Chinese Journal of Tissue Engineering Research
Previous Articles Next Articles
Frictional force of different ligations with NiTi archwires of different sizes
Ma Xiao-zhou1, Li Hong-fa1, Zhao Yan-hong1, Wu Jie1, Zhang Ming-can2, Zhao Wei1
- 1Department of Orthodontics, Stomatological Hospital of Tianjin Medical University, Tianjin 300070, China; 2Stomatological Hospital of Tanggu, Tianjin 300450, China
-
Received:2018-05-31Online:2018-08-08Published:2018-08-08 -
Contact:Li Hong-fa, Chief physician, Department of Orthodontics, Stomatological Hospital of Tianjin Medical University, Tianjin 300070, China -
About author:Ma Xiao-zhou, Master candidate, Department of Orthodontics, Stomatological Hospital of Tianjin Medical University, Tianjin 300070, China -
Supported by:the Scientific Support Project of the Health Department of Binhai New Area of Tianjin, No. 2013Bwky023; the Scientific Research Foundation of the Stomatological Hospital of Tianjin Medical University, No. 2014YKYQ02
CLC Number:
Cite this article
Ma Xiao-zhou, Li Hong-fa, Zhao Yan-hong, Wu Jie, Zhang Ming-can, Zhao Wei. Frictional force of different ligations with NiTi archwires of different sizes[J]. Chinese Journal of Tissue Engineering Research, doi: 10.3969/j.issn.2095-4344.0916.
share this article
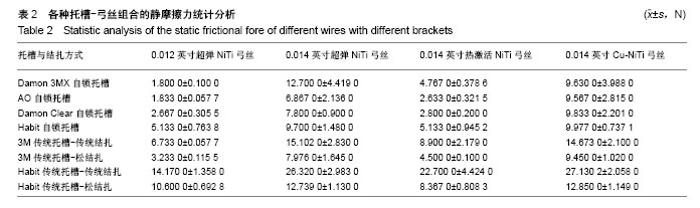
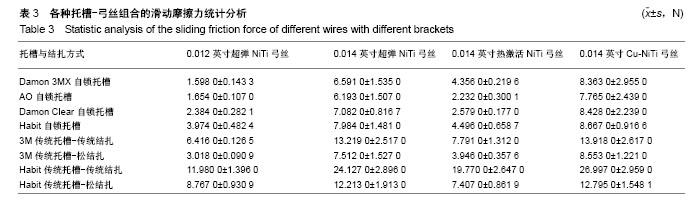
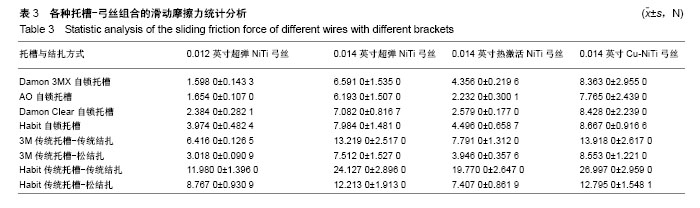
2.1 不同弓丝与不同托槽组合的最大静摩擦力和滑动摩擦力 在8种入槽方式下,使用弓丝A的静摩擦力和滑动摩擦力由低到高的顺序为:1<2<3<6<4<5<8<7,弓丝B为:2<1<3<6<4<8<5<7,弓丝C为:2<3<6<1<4<8<5<7,弓丝D为:2<1<3<6<4<8<5<7。每组弓丝的8种入槽方式排列顺序有相似之处,当使用A,B,D三种弓丝时,金属托槽松结扎的摩擦力都较金属主被动自锁托槽及陶瓷被动自锁托槽的摩擦力大;使用弓丝C时,金属托槽松结扎的摩擦力仅仅大于主动自锁金属托槽及被动自锁陶瓷托槽,可见热激活弓丝可更好地降低松结扎技术的摩擦力,而其在被动自锁金属托槽中的摩擦力较大。在陶瓷托槽范围内,无论哪种弓丝入槽,主动自锁陶瓷托槽的摩擦力都较小,不同的是弓丝尺寸的影响,0.012英寸弓丝在单晶体托槽松结扎下的摩擦力较金属托槽传统结扎的摩擦力大,而0.014英寸弓丝入槽,不论哪种材质,两者的顺序刚好相反。4种弓丝中,弓丝B与弓丝D在8种入槽方式下摩擦力的大小顺序相同(表2)。 4组弓丝在1-7入槽方式下的静摩擦力和滑动摩擦力由小到大依次为:A<C<B<D,只有在第8种入槽方式下的顺序为C<A<B<D。金属托槽松结扎为第6组,非金属托槽松结扎为第8组,说明在进行金属托槽松结扎时,弓丝尺寸较小更占优势,在使用非金属托槽松结扎时,即使弓丝较粗,热激活弓丝更占优势,Cu-NiTi弓丝在两种松结扎方式下的摩擦力都较大(表3)。 此类比较只能看到基本的大小关系,但每种组合之间是否有明显差异待后文研究。"
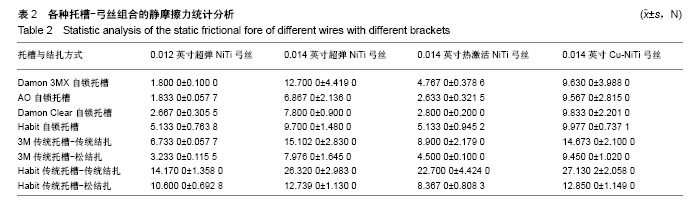
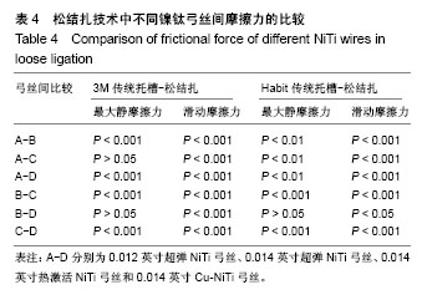
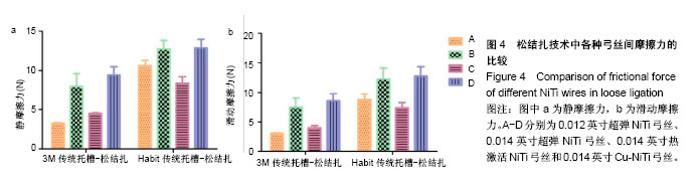
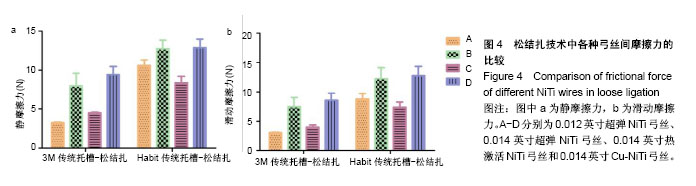
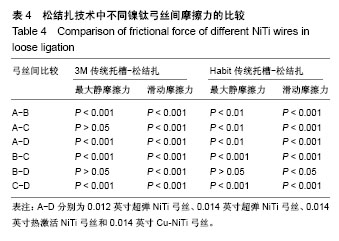
2.2 松结扎中不同镍钛弓丝的摩擦力差异 不同镍钛弓丝在金属托槽松结扎中的两两比较,A与C、B与D的最大静摩擦力无明显差异(P > 0.05),滑动摩擦力两两比较均有明显区别(P < 0.001)。 不同镍钛弓丝在单晶体托槽松结扎中的两两比较,B与D的最大静摩擦力比较无差异(P > 0.05),滑动摩擦力两两比较均不同,B与D两种弓丝比较统计学差异为P < 0.05,其他比较统计学差异为P < 0.001,说明0.014英寸超弹NiTi丝和0.014英寸Cu-NiTi的摩擦力差异较小,见表4、图4。 结合前文可得到,金属托槽松结扎技术中应用4种弓丝的滑动摩擦力大小为:A<C<B<D,非金属托槽松结扎下为:C<A<B<D,前后顺序都有统计学意义,每种弓丝的摩擦力与其他弓丝比较都有差异,不可被代替。"
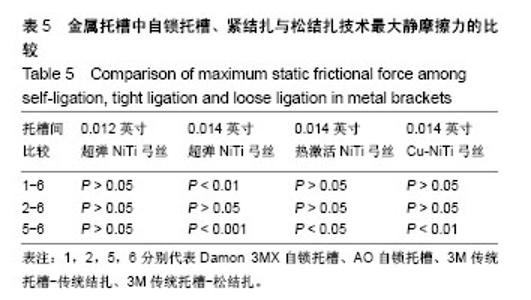
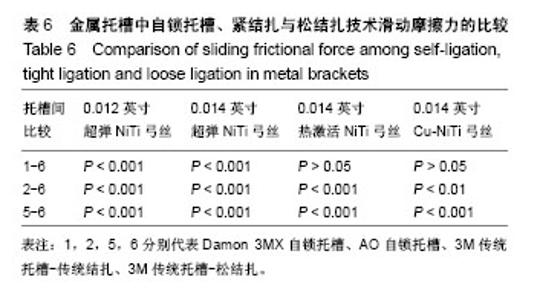
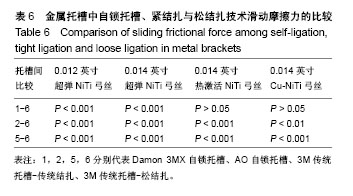
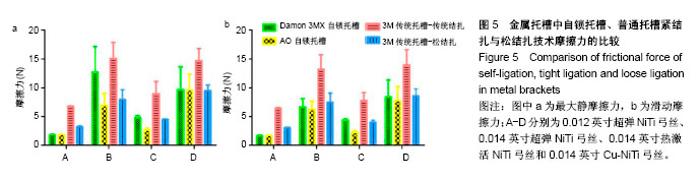
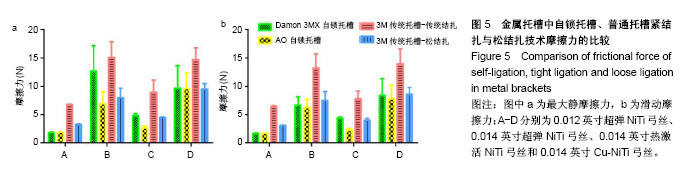
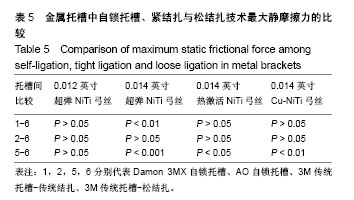
2.3 传统金属托槽松结扎的摩擦力分析 最大静摩擦力:使用A,C,D三种弓丝时,普通金属托槽松结扎与自锁托槽的摩擦力比较无差异(P > 0.05)。弓丝B入槽后,主动自锁托槽和普通金属托槽松结扎之间的摩擦力比较无差异(P > 0.05),但被动自锁托槽和普通金属托槽松结扎的摩擦力比较有差异(P < 0.01)。使用B,C,D弓丝时,普通金属传统结扎和松结扎的摩擦力比较有差异(P < 0.05),在使用弓丝B时的差异性更明显(P < 0.001)。使用弓丝A时,普通金属传统结扎和松结扎的摩擦力比较无明显差异(P > 0.05)。 滑动摩擦力:选用4组弓丝中任何一组,普通金属托槽松结扎和传统结扎及主动自锁托槽的摩擦力两两比较均有差异(P < 0.01);使用弓丝A,B时,被动自锁托槽和普通金属松结扎技术的摩擦力比较有差异;使用弓丝C,D时,被动自锁托槽和普通金属托槽松结扎技术的摩擦力比较无差异。 比较结果说明,普通金属托槽松结扎技术的最大静摩擦力与自锁托槽相似;使用任一弓丝时,普通金属托槽松结扎与主动自锁金属托槽的滑动摩擦力比较差异均有显著性意义(P < 0.01)。使用弓丝C,D时,普通金属托槽松结扎与与被动自锁金属托槽的滑动摩擦力比较差异无差异(P > 0.05),C,D弓丝分别是热激活NiTi弓丝和含铜NiTi弓丝,这两种弓丝在被动自锁托槽和传统托槽松结扎两种入槽方式下的摩擦力值相似,见表5、表6、图5。 结合前文排序结果:使用弓丝A时,摩擦力大小1<2<6<5;弓丝B入槽时,摩擦力大小2<1<6<5;弓丝C入槽时,摩擦力大小2<6<1<5;使用弓丝D时,摩擦力大小2<1<6<5,说明使用弓丝A,B时,自锁托槽、传统金属托槽松结扎和传统金属托槽传统结扎的摩擦力大小有差异,主被动自锁托槽的摩擦力经Meta分析得出无差异[9],可得出弓丝A,B在不同入槽方式下的摩擦力排序一致;使用弓丝C,D时,被动自锁托槽和普通金属托槽松结扎的摩擦力比较无明显差异,可理解为弓丝C,D在不同入槽方式下的摩擦力排序相同。前文得到弓丝B,D入槽后按摩擦力大小的排序一致,经统计学分析发现两者有差异,使用弓丝B时,1和6的摩擦力比较有差异;使用弓丝D时,1和6的摩擦力无差异。"
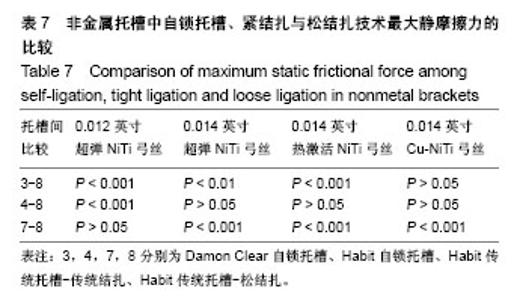
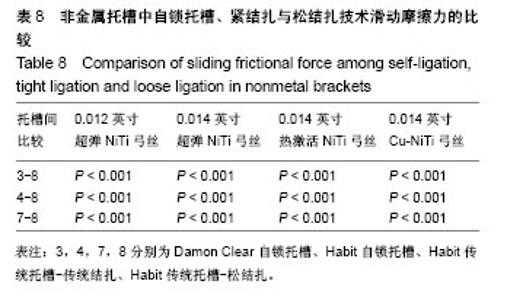
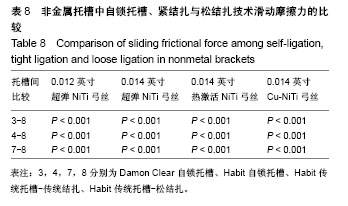
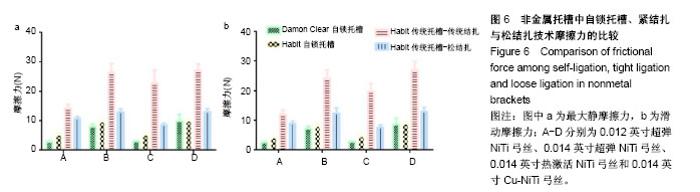
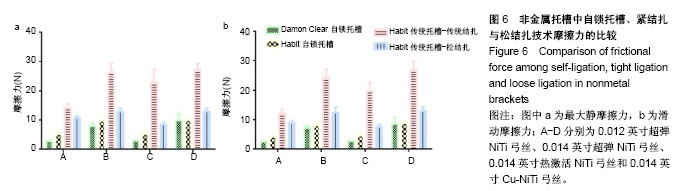
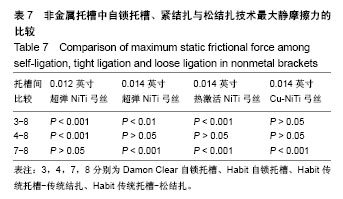
2.4 普通非金属托槽松结扎的摩擦力分析 最大静摩擦力:使用弓丝A,B,C时,普通非金属托槽松结扎与被动自锁陶瓷的摩擦力相比有差异(P < 0.01);使用弓丝D时,普通非金属托槽松结扎与被动自锁陶瓷的摩擦力相比无差异(P > 0.05);使用弓丝B,C,D时,单晶体托槽松结扎与主动自锁陶瓷托槽的摩擦力相比无差异 (P > 0.05),只有使用弓丝A时两者摩擦力比较有差异(P < 0.001);使用弓丝A时,普通非金属托槽松结扎与传统结扎的摩擦力比较无差异(P > 0.05);使用弓丝B,C,D时,普通非金属托槽松结扎与传统结扎的摩擦力比较有差异(P < 0.001)。 滑动摩擦力:使用任一弓丝时,单晶体托槽松结扎与主被动自锁托槽、单晶体托槽传统结扎的摩擦力比较差异均有显著性意义(P < 0.001)。 滑动摩擦力相对最大静摩擦力是主要影响牙齿移动快慢的因素[2],前文提到这4组入槽方式下,4种弓丝摩擦力的大小顺序都为3<4<8<7,可得出单晶体托槽松结扎技术的摩擦力较其传统结扎的摩擦力低,但无法达到自锁托槽,水平,见表7、表8、图6。"
| [1] 郭杰.临床结扎力量与口内托槽沿不锈钢弓丝滑动的摩擦力[J].国外医学:口腔医学分册,2004,31(4):328.[2] 林新平.临床口腔正畸生物力学机制解析[M].北京:人民卫生出版社,2012:106.[3] Shivapuja PK,Berger J.A comparative study of conventional ligation and self-ligationbracket systems.Am J Orthod Dentofacial Orthop.1994;106(5):472-480.[4] Kusy RP,Whitley JQ.Friction between different wire-bracketconfigurations and materials//Seminars in orthodontics.WB Saunders,1997;3(3):166-177.[5] 张明灿,李洪发,武杰等.松结扎在正畸排齐阶段的初步研究[J].中国美容医学,2014,23(8):655-658.[6] 张明灿,赵丽丽,孙海媛,等.不锈钢结扎丝松结扎法在口腔正畸固定矫治术中的应用体会[J].山东医药,2015,55(26):106-107.[7] 段沛沛,张林,赵青,等.自锁托槽矫治系统相关生物力学的研究进展[J].国际口腔医学杂志,2012,39(5): 661-663.[8] 刘刚,杨丽,刘斌,等.口腔正畸摩擦研究进展[J].摩擦学学报, 2018, 38(2):238-246.[9] Papageorgiou SN,Konstantinidis I,Papadopoulou K,et al.A systematic review and meta—analysis of experimental clinical evidence on initial aligning archwires and archwire sequences.Orthod Craniofac Res.2014;17(4):197-215.[10] 林新平.临床口腔正畸生物力学机制解析[M].北京:人民卫生出版社,2012:102.[11] 张昊,王林,马俊青.口腔正畸弓丝表面改性技术的研究进展[J].口腔生物医学,2013,4(4):209-213.[12] 蔡先彬.复合工艺聚四氟乙烯涂层的摩擦学研究[D].苏州大学, 2016.[13] 邵玶,隋解和,冯雪,等.TiNi 合金牙弓丝表面环氧树脂/聚四氟乙烯涂层的组织结构与性能[J].稀有金属材料与工程, 2012,41(5): 822-825.[14] Farronato G,Maijer R,Carìa MP,et al.The effect of Teflon coating on the resistance to sliding of orthodontic archwires. Eur J Orthod.2011;34(4):410-417.[15] 白雪芹,曾祥龙.低摩擦结扎圈在牙齿排齐阶段静摩擦力的实验研究[J].口腔正畸学,2008,15(2):78-80.[16] Henao SP,Kusy RP.Evaluation of the frictional resistance of conventional and self-ligating bracket designs using standardized archwires and dental typodonts.Angle Orthod. 2004;74(2): 202-211.[17] 张丽雯,宋立滨,张瑾,等.不同托槽与弓丝组合滑动摩擦力的实验研究[J].中华口腔正畸学杂志,2017,24(1):10-13.[18] Thorstenson GA,Kusy RP.Comparison of resistance to sliding between different self-ligating brackets with second-order angulation in the dry and saliva states.Am J Orthod Dentofacial Orthop. 2002;121(5):472-482.[19] 杨慧芳,赵建江,王勇.3D打印技术在口腔医学领域中的应用[J].中国医疗设备,2015,30(5):63-65.[20] Kasparova M,Grafova L,Dvorak P,et al.Possibility of reconstruction of dental plaster cast from 3D digital study models. Biomed Eng Online.2013;12(1):49.[21] Tavares A,Braga E,Araújo TM,et al.Digital models: How can dental arch form be verified chairside?Dental Press J Orthod. 2017;22(6):68-73.[22] Darroudi AM,Kuijpersjagtman AM,Ongkosuwito EM,et al.Accuracy of a computed tomography scanning procedure to manufacture digital models.Am J Orthod Dentofacial Orthop.2017;151(5):995-1003.[23] Majstorovic N,Zivkovic S,Glisic B.The advanced model definition and analysis of orthodontic parameters on 3D digital models.Srp Arh Celok Lek.2017;145(11-12):11.[24] 冯全胜,马笮,徐文秀,等.口腔3D打印模型与传统石膏模型精确性对比研究[J].中国老年保健医学,2015,13(3):80-81.[25] Alcan T,Ceylano?lu C,Baysal B.The relationship between digital model accuracy and time-dependent deformation of alginate impressions.Angle Orthod.2009;79(1):30-36.[26] Torassian G,Kau CH,English JD,et al.Digital models vs plaster models using alginate and alginate substitute materials.Angle Orthodontist.2010;80(4):474-481.[27] 李晶,王硕,张达,等.口内扫描数字化模型与硅橡胶制取石膏模型测量的对比研究[J].中华口腔正畸学杂志, 2013,20(3):163-166.[28] Hwang CJ,Shin JS,Cha JY.Metal release from simulated fixed orthodontic appliances.Am J Orthod Dentofacial Orthop.2001; 120(4):383-391.[29] 王天丛,陈文静,王文梅,等.单晶和多晶陶瓷托槽与金属弓丝摩擦力的对比研究[J].口腔医学,2013,33(12):821-823.[30] Thomas S,Sherriff M,Birnie D.A comparative in vitro study of the frictional characteristics of two types of self-ligating brackets and two types of pre-adjusted edgewise brackets tied with elastomeric ligatures.Eur J Orthod. 998;20(5): 589-596.[31] Kapur R,Sinha PK,Nanda RS.Frictional resistance of the Damon SL bracket.J Clin Orthod. 1998;32(8):485.[32] Pizzoni L,Ravnholt G,Melsen B.Frictional forces related to self-ligating brackets.Eur J Orthod.1998;20(3):283-291.[33] Peososki RR,Bagby MD,Erick LC.Static frictional force and surface roughnessof nickel-titanium arch wires.Am J Orthod. 1991;100(4):341-348.[34] 王娅婷,王军.自锁托槽与传统托槽的临床比较[J].国际口腔医学杂志,2010,37(4):492-495.[35] 顾月光,赵春洋,马俊青,等.主动、被动自锁托槽摩擦力的meta分析研究[J].口腔医学,2012,32(5):257-262.[36] Offenbacher S,Beck JD,Moss K,et al.Results from the Periodontitis and Vascular Events (PAVE) Study: a pilot multicentered, randomized, controlled trial to study effects of periodontal therapy in a secondary prevention model of cardiovascular disease.J Periodontol.2009;80(2):190-201.[37] Queiroz GV,Ballester RY,De Paiva JB,et al.Comparative study of frictional forces generated by NiTi archwire deformation in different orthodontic brackets: In vitro evaluation.Dental Press J Orthod.2012;17(4):45-50. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [3] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [4] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [5] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [6] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [7] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [8] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [9] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [10] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [11] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [12] | Wang Hao, Chen Mingxue, Li Junkang, Luo Xujiang, Peng Liqing, Li Huo, Huang Bo, Tian Guangzhao, Liu Shuyun, Sui Xiang, Huang Jingxiang, Guo Quanyi, Lu Xiaobo. Decellularized porcine skin matrix for tissue-engineered meniscus scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3473-3478. |
| [13] | Mo Jianling, He Shaoru, Feng Bowen, Jian Minqiao, Zhang Xiaohui, Liu Caisheng, Liang Yijing, Liu Yumei, Chen Liang, Zhou Haiyu, Liu Yanhui. Forming prevascularized cell sheets and the expression of angiogenesis-related factors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3479-3486. |
| [14] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| [15] | Liu Liyong, Zhou Lei. Research and development status and development trend of hydrogel in tissue engineering based on patent information [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3527-3533. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||