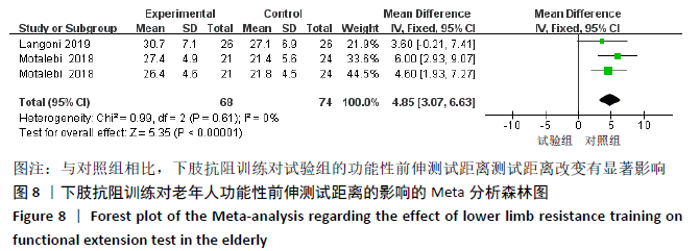
Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (26): 4257-4264.doi: 10.12307/2021.130
A Meta-analysis regarding the effect of lower limb resistance training on walking ability and balance ability in the elderly
Wu Chaoming, Sun Junzhi
- Institute of Sports Medicine and Health, Chengdu Sport University, Chengdu 610041, Sichuan Province, China
-
Received:2020-10-09Revised:2020-10-12Accepted:2020-11-28Online:2021-09-18Published:2021-05-14 -
Contact:Sun Junzhi, PhD, Senior experimentalist, Institute of Sports Medicine and Health, Chengdu Sport University, Chengdu 610041, Sichuan Province, China -
About author:Wu Chaoming, Master candidate, Institute of Sports Medicine and Health, Chengdu Sport University, Chengdu 610041, Sichuan Province, China -
Supported by:the "Twelfth Five-Year" National Science and Technology Support Project, No. 2012BAK21B01-2
CLC Number:
Cite this article
Wu Chaoming, Sun Junzhi. A Meta-analysis regarding the effect of lower limb resistance training on walking ability and balance ability in the elderly[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(26): 4257-4264.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
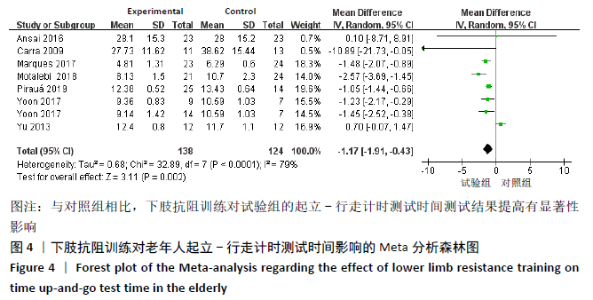
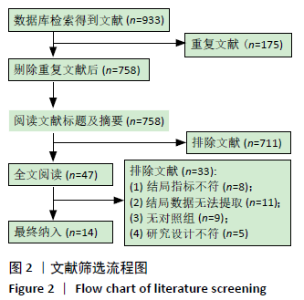
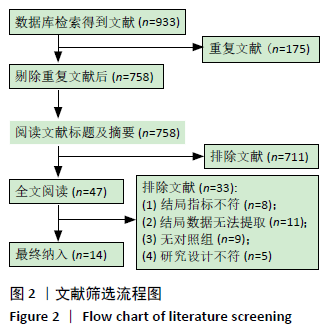
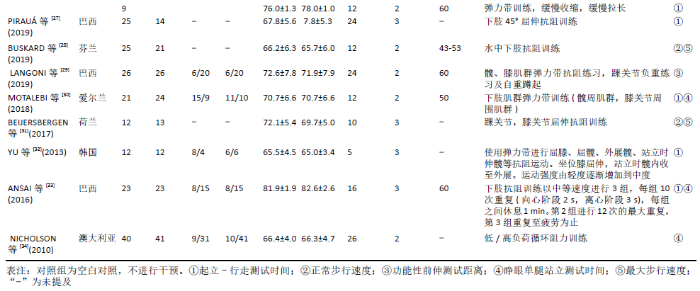
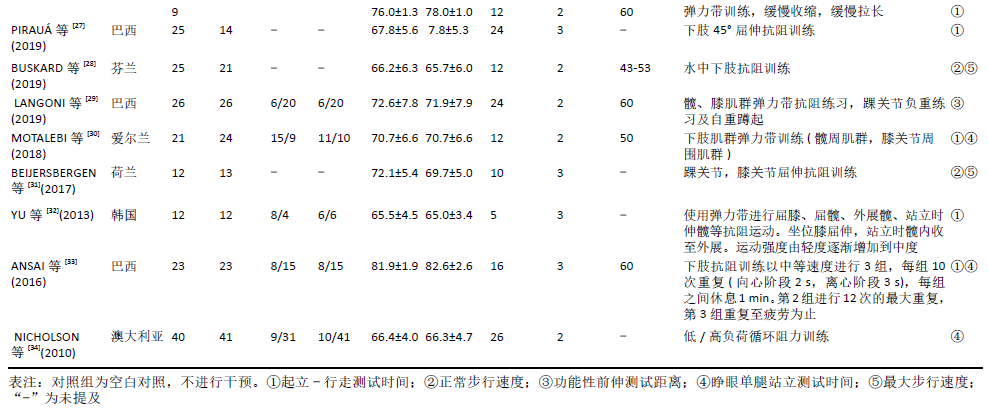
2.4 Meta分析结果 2.4.1 下肢抗阻训练对老年人起立-行走计时测试时间的影响 有7篇文献共纳入8项随机对照试验[22-23,25-27,32-33],同一文献中的不同组别数据比较视为多项研究,Yoon等[26]的研究中试验组为两种不同弹力带训练方法分别与对照组进行比较,因此视为2项随机对照研究。比较下肢抗阻训练后与对照组起立-行走计时测试时间变化情况。图4显示,此8项随机对照试验结果具有高度异质性:I2=79%,P < 0.01,采用随机效应模型进行分析。Meta分析结果显示,合并效应量:MD=-1.17,95%CI:-1.91至-0.43,P < 0.01,结果差异有显著性意义。说明与对照组相比下肢抗阻训练能够有效改善起立-行走计时测试时间。"
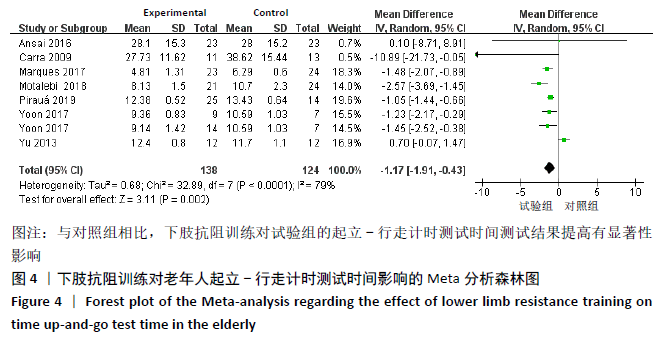
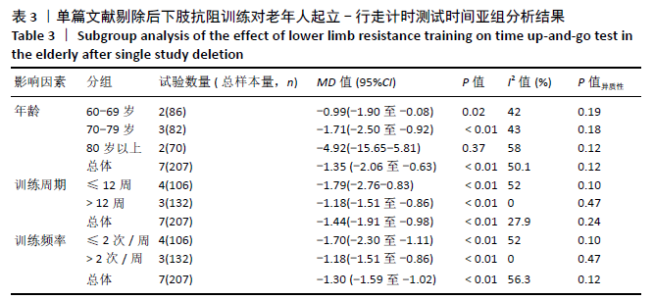
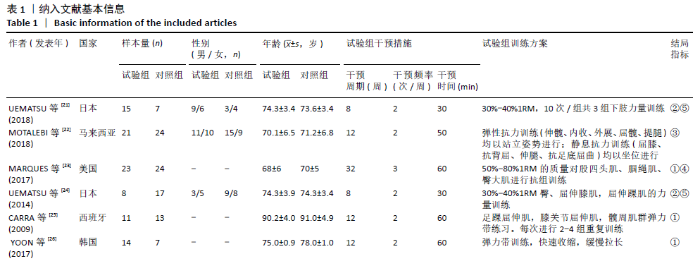
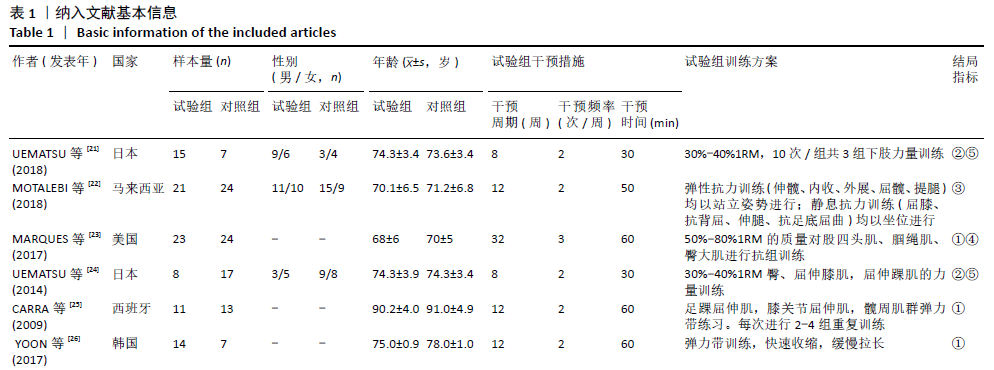
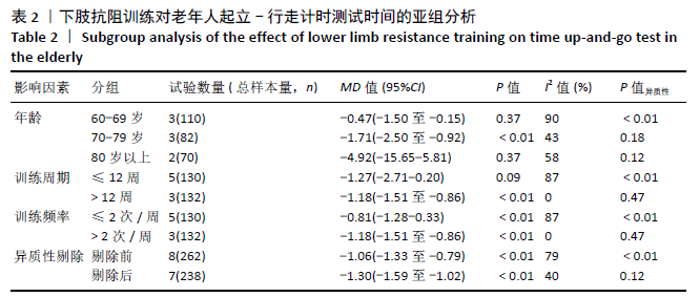
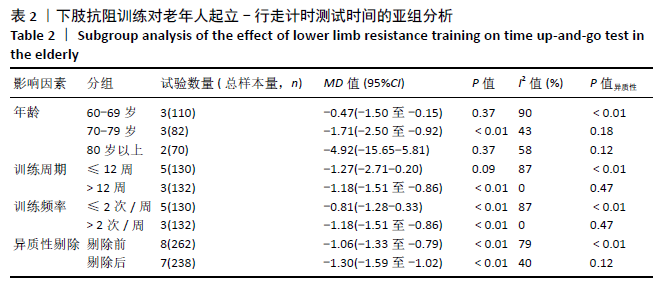
通过敏感性分析对文献质量进行归类,发现异质性来源于YU等[32]的研究。此单篇文献剔除后,异质性水平明显降低(I2=40%,P=0.12),因此采用固定效应模型分析。Meta分析结果显示,合并效应量结果更稳定且结果具有显著性意义(MD=-1.30,95%CI:-1.59至-1.02,P < 0.01)。剔除异质性较大文献后再次对起立-行走计时测试时间进行亚组分析。通过亚组分析发现,下肢抗阻训练能够对80-89岁高龄老人起立-行走计时测试时间改善无显著性意义(P=0.37)。训练周期总合并效应量的异质性为:I2=27.9%,明显降低。因此可以判断训练周期是影响起立-行走计时测试时间的主要因素,见表3。"
| [1] MASCIOCCHI E, MALTAIS M, ROLLAND Y, et al. Time effects on physical performance in older adults in nursing home: a narrative review. J Nutr Health Aging. 2019;23(6):586-594. [2] 陈金凤, 方明旺, 肖成汉, 等.中国老年人日常生活活动能力与抑郁症状的关系研究[J].中国全科医学, 2020, 23(22): 2852-2855, 2862. [3] ALCAZAR J, LOSA-REYNA J, RODRIGUEZ-LOPEZ C, et al. The sit-to-stand muscle power test: an easy, inexpensive and portable procedure to assess muscle power in older people. Exp Gerontol. 2018;112(8): 38-43. [4] JANSSEN WIM GM, BUSSMANN HANS BJ, STAM HJ. Determinants of the Sit-to-Stand Movement: a Review. Phys Ther. 2002;82(9):866-879. [5] ALLISON LK, KIEMEL T, JEKA JJ. Sensory-challenge balance exercises improve multisensory reweighting in fall-prone older adults. J Neurol Phys Ther. 2018;42(2): 84-93. [6] 江婉婷,王兴,王光旭,等.抗阻运动对中老年女性下肢肌肉力量及功能干预效果的Meta分析[J].首都体育学院学报, 2019,31(3):272-280. [7] NACZK M, MARSZALEK S, NACZK A. Inertial training improves strength, balance, and gait speed in elderly nursing home residents. Clin Interv Aging. 2020;15(2):177-184. [8] KRIST L, DIMEO F, KEIL T. Can progressive resistance training twice a week improve mobility, muscle strength, and quality of life in very elderly nursing-home residents with impaired mobility? A pilot study. Clin Interv Aging. 2013;8(6):443-448. [9] TIGGEMANN CL, DIAS CP, RADAELLI R, et al. Effect of traditional resistance and power training using rated perceived exertion for enhancement of muscle strength, power, and functional performance. Age (Dordr). 2016;38(2):42. [10] LEE DK, KANG MH, LEE TS, et al. Relationships among the Y balance test, Berg Balance Scale,and lower limb strength in middle-aged and older females. Braz J Phys Ther. 2015;19(3):227-234. [11] CAO ZB, MAEDA A, SHIMA N, et al. The effect of a 12-week combined exercise intervention program on physical performance and gait kinematics in community-dwelling elderly women. J Physiol Anthropol. 2007;26(3):325-332. [12] PERSCH LN, UGRINOWITSCH C, PEREIRA G, et al. Strength training improves fall-related gait kinematics in the elderly: a randomized controlled trial. Clin Biomech (Bristol, Avon). 2009;24(10):819-825. [13] 王筱筱,李呈,方红,等.平衡训练对老年人跌倒发生及平衡功能影响的Meta分析[J].护理研究,2019,33(5):775-780. [14] HASEGAWA J, SUZUKI H, YAMAUCHI T. Effect of a lower limb strength training program e on physical activity during the snowy season among community-dwelling elderly individuals. Ann Hum Biol. 2019;46(4):323-329. [15] SUNDSTRUP E, JAKOBSEN MD, ANDERSEN LL, et al. Positive effects of 1-year football and strength training on mechanical muscle function and functional capacity in elderly men. Eur J Appl Physiol. 2016;116(6): 1127-1138. [16] SAVELA S, KOMULAINEN P, SIPILA S, et al. Physical activity of the elderly - what kind of and what for? Duodecim. 2015;131(18):1719-1725. [17] PANO-RODRIGUEZ A, BELTRAN-GARRIDO JV, HERNANDEZ-GONZALEZ V, et al. Effects of whole-body electromyostimulation on physical fitness in postmenopausal women: a randomized controlled trial. Sensors (Basel). 2020;20(5):1482-1498. [18] HIGGINS JPT, GREEN S. Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0. The Cochrane Collaboration, 2011. [19] 崔尧,贾威,曾明,等.水中运动治疗对脑卒中患者下肢运动功能及日常生活活动能力效果的Meta分析[J].中国康复理论与实践,2020,26(3):263-277. [20] 罗杰,冷卫东.系统评价/Meta分析理论与实践[M].北京:军事医学科学出版社, 2013. [21] UEMATSU A, HORTOBÁGYI T, TSUCHIYA K, et al. Lower extremity power training improves healthy old adults’ gait biomechanics. Gait Posture. 2018;62(2):303-310. [22] MOTALEBI SA, AMIRZADEH IRANAGH J, MOHAMMADI F, et al. Efficacy of elastic resistance training program for the institutionalized elderly. Topics in Geriatric Rehabilitation. 2018;34(2):105-111. [23] LAMBERTI N, STRAUDI S, MALAGONI AM, et al. Effects of low-intensity endurance and resistance training on mobility in chronic stroke survivors: a pilot randomized controlled study. Eur J Phys Rehabil Med. 2017;53(2):228-239. [24] UEMATSU A, TSUCHIYA K, KADONO N, et al. A behavioral mechanism of how increases in leg strength improve old adults’ gait speed. PLoS One. 2014;9(10):e110350. [25] CARRAL JMC, RODRÍGUEZ AL, CARDALDA IM, et al. Muscle strength training program in nonagenarians – a randomized controlled trial. Rev Assoc Med Bras (1992). 2019;65(6):851-856. [26] YOON DH, KANG D, KIM HJ, et al. Effect of elastic band-based high-speed power training on cognitive function, physical performance and muscle strength in older women with mild cognitive impairment. Geriatr Gerontol Int. 2017;17(5):765-772. [27] PIRAUÁ ALT, CAVALCANTE BR, DE OLIVEIRA VMA, et al. Effect of 24-week strength training on unstable surfaces on mobility, balance, and concern about falling in older adults. Scand J Med Sci Sports. 2019;29(11): 1805-1812. [28] BUSKARD ANL, JACOBS KA, ELTOUKHY MM, et al. Optimal approach to load progressions during strength training in older adults. Med Sci Sports Exerc. 2019;51(11):2224-2233. [29] LANGONI CDS, RESENDE TL, BARCELLOS AB, et al. Effect of exercise on cognition, conditioning, muscle endurance, and balance in older adults with mild cognitive impairment: a randomized controlled trial. J Geriatr Phys Ther. 2019;42(2):E15-E22. [30] MOTALEBI SA, CHEONG LS, IRANAGH JA, et al. Effect of low-cost resistance training on lower-limb strength and balance in institutionalized seniors. Exp Aging Res. 2018;44(1):48-61. [31] BEIJERSBERGEN CMI, GRANACHER U, GÄBLER M, et al. Power Training-induced Increases in Muscle Activation during Gait in Old Adults. Med Sci Sports Exerc. 2017;49(11):2198-2025. [32] YU W, AN C, KANG H. Effects of resistance exercise using thera-band on balance of elderly adults: a randomized controlled trial. J Phys Ther Sci. 2013;25(11):1471-1473. [33] ANSAI JH, AURICHIO TR, GONCALVES R, et al. Effects of two physical exercise protocols on physical performance related to falls in the oldest old: a randomized controlled trial. Geriatr Gerontol Int. 2016;16(4): 492-501. [34] NICHOLSON VP, MCKEAN MR, BURKETT BJ. Low-load high-repetition resistance training improves strength and gait speed in middle-aged and older adults. J Sci Med Sport. 2015;18(5):596-600. [35] LEE IH, PARK SY. Balance improvement by strength training for the elderly. J Phys Ther Sci. 2013;25(12):1591-1594. [36] FRAGALA MS, CADORE EL, DORGO S, et al. Resistance training for older adults: position statement from the national strength and conditioning association. J Strength Cond Res. 2019;33(8):2019-2052. [37] COELHO-JUNIOR HJ, RODRIGUES B, GONÇALVES IO, et al. The physical capabilities underlying timed “Up and Go” test are time-dependent in community-dwelling older women. Exp Gerontol. 2018;104(5):138-146. [38] BARRY E, GALVIN R, KEOGH C, et al. Is the Timed Up and Go test a useful predictor of risk of falls in community dwelling older adults: a systematic review and meta-analysis. BMC Geriatr. 2014;14(14):1471-2318. [39] CLEMSON L, FIATARONE SINGH MA, BUNDY A, et al. Integration of balance and strength training into daily life activity to reduce rate of falls in older people (the LiFE study): randomised parallel trial. BMJ. 2012;345(7):e4547. [40] CADORE EL, CASAS-HERRERO A, ZAMBOM-FERRARESI F, et al. Multicomponent exercises including muscle power training Enhance muscle mass, power output, and functional outcomes in institutionalized frail nonagenarians. Age (Dordr). 2014;36(2): 773-785. [41] LONG J, CAI T, HUANG X, et al. Reference value for the TUG in healthy older people: a systematic review and meta-analysis. Geriatr Nurs. 2020;41(3):325-330. [42] LIU B, HU X, ZHANG Q, et al. Usual walking speed and all-cause mortality risk in older people: a systematic review and meta-analysis. Gait Posture. 2016;44(7):172-177. [43] CRUZ-JIMENEZ M. Normal changes in gait and mobility problems in the elderly. Phys Med Rehabil Clin N Am. 2017;28(4): 713-725. [44] REIS JG, COSTA GC, SCHMIDT A, et al. Do muscle strengthening exercises improve performance in the 6-minute walk test in postmenopausal women? Rev Bras Fisioter. 2012;16(3):236-240. [45] 梁雷超,吕娇娇,黄灵燕,等.认知-姿势控制双任务在老年人跌倒研究中的应用进展[J].中国康复理论,2016,22(11): 1289-1293. [46] HOLTZER R, EPSTEIN N, MAHONEY JR, et al. Neuroimaging of mobility in aging: a tar-geted review. J Gerontol A Biol Sci Med Sci. 2014;69(11):1375-1388. [47] HOLMES KC, GEEVES MA. The structural basis of muscle contraction. Philos Trans R Soc Lond B Biol Sci. 2000;355(1396): 419-431. [48] PETERSON CM, JOHANNSEN DL, RAVUSSIN E. Skeletal muscle mitochondria and aging: a review. Aging Res. 2012;2012:194821. [49] HOLLOWAY GP, HOLWERDA AM, MIOTTO PM, et al. Age-associated impairments in mitochondrial adp sensitivity contribute to redox stress in senescent human skeletal muscle. Cell Rep. 2018;22(7):2837-2848. [50] DE BRUIN ED, MURER K. Effect of additional functional exercises on balance in elderly people. Clin Rehabil. 2007;21(2):112-121. [51] HARTMANN A, MURER K, BIE RA, et al. The effect of a foot gymnastic exercise programme on gait performance in older adults: a randomised controlled trial. Disabil Rehabil. 2009;31(25):2101-2110. [52] HESS JA, WOOLLACOTT M. Effect of high-intensity strength-training on functional measures of balance ability in balance-impaired older adults. J Manipulative Physiol Ther. 2005;28(8):582-590. [53] JOSHUA AM, D’SOUZA V, UNNIKRISHNAN B, et al. Effectiveness of progressive resistance strength training versus traditional balance exercise in improving balance among the elderly-a randomised controlled trial. J Clin Diagn Res. 2014;8(3):98-102. [54] SAÑUDO B, GONZÁLEZ-NAVARRETE Á, ÁLVAREZ-BARBOSA F, et al. Effect of flywheel resistance training on balance performance in older adults. a randomized controlled trial. J Sports Sci Med. 2019;18(2):344-350. |
| [1] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [2] | Chen Jinping, Li Kui, Chen Qian, Guo Haoran, Zhang Yingbo, Wei Peng. Meta-analysis of the efficacy and safety of tranexamic acid in open spinal surgery [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1458-1464. |
| [3] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [4] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [5] | Wang Yongsheng, Wu Yang, Li Yanchun. Effect of acute high-intensity exercise on appetite hormones in adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1305-1312. |
| [6] | Kong Desheng, He Jingjing, Feng Baofeng, Guo Ruiyun, Asiamah Ernest Amponsah, Lü Fei, Zhang Shuhan, Zhang Xiaolin, Ma Jun, Cui Huixian. Efficacy of mesenchymal stem cells in the spinal cord injury of large animal models: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1142-1148. |
| [7] | Wang Jiangna, Zheng Huifen, Sun Wei. Changes in dynamic stability, motor coordination and joint mechanics of the lower extremity during stair descent and performing phone task [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 837-843. |
| [8] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Intravenous, topical tranexamic acid alone or their combination in total knee arthroplasty: a meta-analysis of randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 948-956. |
| [9] | Li Yan, Wang Pei, Deng Donghuan, Yan Wei, Li Lei, Jiang Hongjiang. Electroacupuncture for pain control after total knee arthroplasty: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 957-963. |
| [10] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| [11] | Hua Haotian, Zhao Wenyu, Zhang Lei, Bai Wenbo, Wang Xinwei. Meta-analysis of clinical efficacy and safety of antibiotic artificial bone in the treatment of chronic osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 970-976. |
| [12] | Zhan Fangbiao, Cheng Jun, Zou Xinsen, Long Jie, Xie Lizhong, Deng Qianrong. Intraoperative intravenous application of tranexamic acid reduces perioperative bleeding in multilevel posterior spinal surgery: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 977-984. |
| [13] | Yuan Chunhua, Cui Zhenzhen, Wu De. Meta-analysis of autologous bone marrow mesenchymal stem cell transplantation in the treatment of ischemic stroke [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(31): 5018-5024. |
| [14] | Yang Fengjiao, Wang Xiangbin, Hou Meijin, Yu Jiao, Li Zhenhui, Fu Shengxing, Lin Ziling, Liu Benke. Comparison of gait characteristics between young and elderly people under dual tasks using three-dimensional gait analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 344-349. |
| [15] | Zhong Yuanming, Wan Tong, Zhong Xifeng, Wu Zhuotan, He Bingkun, Wu Sixian. Meta-analysis of the efficacy and safety of percutaneous curved vertebroplasty and unilateral pedicle approach percutaneous vertebroplasty in the treatment of osteoporotic vertebral compression fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 456-462. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||