Chinese Journal of Tissue Engineering Research ›› 2015, Vol. 19 ›› Issue (17): 2648-2654.doi: 10.3969/j.issn.2095-4344.2015.17.005
Previous Articles Next Articles
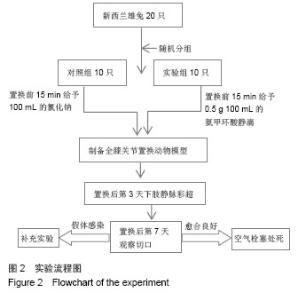
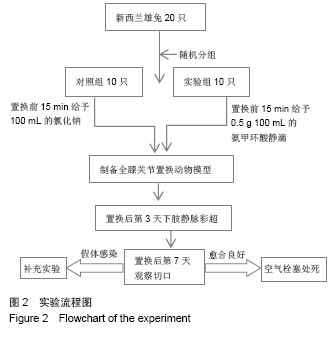
Effects of tranexamic acid on hidden blood loss after total knee arthroplasty in animal models
Yuan Lei, Bao Ni-rong, Zhao Jian-ning
- Clinical Department, Medical School, Nanjing University, Department of Orthopedics, Nanjing General Hospital of Nanjing Military Command of Chinese PLA, Nanjing 210002, Jiangsu Province, China
-
Online:2015-04-23Published:2015-04-23 -
Contact:Zhao Jian-ning, Chief physician, Professor, Doctoral supervisor, Clinical Department, Medical School, Nanjing University, Department of Orthopedics, Nanjing General Hospital of Nanjing Military Command of Chinese PLA, Nanjing 210002, Jiangsu Province, China -
About author:Yuan Lei, Studying for master’s degree, Clinical Department, Medical School, Nanjing University, Department of Orthopedics, Nanjing General Hospital of Nanjing Military Command of Chinese PLA, Nanjing 210002, Jiangsu Province, China -
Supported by:the Clinical Science and Technology Project of Jiangsu Province, No. BL2012002
CLC Number:
Cite this article
Yuan Lei, Bao Ni-rong, Zhao Jian-ning. Effects of tranexamic acid on hidden blood loss after total knee arthroplasty in animal models[J]. Chinese Journal of Tissue Engineering Research, 2015, 19(17): 2648-2654.
share this article
| [1]Fuqiang G, Wanshou G, Wei S, et al. Correlation between the coverage percentage of prosthesis and postoperative hidden blood loss in primary total knee arthroplasty. Chin Med J. 2014; 127(12): 2265-2269.
[2]Sehat KR, Evans RL, Newman JH. Hidden blood loss following hip and knee arthroplasty correct management of blood loss should take hidden loss into account. J Bone Joint Surg. 2004; 86(4):561-565.
[3]Shen H, Li Z, Feng M, et al. Analysis on hidden blood loss of total knee arthroplasty in treating knee osteoarthritis. Chin Medical J. 2011;124(11):1653.
[4]Benoni G, Lethagen S, Nilsson P, et al. Tranexamic acid, given at the end of the operation, does not reduce postoperative blood loss in hip arthroplasty. Acta Orthop. 2000;71(3):250-254.
[5]Cid J, Lozano M. Tranexamic acid reduces allogeneic red cell transfusions in patients undergoing total knee arthroplasty: results of a meta-analysis of randomized controlled trials. Transfusion. 2005;45(8):1302-1307.
[6]Wong J, Abrishami A, El Beheiry H, et al. Topical application of tranexamic acid reduces postoperative blood loss in total knee arthroplasty: a randomized, controlled trial. J Bone Joint Surg Am 2010;92(15):2503.
[7]Ishida K,Tsumura N,Kitagawa A, et al. Intra-articular injection of tranexamic acid reduces not only blood loss but also knee joint swelling after total knee arthroplasty. Int Orthop. 2011;35: 1639-1645.
[8]MacGillivray RG, Tarabichi SB, Hawari MF, et al. Tranexamic acid to reduce blood loss after bilateral total knee arthroplasty: a prospective, randomized double blind study. J Arthroplasty. 2011;26(1): 24-28.
[9]Karam JA, Bloomfield MR, DiIorio TM, et al. Evaluation of the efficacy and safety of tranexamic acid for reducing blood loss in bilateral total knee arthroplasty. J Arthroplasty. 2014;29(3): 501-503.
[10]Iwai T, Tsuji S, Tomita T, et al. Repeat-dose intravenous tranexamic acid further decreases blood loss in total knee arthroplasty. Int Orthop. 2013;37(3): 441-445.
[11]Gandhi R, Evans H M, Mahomed S R, et al. Tranexamic acid and the reduction of blood loss in total knee and hip arthroplasty: a meta-analysis. BMC Res Notes. 2013;6(1): 184.
[12]Gillette BP, DeSimone LJ, Trousdale RT, et al. Low risk of thromboembolic complications with tranexamic acid after primary total hip and knee arthroplasty. Clin Orthop Relat Res 2013;471(1):150.
[13]Aguilera X, Martinez-Zapata MJ, Bosch A. Efficacy and safety of fibrin glue and tranexamic Acid to prevent postoperative blood loss in total knee arthroplasty: a randomized controlled clinical trial. J Bone Joint Surg. 2013;95(22):2001-2007.
[14]Ma YQ, Zhang YC, Zhang H. [Local application of tranexamic acid reduces blood less in unilateral total knee arthroplasty: a retrospective comparason analysis]. Zhonghua Waike Zazhi. 2013;51(1):40-43.
[15]Vigna-Taglianti F, Basso L, Rolfo P, et al. Tranexamic acid for reducing blood transfusions in arthroplasty interventions: a cost-effective practice. Eur J Orthop Surg Traumatol. 2013: 1-7.
[16]Sarzaeem MM, Razi M, Kazemian G, et al. Comparing Efficacy of Three Methods of Tranexamic Acid Administration in Reducing Hemoglobin Drop Following Total Knee Arthroplasty. J Arthroplasty. 2014.
[17]Seo JG, Moon YW, Park SH, et al. The comparative efficacies of intra-articular and IV tranexamic acid for reducing blood loss during total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2013;21(8):1869.
[18]Ahlberg A, Eriksson O, Kjellman H. Diffusion of tranexamic acid to the joint. Acta Orthopaedica. 1976;47(5): 486-488.
[19]Nilsson IM. Clinical pharmacology of aminocaproic and tranexamic acids. J Clin Pathol. 1980;33(Suppl 14):41-47.
[20]Benoni G, Lethagen S, Nilsson P, et al. Tranexamic acid, given at the end of the operation, does not reduce postoperative blood loss in hip arthroplasty. Acta Orthop Scand. 2000;71:250-254.
[21]Good L, Peterson E, Lisander B. Tranexamic acid decreases external blood loss but not hidden blood loss in total knee replacement. Br J Anaesth. 2003;90(5):596.
[22]Lin PC, Hsu CH, Chen WS, et al. Does tranexamic acid save blood in minimally invasive total knee arthroplasty? Clin Orthop Relat Res. 2011;469(7):1995.
[23]余世明,刘建华,徐栋梁,等.兔用生物型人工膝关节假体的设计与制作[J].中华关节外科杂志(电子版), 2009,3(4):63-66.
[24]Bao N, Zhou L, Cong Y, et al. Free fatty acids are responsible for the hidden blood loss in total hip and knee arthroplasty. Med Hypoth. 2013;133(1)104-107.
[25]McManus KT, Velchik MG, Alavi A, et al. Non-invasive assessment of postoperative bleeding in TKA patients with Tc-99m RNCs. J Nuclear Med. 1987;28(8): 565-567.
[26]Zampelis V, Tägil M, Lidgren L, et al. The effect of a biphasic injectable bone substitute on the interface strength in a rabbit knee prosthesis model. J Orthop Surg Res. 2013; 8(1): 25.
[27]Mauerer A, Lange B, Welsch GH, et al. Release of Cu2+ from a copper-filled TiO2 coating in a rabbit model for total knee arthroplasty. J Mat Sci. 2014;25(3):813-821.
[28]余世明,刘建华,徐栋梁,等.兔用生物型人工膝关节假体的设计与制作[J].中华关节外科杂志(电子版), 2009,3(4):63-66.
[29]严志强,张乐,王新亮,等.计算机辅助设计兔解剖型人工膝关节假体[J].广东医学,2014,35(13):1997-2001.
[30]严俊伟,唐成,李祥全,等.全膝关节置换术后感染模型的建立[J]. 中华关节外科杂志(电子版),2014,8(1):60-64.
[31]高福强,李子剑,刘延青,等.初次全膝关节置换术后肢体肿胀程度与隐性失血量的相关性研究[J].中国矫形外科杂志,2011,19(3): 199-202.
[32]Randelli F, D’Anchise R, Ragone V, et al. Is the newest fibrin sealant an effective strategy to reduce blood loss after total knee arthroplasty? A randomized controlled study. J Arthroplasty. 2014;29(8):1516-1520.
[33]Alshryda S,Mason J,Vaghela M,et al.Topical(intra-articular) tranexamic acid reduces blod los and transfusion rates folowingtotal kne replacement:a randomized controled trial(TRANX-K).J Bone Joint Surg Am. 2013;95 (21):1961-1968.
[34]Wind TC, Barfield WR, Moskal JT. The effect of tranexamic acid on transfusion rate in primary total hip arthroplasty. J Arthroplasty. 2014; 29(2):387-389.
[35]甘伟伟,刘斌,谢贵杰.氨甲环酸应用时机对髋关节置换手术患者失血量影响的研究[J].安徽医药, 2014,18(8):1569-1571.
[36]Alcelik I, Pollock RD, Sukeik M, et al. A comparison of outcomes with and without a tourniquet in total knee arthroplasty: a systematic review and meta-analysis of randomized controlled trials. J Arthroplasty. 2012;27(3): 331-340.
[37]Zan PF, Yang Y, Fu D, et al. Releasing of tourniquet before wound closure or not in total knee arthroplasty: a meta-analysis of randomized controlled trials. J Arthroplasty. 2015;30(1):31-37.
[38]陈虎,曹力,杨德盛,等.麻醉方式与全膝关节置换术后深静脉血栓发生率分析[J].中国矫形外科杂志, 2012, 20(5): 402-405.
[39]Jiang X, Hand AR, Shen S, et al. Enhanced tissue plasminogen activator synthesis by the sympathetic neurons that innervate aging vessels. J Neurosci Res. 2003;71(4): 567-574.
[40]Bell TH, Berta D, Ralley F, et al. Factors affecting perioperative blood loss and transfusion rates in primary total joint arthroplasty: a prospective analysis of 1642 patients. Can J Surg. 2009;52(4): 295.
[41]Mega JL, Braunwald E, Wiviott SD. Low doses of rivaroxaban effectively lower the risk of cardiac events. Am J Cardiol. 2013.
[42]Tai TW,Chang CW,Yang CY,et al. Effects of tourniquet use on blood loss and soft-tissue damage in total knee arthroplasty: a randomized controlled trial. J Bone Joint Surg Am. 2012; 94(24): 2209-2215.
[43]Kumar GS, Von Arx OA, Pozo JL. Rate of blood loss over 48 hours following total knee replacement. Knee. 2005;12(4): 307-309. |
| [1] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [2] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [3] | Chen Jinping, Li Kui, Chen Qian, Guo Haoran, Zhang Yingbo, Wei Peng. Meta-analysis of the efficacy and safety of tranexamic acid in open spinal surgery [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1458-1464. |
| [4] | Yuan Jun, Yang Jiafu. Hemostatic effect of topical tranexamic acid infiltration in cementless total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 873-877. |
| [5] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Intravenous, topical tranexamic acid alone or their combination in total knee arthroplasty: a meta-analysis of randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 948-956. |
| [6] | Zhan Fangbiao, Cheng Jun, Zou Xinsen, Long Jie, Xie Lizhong, Deng Qianrong. Intraoperative intravenous application of tranexamic acid reduces perioperative bleeding in multilevel posterior spinal surgery: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 977-984. |
| [7] | Lü Zexiang, Wu Jutai, Jiang Jian, Feng Xiao, Li Tengfei, Wang Yehua. Effect of tranexamic acid combined with carbazochrome sodium sulfonate on blood loss and safety after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 386-390. |
| [8] | Wang Hao, Wang Yitao, Lü Zexiang, Li Tengfei, Wang Shaolong, Wang Yehua. Effect of repeated intravenous tranexamic acid in the perioperative period of proximal femoral nail antirotation for femoral intertrochanteric fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3319-3323. |
| [9] | Liu Jinlei, Yin Li, Zhang Yi, Wang Haitao, Li Zhuangyan, Xia Peige, Qiao Renqiu. Effects of intravenous tranexamic acid combined with periarticular multipoint injection of tranexamic acid cocktail on blood loss and pain after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2833-2839. |
| [10] | Chen Wang, Feng Shuo, Zhang Yu, Chen Xiangyang. Efficacy and safety of tranexamic acid and epsilon-aminocaproic acid in reducing perioperative blood loss during total knee arthroplasty: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(15): 2430-2436. |
| [11] | Gao Fenghe, Chen Tongying, Lin Jiebin, Liang Zujian. Efficacy and safety of tranexamic acid combined with rivaroxaban in primary total knee and hip arthroplasties: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(15): 2453-2460. |
| [12] | Ma Zhen, Liang Da, Wu Xiaolin, Zhong Wei . Safety evaluation of tranexamic acid in reducing perioperative blood loss in high tibial osteotomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(12): 1847-1852. |
| [13] | Zheng Zhihui, Chen Sheng, Guan Keli, Zheng Xun, Chen Haibo, Zeng Qingqiang. Relationship between blood loss of proximal femoral nail anti-rotation fixation and local use combined with intravenous injection of tranexamic acid [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(9): 1359-1364. |
| [14] | Deng Zengfa, He Zhiyong, Liu Kang, Yu Xinping, Liang Jianji, Wang Jinjun, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous combined with topical administration of tranexamic acid on unicompartmental knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(36): 5793-5799. |
| [15] | Zhou Zhi, Xiong Yaqiong. Application of perioperative pulse irrigation combined with tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(36): 5806-5811. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||