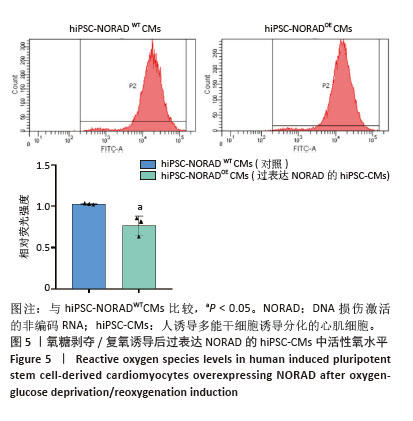
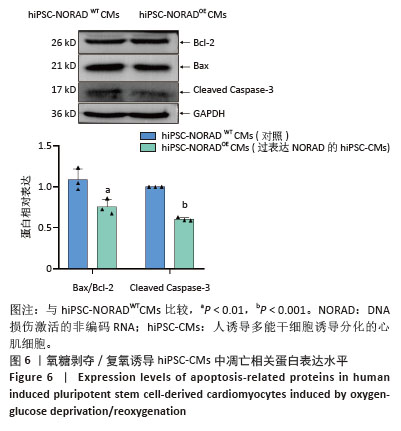
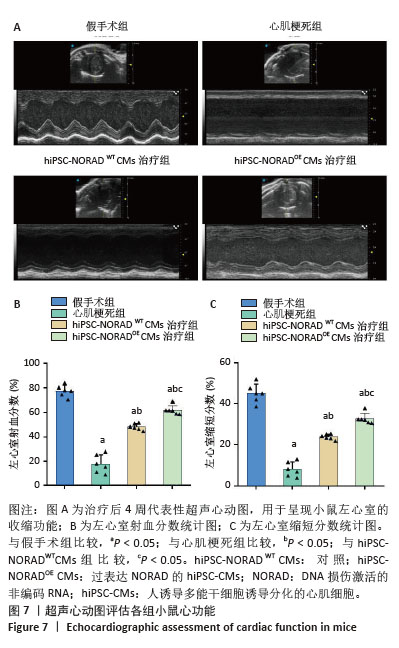
[1] CHORADIA A, BAI K, SONI S, et al. Beyond hot flashes: Exploring the role of estrogen therapy in postmenopausal women for myocardial infarction prevention and recovery. Biomol Biomed. 2024;24(1):4-13.
[2] SALARI N, MORDDARVANJOGHI F, ABDOLMALEKI A, et al. The global prevalence of myocardial infarction: a systematic review and meta-analysis. BMC Cardiovasc Disord. 2023;23(1):206.
[3] HU D, LI R, LI Y, et al. Inflammation-Targeted Nanomedicines Alleviate Oxidative Stress and Reprogram Macrophages Polarization for Myocardial Infarction Treatment. Adv Sci (Weinh). 2024;11(21):e2308910.
[4] MAGADUM A, SINGH N, KURIAN AA, et al. Pkm2 Regulates Cardiomyocyte Cell Cycle and Promotes Cardiac Regeneration. Circulation. 2020;141(15): 1249-1265.
[5] BAE J, SALAMON RJ, BRANDT EB, et al. Malonate Promotes Adult Cardiomyocyte Proliferation and Heart Regeneration. Circulation. 2021; 143(20):1973-1986.
[6] ZHANG H, PEI L, OUYANG Z, et al. AP-1 activation mediates post-natal cardiomyocyte maturation. Cardiovasc Res. 2023;119(2):536-550.
[7] GIACCA M. Cardiac Regeneration After Myocardial Infarction: an Approachable Goal. Curr Cardiol Rep. 2020;22(10):122.
[8] KINO T, KHAN M, MOHSIN S. The Regulatory Role of T Cell Responses in Cardiac Remodeling Following Myocardial Infarction. Int J Mol Sci. 2020;21(14):5013.
[9] YAN W, XIA Y, ZHAO H, et al. Stem cell-based therapy in cardiac repair after myocardial infarction: Promise, challenges, and future directions. J Mol Cell Cardiol. 2024;188:1-14.
[10] KARAKIKES I, AMEEN M, TERMGLINCHAN V, et al. Human induced pluripotent stem cell-derived cardiomyocytes: insights into molecular, cellular, and functional phenotypes. Circ Res. 2015;117(1):80-88.
[11] MUMMERY CL, ZHANG J, NG ES, et al. Differentiation of human embryonic stem cells and induced pluripotent stem cells to cardiomyocytes: a methods overview. Circ Res. 2012;111(3):344-358.
[12] LIN Y, GIL CH, YODER MC. Differentiation, Evaluation, and Application of Human Induced Pluripotent Stem Cell-Derived Endothelial Cells. Arterioscler Thromb Vasc Biol. 2017;37(11):2014-2025.
[13] PATSCH C, CHALLET-MEYLAN L, THOMA EC, et al. Generation of vascular endothelial and smooth muscle cells from human pluripotent stem cells. Nat Cell Biol. 2015;17(8):994-1003.
[14] ENGLE SJ, BLAHA L, KLEIMAN RJ. Best Practices for Translational Disease Modeling Using Human iPSC-Derived Neurons. Neuron. 2018; 100(4):783-797.
[15] POURRIER M, FEDIDA D. The Emergence of Human Induced Pluripotent Stem Cell-Derived Cardiomyocytes (hiPSC-CMs) as a Platform to Model Arrhythmogenic Diseases. Int J Mol Sci. 2020;21(2):657.
[16] SHARMA A, BURRIDGE PW, MCKEITHAN WL, et al. High-throughput screening of tyrosine kinase inhibitor cardiotoxicity with human induced pluripotent stem cells. Sci Transl Med. 2017;9(377):eaaf2584.
[17] SEIBERTZ F, SUTANTO H, DÜLK R, et al. Electrophysiological and calcium-handling development during long-term culture of human-induced pluripotent stem cell-derived cardiomyocytes. Basic Res Cardiol. 2023; 118(1):14.
[18] BHATTACHARYA S, BURRIDGE PW, KROPP EM, et al. High efficiency differentiation of human pluripotent stem cells to cardiomyocytes and characterization by flow cytometry. J Vis Exp. 2014;(91):52010.
[19] DEUSE T, HU X, GRAVINA A, et al. Hypoimmunogenic derivatives of induced pluripotent stem cells evade immune rejection in fully immunocompetent allogeneic recipients. Nat Biotechnol. 2019; 37(3):252-258.
[20] BIAN W, CHEN W, NGUYEN T, et al. miR-199a Overexpression Enhances the Potency of Human Induced-Pluripotent Stem-Cell-Derived Cardiomyocytes for Myocardial Repair. Front Pharmacol. 2021;12:673621.
[21] CAI H, HAN XJ, LUO ZR, et al. Pretreatment with Notoginsenoside R1 enhances the efficacy of neonatal rat mesenchymal stem cell transplantation in model of myocardial infarction through regulating PI3K/Akt/FoxO1 signaling pathways. Stem Cell Res Ther. 2024;15(1):419.
[22] MATTICK JS, AMARAL PP, CARNINCI P, et al. Long non-coding RNAs: definitions, functions, challenges and recommendations. Nat Rev Mol Cell Biol. 2023;24(6):430-447.
[23] LI K, WANG Z. lncRNA NEAT1: Key player in neurodegenerative diseases. Ageing Res Rev. 2023;86:101878.
[24] BRIDGES MC, DAULAGALA AC, KOURTIDIS A. LNCcation: lncRNA localization and function. J Cell Biol. 2021;220(2):e202009045.
[25] NI H, GE Y, ZHUGE Y, et al. LncRNA MIR181A1HG Deficiency Attenuates Vascular Inflammation and Atherosclerosis. Circ Res. 2025;136(8):862-883.
[26] YANG R, YANG B, LIU W, et al. Emerging role of non-coding RNAs in neuroinflammation mediated by microglia and astrocytes. J Neuroinflammation. 2023;20(1):173.
[27] VIERECK J, KUMARSWAMY R, FOINQUINOS A, et al. Long noncoding RNA Chast promotes cardiac remodeling. Sci Transl Med. 2016;8(326): 326ra22.
[28] SOGHLI N, YOUSEFI T, ABOLGHASEMI M, et al. NORAD, a critical long non-coding RNA in human cancers. Life Sci. 2021;264:118665.
[29] ALVES-VALE C, CAPELA AM, TAVARES-MARCOS C, et al. Expression of NORAD correlates with breast cancer aggressiveness and protects breast cancer cells from chemotherapy. Mol Ther Nucleic Acids. 2023; 33:910-924.
[30] SUN DS, GUAN CH, WANG WN, et al. LncRNA NORAD promotes proliferation, migration and angiogenesis of hepatocellular carcinoma cells through targeting miR-211-5p/FOXD1/VEGF-A axis. Microvasc Res. 2021;134:104120.
[31] ZHAO W, WANG L, XU F. LncRNA NORAD stimulates proliferation and migration of renal cancer via activating the miR-144-3p/MYCN axis. Eur Rev Med Pharmacol Sci. 2020;24(20):10426-10432.
[32] ZHANG Y, LI Y. Long non-coding RNA NORAD contributes to the proliferation, invasion and EMT progression of prostate cancer via the miR-30a-5p/RAB11A/WNT/β-catenin pathway. Cancer Cell Int. 2020;20(1):571.
[33] BIAN W, JING X, YANG Z, et al. Downregulation of LncRNA NORAD promotes Ox-LDL-induced vascular endothelial cell injury and atherosclerosis. Aging (Albany NY). 2020;12(7):6385-6400.
[34] ZHANG X, KAN X, SHEN J, et al. Increased long non-coding RNA NORAD reflects serious cardiovascular stenosis, aggravated inflammation status, and higher lipid level in coronary heart disease. J Clin Lab Anal. 2022; 36(11):e24717.
[35] HAN Y, TIAN H, GAO X. NORAD regulates proliferation and apoptosis in cardiomyocytes under high-glucose treatment through miRNA-150-5p/ZEB1 axis. Eur Rev Med Pharmacol Sci. 2020;24(21):11259-11265.
[36] REED GW, ROSSI JE, CANNON CP. Acute myocardial infarction. Lancet. 2017;389(10065):197-210.
[37] BUSSMANN WD, LÖHNER J, KALTENBACH M. Orally administered isosorbide dinitrate in patients with and without left ventricular failure due to acute myocardial infarction. Am J Cardiol. 1977;39(1):91-96.
[38] 覃可乐.成纤维细胞来源外泌体通过激活AMPK通路促进hiPSC-CMs成熟机制研究[D].长沙:中南大学,2023.
[39] PARIZADEH SM, JAFARZADEH-ESFEHANI R, GHANDEHARI M, et al. Stem cell therapy: A novel approach for myocardial infarction. J Cell Physiol. 2019;234(10):16904-16912.
[40] YAMANAKA S. Pluripotent Stem Cell-Based Cell Therapy-Promise and Challenges. Cell Stem Cell. 2020;27(4):523-531.
[41] FAN C, FAST VG, TANG Y, et al. Cardiomyocytes from CCND2-overexpressing human induced-pluripotent stem cells repopulate the myocardial scar in mice: A 6-month study. J Mol Cell Cardiol. 2019;137:25-33.
[42] TAO Z, LOO S, SU L, et al. Angiopoietin-1 enhanced myocyte mitosis, engraftment, and the reparability of hiPSC-CMs for treatment of myocardial infarction. Cardiovasc Res. 2021;117(6):1578-1591.
[43] ABBAS N, PERBELLINI F, THUM T. Non-coding RNAs: emerging players in cardiomyocyte proliferation and cardiac regeneration. Basic Res Cardiol. 2020;115(5):52.
[44] PICCOLI MT, GUPTA SK, THUM T. Noncoding RNAs as regulators of cardiomyocyte proliferation and death. J Mol Cell Cardiol. 2015; 89(Pt A):59-67.
[45] BUGGER H, PFEIL K. Mitochondrial ROS in myocardial ischemia reperfusion and remodeling. Biochim Biophys Acta Mol Basis Dis. 2020;1866(7):165768.
[46] SUN Q, MA H, ZHANG J, et al. A Self-Sustaining Antioxidant Strategy for Effective Treatment of Myocardial Infarction. Adv Sci (Weinh). 2023; 10(5):e2204999.
[47] XIANG M, LU Y, XIN L, et al. Role of Oxidative Stress in Reperfusion following Myocardial Ischemia and Its Treatments. Oxid Med Cell Longev. 2021;2021:6614009.
[48] ZHENG H, XU Y, LIEHN EA, et al. Vitamin C as Scavenger of Reactive Oxygen Species during Healing after Myocardial Infarction. Int J Mol Sci. 2024;25(6):3114.
[49] 李恩,孙利强,刘宗芳,等.瑞舒伐他汀对大鼠心肌梗死后活性氧物质产生及骨膜蛋白和心肌营养素表达的影响[J].中国循环杂志, 2014,29(10):823-827.
[50] LUO Z, XU X, SHO T, et al. ROS-induced autophagy regulates porcine trophectoderm cell apoptosis, proliferation, and differentiation. Am J Physiol Cell Physiol. 2019;316(2):C198-C209.
[51] XIONG X, LIU J, HE Q, et al. Long non-coding RNA NORAD aggravates acute myocardial infarction by promoting fibrosis and apoptosis via miR-577/COBLL1 axis. Environ Toxicol. 2021;36(11):2256-2265.
[52] LI C, ZHANG L, BU X, et al. LncRNA NORAD promotes the progression of myocardial infarction by targeting the miR-22-3p/PTEN axis. Acta Biochim Biophys Sin (Shanghai). 2022;54(4):463-473. |