Chinese Journal of Tissue Engineering Research ›› 2015, Vol. 19 ›› Issue (7): 1028-1035.doi: 10.3969/j.issn.2095-4344.2015.07.009
Previous Articles Next Articles
Conjoined tendon and coracoacromial ligament transfer in the treatment of RockwoodIII acromioclavicular joint dislocation: anatomical and clinical validation
Wang Zhi-zhou1, Yilihamu Tuoheti1, Xu Chao1, Hou Yan-jie1, Guo Hong-liang1, Gan Zi-ming2, Zhang Ai-hong3
- 1Department of Orthopedics, 3Department of Ultrasound, Second Affiliated Hospital of Xinjiang Medical University, Urumqi 830063, Xinjiang Uygur Autonomous Region, China; 2Department of Anatomy, Xinjiang Medical University, Urumqi 830054, Xinjiang Uygur Autonomous Region, China
-
Online:2015-02-12Published:2015-02-12 -
Contact:Yilihamu Tuoheti, M.D., Chief physician, Department of Orthopedics, Second Affiliated Hospital of Xinjiang Medical University, Urumqi 830063, Xinjiang Uygur Autonomous Region, China -
About author:Wang Zhi-zhou, Studying for master’s degree, Department of Orthopedics, Second Affiliated Hospital of Xinjiang Medical University, Urumqi 830063, Xinjiang Uygur Autonomous Region, China
CLC Number:
Cite this article
Wang Zhi-zhou, Yilihamu Tuoheti, Xu Chao, Hou Yan-jie, Guo Hong-liang, Gan Zi-ming. Conjoined tendon and coracoacromial ligament transfer in the treatment of RockwoodIII acromioclavicular joint dislocation: anatomical and clinical validation[J]. Chinese Journal of Tissue Engineering Research, 2015, 19(7): 1028-1035.
share this article
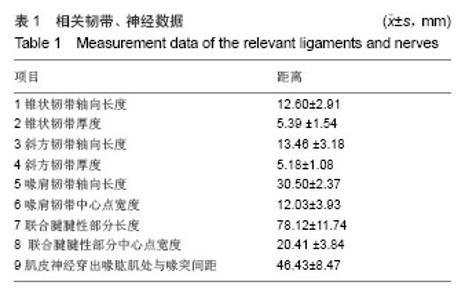
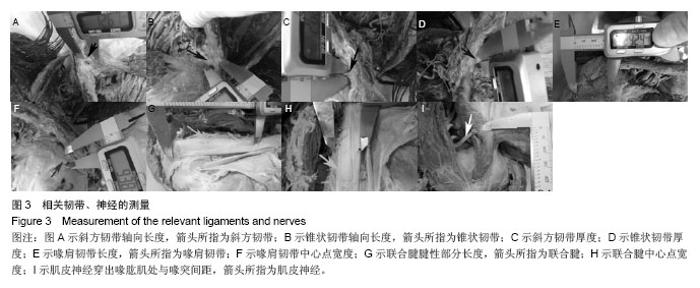
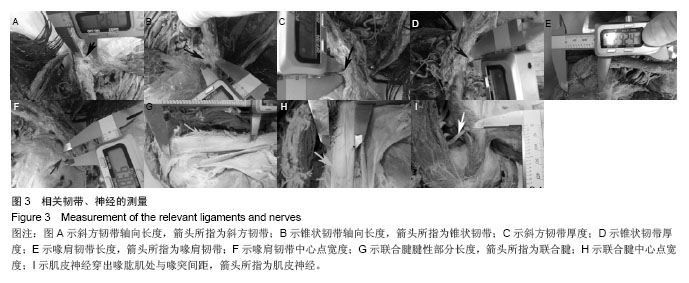
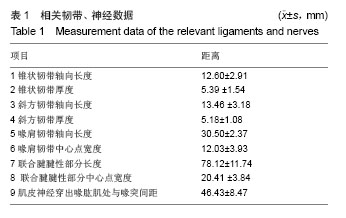
相关韧带、神经数据:喙突和锁骨由喙锁韧带连接在一起,是限制锁骨垂直移位的重要结构,由外侧的斜方韧带和内侧的锥状韧带组成。喙突和肩峰之间存在喙肩韧带,是维持喙肩弓的重要结构。尸体解剖上小心区分锥状韧带和斜方韧带,测的锥状韧带的轴向长度为12.60 mm,中心点厚度为5.39 mm,斜方韧带较锥状韧带略长(平均13.46 mm),厚度几乎一样(平均5.18 mm)。可见斜方韧带和锥状韧带几乎平均分担喙锁间隙的垂直应力。喙肩韧带是维持喙肩弓的重要结构,也是较好的韧带移植来源。测得轴向长度为30.50 mm,中心点宽度为12.03 mm。联合腱腱性部分与肌性部分移行较为模糊,作为自体肌腱移植物只考虑腱性部分,从尸体标本中可测其长度平均为78.12 mm,宽度平均为20.41 mm,可见其可提供充足的移植材料,此外,肌皮神经由C5,6,7神经纤维组成,在胸小肌下缘起自外侧束,在喙突下穿过喙肱肌,由于其存在变异情况,在此测量喙突下首支距离喙突的距离为46.43 mm(见表1,图3)。"
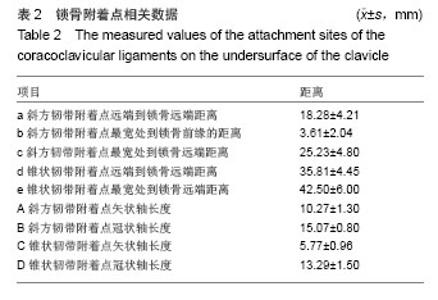
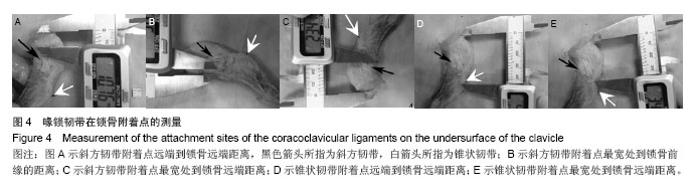
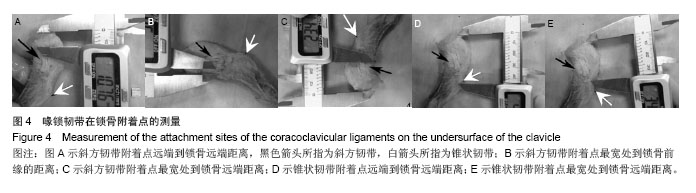
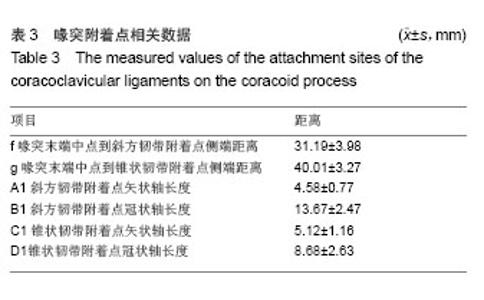
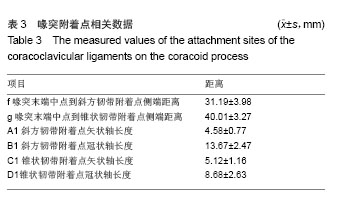
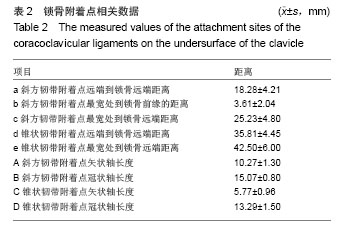
锁骨附着点相关数据:锥状韧带止于锁骨后缘的锥状结节,其附着点远端到锁骨远端距离为35.81 mm,附着点中心处到锁骨远端距离42.50 mm,矢状轴长度平均5.77 mm,冠状轴长度平均13.29 mm,明显长于喙突起点处冠状轴长度(8.68 mm),形如倒锥形结构把喙突和锁骨连在一起,而斜方韧带的附着点冠状轴长度15.07 mm与喙突起点差异不大(13.67 mm),形如四边形与锁骨、喙突之间,其锁骨附着点矢状轴长度为10.27 mm。此外,斜方韧带附着点远端到锁骨远端距离平均为18.28 mm,最宽处到锁骨前缘的距离为3.61 mm,可见其在锁骨止点偏向锁骨前缘,而锥状韧带止于锁骨后缘,共同维持喙锁距离,防止其轴向旋转(见表2,图4)。"
| [1]Nordqvist A, Petersson CJ. Incidence and causes of shoulder girdle injuries in an urban population. J Shoulder Elbow Surg. 1995;4(2):107-112. [2]Chillemi C, Franceschini V, Dei Giudici L, et al. Epidemiology of Isolated Acromioclavicular Joint Dislocation. Emerg Med Int. 2013;2013:171609. [3]Provencher MT, LeClere L, Romeo AA, et al. Avoiding and Managing Complications of Surgery of the Acromioclavicular Joint. Complication Knee Shoulder Surg. 2009: 245-264. [4]Duindam N. Comparison between open and arthroscopic procedures for lateral clavicle resection. Int Orthop. 2013. [5]Beaver AB, Parks BG, Hinton RY. Biomechanical analysis of distal clavicle excision with acromioclavicular joint reconstruction. Am J Sports Med. 2013;41(7):1684-1688. [6]Johansen JA, Grutter PW, McFarland EG, et al. Acromioclavicular joint injuries:indications for treatment and treatment options. J Shoulder Elbow Surg. 2011;20(2 Suppl): 70-82. [7]Kienast B, Thietje R, Queitsch C, et al. Mid-term results after operative treatment of rockwood grade III-V Acromioclavicular joint dislocations with an AC-hook-plate. Eur J Med Res. 2011;16: 52-56. [8]Di Francesco A, Zoccali C, Colafarina O, et al. The use of hook plate in type III and V acromioclavicular Rockwood dislocations: clinical and radiological midterm results and MRI evaluation in 42 patients. Injury. 2012;43: 147-152. [9]ElMaraghy AW, Devereaux MW, Ravichandiran K, et al. Subacromial morphometric assessment of the clavicle hook plate. Injury. 2010;41(6): 613-619. [10]Millett PJ, Braunl S, Gobezie R, et al.Acromioclavicular joint reconstruction with coracoacromial ligament transfer using the docking technique. BMC Musculoskeletal Disorders. 2009;10:6. [11]Baldwin K, Namdari S, Andersen JR, et al. Luggage Tag Technique of Anatomic Fixation of Displaced Acromioclavicular Joint Separations. Clin Orthop Relat Res. 2010;468:259-265. [12]伊力哈木托合提,曲广华,桂和,等.喙肩韧带转位治疗Ⅲ度肩锁关节脱位的临床疗效分析[J].中国骨与关节损伤杂志, 2011,26(5): 414-416. [13]Kovilazhikathu Sugathan H, Dodenhoff RM. Management of Type 3 Acromioclavicular Joint Dislocation: Comparison Long-TermFunctional Results of Two Operative Methods. ISRN Surg. 2012;2012:580504. [14]Sandmann GH, Martetschläger F, Mey L, et al. Reconstruction of displaced acromio-clavicular joint dislocations using a triple suture-cerclage:description of a safe and efficient surgical technique. Patient Safety Surg. 2012;6:25. [15]Dewar FP, Barrington TW. The treatment of chronic acromio-clavicular dislocation. J Bone Joint Surg Br. 1965; 47:32-35. [16]姜春岩,朱以明,王满宜,等.联合腱外侧半肌腱反转移位重建喙锁韧带治疗肩锁关节脱位[J].中华创伤骨科杂志,2005,7(9):803-807. [17]Gille J, Heinrichs G, Unger A, et al. Arthroscopic-assisted hook plate fixation for acromioclavicular joint dislocation. Int Orthop. 2013;37:77-82. [18]Yoo YS, Seo YJ, Noh KC, et al. Arthroscopically assisted anatomical coracoclavicular.ligament reconstruction using tendon graft. Int Orthop. 2011;35:1025-1030. [19]Ranne JO, Sarimo JJ, Rawlins MI, et al. All-arthroscopic double-bundle coracoclavicular ligament reconstruction using autogenous semitendinosus graft:a new technique. Arthrosc Tech. 2012;1(1):e11-e14. [20]Li X, Ma R, Bedi A, et al. Management of acromioclavicular joint injuries. J Bone Joint Surg Am. 2014;96(1):73-84. [21]Cadenat FM.The treatment of dislocations and fractures of the outer end of the clavicle. Int Clin. 1917;1:145-169. [22]Johnston TB, Davies DV, Davies F. Gray’s anatomy. Longmans, Green, London, 1958. [23]Renfree KJ, Riley MK, Wheeler D, et al. Ligamentous anatomy of the distal clavicle. J Shoulder Elbow Surg. 2003;12(4):355-359. [24]Boehm TD, Kirschner S, Fischer A, et al. The relation of the coracoclavicular ligament insertion to th acromioclavicular joint: a cadaver study of relevance to lateral clavicle resection. Acta Orthop Scand. 2003;74(6):718-721. [25]Rios CG, Arciero RA, Mazzocca AD. Anatomy of the clavicle and coracoid process for reconstruction of the coracoclavicular ligaments. Am J Sports Med. 2007;35(5):811-817. [26]Takase K. The coracoclavicular ligaments: an anatomic study. ORIGINAL ARTICLE. Surg Radiol Anat. 2010;32:683-688. [27]刘燕洁,何鸿陶,陈云丰,等.肩锁关节解剖学研究和临床意义[J]. 实用骨科杂志,2012, 18(2):139-142. [28]王古衡,谢仁国,汤锦波,等.同种异体肌腱重建喙锁和肩锁韧带治疗肩锁关节脱位[J].中华手外科杂志,2013,29(3):150-153. [29]Urist MR.Complete dislocations of the acromiclavicular joint; the nature of the traumatic lesion and effective methods of treatment with an analysis of forty-one cases. J Bone Joint Surg Am. 1946;28(4):813-837. [30]Fukuda K, Craig EV, An KN, et al. Biomechanical study of the ligamentous system of the acromioclavicular joint. J Bone Joint Surg. 1986;68(3):434-440. [31]尹维刚,刘秀清,崔成立,等.肱二头肌短头腱喙肱肌腱喙肩韧带重建喙锁韧带的应用解剖[J].中国临床解剖学杂志,2001,19(4): 326-328. [32]黄广智,王璐,阮彩莲,等.肱二头肌短头肌腱转位修复肩锁关节脱位的解剖及临床应用[J]. 中国临床解剖学杂志,2002,20(4): 316-317. [33]金舜瑢,李成福,李康杰,等.肩锁关节脱位改良型Dewar- Barrington式手术12例体会[J].吉林医学,2001,22(2):9. [34]Brunelli G, Brunelli F. The treatment of acromio-clavicular dislocation by transfer of the short head of biceps. Int Orthop. 1988;12(2):105-108. |
| [1] | Fang Yi, Zhao Wenzhi, Pan Deyue, Han Xin, Zhang Lu, He Hongtao, Shi Feng, Tian Tingxiao. Acromioclavicular joint dislocation: how to achieve anatomical reduction, sustained stability and micro-motion [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(5): 796-802. |
| [2] | Fu Jiaxin, Xiao Lianping, Wang Shusen, Li Xiaodong, Han Liqiang, Wang Tonghao. Therapeutic effects of paraspinal approach combined with internal fixation through pedicle of fractured vertebra versus traditional AF screw-rod system for thoracolumbar fractures [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1177-1181. |
| [3] | Qiu Zhongpeng, Li Ke, Li Gang, Liu Keyu, Du Xinhui, Meng Defeng, Shi Chenhui, Wang Weishan. Different treatments for two-part and three-part proximal humeral fractures by Neer classification: follow-up results analyzed using clinical economics [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1188-1195. |
| [4] | Ke Wei, Li Ke, Wang Sibo, Du Xinhui, Qiu Zhongpeng, Kang Zhilin, Wang Weishan, Li Gang . Open reduction and plate fixation versus closed reduction and external fixation for distal radius fractures: scores and linear regression analysis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1196-1202. |
| [5] | Tian Jie, Ru Jiangying. Preservation of the spinous process ligament complex in expanded decompression of lumbar spinal canal: advantages and disadvantages [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1228-1234. |
| [6] | Fan Zhirong, Peng Jiajie, Zhong Degui, Zhou Lin, Su Haitao, Huang Yongquan, Wu Jianglin, Liang Yihao. Suture anchor combined with open reduction and internal fixation versus open reduction and internal fixation for ankle fracture combined with deltoid ligament injury: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1307-1312. |
| [7] | Zhou Yu, Liu Yuehong, Liu Shuping, Chen Xi, Qin Wei, Li Qifeng. Spinal stability of intervertebral grafting reinforced by five or six augmenting screws versus transvertebral grafting reinforced by four augmenting screws for thoracolumbar vertebral fractures [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(4): 505-511. |
| [8] | Li Xianzhou, Wang Qian, Zhang Cunxin . Lumbar spondylolisthesis: status and prospects of implant treatment [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(4): 621-627. |
| [9] | Yin Hao, Zhou Enchang, Pan Zhengjun, Chen Guang, Jiang Hua. Finite element analysis of the four and three cannulated screws combined with buttress plate fixation for the treatment of Pauwels III femoral neck fractures [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(32): 5133-5137. |
| [10] |
Wang Lei, Li Zilong, Yuan Binbin, Wu Qingwei, Tang Fengming.
Clinical effect of locking plate versus anterograde intramedullary nail in the treatment of adult humeral shaft fractures: a meta-analysis
[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(24): 3924-3930.
|
| [11] | Hao Liang, Zhang Zhonglin, Wang Baodong, Bi Zhenggang. Intertrochanteric fracture of the femur: improvement of internal fixation device, surgical changes and related disputes [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(18): 2927-2935. |
| [12] | Yao Liquan, Ling Qinjie, Li Jiaying, Zhong Letian, Zhou Xingping, Liu Jintao, He Erxing, Yin Zhixun. Antibiotic artificial bone implantation for treating pyogenic spondylodiscitis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(14): 2133-2139. |
| [13] | Gong Zhibing, Wu Zhaoke, Zhang Huantang, Xu Zhiqing, Zhuang Zhikun, Zhang Qianjin. Allogeneic cortical bone plate combined with locking plate for Vancouver type B1 and C osteoporotic periprosthetic femoral fractures after hip arthroplasty in older adults [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(12): 1812-1817. |
| [14] | Li Xiaofeng, Xie Furong, Zhan Long, Yang Yuan. Design of locking compression plate through transoral approach [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(12): 1824-1828. |
| [15] | Tian Youyong, Wang Zhiyong. Short-term follow-up of dynamic hip screw versus proximal femoral nail anti-rotation for type AO/OTA A1 intertrochanteric femoral fracture in older adults [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(12): 1834-1839. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||