Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (36): 5793-5799.doi: 10.3969/j.issn.2095-4344.2899
Previous Articles Next Articles
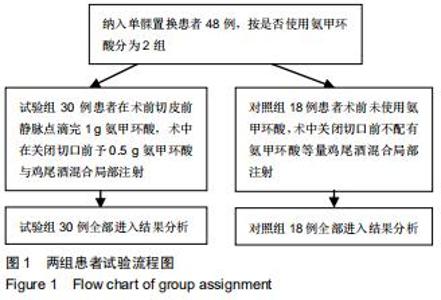
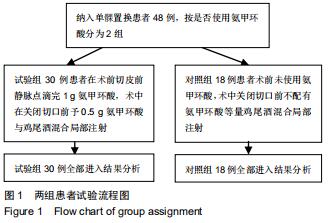
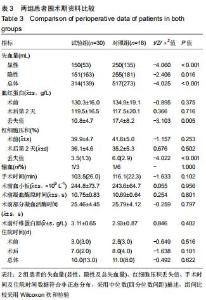
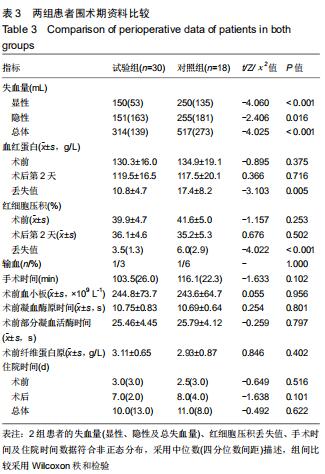
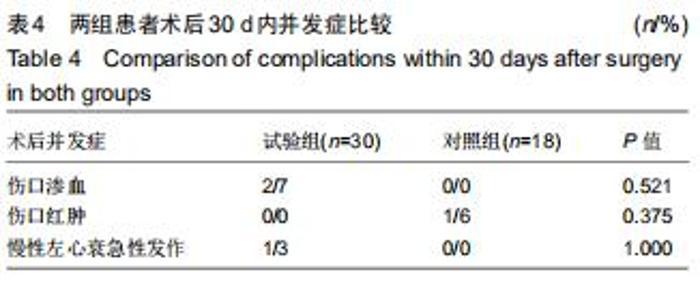
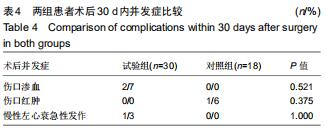
Hemostatic effect and safety of intravenous combined with topical administration of tranexamic acid on unicompartmental knee arthroplasty
Deng Zengfa, He Zhiyong, Liu Kang, Yu Xinping, Liang Jianji, Wang Jinjun, Li Chen, Guo Zhouyang
- Zhongshan People’s Hospital, Zhongshan 528403, Guangdong Province, China
-
Received:2020-02-10Revised:2020-02-18Accepted:2020-03-14Online:2020-12-28Published:2020-10-27 -
Contact:He Zhiyong, Master, Chief physician, Master’s supervisor, Zhongshan People’s Hospital, Zhongshan 528403, Guangdong Province, China -
About author:Deng Zengfa, Master candidate, Zhongshan People’s Hospital, Zhongshan 528403, Guangdong Province, China
CLC Number:
Cite this article
Deng Zengfa, He Zhiyong, Liu Kang, Yu Xinping, Liang Jianji, Wang Jinjun, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous combined with topical administration of tranexamic acid on unicompartmental knee arthroplasty[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(36): 5793-5799.
share this article
|
[1] COOK R, DAVIDSON P, WHITE A. Partial knee replacement could be first choice for some patients with osteoarthritis. BMJ. 2019; 367:15994.
[2] MURRAY DW, PARKINSON RW. Usage of unicompartmental knee arthroplasty. Bone Joint J. 2018;100-B:432-435.
[3] ZHANG Z, MIN J, WANG D, et al. Analysis on the occult blood loss after unicompartment knee arthroplasty. China J Orthop Traumatol. 2017; 30: 1013-1017.
[4] 乔松义,孟祥奇,罗斌,等.单髁置换术与全膝置换术治疗膝骨关节炎疗效的Meta分析[J].中华关节外科杂志(电子版),2019,13(2):189-199.
[5] 徐浩,李志杰,李娅娟,等.关节腔灌注氨甲环酸对关节置换术后失血膝关节功能恢复的影响[J].中华实验外科杂志,2017,34(10):1781-1784.
[6] CONLON NP, BALE EP, HERBISON GP, et al. Postoperative anemia and quality of life after primary hip arthroplasty in patients over 65 years old. Anesth Analg. 2008;106(4):1056-1061.
[7] 龙也,王通,刘佳鑫,等.重组人促红细胞生成素联合铁剂纠正老年股骨转子间骨折患者围术期贫血的临床研究[J].中国修复重建外科杂志,2019,33(6):662-665.
[8] TENGBORN L, BLOMBÄCK M, BERNTORP E. Tranexamic acid--an old drug still going strong and making a revival. Thromb Res. 2015;135:231-242.
[9] SENTILHES L, LASOCKI S, DUCLOY-BOUTHORS AS, et al. Tranexamic acid for the prevention and treatment of postpartum haemorrhage. Br J Anaesth. 2015;114: 576-587.
[10] WALKER PF, FOSTER AD, ROTHBERG PA, et al. Tranexamic acid decreases rodent hemorrhagic shock-induced inflammation with mixed end-organ effects. PloS One. 2018; 13: e208249.
[11] LEVY JH, KOSTER A, QUINONES QJ, et al. Antifibrinolytic Therapy and Perioperative Considerations. Anesthesiology. 2018; 128:657-670.
[12] SONG SJ, LEE HW, BAE DK, et al. Daily blood loss transition after total knee arthroplasty with topical administration of tranexamic acid: Paradoxical blood loss after action of tranexamic acid. J Orthop Surg (Hong Kong). 2020; 28: 615556104.
[13] LEI Y, XIE J, HUANG Q, et al. The antifibrinolytic and anti- inflammatory effects of a high initial-dose tranexamic acid in total knee arthroplasty: a randomized controlled trial. Int Orthop. 2020; 44(3):477-486.
[14] LIU Q, GENG P, SHI L, et al. Tranexamic acid versus aminocaproic acid for blood management after total knee and total hip arthroplasty: A systematic review and meta-analysis. Int J Surg. 2018; 54: 105-112.
[15] DORWEILER MA, BOIN MA, FROEHLE AW, et al. Improved early postoperative range of motion in total knee arthroplasty using tranexamic acid: a retrospective analysis. J Knee Surg. 2019; 32: 160-164.
[16] 褚国庆,刘藜箬,闫明童,等.氨甲环酸静脉联合局部用药减少初次单侧膝关节置换出血[J].中华关节外科杂志(电子版), 2018,12(5):671-675.
[17] 刘新明,陈晓红,殷力.氨甲环酸与混合镇痛药物关节腔注射在TKA手术中应用效果分析[J].中国骨与关节损伤杂志,2018,33(12):1299-1301.
[18] WU J, FENG S, CHEN X, et al. Intra-articular injection of tranexamic acid on perioperative blood loss during unicompartmental knee arthroplasty. Med Sci Monit. 2019;25:5068-5074.
[19] 曾兵,刘刚,贺志盛,等.氨甲环酸关节腔内注射联合置换后3h夹闭引流管对膝关节单髁置换失血量的影响[J].中国组织工程研究,2016, 20(22):3197-3204.
[20] 文涛,薛华明,马童,等.氨甲环酸对减少单髁置换术后出血量的效果评价[J].生物骨科材料与临床研究,2016,13(5):51-54.
[21] 冯硕,吴居泰,查国春,等.关节腔内注射氨甲环酸对单髁置换术围手术期失血量的影响[J].中华骨与关节外科杂志,2016,9(5):402-406.
[22] 罗兵,袁毅,杨家福,等.关节腔注射氨甲环酸并夹闭引流管对膝关节单间室骨性关节炎单髁置换术后出血量的影响[J].中国骨与关节损伤杂志, 2018,33(6):579-582.
[23] POERAN J, RASUL R, SUZUKI S, et al. Tranexamic acid use and postoperative outcomes in patients undergoing total hip or knee arthroplasty in the United States: retrospective analysis of effectiveness and safety. BMJ.2014;349:g4829.
[24] LÓPEZ-HUALDA Á, DAUDER-GALLEGO C, FERREÑO- MÁRQUEZ D, et al. Efficacy and safety of topical tranexamic acid in knee arthroplasty. Med Clin. 2018;151:431-434.
[25] ZHANG Y, YANG B, SUN X, et al. Combined intravenous and intra-articular tranexamic acid administration in total knee arthroplasty for preventing blood loss and hyperfibrinolysis: A randomized controlled trial. Medicine. 2019; 98: e14458.
[26] DASTRUP A, POTTEGÅRD A, HALLAS J, et al. Perioperative tranexamic acid treatment and risk of cardiovascular events or death after total hip arthroplasty: a population-based cohort study from national danish databases. J Bone Joint Surg Am. 2018; 100: 1742-1749.
[27] WU Y, ZENG Y, HU Q, et al. Blood loss and cost-effectiveness of oral vs intravenous tranexamic acid in primary total hip arthroplasty: A randomized clinical trial. Thromb Res. 2018;171:143-148.
[28] WILDE JM, COPP SN, MCCAULEY JC, et al. One dose of intravenous tranexamic acid is equivalent to two doses in total hip and knee arthroplasty. J Bone Joint Surg. 2018; 100:1104-1109.
[29] EL BEHEIRY H, LUBBERDINK A, CLEMENTS N, et al. Tranexamic acid administration to older patients undergoing primary total hip arthroplasty conserves hemoglobin and reduces blood loss. Can J Surg. 2018; 61: 177-184.
[30] GROSS JB. Estimating allowable blood loss: corrected for dilution. Anesthesiology. 1983; 58:277-280.
[31] NADLER SB, HIDALGO JH, BLOCH T. Prediction of blood volume in normal human adults. Surgery. 1962; 51:224-232.
[32] 胡舒,古明晖,蔡立泉,等.氨甲环酸联合铁剂和重组人促红细胞生成素在全髋关节置换术早期康复中的作用研究[J].中华骨与关节外科杂志, 2018,11(3):176-181.
[33] 刘韬,杨建惠,吴敏艳.膝关节单髁置换术与全膝关节置换术治疗单间室膝骨关节炎近中期疗效[J].山西医药杂志,2019,48(14): 1703-1704.
[34] MASARACCHIO M, HANNEY W J, LIU X, et al. Timing of rehabilitation on length of stay and cost in patients with hip or knee joint arthroplasty: A systematic review with meta-analysis. PloS One. 2017; 12: e178295.
[35] SIMAN H, KAMATH AF, CARRILLO N, et al. Unicompartmental knee arthroplasty vs total knee arthroplasty for medial compartment arthritis in patients older than 75 years: comparable reoperation, revision, and complication rates. J Arthroplasty. 2017; 32:1792-1797.
[36] VAN DER LIST JP, SHENG DL, KLEEBLAD LJ, et al. Outcomes of cementless unicompartmental and total knee arthroplasty: A systematic review. Knee. 2017;24:497-507.
[37] 杨玉宝,李海涛,高忠礼,等.氨甲环酸的关节腔灌注对膝关节置换术的影响[J].中华实验外科杂志,2017,34(2):348.
[38] XIE J, ZHANG S, CHEN G, et al. Optimal route for administering tranexamic acid in primary unilateral total hip arthroplasty: Results from a multicenter cohort study. Br J Clin Pharmacol. 2019; 85: 2089-2097.
[39] HUANG ZY, HUANG Q, ZENG HJ, et al. Tranexamic acid may benefit patients undergoing total hip/knee arthroplasty because of haemophilia. BMC Musculoskelet Disord. 2019; 20:402.
[40] LEI Y, XIE J, HUANG Q, et al. The antifibrinolytic and anti-inflammatory effects of a high initial-dose tranexamic acid in total knee arthroplasty: a randomized controlled trial. Int Orthop. 2019.
[41] CHAMBERS S, TIDWELL L, KERKHOF A, et al. Topical tranexamic acid is effective in cementless total knee arthroplasty. Orthop Clin North Am. 2020: 51.
[42] SUKEIK M, ALSHRYDA S, POWELL J, et al. The effect of tranexamic acid on wound complications in primary total Hip Arthroplasty: A meta-analysis. Surgeon. 2020;18(1):53-61.
[43] WANG H, WANG L, LUO Z, et al. Intravenous and subsequent long-term oral tranexamic acid in enhanced-recovery primary total knee arthroplasty without the application of a tourniquet: a randomized placebo-controlled trial. BMC Musculoskelet Disord. 2019;20:478.
[44] HAN X, GONG G, HAN N, et al. Efficacy and safety of oral compared with intravenous tranexamic acid in reducing blood loss after primary total knee and hip arthroplasty: a meta-analysis. BMC Musculoskelet Disord. 2018;19:430.
[45] FILLINGHAM YA, RAMKUMAR DB, JEVSEVAR DS, et al. The safety of tranexamic acid in total joint arthroplasty: a direct meta-analysis. J Arthroplasty. 2018: 33.
[46] PONGCHAROEN B, RUETIWARANGKOON C. Does tranexamic acid reduce blood loss and transfusion rates in unicompartmental knee arthroplasty? J Orthop Sci. 2016; 21: 211-215.
[47] CLAVÉ A, GAUTHIER E, NAGRA NS, et al. Single-stage bilateral medial Oxford Unicompartmental Knee Arthroplasty: A case-control study of perioperative blood loss, complications and functional results. Orthop Traumatol Surg Res. 2018; 104: 943-947.
[48] LEURCHARUSMEE P, SAWADDIRUK P, PUNJASAWADWONG Y, et al. The possible pathophysiological outcomes and mechanisms of tourniquet-induced ischemia-reperfusion injury during total knee arthroplasty. Oxid Med Cell Longev. 2018; 2018:8087598.
[49] ARTHUR JR, SPANGEHL MJ. Tourniquet use in total knee arthroplasty. J Knee Surg. 2019; 32: 719-729.
[50] 崔丹荔,雷一霆,许宏,等.人工全髋关节置换术中首次大剂量联合术后五次静脉应用氨甲环酸的前瞻性临床研究[J].中国修复重建外科杂志,2019,33(8):935-939.
[51] 和佳,张志红,董智,等.氨甲环酸给药途径对初次单侧全膝关节置换术后出血量影响[J].临床军医杂志,2019,47(7):763-764.
[52] MUFARRIH SH, MALIK AT, QURESHI NQ, et al. The effect of tranexamic acid in unilateral and bilateral total knee arthroplasty in the South Asian population: A retrospective cohort study. Int J Surg. 2018; 52:25-29. |
| [1] | Fang Xingyan, Tian Zhenli, Zhao Zheyi, Wen Ping, Xie Tingting. Effects of sodium arsenite on human umbilical vein endothelial cell injury and sphingosine kinases 1/sphingosine 1-phosphate signaling axis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(在线): 1-7. |
| [2] | Zhong Yizheng, Huang Peizhen, Cai Qunbin, Zheng Liqin, He Xingpeng, Dong Hang. Microstructural indexes that determine the trabecular bone maximum stress of micro-finite element models [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1313-1318. |
| [3] | Li Xiaomin, Tian Xiangdong, Tan Yetong, Zhu Guangyu, Wang Rongtian, Wang Jian, Xue Zhipeng, Ma Sheng, Hu Yuanyi, Huang Ye, Ding Tiansong. Changes of lower limb force line and knee function after high tibial osteotomy in osteoporotic medial ventricular knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1325-1329. |
| [4] | Wu Tianliang, Tao Xiuxia, Xu Hongguang. Influence of different bone mineral densities on cage subsidence after stand-alone oblique lateral interbody fusion: three-dimensional finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1352-1358. |
| [5] | Wen Xinghua, Ding Huanwen, Cheng Kai, Yan Xiaonan, Peng Yuanhao, Wang Yuning, Liu Kang, Zhang Huiwu. Three-dimensional finite element model analysis of intramedullary nailing fixation design for large femoral defects in Beagle dogs [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1371-1376. |
| [6] | Zhang Lichuang, Gao Huali, Wang Jingchao, Lin Huijun, Wu Chonggui, Ma Yinghui, Huang Yunfei, Fang Xue, Zhai Weitao. Effect of tendon manipulation with equal emphasis on muscles and bones on accelerating the functional rehabilitation of quadriceps femoris after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1383-1389. |
| [7] | Zheng Hongrui, Zhang Wenjie, Wang Yunhua, He Bin, Shen Yajun, Fan Lei. Femoral neck system combined with platelet-rich plasma in the treatment of femoral neck fracture [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1390-1395. |
| [8] | Du Xueting, Zhang Xiaodong, Chen Yanjun, Wang Mei, Chen Wubiao, Huang Wenhua. Application of compressed sensing technology in two-dimensional magnetic resonance imaging of the ankle joint [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1396-1402. |
| [9] | He Yinhao, Li Xiaosheng, Chen Hongwen, Chen Tiezhu. 3D printed porous tantalum metal in the treatment of developmental dysplasia of the hip: current status and application prospect [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1455-1461. |
| [10] | Dang Yi, Du Chengyan, Yao Honglin, Yuan Nenghua, Cao Jin, Xiong Shan, Zhang Dingmei, Wang Xin. Hormonal osteonecrosis and oxidative stress [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1469-1476. |
| [11] | Sun Jiajia, Zhu Haidi, Lu Yun, Zhang Kai. Comparison of bone metabolism markers between type 2 diabetes mellitus and non-type 2 diabetes mellitus patients with hip fracture [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1156-1160. |
| [12] | Huang Linke, Wei Linhua, Jiang Jie, Liu Qian, Chen Weiwei. Effects of estrogen combined with treadmill exercise on bone mass and articular cartilage in ovariectomized mice [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1166-1171. |
| [13] | Bi Gengchao, Zhang Yanlong, Li Qiuyue, Hu Longwei, Zhang Yu. Knee joint mechanics and activation characteristics of surrounding muscles during deep jumps at different heights and distances [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1211-1218. |
| [14] | Yang Zhishan, Tang Zhenglong. YAP/TAZ, a core factor of the Hippo signaling pathway, is involved in bone formation [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1264-1271. |
| [15] | Bai Yulong, Li Zhonghai, Zhao Yantao, Xia Cencan, Shi Lei. History, current situation and prospect of tissue banks in China [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1306-1312. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||