Chinese Journal of Tissue Engineering Research ›› 2017, Vol. 21 ›› Issue (26): 4234-4239.doi: 10.3969/j.issn.2095-4344.2017.26.023
Previous Articles Next Articles
A comparison between over-the-toe plaster slab and off-loading forefoot shoes following hallux valgus correction
- Huashan Hospital of Fudan University, Shanghai 200040, China
-
Received:2017-04-03Online:2017-09-18Published:2017-09-28 -
Contact:Huang Jia-zhang, M.D., Associate professor, Department of Orthopedics, Huashan Hospital of Fudan University, Shanghai 200040, China -
About author:Geng Xiang, M.D., Physician, Department of Orthopedics, Huashan Hospital of Fudan University, Shanghai 200040, China -
Supported by:the Scientific Research Fund of Shanghai Science and Technology Committee, No. 14411969900
CLC Number:
Cite this article
Geng Xiang, Huang Jia-zhang, Ma Xin, Wang Xu, Zhang Chao, Chen Li, Wang Chen.
share this article
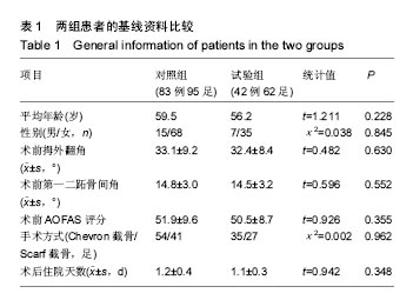
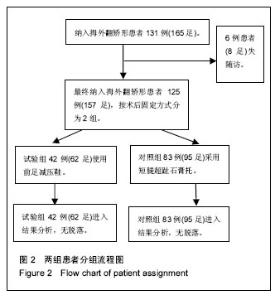
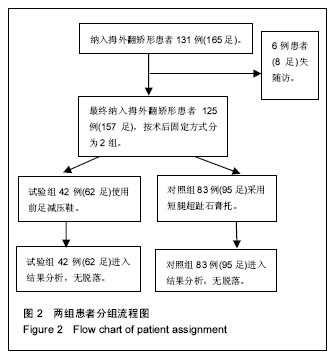
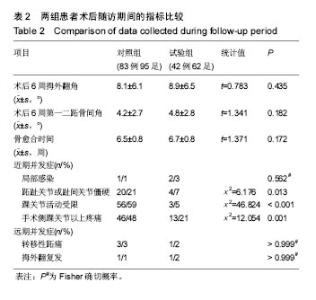
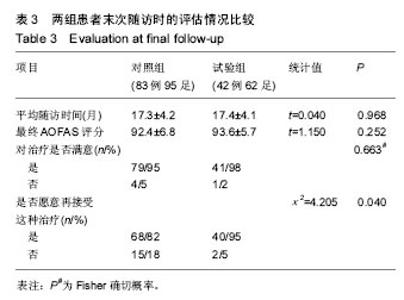
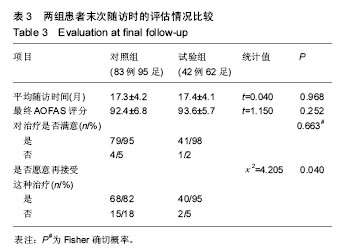
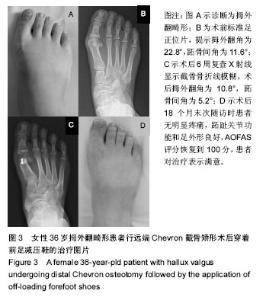
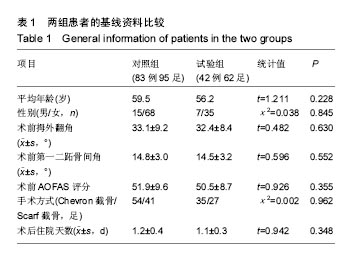
2.2 基线资料比较 2组患者的年龄、性别构成、术前拇外翻角、第一二跖骨间角及AOFAS评分、手术方式构成、术后住院天数的差异均无显著性意义(P > 0.05),见表1。2.3 随访结果 在术后6周时,2组患者矫正后的拇外翻角、第一二跖骨间角以及骨愈合时间差异并无显著性意义(见表2)。进一步经过12-30个月的随访,2组患者最终的AOFAS评分差异亦无显著性意义(见表3)。 在评价整个治疗方式和效果时,穿着前足减压患者的满意率(98%)高于使用超趾石膏托的患者(95%),但差异无显著性意义;而当被问到“如果遇到相同情况是否愿意再次接受这种治疗”的时候,使用石膏托固定的患者仅有82%表示愿意,而这一比例在穿着减压鞋的患者中高达95%,此差异有显著性意义(见表3)。 2.4 不良事件 围手术期对照组、试验组患者分别有1足和2足出现伤口周围红肿,但均为浅表感染,口服抗生素后均顺利愈合;对照组患者去除超趾石膏托后有20足(21%)出现第一跖趾关节僵硬(定义为屈伸活动<30°[25])或趾间关节僵硬(定义为屈伸活动<10°[21]),56足(59%)出现踝关节活动受限(屈伸活动<30°[21]),石膏托固定期间有46足(48%)在手术侧踝关节以上出现疼痛;而相比之下,试验组患者在去除减压鞋后,发生上述不适者分别为4足(7%)、3足(5%)和13足(21%),且此3例踝关节活动受限患者的踝关节X射线均有关节炎征象;通过χ2检验,证实穿着前足减压鞋发生跖趾关节或趾间关节僵硬、踝关节活动受限、手术侧踝关节以上关节或肢体疼痛的概率比使用短腿超趾石膏托固定低,差异有显著性意义(见表2)。 出现远期并发症包括转移性跖痛和拇外翻复发(拇外翻角>20°[26]),其发生率在2组间差异无显著性意义(见表2);所有患者均未出现骨延迟愈合或不愈合、拇内翻以及内固定松动等并发症。 "
| [1]Lee KT, Park YU, Jegal H, et al. Deceptions in hallux valgus: what to look for to limit failures. Foot Ankle Clin. 2014;19(3): 361-370.[2]Carl HD, Pfander D, Swoboda B. Assessment of plantar pressure in forefoot relief shoes of different designs. Foot Ankle Int. 2006;27(2):117-120.[3]Hawson ST. Physical therapy post-hallux abducto valgus correction. Clin Podiatr Med Surg. 2014;31(2):309-322.[4]Chao J. Deep Vein Thrombosis in Foot and Ankle Surgery. Orthop Clin North Am. 2016;47(2):471-475.[5]Hook S, Walker N, Cannon L. The use of post-operative reverse camber shoes following scarf osteotomy. Foot Ankle Surg. 2008;14(4):190-193.[6]Forster MC, Dhar S. A comparison between forefoot plaster and wooden soled shoes following Mitchell's osteotomy for hallux valgus. Ann R Coll Surg Engl. 2002;84(1):43-46.[7]Schuh R, Trnka HJ, Sabo A, et al. Biomechanics of postoperative shoes: plantar pressure distribution, wearing characteristics and design criteria: a preliminary study. Arch Orthop Trauma Surg. 2011;131(2):197-203.[8]Notni A, Fuhrmann RA. [Measuring plantar weight distribution of shoes with forefoot support]. Z Orthop Ihre Grenzgeb. 1999; 137(3):280-283.[9]Pirozzi K, Mcguire J, Meyr AJ. Effect of variable body mass on plantar foot pressure and off-loading device efficacy. J Foot Ankle Surg. 2014;53(5):588-597.[10]Ferrari J. Bunions. Clin Evid (Online). 2009; 11:1112.[11]Fakoor M, Sarafan N, Mohammadhoseini P, et al. Comparison of Clinical Outcomes of Scarf and Chevron Osteotomies and the McBride Procedure in the Treatment of Hallux Valgus Deformity. Arch Bone Jt Surg. 2014;2(1):31-36.[12]Uygur E, Ozkan NK, Akan K, et al. A comparison of Chevron and Lindgren-Turan osteotomy techniques in hallux valgus surgery: a prospective randomized controlled study. Acta Orthop Traumatol Turc. 2016;50(3):255-261.[13]Singh D, Biz C, Corradin M, et al. Comparison of dorsal and dorsomedial displacement in evaluation of first ray hypermobility in feet with and without hallux valgus. Foot Ankle Surg. 2016;22(2):120-124.[14]Poggio D, Melo R, Botello J, et al. Comparison of postoperative costs of two surgical techniques for hallux valgus (Kramer vs. scarf). Foot Ankle Surg. 2015;21(1):37-41.[15]Coughlin MJ, Saltzman CL, Anderson RB. Mann's surgery of the foot and ankle. 9th ed. Philadelphia:Saunders Elsevier. 2014: 210-211.[16]Glod DJ, Fettinger P, Gibbons RW. A comparison of weightbearing pressures in various postoperative devices. J Foot Ankle Surg.1996;35(2):149-154,190.[17]Hecht PJ, Lin TJ. Hallux valgus. Med Clin North Am. 2014; 98(2):227-232.[18]Meng HZ, Zhang WL, Li XC, et al. Radiographic angles in hallux valgus: Comparison between protractor and iPhone measurements. J Orthop Res. 2015;33(8):1250-1254.[19]Chhaya SA, Brawner M, Hobbs P, et al. Understanding hallux valgus deformity: what the surgeon wants to know from the conventional radiograph.Curr Probl Diagn Radiol. 2008;37(3): 127-137.[20]Srivastava S, Chockalingam N, El Fakhri T. Radiographic measurements of hallux angles: a review of current techniques. Foot (Edinb). 2010;20(1):27-31.[21]Kitaoka HB, Alexander IJ, Adelaar RS, et al. Clinical rating systems for the ankle-hindfoot, midfoot, hallux, and lesser toes. Foot Ankle Int. 1994;15(7):349-353.[22]Crespo RE, Arcas OA, Penuela CR, et al. Percutaneous Hallux Valgus Surgery Without Distal Metatarsal Articular Angle Correction. Foot Ankle Spec. 2017. [Epub ahead of print].[23]Karpe P, Killen MC, Pollock RD, et al. Shortening Scarf osteotomy for correction of severe hallux valgus. Does shortening affect the outcome? Foot (Edinb). 2016;29:45-49.[24]Raikin SM, Miller AG, Daniel J. Recurrence of hallux valgus: a review. Foot Ankle Clin. 2014;19(2):259-274.[25]Park HW, Lee KB, Chung JY, et al. Comparison of outcomes between proximal and distal chevron osteotomy, both with supplementary lateral soft-tissue release, for severe hallux valgus deformity: A prospective randomised controlled trial. Bone Joint J. 2013;95-B(4):510-516.[26]Park CH, Ahn JY, Kim YM, et al. Plate fixation for proximal chevron osteotomy has greater risk for hallux valgus recurrence than Kirschner wire fixation. Int Orthop. 2013; 37(6):1085-1092.[27]Dare W, Ebeye O, Nsi C. The prevalence of hallux valgus among three ethnic groups in Delta State, Southern Nigeria. Am-Euras J Sci Res. 2015;10(2):118-120.[28]Loh B, Chen JY, Yew AK, et al. Prevalence of Metatarsus Adductus in Symptomatic Hallux Valgus and Its Influence on Functional Outcome. Foot Ankle Int. 2015;36(11):1316-1321.[29]Harb Z, Kokkinakis M, Ismail H, et al. Adolescent hallux valgus: a systematic review of outcomes following surgery. J Child Orthop. 2015;9(2):105-112.[30]Aiyer AA, Shariff R, Ying L, et al. Prevalence of metatarsus adductus in patients undergoing hallux valgus surgery. Foot Ankle Int. 2014;35(12):1292-1297.[31]Palomo-Lopez P, Becerro-De-Bengoa-Vallejo R, Losa-Iglesias ME, et al. Impact of Hallux Valgus related of quality of life in Women. Int Wound J.2016.[32]Menz HB, Roddy E, Thomas E, et al. Impact of hallux valgus severity on general and foot-specific health-related quality of life. Arthritis Care Res (Hoboken). 2011;63(3):396-404.[33]Vander GR. Correction of Hallux Valgus Interphalangeus With an Osteotomy of the Distal End of the Proximal Phalanx (Distal Akin Osteotomy). Foot Ankle Int. 2017;38(2):153-158.[34]Nunez-Samper M, Viladot R, Ponce SJ, et al. Serious sequellae of the hallux valgus surgery: More options for its surgical treatment. Rev Esp Cir Ortop Traumatol. 2016;60(4): 234-242.[35]Coughlin MJ, Thompson FM. The high price of high-fashion footwear. Instr Course Lect. 1995;44:371-377.[36]Foot and Ankle Working Committee; Chinese Association of Orthopaedic Surgeons Orthopaedic Branch; Chinese Association of Orthopaedic Surgeons. Consensus on Surgical Management of Hallux Valgus from China. Orthop Surg. 2015; 7(4):291-296. |
| [1] | Yao Xiaoling, Peng Jiancheng, Xu Yuerong, Yang Zhidong, Zhang Shuncong. Variable-angle zero-notch anterior interbody fusion system in the treatment of cervical spondylotic myelopathy: 30-month follow-up [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1377-1382. |
| [2] | An Weizheng, He Xiao, Ren Shuai, Liu Jianyu. Potential of muscle-derived stem cells in peripheral nerve regeneration [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1130-1136. |
| [3] | Zhang Jinglin, Leng Min, Zhu Boheng, Wang Hong. Mechanism and application of stem cell-derived exosomes in promoting diabetic wound healing [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1113-1118. |
| [4] | Li Guijun, Fang Xiaohui, Kong Weifeng, Yuan Xiaoqing, Jin Rongzhong, Yang Jun. Finite element analysis of the treatment of hallux valgus deformity by microplate combined with super strong suture elastic fixation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 938-942. |
| [5] | Gao Yi, Ma Yue, Zhao Zeyu. Foot bone self-regulation under weight-bearing standing analyzed by medical imaging measurement [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 959-962. |
| [6] | He Yunying, Li Lingjie, Zhang Shuqi, Li Yuzhou, Yang Sheng, Ji Ping. Method of constructing cell spheroids based on agarose and polyacrylic molds [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 553-559. |
| [7] | He Guanyu, Xu Baoshan, Du Lilong, Zhang Tongxing, Huo Zhenxin, Shen Li. Biomimetic orientated microchannel annulus fibrosus scaffold constructed by silk fibroin [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 560-566. |
| [8] | Chen Xiaoxu, Luo Yaxin, Bi Haoran, Yang Kun. Preparation and application of acellular scaffold in tissue engineering and regenerative medicine [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 591-596. |
| [9] | Kang Kunlong, Wang Xintao. Research hotspot of biological scaffold materials promoting osteogenic differentiation of bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 597-603. |
| [10] | Shen Jiahua, Fu Yong. Application of graphene-based nanomaterials in stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 604-609. |
| [11] | Zhang Tong, Cai Jinchi, Yuan Zhifa, Zhao Haiyan, Han Xingwen, Wang Wenji. Hyaluronic acid-based composite hydrogel in cartilage injury caused by osteoarthritis: application and mechanism [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 617-625. |
| [12] | Li Hui, Chen Lianglong. Application and characteristics of bone graft materials in the treatment of spinal tuberculosis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 626-630. |
| [13] | Gao Cangjian, Yang Zhen, Liu Shuyun, Li Hao, Fu Liwei, Zhao Tianyuan, Chen Wei, Liao Zhiyao, Li Pinxue, Sui Xiang, Guo Quanyi. Electrospinning for rotator cuff repair [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 637-642. |
| [14] | Guan Jian, Jia Yanfei, Zhang Baoxin , Zhao Guozhong. Application of 4D bioprinting in tissue engineering [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(3): 446-455. |
| [15] | Liu Jiali, Suo Hairui, Yang Han, Wang Ling, Xu Mingen. Influence of lay-down angles on mechanical properties of three-dimensional printed polycaprolactone scaffolds [J]. Chinese Journal of Tissue Engineering Research, 2022, 10(16): 2612-2617. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||