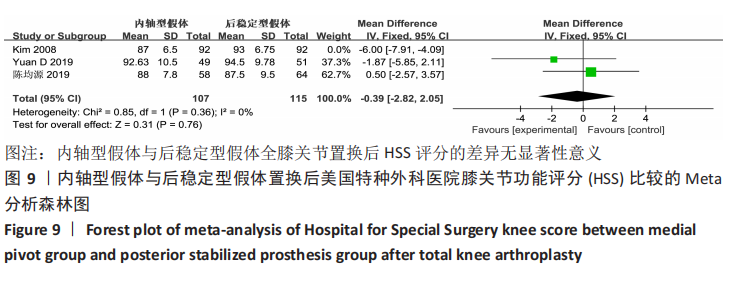
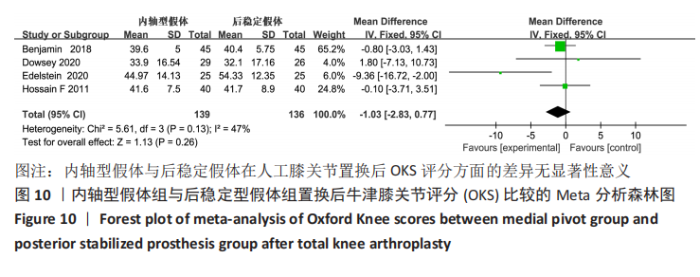
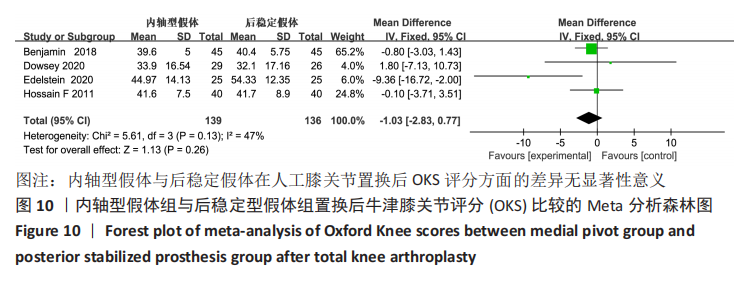
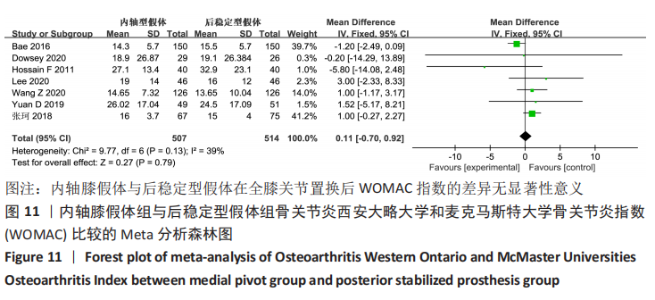
Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (33): 5395-5403.doi: 10.12307/2021.333
Previous Articles Next Articles
Medial pivot versus posterior stabilized prostheses for total knee arthroplasty: a meta-analysis
Gu Mingxi, Zhu Yunong, Tian Fengde, An Ning, Wang Changcheng, Guo Lin
- Second Department of Orthopedics, Zhongshan Hospital of Dalian University, Dalian 116001, Liaoning Province, China
-
Received:2020-12-24Revised:2020-12-31Accepted:2021-01-08Online:2021-11-28Published:2021-08-06 -
Contact:Guo Lin, Chief physician, Professor, MD, Master’s supervisor, Second Department of Orthopedics, Zhongshan Hospital of Dalian University, Dalian 116001, Liaoning Province, China -
About author:Gu Mingxi, Master candidate, Second Department of Orthopedics, Zhongshan Hospital of Dalian University, Dalian 116001, Liaoning Province, China
CLC Number:
Cite this article
Gu Mingxi, Zhu Yunong, Tian Fengde, An Ning, Wang Changcheng, Guo Lin. Medial pivot versus posterior stabilized prostheses for total knee arthroplasty: a meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(33): 5395-5403.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
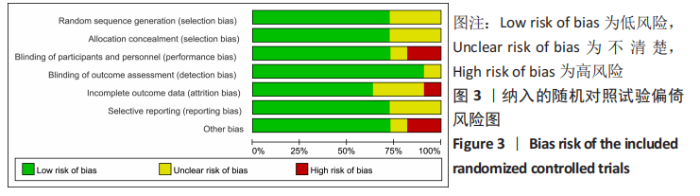
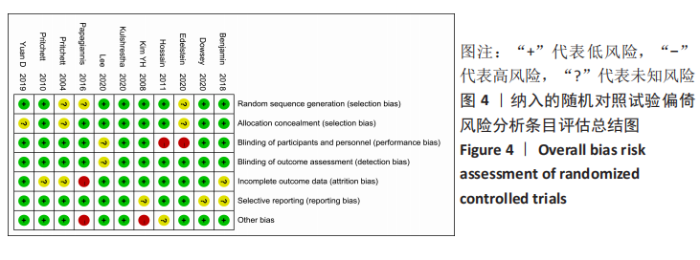
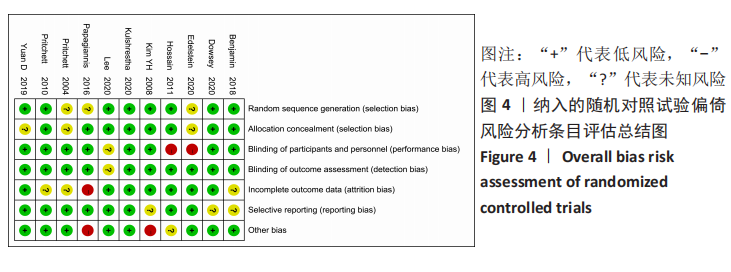
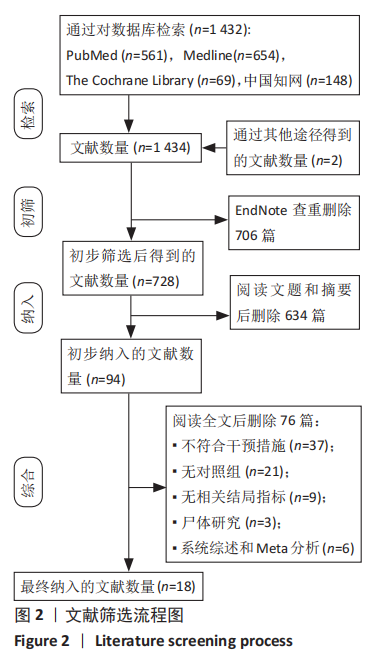
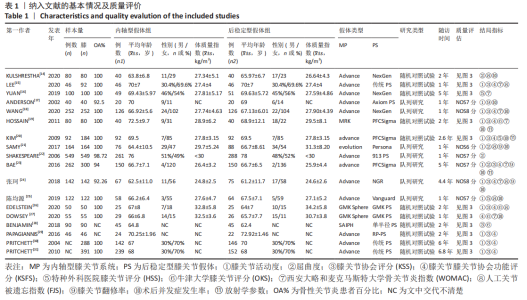
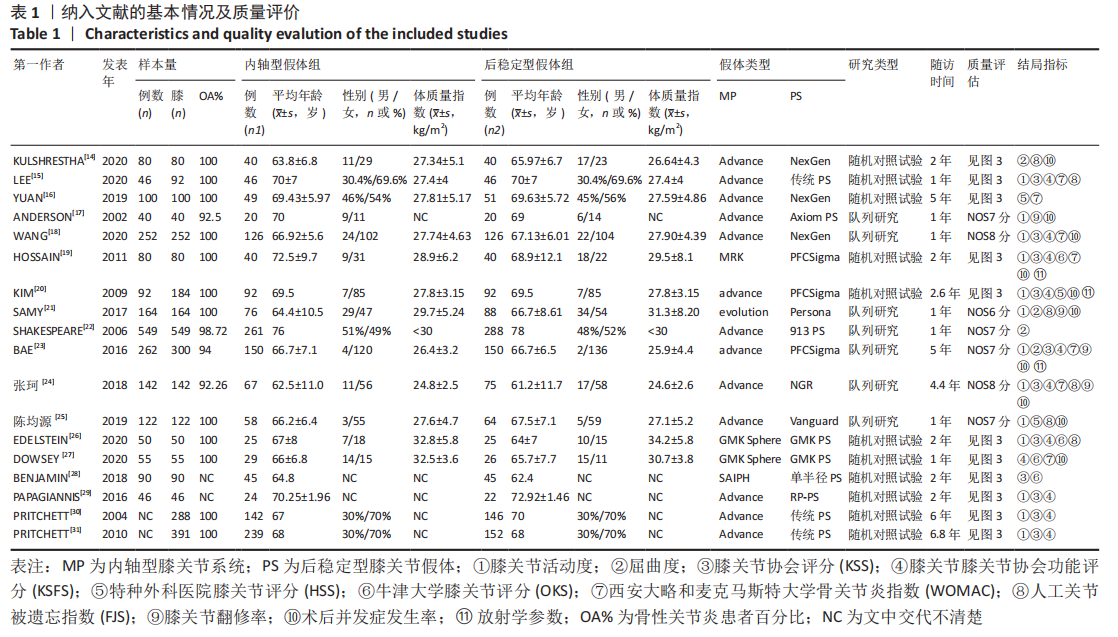
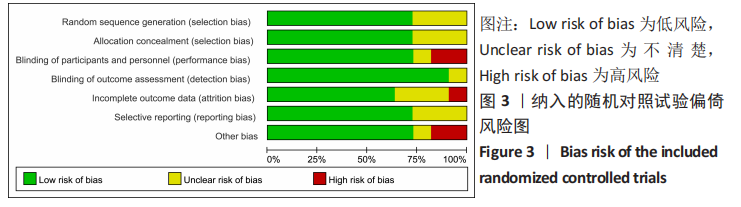
2.3 文献质量评价及偏倚风险评估结果 使用RevMan 5.3软件中的风险和偏倚表对随机对照试验研究进行了文献质量评估,其中8篇文献描述随机序列生成和分配隐藏[14-16,19-20,27-28,31],3篇文献没有详细报告分配隐藏的方法[16,26,29],存在不明确的选择偏倚风险,8篇报告了研究者、受试者和结局评估者充分设 盲[14,16,20,27-31],2篇为单盲试验[19,26], 只对受试者设盲。有10篇纳入的随机对照试验完整性地报告了主要指标的数据[14-16,19-20,27-28,30-31],报道了失访退出的人数和原因,所有纳入分析的随机试验均报告了预定措施的结果,没有高风险偏倚,表明此次纳入研究的随机对照试验随访偏倚和报告偏倚风险较小。有2项研究报告了高风险的其他来源偏倚[20,29],其中KIM等[20]的研究因高感染率提前终止。综合评估,此11项随机对照试验研究的偏倚风险为中 低[14-16,19-20,26-31],无高风险研究。见图3,4。对于非随机对照临床试验的质量评估使用NOS量表,所有7项非随机对照临床试验的NOS评分都高于5分,均属于高质量研究,见表1。"
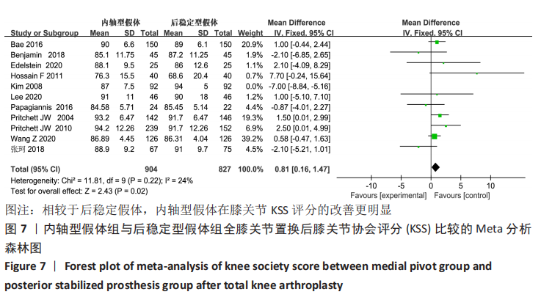
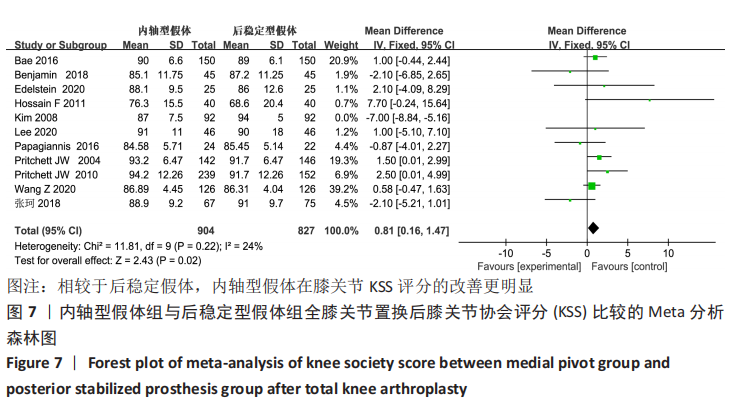
2.4.3 各组膝关节协会KSS评分差异 有13篇文献报告了全膝关节置换后膝关节协会评分[14-15,18-20,23-24,26-31], 但是有2项研究采用New KSS评分标准[14,27],最终纳入了11项研 究[15,18-20,23-24, 26,28-31],异质性检验结果:P < 0.000 01,I2=86%,提示11项研究之间存在明显异质性。逐项删除所纳入文献调查异质性来源,发现在删除了KIM等[20]研究后,异质性显著降低(P=0.22,I2=24%),故采用固定效应模型合并数据分析,结果显示:两组之间KSS评分的差异有显著性意义(MD=0.81,95%CI:0.16-1.47,P=0.02),表明相比于全膝关节置换时选用后稳定假体,采用内轴膝假体置换的患者能在KSS评分方面获得更大改善,见图7。"
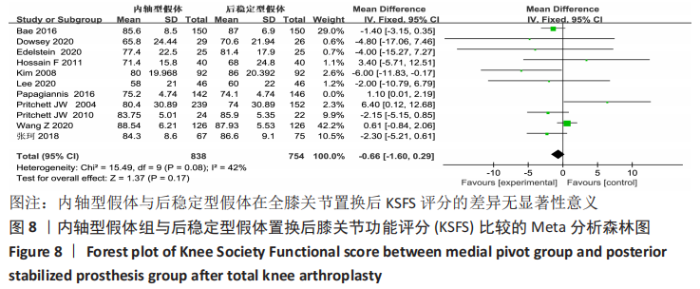
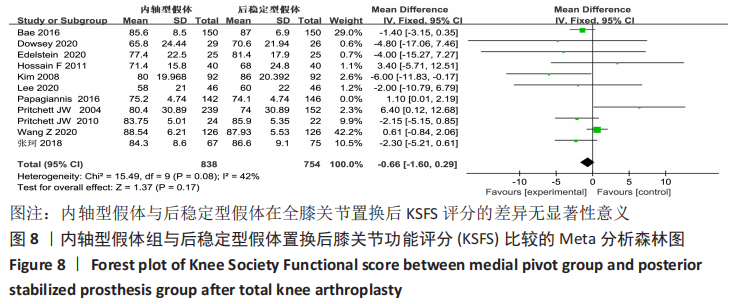
2.4.4 各组膝关节功能KSFS评分差异 纳入研究的文献中有11篇报告了全膝关节置换后的膝关节功能评 分[15,18-20,23-24,26-27,29-31],异质性分析结果显示:P=0.02,I2=53%,表明11项研究之间存在异质性.采用敏感性分析,排除异质性来源文献PAPAGIANNIS等[29]的研究后,异质性显著降低(P=0.08,I2=42%)。采用固定效应模型合并数据并分析,结果两组KSFS评分差异并未改变(MD=-0.66,95%CI:-1.60-0.29,P=0.17),表明异质性来源文献对整体结果无明显影响,两组假体在全膝关节置换后膝关节功能KSFS评分的差异无显著性意义,见图8。"
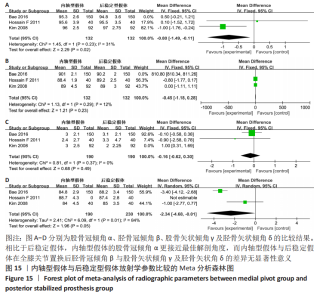
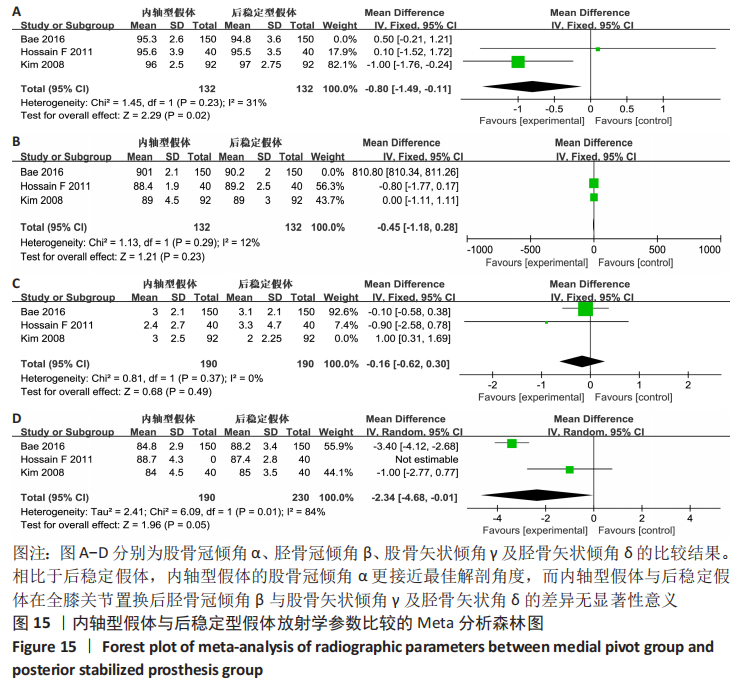
2.4.11 各组假体植入位置放射学参数的差异 根据Knee Society的X射线照相评估系统,通过研究膝关节的前后位(AP)和侧位X射线照相法从4个不同角度评估了股骨成分排列和胫骨成分排列;这些参数包括股骨冠倾角α,胫骨冠倾角β,股骨矢状倾角γ,胫骨矢状倾角δ。有3项研究报告了置换后假体所在的位置[19-20,23],显示了股骨假体和胫骨组件在前后位和矢状位形成的股胫骨角。两组之间的平均α角、β角和γ角经敏感性分析消除异质性后,使用固定效应模型分析数合并据,结果显示两组假体之间股骨冠倾角α的差异有显著性意义(MD=-0.80,95%CI:-1.49至-0.11,P=0.02),胫骨冠倾角β与股骨矢状倾角γ的差异均无显著性意义,见图15。胫骨矢状倾角δ经敏感性分析,异质性无改变,使用随机效应模型分析合并数据,结果显示内轴型假体与后稳定型假体之间的差异无显著性意义(MD=-2.34,95%CI:-4.68至-0.01,P=0.05),见图15。表明全膝关节置换时相较于选用后稳定假体,内轴膝假体具有更佳的稳定性,更符合生理解剖。"
| [1] MURGIER J, LAFFOSSE JM, CAILLIEZ J, et al. Is the prognosis the same for periprosthetic joint infections due to Staphylococcus aureus versus coagulase-negative staphylococci? A retrospective study of 101 patients with 2- year minimum follow-up. Arch Orthop Trauma Surg. 2016; 136(10):1357-1361. [2] DIGENNARO V, ZAMBIANCHI F, MARCOVIGI A, et al. Design and kinematics in total knee arthroplasty. Int Orthop. 2014;38(2):227-233. [3] MACHERAS GA, GALANAKOS SP, LEPETSOS P, et al. A long term clinical outcome of the Medial Pivot Knee Arthroplasty System. Knee. 2017;24(2):447-453. [4] ESPOSITO F, FREDDOLINI M, MARCUCCI M, et al. Biomechanical analysis on total knee replacement patients during gait: medial pivot or posterior stabilized design? Clin Biomech (Bristol, Avon). 2020;78:105068. [5] ATZORI F, SALAMA W, SABATINI L, et al Medial pivot knee in primary total knee arthroplasty. Ann Transl Med. 2016;4(1):6. [6] NISAR S, AHMAD K, PALAN J, et al. Medial stabilised total knee arthroplasty achieves comparable clinical outcomes when compared to other TKA designs: a systematic review and meta-analysis of the current literature. Knee Surg Sports Traumatol Arthrosc. 2020. doi:10.1007/s00167-020-06358-x. [7] KARACHALIOS T, VARITIMIDIS S, BARGIOTAS K, et al. An 11- to 15-year clinical outcome study of the Advance Medial Pivot total knee arthroplasty: pivot knee arthroplasty. Bone Joint J. 2016;98-B(8):1050-1055. [8] SHIMMIN A, MARTINEZ-MARTOS S, OWENS J, et al. Fluoroscopic motion study confirming the stability of a medial pivot design total knee arthroplasty. Knee. 2015;22(6):522-526. [9] STEINBRÜCK A, SCHRÖDER C, WOICZINSKI M, et al. Femorotibial kinematics and load patterns after total knee arthroplasty: an in vitro comparison of posterior-stabilized versus medial-stabilized design. Clin Biomech (Bristol, Avon). 2016;33:42-48. [10] FITCH DA, SEDACKI K, YANG Y. Mid- to long-term outcomes of a medial-pivot system for primary total knee replacement: a systematic review and meta-analysis. Bone Joint Res. 2014;3(10):297-304. [11] CUMPSTON M, LI T, PAGE MJ, et al. Updated guidance for trusted systematic reviews: a new edition of the Cochrane Handbook for Systematic Reviews of Interventions. Cochrane Database Syst Rev. 2019;10:ED000142. [12] STANG A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of non randomized studies in meta-analyses. Eur J Epidemiol. 2010;25(9): 603-605. [13] 王振. 内轴型(MP)与后稳定型(PS)膝关节假体置换后髌股关节功能早期效果对比研究[D].青岛:青岛大学,2019. [14] KULSHRESTHA V, SOOD M, KANADE S, et al. Early outcomes of medial pivot total knee arthroplasty compared to posterior-stabilized design: a randomized controlled trial. Clin Orthop Surg. 2020;12(2):178-186. [15] LEE QJ, WAI YEE EC, WONG YC. No difference in patient preference for medial pivot versus posterior-stabilized design in staged bilateral total knee arthroplasty: a prospective study. Knee Surg Sports Traumatol Arthrosc. 2020;28(12):3805-3809. [16] YUAN D, ZHANG QS, ZHANG K, et al. Total knee arthroplasty using a medial pivot or posterior cruciate-stabilizing prosthesis in Chinese patients. J Knee Surg. 2020;33(9):892-898. [17] ANDERSON MJ, BECKER DL, KIECKBUSCH T. Patellofemoral complications after posterior-stabilized total knee arthroplasty: a comparison of 2 different implant designs. J Arthroplasty. 2002;17(4):422-426. [18] WANG Z, ZHANG YQ, DING CR, et al. Early patellofemoral function of medial pivot prostheses compared with posterior-stabilized prostheses for unilateral total knee arthroplasty. Orthop Surg. 2021. doi:10.1111/os.12895. [19] HOSSAIN F, PATEL S, RHEE SJ, et al. Knee arthroplasty with a medially conforming ball-and-socket tibiofemoral articulation provides better function. Clin Orthop Relat Res. 2011;469(1):55-63. [20] KIM YH, YOON SH, KIM JS. Early outcome of TKA with a medial pivot fixed-bearing prosthesis is worse than with a PFC mobile-bearing prosthesis. Clin Orthop Relat Res. 2009;467(2):493-503. [21] SAMY DA, WOLFSTADT JI, VAIDEE I, et al. A retrospective comparison of a medial pivot and posterior-stabilized total knee arthroplasty with respect to patient-reported and radiographic outcomes. J Arthroplasty. 2018;33(5):1379-1383. [22] SHAKESPEARE D, LEDGER M, KINZEL V. Flexion after total knee replacement. A comparison between the Medial Pivot knee and a posterior stabilised implant. Knee. 2006;13(5):371-373. [23] BAE DK, CHO SD, IM SK, et al. Comparison of midterm clinical and radiographic results between total knee arthroplasties using medial pivot and posterior-stabilized prosthesis: a matched pair analysis. J Arthroplasty. 2016;31(2):419-424. [24] 张珂,王荣,刘江俊,等.双侧膝关节置换内轴膝假体与后稳定型假体的近中期疗效对比研究[J].中华骨与关节外科杂志,2018,11(3):166-170. [25] 陈均源,佘国荣,甘文奕,等.内轴型与后稳定型假体对膝关节置换后快速康复的影响[J].暨南大学学报(自然科学与医学版),2019,40(6):494-500. [26] EDELSTEIN AI, BHATT S, WRIGHT-CHISEM J, et al. The effect of implant design on sagittal plane stability: a randomized trial of medial- versus posterior-stabilized total knee arthroplasty. J Knee Surg. 2020;33(5): 452-458. [27] DOWSEY MM, GOULD DJ, SPELMAN T, et al. A randomized controlled trial comparing a medial stabilized total knee prosthesis to a cruciate retaining and posterior stabilized design: a report of the clinical and functional outcomes following total knee replacement. J Arthroplasty. 2020;35(6):1583-1590.e2. [28] BENJAMIN B, PIETRZAK JRT, TAHMASSEBI J, et al. A functional comparison of medial pivot and condylar knee designs based on patient outcomes and parameters of gait. Bone Joint J. 2018;100-B(1 Supple A):76-82. [29] PAPAGIANNIS GI, ROUMPELAKIS IM, TRIANTAFYLLOU AI, et al. No differences identified in transverse plane biomechanics between medial pivot and rotating platform total knee implant designs. J Arthroplasty. 2016;31(8):1814-1820. [30] PRITCHETT JW. Patient preferences in knee prostheses. J Bone Joint Surg Br. 2004; 86(7):979-982. [31] PRITCHETT JW. Patients prefer a bicruciate-retaining or the medial pivot total knee prosthesis. J Arthroplasty. 2011;26(2): 224-228. [32] EVANS JT, WHITEHOUSE MR. Partial versus total knee replacement for knee osteoarthritis. Lancet. 2019;394(10200): 712-713. [33] BEACH A, REGAZZOLA G, NERI T, et al. The effect of knee prosthesis design on tibiofemoral biomechanics during extension tasks following total knee arthroplasty. Knee. 2019;26(5):1010-1019. [34] BARNES CL, BLAHA JD, DEBOER D, et al. Assessment of a medial pivot total knee arthroplasty design in a cadaveric knee extension test model. J Arthroplasty 2012; 27:1460-1468. [35] WATANABE T, KOGA H, HORIE M, et al. Post-cam design and contact stress on tibial posts in posterior-stabilized total knee prostheses: comparison between a rounded and a squared design. J Arthroplasty. 2017; 32(12):3757-3762. [36] MOEWIS P, HOMMEL H, TREPCZYNSKI A, et al. Author correction: weight bearing activities change the pivot position after total knee arthroplasty. Sci Rep. 2020; 10(1):759. [37] VERRA WC, VAN DEN BOOM LG, JACOBS W, et al. Retention versus sacrifice of the posterior cruciate ligament in total knee arthroplasty for treating osteoarthritis. Cochrane Database Syst Rev. 2013;2013(10):CD004803. [38] LEE WC, KWAN YH, CHONG HC, et al. The minimal clinically important difference for knee society clinical rating system after total knee arthroplasty for primary osteoarthritis. Knee Surg Sports Traumatol Arthrosc. 2017; 25(11):3354-3359. [39] YANG HY, SEON JK, SHIN YJ, et al. Robotic total knee arthroplasty with a cruciate-retaining implant: a 10-year follow-up study. Clin Orthop Surg. 2017;9(2):169-176. [40] JONES CW, JACOBS H, SHUMBORSKI S, et al. Sagittal stability and implant design affect patient reported outcomes after total knee arthroplasty. J Arthroplasty. 2020;35(3):747-751. [41] Liddle AD, Judge A, Pandit H, et al. Adverse outcomes after total and unicompartmental knee replacement in 101,330 matched patients: a study of data from the National Joint Registry for England and Wales. Lancet. 2014;384(9952): 1437-1445. [42] Hall S. Venous thromboembolism prophylaxis after hip or knee arthroplasty. N Engl J Med. 2018;378(19):1848. [43] Nishio Y, Onodera T, Kasahara Y, et al. Intraoperative medial pivot affects deep knee flexion angle and patient-reported outcomes after total knee arthroplasty. J Arthroplasty. 2014;29(4):702-706. (责任编辑:WJ,ZN,ZH) |
| [1] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [2] | Chen Jinping, Li Kui, Chen Qian, Guo Haoran, Zhang Yingbo, Wei Peng. Meta-analysis of the efficacy and safety of tranexamic acid in open spinal surgery [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1458-1464. |
| [3] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [4] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [5] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [6] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [7] | Li Dadi, Zhu Liang, Zheng Li, Zhao Fengchao. Correlation of total knee arthroplasty efficacy with satisfaction and personality characteristics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1346-1350. |
| [8] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [9] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [10] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [11] | Peng Zhihao, Feng Zongquan, Zou Yonggen, Niu Guoqing, Wu Feng. Relationship of lower limb force line and the progression of lateral compartment arthritis after unicompartmental knee arthroplasty with mobile bearing [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1368-1374. |
| [12] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [13] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [14] | Zhang Shangpu, Ju Xiaodong, Song Hengyi, Dong Zhi, Wang Chen, Sun Guodong. Arthroscopic suture bridge technique with suture anchor in the treatment of acromioclavicular dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1417-1422. |
| [15] | Yuan Jiawei, Zhang Haitao, Jie Ke, Cao Houran, Zeng Yirong. Underlying targets and mechanism of Taohong Siwu Decoction in prosthetic joint infection on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1428-1433. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||