Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (3): 409-415.doi: 10.3969/j.issn.2095-4344.0605
Previous Articles Next Articles
Platelet-rich fibrin repairs cartilage defect in a rabbit model of old traumatic knee arthritis in weight-bearing region
Zou Chengda, Chen Xingguang, Su Guanghao, Zhang Ya, Wang Xiaodong
- (Department of Orthopedics, Children’s Hospital of Soochow University, Suzhou 215000, Jiangsu Province, China)
-
Received:2018-07-21Online:2019-01-28Published:2019-01-28 -
Contact:Wang Xiaodong, Professor, Chief physician, Department of Orthopedics, Children’s Hospital of Soochow University, Suzhou 215000, Jiangsu Province, China -
About author:Zou Chengda, Master candidate, Department of Orthopedics, Children’s Hospital of Soochow University, Suzhou 215000, Jiangsu Province, China
CLC Number:
Cite this article
Zou Chengda, Chen Xingguang, Su Guanghao, Zhang Ya, Wang Xiaodong. Platelet-rich fibrin repairs cartilage defect in a rabbit model of old traumatic knee arthritis in weight-bearing region[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(3): 409-415.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
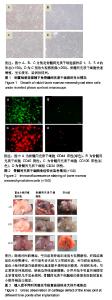
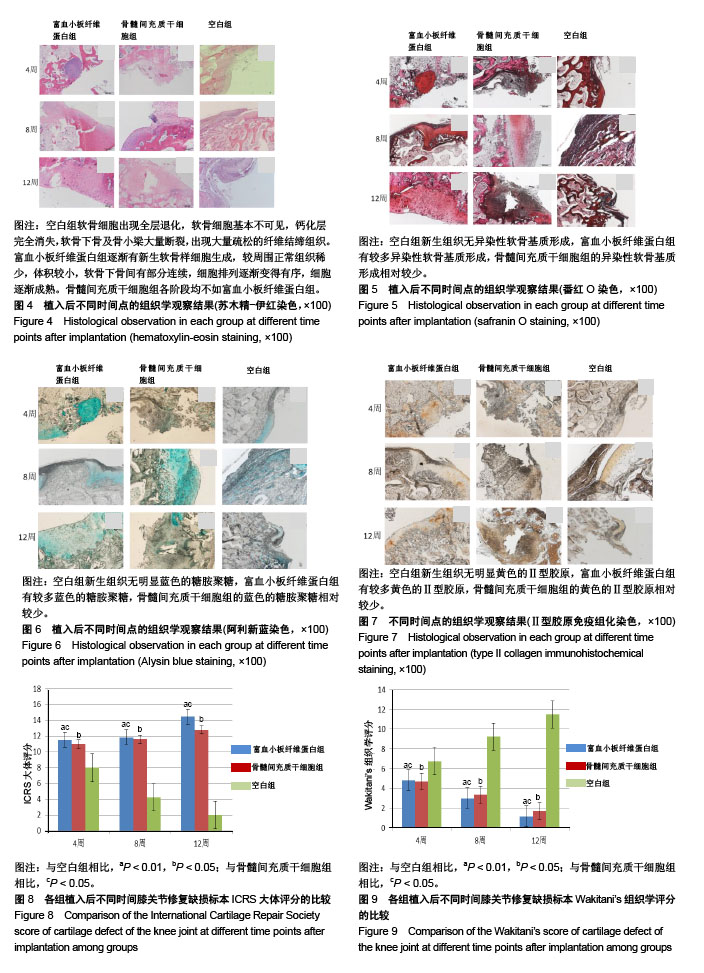
2.1 实验动物数量分析 27只兔子均进入结果分析。 2.2 兔骨髓间充质干细胞的培养与鉴定 骨髓间充质干细胞在培养瓶中呈长梭形,贴壁生长良好,有较强细胞增殖能力,见图1。 免疫荧光显示细胞表面标志物,CD44,CD105阳性,CD34,CD35阴性,提示所培养的细胞为骨髓间充质干细胞,见图2。 2.3 动物一般情况观察 缺损修复后1-3 d,几乎所有实验兔的精神不佳,对外界刺激反应较为迟钝,24 h进食量为平时的1/2-2/3,活动量明显减少,双膝可见梭型肿胀,关节腔可以触及波动感,手术后肢力量减小,活动频次较正常侧减少,步态有跛行,手术侧肢体偶有不着地情况。3-5 d时,富血小板纤维蛋白组和骨髓间充质干细胞组兔子的状态基本恢复正常,进食量和进水量恢复正常,反应较前敏捷,但是手术侧膝关节可见异常活动度,主动活动减少,力量减小,而空白组活动度稍差。3周时空白组出现手术侧肢体活动减少,呈屈曲状,逐渐出现手术侧膝关节的肿胀,可以触及骨性增生,主动活动明显减少,被动屈伸活动明显受限,富血小板纤维蛋白组和骨髓间充质干细胞组兔子无膝关节僵硬的情况出现。此次实验中无伤口明显感染情况发生。 2.4 各组大体外观观察 随着时间推移,①骨髓间充质干细胞组:4周时未见明显新生软骨组织形成,仅见少量乳白色组织覆盖缺损底部;8周时缺损依旧明显,边界变得圆钝,可见少数岛状乳白色组织突出于缺损底部,并且有少量半透明组织形成;12周时缺损持续存在,表面无光泽,缺损边界变得圆钝,基底部被乳白色的组织充填,较8周时缺损有所缩小,关节面凸凹不平,缺损边界处可见白色新生组织,与周围组织界限清晰,软骨表面出现较为明显的退变;②富血小板纤维蛋白组:4周时软骨缺损处可见有较多白色半透明状组织生成,触之柔软,表面光滑,缺损边界仍清晰可见;8周时可以发现缺损进一步修复,表面更加光滑,缺损处基本被半透明组织修复,外观有光泽,与正常软骨外观相似,缺损边界线逐渐模糊,分界开始不明显;12周时膝关节软骨缺损修复良好,大体观察和周围宿主软骨组织几乎完全相同,仅在平滑程度上较正常稍有欠缺;③空白组:4周时可见钻孔处缺损已经有部分修复,缺损处表面可见一层薄薄的白色半透明状组织,其周边同正常软骨组织有部分融合;8周时,出现较多的乳白色组织增生,其表面粗糙,与周围软骨形态不相似,部分和周围组织融合,软骨缺损关节面周围出现部分软骨的磨损,软骨变的薄厚不均匀;12周时,可见未钻孔的关节面也出现大块软骨磨损,深达骨质,可见松质骨,周围有组织增生粘连,关节活动明显受限,见图3。 2.5 各组组织学观察 见图4-7。 骨髓间充质干细胞组:4周时缺损明显,仅边缘部见新生软骨形成,底部有少量纤维状组织形成;8和12周时表现基本相似缺损持续存在,边缘部可见到少量新生软骨形成,缺损处以大量纤维组织填充,细胞排列较为整齐,有软骨细胞和少量Ⅱ型胶原生成。 富血小板纤维蛋白组:4周时有少量新生软骨样细胞生成,较周围正常组织稀少,且有凹陷,体积较小,排列无序,软骨下骨间有部分连续;术后8周时,新生的软骨样组织仍然有稍许凹陷,细胞比正常的小,较前有增大,排列相对无序,软骨下连续性好,番红O染色新生组织有少量异染性软骨基质形成,阿利新蓝染色有部分软骨细胞生成,Ⅱ型胶原抗体免疫组化染色可见少量Ⅱ型胶原;术后12周时,细胞排列有序,较8周是细胞更加成熟,软骨细胞及Ⅱ型胶原更加丰富。 空白组:4周时可见软骨组织与正常的组织比较相似,组织表面基本光滑,软骨细胞部分排列有序,潮线基本完整,交界处可见少量细胞簇集现象,番红O染色出现部分基质染色不均,阿利新蓝和Ⅱ型胶原免疫组化染色未见明显失染;8周时软骨组织表面与正常相比编的粗糙、凹凸不平,出现表层裂隙,软骨细胞列次序进一步紊乱,出现潮线中断,有地方出现核碎、核溶现象,表层细胞簇集现象更加明显,出现部分软骨细胞增生现象,软骨基质出现少量纤维化,软骨下骨质外露、软骨下骨囊性变,阿利新蓝和Ⅱ型胶原免疫组化染色不均匀;12周时软骨组织表层出现较大缺损区,软骨细胞次序紊乱,正常潮线消失,部分区域出现软骨下骨及骨小梁的断裂,软骨全层缺损,钙化层难以分辨,阿利新蓝和Ⅱ型胶原免疫组化染色有大部分层次出现失染。 2.6 各组大体评分和组织学评分 ICRS大体评分和Wakitani’s组织学评分:富血小板纤维蛋白组在各个时间段软骨表面形态方面评分明显优于空白组(P < 0.01)和骨髓间充质干细胞组(P < 0.05)。骨髓间充质干细胞组上述评分显著优于空白组(P < 0.05),见图8,9。"

| [1] Hochrein A, Zinser W, Spahn G, et al. What parameters affect knee function in patients with untreated cartilage defects: baseline data from the German Cartilage Registry. Int Orthop. 2018. doi: 10. 1007/s00264-018-4125-2. [2] Jones KJ, Mosich GM, Williams RJ. Fresh precut osteochondral allograft core transplantation for the treatment of femoral cartilage defects. Arthrosc Tech. 2018;7(8):e791-e795. [3] Kreuz PC, Kalkreuth RH, Niemeyer P, et al. Treatment of a focal articular cartilage defect of the talus with polymer-based autologous chondrocyte implantation: a 12-year follow-up period. J Foot Ankle Surg. 2017;56(4):45-46. [4] Lee BH, Park JN, Lee EJ, et al. Therapeutic efficacy of spherical aggregated human bone marrow-derived mesenchymal stem cells cultured for osteochondral defects of rabbit knee joints. Am J Sports Med. 2018; 46(9):2242-2252. [5] Zhao Z, Zhou X, Guan J, et al. Co-implantation of bone marrow mesenchymal stem cells and chondrocytes increase the viability of chondrocytes in rat osteo-chondral defects. Oncol Lett. 2018;15(5):7021-7027. [6] Böck T, Schill V, Krähnke M, et al. TGF-β1-modified hyaluronic acid/poly(glycidol) hydrogels for chondrogenic differentiation of human mesenchymal stromal cells. Macromol Biosci. 2018:e1700390. [7] Choukroun J, Diss A, Simonpieri A, et al. Platelet-rich fibrin: a second generation platelet concentrate. Part Ⅴ: histologic evaluations of PRF effects on bone allograft maturation in sinus lift. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101(3)299-303. [8] Mosesson MW, Siebenlist KR, Meh DA. The structure and biological features of fibrinogen and fibrin. Ann N Y Acad Sci. 2001;936:11-30. [9] Honda H, Tamai N, Naka N, et al. Bone tissue engineering with bone marrowderived stromal cells integrated with concentrasted growth factor in Rattus norvegicus calvaria defect model. J Artificial Organs. 2013;16(3):305-315. [10] Lohan A, Marzahn U, El SK, et al. Osteochondral articular defect repair using auricle-derived autologous chondrocytes in a rabbit model. Ann Anat. 2014;196(5):317-326. [11] Zhou Q, Wei B, Liu S, et al. Cartilage matrix changes in contralateral mobile knees in a rabbit model of osteoarthritis induced by immobilization. Bmc Musculoskeletal Disorders. 2015;16(1):224. [12] Yamaguchi S, Aoyama T, Ito A, et al. The effect of exercise on the early stages of mesenchymal stromal cell-induced cartilage repair in a rat osteochondral defect model. PLoS One. 2016;11(3):e0151580. [13] Zhang F, Liu D, Wang G, et al. Experimental research of articular cartilage defect repair using micro-fracture and insulin-like growth factor 1 in rabbits. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2014;28(5):591-596.[14] Yeo Y, Geng W, Ito T, et al. Photocrosslinkable hydrogel for myocyte cell culture and injection. Journal of biomedical matericals research. J Biomed Mater Res B Appl Biomater. 2007;81(2):312-322. [15] Shinojima N, Hossain A, Takezaki T, et al. TGF-β mediates homing of bone marrow-derived human mesenchymal stem cells to glioma stem cells. Cancer Res. 2013;73(7): 2333-2344. [16] Tang X, Chen F, Lin Q, et al. Bone marrow mesenchymal stem cells repair the hippocampal neurons and increase the expression of IGF-1 after cardiac arrest in rats. Exp Ther Med. 2017;14(5):4312-4320. [17] Ju X, Xue D, Wang T, et al. Catalpol promotes the survival and vegf secretion of bone marrow-derived stem cells and their role in myocardial repair after myocardial infarction in rats. Cardiovasc Toxicol. 2018. doi: 10. 1007/s12012-018-9460-4. [18] 张文丽,李淑慧,陈诚,等.富血小板纤维蛋白复合自体骨髓间充质干细胞修复兔牙槽骨缺损的研究[J].口腔医学研究, 2015,31(4): 336-339.[19] 杨勇,杨涛,刘斌,等.自体ADSCs复合富血小板纤维蛋白修复家兔耳软骨缺损的实验研究[J].现代生物医学进展,2013,13(12): 2210-2214.[20] Bahmanpour S, Ghasemi M, Sadeghi-Naini M, et al. Effects of platelet-rich plasma & platelet-rich fibrin with and without stromal cell-derived factor-1 on repairing full-thickness cartilage defects in knees of rabbits. Iran J Med Sci. 2016; 41(6):507-517. [21] Permuy M, Guede D, Lópezpeña M, et al. Effects of glucosamine and risedronate alone or in combination in an experimental rabbit model of osteoarthritis. BMC Vet Res. 2014;10(1):97. [22] Permuy M, Guede D, López-Peña M, et al. Effects of diacerein on cartilage and subchondral bone in early stages of osteoarthritis in a rabbit model. BMC Vet Res. 2015;11(1): 1-11. [23] SM Pagura, Thomas SG, Woodhouse LJ, et al. Circulating and synovial levels of IGF-I, cytokines, physical function and anthropometry differ in women awaiting total knee arthroplasty when compared to men. J Orthop Res. 2005; 23(2):397-405. [24] Nesic D, Whiteside R, Brittberg M, et al. Cartilage tissue engineering for degenerative joint disease.Adv Drug Deliv Rev. 2006;58(2):300-322. [25] Ni GX. Development and Prevention of Running-Related Osteoarthritis. Curr Sports Med Rep. 2016;15(5):342. [26] Felson DT. Clinical practice. Osteoarthritis of the knee. N Engl J Med. 2006;354(8):841-848. [27] Critchley SE, Eswaramoorthy R, Kelly DJ. Low-oxygen conditions promote synergistic increases in chondrogenesis during co-culture of human osteoarthritic stem cells and chondrocytes.J Tissue Eng Regen Med. 2018;12(4): 1074-1084. [28] Chen MJ, Whiteley JP, Please CP, et al. Inducing chondrogenesis inMSC/chondrocyte co-cultures using exogenous TGF-β: a mathematical model. J Theor Biol. 2018;439:1-13. [29] Thorstensson CA, Garellick G, Rystedt H, et al. Better management of patients with osteoarthritis: development and nationwide implementation of an evidence-based supported osteoarthritis self-management programme. Musculoskeletal Care. 2015;13(2):67-75. [30] Jing L, Zhang J, Leng H, et al. Repair of articular cartilage defects in the knee with autologous iliac crest cartilage in a rabbit model. Knee Surg Sports Traumatol Arthrosc. 2015; 23(4):1119-1127. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [3] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [4] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [5] | Cheng Jun, Tan Jun, Zhao Yun, Cheng Fangdong, Shi Guojia. Effect of thrombin concentration on the prevention of postoperative cerebrospinal leakage by fibrin glue [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 570-575. |
| [6] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [7] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [8] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [9] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [10] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [11] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [12] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [13] | Wang Hao, Chen Mingxue, Li Junkang, Luo Xujiang, Peng Liqing, Li Huo, Huang Bo, Tian Guangzhao, Liu Shuyun, Sui Xiang, Huang Jingxiang, Guo Quanyi, Lu Xiaobo. Decellularized porcine skin matrix for tissue-engineered meniscus scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3473-3478. |
| [14] | Mo Jianling, He Shaoru, Feng Bowen, Jian Minqiao, Zhang Xiaohui, Liu Caisheng, Liang Yijing, Liu Yumei, Chen Liang, Zhou Haiyu, Liu Yanhui. Forming prevascularized cell sheets and the expression of angiogenesis-related factors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3479-3486. |
| [15] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||