Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (8): 1214-1221.doi: 10.3969/j.issn.2095-4344.1084
Previous Articles Next Articles
Imaging evaluation and biomechanical characteristics of the novel intradiscal electrothermal annuloplasty in pigs
Shu Gao1, Chen Xiaodong2, Zhai Mingyu3, Li Quanxiu2, Liang Pengzhan3, Yang Xuejun2, Zhao Haibo2, Yu Chenqiang2, Bai Xueling4, Li Long4
-
Online:2019-03-18Published:2019-03-18 -
Contact:Chen Xiaodong, MD, Chief physician, Luohu District Hospital of Traditional Chinese Medicine, Shenzhen Luohu Hospital Group, Shenzhen 518000, Guangdong Province, China -
About author:Shu Gao, Master candidate, the Third Clinical Medical College of Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China -
Supported by:the Shenzhen Knowledge Innovation Program, No. JCYJ20150402162418740 (to CXD)
CLC Number:
Cite this article
Shu Gao, Chen Xiaodong, Zhai Mingyu, Li Quanxiu, Liang Pengzhan, Yang Xuejun, Zhao Haibo, Yu Chenqiang, Bai Xueling, Li Long. Imaging evaluation and biomechanical characteristics of the novel intradiscal electrothermal annuloplasty in pigs[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1214-1221.
share this article

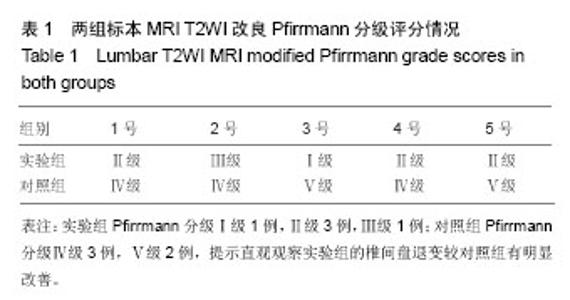
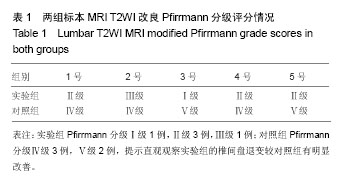
2.1 实验动物数量分析及一般情况 2组实验标本的体质量、雌雄性别、猪龄及术中出血量、手术时间伤口愈合时间比较差异无显著性意义(P > 0.05)。2组10只实验标本手术后均未死亡,术后未出现感染及重大疾病,各个实验动物进食良好、站立、行走、奔跑活动良好、手术切口愈合良好、尿便正常。 2.2 髓核摘除量的比较 实验组、对照组的髓核摘除量分别为(0.51±0.31) cm3及(0.48±0.38) cm3,行两独立样本t 检验,2组差异无显著性意义(t=0.14,P=0.89)。 2.3 X射线成像结果 10个标本均未发现脊柱的恶性病变;实验组的纤维环成形器均未出现松动、后退等情况,见图1。 2.4 螺旋CT检查成像结果 使用Simens公司64层螺旋CT配置的内置测量软件,测量手术节段L4/5的椎间隙高度,见图5。实验组的椎间隙高度与对照组比较差异有显著性意义(P < 0.05)。"

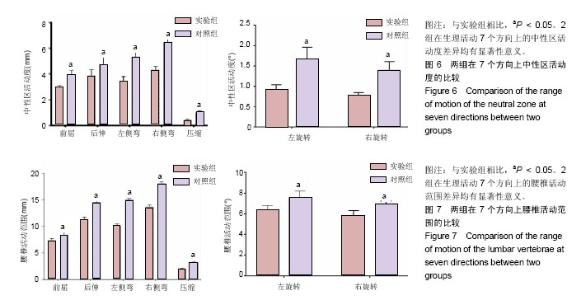
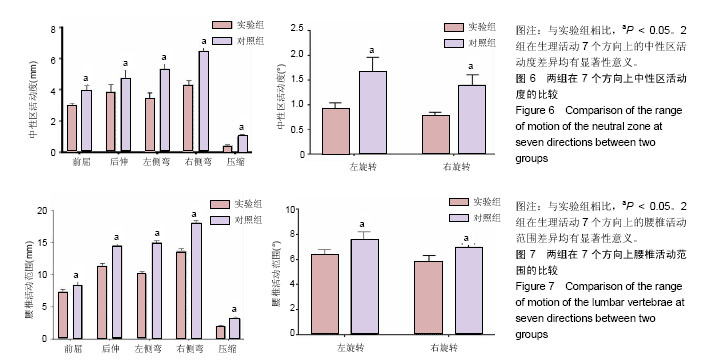
2.6 腰椎稳定性的生物力学加载结果 使用Instron E10000万能材料试验机对2组标本的生物力学进行测试,主要测试中性区活动度及腰椎活动范围。 中性区活动度:2组在生理活动的7个方向上的中性区活动度差异均有显著性意义(P < 0.05),实验组的中性区活动度较对照组小,见图6。说明实验组的腰椎稳定性较对照组好,提示纤维环成形器具有较好的维持中立位状态下腰椎稳定性的作用。 腰椎活动范围:2组在生理活动的7个方向上的腰椎活动范围差异均有显著性意义(P < 0.05),实验组的腰椎活动范围较对照组小,见图7。说明实验组的腰椎稳定性较对照组好,表示纤维环成形器具有较好的维持活动状态下腰椎稳定性的作用。"
| [1] 饶书城,宋跃明,主编.脊柱外科手术学[M]3版.北京:人民卫生出版社,2007: 466.[2] Herron L.Recurrent disc herniation: results of repeat laminectomy and discectomy.Spinal Disord. 1994;7(2):161-166.[3] Gerrit JB,Martin B,Darko L, et al.The high-risk discectomy patient: prevention of reherniation in patients with large anular defects using an anular closure device. Eur Spine J.2013;22:1030-1036.[4] Melrose J, Smith SM, Little CB, et al. Recent advances in annular pathobiology provide insights intorim-lesion mediated intervertebral disc degeneration and potential new approaches to annular repairstrategies.Eur Spine J. 2008;17(9):1131-1148.[5] Wang J, Tsai YY. The leakage pathway and effect of needle gauge on degree of disc injury post anuiarpuncture: a comparative study using aged human and adolescent porcine discs. Spine. 2007;32(17): 1809-1815.[6] 康然,黄桂成,李海声,等.纤维环切开法建立猪腰推间盘退变动物模型[J].实用老年医学,2012,2(2):141-145.[7] Wang YH, Kuo TF, Wang JL. The implantation of non-cell-based materials to prevent the recunrent discherniation: an in vivo porcine model using quantitative discomanometry examination. Eur Spine J. 2007; 16(7):1021-1027.[8] 陈晓东,白雪岭. 椎间盘的纤维环用修补器:中国, ZL 2014 2 0860497. X[P].2016-07-27. [9] 王宇鹏,银和平,吴一民,等.缝合和粘合两种方法修复山羊腰椎间盘纤维环缺损[J].中国组织工程研究,2018, 22(26): 4156-4161. [10] Panjabi MM. The stabilizing system of the spine. Part II. Neutral zone and instability pothesis. Spinal Disord. 1992;5(4):390-396; discussion 397.[11] Lequin MB, Barth M, Thome C, et al. Primary limited lumbar discectomy with an annulus closure device: one-year clinical and radiographic results from a prospective, multi-center study. Korean J Spine. 2012;9(4):340-347.[12] Pfirrmann CW, Metzdorf A ,Zanetti M, et al. Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine. 2001; 26 (17) :1873-1878.[13] 舒高,翟明玉,马鹏飞. 许莫氏结节在腰腿痛患者中的分布特点与腰椎间盘退变之间的关系[J].中国中医骨伤科杂志,2017,25(3):10-13.[14] Bouma GJ, Barth M, Ledic D, et al. The high-risk discectomy patient: prevention of reherniation in patients with large anular defects using an anular closure device. Eur Spine J. 2013;22(5):1030-1036.[15] Li Z, Liu H, Yang H, et al. Both expression of cytokines and posterior annulus fibrosus rupture are essential for pain behavior changes induced by degenerative intervertebral disc: An experimental study in rats. J Orthop Res. 2014; 32(2) :262-272.[16] Yin M, Mo W, Wu H, et al. Efficacy of caudal epidural steroid injection with targeted indwelling catheter and manipulation in managing patients with lumbar disk herniation and radiculopathy: a prospective, randomized, single-blind controlled trial. World Neurosurg. 2018;114: e29-e34.[17] Mariconda M, Galasso O, Attingenti P, et al. Frequency and clinical meaning of long-term degenerative changes after lumbar discectomy visualized on imaging tests. Eur Spine J. 2010;19(1):136-143.[18] McGirt MJ, Ambrossi GL, Datoo G, et al. Recurrent disc herniation and long-term back pain after primary lumbar discectomy: review of outcomes reported for limited versus aggressive disc removal.Neurosurgery. 2009;64(2):338-344; discussion 344-345.[19] Barth M, Diepers M, Weiss C, et al. Two-year outcome after lumbar microdiscectomy versus microscopic sequestrectomy:part 2: radiographic evaluation and correlation with clinical outcome. Spine. 2008;33(3):273-279.[20] Gao SG, Lei GH, He HB, et al. Biomechanical comparison of lumbar total disc arthroplasty, discectomy, and fusion: effect on adjacentlevel disc pressure and facet joint force. J Neurosurg Spine. 2011;15(5): 507-514.[21] Shahadi F, Luecke M, Preuss M, et al. Measurement of intradiscal pressure after lumbar discectomy.Zentralbl Neurochir. 2008;69(2): 87-89.[22] Chen YC, Lee SH, Chen D. Intradiscal pressure study of percutaneous disc decompression with nucleoplasty in human cadavers.Spine. 2003;28(7):661-665.[23] Steffen T, Baramki HG, Rubin R, et al. Lumbar intradiscal pressure measured in the anterior and posterolateral annular regions during asymmetrical loading. Clin Biomech (Bristol, Avon). 1998;13(7): 495-505.[24] Adams MA, McNally DS, Dolan P. ‘Stress’ distributions inside intervertebral discs. The effects of age and degeneration. J Bone Joint Surg Br. 1996;78(6):965-972.[25] Trummer M, Eustacchio S, Barth M, et al. Protecting facet joints post-lumbar discectomy: Barricaid annular closure device reduces risk of facet degeneration. Clin Neurol Neurosurg. 2013;115(8):1440-1445.[26] Parker SL, Grahovac G, Vukas D, et al. Effect of an annular closure device(Barricaid) on same level recurrent disc herniation and disc height loss after primary lumbar discectomy:two-year results of a multi-center prospective cohort study. Clin Spine Surg. 2016; 29(10): 454-460.[27] Haefell M, Kalberer F, Saegesser D, et al. The course of macroscopic degeneration In the human lumbar intervertebral discs. Spine. 2006;31(14) : 1522-1531.[28] Gregory DE, Callaghan JP. A comparison of uniaxial and biaxial mechanical properties of the annulus fibrosus: a porcine model. J Biomech Eng. 2011;133(2) : 1-5.[29] Lisi AJ, O’Neill CW, Lindsey DP, et al. Measurement of in vivo lumbar intervertebral disc pressure during spinal manipulation: a feasibility study. J Appl Biomech.2006;22(3):234-239.[30] Heuer F, Ulrich S, Claes L, et al. Biomechanical evaluation of conventional anulus fibrosus closure methods required for nucleus replacement. Laboratory investigation. J Neurosurg Spine. 2008;9(3): 307-313.[31] Chiang CJ, Cheng CK, Sun JS, et al. The effect of a new anular repair after discectomy in intervertebral disc degeneration: an experimental study using a porcine spine model. Spine. 2011;36(10):761-769.[32] Wilke HJ, Ressel L, Heuer F, et al. Can prevention of a reherniation be investigated? Establishment of a herniation model and experiments with an anular closure device. Spine. 2013;38(10):E587-E593. |
| [1] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [2] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [3] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [4] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [5] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Multiple problems in the selection of implants for patellar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1440-1445. |
| [6] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [7] | Xu Yulin, Shen Shi, Zhuo Naiqiang, Yang Huilin, Yang Chao, Li Yang, Zhao Heng, Zhao Lu. Biomechanical comparison of three different plate fixation methods for acetabular posterior column fractures in standing and sitting positions [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 826-830. |
| [8] | Cai Qunbin, Zou Xia, Hu Jiantao, Chen Xinmin, Zheng Liqin, Huang Peizhen, Lin Ziling, Jiang Ziwei. Relationship between tip-apex distance and stability of intertrochanteric femoral fractures with proximal femoral anti-rotation nail: a finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 831-836. |
| [9] | Zhang Wei, Hu Jiang, Tang Liuyi, Wan Lun, Yu Yang, Lin Shu, Tang Zhi, Wang Fei. Advantages of robot assisted percutaneous biopsy in the diagnosis of spinal lesions [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 844-848. |
| [10] | Song Chengjie, Chang Hengrui, Shi Mingxin, Meng Xianzhong. Research progress in biomechanical stability of lateral lumbar interbody fusion [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 923-928. |
| [11] | Xie Chongxin, Zhang Lei. Comparison of knee degeneration after anterior cruciate ligament reconstruction with or without remnant preservation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 735-740. |
| [12] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [13] | Fu Shuanhu, Qin Kai, Lu Dahan, Qin Haibiao, Gu Jin, Chen Yongxi, Qin Haoran, Wei Jiading, Wu Liang, Song Quansheng. Lumbar spinal tuberculosis implanted with artificial bone with streptomycin sulfate and percutaneous pedicle screw under transforaminal endoscopy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 493-498. |
| [14] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [15] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||