Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (14): 2177-2182.doi: 10.3969/j.issn.2095-4344.1656
Previous Articles Next Articles
Autologous platelet gel-collagen biologically active composite membrane for repair of periodontal bone defect in rats
Zhang Xufeng1, Fu Qiya1, Zheng Genjian1, Guo Yusu1, Chen Danyu1, Fu Fangman1, Wu Hui1, Wang Lin2
- 1Department of Oral Medicine, the First Affiliated Hospital of Hainan Medical University, Haikou 570102, Hainan Province, China; 2Department of Stomatology, Hainan Provincial People’s Hospital, Haikou 570311, Hainan Province, China
-
Received:2018-11-12 -
Contact:Wang Lin, MD, Chief physician, Department of Stomatology, Hainan Provincial People's Hospital, Haikou 570311, Hainan Province, China -
About author:Zhang Xufeng, Master, Associate chief physician, Department of Oral Medicine, the First Affiliated Hospital of Hainan Medical University, Haikou 570102, Hainan Province, China -
Supported by:the Natural Science Foundation of Hainan Province in 2014, No. 814315 (to WL)
CLC Number:
Cite this article
Zhang Xufeng, Fu Qiya, Zheng Genjian, Guo Yusu, Chen Danyu, Fu Fangman, Wu Hui, Wang Lin. Autologous platelet gel-collagen biologically active composite membrane for repair of periodontal bone defect in rats[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(14): 2177-2182.
share this article
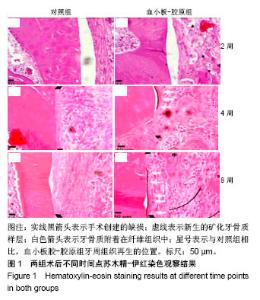
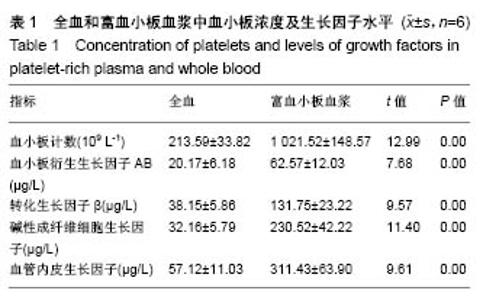
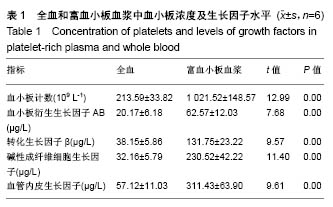
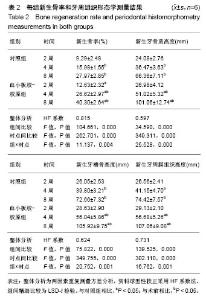
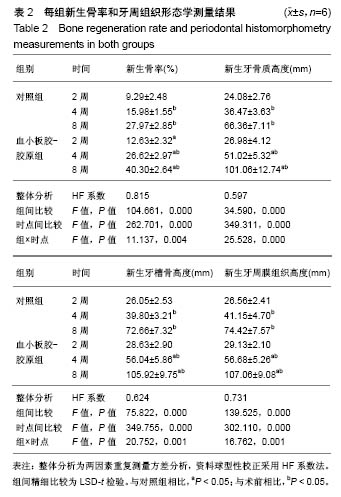
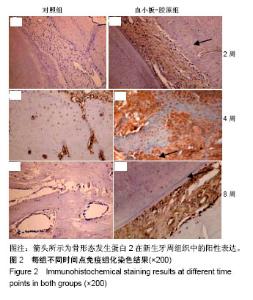
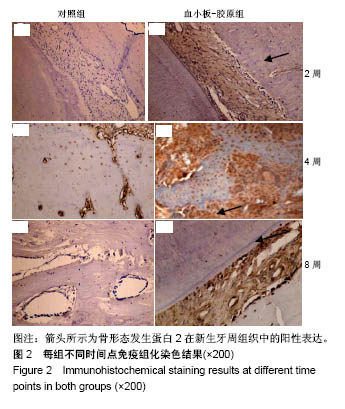
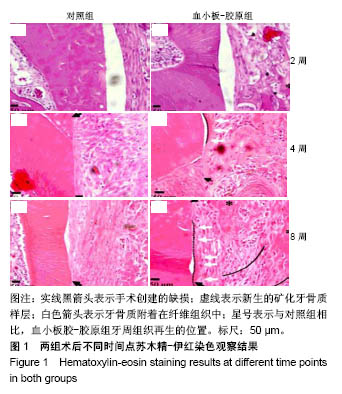
2.3 实验动物大体观察 所有大鼠术后1 d后恢复基本活动,饮水、进食恢复正常。所有动物术后切口无感染、无炎症,伤口愈合良好。 2.4 组织学观察结果 术后2周:血小板胶-胶原组和对照组在组织缺损部位附近均可见大量炎性细胞和大量纤维组织,且血小板胶-胶原组在缺损部位有少量新骨形成,但受损的牙本质或牙骨质表面上都没有牙骨形成的迹象。术后4周:对照组可见大量纤维组织,在缺损部位处有少量的新生骨组织。血小板胶-胶原组纤维组织少量增生,且有一定程度的新生骨组织和牙骨质生成。NC层呈现出细胞状,与相邻未损伤牙骨质层融为一体,骨样细胞出现在陷窝内,与骨纤维胶原处相互交错状态。然而,2组的纤维组织大部分无规则生长。术后8周:对照组伴随着牙骨质和结缔组织的附着有少量的新生骨形成。血小板胶-胶原组新生牙骨质和牙槽骨与新生结缔组织附着生长,形成矿化组织,且在大部分区域与周围的牙槽骨融合。牙周韧带胶原纤维的组织生长规则,新形成的牙骨质样组(包括牙骨质样细胞)出现在暴露的牙本质表面上,见图1。"
| [1] Moradian H, Rafiee A, Ayatollahi M. Design and fabrication of a novel transplant combined with human bone marrow mesenchymal stem cells and platelet-rich fibrin: new horizons for periodontal tissue regeneration after dental trauma.Iran J Pharm Res. 2017;16(4):1370-1378.[2] Jimbo R, Singer J, Tovar N, et al. Regeneration of the cementum and periodontal ligament using local BDNF delivery in class II furcation defects. J Biomed Mater Res B Appl Biomater. 2018;106(4):1611-1617.[3] Ogawa K, Miyaji H, Kato A, et al. Periodontal tissue engineering by nano beta-tricalcium phosphate scaffold and fibroblast growth factor-2 in one-wall infrabony defects of dogs. J Periodontal Res. 2016;51(6):758-767.[4] Heng NH,Zahlten J,Cordes V,et al. Effects of enamel matrix derivative and transforming growth factor-β1 on connective tissue growth factor in human periodontal ligament fibroblasts. J Periodontol,. 2015;86(4):569-577.[5] Rakhmatia YD, Ayukawa Y, Furuhashi A, et al. Current barrier membranes: titanium mesh and other membranes for guided bone regeneration in dental applications. J Prosthodont Res. 2013;57(1):3-14.[6] 陈凤超,陈民才,颜彤彤,等.同种异体富血小板血浆对创面胶原合成的作用及其机制研究[J].中华外科杂志,2017,55(4):303-307.[7] 李晋,王秉新.Bio-Oss结合Bio-Gide修复牙槽临界骨缺损的效果[J].中国老年学杂志,2013,33(15):3666-3667.[8] Duruel T, Çakmak AS, Akman A, et al. Sequential IGF-1 and BMP-6 releasing chitosan/alginate/PLGA hybrid scaffolds for periodontal regeneration. Int J Biol Macromol. 2017;104(Pt A): 232-241.[9] Dhurat R, Sukesh M. Principles and methods of preparation of platelet-rich plasma: a review and author's perspective. J Cutan Aesthet Surg. 2014;7(4):189-197.[10] Takeuchi T, Bizenjima T, Ishii Y, et al. Enhanced healing of surgical periodontal defects in rats following application of a self-assembling peptide nanofibre hydrogel. J Clin Periodontol. 2016;43(3):279-288.[11] 李睿,王春兰,范月静,等.纳米胶原基骨修复牙周病及根尖周病骨缺损[J].中国组织工程研究,2012,16(34):6317-6320.[12] 詹雅琳,胡文杰,徐涛,等.罹患重度牙周炎磨牙拔除后应用去蛋白牛骨基质与可吸收胶原膜进行位点保存的组织学研究[J].北京大学学报(医学版),2017, 49(1):169-175.[13] Zhou T, Liu X, Sui B, et al. Development of fish collagen/bioactive glass/ chitosan composite nanofibers as a GTR/GBR membrane for inducing periodontal tissue regeneration. Biomed Mater. 2017;12(5): 055004.[14] Hudson DM, Garibov M, Dixon DR, et al. Distinct post-translational features of type I collagen are conserved in mouse and humanperiodontal ligament. J Periodontal Res. 2017;52(6):1042-1049.[15] Sartori M, Giavaresi G, Parrilli A, et al. Collagen type I coating stimulates bone regeneration and osteointegration of titanium implants in the osteopenic rat. Int Orthop. 2015;39(10):2041-2052.[16] Capella-Monsonís H, Coentro JQ, Graceffa V, et al. An experimental toolbox for characterization of mammalian collagen type I in biological specimens. Nat Protoc. 2018;13(3):507-529. [17] Jo JY, Jeong SI, Shin YM, et al. Sequential delivery of BMP-2 and BMP-7 for bone regeneration using a heparinized collagen membrane. Int J Oral Maxillofac Surg. 2015;44(7):921-928.[18] De Pascale MR, Sommese L, Casamassimi A, et al. Platelet derivatives in regenerative medicine: an update. Transfus Med Rev. 2015;29(1):52-61.[19] 楚佳奇,孙杰聪,李鹏,等.富血小板血浆联合人脐带间充质干细胞移植对大鼠骨质疏松骨折愈合的影响[J].中国骨质疏松杂志, 2016,22(3):283-287.[20] 李君,梁刘凤,钟雯怡,等.羊富血小板胶细胞基质在2种牙周缺损模型中的修复效果[J].口腔材料器械杂志,2016,25(4):204-208.[21] Yu T, Pan H, Hu Y, et al. Autologous platelet-rich plasma induces bone formation of tissue-engineered bone with bone marrow mesenchymal stem cells on beta-tricalcium phosphate ceramics. J Orthop Surg Res. 2017;12(1):178.[22] Shafieian R, Matin MM, Rahpeyma A, et al. Effects of human adipose-derived stem cells and platelet-rich plasma on healing response of canine alveolar surgical bone defects. Arch Bone Jt Surg. 2017;5(6): 406-418.[23] De Pascale MR, Sommese L, Casamassimi A, et al. Platelet derivatives in regenerative medicine: an update. Transfus Med Rev. 2015;29(1):52-61.[24] Willemsen JC, van der Lei B, Vermeulen KM, et al. The effects of platelet-rich plasma on recovery time and aesthetic outcome in facial rejuvenation: preliminary retrospective observations. Aesthetic Plast Surg. 2014;38(5):1057-1063.[25] Piccin A, Rebulla P, Pupella S, et al. Impressive tissue regeneration of severe oral mucositis post stem cell transplantation using cord blood platelet gel. Transfusion. 2017;57(9):2220-2224.[26] Mori M, Rossi S, Bonferoni MC, et al. Calcium alginate particles for the combined delivery of platelet lysate and vancomycin hydrochloride in chronic skin ulcers. Int J Pharm. 2014;30,461(1-2):505-513.[27] 王淑君.血小板胶促进创面愈合的研究进展[J].医学研究生学报,2017,30(3): 333-336.[28] Fioravanti C, Frustaci I, Armellin E, et al. Autologous blood preparations rich in platelets, fibrin and growth factors. Oral Implantol (Rome). 2016; 8(4):96-113.[29] Yamano S, Haku K, Yamanaka T, et al. The effect of a bioactive collagen membrane releasing PDGF or GDF-5 on bone regeneration. Biomaterials. 2014;35(8):2446-2453.[30] Stampanoni Bassi M, Iezzi E, Marfia GA, et al. Platelet-derived growth factor predicts prolonged relapse-free period in multiple sclerosis. J Neuroinflammation. 2018;15(1):108.[31] Torres K, Pietrzyk ?, Plewa Z, et al. TGF-β and inflammatory blood markers in prediction of intraperitoneal adhesions. Adv Med Sci. 2017;63(2):220-223. [32] 顾涛,张彦秋,刘立杰,等.非小细胞肺癌患者化疗前后血清VEGF/血小板数和TGF-β1检测的临床意义[J].中国实验诊断学, 2017,21(4):585-588.[33] Oryan A, Moshiri A, Meimandi-Parizi A, et al. Role of xenogenous bovine platelet gel embedded within collagen implant on tendon healing: an in vitro and in vivo study. Exp Biol Med (Maywood). 2015;240(2):194-210.[34] Kobayashi E, Flückiger L, Fujioka-Kobayashi M, et al. Comparative release of growth factors from PRP, PRF and advanced-PRF. Clin Oral Investig. 2016;20(9):2353-2360.[35] 林静,陈超,林敏魁,等.牙周组织工程中动物模型的研究进展[J].全科口腔医学电子杂志,2016,3(20):10-12.[36] Kaku M, Kitami M, Rosales Rocabado JM, et al. Recruitment of bone marrow-derived cells to the periodontal ligament via the stromal cell-derived factor-1/C-X-C chemokine receptor type 4 axis.J Periodontal Res. 2017;52(4):686-694.[37] Scioli MG, Bielli A, Gentile P, et al. Combined treatment with platelet-rich plasma and insulin favours chondrogenic and osteogenic differentiation of human adipose-derived stem cells in three-dimensional collagen scaffolds. J Tissue Eng Regen Med. 2017;11(8):2398-2410. [38] 许繁,杨德圣.Bio-Gide胶原膜对兔骨髓间充质干细胞增殖和成骨分化的影响[J].中国组织工程研究,2014,18(30):4797-4803.[39] Holmes HL, Wilson B, Goerger JP, et al. Facilitated recruitment of mesenchymal stromal cells by bone marrow concentrate and platelet rich plasma. PLoS One. 2018;13(3):e0194567.[40] Hirakawa Y, Manaka T, Orita K, et al. The accelerated effect of recombinant human bone morphogenetic protein 2 delivered by β-tricalcium phosphate on tendon-to-bone repair process in rabbit models. J Shoulder Elbow Surg. 2018;27(5):894-902. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Jiang Hongying, Zhu Liang, Yu Xi, Huang Jing, Xiang Xiaona, Lan Zhengyan, He Hongchen. Effect of platelet-rich plasma on pressure ulcers after spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1149-1153. |
| [3] | Shen Jinbo, Zhang Lin. Micro-injury of the Achilles tendon caused by acute exhaustive exercise in rats: ultrastructural changes and mechanism [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1190-1195. |
| [4] | Liang Xueqi, Guo Lijiao, Chen Hejie, Wu Jie, Sun Yaqi, Xing Zhikun, Zou Hailiang, Chen Xueling, Wu Xiangwei. Alveolar echinococcosis protoscolices inhibits the differentiation of bone marrow mesenchymal stem cells into fibroblasts [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 996-1001. |
| [5] | Duan Liyun, Cao Xiaocang. Human placenta mesenchymal stem cells-derived extracellular vesicles regulate collagen deposition in intestinal mucosa of mice with colitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1026-1031. |
| [6] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [7] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| [8] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [9] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [10] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [11] | Liu Liu, Zhou Qingzhu, Gong Zhuo, Liu Boyan, Yang Bin, Zhao Xian. Characteristics and manufacturing techniques of collagen/inorganic materials for constructing tissue-engineered bone [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 607-613. |
| [12] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [13] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [14] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [15] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||