Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (12): 1962-1968.doi: 10.12307/2024.008
Knee function recovery in patients with anterior cruciate ligament reconstruction after blood flow restriction training: a meta-analysis
Zuo Huiwu1, Geng Zhizhong2, Chen Peng1, Lin Xikai1, Chen Jian1
- 1College of Sports Medicine, Wuhan Sports University, Wuhan 430079, Hubei Province, China; 2School of Kinesiology, Shanghai University of Sport, Shanghai 200438, China
-
Received:2023-01-06Accepted:2023-03-04Online:2024-04-28Published:2023-08-23 -
Contact:Chen Jian, PhD, Associate professor, Master’s supervisor, College of Sports Medicine, Wuhan Sports University, Wuhan 430079, Hubei Province, China -
About author:Zuo Huiwu, Master candidate, College of Sports Medicine, Wuhan Sports University, Wuhan 430079, Hubei Province, China -
Supported by:Scientific Research Plan Project of Hubei Provincial Department of Education, No. B2021193 (to CJ)
CLC Number:
Cite this article
Zuo Huiwu, Geng Zhizhong, Chen Peng, Lin Xikai, Chen Jian. Knee function recovery in patients with anterior cruciate ligament reconstruction after blood flow restriction training: a meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(12): 1962-1968.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
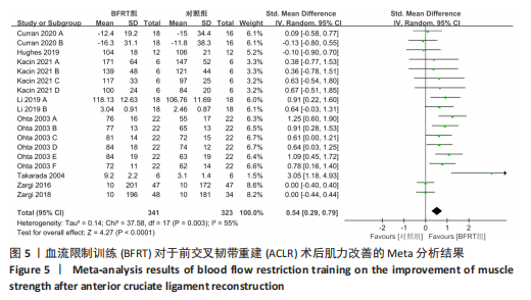
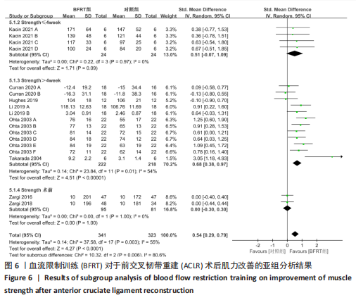
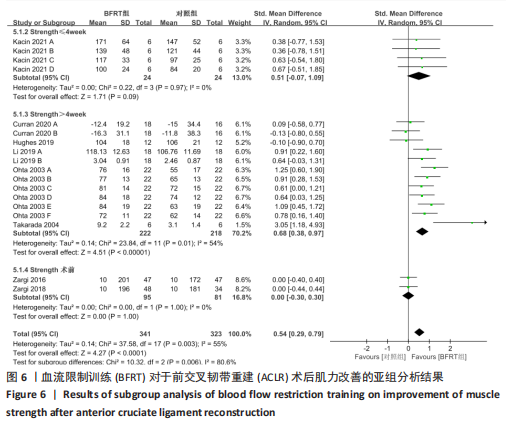
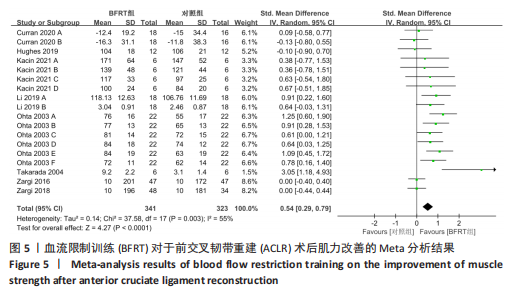
2.4 Meta分析结果 2.4.1 膝关节周围肌力 共纳入8篇随机对照试验的18项试验[20-21,26-28,30-32],试验组和对照组的合并样本量共664例。由于研究间存在中等异质性(I2=55%,P=0.003),故采用随机效应模型进行分析;由于测量单位不同,故采用SMD进行合并。结果显示,BFRT组干预后肌力改善显著优于常规抗阻训练组[SMD=0.54,95%CI(0.29,0.79),P < 0.000 1],见图5。亚组分析中发现,当干预时间≤4周时,BFRT组肌力与常规抗阻训练组差异无显著性意义[SMD=0.51,95%CI(-0.07,1.09),P=0.09];当干预时间 > 4周时,BFRT组肌力显著优于常规抗阻训练组[SMD=0.68,95%CI(0.38,0.97),P < 0.000 01];术前干预试验中,两组无统计学差异[SMD=0.00,95%CI(-0.30,0.30),P=1.00],见图6。敏感性分析表明,1项研究具有较高敏感性[31],将其剔除后对剩余文献进行Meta分析,研究间异质性减小(I2=47%,P=0.02),且合并结果较稳定[SMD=0.50,95%CI(0.27,0.73),P < 0.01]。"
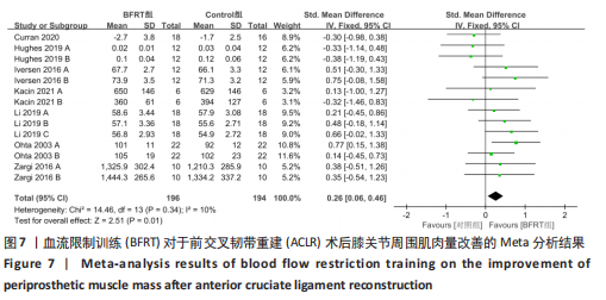
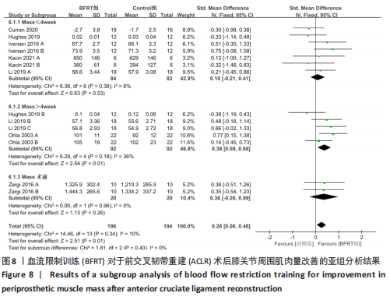
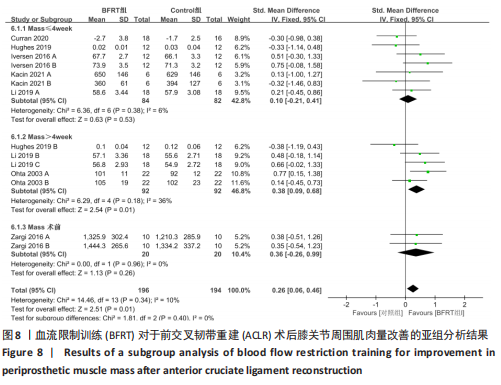
2.4.2 膝关节周围肌肉量 共纳入7篇随机对照试验的14项试验[20-21,26-27,29-30,32],试验组和对照组的合并样本量共390例。由于研究间异质性较低(I2=10%,P=0.34),故采用固定效应模型进行分析;由于测量单位不同,故采用SMD进行合并。结果显示,BFRT组干预后膝关节肌肉量改善显著优于常规抗阻训练组[SMD=0.26,95%CI(0.06,0.46),P=0.01],见图7。亚组分析中发现,当干预时间≤4周时,BFRT组肌肉量与常规抗阻训练组差异无显著性意义[SMD=0.10,95%CI(-0.21,0.41),P=0.53];当干预时间 > 4周时,BFRT组肌肉量改善显著优于常规抗阻训练组[SMD=0.38,95%CI(0.09,0.68),P=0.01];在术前干预试验中,两组差异无显著性意义[SMD=0.36,95%CI(-0.26,0.99),P=0.26],见图8。"
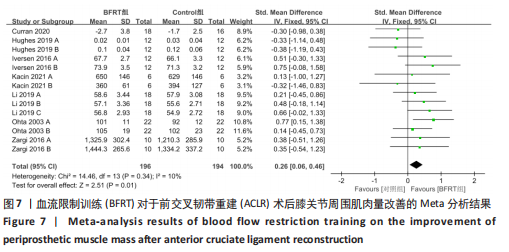
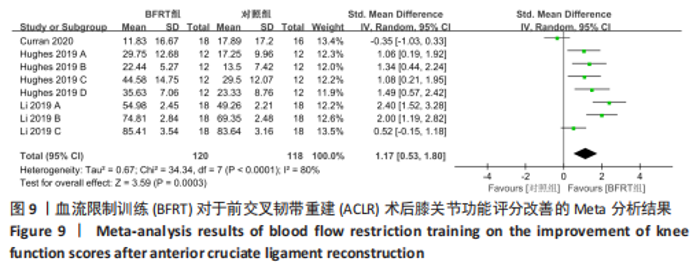
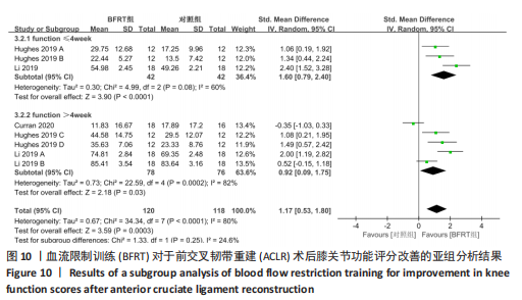
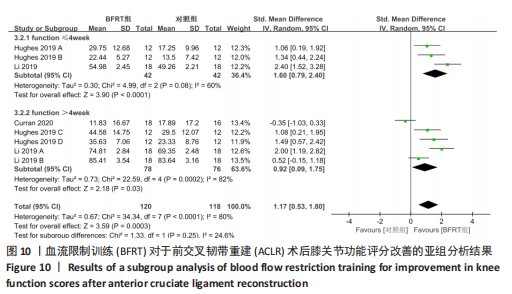
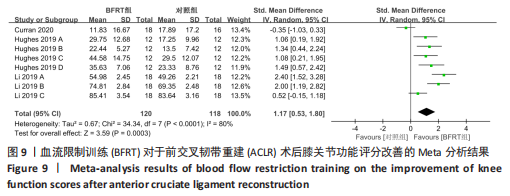
2.4.3 膝关节功能评价 共纳入3篇随机对照试验的8项试验[20,26-27],试验组和对照组的合并样本量共238例。由于研究间异质性较高(I2=80%,P < 0.01),故采用随机效应模型进行分析;由于测量单位不同,故采用SMD进行合并。结果显示,在膝关节功能改善方面,BFRT组显著优于常规抗阻训练组[SMD=1.17,95%CI(0.53,1.80),P=0.000 3],见图9。亚组分析中发现,当干预时间≤4周[SMD=1.60,95%CI(0.79,2.40),P < 0.000 1]及 > 4周[SMD=0.92,95%CI(0.09,1.75),P=0.03]时,BFRT组与常规抗阻训练组差异均有显著性意义,见图10。"
| [1] FILBAY SR, GRINDEM H. Evidence-based recommendations for the management of anterior cruciate ligament (ACL) rupture. Best Pract Res Clin Rheumatol. 2019;33(1):33-47. [2] LAI CCH, ARDERN CL, FELLER JA, et al. Eighty-three per cent of elite athletes return to preinjury sport after anterior cruciate ligament reconstruction: a systematic review with meta-analysis of return to sport rates, graft rupture rates and performance outcomes. Br J Sports Med. 2018;52(2):128-138. [3] SANDERS TL, MARADIT KREMERS H, BRYAN AJ, et al. Incidence of Anterior Cruciate Ligament Tears and Reconstruction: A 21-Year Population-Based Study. Am J Sports Med. 2016;44(6):1502-1507. [4] PASCHOS NK, HOWELL SM. Anterior cruciate ligament reconstruction: principles of treatment. EFORT Open Rev. 2017;1(11):398-408. [5] MALL NA, CHALMERS PN, MORIC M, et al. Incidence and trends of anterior cruciate ligament reconstruction in the United States. Am J Sports Med. 2014;42(10):2363-2370. [6] 陈连旭,付立功.前交叉韧带断裂和重建的临床流行病学分析[J].中国组织工程研究,2016, 20(24):3602-3608. [7] HEWETT TE, DI STASI SL, MYER GD. Current concepts for injury prevention in athletes after anterior cruciate ligament reconstruction. Am J Sports Med. 2013;41(1):216-224. [8] BIRCHMEIER T, LISEE C, KANE K, et al. Quadriceps Muscle Size Following ACL Injury and Reconstruction: A Systematic Review. J Orthop Res. 2020;38(3):598-608. [9] VAN GRINSVEN S, VAN CINGEL RE, HOLLA CJ, et al. Evidence-based rehabilitation following anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc. 2010;18(8):1128-1144. [10] MONK AP, DAVIES LJ, HOPEWELL S, et al. Surgical versus conservative interventions for treating anterior cruciate ligament injuries. Cochrane Database Syst Rev. 2016;4(4):CD011166. [11] THOMAS AC, WOJTYS EM, BRANDON C, et al. Muscle atrophy contributes to quadriceps weakness after anterior cruciate ligament reconstruction. J Sci Med Sport. 2016;19(1):7-11. [12] PALMIERI-SMITH RM, THOMAS AC. A neuromuscular mechanism of posttraumatic osteoarthritis associated with ACL injury. Exerc Sport Sci Rev. 2009;37(3):147-153. [13] KOCHMAN M, KASPRZAK M, KIELAR A. ACL Reconstruction: Which Additional Physiotherapy Interventions Improve Early-Stage Rehabilitation? A Systematic Review. Int J Environ Res Public Health. 2022;19(23):15893. [14] CULVENOR AG, GIRDWOOD MA, JUHL CB, et al. Rehabilitation after anterior cruciate ligament and meniscal injuries: a best-evidence synthesis of systematic reviews for the OPTIKNEE consensus. Br J Sports Med. 2022;56(24):1445-1453. [15] WORTMAN RJ, BROWN SM, SAVAGE-ELLIOTT I, et al. Blood Flow Restriction Training for Athletes: A Systematic Review. Am J Sports Med. 2021;49(7):1938-1944. [16] PIGNANELLI C, CHRISTIANSEN D, BURR JF. Blood flow restriction training and the high-performance athlete: science to application. J Appl Physiol (1985). 2021;130(4):1163-1170. [17] 魏佳,李博,冯连世,等.血流限制训练的方法学因素及潜在安全性问题[J].中国体育科技, 2019,55(3):3-12. [18] HUGHES L, PATON B, ROSENBLATT B, et al. Blood flow restriction training in clinical musculoskeletal rehabilitation: a systematic review and meta-analysis. Br J Sports Med. 2017;51(13):1003-1011. [19] 李新通,潘玮敏,覃华生,等.血流限制训练:加速肌肉骨骼康复的新方法[J].中国组织工程研究,2019,23(15):2415-2420. [20] 李奇,李蕊,罗昌禄,等.血流限制性运动对前交叉韧带重建术后膝关节功能的影响[J].广东医学,2019,40(10):1405-1408. [21] KACIN A, DROBNIČ M, MARŠ T, et al. Functional and molecular adaptations of quadriceps and hamstring muscles to blood flow restricted training in patients with ACL rupture. Scand J Med Sci Sports. 2021;31(8):1636-1646. [22] BOBES ÁLVAREZ C, ISSA-KHOZOUZ SANTAMARÍA P, FERNÁNDEZ-MATÍAS R, et al. Comparison of Blood Flow Restriction Training versus Non-Occlusive Training in Patients with Anterior Cruciate Ligament Reconstruction or Knee Osteoarthritis: A Systematic Review. J Clin Med. 2020;10(1):68. [23] WENGLE L, MIGLIORINI F, LEROUX T, et al. The Effects of Blood Flow Restriction in Patients Undergoing Knee Surgery: A Systematic Review and Meta-analysis. Am J Sports Med. 2022;50(10): 2824-2833. [24] GIBSON W, WAND BM, O’CONNELL NE. Transcutaneous electrical nerve stimulation (TENS) for neuropathic pain in adults. Cochrane Database Syst Rev. 2017;9(9):CD011976. [25] HAYDEN JA, ELLIS J, OGILVIE R, et al. Exercise therapy for chronic low back pain. Cochrane Database Syst Rev. 2021;9(9):CD009790. [26] CURRAN MT, BEDI A, MENDIAS CL, et al. Blood Flow Restriction Training Applied With High-Intensity Exercise Does Not Improve Quadriceps Muscle Function After Anterior Cruciate Ligament Reconstruction: A Randomized Controlled Trial. Am J Sports Med. 2020;48(4):825-837. [27] HUGHES L, ROSENBLATT B, HADDAD F, et al. Comparing the Effectiveness of Blood Flow Restriction and Traditional Heavy Load Resistance Training in the Post-Surgery Rehabilitation of Anterior Cruciate Ligament Reconstruction Patients: A UK National Health Service Randomised Controlled Trial. Sports Med. 2019;49(11):1787-1805. [28] ŽARGI T, DROBNIČ M, STRAŽAR K, et al. Short-Term Preconditioning With Blood Flow Restricted Exercise Preserves Quadriceps Muscle Endurance in Patients After Anterior Cruciate Ligament Reconstruction. Front Physiol. 2018;9:1150. [29] IVERSEN E, RØSTAD V, LARMO A. Intermittent blood flow restriction does not reduce atrophy following anterior cruciate ligament reconstruction. J Sport Health Sci. 2016;5(1):115-118. [30] GRAPAR ZARGI T, DROBNIC M, JKODER J, et al. The effects of preconditioning with ischemic exercise on quadriceps femoris muscle atrophy following anterior cruciate ligament reconstruction: a quasi-randomized controlled trial. Eur J Phys Rehabil Med. 2016;52(3):310-320. [31] TAKARADA Y, TSURUTA T, ISHII N. Cooperative effects of exercise and occlusive stimuli on muscular function in low-intensity resistance exercise with moderate vascular occlusion. Jpn J Physiol. 2004;54(6):585-592. [32] Ohta H, Kurosawa H, Ikeda H, et al. Low-load resistance muscular training with moderate restriction of blood flow after anterior cruciate ligament reconstruction. Acta Orthop Scand. 2003; 74(1):62-68. [33] PERRATON L, CLARK R, CROSSLEY K, et al. Impaired voluntary quadriceps force control following anterior cruciate ligament reconstruction: relationship with knee function. Knee Surg Sports Traumatol Arthrosc. 2017;25(5):1424-1431. [34] NEUMAN P, OWMAN H, MÜLLER G, et al. Knee cartilage assessment with MRI (dGEMRIC) and subjective knee function in ACL injured copers: a cohort study with a 20 year follow-up. Osteoarthritis Cartilage. 2014;22(1):84-90. [35] CENTNER C, WIEGEL P, GOLLHOFER A, et al. Effects of Blood Flow Restriction Training on Muscular Strength and Hypertrophy in Older Individuals: A Systematic Review and Meta-Analysis. Sports Med. 2019;49(1):95-108. [36] LIXANDRÃO ME, UGRINOWITSCH C, BERTON R, et al. Magnitude of Muscle Strength and Mass Adaptations Between High-Load Resistance Training Versus Low-Load Resistance Training Associated with Blood-Flow Restriction: A Systematic Review and Meta-Analysis. Sports Med. 2018;48(2):361-378. [37] PECK BD, BRIGHTWELL CR, JOHNSON DL, et al. Anterior Cruciate Ligament Tear Promotes Skeletal Muscle Myostatin Expression, Fibrogenic Cell Expansion, and a Decline in Muscle Quality. Am J Sports Med. 2019;47(6):1385-1395. [38] NOEHREN B, ANDERSEN A, HARDY P, et al. Cellular and Morphological Alterations in the Vastus Lateralis Muscle as the Result of ACL Injury and Reconstruction. J Bone Joint Surg Am. 2016;98(18):1541-1547. [39] HWANG PS, WILLOUGHBY DS. Mechanisms Behind Blood Flow-Restricted Training and its Effect Toward Muscle Growth. J Strength Cond Res. 2019;33 Suppl 1:S167-S179. [40] COUNTS BR, DANKEL SJ, BARNETT BE, et al. Influence of relative blood flow restriction pressure on muscle activation and muscle adaptation. Muscle Nerve. 2016;53(3):438-445. [41] SPRANGER MD, KRISHNAN AC, LEVY PD, et al. Blood flow restriction training and the exercise pressor reflex: a call for concern. Am J Physiol Heart Circ Physiol. 2015;309(9):H1440-H1452. [42] PANAGOPOULOS A, GIANNATOS V, MOROS G, et al. Isokinetic Muscle Strength and Knee Function in Anatomical Anterior Cruciate Ligament Reconstruction With Hamstring Autografts: A Prospective Randomized Comparative Study Between Suspensory and Expandable Femoral Fixation in Male Patients. Cureus. 2022;14(12): e32482. [43] ITHURBURN MP, LONGFELLOW MA, THOMAS S, et al. Knee Function, Strength, and Resumption of Preinjury Sports Participation in Young Athletes Following Anterior Cruciate Ligament Reconstruction. J Orthop Sports Phys Ther. 2019; 49(3):145-153. [44] GRINDEM H, SNYDER-MACKLER L, MOKSNES H, et al. Simple decision rules can reduce reinjury risk by 84% after ACL reconstruction: the Delaware-Oslo ACL cohort study. Br J Sports Med. 2016;50(13):804-808. [45] ITHURBURN MP, PATERNO MV, FORD KR, et al. Young Athletes With Quadriceps Femoris Strength Asymmetry at Return to Sport After Anterior Cruciate Ligament Reconstruction Demonstrate Asymmetric Single-Leg Drop-Landing Mechanics. Am J Sports Med. 2015;43(11):2727-2737. [46] LADLOW P, COPPACK RJ, DHARM-DATTA S, et al. Low-Load Resistance Training With Blood Flow Restriction Improves Clinical Outcomes in Musculoskeletal Rehabilitation: A Single-Blind Randomized Controlled Trial. Front Physiol. 2018; 9:1269. [47] PTASINSKI AM, DUNLEAVY M, ADEBAYO T, et al. Returning Athletes to Sports Following Anterior Cruciate Ligament Tears. Curr Rev Musculoskelet Med. 2022;15(6):616-628. [48] JENKINS SM, GUZMAN A, GARDNER BB, et al. Rehabilitation After Anterior Cruciate Ligament Injury: Review of Current Literature and Recommendations. Curr Rev Musculoskelet Med. 2022;15(3):170-179. [49] SALAGAS A, TSOUKOS A, TERZIS G, et al. Effectiveness of either short-duration ischemic pre-conditioning, single-set high-resistance exercise, or their combination in potentiating bench press exercise performance. Front Physiol. 2022;13:1083299. [50] WAHLSTRØM KL, BJERRUM E, GÖGENUR I, et al. Effect of remote ischaemic preconditioning on mortality and morbidity after non-cardiac surgery: meta-analysis. BJS Open. 2021;5(2):zraa026. [51] JIN Z, ZHENG E, SARELI C, et al. Monocyte Chemotactic Protein-Induced Protein 1 (MCPIP-1): A Key Player of Host Defense and Immune Regulation. Front Immunol. 2021;12:727861. |
| [1] | Bai Chen, Yang Wenqian, Meng Zhichao, Wang Yuze. Strategies for repairing injured anterior cruciate ligament and promoting graft healing [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1457-1463. |
| [2] | Zhong Jun, Wang Wen. Network meta-analysis of different anatomical repair strategies to improve chronic lateral ankle instability [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1470-1476. |
| [3] | Zhang Xihui, Li Zhengrong, Li Shineng, Xing Zengyu, Wang Jiao. Effect of rehabilitation training guided by Pro-kin balance system on proprioception and balance function of the affected knee after anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1259-1264. |
| [4] | Ma Shuwei, He Sheng, Han Bing, Zhang Liaoyun. Exosomes derived from mesenchymal stem cells in treatment of animals with acute liver failure: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1137-1142. |
| [5] | Zhang Zeyi, Yang Yimin, Li Wenyan, Zhang Meizhen. Effect of foot progression angle on lower extremity kinetics of knee osteoarthritis patients of different ages: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 968-975. |
| [6] | Hu Zhixing, Li Qun, Yang Chao, Wang Xiaoxiao, Fang Luochangting, Hou Wuqiong, Lin Na, Chen Weiheng, Liu Chunfang, Lin Ya. Network meta-analysis of the modeling effects of different factors on rabbit models of steroid-induced osteonecrosis of femoral head [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 976-984. |
| [7] | Yu Zhaoyu, Tan Lixin, Sun Kai, Lu Yao, Li Yong. Meta-analysis of cement-augmented pedicle screw for thoracolumbar degenerative diseases with osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(5): 813-820. |
| [8] | Abuduwupuer·Haibier, Alimujiang·Yusufu, Maihemuti·Yakufu, Maimaitimin·Abulimiti, Tuerhongjiang·Abudurexiti. Meta-analysis of efficacy and safety of terlipatide and bisphosphate in the treatment of postmenopausal osteoporosis fractures [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 639-645. |
| [9] | Bai Xiaotian, Chen Zhaoying, Song Yiling, Wang Ye, Liu Jingmin. Effect of minimalist shoes on foot muscle morphology: systematic evaluation and Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 646-650. |
| [10] | Wang Juan, Wang Ling, Zuo Huiwu, Zheng Cheng, Wang Guanglan, Chen Peng. Rehabilitative efficacy of kinesio taping following anterior cruciate ligament reconstruction: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 651-656. |
| [11] | Chang Wanpeng, Zhang Zhongwen, Yang Yulin, Zi Yang, Yang Mengqi, Du Bingyu, Wang Nan, Yu Shaohong. Efficacy of rehabilitation exoskeleton robots on post-stroke lower limb motor dysfunction: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(2): 321-328. |
| [12] | Xie Enli, Tao Huimin. Application trends of blood flow restriction training in clinical rehabilitation [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(2): 258-262. |
| [13] | Wang Ling, Jiang Xia, Chen Peng, Zheng Cheng, Xu Jinrong. Biomechanical characteristics of the lower limbs of athletes after anterior cruciate ligament reconstruction during bilateral vertical jumping [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(14): 2215-2220. |
| [14] | Xiong Bohan, Lu Xiaojun, Xue Wenqiang, Liu Jinrui, Gao Xianling, Yu Hong, Li Yajuan, Liu Haolong, Li Yanlin. Protective effect of anterior cruciate ligament reconstruction assisted by internal tension-reduction technique on the articular cartilage of southern Yunnan small-ear pigs [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(14): 2221-2226. |
| [15] | Zhang Yue, Guo Yingjie, Cheng Yang, Yang Tingting. Effect of blood flow restriction training on the fitness benefit of upper limb muscles [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(14): 2248-2253. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||