Chinese Journal of Tissue Engineering Research ›› 2022, Vol. 26 ›› Issue (35): 5707-5715.doi: 10.12307/2022.1009
Previous Articles Next Articles
Hot topics and international frontiers of electromyography in the field of body movements
Liu Yang1, Zhu Zhiqiang2, Zhao Xiaowei1, Xiang Yujie1, Xiao Jian1, Cheng Lifen1
- 1School of Physical Education, Nanchang Normal University, Nanchang 330023, Jiangxi Province, China; 2Harbin Sport University, Harbin 150001, Heilongjiang Province, China
-
Received:2022-02-07Accepted:2022-03-03Online:2022-12-18Published:2022-05-18 -
Contact:Zhu Zhiqiang, PhD, Professor, Doctoral supervisor, Harbin Sport University, Harbin 150001, Heilongjiang Province, China Cheng Lifen, PhD candidate, Professor, School of Physical Education, Nanchang Normal University, Nanchang 330023, Jiangxi Province, China -
About author:Liu Yang, PhD, Associate professor, School of Physical Education, Nanchang Normal University, Nanchang 330023, Jiangxi Province, China -
Supported by:the Science and Technology Research Project of Jiangxi Provincial Department of Education, No. GJJ212628 (to LY)
CLC Number:
Cite this article
Liu Yang, Zhu Zhiqiang, Zhao Xiaowei, Xiang Yujie, Xiao Jian, Cheng Lifen. Hot topics and international frontiers of electromyography in the field of body movements[J]. Chinese Journal of Tissue Engineering Research, 2022, 26(35): 5707-5715.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
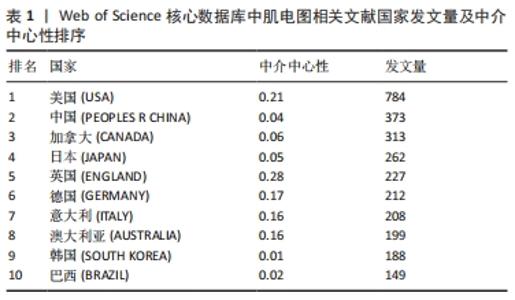
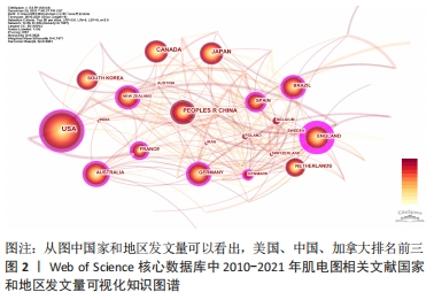
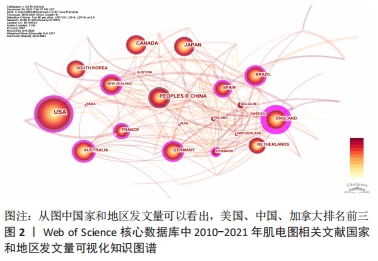
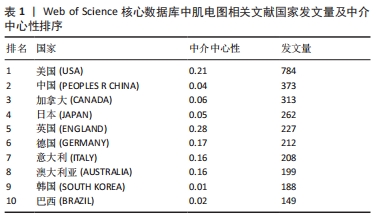
不同国家和地区的发文量及影响力不同:排名第1是美国(USA),发文量为784篇,中介中心性为0.21;第2是中国(PEOPLES R CHINA),发文数量373篇,中介中心性0.04;第3为加拿大(CANADA),发文量为313篇,中介中心性0.06;第4是日本(JAPAN),发文量为262篇,中介中心性0.05;第5是英国(ENGLAND),发文量为227篇,中介中心性0.28;第6是德国(GERMANY)发文量为212篇,中介中心性0.17;第7是意大利(ITALY),发文量为208篇,中介中心性0.16;第8是澳大利亚(AUSTRALIA),发文量为199篇,中介中心性0.16;第9是韩国(SOUTH KOREA),发文量为188篇,中介中心性0.01;第10是巴西(BRAZIL),发文量为149篇,中介中心性0.02。从发文量来看,美国、中国和加拿大排名前3名;从中介中心性来看(紫色外圈),美国、英国和法国排名前3。见表1。 "
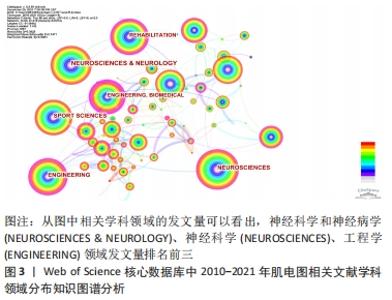
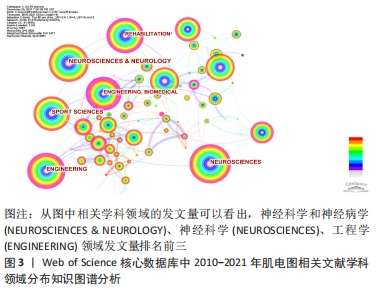
2.1.2 文献学科领域分布 Citespace V界面中,节点类型(Node Types)选择category(学科领域),时间分割(time slicing)选择1年运行后共形成了节点n=96,E=216,Q=0.382 6 > 0.3,神经科学和神经病学(NEUROSCIENCES & NEUROLOGY);神经科学发文量为2 182篇;工程学(ENGINEERING)发文量为756篇;体育科学(SPORT SCIENCES)发文量为716篇;康复工程(REHABILITATION)发文量为586篇,生物医学(CLINICAL NEUROLOGY)发文量为472篇;生理学(PHYSIOLOGY)发文量为380篇;临床神经病学(CLINICAL NEUROLOGY)发文量为376篇;骨科(ORTHOPEDICS)发文量为230篇;心理学(PSYCHOLOGY)发文量为196篇;科学和技术-其他主题(SCIENCE & TECHNOLOGY-OTHER TOPICS)发文量为170篇,可以说表面肌电技术在人体中较多领域广泛应用,主要在神经领域、工程学和体育科学领域发文量较多,排在前3位。见图3。"

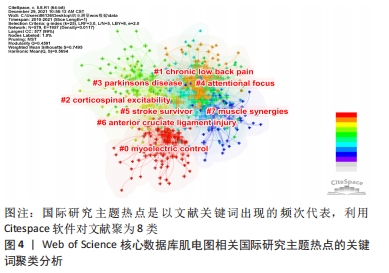
2.2 国际研究主题热点分析 研究主题热点是在某一个时间段内,有内在联系的、数量相对较多的一组论文所探讨的研究问题或专题,出现频次高的关键词和名词短语通常用来代表某一研究领域的热点主题[8]。Citespace V软件的节点类型(Node Types)选择keyword,时间分割(time slicing)选择1年,阈值项选择“Top N per slice”,节点阈值设定为每个切片中频次最高的50。修剪选择minimum spaning tree点击运行。在运动图像窗口点击自动聚类,共聚成了8个聚类,形成了节点n=579,E=1 957,Q=0.459 1 > 0.3。这8聚类也是主要肌电图学在人体测量应用主要分类:第1类肌电控制(myoelectric control);第2聚类慢性下腰痛(chronic low back pain);第3聚类皮质脊髓兴奋性(corticospinal excitability);第4聚类帕金森病(Parkinson’s disease);第5聚类注意力(attentional focus);第6聚类中风存活患者(stroke survivor);第7聚类膝关节前交叉韧带损伤(anterior cruciate ligament 简称ACL);第8聚类肌肉协同(muscle synergies)。见图4。"
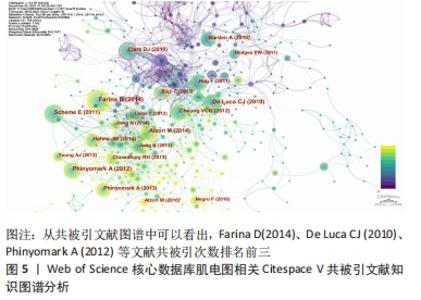
第1聚类:肌电控制(myoelectric control),该聚类探究的是提取、预处理、处理原始肌电信号的方法,如现阶段工程学领域的肌电数据识别提取方法等工程学研究不断深入或利用机器学习[9]、深度学习(deep learning)[10]、模式识别(pattern recognition)以及各种人体运动中测量方法和文献不断出现。相关研究报道为肌电图应用寻找处理肌电数据方法提供文献支撑和参考,如采用非负矩阵因式分解法,从不同肌肉的肌电图数据中提取肌肉协同效应的方法[11]。 第2聚类:慢性下腰痛(chronic low back pain)[12-17],该聚类关注躯干肌肉活动(trunk muscle activity);下腰痛(low back pain);预期姿势调整(anticipatory postural adjustment);背部疼痛(back pain)等相关研究,这些关键词主要针对职业病/办公室人群或者腰部损伤人群相关报道。 第3聚类:皮质脊髓兴奋性(corticospinal excitability)[18-27],人类脊髓损伤(human spinal cord injury)等关键词[28],这些关键词是表面肌电技术测量应用到人体康复、假肢等领域。 第4聚类:帕金森病(Parkinson’s disease)[29-36],面部肌肉激活模式(facial muscle activation pattern),节律性肌肉活动(rhythmic muscle activity),运动性震颤(kinetic tremor),自主收缩(voluntary movement)等关键词,这些关键词聚类主要关注患有神经系统疾病节律性肌肉活动帕金森病患者治疗和机制研究。 第5聚类:注意焦点状态(attentional focus)[37-41],同在一个类中有神经肌肉激活(neuromuscular activation),如不同注意焦点状态对肌肉抗阻活动的影响,评价肌肉力量和训练经验对肌肉活动的可能影响。一般来说,内部注意力集中已经被证明可以增强对运动的有意识控制,从而在运动系统中诱发“噪音”。 第6聚类:脑卒中存活患者(stroke survivor)[10,42-47],脑卒中后患者(post-stroke patient)[48],慢性脑卒中(chronic stroke)。此关键词聚类,关注中风患者的电刺激或者训练后干预情况,近些年备受专家、学者关注。 第7聚类:前交叉韧带(anterior cruciate ligament injury,简称ACL)损伤[49-54],该聚类探究关注肌电关注膝关节损伤,以及生物力学分析(biomechanical analysis)[55],表面肌电信号(sEMG)具有分析人体下肢运动能力,包括人类步态步态评估(human gait)和关节角度估计等,可以为人体与外骨骼矫形器的交互作用提供高水平支持。 第8聚类:肌肉协同(muscle synergies)[56-63],健康人动作控制(healthy human | motor control);神经力学适应(neuromechanical adaptation),环境依赖性变化(context-dependent change);健康成人(healthy adult),肌肉力量(muscle force)[48]。肌肉协同和动作控制方面研究如在运动过程中利用多通道肌电记录仪将肌电记录下来,然后根据运动中每块肌肉放电顺序和肌电幅度,结合高速摄像等技术,对人体动作进行评估和诊断[64]。 2.3 国际研究前沿分析 2.3.1 共被引文献图谱分析 节点类型(Node Types)选择Reference 时间分割(time slicing)选择1年,阈值项选择“Top N per slice”,节点阈值设定为每个切片中频次最高的50。在控制面板中,阈值(Threshold)设置25,字体大小(font size)设置为5,节点(node size)设置200,运行Citespace软件后共得到节点n=925,E=2 374,Q=0.382 6 > 0.3,生成图5。 "
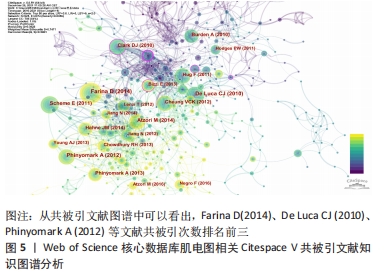

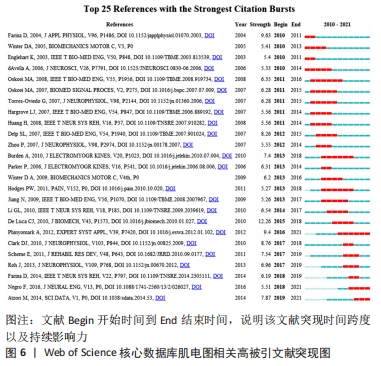
从分析结果可以看出,按引用次数排名第1位的文献是(Farina D,2014),共被引用次数为72次;第2位文献是(De Luca CJ,2010),共被引用次数为53次;第3位文献是(Phinyomark A,2012),共被引用次数为51次;第4位文献是(Atzori M,2014),共被引用次数为45次;第5位文献是(Scheme E,2011),共被引用次数为41次;第6位文献是(Hahne JM,2014),共被引用次数为38次;第7位文献是(Clark DJ,2010),共被引用次数为36次;第8位文献是(Cheung VCK,2012),共被引用次数为35次;第9位文献是(Phinyomark A,2013),共被引用次数为35次;第10位文献是(Burden A,2013),共被引用次数为35次。从共被引文献可知相关文献在一定的时间段内论文的高被引的次数,说明文献的重要性,见表2,通过文献传输的方式下载和阅读,了解前沿趋势。 "


(1)早期研究前沿(2010-2016):重点关注表面肌电图的整体特征与潜在的生理过程之间的关系研究[65],多数文献存在学术争议包括肌电采集、处理的方法(线性、非线性肌电信号处理)以及到肌电信号的检测、处理、分类和指标选择(RMS、IEMG、MDF…等)。肌电信号由原始生物电信号和干扰噪声信号组成,原始肌电图的振幅可以通过滤波、平滑和重新线性化的方案来进行处理,如利用小波分析或者因子分解算法提取原始生物电信号[66]。 原始肌电信号处理也受很多因素的影响,如噪声干扰(检测仪器、环境电磁0-60 Hz低频部分)、电极粘贴方法如电极间距离[67]、采样时姿势、电阻影响、动作方式(解剖和生理)、脂肪厚度、性别与年龄、容积传导等等对原始肌电信号影响较大。由于多数肌电控制方案都利用了表面肌电的宏观特征,而这些特征又依赖于信号中所包含的神经和外周信息,其表现受到影响动作电位形状或神经驱动到肌肉因素的影响[65]。电极对重新定位、电极-皮肤之间阻抗变化(如出汗、毛发)、肌肉与电极相对运动因素包括肌纤维拉长、缩短或向心、离心收缩时的解剖学位置变化影响肌电信号采集。受试者个体之间动作电位形状的分布存在差异,不同肌肉、个体之间比较时,要注意进行肌电均方根值标准化。依据研究方案设计不同,表面肌电图时域、频域分析方法有较大差异。除了上述因素,较多影响因素不是直观的,肌电设备进行人体肢体动作试验时要特别注意肌电设备操作条件,规避影响肌电图/信号的因素,保证表面肌电信息采集客观性以及分析的准确性。 (2)最新研究前沿(2017-2021):肌电图最新前沿领域研究在商业和临床研究有较多延伸。肌萎缩性脊髓侧索硬化症(Amyotrophic lateral sclerosis,简称渐冻症)、脑干中风、脑或脊髓损伤、脑瘫、肌肉营养不良、多发性硬化症和许多其他疾病会损害控制肌肉的神经通路或损害运动细胞。那些受影响最严重的患者可能会失去所有的自主肌肉控制能力,并可能完全锁定在身体内,无法以任何方式进行交流。现代生命支持技术可以让大多四肢瘫痪/残疾患者,能够更好地适应生活,让他们能与外界进行互动、减轻痛苦。假肢或者辅助性设备是利用人机交互界面的肌电信号实现神经康复辅助设备的控制,在研究过程中,利用肌电设备探测大脑和其他脊髓上区域[68]、周围神经或肌组织接口肌电信号信息得以实现人机交互,如通过采集正常人体肌肉活动动作的表面肌电活动信号信息来设计假体肌电信号模式[69],或制作假肢肌电激活数学模型进行人机功效学等领域探索[70-71]。 "

| [1] GROSS D, GRASSINO A, ROSS WR, et al. Electromyogram pattern of diaphragmatic fatigue. J Appl Physiol Respir Environ Exerc Physiol. 1979;46(1):1-7. [2] DE LUCA CJ. Myoelectrical manifestations of localized muscular fatigue in humans. Crit Rev Biomed Eng. 1984;11(4):251-279. [3] 江婉婷,王兴,江志鹏. 国外肌肉衰减综合征的运动疗法研究热点与内容分析——基于科学知识图谱的可视化研究[J].体育科学, 2017,37(6):75-83. [4] 刘洋,王德新,程丽芬,等.基于运动生物力学视角研究运动性疲劳干预方案的可视化知识图谱分析[J].中国组织工程研究,2019, 23(27):4291-4299. [5] 邢聪,吴瑛,项贤林.美国运动损伤前沿研究热点与内容分析--基于科学知识图谱的可视化研究[J].体育科学,2016,36(9):66-72. [6] 水祎舟,黄竹杭.耿建华. 国外足球运动体能训练前沿热点与演化分析--基于科学知识图谱的可视化研究[J].体育科学,2016(1):67-78. [7] 李小芬,许佳慧.国内外体育舞蹈研究进展分析——基于科学知识图谱的可视化研究[J].北京体育大学学报,2018,41(4):89-97. [8] 李欢.彭燕.近十年录像示范法在自闭症谱系障碍干预研究中的国际热点主题和研究前沿分析[J].中国特殊教育,2018(10):26-32. [9] SHE H, ZHU JY, TIAN Y, et al. SEMG Feature Extraction Based on Stockwell Transform Improves Hand Movement Recognition Accuracy. Sensors (Basel). 2019;19(20):4457. [10] LI Y, ZHANG X, GONG Y, et al. Motor Function Evaluation of Hemiplegic Upper-Extremities Using Data Fusion from Wearable Inertial and Surface EMG Sensors. Sensors (Basel). 2017;17(3):582. [11] KRISTIANSEN M, SAMANI A, MADELEINE P, et al. Muscle synergies during bench press are reliable across days. J Electromyogr Kinesiol. 2016;30:81-88. [12] ALSUBAIE AM, MARTINEZ-VALDES E, DE NUNZIO AM, et al. Trunk control during repetitive sagittal movements following a real-time tracking task in people with chronic low back pain. J Electromyogr Kinesiol. 2021;57:102533. [13] CHRISTE G, AUSSEMS C, JOLLES BM, et al. Patients With Chronic Low Back Pain Have an Individual Movement Signature: A Comparison of Angular Amplitude, Angular Velocity and Muscle Activity Across Multiple Functional Tasks. Front Bioeng Biotechnol. 2021;9:76974. [14] DANEAU C, TÉTREAU C, DEROCHE T, et al. Impact of load expectations on neuromuscular and postural strategies during a freestyle lifting task in individuals with and without chronic low back pain.PLoS One. 2021;16(2):e0246791. [15] JONES SL, HITT JR, HENRY SM. Dual goals of trunk restriction and stability are prioritized by individuals with chronic low back pain during a volitional movement.Gait Posture. 2021;90:16-22. [16] LI X, LO WLA, LU SW, et al. Trunk muscle activity during pressure feedback monitoring among individuals with and without chronic low Back pain. BMC Musculoskelet Disord. 2020;21(1):569. [17] SHIGETOH H, NISHI Y, OSUMI M, et al. Combined abnormal muscle activity and pain-related factors affect disability in patients with chronic low back pain: An association rule analysis.PLoS One. 2020;15(12):e0244111. [18] BETTI S, CASTIELLO U, GUERRA S, et al. Overt orienting of spatial attention and corticospinal excitability during action observation are unrelated.PLoS One. 2017;12(3):e0173114. [19] COPITHORNE DB, FORMAN DA, POWER KE. Premovement Changes in Corticospinal Excitability of the Biceps Brachii are Not Different Between Arm Cycling and an Intensity-Matched Tonic Contraction. Motor Control. 2015;19(3):223-241. [20] DEMPSEY LM, KAVANAGH JJ. Muscarinic receptor blockade causes postcontraction enhancement in corticospinal excitability following maximal contractions. J Neurophysiol. 2021;125(4):1269-1278. [21] GRANDJEAN J, DEROSIERE G, VASSILIADIS P, et al. Towards assessing corticospinal excitability bilaterally: Validation of a double-coil TMS method. J Neurosci Methods. 2018;293:162-168. [22] HELM F, MARINOVIC W, KRÜGER B, et al. Corticospinal excitability during imagined and observed dynamic force production tasks: effortfulness matters. Neuroscience. 2015;290:398-405. [23] HYDE C, FUELSCHER I, WILLIAMS J, et al. Corticospinal excitability during motor imagery is reduced in young adults with developmental coordination disorder. Res Dev Disabil. 2018;72:214-224. [24] MATSUMOTO A, LIANG N, UEDA H, et al. Corticospinal Excitability of the Lower Limb Muscles During the Anticipatory Postural Adjustments: A TMS Study During Dart Throwing.Front Hum Neurosci. 2021;15:703377. [25] MIZUGUCHI N, UMEHARA I, NAKATA H, et al. Modulation of corticospinal excitability dependent upon imagined force level. Exp Brain Res. 2013;230(2):243-249. [26] POWER KE, COPITHORNE DB. Increased corticospinal excitability prior to arm cycling is due to enhanced supraspinal but not spinal motoneurone excitability. Appl Physiol Nutr Metab. 2013;38(11):1154-1161. [27] ROWLAND RS, JENKINSON N, CHIOU SY. Age-Related Differences in Corticospinal Excitability and Anticipatory Postural Adjustments of the Trunk. Front Aging Neurosci. 2021;13:718784. [28] KRUCOFF MO, ZHUANG K, MACLEOD D, et al. A novel paraplegia model in awake behaving macaques. J Neurophysiol. 2017;118(3):1800-1808. [29] GUILLOT A, DI RIENZO F, MACINTYRE T, et al. Imagining is not doing but involves specific motor commands: a review of experimental data related to motor inhibition. Front Hum Neurosci. 2012;6:247. [30] KNOX J, GUPTA A, BANWELL HA, et al. Comparison of EMG signal of the flexor hallucis longus recorded using surface and intramuscular electrodes during walking. J Electromyogr Kinesiol. 2021;60:8. [31] KUBIAK CA, SVIENTEK SR, DEHDASHTIAN A, et al. Physiologic signaling and viability of the muscle cuff regenerative peripheral nerve interface (MC-RPNI) for intact peripheral nerves. J Neural Eng. 2021;18(4): doi: 10.1088/1741-2552/ac1b6b. [32] KUĆ J, SZAREJKO KD, ALEKSANDROWICZ K, et al. The role of soft tissue mobilization in reducing orofacial and general complaints in a patient with Kimmerle anomaly and temporomandibular joint disorder: A case report. Cranio. 2021;39(1):74-87. [33] KWONG E, NG KK, LEUNG MT, et al. Application of Ultrasound Biofeedback to the Learning of the Mendelsohn Maneuver in Non-dysphagic Adults: A Pilot Study.Dysphagia. 2021;36(4):650-658. [34] LABANCA L, MOSCA M, GHISLIERI M, et al. Muscle activations during functional tasks in individuals with chronic ankle instability: a systematic review of electromyographical studies. Gait Posture. 2021;90:340-373. [35] LANE K, CHANDLER E, PAYNE D, et al. Stroke survivors’ recommendations for the visual representation of movement analysis measures: a technical report. Physiotherapy. 2020;107:36-42. [36] LAVIGNE G, KATO T, HERRERO BABILONI A, et al. Research routes on improved sleep bruxism metrics: Toward a standardised approach. J Sleep Res. 2021;30(5):e13320. [37] CALATAYUD J, VINSTRUP J, JAKOBSEN MD, et al. Mind-muscle connection training principle: influence of muscle strength and training experience during a pushing movement. Eur J Appl Physiol. 2017;117(7):1445-1452. [38] CALATAYUD J, VINSTRUP J, JAKOBSEN MD, et al. Attentional Focus and Grip Width Influences on Bench Press Resistance Training. Percept Mot Skills. 2018;125(2):265-277. [39] HALPERIN I, HUGHES S, PANCHUK D, et al. The Effects of Either a Mirror, Internal or External Focus Instructions on Single and Multi-Joint Tasks. PLoS One. 2016;11(11):e0166799. [40] TURNER C, CROW S, CROWTHER T, et al. Preventing non-contact ACL injuries in female athletes: What can we learn from dancers? Phys Ther Sport. 2018;31:1-8. [41] WULF G, DUFEK JS, LOZANO L, et al. Increased jump height and reduced EMG activity with an external focus. Hum Mov Sci. 2010;29(3):440-448. [42] BARRY AJ, MURRAY WM, KAMPER DG. Development of a dynamic index finger and thumb model to study impairment. J Biomech. 2018;77:206-210. [43] BOYACI A, TOPUZ O, ALKAN H, et al. Comparison of the effectiveness of active and passive neuromuscular electrical stimulation of hemiplegic upper extremities: a randomized, controlled trial. Int J Rehabil Res. 2013;36(4):315-322. [44] BURNS A, ADELI H, BUFORD JA. Upper Limb Movement Classification Via Electromyographic Signals and an Enhanced Probabilistic Network. J Med Syst. 2020;44(10):176. [45] CHAE J, HARLEY MY, HISEL TZ, et al. Intramuscular Electrical Stimulation for Upper Limb Recovery in Chronic Hemiparesis: An Exploratory Randomized Clinical Trial. Neurorehabil Neural Repair. 2009;23(6):569-578. [46] PIZZAMIGLIO S, DESOWSKA A, SHOJAII P, et al. Muscle co-contraction patterns in robot-mediated force field learning to guide specific muscle group training.Neurorehabilitation. 2017;41(1):17-29. [47] VERMILLION BC, DROMERICK AW, LEE SW. Toward Restoration of Normal Mechanics of Functional Hand Tasks Post-Stroke: Subject-Specific Approach to Reinforce Impaired Muscle Function. IEEE Trans Neural Syst Rehabil Eng. 2019;27(8):1606-1616. [48] CHOU LW, PALMER JA, BINDER-MACLEOD S, et al. Motor unit rate coding is severely impaired during forceful and fast muscular contractions in individuals post stroke.J Neurophysiol. 2013;109(12):2947-2954. [49] LIU L. Biomechanical analysis of sidestep cutting movement which causes anterior cruciate ligament injury during sports. Med Sport. 2019;72(4):586-595. [50] MAROTTA N, DEMECO A, DE SCORPIO G, et al. Late Activation of the Vastus Medialis in Determining the Risk of Anterior Cruciate Ligament Injury in Soccer Players. J Sport Rehabil. 2020;29(7):952-955. [51] SHANBEHZADEH S, MOHSENI BANDPEI MA, EHSANI F. Knee muscle activity during gait in patients with anterior cruciate ligament injury: a systematic review of electromyographic studies. Knee Surg Sports Traumatol Arthrosc. 2017;25(5):1432-1442. [52] THEISEN D, RADA I, BRAU A, et al. Muscle Activity Onset Prior to Landing in Patients after Anterior Cruciate Ligament Injury: A Systematic Review and Meta-Analysis. PLoS One. 2016;11(5):e0155277. [53] TRULSSON A, MILLER M, HANSSON GÅ, et al. Altered movement patterns and muscular activity during single and double leg squats in individuals with anterior cruciate ligament injury. BMC Musculoskelet Disord. 2015;16:28. [54] XIE D, URABE Y, OCHIAI J, et al. Sidestep cutting maneuvers in female basketball players: Stop phase poses greater risk for anterior cruciate ligament injury. Knee. 2013;20(2):85-89. [55] WANG IL, GRAHAM RB, BOURDON EJP, et al. Biomechanical Analysis of Running Foot Strike in Shoes of Different Mass. J Sport Sci Med. 2020;19(1):130-137. [56] BOTZHEIM L, LACZKO J, TORRICELLI D, et al. Effects of gravity and kinematic constraints on muscle synergies in arm cycling. J Neurophysiol. 2021;125(4):1367-1381. [57] CHENG R, SUI Y, SAYENKO D, et al. Motor Control After Human SCI Through Activation of Muscle Synergies Under Spinal Cord Stimulation. IEEE Trans Neural Syst Rehabil Eng. 2019;27(6):1331-1340. [58] ESCALONA MJ, BOURBONNAIS D, GOYETTE M, et al. Effects of Varying Overground Walking Speeds on Lower-Extremity Muscle Synergies in Healthy Individuals.Motor Control. 2021;25(2):234-251. [59] GENG Y, DENG H, SAMUEL OW, et al. Modulation of muscle synergies for multiple forearm movements under variant force and arm position constraints.J Neural Eng. 2020;17(2):026015. [60] MASOUMDOOST A, SAADATYAR R, KOBRAVI HR. A muscle synergies-based movements detection approach for recognition of the wrist movements.EURASIP J Adv Signal Process. 2020;2020(1):19. [61] MICHAUD F, SHOURIJEH MS, FREGLY BJ, et al. Do Muscle Synergies Improve Optimization Prediction of Muscle Activations During Gait? Front Comput Neurosci. 2020;14:54. [62] MILETI I, ZAMPOGNA A, SANTUZ A, et al. Muscle Synergies in Parkinson’s Disease. Sensors. 2020;20(11):21. [63] PELLEGRINO L, COSCIA M, CASADIO M. Muscle activities in similar arms performing identical tasks reveal the neural basis of muscle synergies. Exp Brain Res. 2020;238(1):121-138. [64] WANG XJ, DONG DP, CHI XK, et al. sEMG-based consecutive estimation of human lower limb movement by using multi-branch neural network. Biomed Signal Process Control. 2021;68:9. [65] FARINA D, MERLETTI R, ENOKA RM. The extraction of neural strategies from the surface EMG. J Appl Physiol (1985). 2004;96(4):1486-1495. [66] CHEUNG VC, TUROLLA A, AGOSTINI M, et al. Muscle synergy patterns as physiological markers of motor cortical damage. Proc Natl Acad Sci U S A. 2012;109(36):14652-14656. [67] DE LUCA CJ, GILMORE LD, KUZNETSOV M, et al. Filtering the surface EMG signal: Movement artifact and baseline noise contamination. J Biomech. 2010;43(8):1573-1579. [68] CHOWDHURY A, DUTTA A, PRASAD G. Corticomuscular Co-Activation Based Hybrid Brain-Computer Interface for Motor Recovery Monitoring. IEEE Access. 2020;8:174542-174557. [69] ZHANG X, LI R, LI H, et al. Novel approach for electromyography-controlled prostheses based on facial action. Med Biol Eng Comput. 2020;58(11):2685-2698. [70] ATZORI M, GIJSBERTS A, CASTELLINI C, et al. Electromyography data for non-invasive naturally-controlled robotic hand prostheses. Sci Data. 2014;1:140053. [71] FARINA D, JIANG N, REHBAUM H, et al. The Extraction of Neural Information from the Surface EMG for the Control of Upper-Limb Prostheses: Emerging Avenues and Challenges. IEEE Trans Neural Syst Rehabil Eng. 2014;22(4):797-809. [72] ABE D, HOTTA N, FUKUOKA Y, et al. Biomechanical Analysis of Gait and Sit-to-Stand Patterns Using a Specially Made Knee Supporter in Healthy Young and Elderly Individuals. J Physiol Anthropol. 2010;29(2):65-70. [73] KRASNOW D, WILMERDING MV, STECYK S, et al. Biomechanical Research in Dance: A Literature Review. Med Probl Perform Art. 2011; 26(1):3-23. [74] WONG DWC, LEE WCC, LAM WK. Biomechanics of Table Tennis: A Systematic Scoping Review of Playing Levels and Maneuvers. Appl Sci Basel. 2020;10(15):21. [75] MANOLOPOULOS E, KATIS A, MANOLOPOULOS K, et al. Effects of a 10-week resistance exercise program on soccer kick biomechanics and muscle strength. J Strength Cond Res. 2013;27(12):3391-3401. [76] STÖGGL T, LINDINGER S, MÜLLER E. Biomechanical validation of a specific upper body training and testing drill in cross-country skiing. Sports Biomech. 2006;5(1):23-46. [77] LIU AM, CHU IH, LIN HT, et al. Training Benefits and Injury Risks of Standing Yoga Applied in Musculoskeletal Problems: Lower Limb Biomechanical Analysis. Int J Environ Res Public Health. 2021;18(16): 8402. [78] FORGHANY S, NESTER CJ, RICHARDS B, et al. Rollover footwear affects lower limb biomechanics during walking. Gait Posture. 2014;39(1): 205-212. [79] MACKALA K, STODÓŁKA J, SIEMIENSKI A, et al. Biomechanical analysis of standing long jump from varying starting positions. J Strength Cond Res. 2013;27(10):2674-2684. [80] RAO G, BERTON E, AMARANTINI D, et al. An EMG-Driven Biomechanical Model That Accounts for the Decrease in Moment Generation Capacity During a Dynamic Fatigued Condition. J Biomech Eng. 2010; 132(7):071003. [81] FEGER MA, DONOVAN L, HERB CC, et al. Effects of 4-week impairment-based rehabilitation on jump-landing biomechanics in chronic ankle instability patients. Phys Ther Sport. 2021;48:201-208. [82] CABRAL ALCES, JORGE JG, DIONISIO VC. Biomechanical analysis during single-leg squat in individuals with knee osteoarthritis. Knee. 2021;28:362-370. [83] DAI B, SORENSEN CJ, DERRICK TR, et al. The Effects of Postseason Break on Knee Biomechanics and Lower Extremity EMG in a Stop-Jump Task: Implications for ACL Injury. J Appl Biomech. 2012;28(6):708-717. [84] COOREVITS P, DANNEELS L, CAMBIER D, et al. Correlations between short-time Fourier- and continuous wavelet transforms in the analysis of localized back and hip muscle fatigue during isometric contractions. J Electromyogr Kinesiol. 2008;18(4):637-644. [85] 戴艳.运动性疲劳的产生机制及恢复措施的研究[J].沈阳体育学院学报,2004,23(3):333-335. [86] 付克翠,陈菊平,陈元武.运动性疲劳概述[J].四川体育科学, 2004(2):30-32. [87] 王军,王有清.运动性疲劳的测定和消除[J].当代教育论坛, 2003(3):96-96. [88] ABBOUD J, NOUGAROU F, LORANGER M, et al. Test-retest reliability of trunk motor variability measured by large-array surface electromyography. J Manipulative Physiol Ther. 2015;38(6):359-364.. [89] STULEN FB, DELUCA CJ. Frequency parameters of the myoelectric signal as a measure of muscle conduction velocity. IEEE Trans Biomed Eng. 1981;28(7):515-523. [90] SCHWEITZER TW, FITZGERALD JW, BOWDEN JA, et al. Spectral analysis of human inspiratory diaphragmatic electromyograms. J Appl Physiol Respir Environ Exerc Physiol. 1979;46(1):152. [91] COOREVITS P, DANNEELS L, CAMBIER D, et al. Assessment of the validity of the Biering-Sorensen test for measuring back muscle fatigue based on EMG median frequency characteristics of back and hip muscles. J Electromyogr Kinesiol. 2008;18(6):997-1005. [92] ROLDÁN JIMÉNEZ C, BENNETT P, ORTIZ GARCÍA A, et al. Fatigue Detection during Sit-To-Stand Test Based on Surface Electromyography and Acceleration: A Case Study. Sensors (Basel). 2019;19(19):14. [93] HIEMSTRA LA, LO IK, FOWLER PJ. Effect of fatigue on knee proprioception: implications for dynamic stabilization. J Orthop Sports Phys Ther. 2001;31(10):598. [94] BAILLY F, CEGLIA A, MICHAUD B, et al. Real-Time and Dynamically Consistent Estimation of Muscle Forces Using a Moving Horizon EMG-Marker Tracking Algorithm-Application to Upper Limb Biomechanics. Front Bioeng Biotechnol. 2021;9:642742. [95] 弗拉基米尔. 运动生物力学:运动成绩的提高与运动损伤的预防[M].北京:人民体育出版社.2004 [96] CROCE RV, MILLER JP, SMITH WJ, et al. Surface electromyographic alterations of the knee extensor musculature based on contraction intensity and velocity. Isokinetics Exerc Sci. 2012;20(3):155-165. [97] BABYAR SR, HOLLAND TJ, ROTHBART D, et al. Electromyographic Analyses of Trunk Musculature after Stroke: An Integrative Review. Top Stroke Rehabil. 2021:1-16. doi: 10.1080/10749357.2021.1940725. [98] ZHANG XF, LI X, DAI JT, et al. The design of a hemiplegic upper limb rehabilitation training system based on surface EMG signals. J Adv Mech Des Syst Manuf. 2018;12(1):12. [99] DENIZOGLU KULLI H, KARABULUT D, SAKA T, et al. Force irradiation effect of kinesiotaping on contralateral muscle activation. Hum Mov Sci. 2019;66:310-317. [100] ADAMSON M, MACQUAIDE N, HELGERUD J, et al. Unilateral arm strength training improves contralateral peak force and rate of force development. Eur J Appl Physiol. 2008;103:553-559. [101] DRAGERT K, ZEHR EP. High-intensity unilateral dorsiflexor resistance training results in bilateral neuromuscular plasticity after stroke. Exp Brain Res. 2013;225(1):93-104. [102] DEVINE KL, LEVEAU BF, YACK HJ. Electromyographic Activity Recorded from an Unexercised Muscle During Maximal Isometric Exercise of the Contralateral Agonists and Antagonists. Phys Ther. 1981;61:898-903. [103] POST M, BAKELS R, ZIJDEWINd I. Inadvertent Contralateral Activity during a Sustained Unilateral Contraction Reflects the Direction of Target Movement. J Neurosci. 2009;29:6353-6357. [104] ZIJDEWIND I, BUTLER JE, GANDEVIA SC, et al. The origin of activity in the biceps brachii muscle during voluntary contractions of the contralateral elbow flexor muscles. Exp Brain Res. 2006;175:526-535. |
| [1] | Wang Shuai, Wang Liancheng, Zhang Shuhao, Li Fuli, Dong Jiaxing, Zhang Yajie. Correlation of the electromyography ratio of the paraspinal muscles on the convex and concave sides with Cobb angle, apical vertebra translation, and coronal balance distance in adolescent idiopathic scoliosis patients [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1402-1406. |
| [2] | Zhao Jing, Liu Xiaobo, Zhang Yue, Zhang Jiaming, Zhong Dongling, Li Juan, Jin Rongjiang. Visualization analysis of neuromuscular electrical stimulation therapy based on CiteSpace: therapeutic effects, hot spots, and developmental trends [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1234-1241. |
| [3] | She Jian, Zhao Jing, Zhang Jiaming, Xia Haisha, Zhong Dongling, Li Yuxi, Zheng Zhong, Li Juan, Jin Rongjiang. Visualization analysis of literature on eye tracking in cognitive behaviors of autistic patients [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(35): 5724-5732. |
| [4] | Li Xiaojun, Li Jia, Gao Feng, Li Lang, Li Qin, Ouyang Xiangyu. Functional differentiation and visualization of nerve fibers in the human sciatic nerve [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(32): 5148-5154. |
| [5] | Li Qinlong, Zhou Yue, Wang Shuo. Changing step frequency influences energy expenditure, surface electromyography, and gait characteristics when running at anaerobic threshold [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(26): 4153-4159. |
| [6] | Li Zhishuai, Zhang Hongqian, Liu Jianquan, Zhang Hankun, Li Li. Visualization analysis of current research hotspots on rehabilitation treatment after anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(26): 4234-4241. |
| [7] | Chen Jin, Li Jiabin, Gu Mingxing, Tang Rong, Lu Jianxia. Effect of deep muscle stimulation on psoas surface electromyography and spatiotemporal and kinetic gait parameters in patients with chronic non-specific low back pain [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(18): 2894-2899. |
| [8] | Dong Jiale, Wei Yuanhao, Zhang Hongwu. Visualization analysis of bone defect treatment based on knowledge map [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(18): 2906-2913. |
| [9] | Chen Keyi, Wang Dingxuan, Zhang Mengyao. Low-load compression training of the extremities influences surface electromyography and isokinetic flexor and extensor strength of core muscles [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(17): 2744-2748. |
| [10] | Xue Xiali, Deng Zhongyi, Sun Junzhi, Li Ning, Ren Wenbo, Zhou Ling, He Ye. Hot spots and frontiers of rehabilitation robot research in recent 10 years: a bibliometric analysis based on the Web of Science database [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(14): 2214-2222. |
| [11] | Wang Susu, Li Lifeng, Zhang Yimin. Visualization analysis on research progress and hotspots of exercise therapy for sarcopenia in older adults in recent decade [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(14): 2223-2230. |
| [12] | Ouyang Yiyi, Peng Jie, Wang Kun, Zhang Tingran, Luo Jiong. Changes in biomechanical characteristics of children’s lower limbs during visual deprivation and dual tasks [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(12): 1834-1842. |
| [13] | Shang Wandi, Wang Xingze, Wei Xiaoyan. Effects of different types of abdominal support on lumbar-back muscle surface electromyography signals in people with abdominal obesity [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(11): 1656-1661. |
| [14] | Wang Mengting, Gu Yanping, Ren Wenbo, Qin Qian, Bai Bingyi, Liao Yuanpeng. Research hotspots of blood flow restriction training for dyskinesia based on visualization analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1264-1269. |
| [15] | Zhang Peng, Zhang Junxia. Surface electromyography characteristics of lower limbs in heterogeneous gait environment [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(36): 5814-5820. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||