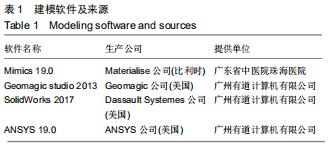
Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (30): 4775-4781.doi: 10.3969/j.issn.2095-4344.2841
Previous Articles Next Articles
Three-dimensional finite element analysis of the influence of bone cement dispersion type on the stress of adjacent vertebrae after vertebroplasty
Chen Rongbin1, Bai Jie2, Li Yong1, Zhang Jinxin1, Lu Yao1, Wu Zhaodian1
- 1Third Department of Orthopedics, Zhuhai Branch of Guangdong Province Hospital of Traditional Chinese Medicine, Zhuhai 519015, Guangdong Province, China; 2Second Clinical Medical College of Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China
-
Received:2019-12-12Revised:2019-12-19Accepted:2019-02-14Online:2020-10-28Published:2020-09-18 -
Contact:Chen Rongbin, Master, Physician, Third Department of Orthopedics, Zhuhai Branch of Guangdong Province Hospital of Traditional Chinese Medicine, Zhuhai 519015, Guangdong Province, China -
About author:Chen Rongbin, Master, Physician, Third Department of Orthopedics, Zhuhai Branch of Guangdong Province Hospital of Traditional Chinese Medicine, Zhuhai 519015, Guangdong Province, China -
Supported by:the Guangdong Medical Science and Technology Research Fund, No. 2017117222739562; a grant from Guangdong Administration of traditional Chinese Medicine, No. 20180322101734
CLC Number:
Cite this article
Chen Rongbin, Bai Jie, Li Yong, Zhang Jinxin, Lu Yao, Wu Zhaodian. Three-dimensional finite element analysis of the influence of bone cement dispersion type on the stress of adjacent vertebrae after vertebroplasty[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(30): 4775-4781.
share this article
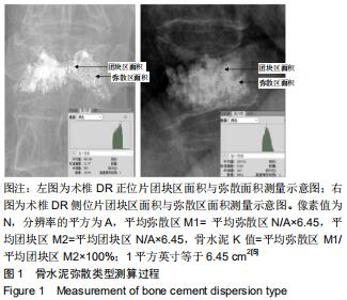
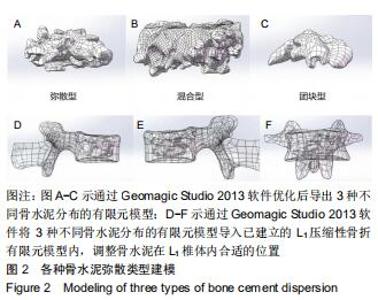
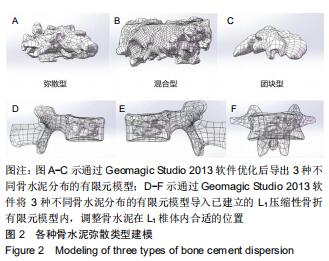
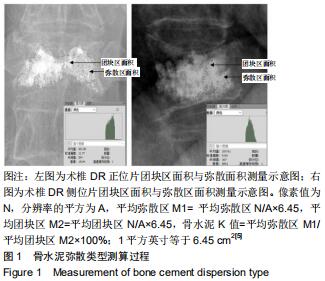
1.5.2 三种骨水泥弥散类型有限元模型的建立 依据经皮椎体成形术后复查的正侧位DR资料,在PACS影像工作站系统导出图像,利用PhotoshopCS5图形处理软件,对图像进行对比度及亮度等调整图像锐利度,区分高密度区和低密度区,选出连续的均匀高密度区为骨水泥团块区域及光点弥散的不均匀密度区为骨水泥弥散区域,通过查看对应选区的直方图查找像素值,对骨水泥均匀分布及不均匀分布区域重复测量3次后取平均像素值,记像素值为N,分辨率的平方为A,平均弥散区域面积为M1,平均团块区域面积为M2,参考文献[13]利用像素值与分辨率的换算,即1平方英寸等于6.45 cm2,计算平均弥散区域面积和平均团块区域面积(平均弥散区M1=平均弥散区N/A×6.45,平均团块区M2=平均团块区N/A×6.45)。计算骨水泥平均弥散区与平均团块区面积的比值(K)[14],定义K值<50%为团块型,50%≤K值≤100%为混合型,K值>100%为弥散型,测算方法见图1。 "

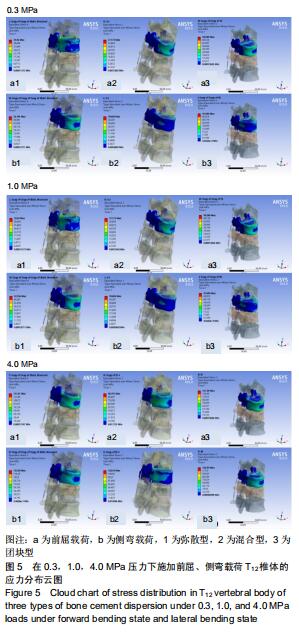
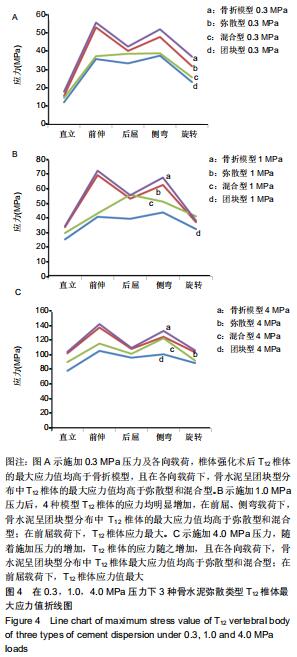
2.2 各级压力和不同载荷方向下T12椎体的最大应力值比较与分布情况 在各级压力和各向载荷下,椎体强化术后T12椎体的最大Von mises应力值均较骨折模型增加,且其最大应力的增加与轴向压力的逐步递增施加呈正相关。在施加0.3,1.0,4.0 MPa轴向压力下,术椎骨水泥呈团块型分布T12椎体所受的载荷均明显高于混合型及弥散型,骨水泥呈混合型分布在各级压力及各向载荷下T12椎体承受的最大应力最低。在3级压力下,T12椎体承受最大应力均出现在前屈及侧弯运动中,其中3种骨水泥弥散类型在施加前屈载荷T12椎体的最大应力值,0.3 MPa压力下分别为:弥散型52.764 MPa,团块型55.269 MPa,混合型 37.173 MPa;1.0 MPa压力下分别为:弥散型68.735 MPa,团块型71.597 MPa,混合型42.852 MPa;4.0 MPa压力分别为:弥散型137.21 MPa,团块型141.59 MPa,混合型115.35 MPa,见图4。3种骨水泥弥散类型在各级压力及载荷下T12椎体的最大应力值之间比较,差异无显著性意义(P > 0.05)。 "

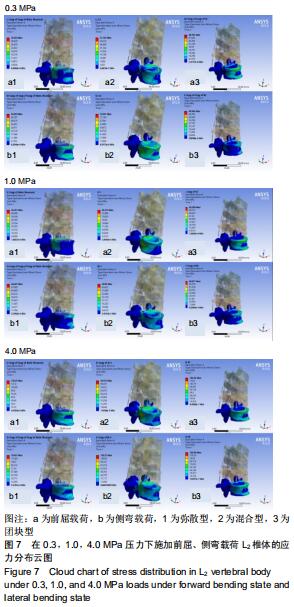
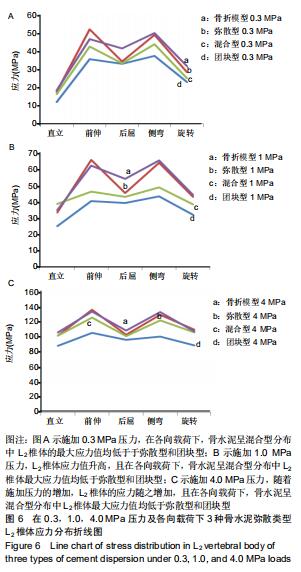
2.3 在3级压力和不同载荷方向下L2椎体的最大应力值比较与分布情况 逐步施加0.3,1.0,4.0 MPa压力,3种骨水泥弥散类型L2椎体承受最大应力呈线性增加,在各向载荷下,骨水泥呈混合型分布时L2椎体的最大应力值均低于弥散型和团块型,且在前屈及侧弯载荷下,L2椎体应力值均明显高于其他载荷方向,最大应力值均出现在前屈运动中,其中0.3 MPa压力下分别为:弥散型52.039 MPa,团块型46.781 MPa,混合型42.541 MPa;1.0 MPa压力下分别为:弥散型65.71 MPa,团块型62.29 MPa,混合型46.32 MPa;4.0 MPa压力分别为:弥散型136.35 MPa,团块型133.43 MPa,混合型125.81 MPa,见图6。3种骨水泥弥散类型在各级压力及载荷下L2椎体最大应力值之间比较,差异无显著性意义(P > 0.05)。 "
|
[1] STEVENSON M, GOMERSALLT, LLOYD JONES M, et al. Percutaneous vertebroplasty and percutaneous balloon kyphoplasty for the treatment of osteoporotic vertebral fractures: A systematic review and cost-effectiveness analysis. Health Technol Assess. 2014;18(17):1-290.
[2] TSOUMAKIDOU G, TOO CW, KOCH G, et al. CIRSE guidelines on percutaneous vertebral augmentation. Cardiovasc Intervent Radiol.2017;40(3): 331-342.
[3] SEO DH, OH SH, YOON KW, et al. Risk factors of new adjacent compression fracture after percutaneous vertebroplasty: effectiveness of bisphosphonate in osteoporotic or osteopenic elderly patients. Korean J Neurotrauma. 2014;10(2):86-91.
[4] ZHAI W, JIA Y, WANG J, et al. The clinical effect of percutaneous kyphoplasty for the treatment of multiple osteoporotic vertebral compression fractures and the prevention of new vertebral fractures. Int J Clin Exp Med. 2015;8(8):13473-13481.
[5] SUN YC, TENG MM, YUAN WS, et al. Risk of post-vertebroplasty fracture in adjacent vertebral bodies appears correlated with the morphologic extent of bone cement. J Chin Med Assoc. 2011; 74(8):357-362.
[6] YI X, LU H, TIAN F, et al. Recompression in new levels after percutaneous vertebroplasty and kyphoplasty compared with conservative treatment. Arch Orthop Trauma Surg. 2014;134(1): 21-30.
[7] HE X, LI H, MENG Y, et al. Percutaneousky- phoplasty evaluated by cement volume and distribution:an analysis of clinical data. Pain Physician. 2016;19(7):495- 506.
[8] CHO AR,CHO SB,LEE JH. Effect of augmentation material stiffness on adjacent vertebrae after osteoporotic vertebroplasty using finite element analysis with different loading methods. Pain Physician. 2015;18:E1101-1110.
[9] SCHULTE TL, KEILER A, RIECHELMANN F, et al. Biomechanical comparison of vertebral augmentation with silicone and PMMA cement and two filling grades. Eur Spine J. 2013;22(12): 2695-2701.
[10] LIEBSCHNER MAK, ROSENBERG WS, KEAVENY TM. Effects of bone cement volume and distribution on vertebral stiffness af- ter vertebroplasty. Spine. 2001;26(14): 1547-1554.
[11] 李飞虎,谢恩,郝定均,等.PVP术后相邻节段椎体应力分布的有限元分析[J].中国骨与关节损伤杂志,2017,32(11):1135-1137.
[12] LIANG D, YE LQ, JIANG XB, et al. Biomechanical effects of cement distribution in the fractured area on osteoporotic vertebral compression fractures: a three-dimensional finite element analysis. J Surg Res. 2015; 195(1):246-256. [13] 谢亮.Photoshop像素法在计算地图面积中的应用[J].电脑知识与技术,2010,6(15):4021-4022.
[14] 赵永生,李强,历强,等.骨水泥弥散类型对治疗骨质疏松性椎体压缩骨折的影响[J].中国骨伤,2017,30(5):446-452.
[15] 陈伟健,谢炜星等.胸腰段骨质疏松性椎体压缩性骨折有限元模型的建立[J].山东医药,2018,58(32):55-58.
[16] 费琦,李秋军,李东,等.椎体后凸成形术后骨水泥椎间盘渗漏对邻近节段力学影响的有限元分析[J].中华医学杂志, 2011,91(1):51-55.
[17] 徐建彪,张伟学,王鸿晨,等.骨水泥注入量对经皮椎体后凸成形术后相邻椎体应力影响的有限元分析[J].脊柱外科杂志,2017,15(3): 177-181.
[18] 刘仕友,路青林,郑伟,等.椎体后凸成形椎间盘骨水泥渗漏时行相邻椎体预防性强化的有限元分析[J].中国组织工程研究,2012,16(22): 4001-4005.
[19] BLIEMEL C, OBERKIRCHER L, BUECKING B, et al. Higher incidence of new vertebral fractures following percutaneous vertebroplasty and kyphoplasty—fact or fiction? Acta Orthop Belg. 2012;78(2):220-229.
[20] BERLEMANN U, FERGUSON SJ, NOLTE LP, et al. Adjacent vertebral failure after vertebroplasty. A biomechanical investigation. J Bone Joint Surg Br. 2002;84(5): 748-752.
[21] BAROUD G, BOHNER M. Biomechanicalimpactof vertebroplasty. Postoperative biomechanics of vertebroplasty. Joint Bon Spine. 2006;73(2):144-150.
[22] HUANG TJ, KOU YH, YIN XF, et al. Clinical characteristics and risk factors of newly developed vertebral fractures after vertebral augmentation. Beijing Da Xue Xue Bao. 2015;47(2): 237-241.
[23] QIN DA, SONG JF, WEI J, et al. Analysis of the reason of secondary fracture after percutaneous vertebroplasty for osteo- porotic vertebral compression fractures. Zhongguo Gu Shang. 2014;27(9): 730-733.
[24] NAGARAJA S, AWADA HK, DREHER ML, et al. Effects of verte- broplasty on endplate subsidence in elderly female spines. J Neurosurg Spine. 2015;22(3): 273-282.
[25] BREKELMANS WA, POORT HW, SLOOFF TJ. A new method to analyze the mechanical behaviour of skeletal parts. Acta Ortho Scand. 1972;43: 301.
[26] 王吉博.有限元法评估经皮椎体成形和后凸成形治疗脊柱三明治骨折的生物力学变化[J].中国组织工程研究,2017,21(35):5703-5708.
[27] SHAMAMI DZ, KARIMI A, BEIGZADEH B, et al. A 3D finite element study for stress analysis in bone tissue around single implants with different materials and various bone qualities. J Biom Tissue Eng. 2014;4(8):632-637.
[28] 林娟颖,刘晓颖,邢立杰,等.基于有限元法的跟骨生物力学分析[J].医用生物力学,2018,33(1):37-41.
[29] 周伟,刘贵省,周丽萍,等.不同方式灌注骨水泥治疗骨质疏松性椎体压缩骨折的比较[J].中国组织工程研究,2017,21(14):2147-2152.
[30] 方驰华,周五一,黄立伟,等.虚拟中国人女性一号肝脏图像三维重建和虚拟手术的切割[J].中华外科杂志,2005,43(11):748-752.
[31] 刘文军,钟世镇.虚拟中国人女性一号松质骨图像数据的配准与三维重建[J].中国临床解剖学杂志,2004,22(4):380-383.
[32] 张建国,芦俊鹏,阮世捷,等.以头部为例的人体有限元几何重建的方法初步探讨[J].微机计算机信息(管控一体化), 2006,22(22):249-252.
[33] 李家琼,王冬梅,孙璟川,等.骨水泥对椎体成形术治疗胸腰椎骨质疏松压缩性骨折的生物力学影响[J].医用生物力学,2018,33(1):6-12.
[34] BERLEMANN U, FERGUSON SJ, NOLTE LP, et al. Adjacent vertebral failure after vertebroplasty. A biomechanical investigation. J Bone Joint Surg(Br). 2002;84(5):748-752.
[35] 韦竑宇,谭明生,梁立.单侧多穿刺通道注射骨水泥法在骨质疏松椎体压缩骨折经皮椎体成形术中的应用[J].中国骨伤,2013,26(12):1010-1014.
[36] 吴钊钿,陈荣彬,李勇,等.骨水泥弥散类型与椎体成形术后再发术椎塌陷的相关性分析[J].中国医药导报,2018,15(27):6.
[37] 何奇龙,陈荣彬,李勇.骨水泥的弥散情况对经皮椎体成形的疗效影响[J].中国中医骨伤科杂志,2018,26(6):51-55. [38] LIEBSCHNER MA, ROSENBERG WS, KEAVENY TM. Effects of bone ce- ment volume and distribution on vertebral stiffness after vertebro-plasty. Spine(Phila Pa 1976). 2001;26(14):1547-1554. |
| [1] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [2] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [3] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [4] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [5] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| [6] | Zhang Chao, Lü Xin. Heterotopic ossification after acetabular fracture fixation: risk factors, prevention and treatment progress [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1434-1439. |
| [7] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Multiple problems in the selection of implants for patellar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1440-1445. |
| [8] | Wang Debin, Bi Zhenggang. Related problems in anatomy mechanics, injury characteristics, fixed repair and three-dimensional technology application for olecranon fracture-dislocations [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1446-1451. |
| [9] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [10] | Tang Hui, Yao Zhihao, Luo Daowen, Peng Shuanglin, Yang Shuanglin, Wang Lang, Xiao Jingang. High fat and high sugar diet combined with streptozotocin to establish a rat model of type 2 diabetic osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1207-1211. |
| [11] | Li Zhongfeng, Chen Minghai, Fan Yinuo, Wei Qiushi, He Wei, Chen Zhenqiu. Mechanism of Yougui Yin for steroid-induced femoral head necrosis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1256-1263. |
| [12] | Pei Lili, Sun Guicai, Wang Di. Salvianolic acid B inhibits oxidative damage of bone marrow mesenchymal stem cells and promotes differentiation into cardiomyocytes [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1032-1036. |
| [13] | Yuan Jun, Yang Jiafu. Hemostatic effect of topical tranexamic acid infiltration in cementless total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 873-877. |
| [14] | Hou Guangyuan, Zhang Jixue, Zhang Zhijun, Meng Xianghui, Duan Wen, Gao Weilu. Bone cement pedicle screw fixation and fusion in the treatment of degenerative spinal disease with osteoporosis: one-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 878-883. |
| [15] | He Li, Tian Wei, Xu Song, Zhao Xiaoyu, Miao Jun, Jia Jian. Factors influencing the efficacy of lumbopelvic internal fixation in the treatment of traumatic spinopelvic dissociation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 884-889. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||