Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (14): 2133-2139.doi: 10.3969/j.issn.2095-4344.1662
Antibiotic artificial bone implantation for treating pyogenic spondylodiscitis
Yao Liquan, Ling Qinjie, Li Jiaying, Zhong Letian, Zhou Xingping, Liu Jintao, He Erxing, Yin Zhixun
- Department of Spinal Surgery, the First Affiliated Hospital of Guangzhou Medical University, Guangzhou 510120, Guangdong Province, China
-
Received:2018-12-26 -
Contact:He Erxing, Master, Chief physician, Department of Spinal Surgery, the First Affiliated Hospital of Guangzhou Medical University, Guangzhou 510120, Guangdong Province, China -
About author:Yao Liquan, Master, Department of Spinal Surgery, the First Affiliated Hospital of Guangzhou Medical University, Guangzhou 510120, Guangdong Province, China -
Supported by:the Science and Technology Program of Department of Science and Technology of Guangdong Province, No. 2014A020212369 (to YZX); the Applied Basic Project of Science and Technology Bureau of Guangzhou, No. 2013J4100041 (to YZX)
CLC Number:
Cite this article
Yao Liquan, Ling Qinjie, Li Jiaying, Zhong Letian, Zhou Xingping, Liu Jintao, He Erxing, Yin Zhixun. Antibiotic artificial bone implantation for treating pyogenic spondylodiscitis[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(14): 2133-2139.
share this article
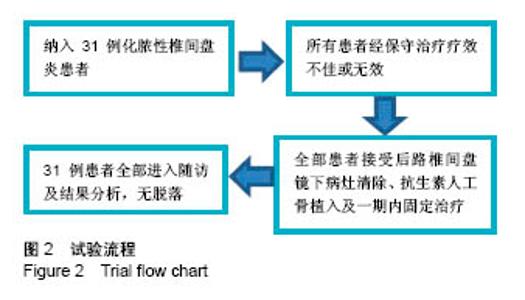
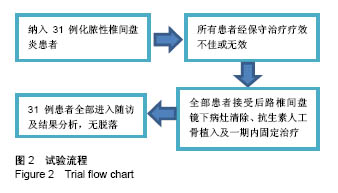
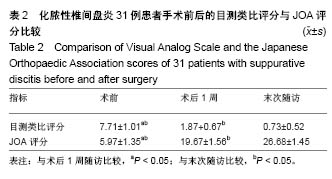
2.2 治疗结果 31例患者均顺利完成手术(24例经椎板间隙入路,7例经斜侧椎间孔入路),所有患者术后腰痛及下肢放射痛得到即刻缓解。手术时间(134±19) min,术中出血量(98±22) mL。所有病例术中均见病变椎间盘呈炎症坏死样改变,椎间隙不同程度变窄,并伴相邻终板及椎体终板下骨质不同程度的破坏。6例术中切开病变椎间盘纤维环,可见少量黄白色脓液流出;2例术中可见椎管内硬膜外脓肿病灶;5例患者术中可见脱出椎间盘髓核压迫硬脊膜囊及神经根,均顺利被清除。31例患者病理结果均显示椎间盘组织及软骨终板呈炎症性坏死改变,可见大量中性粒细胞、浆细胞浸润及部分变性坏死细胞。 细菌培养结果:革兰阳性菌中金黄色葡萄球菌5例,表皮葡萄球菌3例,白色葡萄球菌1例,无乳链球菌(B群)1例;革兰阴性菌中大肠埃希菌2例;培养阴性19例。 2.3 治疗效果 该手术方式通过内镜工作通道直接经椎间孔到达椎间隙进行病灶清除,无需剥离椎旁肌,创伤小,内镜直视下更好的保护神经根及硬脊膜囊,且术中保留棘突、椎板及一侧完整关节突关节,若通过后外侧入路经Kambin三角进入椎间隙,可完整保留患者脊柱骨性结构,联合椎弓根螺钉固定,保持了脊柱稳定性。椎间植入抗生素硫酸钙人工骨,可提高并维持局部抗生素浓度,有效控制感染病灶。 所有病例手术过程中均无硬脊膜及神经根损伤,术后患者疼痛即刻减轻,术后1-4 d均可佩戴腰围下地活动,平均下地时间为(2.00±0.95) d,下地活动后即可进行适度腰背肌锻炼;31例患者手术切口均一期愈合,术后5-10 d腰腿痛消失并顺利出院。2例出现单侧下肢趾背伸肌力下降患者,术前为2级,出院时趾背伸肌力均恢复至3+级,末次随访均恢复至4级。 2.4 随访结果及观察指标 实验室指标:31例术前血沉平均为(62.45±25.62) mm/h,术后第1天复查血沉平均为(69.25±24.23) mm/h,术后1周血沉明显下降,平均为(24.22±7.14) mm/h,术后1个月全部恢复正常;术前C-反应蛋白平均为(80.5±27.3) mg/L,术后第1天复查C-反应蛋白平均为(95.1±33.3) mg/L,术后1周明显下降,平均为(18.9±7.2) mg/L,术后1个月全部恢复正常。所有患者术后第3,6个月复查血沉及C-反应蛋白均正常。 目测类比评分及JOA评分:30例患者术后术后1周、末次随访时的目测类比评分及JOA评分与术前比较差异有显著性意义(P < 0.05),见表2。末次随访时JOA改善率,优90%(28例),良10%(3例)。"
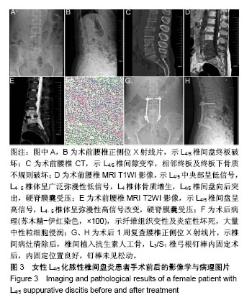
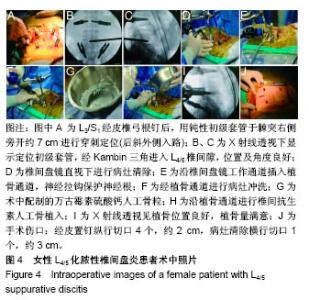
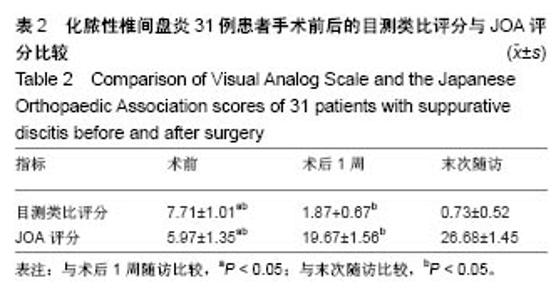
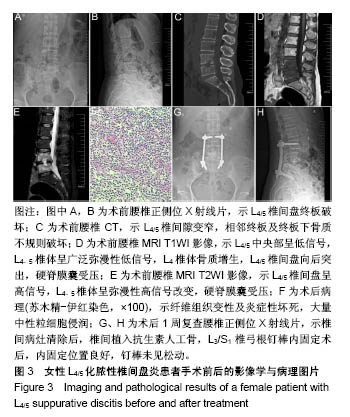
2.6 典型病例 63岁女性患者,既往有乳腺癌病史,因“腰骶部疼痛1个月、双下肢放射痛2周”入院,入院诊断:L4/5化脓性椎间盘炎;右乳腺癌改良根治术后。患者入院体温38.9 ℃,腰背部疼痛明显,L4-5棘突及椎旁肌肉压痛阳性,伴双侧臀部及双侧大腿后外侧放射性疼痛,肌力、感觉均正常,生理反射存在,病理反射未引出。入院后查血常规:白细胞13.4×109 L-1,中性粒细胞83%,血沉128 mm/h,C-反应蛋白63.6 mg/L,降钙素原正常。术前目测类比评分8分,JOA评分6分。 患者入院后行L4、5椎体及L4/5椎间盘穿刺活检术,病例结果提示送检组织炎症性病理改变,培养结果提示无乳链球菌(B群)感染。入院完善术前检查评估后予后路内镜下病灶清除、抗生素人工骨植入联合一期L3/S1经皮椎弓根螺钉内固定术,术中取标本送病理检查及进行细菌培养,术程顺利,术中手术时间出血50 mL。术后第1天血常规:白细胞12.7×109 L-1,中性粒细胞76%,血沉65 mm/h,C-反应蛋白20.9 mg/L,降钙素原正常,目测类比评分2分,JOA评分19分。术后1周血常规:白细胞8.64×109 L-1,中性粒细胞65%,血沉21 mm/h,C-反应蛋白10.3 mg/L,降钙素原正常;目测类比评分1分,JOA评分26分。术后1个月血常规、血沉及C-反应蛋白均回复正常,目测类比评分1分,JOA评分28分。术后病理结果提示炎性组织改变,中性粒细胞浸润;培养结果提示无乳链球菌(B群)感染。术后根据药敏结果予敏感抗生素莫西沙星治疗。患者术后腰腿疼痛即刻缓解,术后第2天佩戴腰围下地活动,术后1周顺利出院。该患者资料图片见图3,4。"
| [1] Pola E,Taccari F,Autore G,et al.Multidisciplinary management of pyogenic spondylodiscitis: Epidemiological and clinical features, prognostic factors and long-term outcomes in 207 patients. Eur Spine J.2018;27(Suppl 2):229-236.[2] Petkova AS,Zhelyazkov CB,Kitov BD.Spontaneous Spondylodiscitis - Epidemiology, Clinical Features, Diagnosis and Treatment.Folia Med(Plovdiv).2017;59(3):254-260.[3] Vcelak J,Chomiak J,Toth L.Surgical treatment of lumbar spondylodiscitis: A comparison of two methods.Int Orthop. 2014; 38(7):1425-1434.[4] Herren C,Jung N,Pishnamaz M,et al.Spondylodiscitis: Diagnosis and treatment options. Dtsch Arztebl Int. 2017;114(51-52):875-882.[5] Zarghooni K,Röllinghoff M,Sobottke R,et al.Treatment of spondylodiscitis.Int Orthop.2012;36(2):405-411.[6] Choi EJ,Kim SY,Kim HG,et al.Percutaneous endoscopic debridement and drainage with four different approach methods for the treatment of spinal infection.Pain Physician. 2017;20(6): E933-E940.[7] Ito M,Abumi K,Kotani Y,et al.Clinical outcome of posterolateral endoscopic surgery for pyogenic spondylodiscitis: Results of 15 patients with serious comorbid conditions.Spine (Phila Pa 1976). 2007;32(2):200-206.[8] Fu TS,Chen LH,Chen WJ.Minimally invasive percutaneous endoscopic discectomy and drainage for infectious spondylodiscitis. Biomed J.2013;36(4):168-174.[9] 王春增,张兆川,赵猛,等.椎间孔镜下病灶清除冲洗治疗腰椎非特异性感染的疗效[J].实用骨科杂志, 2018,24(1):60-63.[10] Abbasi H,Abbasi A.Oblique lateral lumbar interbody fusion (OLLIF): Technical notes and early results of a single surgeon comparative study.Cureus.2015;7(10):e351.[11] 丁艳丽,杨静.骨科配戴腰围病人的规范健康教育指导[J].中国保健营养(上旬刊),2013,23(7):3994.[12] 李倩.腰围佩戴时间的长短对腰椎间盘突出症患者的影响[J].饮食保健, 2016,3(17):188.[13] Lener S,Hartmann S,Barbagallo GMV,et al.Management of spinal infection: A review of the literature.Acta Neurochir (Wien). 2018; 160(3):487-496.[14] Rutges JP,Kempen DH,van Dijk M,et al.Outcome of conservative and surgical treatment of pyogenic spondylodiscitis: A systematic literature review.Eur Spine J. 2016;25(4):983-999.[15] Tsai TT,Yang SC,Niu CC,et al.Early surgery with antibiotics treatment had better clinical outcomes than antibiotics treatment alone in patients with pyogenic spondylodiscitis: A retrospective cohort study.BMC Musculoskelet Disord. 2017;18(1):175.[16] 舍炜,陈根元,侯卫华,等.显微内窥镜下腰椎间盘摘除和传统开放手术治疗腰椎间盘突出症的Meta分析[J].中国组织工程研究与临床康复, 2010,14(48):9090-9094.[17] Foley KT,Smith MM,Rampersaud YR.Microendoscopic approach to far-lateral lumbar disc herniation.Neurosurg Focus.1999;7(5):e5.[18] Perez-Cruet MJ,Foley KT,Isaacs RE,et al. Microendoscopic lumbar discectomy: technical note. Neurosurgery.2002;51(5 Suppl): S129-S136.[19] Pao J,Chen W,Chen P.Clinical outcomes of microendoscopic decompressive laminotomy for degenerative lumbar spinal stenosis. Eur Spine J.2009;18(5):672-678.[20] 马向阳,杨浩志,邹小宝,等.一期极外侧入路病灶清除植骨融合闭式冲洗引流联合后路内固定术治疗原发性腰椎间隙感染[J].中国脊柱脊髓杂志,2018,28(8):726-731.[21] 刘海平,郝定均,王晓东,等.原发性腰椎间隙感染病灶清除植骨融合内固定临床疗效分析[J].实用骨科杂志,2017,23(5):390-394.[22] 杨小春,常龙,尚雁冰,等.后路病灶清除、植骨融合治疗非特异性腰椎椎间隙感染[J].中华骨科杂志, 2017,37(18):1136-1142.[23] 张成程,陈建明,李占清,等.后路病灶清除内固定+负载抗生素硫酸钙治疗腰椎间隙感染[J].西南国防医药, 2017,27(11):1220-1222.[24] Anagnostakos K, Koch K.Pharmacokinetic properties and systemic safety of Vancomycin-Impregnated cancellous bone grafts in the treatment of spondylodiscitis. Biomed Res Int.2013;2013:358217.[25] Sanicola SM,Albert SF.The in vitro elution characteristics of vancomycin and tobramycin from calcium sulfate beads. J Foot Ankle Surg.2005;44(2):121-124.[26] Laycock P,Cooper J,Howlin R,et al.In vitro efficacy of antibiotics released from calcium sulfate bone void filler beads.Materials. 2018;11(11):2265.[27] 魏劲松,曾荣,林颢,等.硫酸钙骨粉混合抗生素在腰椎原发性椎间隙感染手术治疗中的应用[J].颈腰痛杂志,2009,30(3):214-216.[28] Chen L,Cheng J,Li B,et al.Posterior debridement, interbody fusion, internal fixation for treatment of lumbar discitis.Zhongguo Gu Shang. 2017;30(5):475-478.[29] 李龙,盛伟斌,杨森,等.原发性腰椎椎间隙感染:病灶清除植骨及椎弓根螺钉置入内固定的联合修复[J].中国组织工程研究, 2015,19(13): 2063-2068.[30] Lim JK,Kim SM,Jo DJ,et al.Anterior interbody grafting and instrumentation for advanced spondylodiscitis.J Korean Neurosurg Soc.2008;43(1):5-10.[31] Wang X,Tao H,Zhu Y,et al.Management of postoperative spondylodiscitis with and without internal fixation.Turk Neurosurg. 2015;25(4):513-518. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [3] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [4] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [5] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [6] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [7] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [8] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [9] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [10] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [11] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [12] | Wang Hao, Chen Mingxue, Li Junkang, Luo Xujiang, Peng Liqing, Li Huo, Huang Bo, Tian Guangzhao, Liu Shuyun, Sui Xiang, Huang Jingxiang, Guo Quanyi, Lu Xiaobo. Decellularized porcine skin matrix for tissue-engineered meniscus scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3473-3478. |
| [13] | Mo Jianling, He Shaoru, Feng Bowen, Jian Minqiao, Zhang Xiaohui, Liu Caisheng, Liang Yijing, Liu Yumei, Chen Liang, Zhou Haiyu, Liu Yanhui. Forming prevascularized cell sheets and the expression of angiogenesis-related factors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3479-3486. |
| [14] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| [15] | Liu Liyong, Zhou Lei. Research and development status and development trend of hydrogel in tissue engineering based on patent information [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3527-3533. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||