Chinese Journal of Tissue Engineering Research ›› 2022, Vol. 26 ›› Issue (12): 1963-1968.doi: 10.12307/2022.524
A systematic review of children’s foot type classification methods
Tang Yunqi1, Zou Lingqiu1, Li Yi2, Wang Zhikang1, Hui Xue1, Li Lingjun1, Guo Xinyu1
- 1College of Art and Design, Shaanxi University of Science and Technology, Xi’an 710021, Shaanxi Province, China; 2Department of Foot and Ankle Surgery, Honghui Hospital Affiliated to Medical College of Xi’an Jiaotong University, Xi’an 710054, Shaanxi Province, China
-
Received:2021-03-06Revised:2021-03-08Accepted:2021-03-31Online:2022-04-28Published:2021-12-15 -
Contact:Li Yi, MD, Chief physician, Department of Foot and Ankle Surgery, Honghui Hospital Affiliated to Medical College of Xi’an Jiaotong University, Xi’an 710054, Shaanxi Province, China -
About author:Tang Yunqi, MD, Associate professor, College of Art and Design, Shaanxi University of Science and Technology, Xi’an 710021, Shaanxi Province, China -
Supported by:the Major Scientific Research Project of Shaanxi Provincial Education Department, No. 21JT002 (to TYQ); a grant from Xi’an Science and Technology Department, No. SF1512(2) (to LY); Shaanxi Provincial Social Development Science and Technology Project, No. 2016SF-333 (to LY)
CLC Number:
Cite this article
Tang Yunqi, Zou Lingqiu, Li Yi, Wang Zhikang, Hui Xue, Li Lingjun, Guo Xinyu. A systematic review of children’s foot type classification methods[J]. Chinese Journal of Tissue Engineering Research, 2022, 26(12): 1963-1968.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
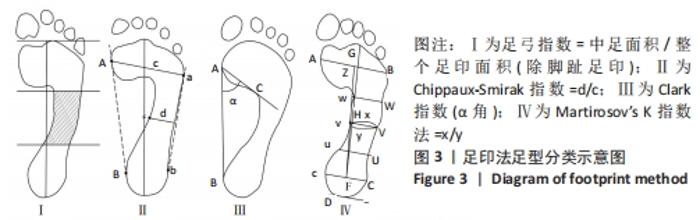
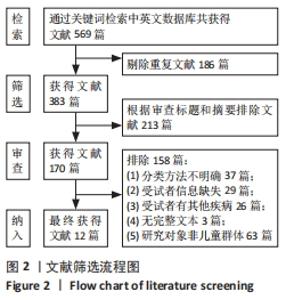
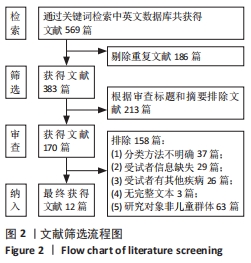
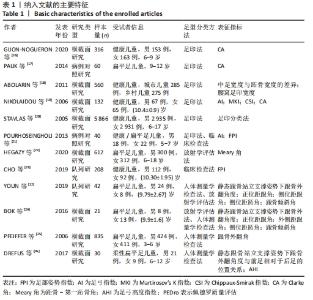
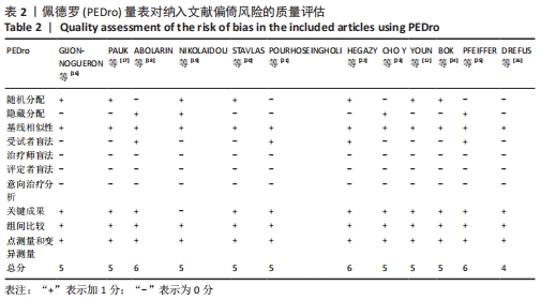
有8篇文献的佩德罗质量评估为5分[12,16-17,19-21,23-24],3篇文献的佩德罗评估为6分[18,22,25],1篇文献的佩德罗评估为4分[26]。有7篇文献采用了随机分配的方法[12,16-17,19-20,22];4篇文献采用了隐藏分配方法[18-19,23,25];纳入的所有文献均具有基线相似性;所有文献都不具有治疗师盲法、评定者盲法和意向治疗分析;所有文献均具有关键成果、组间比较、点测量和变异。文章总体质量水平为中等。 2.4 儿童足型分类分析结果 2.4.1 足印法 有研究提出的足弓指数法是中间1/3的足印面积与除脚趾外的整体足印面积之比,见图3Ⅰ。足弓指数≤0.21为高弓足,Ⅰ≥0.26为扁平足,介于0.21-0.26为正常足[19]。而在POURHOSEINGHOLI等[21]的研究中足型分类标准稍有不同,当足弓指数≤0.21为高弓足,≥0.28为扁平足,介于0.21-0.28为正常足。 Chippaux-Smirak指数定义为中足足印宽占前掌足印宽的百分比,见图3Ⅱ,根据CSI将足型分为5个类型:高弓足(0%)、正常足(0.1%-29.9%)、轻微扁平足(30%-39.9%)、中度扁平足(40%-44.9%)和重度扁平足(≥45%)[19]。 Clarke角定义为前足内侧和后足足印内侧的切线与第一跖骨内侧点和腰窝内侧凹陷点连线的夹角[16],见图3Ⅲ。PAUK等[17]在评估儿童脚型时使用Clarke角,当Clarke角< 42°为扁平足,Clarke角> 48°为高弓足,Clarke角在42°-48°为正常足。此外,Gijon-Nogueron等[16]和Nikolaidou等[19]将足型更详细的区分成以下5种:严重扁平足(0°-29.9°)、中度扁平足(30°-34.9°)、正常足(35°-42°)、高弓足(> 42°)。 Martirosov’s K指数根据x与y的比值将足分为高弓足(≤0.76)、正常足(0.77-1.03)、低弓足(1.04-1.16)和扁平足(≥1.17)4种类型[19],见图3Ⅳ。"
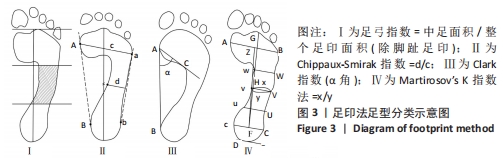
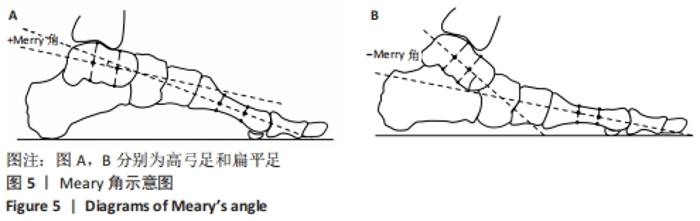
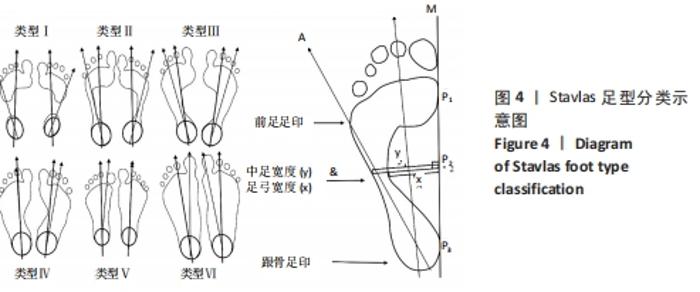
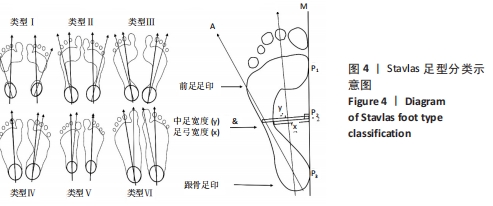
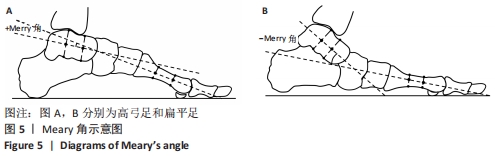
Ⅰ型表示重度高弓足,x=y;Ⅱ型表示轻度高弓足,y>x≥3/4 y;Ⅲ型表示正常足,3/4 y > x≥2/4 y;Ⅳ型与Ⅲ型类似,2/4 y>x≥1/4 y;Ⅴ型表示扁平足,1/4 y > x≥0;Ⅵ型表示重度扁平足,x > y。 2.4.3 足印形态评估法 ABOLARIN等[18]对中足足印的宽度进行足型分类。中足宽度比跖骨宽度短1 cm以内为扁平足,足印内侧边缘有隆起为严重扁平足,腰窝足印宽度小于1 cm为高弓足[18],其他足印均为正常足。 2.4.4 放射学评估法分析结果 Meary角定义为足部负重侧位X射线片距骨长轴中线与第一跖骨长轴之间的夹角[22],见图5。在正常负重状态下,距骨纵轴中线与第一跖骨的长轴汇成一条直线。Meary角的正常范围是-4°至+4°。Meary角> +4°为高弓足,Meary角< -4°为扁平足[22]。"
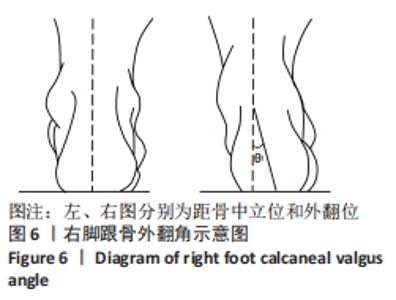
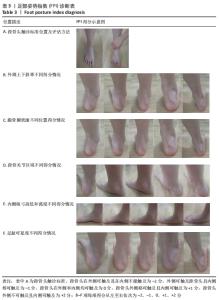
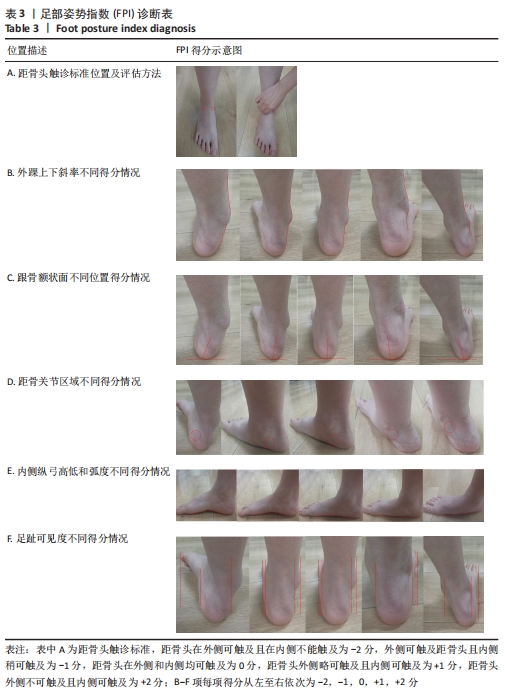
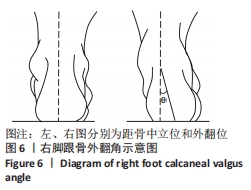
在足部姿势指数的6个项目下,每项标准得分为-2,-1,0,+1,+2分。其中0分为正常,-2分为重度旋后 (supination),+2分为重度旋前(pronation)。得分范围为-12至+12,正值越大,说明足旋前程度越高。0-5分为正常足,+6至+9分为扁平足,+10分以上为重度扁平足,-1至-4为高弓足,-5至-12分为重度高弓足[23]。 2.4.6 人体测量学检查法分析结果 如图6所示,后足角即跟骨外翻角[11],定义为在矢状面上小腿平分线与跟骨平分线上的夹角。外翻角度在-4°-4°为正常足;外翻角度在5°-20°为生理性扁平足;外翻角度≥20°为病理性扁平足;外翻角度≤-5°为高弓足[11]。"
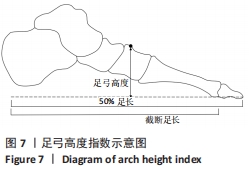
通过跟骨站立姿势和前足到后足的位置关系将儿童足型分为3种类型。扁平足:静态跟骨站立姿势角度≥4°外翻或前足相对于后足≥4°内翻;正常足:静态跟骨支撑姿势0°-2°的外翻且前足相对于后足0°-4°的内翻;高弓足:静态跟骨站立姿势≥0°的内翻且前足相对于后 足≥1°的外翻[26]。 足弓高度指数是临床实践中常用的一种易于操作的足型分类方法[27],见图7。足弓高度指数=足背高度(取足长的50%)/截断足长(从跟骨后端到第一跖骨的长度)[26]。坐姿状态下足型分类标准为:扁平足(≤0.365)、正常足(0.365-0.390)、高弓足(≥0.390)[26]。站立状态下足型分类标准为:扁平足(≤0.345)、正常足(0.345-0.370)及高弓足(≥0.370)[26]。"
| [1] HARRIS EJ. The natural history and pathophysiology of flexible flatfoot. Clin Podiatr Med Surg. 2010; 27(1):1-23. [2] FRANCO AH. Pes cavus and pes planus. Analyses and treatment. Phys Ther. 1987;67(5):688-694. [3] 张燊,张希妮,崔科东,等.足弓的运动功能进展及其在人体运动中的生物力学贡献[J].体育科学,2018,38(5):73-79. [4] 赵碎浪,杨峰,傅陆军,等.足型分类方法研究进展[J].中国皮革,2020,49(7):7-12. [5] CHEN KC, TUNG LC, TUNG CH, et al. An investigation of the factors affecting flatfoot in children with delayed motor development. Res Dev Disabil. 2014; 35(3):639-645. [6] EVANS AM, ROME K. A Cochrane review of the evidence for non-surgical interventions for flexible pediatric flat feet. Eur J Phys Rehabil Med. 2011; 47(1):69-89. [7] ROME K, ASHFORD R, EVANS A. Non-surgical interventions for paediatric pes planus. Cochrane Database Syst Rev. 2010;7(7):CD006311. [8] TONG JW, KONG PW. Association between foot type and lower extremity injuries: systematic literature review with meta-analysis. J Orthop Sports Phys Ther. 2013;43(10):700-714. [9] Dorsey W, MCCIAY IS, HAMILL J. Lower extremity kinematic and kinetic differences in runners with high and low arches. J Appl Biomech. 2001;17(2):153-163. [10] HOLLANDER K, STEBBINS J, ALBERTSEN IM, et al. Arch index and running biomechanics in children aged 10-14 years. Gait Posture. 2018;61:210-214. [11] WHITFORD D, ESTERMAN A. A randomized controlled trial of two types of in-shoe orthoses in children with flexible excess pronation of the feet. Foot Ankle Int. 2007;28(6):715-723. [12] YOUN KJ, AHN SY, KIM BO, et al. Long-term effect of rigid foot orthosis in children older than six years with flexible flat foot. Ann Rehabil Med-ARM. 2019;43(2):224-229. [13] MORRISON SC, TAIT M, BONG E, et al. Symptomatic pes planus in children: a synthesis of allied health professional practices. J Foot Ankle Res. 2020;13(1): 5-7. [14] 汤运启,李静,王志康,等.矫形鞋垫对扁平足人群足底压力分布的影响[J].中国皮革,2019, 48(11):55-61. [15] DARS S, UDEN H, BANWELL HA, et al. The effectiveness of non-surgical intervention (Foot Orthoses) for paediatric flexible pes planus: a systematic review: update. PLoS One. 2018;13(2): e0193060. [16] GIJON-NOGUERON G, MARCHENA-RODRIGUEZ A, MONTES-ALGUACIL J, et al. Evaluation of the paediatric foot using footprints and foot posture index: a cross-sectional study. J Paediatr Child Health. 2020;56(2):201-206. [17] PAUK J, IHNATOUSKI M, NAJAFI B. Assessing plantar pressure distribution in children with flatfoot arch: application of the Clarke angle. J Am Podiatr Med Assoc. 2014;104(6):622-632. [18] ABOLARIN T, AIYEGBUSI A, TELLA A, et al. Predictive factors for flatfoot: the role of age and footwear in children in urban and rural communities in South West Nigeria. Foot. 2011;21(4):188-192. [19] NIKOLAIDOU ME, BOUDOLOS KD. A footprint-based approach for the rational classification of foot types in young schoolchildren. Foot. 2006;16(2):82-90. [20] STAVLAS P, GRIVAS TB, MICHAS C, et al. The evolution of foot morphology in children between 6 and 17 years of age: a cross-sectional study based on footprints in a Mediterranean population. J Foot Ankle Surg. 2005;44(6):424-428. [21] POURHOSEINGHOLI E, POURHOSEINGHOLI MA. Comparison of arch index of flat foot and healthy foot in pre-school children. Thrita. 2013;2(3):15-18. [22] HEGAZY FA, ABOELNASR EA, SALEM Y, et al. Validity and diagnostic accuracy of foot posture Index-6 using radiographic findings as the gold standard to determine paediatric flexible flatfoot between ages of 6–18 years: a cross-sectional study. Musculoskel Sci Prac. 2020;46:102-107. [23] CHO Y, PARK JW, NAM K. The relationship between foot posture index and resting calcaneal stance position in elementary school students. Gait Posture. 2019;74:142-147. [24] BOK SK, LEE H, KIM BO, et al. The effect of different foot orthosis inverted angles on plantar pressure in children with flexible flatfeet. PLoS One. 2016; 11(7):e0159831. [25] PFEIFFER M, KOTZ R, LEDL T, et al. Prevalence of flat foot in preschool-aged children. Pediatrics. 2006; 118(2):634-639. [26] DREFUS LC, KEDEM P, MANGAN SM, et al. Reliability of the arch height index as a measure of foot structure in children. Pediatr Phys Ther. 2017;29(1): 83-88. [27] JAFARNEZHADGERO A, MADADI SHAD M, FERBER R. The effect of foot orthoses on joint moment asymmetry in male children with flexible flat feet. J Bodyw Mov Ther. 2018;22(1):83-89. [28] HOSL M, BOHM H, OESTREICH C, et al. Self-perceived foot function and pain in children and adolescents with flexible flatfeet -Relationship between dynamic pedobarography and the foot function index. Gait Posture. 2020;77(5):225-230. [29] LING E, LEPOW B, ZHOU H, et al. The impact of diabetic foot ulcers and unilateral offloading footwear on gait in people with diabetes. Clin Biomech. 2020;73:157-161. [30] BÖHM H, DÖDERLEIN L, FUJAK A, et al. Is there a correlation between static radiographs and dynamic foot function in pediatric foot deformities? Foot Ankle Surg. 2019;26(7):801-809. [31] 白啸天,霍洪峰.足踝功能的生物力学测评:构建足静态和动态评价指标[J].中国组织工程研究,2021,25(17):2747-2754. |
| [1] | Li Kun, Gao Erke, Xiong Feng, Wang Xing, Wu Danqi, Li Zhijun, Zhang Shaojie, Liu Yanan, Duo Lan, Li Ziyu. Feasibility of axial transpedicle screw internal fixation in children aged 1 to 6 years [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1383-1387. |
| [2] | Liu Yuhang, Zhou Jianqiang, Xu Xuebin, Qu Xingyue, Li Ziyu, Li Kun, Wang Xing, Li Zhijun, Li Xiaohe, Zhang Shaojie. Establishment and validation of finite element model of lower cervical spine in 6-year-old children [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 870-874. |
| [3] | Song Yan, Zheng Kun, Wei Haoxin, Lu Dezhi, Xu Yuanjing, Wang Xiaowen, Wang Jinwu. reliability of flat feet evaluated by foot posture index and its application in three-dimensional printing insoles [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(3): 344-349. |
| [4] | Kan Jie. Guidelines for exercise during pregnancy in developed countries and revelation for the Healthy China Action [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(2): 308-314. |
| [5] | Li Kun, Wang Xing, Li Zhijun, Gao Shang, Sun Hao, Xiong Feng, Wang Peng . Three-dimensional finite element analysis of anterior cervical fixation system in children [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(12): 1866-1871. |
| [6] | Luo Lin, Song Naiqing, Huang Jin, Zou Xiaodong. Review and prospect of international research on preschool children’s movement development assessment: a CiteSpace-based visual analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1270-1276. |
| [7] | Xiong Feng, Li Kun, Zhou Shuyu, Wang Peng, Dang Yexing, Li Zhijun, Zhang Shaojie. Feasibility of atlantoaxial pedicle screw or lateral mass screw fixation in preschool children [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(36): 5804-5809. |
| [8] | Ji Zhongqiu, Li Jiahui, Zhao Panchao, Jiang Guiping. Biomechanical characteristics of children with different body weights during vertical jump [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(33): 5281-5287. |
| [9] | Zhong Ruixin, Gao Haiyan, Huang Haoran, Teng Xueren, Dai Shiyou. Anatomical features of anterior cruciate ligament on MRI in children, adolescents and adults [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(30): 4812-4817. |
| [10] | Tan Jiachang, Yuan Zhenchao, Wu Zhenjie, Liu Bin, Zhao Jinmin. Biomechanical analysis of elastic nail combined with end caps and wire fixation for long oblique femoral shaft fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 334-338. |
| [11] | Li Kun, Li Zhijun, , Zhang Shaojie, Gao Shang, Wang Xing, Sun Hao, He Yujie, Wang Haiyan, Cai Yongqiang, , Xu Xuebin. Titanium plate placement for internal fixation of slopes in children aged 1-6 years: digital morphological analysis of mechanical support [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(27): 4289-4293. |
| [12] | Li Kun, Li Zhijun, Zhang Shaojie, Gao Shang, Sun Hao, Yang Xi, Wang Xing, Dai Lina . A 4-year-old child model of occipito-atlanto-axial joints established by finite element dynamic simulation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3773-3778. |
| [13] | Qu Xingyue, Zhou Jianqiang, Xu Xuebin, Zhang Shaojie, Li Zhijun, Wang Xing. Finite element analysis of screw-bone anti-pullout in four models of anterior lower cervical fixation in children [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2816-2821. |
| [14] | Li Yang, Jiang Shuyun, Li Yiying, Yu Yan, Lu Xiaoying, Wang Danci . Spatiotemporal, kinematic and kinetic characteristics of gait in children with genu valgus [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(15): 2303-2308. |
| [15] | Liu Yongyu, Xu Jingli, Lin Tianye, Wu Feng, Shen Chulong, Xiong Binglang, Zou Qizhao, Lai Qizhong, Zhang Qingwen . Medium-and long-term follow-up of Salter pelvic osteotomy and implant fixation for children with developmental hip dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(15): 2380-2384. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||