Chinese Journal of Tissue Engineering Research ›› 2022, Vol. 26 ›› Issue (26): 4234-4241.doi: 10.12307/2022.829
Previous Articles Next Articles
Visualization analysis of current research hotspots on rehabilitation treatment after anterior cruciate ligament reconstruction
Li Zhishuai1, Zhang Hongqian2, Liu Jianquan1, Zhang Hankun1, Li Li1
- 1The Affiliated Hospital of Qingdao Binhai University, Qingdao Binhai University Medical School, Qingdao 266405, Shandong Province, China; 2Weifang Medical University, Weifang 261053, Shandong Province, China
-
Received:2021-11-01Accepted:2021-12-07Online:2022-09-18Published:2022-03-09 -
Contact:Li Li, MD, Attending physician, the Affiliated Hospital of Qingdao Binhai University, Qingdao Binhai University Medical School, Qingdao 266405, Shandong Province, China -
About author:Li Zhishuai, Master, Attending physician, the Affiliated Hospital of Qingdao Binhai University, Qingdao Binhai University Medical School, Qingdao 266405, Shandong Province, China Zhang Hongqian, Master candidate, Weifang Medical University, Weifang 261053, Shandong Province, China Li Zhishuai and Zhang Hongqian contributed equally to this work. -
Supported by:Shandong Provincial Medicine and Health Technology Development Plan, Nos. 202020011222 (to LZS) and 202020011232 (to LL); Shandong Provincial College Youth Talent Induction Program for Rehabilitation Therapy Research Innovation Teams (to LZS and LL [project participants])
CLC Number:
Cite this article
Li Zhishuai, Zhang Hongqian, Liu Jianquan, Zhang Hankun, Li Li. Visualization analysis of current research hotspots on rehabilitation treatment after anterior cruciate ligament reconstruction[J]. Chinese Journal of Tissue Engineering Research, 2022, 26(26): 4234-4241.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks

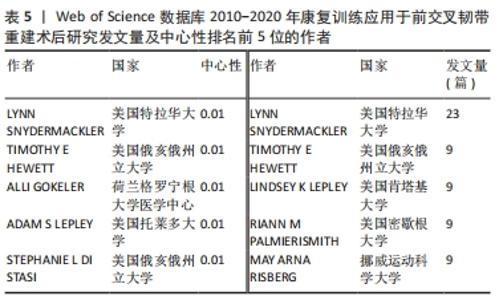
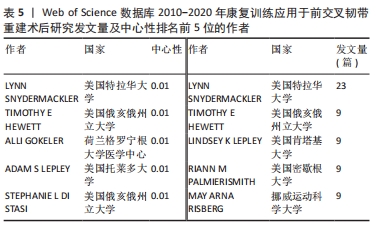
2.4 作者分布 在统计的作者合作网络图5中,可见近11年来共1 298个作者参与了该领域的研究,表5显示出中发文数量前5的作者依次为LYNN SNYDERMACKLER(23篇)、TIMOTHY E HEWETT(9篇)、LINDSEY K LEPLEY(9篇)、RIANN M PALMIERISMITH(9篇)、MAY ARNA RISBERG(9篇)。其中发文量最多的作者来自特拉华大学健康科学学院物理治疗系的教授LYNN SNYDERMACKLER,他在前交叉韧带重建术后康复领域涉及的研究主题有渐进式运动疗法和振动训练在前交叉韧带重建术后的效果、基于步态生物力学的肢体对称性分析、患者结局评估等[10-15]。"


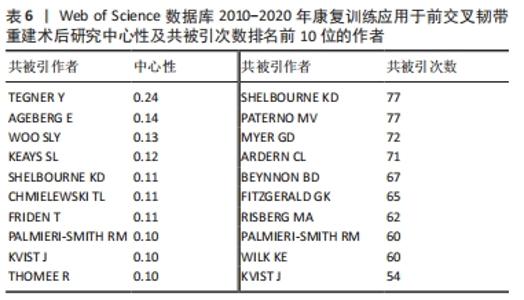
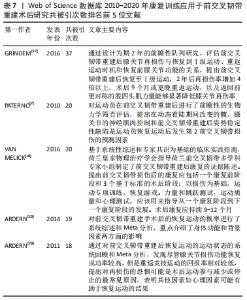
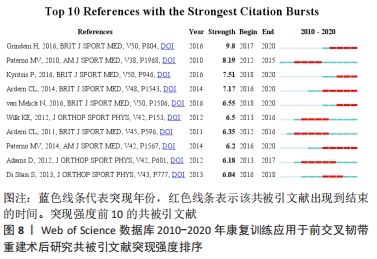
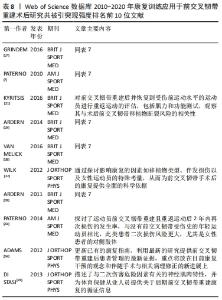
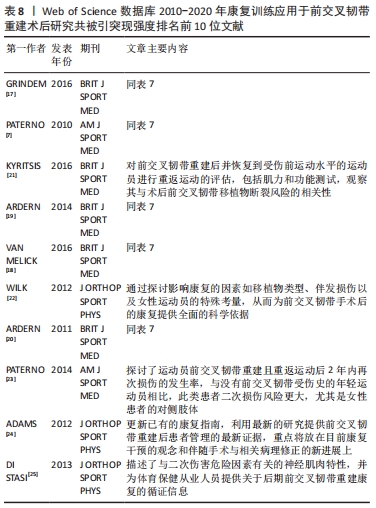
2.5 研究热点分析 2.5.1 文献共被引分析 文献共被引是1篇文献被2篇或多篇文献同时引用[16],基于共被引文献的共现分析和突现分析,可预测该领域近几年的研究热点及趋势。运行CiteSpace得到共被引文献知识图谱,见图7;共被引次数排名前5文献[7,17-20],见表7;共被引文献突现强度排序,见图8。其中来自挪威一个康复研究中心(NAR)的学者Grindem H被引频次最高,达37次,其文章在2018和2019年均被引用11次,详见表7。文献共被引突现分析可展现一段时间内被引频次较高的文献,图8和表8列出了突现强度前10的被引文献,依次为参考文献[7,17-25],其中近3年有5篇文献,且突现强度排名靠前。"

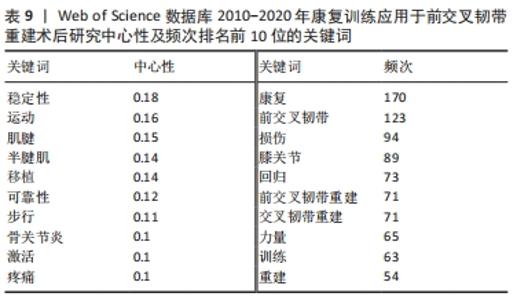
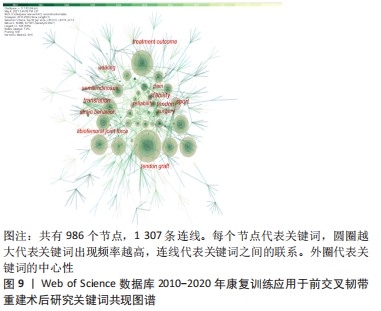
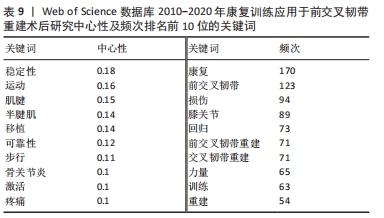
2.5.2 关键词共现分析 关键词是文章主要内容的提炼,出现次数越多代表研究主题热度越高,对关键词进行分析,可体现该领域的研究热点,判断发展方向。表9和图9列出共现较高的关键词。排名前10位的关键词中心性均>0.1,中介中心性取值0-1,是衡量节点在网络中重要性的指标,若其≥0.1说明中心性较高。中心性前3的关键词依次是:stability(稳定性)、sport(体育运动)、tendon(肌腱)。除去与主题相关的关键词:rehabilitation(康复)、anterior cruciate ligament(前交叉韧带),频次前3的关键词为injury(损伤)、return(回归)、strength(力量),详见表9。"
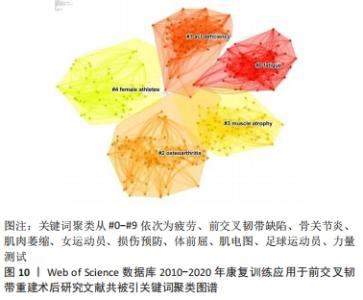
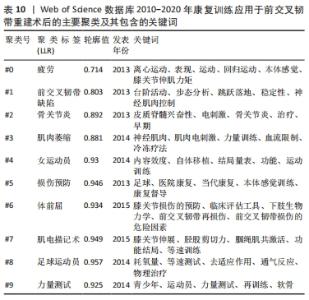
2.5.3 关键词聚类分析 关键词聚类是将关联紧密的关键词聚成一类,观察目前某个技术或学科领域形成了哪些研究类团,聚类号越小类团中成员数量越多,轮廓值表示类团内部成员之间的紧密程度,当>0.7时表示紧密良好或类团成员类似,聚类比较成功[26]。通过对关键词进行LLR聚类分析,在得到的聚类图10中,模块化Q值为0.726(>0.3),轮廓值S为0.895 9(>0.7),表示聚类较好,同质性较高。排名前5的聚类分别为“#0 fatigue(疲劳)、#1 acl deficiency(前交叉韧带缺陷)、#2 osteoarthritis(骨关节炎)、#3 muscle atrophy(肌肉萎缩)、#4 female athletes(女运动员)”,详见表10。"
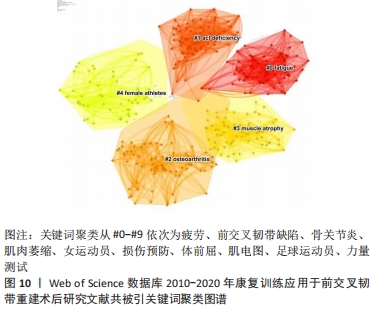

图11可分为3个阶段,其中早期2010-2013年,突现关键词为patellar tendon(髌韧带)、closed kinetic chain(闭链训练)、stability(稳定性)、lower extremity(下肢);中期2015-2017年为force development(力量部署)、articular cartilage(关节软骨)、soccer player(足球运动员);近期2018-2020年为return(回归)、cruciate ligament reconstruction(交叉韧带重建)、risk(风险)、sport(运动)、muscle strength(肌力)、injury(损伤)、reliability(信度)。"

| [1] HERZOG MM, MARSHALL SW, LUND JL, et al. Trends in incidence of ACL reconstruction and concomitant procedures among commercially insured individuals in the United States, 2002-2014. Sports Health. 2018;10(6):523-531. [2] MALEMPATI C, JURJANS J, NOEHREN B, et al. Current rehabilitation concepts for anterior cruciate ligament surgery in athletes. Orthopedics. 2015;38(11):6689-6696. [3] SLATER LV, HART JM, KELLY AR, et al. Progressive changes in walking kinematics and kinetics after anterior cruciate ligament injury and reconstruction: a review and meta-analysis. J Athl Train. 2017;52(9):847-860. [4] CAI WS, LI HH, KONNO SI, et al. Patellofemoral MRI alterations following single bundle ACL reconstruction with hamstring autografts are associated with quadriceps femoris atrophy. Curr Med Sci. 2019; 39(6):1029-1036. [5] REIDER B, ARCAND MA, DIEHL LH, et al. Proprioception of the knee before and after anterior cruciate ligament reconstruction. Arthroscopy. 2003;19(1):2-12. [6] SHI H, HUANG H, REN S, et al. The relationship between quadriceps strength asymmetry and knee biomechanics asymmetry during walking in individuals with anterior cruciate ligament reconstruction. Gait Posture. 2019;73:74-79. [7] PATERNO MV, SCHMITT LC, FORD KR, et al. Biomechanical measures during landing and postural stability predict second anterior cruciate ligament injury after anterior cruciate ligament reconstruction and return to sport. Am J Sports Med. 2010;38(10):1968-1978. [8] YABROUDI MA, IRRGANG JJ. Rehabilitation and return to play after anatomic anterior cruciate ligament reconstruction. Clin Sports Med. 2013;32(1):165-175. [9] 陈悦,陈超美,刘则渊,等.CiteSpace知识图谱的方法论功能[J].科学学研究,2015,33(2):242-253. [10] FAILLA MJ, LOGERSTEDT DS, GRINDEM H, et al. Does Extended Preoperative Rehabilitation Influence Outcomes 2 Years After ACL Reconstruction? A Comparative Effectiveness Study Between the MOON and Delaware-Oslo ACL Cohorts [published correction appears in Am J Sports Med. 2017;45(5):NP9]. Am J Sports Med. 2016;44(10): 2608-2614. [11] THOMA LM, GRINDEM H, LOGERSTEDT D, et al. Coper classification early after anterior cruciate ligament rupture changes with progressive neuromuscular and strength training and is associated with 2-year success: the delaware-oslo acl cohort study. Am J Sports Med. 2019; 47(4):807-814. [12] DI STASI SL, SNYDER-MACKLER L. The effects of neuromuscular training on the gait patterns of ACL-deficient men and women. Clin Biomech (Bristol, Avon). 2012;27(4):360-365. [13] CAPIN JJ, ZARZYCKI R, ITO N, et al. Gait mechanics in women of the acl-sports randomized control trial: interlimb symmetry improves over time regardless of treatment group. J Orthop Res. 2019;37(8):1743-1753. [14] HARTIGAN EH, AXE MJ, SNYDER-MACKLER L. Time line for noncopers to pass return-to-sports criteria after anterior cruciate ligament reconstruction. J Orthop Sports Phys Ther. 2010;40(3):141-154. [15] JOHNSON JL, IRRGANG JJ, RISBERG MA, et al. Comparing the responsiveness of the global rating scale with legacy knee outcome scores: a delaware-oslo cohort study. Am J Sports Med. 2020;48(8): 1953-1960. [16] CHEN CM. Predictive effects of structural variation on citation counts. J J Am Soc Inf Sci Technol. 2012. DOI: 10.1002/asi.21694. [17] GRINDEM H, SNYDER-MACKLER L, MOKSNES H, et al. Simple decision rules can reduce reinjury risk by 84% after ACL reconstruction: the Delaware-Oslo ACL cohort study. Br J Sports Med. 2016;50(13): 804-808. [18] VAN MELICK N, VAN CINGEL RE, BROOIJMANS F, et al. Evidence-based clinical practice update:practice guidelines for anterior cruciate ligament rehabilitation based on a systematic review and multidisciplinary consensus. Br J Sports Med. 2016;50(24):1506-1515. [19] ARDERN CL, TAYLOR NF, FELLER JA, et al. Fifty-five per cent return to competitive sport following anterior cruciate ligament reconstruction surgery:an updated systematic review and meta-analysis including aspects of physical functioning and contextual factors. Br J Sports Med. 2014;48(21):1543-1552. [20] ARDERN CL, WEBSTER KE, TAYLOR NF, et al. Return to sport following anterior cruciate ligament reconstruction surgery:a systematic review and meta-analysis of the state of play. Br J Sports Med. 2011;45(7): 596-606. [21] KYRITSIS P, BAHR R, LANDREAU P, et al. Likelihood of ACL graft rupture:not meeting six clinical discharge criteria before return to sport is associated with a four times greater risk of rupture. Br J Sports Med. 2016;50(15):946-951. [22] WILK KE, MACRINA LC, CAIN EL, et al. Recent advances in the rehabilitation of anterior cruciate ligament injuries. J Orthop Sports Phys Ther. 2012;42(3):153-171. [23] PATERNO MV, RAUH MJ, SCHMITT LC, et al. Incidence of Second ACL injuries 2 years after primary ACL reconstruction and return to sport. Am J Sports Med. 2014;42(7):1567-1573. [24] ADAMS D, LOGERSTEDT DS, HUNTER-GIORDANO A, et al. Current concepts for anterior cruciate ligament reconstruction: a criterion-based rehabilitation progression. J Orthop Sports Phys Ther. 2012; 42(7):601-614. [25] DI STASI S, MYER GD, HEWETT TE. Neuromuscular training to target deficits associated with second anterior cruciate ligament injury. J Orthop Sports Phys Ther. 2013;43(11):777-792, A1-A11. [26] CHEN CM, IBEKWE-SANJUAN F, HOU JH. The structure and dynamics of cocitation clusters: a multiple-perspective cocitation analysis. J Am Soc Inf Sci Technol. 2010;61(7):1386-1409. [27] 周天平,徐一宏,徐卫东.前交叉韧带重建相关研究的文献计量学分析[J].中华关节外科杂志(电子版),2020,14(5):612-618. [28] LIU K, QIAN J, GAO Q, et al. Effects of Kinesio taping of the knee on proprioception, balance, and functional performance in patients with anterior cruciate ligament rupture: a retrospective case series. Medicine (Baltimore). 2019;98(48):e17956. [29] SHEN M, CHE S, YE D, et al. Effects of backward walking on knee proprioception after ACL reconstruction. Physiother Theory Pract. 2021;37(10):1109-1116. [30] ZHEN D, QIU B, WANG W, et al. Proprioceptive changes measured by histopathological and electrophysiological evaluations after NGF injection of anterior cruciate ligament reconstruction. Ann Palliat Med. 2020;9(1):37-44. [31] LI W, LI Z, QIE S, et al. Biomechanical evaluation of preoperative rehabilitation in patients of anterior cruciate ligament injury. Orthop Surg. 2020;12(2):421-428. [32] ZHANG X, HUANG H, YU Y, et al. Impact of whey protein isolate and eccentric training on quadriceps mass and strength in patients with anterior cruciate ligament rupture: a randomized controlled trial. J Rehabil Med. 2020;52(3):jrm00035. [33] FU CL, YUNG SH, LAW KY, et al. The effect of early whole-body vibration therapy on neuromuscular control after anterior cruciate ligament reconstruction: a randomized controlled trial. Am J Sports Med. 2013; 41(4):804-814. [34] 王彬,李颖智,刘晓宁,等.前交叉韧带重建后康复研究进展[J].中国实验诊断学,2018,22(12):2199-2203. [35] LIM JM, CHO JJ, KIM TY, et al. Isokinetic knee strength and proprioception before and after anterior cruciate ligament reconstruction: a comparison between home-based and supervised rehabilitation. J Back Musculoskelet Rehabil. 2019;32(3):421-429. [36] KAYA D, GUNEY-DENIZ H, SAYACA C, et al. Effects on lower extremity neuromuscular control exercises on knee proprioception, muscle strength, and functional level in patients with ACL reconstruction. Biomed Res Int. 2019;2019:1694695. [37] GHADERI M, LETAFATKAR A, ALMONROEDER TG, et al. Neuromuscular training improves knee proprioception in athletes with a history of anterior cruciate ligament reconstruction: a randomized controlled trial. Clin Biomech (Bristol, Avon). 2020;80:105157. [38] SOUISSI S, CHAOUACHI A, BURNETT A, et al. Leg asymmetry and muscle function recovery after anterior cruciate ligament reconstruction in elite athletes: a pilot study on slower recovery of the dominant leg. Biol Sport. 2020;37(2):175-184. [39] HETSRONI I, WIENER Y, BEN-SIRA D, et al. Symmetries in muscle torque and landing kinematics are associated with maintenance of sports participation at 5 to 10 years after ACL reconstruction in young men. Orthop J Sports Med. 2020;8(6):2325967120923267. [40] SHIM JK, CHOI HS, SHIN JH. Effects of neuromuscular training on knee joint stability after anterior cruciate ligament reconstruction. J Phys Ther Sci. 2015;27(12):3613-3617. [41] MUNSCH AE, PIETROSIMONE B, FRANZ JR. The effects of knee extensor moment biofeedback on gait biomechanics and quadriceps contractile behavior. PeerJ. 2020;8:e9509. [42] CAPIN JJ, ZARZYCKI R, ITO N, et al. Gait mechanics in women of the ACL-SPORTS randomized control trial: interlimb symmetry improves over time regardless of treatment group. J Orthop Res. 2019;37(8): 1743-1753. [43] EITZEN I, MOKSNES H, SNYDER-MACKLER L, et al. Functional tests should be accentuated more in the decision for ACL reconstruction. Knee Surg Sports Traumatol Arthrosc. 2010;18(11): 1517-1525. [44] EBERT JR, WEBSTER KE, EDWARDS PK, et al. Current perspectives of Australian therapists on rehabilitation and return to sport after anterior cruciate ligament reconstruction: a survey. Phys Ther Sport. 2019;35:139-145. [45] NORTE GE, SOLAAS H, SALIBA SA, et al. The relationships between kinesiophobia and clinical outcomes after ACL reconstruction differ by self-reported physical activity engagement. Phys Ther Sport. 2019; 40:1-9. [46] MAHOOD C, PERRY M, GALLAGHER P, et al. Chaos and confusion with confidence: managing fear of Re-Injury after anterior cruciate ligament reconstruction. Phys Ther Sport. 2020;45:145-154. [47] RODRIGUEZ RM, MARROQUIN A, COSBY N. Reducing fear of reinjury and pain perception in athletes with first-time anterior cruciate ligament reconstructions by implementing imagery training. J Sport Rehabil. 2019;28(4):385-389. |
| [1] | Wang Jianping, Zhang Xiaohui, Yu Jinwei, Wei Shaoliang, Zhang Xinmin, Xu Xingxin, Qu Haijun. Application of knee joint motion analysis in machanism based on three-dimensional image registration and coordinate transformation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(在线): 1-5. |
| [2] | Li Zhiyi, He Pengcheng, Bian Tianyue, Xiao Yuxia, Gao Lu, Liu Huasheng. Bibliometric and visualized analysis of ferroptosis mechanism research [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1202-1209. |
| [3] | Zhao Jing, Liu Xiaobo, Zhang Yue, Zhang Jiaming, Zhong Dongling, Li Juan, Jin Rongjiang. Visualization analysis of neuromuscular electrical stimulation therapy based on CiteSpace: therapeutic effects, hot spots, and developmental trends [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1234-1241. |
| [4] | Wu Bingshuang, Wang Zhi, Tang Yi, Tang Xiaoyu, Li Qi. Anterior cruciate ligament reconstruction: from enthesis to tendon-to-bone healing [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1293-1298. |
| [5] | Shao Yangyang, Zhang Junxia, Jiang Meijiao, Liu Zelong, Gao Kun, Yu Shuhan. Kinematics characteristics of lower limb joints of young men running wearing knee pads [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 832-837. |
| [6] | Zhou Jianguo, Liu Shiwei, Yuan Changhong, Bi Shengrong, Yang Guoping, Hu Weiquan, Liu Hui, Qian Rui. Total knee arthroplasty with posterior cruciate ligament retaining prosthesis in the treatment of knee osteoarthritis with knee valgus deformity [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 892-897. |
| [7] | Yang Kuangyang, Wang Changbing. MRI evaluation of graft maturity and knee function after anterior cruciate ligament reconstruction with autogenous bone-patellar tendon-bone and quadriceps tendon [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 963-968. |
| [8] | Li Jie, Zhang Haitao, Chen Jinlun, Ye Pengcheng, Zhang Hua, Zhou Bengen, Zhao Changqing, Sun Youqiang, Chen Jianfa, Xiang Xiaobing, Zeng Yirong. Anterior cruciate ligament rupture and patellofemoral joint stability before sagittal and axial measurement using MRI [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 969-972. |
| [9] | Wei Xing, Liu Shufang, Mao Ning. Roles and values of blood flow restriction training in the rehabilitation of knee joint diseases [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 774-779. |
| [10] | Lu Qinxue, Xu Ning, Yang Yinglan, Han Qianqian, Duanmu Xianyu, Guo Yuwei, Han Qing. Femoroacetabular impingement: strength trainings for nerve-muscle, peripheral muscle and core muscle [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 786-791. |
| [11] | Liu Shaohua, Zhou Guanming, Chen Xicong, Xiao Keming, Cai Jian, Liu Xiaofang. Changes in kinematic parameters after unicompartmental knee arthroplasty and high tibial osteotomy [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(3): 390-396. |
| [12] | Zou Mengyao, Wang Junhua, Qin Pengfei, Zhong Weihua. Knowledge graph analysis of virtual reality technology in stroke treatment [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(26): 4224-4233. |
| [13] | Cao Fuyang, Xu Jianzhong, Lu Shitao, Tan Jun, Jiang Xu, Yang Meng, Shi Jianming, Chang Yingjian. Autologous, mixed and ligament advanced reinforcement system ligaments reconstruction of anterior cruciate ligament: evaluation of bone tunnel enlargement value, ligament growth factor and knee function [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(21): 3281-3290. |
| [14] | Zhang Xuepu, Wu Yuexin, Zhao Haosen, Ban Zhaoliang, Ma Xiaohu, Tong Gang, Yang Limin. A circular RNA, circ_0040646, regulates the proliferation, differentiation, and apoptosis of knee osteoarthritis chondrocytes by targeted inhibition of microRNA-188-3p [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(20): 3141-3146. |
| [15] | Diao Yulei, Zong Xiaorui, Deng Zhibo, Shu Han. Analgesic effect of adductor canal block versus femoral nerve block after autogenous bone-tendon-bone reconstruction of the anterior cruciate ligament: an updated Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(2): 315-320. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||