Chinese Journal of Tissue Engineering Research ›› 2018, Vol. 22 ›› Issue (26): 4174-4178.doi: 10.3969/j.issn.2095-4344.0939
Previous Articles Next Articles
Arthroscopic reconstruction for acute and chronic anterior cruciate ligament injuries using autologous or allogeneic tendon graft: an evaluation of reconstruction effects
Xiang Shan-shan1, Fu Ming2, Zhang Zhi-qi2, Yang Zi-bo2, Chen Zhong-xian1
- 1Department of Orthopaedics, Jiangmen Hospital of Sun Yat-sen University, Jiangmen 529000, Guangdong Province, China; 2Department of Joint Surgery, First Affiliated Hospital of Sun Yat-sen University, Guangzhou 510080, Guangdong Province, China
-
Received:2018-03-02 -
Contact:Fu Ming, Chief physician, Professor, Department of Joint Surgery, First Affiliated Hospital of Sun Yat-sen University, Guangzhou 510080, Guangdong Province, China -
About author:Xiang Shan-shan, Master, Attending physician, Department of Orthopaedics, Jiangmen Hospital of Sun Yat-sen University, Jiangmen 529000, Guangdong Province, China
CLC Number:
Cite this article
Xiang Shan-shan, Fu Ming, Zhang Zhi-qi, Yang Zi-bo, Chen Zhong-xian. Arthroscopic reconstruction for acute and chronic anterior cruciate ligament injuries using autologous or allogeneic tendon graft: an evaluation of reconstruction effects[J]. Chinese Journal of Tissue Engineering Research, 2018, 22(26): 4174-4178.
share this article
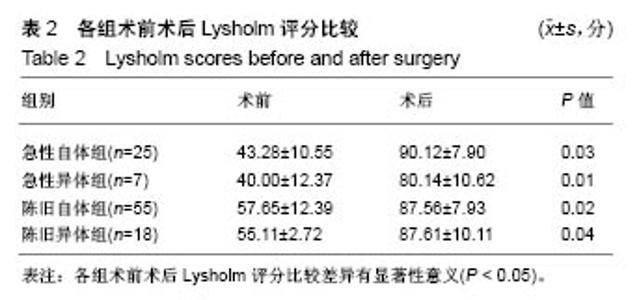
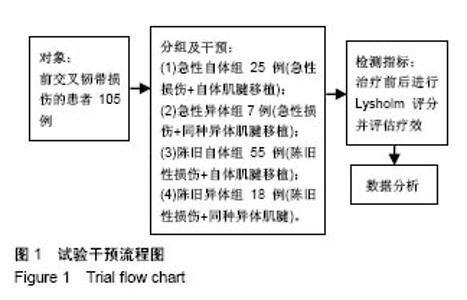
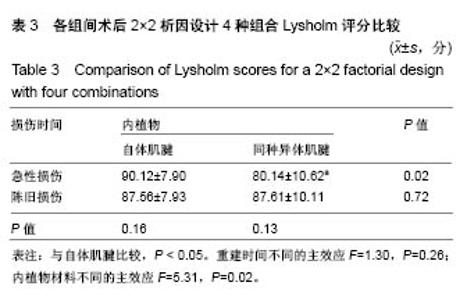
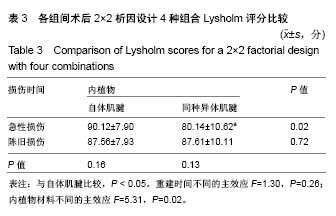
2.2 膝关节功能变化 各组手术前后Lysholm评分,见表2;各组间术后2×2析因设计4种组合Lysholm评分,见表3。 术后4组间根据析因设计的方差分析得到:①重建时间不同的主效应无显著性意义(F=1.30,P=0.26),急性损伤和陈旧性损伤的前交叉韧带重建后Lysholm评分无差异;②内植物材料不同的主效应有显著性意义(F=5.31,P=0.02),自体肌腱重建患者术后Lysholm评分高于异体肌腱重建患者;③重建时间和内植物材料的交互效应有显著性意义(F=5.41,P=0.02),此时各因素主效应已无实际意义。进一步做各因素的单独效应分析:①急性损伤时,使用自体肌腱和同种异体肌腱评分差异有显著性意义(P=0.02);②陈旧性损伤时,使用自体肌腱和同种异体肌腱评分差异无显著性意义(P=0.72);③使用自体肌腱时,急性损伤和陈旧性损伤评分差异无显著性意义(P=0.16);④使用异体肌腱时,急性损伤和陈旧性损伤评分差异无显著性意义(P=0.13)。 2.3 不良反应、排异反应及生物相容性分析 手术后主要的不良反应有伤口感染、下肢深静脉血栓及异体肌腱的排异反应(相关病例均予以排除,未纳入研究),虽然异体肌腱广泛使用深低温冷冻及射线照射处理,但未能完全消除其排斥反应的发生率。"
| [1] Hurd WJ, Axe MJ, Snyder-Mackler L. Influence of age, gender, and injury mechanism on the development of dynamic knee stability after acute ACL rupture. J Orthop Sports Phys Ther. 2008;38(2):36-41. [2] Renstrom P, Ljungqvist A, Arendt E, et al. Non-contact ACL injuries in female athletes: an International Olympic Committee current concepts statement. Br J Sports Med. 2008;42(6):394-412.[3] Anderson AF, Anderson CN. Correlation of meniscal and articular cartilage injuries in children and adolescents with timing of anterior cruciate ligament reconstruction. Am J Sports Med. 2015;43(2):275-281.[4] Anstey DE, Heyworth BE, Price MD, et al. Effect of timing of ACL reconstruction in surgery and development of meniscal and chondral lesions. Phys Sports Med. 2012;40(1):36-40.[5] Li B, Bai L, Fu Y, et al. Effect of timing of surgery in partially injured ACLs. Orthopedics. 2012;35(5):408-412.[6] Herbst E, Hoser C, Gfoller P, et al. Impact of surgical timing on the outcome of anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc. 2017;25(2):569-577.[7] Mook WR, Miller MD, Diduch DR, et al. Multiple-ligament knee injuries: a systematic review of the timing of operative intervention and postoperative rehabilitation. J Bone Joint Surg Am. 2009;91(12):2946-2957.[8] Brambilla L, Pulici L, Carimati, et al. Prevalence of associated lesions in anterior cruciate ligament reconstruction: correlation with surgical timing and with patient age, sex, and body mass index. Am J Sports Med. 2015;43(12):2966-2973.[9] Kwok CS, Harrison T, Servant C. The optimal timing for anterior cruciate ligament reconstruction with respect to the risk of postoperative stiffness. Arthroscopy. 2013;29(3): 556-565.[10] Krutsch W, Zellner J, Baumann F, et al. Timing of anterior cruciate ligament reconstruction within the first year after trauma and its influence on treatment of cartilage and meniscus pathology. Knee Surg Sports Traumatol Arthrosc. 2017;25(2):418-425.[11] Camp CL, Lebaschi A, Cong GT, et al. Timing of postoperative mechanical loading affects healing following anterior cruciate ligament reconstruction: analysis in a murine model. J Bone Joint Surg Am. 2017;99(16):1382-1391.[12] Kennedy J, Jackson MP, O'Kelly P, et al. Timing of reconstruction of the anterior cruciate ligament in athletes and the incidence of secondary pathology within the knee. J Bone Joint Surg Br. 2010;92(3):362-366.[13] Andernord D, Karlsson J, Musahl V, et al. Timing of surgery of the anterior cruciate ligament. Arthroscopy. 2013;29(11): 1863-1871.[14] Chong RW, Tan JL. Rising trend of anterior cruciate ligament injuries in females in a regional hospital. Ann Acad Med Singapore. 2004;33(3):298-301.[15] Kaeding CC, Aros B, Pedroza A, et al. Allograft versus autograft anterior cruciate ligament reconstruction: predictors of failure from a moon prospective longitudinal cohort. Sports Health. 2011;3(1):73-81.[16] Rice RS, Waterman BR, Lubowitz JH. Allograft versus autograft decision for anterior cruciate ligament reconstruction: an expected-value decision analysis evaluating hypothetical patients. Arthroscopy. 2012;28(4):539-547.[17] Hu J, Qu J, Xu D et al. Allograft versus autograft for anterior cruciate ligament reconstruction: an up-to-date meta-analysis of prospective studies. Int Orthop. 2013;37(2):311-320.[18] Aslan A, Ozer O, Baydar ML, et al. Anterior cruciate ligament injuries: does surgical treatment with autograft versus allograft option affect the clinical results? Ulus Travma Acil Cerrahi Derg. 2012;18(2):153-161.[19] Paschos NK, Howell SM. Anterior cruciate ligament reconstruction: principles of treatment. EFORT Open Reviews. 2016;1(11):398-408.[20] Kane PW, Wascher J, Dodson CC, et al. Anterior cruciate ligament reconstruction with bone-patellar tendon-bone autograft versus allograft in skeletally mature patients aged 25 years or younger. Knee Surg Sports Traumatol Arthrosc. 2016; 24(11):3627-3633.[21] Sun K, Zhang J, Wang Y, et al. Arthroscopic anterior cruciate ligament reconstruction with at least 2.5 years’ follow-up comparing hamstring tendon autograft and irradiated allograft. Arthroscopy. 2011;27(9):1195-1202.[22] Islam MZ, Rahman M, Ali ME, et al. Arthroscopic anterior cruciate ligament reconstruction with triplet autograft of semitendinosus tendon. Mymensingh Med J. 2017;26(3): 545-550.[23] Wasserstein D, Sheth U, Cabrera A, et al. A systematic review of failed anterior cruciate ligament reconstruction with autograft compared with allograft in young patients. Sports Health. 2015;7(3):207-216.[24] Barrera Oro F, Sikka R, Wolters B, et al. Autograft versus allograft: an economic cost comparison of anterior cruciate ligament reconstruction. Arthroscopy. 2011;27(9):1219-1225.[25] Bottoni CR, Smith EL, Shaha J, et al. Autograft versus allograft anterior cruciate ligament reconstruction: a prospective, randomized clinical study with a minimum 10-year follow-up. Am J Sports Med. 2015;43(10):2501-2509.[26] Zeng C, Gao S, Li H, et al. Autograft versus allograft in anterior cruciate ligament reconstruction: a meta-analysis of randomized controlled trials and systematic review of overlapping systematic reviews. Arthroscopy. 2016;32(1): 153-163.[27] Mariscalco MW, Magnussen RA, Mehta D, et al. Autograft versus nonirradiated allograft tissue for anterior cruciate ligament reconstruction: a systematic review. Am J Sports Med. 2014;42(2):492-499.[28] Engelman GH, Carry PM, Hitt KG, et al. Comparison of allograft versus autograft anterior cruciate ligament reconstruction graft survival in an active adolescent cohort. Am J Sports Med. 2014;42(10):2311-2318.[29] Jia YH, Sun PF. Comparison of Clinical Outcome of Autograft and Allograft Reconstruction for Anterior Cruciate Ligament Tears. Chin Med J. 2015;128(23):3163-3166.[30] Yang R, Deng H, Hou J, et al. Comparison of Knee Stability and Synovial Fluid Alterations in Anterior Cruciate Ligament Reconstruction With a Hamstring Autograft or an Allograft. Orthopedics. 2017;40(15):e892-e897.[31] Cooper MT, Kaeding C. Comparison of the hospital cost of autograft versus allograft soft-tissue anterior cruciate ligament reconstructions. Arthroscopy. 2010;26(11):1478–1482.[32] Cvetanovich GL, Mascarenhas R, Saccomanno MF, et al. Hamstring autograft versus soft-tissue allograft in anterior cruciate ligament reconstruction: a systematic review and meta-analysis of randomized controlled trials. Arthroscopy. 2014;30(12):1616-1624.[33] Mascarenhas R, Erickson BJ, Sayegh ET, et al. Is there a higher failure rate of allografts compared with autografts in anterior cruciate ligament reconstruction: a systematic review of overlapping meta-analyses. Arthroscopy. 2015;31(2): 364-372.[34] Noyes FR, Barber-Westin SD. Posterior cruciate ligament allograft reconstruction with and without a ligament augmentation device. Arthroscopy. 1994;10(4):371-382.[35] 冯华,洪雷,耿向苏,等.前十字韧带损伤合并内侧半月板ramp损伤[J].中华骨科杂志,2005,25(11):651-655.[36] Mccarthy M, Mallett K, Abola M, et al. Hospital for special surgery ACL registry: 2-year outcomes suggest low revision and return to OR rates. HSS J. 2017;13(2):119-127.[37] Sklenský J, Vališ P, Repko M, et al. The Use of BTB Allograft in Revision Reconstruction of the Anterior Cruciate Ligament and Its Success Rate in Terms of Subjective Patient Satisfaction. Acta Chir Orthop Traumatol Cech. 2017;84(2): 106-113.[38] Catterall JB, Stabler TV, Flannery CR, et al. Changes in serum and synovial fluid biomarkers after acute injury (NCT00332254). Arthritis Res Ther. 2010;12(6):R229.[39] 林子洪,傅明,康焱,等.前交叉韧带切除后股骨关节软骨变化的初步实验研究[J].中华关节外科杂志(电子版),2008,2(5):554-565.[40] Jackson DW, Corsetti J, Simon T M. Biologic incorporation of allograft anterior cruciate ligament replacements. Clin Orthop Relat Res. 1996;(324):126-133.[41] Malinin TI, Levitt RL, Bashore C. A study of retrieved allografts used to replace anterior cruciate ligaments. Arthroscopy. 2002;18(2):163-170.[42] Jaureguito JW, Paulos LE. Why grafts fail. Clin Orthop Relat Res. 1996;(325):25-41. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [3] | Liu Shaohua, Zhou Guanming, Chen Xicong, Xiao Keming, Cai Jian, Liu Xiaofang. Influence of anterior cruciate ligament defect on the mid-term outcome of fixed-bearing unicompartmental knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 860-865. |
| [4] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [5] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [6] | Ma Ziyue, Ju Xiaochen, Zhang Lei, Sun Rongxin. Tendon-bone healing in anterior cruciate ligament reconstruction with and without remnant preservation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 582-587. |
| [7] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [8] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [9] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [10] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [11] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [12] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [13] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [14] | Wang Hao, Chen Mingxue, Li Junkang, Luo Xujiang, Peng Liqing, Li Huo, Huang Bo, Tian Guangzhao, Liu Shuyun, Sui Xiang, Huang Jingxiang, Guo Quanyi, Lu Xiaobo. Decellularized porcine skin matrix for tissue-engineered meniscus scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3473-3478. |
| [15] | Mo Jianling, He Shaoru, Feng Bowen, Jian Minqiao, Zhang Xiaohui, Liu Caisheng, Liang Yijing, Liu Yumei, Chen Liang, Zhou Haiyu, Liu Yanhui. Forming prevascularized cell sheets and the expression of angiogenesis-related factors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3479-3486. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||