Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (10): 1575-1580.doi: 10.3969/j.issn.2095-4344.1636
Previous Articles Next Articles
Biocompatibility of anodic titanium oxide: an experimental research
Liu Shaoyang, Zou Hanlin
- Department of Orthopedics, Shanghai Putuo District Central Hospital, Shanghai 200062, China
-
Received:2018-11-09 -
Contact:Zou Hanlin, Department of Orthopedics, Shanghai Putuo District Central Hospital, Shanghai 200062, China -
About author:Liu Shaoyang, Master, Physician, Department of Orthopedics, Shanghai Putuo District Central Hospital, Shanghai 200062, China
CLC Number:
Cite this article
Liu Shaoyang, Zou Hanlin . Biocompatibility of anodic titanium oxide: an experimental research[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(10): 1575-1580.
share this article
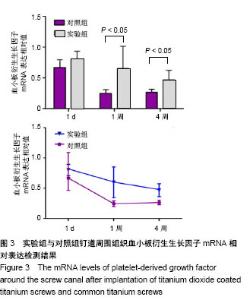
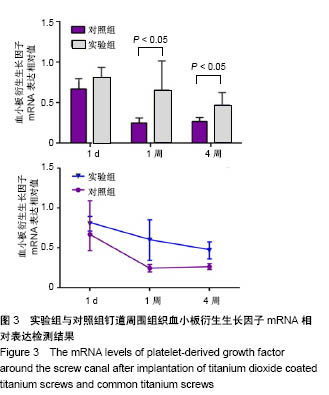
2.3 钛螺钉植入兔胫骨后的钉道周围生长因子检测结果 植入1 d末,两组血小板衍生生长因子mRNA表达相近,实验组略高于对照组,但差异无统计学意义(1.124±0.512,0.974±0.766,t=0.004,P=0.997)。植入1周末,对照组血小板衍生生长因子mRNA表达开始下降,实验组血小板衍生生长因子mRNA表达略升高,实验组血小板衍生生长因子mRNA表达高于对照组(1.353±0.450,0.191±0.088,P=0.045)。植入4周末,两组血小板衍生生长因子mRNA表达都开始下降,实验组血小板衍生生长因子mRNA表达高于对照组(0.572±0.291,0.186±0.217,t=-5.301,P < 0.01)。两组钉道周围组织血小板衍生生长因子mRNA相对表达变化,见图3,在整个实验过程中,实验组血小板衍生生长因子mRNA表达一直维持在较高水平。"
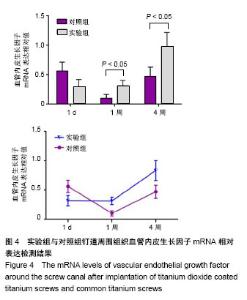
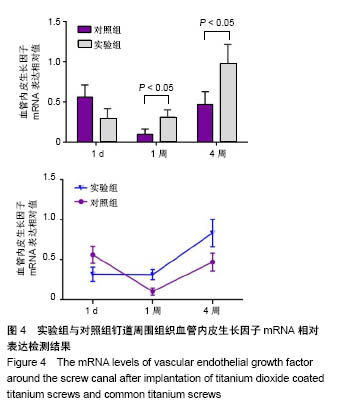
植入1 d末,两组血管内皮生长因子mRNA表达相近,实验组略低于对照组,但差异无统计学意义(0.302±0.045,0.178±0.039,t=0.506,P=0.056)。植入1周末,两组血管内皮生长因子mRNA表达都开始下降,对照组血管内皮生长因子mRNA表达下降更多,实验组血管内皮生长因子mRNA表达高于对照组(0.430±0.226,0.164±0.054,P= 0.019)。植入4周末,两组血管内皮生长因子mRNA表达都开始上升,实验组血管内皮生长因子mRNA表达高于对照组(0.287±0.018,0.516±0.016,t=-5.215,P <0.01)。两组钉道周围组织血管内皮生长因子mRNA相对表达变化,见图4。"
| [1] Moroni A, Vannini F, Mosca M, et al.State of the art review: techniques to avoid pin loosening and infection in external fixation. J Orthop Trauma.2002;16(3):189-195.[2] Mutsuzaki H, Sogo Y, Oyane A, et al.Improved bonding of partially osteomyelitic bone to titanium pins owing to biomimetic coating of apatite.Int J Mol Sci. 2013;14(12): 24366-14379.[3] Pieske O, Kaltenhauser F, Pichlmaier L, et al.Clinical benefit of hydroxyapatite-coated pins compared with stainless steel pins in external fixation at the wrist: A randomised prospective study. Injury. 2010;41(10):1031-1036.[4] Holt J, Hertzberg B, Weinhold P, et al.Decreasing bacterial colonization of external fixation pins through nitric oxide release coatings.J Orthop Trauma. 2011;25(7):432-437.[5] Guo C, Wang K, Hou S, et al. H2O2 and/or TiO2 photocatalysis under UV irradiation for the removal of antibiotic resistant bacteria and their antibiotic resistance genes. J Hazard Mater. 2017; 323(Pt B):710-718.[6] Jimenez-Tototzintle M, Ferreira IJ, Da Silva Duque S, et al. Removal of contaminants of emerging concern (CECs) and antibiotic resistant bacteria in urban wastewater using UVA/TiO2/H2O2 photocatalysis. Chemosphere. 2018;210: 449-457.[7] Moreira NFF, Narciso-Da-Rocha C, Polo-Lopez MI, et al.Solar treatment (H2O2, TiO2-P25 and GO-TiO2 photocatalysis, photo-Fenton) of organic micropollutants, human pathogen indicators, antibiotic resistant bacteria and related genes in urban wastewater. Water Res.2018;135:195-206.[8] Esfandiari N, Simchi A, Bagheri R.Size tuning of Ag-decorated TiO(2) nanotube arrays for improved bactericidal capacity of orthopedic implants. J Biomed Mater Res A.2014;102(8):2625-2635.[9] Zhang H,Sun Y,Tian A,et al.Improved antibacterial activity and biocompatibility on vancomycin-loaded TiO2 nanotubes: in vivo and in vitro studies. Int J Nanomedicine. 2013;8: 4379-4389.[10] Maurer TB, Ochsner PE, Schwarzer G, et al.Increased loosening of cemented straight stem prostheses made from titanium alloys. An analysis and comparison with prostheses made of cobalt-chromium-nickel alloy.Int Orthop. 2001;25(2): 77-80.[11] Shim J, Seo YS, Oh BT, et al. Microbial inactivation kinetics and mechanisms of carbon-doped TiO 2 (C-TiO 2) under visible light. J Hazard Mater. 2016;306:133-139.[12] Gao A, Hang R, Huang X, et al.The effects of titania nanotubes with embedded silver oxide nanoparticles on bacteria and osteoblasts. Biomaterials. 2014;35(13): 4223-4235.[13] Leitner L, Malaj I, Sadoghi P, et al.Pedicle screw loosening is correlated to chronic subclinical deep implant infection: a retrospective database analysis. Eur Spine J. 2018; 27(10): 2529-2535.[14] Agrawal A. Pedicle screw nut loosening: potentially avoidable causes of spine instrumentation failure. Asian Spine J. 2014; 8(2): 224-226.[15] Lawes TJ, Scott JC, Goodship AE.Increased insertion torque delays pin-bone interface loosening in external fixation with tapered bone screws. J Orthop Trauma.2004;18(9):617-622.[16] Hee HT, Khan MS, Goh JC, et al.Insertion torque profile during pedicle screw insertion of the thoracic spine with and without violation of the pedicle wall: comparison between cylindrical and conical designs. Spine (Phila Pa 1976). 2006; 31(22):E840-846.[17] Chatzistergos PE, Magnissalis EA, Kourkoulis SK.Numerical simulation of bone screw induced pretension: the cases of under-tapping and conical profile. Med Eng Phys. 2014;36(3): 378-386.[18] Pettine KA, Chao EY, Kelly PJ. Analysis of the external fixator pin-bone interface. Clin Orthop Relat Res. 1993;(293):18-27.[19] Siamos G, Winkler S, Boberick KG. Relationship between implant preload and screw loosening on implant-supported prostheses.J Oral Implantol.2002;28(2): 67-73.[20] 姚珍松,唐永超,陈康,等.骨水泥螺钉强化固定伴骨质疏松腰椎滑脱症的稳定性及椎间融合[J].中国组织工程研究, 2016,20(4): 517-521.[21] Partale K, Klein P, Schell H, et al.Poly(D,L-lactide) coating is capable of enhancing osseous integration of Schanz screws in the absence of infection. J Biomed Mater Res B Appl Biomater. 2005; 74(1):608-616.[22] Rammelt S, Illert T, Bierbaum S, et al.Coating of titanium implants with collagen, RGD peptide and chondroitin sulfate. Biomaterials.2006;27(32):5561-5571.[23] 韩建业,于振涛,周廉.羟基磷灰石/TiO2生物活性复合涂层的研究进展[C].第六届中国功能材料及其应用学术会议论文集, 2007:1808-1812.[24] Brammer KS, Oh S, Cobb CJ, et al.Improved bone-forming functionality on diameter-controlled TiO2 nanotube surface. Acta Biomaterialia. 2009;5(8):3215-3223.[25] Ercan B, Webster TJ. The effect of biphasic electrical stimulation on osteoblast function at anodized nanotubular titanium surfaces. Biomaterials. 2010;31(13):3684-3693.[26] Uhm SH, Song DH, Kwon JS, et al.Tailoring of antibacterial Ag nanostructures on TiO2 nanotube layers by magnetron sputtering.J Biomed Mater Res B Appl Biomater. 2014; 102(3):592-603.[27] Singh AV, Vyas V, Patil R, et al. Quantitative characterization of the influence of the nanoscale morphology of nanostructured surfaces on bacterial adhesion and biofilm formation. PLoS One.2011;6(9): e25029.[28] Gunasekaran T, Nigusse T, Dhanaraju MD. Silver nanoparticles as real topical bullets for wound healing. J Am Coll Clin Wound Spec. 2011;3(4):82-96.[29] Franchini A, Ottaviani E. Repair of molluscan tissue injury: role of PDGF and TGF-beta1. Tissue Cell. 2000;32(4): 312-321.[30] Si HP, Lu ZH, Lin YL, et al. Transfect bone marrow stromal cells with pcDNA3.1-VEGF to construct tissue engineered bone in defect repair. Chin Med J (Engl). 2012;125(5): 906-911.[31] Eming SA, Krieg T. Molecular mechanisms of VEGF-A action during tissue repair. J Investig Dermatol Symp Proc. 2006; 11(1):79-86.[32] Hong YK, Lange-Asschenfeldt B,Velasco P, et al. VEGF-A promotes tissue repair-associated lymphatic vessel formation via VEGFR-2 and the alpha1beta1 and alpha2beta1 integrins. FASEB J. 2004; 18(10): 1111-1113.[33] Mutsuzaki H,Ito A,Sakane M,et al. Fibroblast growth factor-2-apatite composite layers on titanium screw to reduce pin tract infection rate. J Biomed Mater Res B Appl Biomater. 2008;86(2):365-374.[34] Mutsuzaki H, Ito A, Sakane M, et al. Calcium phosphate coating formed in infusion fluid mixture to enhance fixation strength of titanium screws. J Mater Sci Mater Med. 2007; 18(9):1799-1808. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [3] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [4] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [5] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [6] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [7] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [8] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [9] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [10] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [11] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [12] | Wang Hao, Chen Mingxue, Li Junkang, Luo Xujiang, Peng Liqing, Li Huo, Huang Bo, Tian Guangzhao, Liu Shuyun, Sui Xiang, Huang Jingxiang, Guo Quanyi, Lu Xiaobo. Decellularized porcine skin matrix for tissue-engineered meniscus scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3473-3478. |
| [13] | Mo Jianling, He Shaoru, Feng Bowen, Jian Minqiao, Zhang Xiaohui, Liu Caisheng, Liang Yijing, Liu Yumei, Chen Liang, Zhou Haiyu, Liu Yanhui. Forming prevascularized cell sheets and the expression of angiogenesis-related factors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3479-3486. |
| [14] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| [15] | Liu Liyong, Zhou Lei. Research and development status and development trend of hydrogel in tissue engineering based on patent information [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3527-3533. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||