Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (10): 1507-1513.doi: 10.3969/j.issn.2095-4344.1618
Previous Articles Next Articles
Bone cement distribution form and diffusion degree after percutaneous vertebroplasty: an analysis based on Mimics software and its clinical significance
Yuan Dechao1, Wu Chao1, 2, Deng Jiayan2, Tan Lun1, Lin Xu1, Wang Xiangyu1
- 1Department of Orthopedics, 2Digital Medical Center, Zigong No. 4 People’s Hospital, Zigong 643000, Sichuan Province, China
-
Received:2018-11-13Online:2019-04-08Published:2019-04-08 -
Contact:Wu Chao, Master, Chief physician, Department of Orthopedics, Zigong No. 4 People’s Hospital, Zigong 643000, Sichuan Province, China -
About author:Yuan Dechao, Master, Physician, Department of Orthopedics, Zigong No. 4 People’s Hospital, Zigong 643000, Sichuan Province, China -
Supported by:the Major Scientific Research Plan of Sichuan Province, No. 2016JY0108 (to WC); the Major Scientific Research Plan of Zigong City, No. 2017ZC43 (to YDC)
CLC Number:
Cite this article
Yuan Dechao, Wu Chao, Deng Jiayan, Tan Lun, Lin Xu, Wang Xiangyu . Bone cement distribution form and diffusion degree after percutaneous vertebroplasty: an analysis based on Mimics software and its clinical significance[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(10): 1507-1513.
share this article
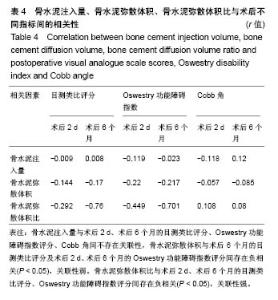
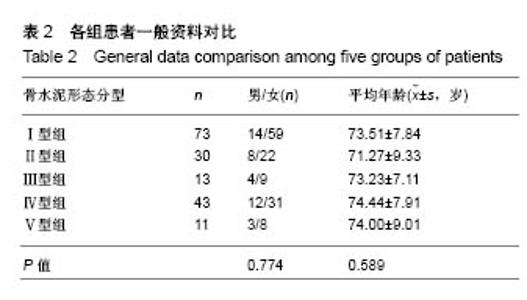
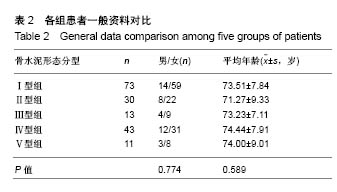
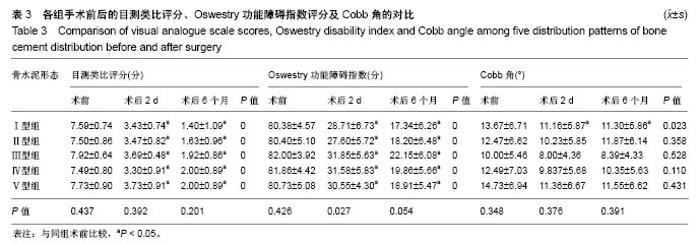
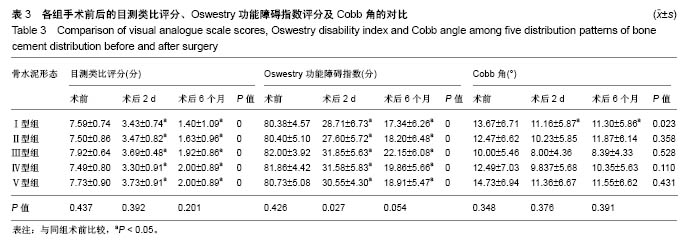
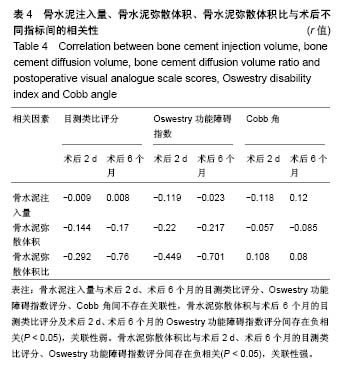
2.5 骨水泥弥散程度 术中实际骨水泥注射量为2.0- 7.5 mL,平均(5.19±1.13) mL,骨水泥弥散体积为3.01- 9.84 mL,平均(6.69±1.19) mL,术中实际骨水泥注入量与弥散体积比较差异有显著性意义(P < 0.05)。骨水泥弥散体积比为13.09%-27.09%,平均为(20.93±3.13)%。骨水泥注入量与术后2 d、术后6个月的目测类比评分、Oswestry功能障碍指数评分、Cobb角间不存在关联性,骨水泥弥散体积与术后6个月的目测类比评分及术后2 d、术后6个月的Oswestry功能障碍指数评分间存在负相关(P < 0.05),关联性弱。骨水泥弥散体积比与术后2 d、术后6个月的目测类比评分、Oswestry功能障碍指数评分间存在负相关(P < 0.05),关联性强,见表4。"
| [1] 王志宝,孙铁山,李国平.近20年来中国人口老龄化的区域差异及其演化[J].人口研究,2013,37(1):66-77.[2] Alpantaki K, Dohm M, Korovessis P,et al.Surgical options for osteoporotic vertebral compression fractures complicated with spinal deformity and neurologic deficit. Injury. 2018; 49(2):261-271.[3] Schupfner R, Stoevelaar H, Blattert T, et al.Treatment of osteoporotic vertebral compression fractures: Applicability of appropriateness criteria in clinical practice. Pain Physician. 2016; 19(1):113-120.[4] 邱贵兴,裴福兴,胡侦明,等.中国骨质疏松性骨折诊疗指南[J].中华骨与关节外科杂志,2015,8(5):371-375.[5] Luthman S, Widén J,Borgström F.Appropriateness criteria for treatment of osteoporotic vertebral compression fractures. Osteoporos Int.2017; 29(4):793-804.[6] Wang B, Guo H, Yuan L, et al.A prospective randomized controlled study comparing the pain relief in patients with osteoporotic vertebral compression fractures with the use of vertebroplasty or facet blocking.Eur Spine J. 2016; 25(11):3486-3494.[7] Li YX, Guo DQ, Zhang SC, et al.Risk factor analysis for re-collapse of cemented vertebrae after percutaneous vertebroplasty (pvp) or percutaneous kyphoplasty (pkp). Int Orthop. 2018; 42(9): 2131-2139.[8] 江晓兵,莫凌,梁德,等.骨水泥在椎体骨折线内弥散情况对椎体成形术治疗效果的影响[J].中国脊柱脊髓杂志, 2014,24(2):144-149.[9] 贺宝荣,许正伟,郝定均,等.骨水泥在骨质疏松性骨折椎体内分布状态与生物力学性能的关系[J].中华骨科杂志, 2012,32(8):768-773.[10] 黄文东.骨水泥弥散体积在椎体成形术中概念的建立和初步应用[D].广州:广州医科大学,2010.[11] 江晓兵,黄伟权,庞智晖,等.基于Mimics软件计算椎体强化术后椎体内骨水泥体积及骨水泥/椎体体积比的新方法[J].中国脊柱脊髓杂志, 2013,23(3):238-243.[12] Song BK, Eun JP,Oh YM. Clinical and radiological comparison of unipedicular versus bipedicular balloon kyphoplasty for the treatment of vertebral compression fractures. Osteoporos Int.2009; 20(10):1717-1723.[13] 张大鹏,毛克亚,强晓军,等.椎体增强术后骨水泥分布形态分型及其临床意义[J].中华创伤杂志,2018,34(2):130-137.[14] Yang EZ, Xu JG, Huang GZ, et al.Percutaneous vertebroplasty versus conservative treatment in aged patients with acute osteoporotic vertebral compression fractures. Spine (Phila Pa 1976). 2016; 41(8): 653-660.[15] Zhang L, Liu Z, Wang J, et al. Unipedicular versus bipedicular percutaneous vertebroplasty for osteoporotic vertebral compression fractures: a prospective randomized study.BMC Musculoskelet Disord. 2015;16:145.[16] Zhang Y, Shi L, Tang P, et al.Comparison of the efficacy between two micro-operative therapies of old patients with osteoporotic vertebral compression fracture: A network meta-analysis. J Cell Biochem. 2017; 118(10):3205-3212.[17] Chang X, Lv Y-F, Chen B, et al. Vertebroplasty versus kyphoplasty in osteoporotic vertebral compression fracture: A meta-analysis of prospective comparative studies.Int Orthop.2014; 39(3):491-500.[18] Blasco J, Martinez-Ferrer A, Macho J, et al.Effect of vertebroplasty on pain relief, quality of life, and the incidence of new vertebral fractures: A 12-month randomized follow-up, controlled trial.J Bone Miner Res. 2012; 27(5):1159-1166.[19] Clark W, Bird P, Gonski P, et al.Safety and efficacy of vertebroplasty for acute painful osteoporotic fractures (vapour): A multicentre, randomised, double-blind, placebo-controlled trial.Lancet. 2016; 388:1408-1416.[20] Lin JH, Chien LN, Tsai WL, et al.Early vertebroplasty associated with a lower risk of mortality and respiratory failure in aged patients with painful vertebral compression fractures: A population-based cohort study in taiwan. Spine J. 2017; 17(9):1310-1318.[21] Palmer S, Barnett S, Cramp M, et al.Effects of postural taping on pain, function and quality of life following osteoporotic vertebral fractures-a feasibility trial.Musculoskeletal Care.2018;16(3): 345-352.[22] Schiller J, Korallus C, Bethge M, et al.Effects of acupuncture on quality of life and pain in patients with osteoporosis-a pilot randomized controlled trial.Arch Osteoporos. 2016;11(1):34.[23] Hou Y, Yao Q, Zhang G, et al.Polymethylmethacrylate distribution is associated with recompression after vertebroplasty or kyphoplasty for osteoporotic vertebral compression fractures: A retrospective study.PLoS One. 2018;13(6):e0198407.[24] Chen Q, Liu L,Liang G.Distribution characteristics of bone cement used for unilateral puncture percutaneous vertebroplasty in multiple planes. Orthopade.2018; 47(7):585-589.[25] Sun HB, Jing XS, Liu YZ, et al.The optimal volume fraction in percutaneous vertebroplasty evaluated by pain relief, cement dispersion, and cement leakage: A prospective cohort study of 130 patients with painful osteoporotic vertebral compression fracture in the thoracolumbar vertebra.World Neurosurg.2018; 114:677-688.[26] Zhang L, Wang Q, Wang L, et al.Bone cement distribution in the vertebral body affects chances of recompression after percutaneous vertebroplasty treatment in elderly patients with osteoporotic vertebral compression fractures. Clin Interv Aging. 2017;12:431-436.[27] 林上进,林伟龙,杨丰建,等. Pvp术骨水泥形态类型与术后伤椎高度丢失的关系研究[J].老年医学与保健,2017,23(4):309-313.[28] Garg B,Mehta N. Current status of 3d printing in spine surgery. J Clin Orthop Trauma. 2018; 9(3):218-225.[29] Hsu MR, Haleem MS,Hsu W. 3D Printing Applications in Minimally Invasive Spine Surgery. Minim Invasive Surg. 2018;2018:4760769.[30] Khan U, Yasin A, Abid M, et al.A Methodological Review of 3D Reconstruction Techniques in Tomographic Imaging.J Med Syst. 2018;42(10):190.[31] Li J, Lin J, Xu J, et al.A novel approach for percutaneous vertebroplasty based on preoperative computed tomography-based three-dimensional model design. World Neurosurg. 2017;105: 20-26.[32] Li J, Lin J, Yang Y, et al.3-dimensional printing guide template assisted percutaneous vertebroplasty: Technical note.J Clin Neurosci. 2018; 52:159-164.[33] Yu W, Liang D, Yao Z, et al.Risk factors for recollapse of the augmented vertebrae after percutaneous vertebroplasty for osteoporotic vertebral fractures with intravertebral vacuum cleft. Medicine(Baltimore).2017;96(2):e5675.[34] 付兆宗,陈忠羡,秦英,等.骨水泥分布指数对椎体成形术后症状性邻近节段骨折的影响[J].南方医科大学学报, 2017,37(7):947-951.[35] Li H, Yang D, Ma L, et al.Risk factors associated with adjacent vertebral compression fracture following percutaneous vertebroplasty after menopause: A retrospective study.Med Sci Monit. 2017; 23:5271-5276.[36] Ye L, Liang, Jiang X, et al.Risk factors for the occurrence of insufficient cement distribution in the fractured area after percutaneous vertebroplasty in osteoporotic vertebral compression fractures. Pain Physician. 2018; 21(1):33-42.[37] 王拴池,王芳芳,陶晓冰.数字骨科分析 PVP 术后骨水泥弥散程度及其与临床疗效的关联性[J].实用骨科杂志, 2018,24(2):104-107.[38] Wang S,Wang H,Niu L.Clinical efficacy of pvp and pkp in the treatment of ovcfs after bilateral resection of ovarian cancer.Oncol Lett. 2018; 16(1):151-156.[39] Wang H, Sribastav S, Ye F, et al.Comparison of percutaneous vertebroplasty and balloon kyphoplasty for the treatment of single level vertebral compression fractures: A meta-analysis of the literature.Pain Physician.2015; 18(3):209-222.[40] Zhou T, Lin H, Wang H, et al.Comparative study on the biomechanics between improved pvp and traditional pkp in the treatment of vertebral peripheral wall damage-type ovcf. Exp Ther Med. 2017; 14(1):575-580.[41] Guo Z, Wang W, Gao W, et al. Comparison the clinical outcomes and complications of high-viscosity versus low-viscosity in osteoporotic vertebral compression fractures. Medicine(Baltimore). 2017; 96(48):e8936. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [3] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [4] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [5] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [6] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [7] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [8] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [9] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [10] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [11] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [12] | Wang Hao, Chen Mingxue, Li Junkang, Luo Xujiang, Peng Liqing, Li Huo, Huang Bo, Tian Guangzhao, Liu Shuyun, Sui Xiang, Huang Jingxiang, Guo Quanyi, Lu Xiaobo. Decellularized porcine skin matrix for tissue-engineered meniscus scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3473-3478. |
| [13] | Mo Jianling, He Shaoru, Feng Bowen, Jian Minqiao, Zhang Xiaohui, Liu Caisheng, Liang Yijing, Liu Yumei, Chen Liang, Zhou Haiyu, Liu Yanhui. Forming prevascularized cell sheets and the expression of angiogenesis-related factors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3479-3486. |
| [14] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| [15] | Liu Liyong, Zhou Lei. Research and development status and development trend of hydrogel in tissue engineering based on patent information [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3527-3533. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||