Chinese Journal of Tissue Engineering Research ›› 2026, Vol. 30 ›› Issue (29): 7648-7653.doi: 10.12307/2026.414
Previous Articles Next Articles
Systematic review of the effect of 3D-printed exoskeleton on hand function rehabilitation in stroke patients
Tang Ya1, Li Long2, Huang Du3, Huang Zhaolu1
- 1Qiandongnan Vocational and Technical College for Nationalities, Kaili 556000, Guizhou Province, China; 2Guizhou University, Guiyang 550025, Guizhou Province, China; 3China Railway Chengdu Bureau Group Ltd., Kaili 556000, Guizhou Province, China
-
Received:2025-09-29Revised:2025-12-16Online:2026-10-18Published:2026-03-06 -
Contact:Li Long, PhD, Associate professor, Guizhou University, Guiyang 550025, Guizhou Province, China -
About author:Tang Ya, MS, Lecturer, Qiandongnan Vocational and Technical College for Nationalities, Kaili 556000, Guizhou Province, China -
Supported by:Guizhou Provincial Association for Science and Technology 2025 Annual "New Quality Frontier" Leading Project, No. 2025XZQYXM-01-20 (to TY); Guizhou Provincial Joint Fund for Healthcare High-Quality Development Medical Research, No. 2024GZYXKYJJXM0145 (to LL); College-Level Funding Program of Qiandongnan Vocational and Technical College for Nationalities, No. 24zyyjsk02 (to TY)
CLC Number:
Cite this article
Tang Ya, Li Long, Huang Du, Huang Zhaolu. Systematic review of the effect of 3D-printed exoskeleton on hand function rehabilitation in stroke patients[J]. Chinese Journal of Tissue Engineering Research, 2026, 30(29): 7648-7653.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
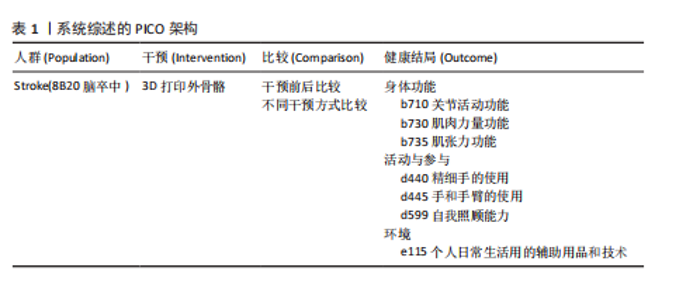
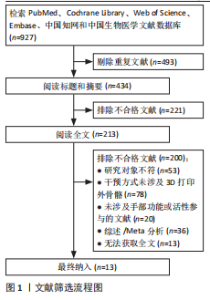
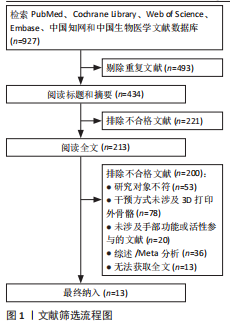
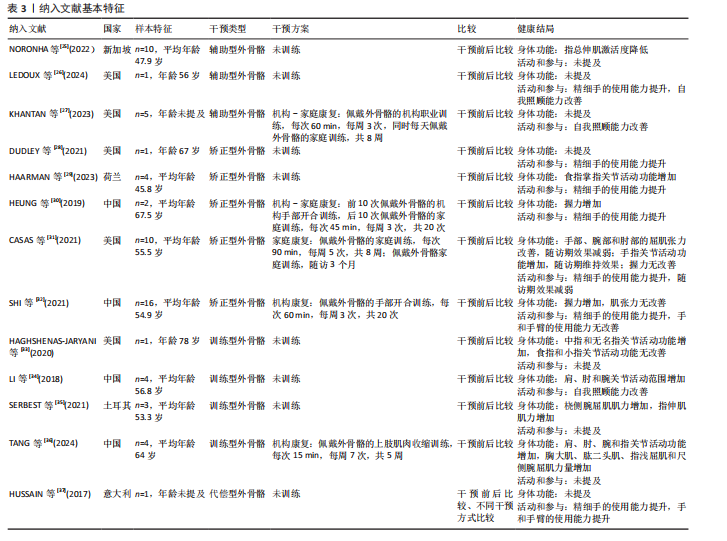
耳其共6个国家,共涉及62例脑卒中患者,见表3。 2.4 干预类型 基于Brunnstrom分期标准,将外骨骼划分为4种类型,各类外骨骼具有明确的临床适应分期和康复干预目标。 辅助型外骨骼适用于Brunnstrom Ⅰ期患者,通过稳定的抓握力辅助技术,补偿患者缺失的自主肌肉收缩能力,帮助患者完成抓握、持物等日常生活活动,核心目标是改善精细动作能力和生活自理能力[25-27]。 矫正型外骨骼适用于Brunnstrom Ⅱ-Ⅲ期患者,采用双重干预机制:一方面通过可调节负荷持续牵伸手部屈肌群,缓解因肌张力增高导致的痉挛状态;另一方面通过结构化抓握训练,逐步增强手部肌肉控制能力,促进功能性抓握的恢复[28-32]。 训练型外骨骼适用于Brunnstrom Ⅳ-Ⅵ期患者,以神经肌肉再教育和运动模式重塑为设计理念。研究进展体现在三方面:训练模式方面,SERBEST等[35]开发的手部外骨骼系统整合了被动和主动两种训练模式,HAGHSHENAS-JARYANI等[33]开发的手部外骨骼系统整合了被动、辅助和主动3种训练模式,均支持根据康复进程动态调节训练强度;结构设计方面,LI等[34]开发的七自由度上肢外骨骼通过人体工学仿生设计,实现了与患者运动轨迹的高度匹配;控制技术方面,TANG等[36]的四自由度上肢外骨骼通过融合运动意图识别技术,采用离线-在线联合训练策略,显著提升了多关节分离运动的评估精确度和干预个性化水平。 代偿型外骨骼适用于功能恢复停滞于Brunnstrom Ⅳ-Ⅵ期或存在不可逆损伤的患者,HUSSAIN等[37]研发的外骨骼将机器人手指与移动臂有机结合,在辅助完成功能性活动的同时,通过生物反馈机制实时激励患者发挥残余功能,避免了过度依赖外骨骼的问题。 2.5 干预方案 8篇研究仅评估了患者佩戴外骨骼前后的即时效果,未实施系统性治疗方案"
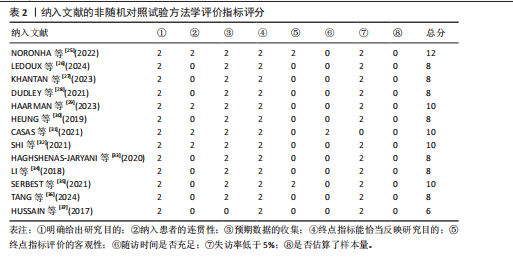
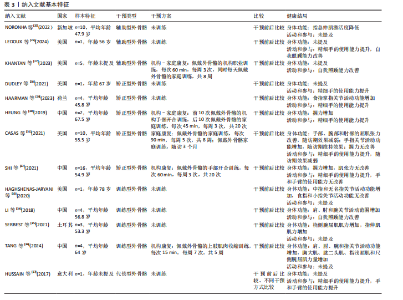
的评估。而在长期干预研究中,5篇研究的干预方案在训练时长、频率和周期方面存在明显差异:每次训练时长为15-90 min,训练频率为每周3-7次,干预周期为5-8周。根据康复场所的不同,可将干预方式分为机构康复、家庭康复和机构-家庭康复三类。 机构康复方面,TANG等[36]研究采用外骨骼辅助的胸大肌、肱二头肌、指浅屈肌和尺侧腕屈肌主动收缩训练,每次15 min,每周7次,持续5周;SHI等[32]实施外骨骼辅助的手部开合训练,每次60 min,每周3次,持续20次。家庭康复方面,CASAS等[31]采用外骨骼辅助的日常生活训练,每次90 min,每周5次,持续8周,并在后续3个月的随访期内继续使用外骨骼进行训练。机构-家庭康复方面,KHANTAN 等[27]的干预方式包含两个部分:佩戴外骨骼的机构职业训练,每次60 min,每周3次,同时每天进行佩戴外骨骼的家庭训练,共8周。HEUNG等[30]的干预方式包含2个阶段:前10次佩戴外骨骼的机构手部开合训练,后10次佩戴外骨骼的家庭训练,每次45 min,每周3次,共20次。 2.6 健康结局 2.6.1 关节活动功能 在矫正型外骨骼的应用中,HAARMAN等[29]发现,手指外骨骼可使示指掌指关节的伸展活动范围显著增加(43.5±27.4)°(P=0.038)。CASAS等[31]通过8周的抓握训练发现,手部外骨骼对除拇指外的4个手指的活动范围显著增加(19.8±24.4)°(P=0.031),且这一效果在3个月随访期内仍保持(18.9±10.3)°的增益(P=0.001)。 在训练型外骨骼的应用中,HAGHSHENAS- JARYANI等[33]发现,手部外骨骼增加中指和无名指屈曲角度达到100°目标值,而示指和小指稳定于80°;LI等[34]发现,上肢外骨骼对肩、肘、腕的活动范围均有提升作用,尤其是腕关节活动范围增加174%;TANG等[36]通过5周上肢肌肉训练发现,上肢外骨骼增加肩、肘、腕及指关节活动范围,平均增幅为10.3%。 2.6.2 肌肉力量功能 在辅助型外骨骼的应用中,NORONHA等[25]发现患者指总伸肌的肌电振幅平均减少14.0%(P < 0.01)。 在矫正型外骨骼的应用中,HEUNG等[30]发现2例患者握力均增加1.1 kg;SHI等[32]通过20次的手部开合训练发现,患者握力由(4.7±2.8) kg显著增加至(6.9±3.7) kg(P < 0.001);但CASAS等[31]通过8周的抓握训练发现,患者握力无显著变化(P=0.31)。 在训练型外骨骼的应用中,SERBEST等[35]发现,桡侧腕屈肌的肌电振幅增加197.8%,指伸肌的肌电振幅增加184.1%;TANG等[36]通过5周上肢肌肉收缩训练发现,胸大肌、肱二头肌、指浅屈肌和尺侧腕屈肌的肌电振幅平均增加11.4%。 2.6.3 肌张力功能 在矫正型外骨骼的应用中,CASAS等[31]通过8周的抓握训练发现,手指、腕和肘关节的屈肌改良Ashworth量表评分显著降低(0.2±0.2)分(P=0.022),但这一效果在3个月后未能维持(P=0.155)。而SHI等[32]通过20次的手部开合训练发现,患者手指屈肌改良Ashworth量表评分仅从(1.4±0.8)分略微下降至(1.3±0.7)分(P=0.423),无统计学意义。 2.6.4 活动和参与 在辅助型外骨骼的应用中,LEDOUX等[26]研究中抓握测试结果显示患者可稳定抓握手机、香蕉、一次性水瓶和螺丝刀等物品,反映精细手使用能力提升;日常生活活动能力测试结果显示患者能通过双手协同完成开关水瓶与水果切片的复合动作,反映自我照顾能力提升。KHANTAN等[27]发现加拿大作业表现量表评分增加,反映患者自我照顾能力提升。 矫正型外骨骼的疗效通过多项标准化量表评估得到验证。①盒块试验评估精细手使用能力。DUDLEY等[28]发现移动方块数增加5个;HAARMAN等[29]发现移动方块数增加6个;HEUNG等[30]发现2例患者移动方块数分别增加2个和12个;SHI等[32]发现20次的手部开合训练后,移动木块数从(3.1±6.5)个显著增加至(4.9±9.5)个(P=0.024)。②采用Fugl-Meyer上肢评定量表评估精细手使用能力(腕手子项)以及手和手臂使用能力(肩肘子项)。DUDLEY等[28]发现手部评分提高10分;HEUNG等[30]发现2例患者手部评分分别提高5分和3分;SHI等[32]发现20次的手部开合训练后,上肢"

评分从(22.4±9.6)分显著提高至(25.7±12.1)分(P=0.003),腕手部评分从(6.6±3.3)分显著提高至(8.9±4.3)分(P=0.001),而肩肘部评分从(13.5±6.3)分提高至(14.4±7.5)分(P=0.206)未达到统计学显著水平;CASAS等[31]发现8周的抓握训练后上肢评分提高(2.8±5.6)分(P=0.147),3个月的随访期提高(3.4±4.6)分(P=0.055),均未达到统计学显著水平。③上肢动作研究量表评估精细手使用能力(抓、握、捏子项)以及手和手臂使用能力(粗大运动子项)。SHI等[32]发现20次的手部开合训练后评分从(13.7±14.6)分显著提高至(16.1±15.3)分(P=0.032);CASAS等[31]发现8周的抓握训练后评分显著提高(3.4±4.5)分(P=0.039),但3个月后随访时效果减弱至(1.1±3.6)分(P=0.375),未达到统计学显著水平。 在训练型外骨骼的应用中,LI等[34]的日常生活活动能力测试结果显示患者可以在外骨骼辅助下完成饮水动作,反映自我照顾能力提升。 在代偿型外骨骼的应用中,HUSSAIN等[37]发现盒块试验移动方块数增加8个,反映精细手使用能力提升;Frenchay手臂测试得分提高3分,反映手和手臂使用能力提升。 2.6.5 3D打印外骨骼可用性 LEDOUX等[26]通过非结构化访谈发现,绑带设计便于穿脱与调整,泡沫衬垫与灵活的结构提升了佩戴舒适感,且手部与抓握物体之间的无阻碍接触感获得了较高的用户满意度。DUDLEY等[28]的系统可用性量表达到90分,用户辅助技术满意度评估问卷结果显示外骨骼平均得分为4分,其中在尺寸、质量和调整方面得分较高。CASAS等[31]采用运动活动日志评估患者在家庭日常生活活动中的肢体使用频率,结果显示8周的训练期内手部使用频率显著提高(0.6±0.6)分(P=0.018),且在3个月随访时较干预前显著提高(0.7±0.5)分(P=0.005)。NORONHA等[25]的问卷调查结果显示,外骨骼在减少损伤、功能帮助和用户体验的主观评分较高。KHANTAN等[27]的参与者均认为外骨骼轻便、便携、贴合且舒适,易于穿戴和脱卸,这使他们愿意在社交场合中使用它。SERBEST等[35]发现,患者需要花费很长时间独立佩戴外骨骼,在他人的帮助下可5-10 min内完成佩戴,一两分钟内取下。"

| [1] 《中国卒中中心报告2022》概要[J].中国脑血管病杂志,2024,21(8):565-576. [2] CHENG C, LIU T, ZHANG B, et al. Effects of robot-assisted hand function therapy on brain functional mechanisms: a synchronized study using fNIRS and sEMG. Front Med (Lausanne). 2024;11:1411616. [3] WANG X, CHEN X, CHAN KLC, et al. Does the alternating timing of rTMS combined with soft-hand rehabilitation robot affect the recovery of hand function in patients after stroke? A study protocol for a multicentre randomised controlled trial. BMJ Open. 2025; 15(3):e094672. [4] TATER P, PANDEY S. Post-stroke movement disorders: clinical spectrum, pathogenesis, and management. Neurol India. 2021;69(7):272-283. [5] ZHAO Y, ZHANG X, CHEN X, et al. Neuronal injuries in cerebral infarction and ischemic stroke: from mechanisms to treatment(review). Int J Mol Med. 2022;49(2):15. [6] AGGOGERI F, MIKOLAJCZYK T, O’KANE J. Robotics for rehabilitation of hand movement in stroke survivors. Adv Mech Eng. 2019;11(4):1687814019841921. [7] 姚玉峰,裴硕,郭军龙,等.上肢康复机器人研究综述[J].机械工程学报,2024,60(11): 115-134. [8] MOGGIO L, DE SIRE A, MAROTTA N, et al. Exoskeleton versus end-effector robot-assisted therapy for finger-hand motor recovery in stroke survivors: systematic review and meta-analysis. Top Stroke Rehabil. 2022;29(8):539-550. [9] ROJEK I, KACZMAREK M, KOTLARZ P, et al. Hand exoskeleton—development of own concept. Appl Sci. 2023;13(5):3238. [10] PEREIRA RJR, ALMEIDA FAD, GOMES GF, et al. A multiobjective optimization parameters applied to additive manufacturing: doe-based approach to 3D printing. Structures. 2023;55:1710-1731. [11] MAK SKD, ACCOTO D. Review of current spinal robotic orthoses. Healthcare. 2021;9(1):70. [12] TRIWIYANTO T, WAKIDI LF, PAWANA IPA. Exoskeleton for Upper Limb Rehabilitation (EULR) with 3D printing technology based on force sensor. HardwareX. 2025;23:e00665. [13] KERMAVNAR T, SHANNON A, O’SULLIVAN LW. The application of additive manufacturing/3D printing in ergonomic aspects of product design: a systematic review. Appl Ergon. 2021; 97:103528. [14] OU YK, WANG YL, CHANG HC, et al. Design and development of a wearable exoskeleton system for stroke rehabilitation. Healthcare. 2020;8(1):18-28. [15] 王玉金,聂子芸,罗梦霞,等.手功能康复机器人及其运动意图识别研究进展[J].重庆理工大学学报(自然科学),2025, 39(5):156-162. [16] DEMECO A, FORESTI R, FRIZZIERO A, et al. The upper limb orthosis in the rehabilitation of stroke patients: the role of 3D printing. Bioengineering (Basel). 2023;10(11):1256. [17] DE IACO L, VEERBEEK JM, KET JCF, et al. Upper limb robots for recovery of motor arm function in patients with stroke: a systematic review and meta-analysis. Neurology. 2024; 103(2):e209495. [18] WANG H, WU X, LI Y, et al. Efficacy of robot-assisted training on upper limb motor function after stroke: a systematic review and network meta-analysis. Arch Rehabil Res Clin Transl. 2024;7(1):100387. [19] MORENO-SANJUAN V, CISNAL A, FRAILE JC, et al. Design and characterization of a lightweight underactuated raca hand exoskeleton for neurorehabilitation. Robot Auton Syst. 2021; 143:103828. [20] 邱卓英.《国际功能、残疾和健康分类》研究总论[J].中国康复理论与实践,2003, 9(1):7-10. [21] 王萌亚,王仲朋,陈龙,等.卒中后运动神经反馈康复训练研究进展与前景[J].中国生物医学工程学报,2019,38(6):742-752. [22] HARRISON JE, WEBER S, JAKOB R, et al. ICD-11: an international classification of diseases for the twenty-first century. BMC Med Inform Decis Mak. 2021;21(Suppl 6):206. [23] World Health Organization. International classification of functioning, disability, and health: children & youth version: ICF-CY. World Health Organization. 2007. [24] 蒋春燕,李丹,张建梅,等.康复护理促进烧伤患者生活质量的Meta分析[J].中国康复理论与实践,2016,22(3):345-349. [25] NORONHA B, NG CY, LITTLE K, et al. Soft, lightweight wearable robots to support the upper limb in activities of daily living: a feasibility study on chronic stroke patients. IEEE Trans Neural Syst Rehabil Eng. 2022;30: 1401-1411. [26] LEDOUX ED, BARTH EJ. Design, modeling, and preliminary evaluation of a 3D-printed wrist-hand grasping orthosis for stroke survivors. Wearable Technol. 2024;5:e12. [27] KHANTAN M, AVERY M, AUNG PT, et al. The NuroSleeve, a user-centered 3D printed hybrid orthosis for individuals with upper extremity impairment. J Neuroeng Rehabil. 2023;20(1):103. [28] DUDLEY DR, KNARR BA, SIU KC, et al. Testing of a 3D printed hand exoskeleton for an individual with stroke: a case study. Disabil Rehabil Assist Technol. 2021;16(2):209-213. [29] HAARMAN CJW, HEKMAN EEG, RIETMAN JS, et al. Mechanical design and feasibility of a finger exoskeleton to support finger extension of severely affected stroke patients. IEEE Trans Neural Syst Rehabil Eng. 2023;31:1268-1276. [30] HEUNG KHL, TANG ZQ, HO L, et al. Design of a 3D printed soft robotic hand for stroke rehabilitation and daily activities assistance. IEEE Int Conf Rehabil Robot. 2019;2019:65-70. [31] CASAS R, SANDISON M, NICHOLS D, et al. Home-Based therapy after stroke using the hand spring operated movement enhancer (HandSOME II). Front Neurorobot. 2021; 17(15):773477. [32] SHI XQ, HEUNG HL, TANG ZQ, et al. Effects of a soft robotic hand for hand rehabilitation in chronic stroke survivors. J Stroke Cerebrovasc Dis. 2021;30(7):105812. [33] HAGHSHENAS-JARYANI M, PATTERSON RM, BUGNARIU N, et al. A pilot study on the design and validation of a hybrid exoskeleton robotic device for hand rehabilitation. J Hand Ther. 2020;33(2):198-208. [34] LI N, YANG T, YU P, et al. Bio-inspired upper limb soft exoskeleton to reduce stroke-induced complications. Bioinspir Biomim. 2018;13(6):066001. [35] SERBEST K, KUTLU M, ELDOGAN O, et al. Development and control of a home-based training device for hand rehabilitation with a spring and cable driven mechanism. Biomed Tech (Berl). 2021;66(4):395-403. [36] TANG ZC, CUI ZZ, WANG H, et al. A 4-DOF exosuit using a hybrid eeg-based control approach for upper-limb rehabilitation. IEEE J Transl Eng Health Med. 2024;12:622-634. [37] HUSSAIN I, SALVIETTI G, SPAGNOLETTI G, et al. A soft supernumerary robotic finger and mobile arm support for grasping compensation and hemiparetic upper limb rehabilitation. Robot Auton Syst. 2017;93:1-12. [38] NORONHA B, ACCOTO D. Exoskeletal devices for hand assistance and rehabilitation: a comprehensive analysis of state-of-the-art technologies. IEEE T Med Robot Bio. 2021; 3(2):525-538. [39] ANDRÉS-ESPERANZA J, ISERTE-VILAR JL, RODA-CASANOVA V. Design and optimization of a custom-made six-bar exoskeleton for pulp pinch grasp rehabilitation in stroke patients. Biomimetics (Basel). 2024;9(10):616. [40] GU Y, XU Y, SHEN Y, et al. A review of hand function rehabilitation systems based on hand motion recognition devices and artificial intelligence. Brain Sci. 2022;12(8):1079. [41] YU J, LUO L, ZHU W, et al. A novel low-pressure robotic glove based on ct-optimized finger joint kinematic model for long-term rehabilitation of stroke patients. IEEE Trans Neural Syst Rehabil Eng. 2024;32:53-62. [42] ESPOSITO D, CENTRACCHIO J, ANDREOZZI E, et al. Design of a 3D-printed hand exoskeleton based on force-myography control for assistance and rehabilitation. Machines. 2022;10(1):57. [43] JOCHUMSEN M, JANJUA TAM, ARCEO JC, et al. Induction of neural plasticity using a low-cost open source brain-computer interface and a 3D-printed wrist exoskeleton. Sensors (Basel). 2021;21(2):572. [44] ARAUJO RS, SILVA CR, NETTO SPN, et al. Development of a low-cost eeg-controlled hand exoskeleton 3D printed on textiles. Front Neurosci. 2021;15:661569. [45] OU YK, WANG YL, CHANG HC, et al. Design and development of a wearable exoskeleton system for stroke rehabilitation. Healthcare (Basel). 2020;8(1):18. [46] RUDD G, DALY L, JOVANOVIC V, et al. A low-cost soft robotic hand exoskeleton for use in therapy of limited hand–motor function. Applied Sciences. 2019;9(18):3751. [47] 吴远,高强.Brunnstrom六期评估法在脑卒中偏瘫康复中的应用价值和局限性[J].中国康复医学杂志,2021,36(4):505-509. [48] KABIR R, SUNNY MSH, AHMED HU, et al. Hand rehabilitation devices: a comprehensive systematic review. Micromachines (Basel). 2022;13(7):1033. [49] YEH SJ, WANG YC, FANG WC, et al. Effectiveness of powered hand exoskeleton on upper extremity function in people with chronic stroke. Actuators. 2025;14(2):67. [50] CHOWDHURY A, NISHAD SS, MEENA YK, et al. Hand-Exoskeleton assisted progressive neurorehabilitation using impedance adaptation based challenge Level Adjustment Method. IEEE Trans Haptics. 2018;12(2):128-140. [51] WANG X, CHEN X, CHAN KLC, et al. Does the alternating timing of rTMS combined with soft-hand rehabilitation robot affect the recovery of hand function in patients after stroke? A study protocol for a multicentre randomised controlled trial. BMJ Open. 2025; 15(3):e094672. [52] CRAMER SC, DODAKIAN L, LE V, et al. National institutes of health strokenet telerehab investigators. efficacy of home-based telerehabilitation vs in-clinic therapy for adults after stroke: a randomized clinical trial. JAMA Neurol. 2019;76(9):1079-1087. [53] YANG YS, TSENG CH, FANG WC, et al. Effectiveness of a New 3D-Printed Dynamic Hand-Wrist Splint on Hand Motor Function and Spasticity in Chronic Stroke Patients. J Clin Med. 2021;10(19):4549. [54] SINGH N, SAINI M, KUMAR N, et al. Evidence of neuroplasticity with robotic hand exoskeleton for post-stroke rehabilitation: a randomized controlled trial. J Neuroeng Rehabil. 2021; 18(1):76. [55] MUBIN O, ALNAJJAR F, JISHTU N, et al. Exoskeletons with virtual reality, augmented reality, and gamification for stroke patients’ rehabilitation: systematic review. JMIR Rehabil Assist Technol. 2019;6(2):e12010. |
| [1] | Liu Jinlong, Abuduwupuer·Haibier, Bai Zhen, Su Danyang, Miao Xin, Li Fei, Yang Xiaopeng. Efficacy of different nonsurgical treatments for adolescent idiopathic scoliosis: a systematic review and network meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2370-2379. |
| [2] | Gao Feng, Zhang Jun, Yu Wenjun, Chanyu Yujing, Zhao Le, Hu Yuting, Wang Junhua, Liu Yongfu. Effects of wrist-hand orthosis on hand dysfunction in stroke patients: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2124-2131. |
| [3] | Wang Zhipeng, Zhang Xiaogang, Zhang Hongwei, Zhao Xiyun, Li Yuanzhen, Guo Chenglong, Qin Daping, Ren Zhen. A systematic review of application value of machine learning to prognostic prediction models for patients with lumbar disc herniation [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(3): 740-748. |
| [4] | Yu Weijie, Cao Dongdong, Guo Tianci, Niu Puyu, Yang Jialin, Wang Simin, Liu Aifeng. Risk prediction models of recurrence after percutaneous endoscopic lumbar discectomy: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(3): 749-759. |
| [5] | Chu Rui, Li Mingming, Xie Yeshou, Ni Tao, Du Yinuo. Traditional Chinese sports intervene in sarcopenia and its complications in the elderly: a meta-analysis on improving muscle strength, mass, and physical function [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(24): 6354-6364. |
| [6] | Peng Hao, Jiang Yang, Song Yanping, Wu Quan, Yao Na, Chen Qigang, Shen Zhen. H-type angiogenesis and its role in various skeletal disease animal models [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(16): 4154-4165. |
| [7] | Yang Bin, Tao Guangyi, Yang Shun, Xu Junjie, Huang Junqing . Visualization analysis of research hotspots of artificial intelligence in field of spinal cord nerve injury and repair [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(4): 761-770. |
| [8] | Yan Jing, Qin Qiujun, Li Fen, Zhou Jun, Ding Yuanyuan, Jin Chunlin. A systematic review of osteoporosis-specific quality-of-life scales [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(35): 7649-7655. |
| [9] | Yu Bingbing, Wang Tingting, Fang Junlin, Guo Yun, Huang Yingru. Acupuncture for treatment of postmenopausal osteoporosis: meta-analysis, systematic evaluation and trial sequential analysis [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(29): 6305-6316. |
| [10] | Wang Jiaru, Zhang Ying, Yang Yong, Qi Wen, Xiao Huaye, Ma Qiuping, Yang Lianzhao, Luo Ziwei, He Yaqing, Zhang Jiangyin, Wei Jiawen, Meng Yuan, Tan Silian. Systematic review of machine learning models for predicting functional recovery and prognosis in stroke [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(29): 6317-6325. |
| [11] | Zhang Yunyi, Liu Songtao, Xie Shaodong, Zhu Haifeng, Qian Guifeng, Huo Ming, Zhou Jie, Deng Zixuan. Platelet rich plasma versus hyaluronic acid in treatment of knee osteoarthritis: an overview of systematic reviews [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(28): 6138-6145. |
| [12] | Cao Haijie, Song Huijie, Sun Yalu, Zhang Guangyou, Li Xiang. A wearable exoskeleton with posture feedback improves abnormal gait in patients with stroke [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(24): 5127-5133. |
| [13] | Deng Yiran, Wang Xianliang, Li Dandan. Meta-analysis of exercise intervention on cardiopulmonary function in stroke patients [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(24): 5203-5211. |
| [14] | Liang Jiajia, Sun Jiaojiao, Liu Wenjie, Xing Zheng, Li Qi, Li Qingwen, Chu Xiaolei . Electromyographic biofeedback therapy and motor function recovery after spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(14): 3002-3010. |
| [15] | Xu Yi, Deng Yubin. Exoskeleton-assisted walking rehabilitation for spinal cord injury: CiteSpace analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(33): 5403-5412. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||