Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (18): 2816-2821.doi: 10.3969/j.issn.2095-4344.3843
Previous Articles Next Articles
Finite element analysis of screw-bone anti-pullout in four models of anterior lower cervical fixation in children
Qu Xingyue1, Zhou Jianqiang2, Xu Xuebin1, Zhang Shaojie3, Li Zhijun3, 4, Wang Xing3, 4
- 1Graduate School, 3Department of Anatomy of Basic Medical School, 4Center of Digital Medicine, Inner Mongolia Medical University, Hohhot 010059, Inner Mongolia Autonomous Region, China; 2First Hospital of Hohhot, Hohhot 010000, Inner Mongolia Autonomous Region, China
-
Received:2020-07-20Revised:2020-07-22Accepted:2020-08-19Online:2021-06-28Published:2021-01-11 -
Contact:Zhang Shaojie, Associate professor, Master’s supervisor, Department of Anatomy of Basic Medical School, Inner Mongolia Medical University, Hohhot 010059, Inner Mongolia Autonomous Region, China -
About author:Qu Xingyue, Master, Graduate School, Inner Mongolia Medical University, Hohhot 010059, Inner Mongolia Autonomous Region, China Zhou Jianqiang, Master, First Hospital of Hohhot, Hohhot 010000, Inner Mongolia Autonomous Region, China Qu Xingyue and Zhou Jianqiang contributed equally to this article. -
Supported by:the National Natural Science Foundation of China, No. 81660358 (to ZSJ); the National Natural Science Foundation of China, No. 81860383 (to LZJ); the National Natural Science Foundation of China, No. 81860382 (to WX); the Natural Science Foundation of Inner Mongolia Autonomous region, No. 2019MS08017 (to ZSJ)
CLC Number:
Cite this article
Qu Xingyue, Zhou Jianqiang, Xu Xuebin, Zhang Shaojie, Li Zhijun, Wang Xing. Finite element analysis of screw-bone anti-pullout in four models of anterior lower cervical fixation in children[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2816-2821.
share this article
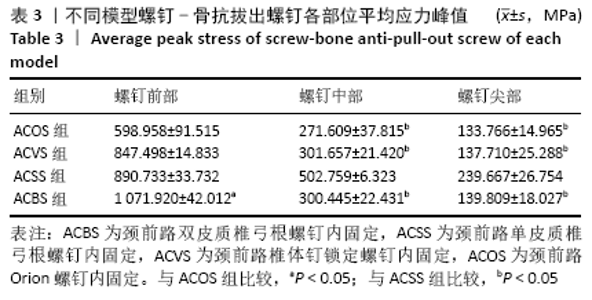
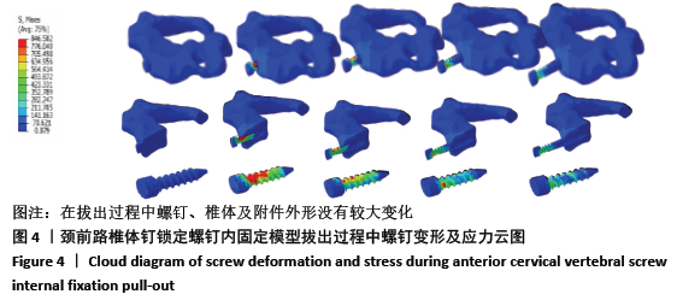
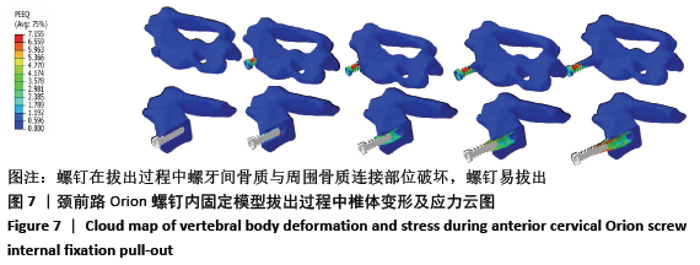
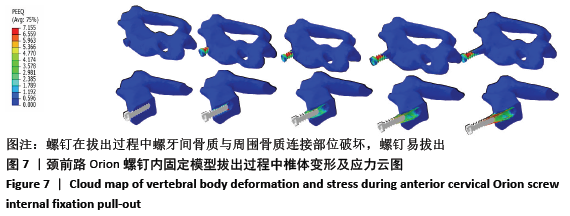
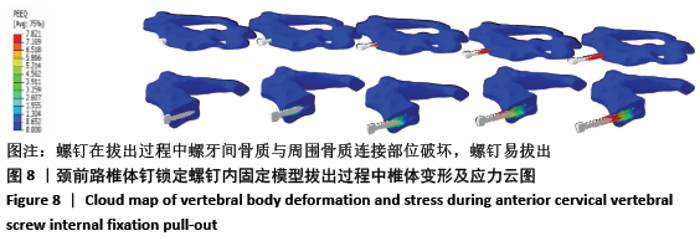
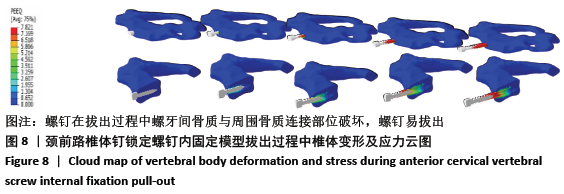
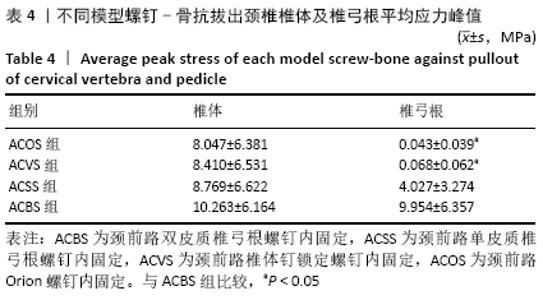
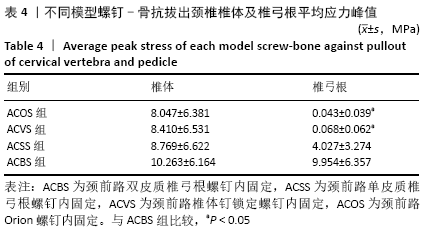
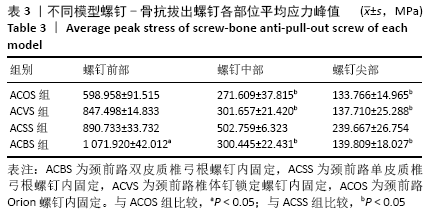
2.3 各种内固定模型螺钉抗拔出应力峰值比较 按照螺钉长度平均分成15份,其中前部5份、中部5份、尖部5份,测出4种内固定模型螺钉前、中、后3个部位的抗拔出应力峰值;按照双皮质螺钉通道长度将颈椎平均分成5份,分别测出4种内固定模型螺钉-骨抗拔出颈椎椎体及椎弓根应力峰值。 由表3可知,ACBS组螺钉前部应力峰值最大,ACSS组螺钉中部应力峰值最大,考虑ACBS组实验过程中螺钉尖部与后方骨皮质一直未松动,可以认为在骨质破坏一瞬间应力传递于骨质破坏部分停止,未传导至螺钉尖部,所以在螺钉尖部应力较ACSS组小。ACBS组螺钉前部平均应力峰值与ACOS组存在显著性差异(χ2=16.714,P=0.001);ACSS组螺钉中部平均应力峰值与其余3组均存在显著差异(F=58.828,P=0.000 01);ACSS组螺钉尖部平均应力峰值与其余3组均存在显著差异(F=27.691,P=0.000 01)。 "
| [1] KATAR S, AYDIN OP, OZEL M, et al. Pediatric Spinal Traumas. Pediatr Neurosurg. 2020;55(2):86-91. [2] ERBULUT DU, ZAFARPARANDEH I, HASSAN CR, et al. Determination of the biomechanical effect of an interspinous process device on implanted and adjacent lumbar spinal segments using a hybrid testing protocol: a finite-element study. J Neurosurg Spine. 2015;23(2):200-208. [3] HALL DE, BOYDSTON W. Pediatric Neck Injuries. Pediatr Rev. 1999;20(1):13-20. [4] EASTER JS, BARKIN R, ROSEN CL, et al. Cervical spine injuries in children, part II: management and special considerations. J Emerg Med. 2011;41(3): 252-256. [5] ZAFARPARANDEH I, ERBULUT DU, LAZOGLU I, et al. Development of a finite element model of the human cervical spine. Turk Neurosurg. 2014;24(3): 312-318. [6] FU M, LIN L, KONG X, et al. Construction andaccuracy assessment of patient-specific biocompatible drill template forcervical anterior transpedicular screw (ATPS) insertion: an in vitro study. PLoS One. 2013;8(1):e53580. [7] TAN KA, LIN SX, CHIN BZ, et al. Anatomic techniques for cervical pedicle screw placement. J Spine Surg. 2020;6(1):262-273. [8] WU HH, TANG T, YU X, et al. Stability of two anterior fixations for three-column injury in the lower cervical spine: biomechanical evaluation of anterior pedicle screw-plate fixation. J Int Med Res. 2018;46(4):1455-1460. [9] ROBINSON RA, SMITH GW. Anterolateral cervical disc removal and interbody fusion for cervical disc syndrome. Sas J. 2010;4(1):34-35. [10] DE OLIVEIRA JC. Anterior plate fixation of traumatic lesions of the lower cervical spine. Spine (Phila Pa 1976). 1987;12(4):324-329. [11] HAID RW, FOLEY KT, RODTS GE, et al. The Cervical Spine Study Group anterior cervical plate nomenclature. Neurosurg Focus. 2002;12(1):1-6. [12] ZHAO LJ, XU RM, JIANG WY, et al. A new technique for anterior cervical pedicle screw implantation. Orthop Surg. 2011;3(3):193-198. [13] KOTHE R, RÜTHER W, SCHNEIDER E, et al. Biomechanical Analysis of transpedicular screw fixation in the subaxial cervical Spine. Spine (Phila Pa 1976). 2004;29(17):1869-1875. [14] YUKAWA Y, KATO F, ITO K, et al. Anterior cervical pedicle screw and plate fixation using fluoroscope-assisted pedicle axis view imaging: a preliminary report of a new cervical reconstruction technique. Eur Spine J. 2009;18(6):911-916. [15] KOLLER H, ACOSTA F, TAUBER M, et al. Cervical anterior transpedicularscrew fixation (ATPS)--Part II. Accuracy of manual insertion and pull-outstrength of ATPS. Eur Spine J. 2008;17(4):539-555. [16] ZHAO LJ, CHEN JQ, LIU JY, et al. Biomechanical analysis on of anterior transpedicular screw-fixation after two-level cervical corpectomy using finite element method. Clin Biomech. 2018;60(undefined):76-82. [17] 吕文乐,阮世捷,李海岩,等.6岁儿童全颈有限元模型的构建及验证[J].医用生物力学, 2016,31(2):95-101. [18] 罗培杰,袁凯,李大星,等.长、短节段椎弓根螺钉并骨水泥强化治疗骨质疏松性胸腰段椎体骨折的有限元分析[J].中国组织工程研究, 2020,24(3):342-347. [19] ZHANG QH, TAN SH, CHOU SM. Effects of bone materials on the screw pull-out strength in human spine. Med Eng Phys. 2006;28(8):795-801. [20] 胡晓晖,洪翔,何冰,等.基于Simpleware全颈椎三维有限元模型的构建与分析[J].医用生物力学,2014,29(6):530-535. [21] ARAMOMI M, MASAKI Y, KOSHIZUKA S, et al. Anterior pedicle screw fixation for multilevel cervical corpectomy and spinal fusion. Acta Neurochir. 2008;150(6):575-582. [22] JONES EL, HELLER JG, SILCOX DH, et al. Cervical pedicle screws versus lateral mass screws:Anatomic feasibility and biomechanical comparison. Spine (Phila Pa 1976). 1997;22(9):977-982. [23] HEDEQUIST D. Modern instrumentation of the pediatric occiput and upper cervical spine: review article. HSS J. 2015;11(1):9-14. [24] XU M, YANG J, LIEBERMAN IH, et al. Finite element method-based study of pedicle screw–bone connection in pullout test and physiological spinal loads. Med Eng Phys. 2019;67(undefined):11-21. [25] HUSSAIN M, NATARAJAN RN, CHAUDHARY G, et al. Relative contributions of strain-dependent permeability and fixed charged density of proteoglycans in predicting cervical disc biomechanics: a poroelastic C5-C6 finite element model study. Med Eng Phys. 2011;33(4):438-455. [26] BECHTOL CO, FERGUSON AB, LAING PG. Metals and engineering in bone and joint Surgery. Cal West Med. 1959;91(5):303-304. [27] HELLER JG, ESTES BT, ZAOUALI M, et al. Biomechanical study of screws in the lateral masses: variables affecting pull-out resistance. J Bone Joint Surg Am. 1996;78(9):1315-1321. [28] ESCHLER A, ENDER SA, SCHIML K, et al. Bony healing of unstable thoracolumbar burst fractures in the elderly using percutaneously applied titanium mesh cages and a transpedicular fixation system with expandable screws. PLoS One. 2015; 10(4):e0124591. [29] YASUTSUGU Y, FUMIHIKO K, KEIGO I, et al. Anterior cervical pedicle screw and plate fixation using fluoroscope-assisted pedicle axis view imaging: a preliminary report of a new cervical reconstruction technique. Eur Spine J. 2009;18(6):911-916. [30] LIU GY, XU RM, MA WH, et al. A static mechanical comparison between two transarticular internal fixation techniques in the lower cervical spine. Zhonghua Yi Xue Za Zhi. 2007;23(7):1599-1602. [31] XIAO H, YANG J, FENG X, et al. Comparing complications of vertebroplasty and kyphoplasty for treating osteoporotic vertebral compression fractures:a meta-analysis of the randomized and non-randomized controlled studies. Eur J Orthop Surg Traumatol. 2015;25 Suppl 1:S77-S85. [32] 王景续.采用椎弓根钉“双皮质”固定治疗老年骨质疏松性椎体骨折的近期疗效观察[J].中国矫形外科杂志,2011,19(22):1863-1865. [33] 杨卫良,祈全,陆晓峰,等.椎弓根钉“双皮质”固定技术治疗老年人腰椎滑脱及腰椎失稳症[J].中国组织工程研究与临床康复,2009, 13(48):9526-9530. [34] KARAMI KJ, BUCKENMEYER LE, KIAPOUR AM, et al. Biomechanical evaluation of the pedicle screw insertion depth effect on screw stability under cyclic loading and subsequent pullout. J Spinal Disord Tech. 2015;28(3):E133-139. |
| [1] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [2] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [3] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [4] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [5] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [6] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [7] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [8] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [9] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [10] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [11] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [12] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [13] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [14] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [15] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||