Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (13): 1969-1974.doi: 10.3969/j.issn.2095-4344.2014.13.001
Mechanical analysis of total hip replacement with cup of different diameters in patients with developmental dysplasia of hip
Xu Jie, Ma Ruo-fan, Cai Zhi-qing, Li Deng
- Department of Orthopedics, Sun Yat-sen Memorial Hospital, Sun Yat-sen University, Guangzhou 510120, Guangdong Province, China
-
Received:2014-01-16Online:2014-03-26Published:2014-03-26 -
About author:Xu Jie, M.D., Associate professor, Associate chief physician, Department of Orthopedics, Sun Yat-sen Memorial Hospital, Sun Yat-sen University, Guangzhou 510120, Guangdong Province, China
CLC Number:
Cite this article
Xu Jie, Ma Ruo-fan, Cai Zhi-qing, Li Deng. Mechanical analysis of total hip replacement with cup of different diameters in patients with developmental dysplasia of hip[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(13): 1969-1974.
share this article
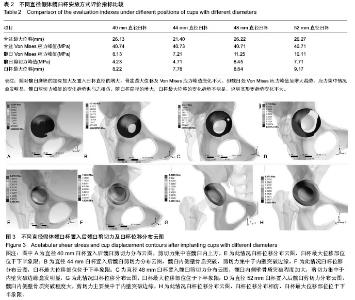
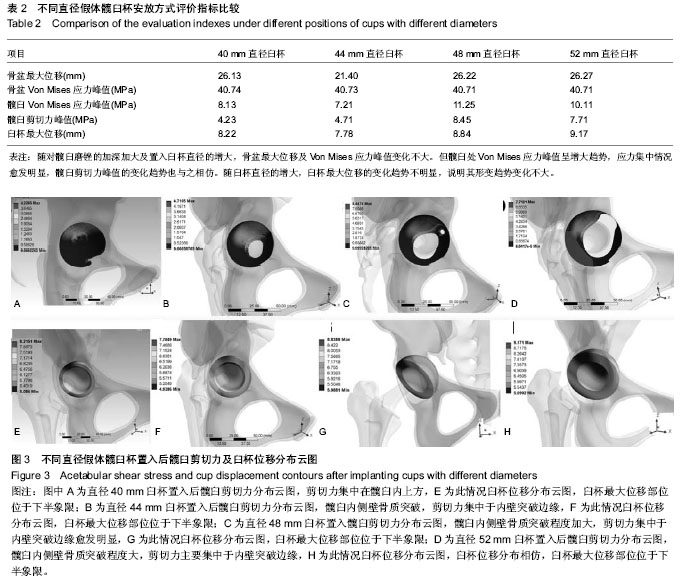
试验基于临床发育性髋关节脱位患者的术前三维CT 图像,建立了CroweⅡ型骨盆三维有限元模型。模型较精细,包括410 164个节点,264 187个单元,变形髋臼位置显示清晰。模拟患侧单下肢站立的情况,对骨盆受力情况进行初步分析。 2.1 各模型骨盆位移及应力分布变化 在设定了一定的约束之后,骨盆在受到力学加载后可能会出现沿冠状面或矢状面的位移,从而会影响到关节的力学环境。从图1A-D中可以看出各模型的位移情况,在此种载荷条件下骨盆的最大位移在髂骨翼的后部。臼杯使用尺寸的不同,骨盆的位移基本相同。大杯打磨掉更多的骨质使得髋臼处骨质变薄,但就整个骨盆的强度和刚度而言没出现明显下降。 而就整个骨盆的应力分布云图所见(图1E-H),最大应力集中区域为髂骨翼下方接近坐骨大切迹处,随臼杯直径的变化未见明显变化趋势(表2)。 2.2 各模型髋臼Von Mises应力分布变化 通过应力云图可以看到,由于髋臼骨床形态学的改变,单腿站立时应力主要集中在髋臼顶部及内侧壁。各模型髋臼上的Von Mises应力比较,从髋臼峰值Von Mises应力的比较看,44 mm臼杯模型最小,随臼杯直径的加大,应力峰值加大。对比整个臼杯的受力情况,40 mm臼杯置入后,除髋臼顶外,髋臼其余部分应力分布较为均匀,这在44 mm臼杯置入模型中同样可见,同时因44 mm直径臼杯较40 mm直径臼杯接触面积更大,单位面积所受应力相对较少。至48 mm直径臼杯置入模型,因髋臼内侧已有部分突破,云图可见髋臼顶应力集中区偏下方处出现应力值较低区,此区域在 52 mm直径臼杯置入模型因骨质突破更为明显而有所扩大,使得除髋臼顶部应力集中区外,其余部分应力分布欠均匀(图2,表2)。"

| [1] Aksoy C, Yilgor C, Demirkiran G, et al. Evaluation of acetabular development after Dega acetabuloplasty in developmental dysplasia of the hip. J Pediatr Orthop B. 2013; 22(2):91-95.[2] Bracken J, Tran T, Ditchfield M. Developmental dysplasia of the hip: controversies and current concepts. J Paediatr Child Health. 2012;48(11):963-973.[3] Nemeth BA, Narotam V. Developmental dysplasia of the hip. Pediatr Rev. 2012. 33(12): 553-561.[4] Rogers BA, Garbedian S, Kuchinad RA, et al. Total hip arthroplasty for adult hip dysplasia. J Bone Joint Surg Am. 2012;94(19): 1809-1821.[5] Westacott D, Pattison G, Cooke S. Developmental dysplasia of the hip. Community Pract. 2012;85(11): 42-44.[6] Hvid I. Neonatal hip instability, developmental dysplasia of the acetabulum, and the risk of early osteoarthrosis. Acta Orthop. 2008;79(3): 311-312.[7] Inan M, Chan G, Bowen JR. The correction of leg-length discrepancy after treatment in developmental dysplasia of the hip by using a percutaneous epiphysiodesis. J Pediatr Orthop B. 2008;17(1): 43-46.[8] Bozek M, Bielecki T, Nowak R, et al. Arthroplasty in patients with congenital hip dysplasia--early evaluation of a treatment method. Ortop Traumatol Rehabil. 2013; 15(1):49-59.[9] Li H, Wang L, Dai K, et al. Autogenous impaction grafting in total hip arthroplasty with developmental dysplasia of the hip. J Arthroplasty. 2013;28(4): 637-643.[10] Schofer MD, Pressel T, Schmitt J, et al. Reconstruction of the acetabulum in THA using femoral head autografts in developmental dysplasia of the hip. J Orthop Surg Res. 2011; 6: 32.[11] Yang S, Cui Q. Total hip arthroplasty in developmental dysplasia of the hip: Review of anatomy, techniques and outcomes. World J Orthop. 2012; 3(5): 42-48.[12] 艾进伟, 韩叶萍. Zweymüller系统在Crowe-Ⅲ、Ⅳ型髋臼发育不良全髋置换中的应用[J]. 中国组织工程研究与临床康复,2008, 12(44): 8615-8618.[13] Hintermann B, Morscher EW. Total hip replacement with solid autologous femoral head graft for hip dysplasia. Arch Orthop Trauma Surg. 1995;114(3): 137-144.[14] Mulroy RD Jr, Harris WH. Failure of acetabular autogenous grafts in total hip arthroplasty. Increasing incidence: a follow-up note. J Bone Joint Surg Am. 1990; 72(10):1536-1540.[15] Mitsuo N. Recent research and development in titanium alloys for biomedical applications and healthcare goods. Sci Technol Advan Mater. 2003;4:445-454.[16] Callaghan JJ, Rosenberg AC, Rubash HE, et al. The adult hip. lippincott. 1st ed. Williams & Wilkins, 1988: 15.[17] 赵诗奎. 氧化锆基纳微米复合陶瓷模具材料及其摩擦磨损特性研究[D]. 山东轻工业学院. 2009.[18] Herman S, Jaklic A, Herman S, et al. Hip stress reduction after Chiari osteotomy. Med Biol Eng Comput. 2002;40(4): 369-375.[19] Hipp JA, Sugano N, Millis MB, et al. Planning acetabular redirection osteotomies based on joint contact pressures. Clin Orthop Relat Res. 1999;(364): 134-143.[20] 李永奖,张力成,杨国敬,等.全髋关节置换术后假体脱位的有限元研究[J].中医正骨,2007,19(12): 66-68.[21] 樊继波,覃勇,李莎,等.骨质疏松症全髋关节有限元模型的建立与分析[J].中国骨质疏松杂志,2011, 17(11): 989-992.[22] 胡敏,王兵,赵宏斌,等.先天性髋关节脱臼的干预策略进展[J].中国临床康复, 2005,9(2):198-199.[23] Scholz R, Hoffmann F, von Sachsen S, et al. Validation of density-elasticity relationships for finite element modeling of human pelvic bone by modal analysis. J Biomech. 2013; 46(15): 2667-2673.[24] Zhao X, Chosa E, Yamako G, et al. Effect of acetabular reinforcement ring with hook for acetabular dysplasia clarified by three-dimensional finite element analysis. J Arthroplasty. 2013;28(10): 1765-1769.[25] Er MS, Verim O, Altinel L, et al. Three-dimensional finite element analysis used to compare six different methods of syndesmosis fixation with 3.5- or 4.5-mm titanium screws: a biomechanical study. J Am Podiatr Med Assoc. 2013;103(3):174-180.[26] Goffin JM, Pankaj P, Simpson AH. The importance of lag screw position for the stabilization of trochanteric fractures with a sliding hip screw: a subject-specific finite element study. J Orthop Res. 2013;31(4): 596-600.[27] 曹振华,闫金玉,银和平,等.数字及逆向工程技术在复杂骨科应用进展[J].中国组织工程研究, 2012,16(39): 7370-7374.[28] 陈宣煌,林海滨.数字化设计在脊柱疾病中的应用[J].中国组织工程研究, 2012, 16(22): 4159-4168.[29] Lerch M, Weigel N, Windhagen H, et al. Finite element model of a novel short stemmed total hip arthroplasty implant developed from cross sectional CT scans. Technol Health Care. 2013;21(5): 493-500.[30] Lam L, Drew T, Boscainos P. Effect of Acetabular Orientation on Stress Distribution of Highly Cross-linked Polyethylene Liners. Orthopedics. 2013;36(11): e1346-e1352.[31] 徐灵军,朱海波,张银网,等.人工髋关节活体有限元建模及力学分析[J].中国组织工程研究, 2012,16(26): 4770-4775.[32] 赵海波,龙腾河,杨伟江,等.CT和有限元数字化骨盆模型构建的研究和临床应用[J].中国组织工程研究, 2012, 16(39): 7327-7332.[33] 覃小东,符俏.人工髋关节假体的分类及设计[J].中国组织工程研究, 2012, 16(35): 6607-6614.[34] Chen DW, Lin CL, Hu CC, et al. Biomechanical consideration of total hip arthroplasty following failed fixation of femoral intertrochanteric fractures - a finite element analysis. Med Eng Phys. 2013;35(5): 569-575.[35] Elkins JM, Stroud NJ, Rudert MJ, et al. The capsule's contribution to total hip construct stability--a finite element analysis. J Orthop Res. 2011;29(11): 1642-1648.[36] Epasto G, Foti A, Guglielmino E, et al. Total hip arthroplasty by using a cementless ultrashort stem: a subject-specific finite element analysis for a young patient clinical case. Proc Inst Mech Eng H. 2013; 227(7): 757-766.[37] Munro JT, Anderson IA, Walker CG, et al. Finite element analysis of retroacetabular osteolytic defects following total hip replacement. J Biomech. 2013;46(14):2529-2533.[38] Britton JR, Walsh LA, Prendergast PJ. Mechanical simulation of muscle loading on the proximal femur: analysis of cemented femoral component migration with and without muscle loading. Clin Biomech (Bristol, Avon). 2003;18(7). 637-646.[39] Taylor ME, Tanner KE, Freeman MA, et al. Stress and strain distribution within the intact femur: compression or bending? Med Eng Phys. 1996;18(2): 122-131.[40] Phillips Andrew TM. Numerical modelling of the pelvis and acetabular construct following hip arthroplasty. PhD thesis, The University of Edinburgh, 2005.[41] 安明勋.人工髋关节假体的设计及界面应力分析[J].中国组织工程研究, 2012, 16(30): 5634-5638.[42] Gallo J, Goodman SB, Konttinen YT, et al. Osteolysis around total knee arthroplasty: a review of pathogenetic mechanisms. Acta Biomater. 2013;9(9): 8046-8058. |
| [1] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [2] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [3] | Zhang Chao, Lü Xin. Heterotopic ossification after acetabular fracture fixation: risk factors, prevention and treatment progress [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1434-1439. |
| [4] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Multiple problems in the selection of implants for patellar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1440-1445. |
| [5] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [6] | Xu Yulin, Shen Shi, Zhuo Naiqiang, Yang Huilin, Yang Chao, Li Yang, Zhao Heng, Zhao Lu. Biomechanical comparison of three different plate fixation methods for acetabular posterior column fractures in standing and sitting positions [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 826-830. |
| [7] | Cai Qunbin, Zou Xia, Hu Jiantao, Chen Xinmin, Zheng Liqin, Huang Peizhen, Lin Ziling, Jiang Ziwei. Relationship between tip-apex distance and stability of intertrochanteric femoral fractures with proximal femoral anti-rotation nail: a finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 831-836. |
| [8] | Song Chengjie, Chang Hengrui, Shi Mingxin, Meng Xianzhong. Research progress in biomechanical stability of lateral lumbar interbody fusion [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 923-928. |
| [9] | Liu Zhao, Xu Xilin, Shen Yiwei, Zhang Xiaofeng, Lü Hang, Zhao Jun, Wang Zhengchun, Liu Xuzhuo, Wang Haitao. Guiding role and prospect of staging and classification combined collapse prediction method for osteonecrosis of femoral head [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 929-934. |
| [10] | Xie Chongxin, Zhang Lei. Comparison of knee degeneration after anterior cruciate ligament reconstruction with or without remnant preservation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 735-740. |
| [11] | Nie Shaobo, Li Jiantao, Sun Jien, Zhao Zhe, Zhao Yanpeng, Zhang Licheng, Tang Peifu. Mechanical stability of medial support nail in treatment of severe osteoporotic intertrochanteric fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 329-333. |
| [12] | Tan Jiachang, Yuan Zhenchao, Wu Zhenjie, Liu Bin, Zhao Jinmin. Biomechanical analysis of elastic nail combined with end caps and wire fixation for long oblique femoral shaft fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 334-338. |
| [13] | Chen Lu, Zhang Jianguang, Deng Changgong, Yan Caiping, Zhang Wei, Zhang Yuan. Finite element analysis of locking screw assisted acetabular cup fixation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 356-361. |
| [14] | Fan Yinuo, Guan Zhiying, Li Weifeng, Chen Lixin, Wei Qiushi, He Wei, Chen Zhenqiu. Research status and development trend of bibliometrics and visualization analysis in the assessment of femoroacetabular impingement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 414-419. |
| [15] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Comparison of the advantages and disadvantages of multiple implants in treatment of traumatic dislocation of sternoclavicular joint [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 443-448. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||