155例患者记录了术后恶心呕吐的发生率比较[11,16,18],无显著异质性(I2=0%),同样未发现两组间有显著性差异(RR=1.02,95%CI:0.79-1.32,P=0.86),见图14。 "
| [1] LI S, LUO X, WANG P, et al. Clinical outcomes of gap balancing vs measured resection in total knee arthroplasty: a systematic review and meta-analysis involving 2259 subjects. J Arthroplasty. 2018;33(8):2684-2693. [2] AHMED GO, ELSWEIFY K, AHMED AF, et al. Usability of the AAOS Appropriate Use Criteria (AUC) for the surgical management of knee osteoarthritis in clinical practice. Knee Surg Sports Traumatol Arthrosc. 2020;28(7):2077-2081. [3] MA HH, CHOU TA, TSAI SW, et al. The efficacy of continuous versus single-injection femoral nerve block in Total knee Arthroplasty: a systematic review and Meta-analysis. BMC Musculoskelet Disord. 2020;21(1):121-129. [4] FEIBEL RJ, DERVIN GF, KIM PR, et al. Major complications associated with femoral nerve catheters for knee arthroplasty: a word of caution. J Arthroplasty. 2009;24(6 Suppl): 132-137. [5] BORYS M, DOMAGALA M, WENCLAW K, et al. Continuous femoral nerve block is more effective than continuous adductor canal block for treating pain after total knee arthroplasty: a randomized, double-blind, controlled trial. Medicine (Baltimore). 2019;98(39):e17358. [6] WEI BJ,DONG A,ANAHI P, et al. Adjuncts to local anesthetic wound infiltration for postoperative analgesia: a systematic review. Reg Anesth Pain Med. 2020;45(8):645-655. [7] ONG P, TANG X, CHENG R, et al. Comparison of the efficacy of different analgesia treatments for total knee arthroplasty: a network meta-analysis. Clin J Pain. 2018;34(11):1047-1060. [8] ZHANG LK, MA JX, KUANG MJ, et al. Comparison of periarticular local infiltration analgesia with femoral nerve block for total knee arthroplasty: a meta-analysis of randomized controlled trials. J Arthroplasty. 2018;33(6):1972-1978. [9] ALBRECHT E, GUYEN O, JACOT-GUILLARMOD A, et al. The analgesic efficacy of local infiltration analgesia vs femoral nerve block after total knee arthroplasty: a systematic review and Meta-analysis. Br J Anaesth. 2016;116(5):597-609. [10] ZHAO X, QIN J, TAN Y, et al. Efficacy of steroid addition to multimodal cocktail periarticular injection in total knee arthroplasty: a Meta-analysis. J Orthop Surg Res. 2015;10(1):75-86. [11] TOFTDAHL K, NIKOLAJSEN L, HARALDSTED V, et al. Comparison of peri- and intraarticular analgesia with femoral nerve block after total knee arthroplasty: a randomized clinical trial. Acta Orthop. 2007;78(2):172-179. [12] CARLI F, CLEMENTE A, ASENJO JF, et al. Analgesia and functional outcome after total knee arthroplasty: periarticular infiltration vs continuous femoral nerve block. Br J Anaesth. 2010;105(2):185-195. [13] AFFAS F, NYGARDS EB, STILLER CO, et al. Pain control after total knee arthroplasty: a randomized trial comparing local infiltration anesthesia and continuous femoral block. Acta Orthop. 2011;82(4):441-447. [14] ASHRAF A, RAUT VV, CANTY SJ, et al. Pain control after primary total knee replacement. A prospective randomised controlled trial of local infiltration versus single shot femoral nerve block. Knee. 2013;20(5):324-327. [15] CHAUMERON A, AUDY D, DROLET P, et al. Periarticular injection in knee arthroplasty improves quadriceps function. Clin Orthop Relat Res. 2013;471(7):2284-2295. [16] MOGHTADAEI M, FARAHINI H, FAIZ SH, et al. Pain management for total knee arthroplasty: single-injection femoral nerve block versus local infiltration analgesia. Iran Red Crescent Med J. 2014;16(1):e13247. [17] CHOI S, O’HARE T, GOLLISH J, et al. Optimizing pain and rehabilitation after knee arthroplasty: a two-center, randomized trial. Anesth Analg. 2016;123(5):1316-1324. [18] KUROSAKA K, TSUKADA S, SEINO D, et al. Local infiltration analgesia versus continuous femoral nerve block in pain relief after total knee arthroplasty: a randomized controlled trial. J Arthroplasty. 2016;31(4):913-917. [19] VARSHNEY RK, PRASAD MK, GARG M. Comparison of continuous femoral nerve block with local infiltration for postoperative analgesia in unilateral total knee arthroplasty- a randomized controlled trial. Anaesth Pain Inten Care. 2019;23(3):268-273. [20] FU H, WANG J, ZHANG W, et al. Potential superiority of periarticular injection in analgesic effect and early mobilization ability over femoral nerve block following total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2017;25(1):291-298. [21] KUANG MJ, XU LY, MA JX, et al. Adductor canal block versus continuous femoral nerve block in primary total knee arthroplasty: a Meta-analysis. Int J Surg. 2016;31(3):17-24. [22] LAU HP, YIP KM, JIANG CC. Regional nerve block for total knee arthroplasty. J Formos Med Assoc. 1998;97(6):428-430. [23] 周宗科,翁习生,曲铁兵,等.中国髋、膝关节置换加速康复-围术期管理策略专家共识[J].中华骨与关节外科杂志,2016,9(1):1-9. [24] SEET E, LEONG WL, YEO AS, et al. Effectiveness of 3-in-1 continuous femoral block of differing concentrations compared to patient controlled intravenous morphine for post total knee arthroplasty analgesia and knee rehabilitation. Anaesth Inten Care. 2006;34(1):25-30. [25] HUNT KJ, BOURNE MH, MARIANI EM. Single-injection femoral and sciatic nerve blocks for pain control after total knee arthroplasty. J Arthroplasty. 2009;24(4):533-538. [26] KERR DR, KOHAN L. Local infiltration analgesia: a technique for the control of acute postoperative pain following knee and hip surgery: a case study of 325 patients. Acta Orthop. 2008;79(2):174-183. [27] BUSCH CA, SHORE BJ, BHANDARI R, et al. Efficacy of periarticular multimodal drug injection in total knee arthroplasty. A randomized trial. J Bone Joint Surg Am. 2006; 88(5):959-963. [28] TIAN Y, TANG S, SUN S, et al. Comparison between local infiltration analgesia with combined femoral and sciatic nerve block for pain management after total knee arthroplasty. J Orthop Surg Res. 2020;15(1):41. [29] DILLON JP, BRENNAN L, MITCHELL D. Local infiltration analgesia in hip and knee arthroplasty: an emerging technique. Acta Orthop Belg. 2012;78(2):158-163. [30] SARDANA V, BURZYNSKI JM, SCUDERI GR. Adductor canal block or local infiltrate analgesia for pain control after total knee arthroplasty? A systematic review and meta-analysis of randomized controlled trials. J Arthroplasty. 2019;34(1):183-189. |
| [1] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [2] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [3] | Chen Jinping, Li Kui, Chen Qian, Guo Haoran, Zhang Yingbo, Wei Peng. Meta-analysis of the efficacy and safety of tranexamic acid in open spinal surgery [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1458-1464. |
| [4] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [5] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [6] | Wang Yongsheng, Wu Yang, Li Yanchun. Effect of acute high-intensity exercise on appetite hormones in adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1305-1312. |
| [7] | Kong Desheng, He Jingjing, Feng Baofeng, Guo Ruiyun, Asiamah Ernest Amponsah, Lü Fei, Zhang Shuhan, Zhang Xiaolin, Ma Jun, Cui Huixian. Efficacy of mesenchymal stem cells in the spinal cord injury of large animal models: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1142-1148. |
| [8] | Zhao Zhongyi, Li Yongzhen, Chen Feng, Ji Aiyu. Comparison of total knee arthroplasty and unicompartmental knee arthroplasty in treatment of traumatic osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 854-859. |
| [9] | Zhang Nianjun, Chen Ru. Analgesic effect of cocktail therapy combined with femoral nerve block on total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 866-872. |
| [10] | Yuan Jun, Yang Jiafu. Hemostatic effect of topical tranexamic acid infiltration in cementless total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 873-877. |
| [11] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Intravenous, topical tranexamic acid alone or their combination in total knee arthroplasty: a meta-analysis of randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 948-956. |
| [12] | Li Yan, Wang Pei, Deng Donghuan, Yan Wei, Li Lei, Jiang Hongjiang. Electroacupuncture for pain control after total knee arthroplasty: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 957-963. |
| [13] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| [14] | Hua Haotian, Zhao Wenyu, Zhang Lei, Bai Wenbo, Wang Xinwei. Meta-analysis of clinical efficacy and safety of antibiotic artificial bone in the treatment of chronic osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 970-976. |
| [15] | Zhan Fangbiao, Cheng Jun, Zou Xinsen, Long Jie, Xie Lizhong, Deng Qianrong. Intraoperative intravenous application of tranexamic acid reduces perioperative bleeding in multilevel posterior spinal surgery: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 977-984. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||