Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (31): 5068-5074.doi: 10.3969/j.issn.2095-4344.2014.31.025
Previous Articles Next Articles
Clinical application of intra-articular injection drugs in orthopedics: features and value
Ma Jin-hui1, Sun Wei2, Gao Fu-qiang2, Wang Yun-ting2, Li Zi-rong2
- 1Department of Orthopedics, 2Department of Orthopedic Surgery, Osteonecrosis and Joint Reservation Reconstruction Center, China-Japan Friendship Hospital, Peking University, Beijing 100029, China
-
Received:2014-05-07Online:2014-07-23Published:2014-07-23 -
Contact:Sun Wei, Chief physician, Associate professor, Master’s supervisor, Department of Orthopedic Surgery, Osteonecrosis and Joint Reservation Reconstruction Center, China-Japan Friendship Hospital, Peking University, Beijing 100029, China -
About author:Ma Jin-hui, Studying for master’s degree, Department of Orthopedics, China-Japan Friendship Hospital, Peking University, Beijing 100029, China -
Supported by:the National Natural Science Foundation of China, No. 81372013; the General Project of China-Japan Friendship Hospital, No. 2013-MS-27
CLC Number:
Cite this article
Ma Jin-hui, Sun Wei, Gao Fu-qiang, Wang Yun-ting, Li Zi-rong. Clinical application of intra-articular injection drugs in orthopedics: features and value[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(31): 5068-5074.
share this article
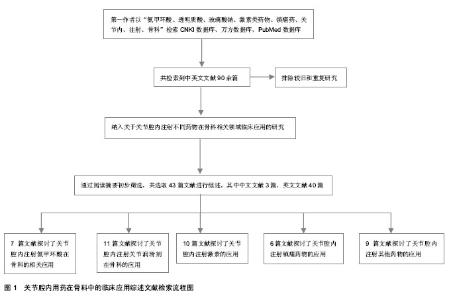
2.1 关节腔内注射止血剂——氨甲环酸 氨甲环酸是赖氨酸合成的衍生物,作用机制为与纤溶酶原结合,阻止纤溶酶降解纤维蛋白,起到抗纤溶作用,但不增加纤维蛋白的合成[8]。 关节内注射氨甲环酸可以减少全膝关节置换后失血量及患者的输血需要,氨甲环酸分子主要在局部伤口的活动性出血点起作用,而并不是在出血的血管内部发挥作用,同时基于关节内的氨甲环酸对纤溶蛋白降解过程存在竞争性与非竞争性抑制作用,继发于非竞争性抑制纤维蛋白溶解作用,其极可能具有促进纤维蛋白凝血块稳定的作用,将有效减少来自于受损伤组织表面所渗出、漏出的血液丢失[9]。 此外,关节内注射氨甲环酸与静脉注射比较,能更有效地减少行全膝关节置换患者术后引流管中的血液流失量及术后输血量及输血次数,且不良反应小,尤其适用于患有心血管疾病、肾功能不全等高危患者。同时氨甲环酸能够通过维持患者的血流动力学稳定、减少输血而产生的不良反应、并发症来改善全膝关节置换后患者的一般情况,有助于患者的早期康复及进行早期功能锻炼,减少患者住院时间,降低因住院时间长可能引起的肺部感染等并发症的发生率[10]。研究表明,在接受全膝关节置换的患者中局部(用配有氨甲环酸的盐水冲洗切口)与关节内联合应用氨甲环酸平均减少246 mL的隐性失血,在术后不放置引流的情况下同样可以减少患者术后的失血量与输血需要[11]。Mutsuzaki等[12]指出,在非骨水泥型全膝关节置换手术切口缝合后、松止血带之前,通过患者膝部留置的引流管注射氨甲环酸,并立刻夹闭引流管1 h,可以减少患者置换后48 h内引流管引流量、血液流失与输血需要,与没有注射氨甲环酸和夹闭引流管的患者相比,置换后第7天的血红蛋白水平明显升高,同时由于术后出血的减少,这些患者皮下与关节内血肿的发生率也显著减少。Ishida等[13]同样指出,在全膝关节置换结束时通过引流管向膝关节腔内注射氨甲环酸不仅可以减少置换后失血量,还具有缓解膝关节肿胀的功效,作用机制主要是通过减少膝关节内的隐性失血,这将很有可能降低全膝关节置换后患者的不适感。 文献报道,计算机辅助下的全膝关节置换后患者手术切口关闭后,向关节腔内注射低剂量的氨甲环酸溶液(把250 mg的氨甲环酸溶于25 mL生理盐水中,相当于氨甲环酸的浓度为10 g/L),并立刻夹闭引流管2 h,不但可以维持关节内的氨甲环酸药物浓度,并且由于有足够时间使药物达到抗纤溶作用,还可以阻止血液流动增加而造成的较快速血液流失[14]。关节内注射氨甲环酸联合引流管夹闭可以产生增加局部血栓形成、延长纤维蛋白凝块溶解时间的效应,并且这种效应是暂时的,不会增加远期并发症。 由上可知,关节腔内注射氨甲环酸具有以下优点:一是方法简单,易于操作,花费较低;二是关节腔内注射氨甲环酸联合引流管夹闭可以使关节局部达到较高的药物浓度,具促进血栓形成,缩短受损伤血管闭塞时间的作用[7],避免了静脉用药导致药物全身吸收而带来的全身不良反应;三是关节内注射氨甲环酸不仅可以减少患者术后引流管中的失血量、输血需要与输血率,而且可以减少关节内部的隐性失血,缓解关节肿胀和关节内血肿,令患者术后的满意度提高。因此,关节内注射氨甲环酸较静脉应用是一种更加有效的手段。 2.2 关节腔内注射关节润滑剂——透明质酸、玻璃酸钠 透明质酸是一种高分子直链多聚糖[15],由滑液中的B细胞及单核巨噬细胞所分泌[16],广泛存在于人体的结缔组织基质中。其化学结构的不规则卷曲状态及溶解状态下的流体动力学特性,使其具有高度的黏弹性、可塑变形性和渗透性。同时透明质酸还具有分子屏障的作用,可以阻止炎症递质在关节腔内扩散,抑制纤维母细胞活动和淋巴细胞游走[17],降低滑膜下的痛觉器与感觉纤维的兴奋性,从而保护关节的结构,维持关节内环境的稳定[18]。 有动物实验报道,对于需要固定8周的膝关节损伤动物模型[19],对其关节内注射透明质酸可以减少长期固定后的关节黏连,降低滑膜组织中的胶原蛋白含量,增加固定后的关节活动范围。此动物实验提示,对于需要关节固定至少8周的患者,包括接受关节镜下前交叉韧带或后交叉韧带重建的患者、关节内或外骨折的患者、严重创伤后行关节清创的患者等等,关节内应用透明质酸可以预防关节粘连,改善关节活动度。关节内注射透明质酸被公认为是一种可以减轻关节软骨摩擦的有效方法,广泛应用于骨关节炎的治疗与预防,还可以预防膝关节、颞下颌关节、屈肌腱和肩袖手术后的粘连[19]。"
| [1] Evans CH, Kraus VB, Setton LA. Progress in intra-articular therapy. Nat Rev Rheumatol. 2014;10(1):11-22. [2] Zhao-yu C, Yan G, Wei C, et al. Reduced blood loss after intra-articular tranexamic acid injection during total knee arthroplasty: a meta-analysis of the literature. Knee Surg Sports Traumatol Arthrosc. 2013. [Epub ahead of print] [3] Lo GH, LaValley M, McAlindon T, et al. Intra-articular hyaluronic acid in treatment of knee osteoarthritis: a meta-analysis. JAMA. 2003;290(23): 3115-3121. [4] Lavelle W, Lavelle ED, Lavelle L. Intra-articular injections. Anesthesiol Clin. 2007;25(4): 853-862. [5] Hollander JL, Brown EM Jr, Jessar RA, et al. Hydrocortisone and cortisone injected into arthritic joints; comparative effects of and use of hydrocortisone as a local antiarthriti agent. JAMA.1951;147(17):1629-1635. [6] Maricar N, Callaghan MJ, Felson DT, et al. Predictors of response to intra-articular steroid injections in knee osteoarthritis-a systematic review. Rheumatology (Oxford). 2013;52(6): 1022-1032. [7] Furtado RN, Oliveira LM, Natour J. Polyarticular corticosteroid injection versus systemic administration in treatment of rheumatoid arthritis patients: a randomized controlled study.J Rheumatol. 2005;32(9):1691-1698. [8] Rama KR,Apsingi S,Poovali S,et al. Timing of tourniquet releasc in knee arthmplasty. Meta-analysis of randomized, controlled trials. J Bone Joint Surg Am. 2007; 89(4):699-705. [9] Roy SP, Tanki UF, Dutta A, et al. Efficacy of intra-articular tranexamic acid in blood loss reduction following primary unilateral total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2012;20(12): 2494-2501. [10] Seo JG, Moon YW, Park SH, et al. The comparative efficacies of intra-articular and IV tranexamic acid for reducing blood loss during total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2013;21(8): 1869-1874. [11] Craik JD, Shafie SAEI, Kidd AG, et al. Can local administration of tranexamic acid during total knee arthroplasty reduce blood loss and transfusion requirements in the absence of surgical drains? Eur J Orthop Surg Traumatol. 2014;24(3):379-384. [12] Mutsuzaki H, Ikeda K. Intra-articular injection of tranexamic acid via a drain plus drain-clamping to reduce blood loss in cementless total knee arthroplasty. J Orthop Surg Res. 2012; 7(1): 32. [13] Ishida K, Tsumura N, Kitagawa A, et al. Intra-articular injection of tranexamic acid reduces not only blood loss but also knee joint swelling after total knee arthroplasty. Int Orthop. 2011; 35(11): 1639-1645. [14] Sa-ngasoongsong P, Channoom T, Kawinwonggowit V, et al. Postoperative blood loss reduction in computer-assisted surgery total knee replacement by low dose intra-articular tranexamic acid injection together with 2-hour clamp drain: a prospective triple-blinded randomized controlled trial. Orthop Rev (Pavia). 2011;3(2): e12. [15] Gaffney J, Matou-Nasri S, Grau-Olivares M, et al. Therapeutic applications of hyaluronan. Mol Biosyst. 2010; 6(3): 437-443. [16] Curran MP. Hyaluronic acid (Supartz®): a review of its use in osteoarthritis of the knee. Drugs Aging. 2010;27(11): 925-941. [17] Lázaro JAS, Granado PC, del Sol MG, et al. The role of different hyaluronic acids in the articular cartilage of rabbit. Open Orthop J. 2010;4: 44-47. [18] 刘成龙,郭亭,赵建宁.关节腔内用药治疗膝关节骨关节炎的探讨[J].中国骨伤杂志,2012,25(10),877-879. [19] Wang M, Liu C, Xiao W. Intra-articular injection of hyaluronic acid for the reduction in joint adhesion formation in a rabbit model of knee injury. Knee Surg Sports Traumatol Arthrosc. 2013. [Epub ahead of print] [20] Lu HT, Sheu MT, Lin YF, et al. Injectable hyaluronic-acid-增doxycycline hydrogel therapy in experimental rabbit osteoarthritis. BMC Vet Res. 2013;9(1): 68. [21] Oka H, Akune T, Muraki S, et al. The mid-term efficacy of intra-articular hyaluronic acid injections on joint structure: a nested case control study. Mod Rheumatol. 2013;23(4): 722-728. [22] Abate M, Scuccimarra T, Vanni D, et al. Femoroacetabular impingement: is hyaluronic acid effective? Knee Surg Sports Traumatol Arthrosc. 2013. [Epub ahead of print] [23] Nganvongpanit K, Boonsri B, Sripratak T, et al. Effects of one-time and two-time intra-articular injection of hyaluronic acid sodium salt after joint surgery in dogs. J Vet Sci. 2013; 14(2): 215-222. [24] Migliore A, Bella A, Bisignani M, et al. Total hip replacement rate in a cohort of patients affected by symptomatic hip osteoarthritis following intra-articular sodium hyaluronate (MW 1,500–2,000 kDa) ORTOBRIX study. Clin Rheumatol. 2012;31(8): 1187-1196. [25] Lorbach O, Kieb M, Scherf C, et al. Good results after fluoroscopic-guided intra-articular injections in the treatment of adhesive capsulitis of the shoulder. Knee Surg Sports Traumatol Arthrosc. 2010;18(10): 1435-1441. [26] Giraddi GB, Siddaraju A, Kumar B, et al. Internal Derangement of Temporomandibular Joint: An Evaluation of Effect of Corticosteroid Injection Compared with Injection of Sodium Hyaluronate after Arthrocentesis. J Maxillofac Oral Surg. 2012;11(3): 258-263. [27] Lu YC, Evans CH, Grodzinsky AJ. Effects of short-term glucocorticoid treatment on changes in cartilage matrix degradation and chondrocyte gene expression induced by mechanical injury and inflammatory cytokines. Arthritis Res Ther. 2011;13(5): R142. [28] Song YW, Zhang T, Wang WB. Gluococorticoid could influence extracellular matrix synthesis through Sox9 via p38 MAPK pathway. Rheumatol Int. 2012;32(11): 3669-3673. [29] Habib G, Jabbour A, Artul S, et al. Intra-articular methylprednisolone acetate injection at the knee joint and the hypothalamic–pituitary–adrenal axis: a randomized controlled study.Clin Rheumatol. 2014;33(1): 99-103. [30] Wang X, Jia D, Chen X, et al. Comparison of intra-articular low-dose sufentanil, ropivacaine, and combined sufentanil and ropivacaine on post-operative analgesia of isolated anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc. 2013;21(5): 1140-1145. [31] Senthilkumaran S, Tate R, Read JRM, et al. Intra-articular morphine and bupivicaine for post-operative analgesia in anterior cruciate ligament reconstruction: a prospective randomised controlled trial. Knee Surg Sports Traumatol Arthrosc. 2010;18(6): 731-735. [32] Zink W, Zausig YA, Graf BM. Intra-articular injection of levobupivacaine. Anaesthesist. 2013;62(3): 213-212. [33] Dragoo JL, Braun HJ, Kim HJ et al.The in vitro chondrotoxicity of single-dose local anes thetics. Am J Sports Med. 2012;40: 794-799. [34] Park J, Sutradhar BC, Hong G et al. Comparison of the cytotoxic effects of bupivacaine, lidocaine, and mepivacaine in equine articular chondrocytes. Vet Anaesth Analg. 2011; 38:127-133. [35] Iannitti T, Lodi D, Palmieri B. Intra-Articular Injections for the Treatment of Osteoarthritis Focus on the Clinical Use of Hyaluronic Acid. Drugs R D. 2011; 11(1): 13-27. [36] Sun R,Zhao W,Hao Q,et al. Intra-articular clonidine for post-operative analgesia following arthroscopic knee surgery: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc. 2013. [37] 于其龙,王宗江.骨肽关节内注射治疗膝骨性关节炎的疗效观察[J].中国医药指南,2010,8(30):29-30. [38] 阮莲芝.骨肽注射液的临床应用[J].中国临床药学杂志,2008, 17(5): 320-322. [39] Rodriguez-Merchan EC. Intra-articular Injections of Hyaluronic Acid and Other Drugs in the Knee Joint. HSS J. 2013;9(2): 180-182. [40] Frizziero A, Giannotti E, Ferraro C, et al. Platelet rich plasma intra-articular injections: a new therapeutic strategy for the treatment of knee osteoarthritis in sport rehabilitation. A systematic review. Sport Sciences for Health. 2012;8(1): 15-22. [41] Nagai T, Kyo A, Hasui K, et al. Efficacy of an immunotoxin to folate receptor beta in the intra-articular treatment of antigen-induced arthritis. Arthritis Res Ther. 2012;14: R106. [42] Mokbel AN, El Tookhy OS, Shamaa AA, et al. Homing and reparative effect of intra-articular injection of autologus mesenchymal stem cells in osteoarthritic animal model. BMC Musculoskelet Disord. 2011;12(1): 259. [43] Desando G, Cavallo C, Sartoni F, et al. Intra-articular delivery of adipose derived stromal cells attenuates osteoarthritis progression in an experimental rabbit model. Arthritis Res Ther. 2013;15(1): R22. |
| [1] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [2] | Peng Zhihao, Feng Zongquan, Zou Yonggen, Niu Guoqing, Wu Feng. Relationship of lower limb force line and the progression of lateral compartment arthritis after unicompartmental knee arthroplasty with mobile bearing [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1368-1374. |
| [3] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [4] | Chen Jinping, Li Kui, Chen Qian, Guo Haoran, Zhang Yingbo, Wei Peng. Meta-analysis of the efficacy and safety of tranexamic acid in open spinal surgery [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1458-1464. |
| [5] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [6] | Liu Xiangxiang, Huang Yunmei, Chen Wenlie, Lin Ruhui, Lu Xiaodong, Li Zuanfang, Xu Yaye, Huang Meiya, Li Xihai. Ultrastructural changes of the white zone cells of the meniscus in a rat model of early osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1237-1242. |
| [7] | Yuan Jun, Yang Jiafu. Hemostatic effect of topical tranexamic acid infiltration in cementless total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 873-877. |
| [8] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Intravenous, topical tranexamic acid alone or their combination in total knee arthroplasty: a meta-analysis of randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 948-956. |
| [9] | Zhan Fangbiao, Cheng Jun, Zou Xinsen, Long Jie, Xie Lizhong, Deng Qianrong. Intraoperative intravenous application of tranexamic acid reduces perioperative bleeding in multilevel posterior spinal surgery: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 977-984. |
| [10] | Liu Xin, Yan Feihua, Hong Kunhao. Delaying cartilage degeneration by regulating the expression of aquaporins in rats with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 668-673. |
| [11] | Ma Zetao, Zeng Hui, Wang Deli, Weng Jian, Feng Song. MicroRNA-138-5p regulates chondrocyte proliferation and autophagy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 674-678. |
| [12] | Cao Xuhan, Bai Zixing, Sun Chengyi, Yang Yanjun, Sun Weidong. Mechanism of “Ruxiang-Moyao” herbal pair in the treatment of knee osteoarthritis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 746-753. |
| [13] | Li Yonghua, Feng Qiang, Tan Renting, Huang Shifu, Qiu Jinlong, Yin Heng. Molecular mechanism of Eucommia ulmoides active ingredients treating synovitis of knee osteoarthritis: an analysis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 765-771. |
| [14] | Song Shan, Hu Fangyuan, Qiao Jun, Wang Jia, Zhang Shengxiao, Li Xiaofeng. An insight into biomarkers of osteoarthritis synovium based on bioinformatics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 785-790. |
| [15] | Deng Zhenhan, Huang Yong, Xiao Lulu, Chen Yulin, Zhu Weimin, Lu Wei, Wang Daping. Role and application of bone morphogenetic proteins in articular cartilage regeneration [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 798-806. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||