Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (7): 1273-1280.doi: 10.3969/j.issn.2095-4344.2013.07.023
Previous Articles Next Articles
Ibandronate controls osteoprotegerin release from osteoblasts
Zhu Cai-yu1, Zheng Rong2, Wu Li-peng1, Li Ting2
- 1 Department of Orthodontics, Second Affiliated Hospital of Jiamusi University, Jiamusi 154002, Heilongjiang Province, China
2 Second Affiliated Hospital of Jiamusi University, Jiamusi 154002, Heilongjiang Province, China
-
Received:2012-09-12Revised:2013-01-17Online:2013-02-12Published:2013-03-21 -
Contact:Wu Li-peng, Professor, Department of Orthodontics, Second Affiliated Hospital of Jiamusi University, Jiamusi 154002, Heilongjiang Province, China wlpkq@sina.com -
About author:Zhu Cai-yu★, Studying for master’s degree, Department of Orthodontics, Second Affiliated Hospital of Jiamusi University, Jiamusi 154002, Heilongjiang Province, China ziyu_yu1988@163.com
CLC Number:
Cite this article
Zhu Cai-yu, Zheng Rong, Wu Li-peng, Li Ting. Ibandronate controls osteoprotegerin release from osteoblasts[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(7): 1273-1280.
share this article

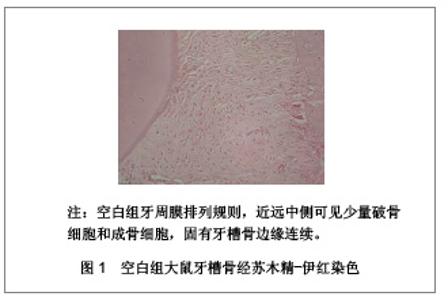
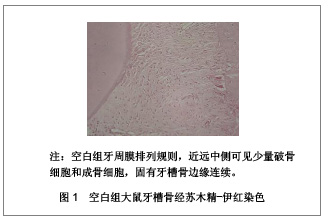
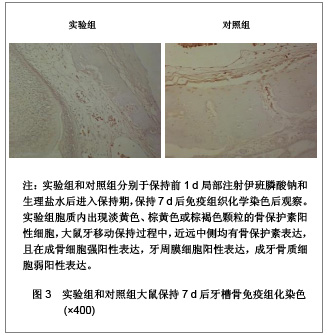
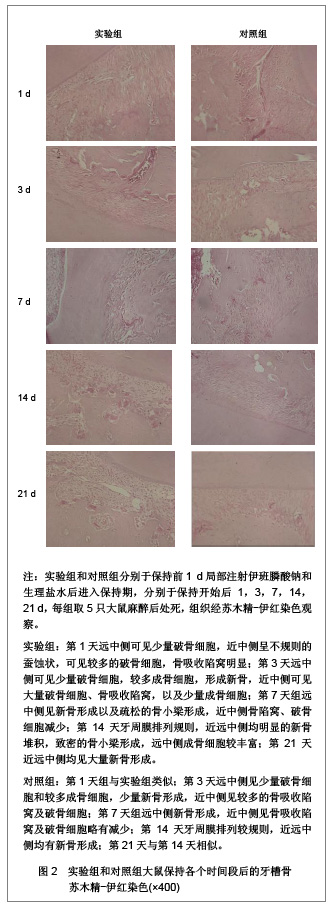
实验组和对照组大鼠牙槽骨经苏木精-伊红染色后的显微镜成像见图2。实验组:第1天远中侧可见少量破骨细胞,近中侧呈不规则的蚕蚀状,可见较多的破骨细胞,骨吸收陷窝明显;第3天远中侧可见少量破骨细胞,较多成骨细胞,形成新骨,近中侧可见大量破骨细胞、骨吸收陷窝,以及少量成骨细胞;第7天组远中侧见新骨形成以及疏松的骨小梁形成,近中侧骨陷窝、破骨细胞减少;第14天牙周膜排列规则,近远中侧均明显的新骨堆积,致密的骨小梁形成,远中侧成骨细胞较丰富;第21天近远中侧均见大量新骨形成。对照组:第1天组与实验组类似;第3天远中侧见少量破骨细胞和较多成骨细胞,少量新骨形成,近中侧见较多的骨吸收陷窝及破骨细胞;第7天组远中侧新骨形成,近中侧见骨吸收陷窝及破骨细胞略有减少;第14天牙周膜排列较规则,近远中侧均有新骨形成;第21天与第14天相似。"
| [1] 刘东刚,王杰军.双膦酸盐类药物的发展[J].中国肿瘤临床,2003, 30(9): 678-683.[2] Pivot X, Lortholary A, Abadie-Lacourtoisie S, et al. Renal safety of ibandronate 6 mg infused over 15 min versus 60 min in breast cancer patients with bone metastases: a randomized open-label equivalence trial. Breast. 2011; 20(6):510-514.[3] Walter C, Al-Nawas B, du Bois A, et al. Incidence of bisphosphonate-associated osteonecrosis of the jaws in breast cancer patients. Cancer. 2009;115(8):1631-1637.[4] Fischer RG, KlingeB. Clinical and histological evaluation of ligature-induced periodontitis in the domestic ferret. J Clin Periodontol. 1994;21(4):230-239.[5] King GJ, Keeling SD, McCoy EA, et al. Measuring dental drift and orthodontic tooth movement in response to various initial forces in adult rat. Am J Orthod Dentofacial Orthop. 1991; 99(5):456-465.[6] 段继强,王宸,张磊,等.骨折局部应用伊班膦酸钠最适剂量选择的动物实验研究[J].现代医学,2010,38(2):96-101.[7] 刘世颖,陈远萍,刘天悦,等.实验性正畸牙移动保持期动物模型的建立[J].中国实用口腔科杂志,2009,2(9):537-539.[8] 郑伟,汪宝军,叶立民.灰度值、光学密度值与免疫组化片阳性表达强弱的关系[J].临床与实验病理学杂志,2003,19(5):566-567.[9] 莫水学,陈扬熙.孕鼠正畸牙移动牙周组织DMP1表达变化的研究[J].广西医科大学学报,2010,27(06):826-828.[10] 王光,丁寅,潘峰,等.大鼠正畸牙移动中牙周组织内STRO-1动态变化的研究[J].口腔医学研究,2008,24(02):124-126.[11] 郭杰,赵青,陈扬熙.动情周期不同阶段正畸牙移动影响牙周组织胰岛素样生长因子表达的研究[J].华西口腔医学杂志,2008, 26(04):439-442.[12] 郭杰,赵青,陈扬熙,等.正畸牙移动对大鼠血清和局部牙周组织雌激素水平的影响[J].上海口腔医学,2007,16(06):618-622.[13] 孙应明.P物质缓释系统对正畸大鼠牙周破骨细胞数目的影响[J].中国美容医学,2007,16(02):153-156.[14] 孙应明,罗颂椒.免疫荧光法观察正畸大鼠牙周P物质神经纤维变化的研究[J].东南国防医药,2006,8(04):249-250,260.[15] 张晓东,林珠,李永明,等.大鼠牙齿移动牙周组织中Ⅰ型胶原和MMP-1及TIMP-1的表达[J].中国美容医学,2005,14(01):12-14.[16] 刘建林,林珠,李永明.局部注射VEGF对大鼠正畸牙齿移动的影响[J].中国美容医学,2004,13(03):272-274.[17] 李永明,罗颂椒.破骨细胞分化因子mRNA在大鼠正畸牙槽骨改建过程中的表达和分布[J].牙体牙髓牙周病学杂志,2004,14(05): 250-253.[18] 常少海,叶剑涛,刘东雄,等.碱性成纤维细胞生长因子在正畸大鼠牙周组织中的表达[J].新医学,2003,34(z1):77-79.[19] Soares PB, Fernandes Neto AJ, Magalhães D, et al. Effect of bone loss simulation and periodontal splinting on bone strain: Periodontal splints and bone strain. Arch Oral Biol. 2011;56 (11): 1373-1381.[20] Lossdörfer S, Abuduwali N, Jäger A. Bone morphogenetic protein-7 modifies the effects of insulin-like growth factors and intermittent parathyroid hormone (1-34) on human periodontal ligament cell physiology in vitro. J Periodontol. 2011;82(6): 900-908.[21] Dao V, Renjen R, Prasad HS, et al. Cementum, pulp, periodontal ligament, and bone response after direct injury with orthodontic anchorage screws: a histomorphologic study in an animal model. J Oral Maxillofac Surg. 2009;67(11): 2440-2445.[22] Murphy KG, Wilcko MT, Wilcko WM, et al. Periodontal accelerated osteogenic orthodontics: a description of the surgical technique. J Oral Maxillofac Surg. 2009;67(10): 2160-2166.[23] Cattaneo PM, Dalstra M, Melsen B. Strains in periodontal ligament and alveolar bone associated with orthodontic tooth movement analyzed by finite element. Orthod Craniofac Res. 2009;12(2):120-128.[24] Cornelis MA, Scheffler NR, Mahy P, et al. Modified miniplates for temporary skeletal anchorage in orthodontics: placement and removal surgeries. J Oral Maxillofac Surg. 2008;66(7): 1439-1445.[25] Sidiropoulou-Chatzigiannis S, Kourtidou M, Tsalikis L. The effect of osteoporosis on periodontal status, alveolar bone and orthodontic tooth movement. A literature review. J Int Acad Periodontol. 2007;9(3):77-84.[26] Bildt MM, Henneman S, Maltha JC, et al. CMT-3 inhibits orthodontic tooth displacement in the rat. Arch Oral Biol. 2007; 52(6):571-578.[27] Meikle MC. Remodeling the dentofacial skeleton: the biological basis of orthodontics and dentofacial orthopedics. J Dent Res. 2007;86(1):12-24.[28] Yoshimatsu M, Shibata Y, Kitaura H, et al. Experimental model of tooth movement by orthodontic force in mice and its application to tumor necrosis factor receptor-deficient mice. J Bone Miner Metab. 2006;24(1):20-27.[29] Risubut S, Teerakapong A, Vattraphodes T, et al. Effect of local delivery of alendronate on bone formation in bioactive glass grafting in rats. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;104(4):e11-16.[30] Russell RG, Xia Z, Dunford JE, et al. Bisphosphonates:an update on mechanisms of action and how these relate to clinical efficacy. Ann N Y Acad Sci. 2007;1117:209-257.[31] Xiong Y, Yang HJ, Feng J, et al. Effects of alendronate on the proliferation and osteogenic differentiation of MG-63 cells. J Int Med Res. 2009;37(2):407-416.[32] Kim HK, Kim JH, Abbas AA, et al. Alendronate enhances osteogenic differentiation of bone marrow stromal cells:a preliminary study. Clin Orthop Relat Res. 2009;467(12): 3121-3128.[33] Kwon BS, Wang S, Udagawa N, et al. TRI,a new member of the tumor necrosis factor receptor family, induces fibroblast proliferation and inhibits osteoclastogenesis and bone resorption. FASEB J. 1998;12(10):845-854.[34] Udagawa N, Takahashi N, Jimi E, Matsuzaki, et al. Osteoblasts/stromal cells stimulate osteoclast activation through expression of osteoclast differentiation factor RANKL but not macrophage colony-stimulating factor. Bone. 1999; 25(5):517-523. |
| [1] | Wu Zhilin, , He Qin, Wang Pingxi, Shi Xian, Yuan Song, Zhang Jun, Wang Hao . DYRK2: a novel therapeutic target for rheumatoid arthritis combined with osteoporosis based on East Asian and European populations [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1569-1579. |
| [2] | Zhang Haiwen, Zhang Xian, Xu Taichuan, Li Chao. Bibliometric and visual analysis of the research status and trends of senescence in osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1580-1591. |
| [3] | Chen Ju, Zheng Jinchang, Liang Zhen, Huang Chengshuo, Lin Hao, Zeng Li. Effect and mechanism of beta-caryophyllene in mice with osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1341-1347. |
| [4] | Wen Guangwei, Zhen Yinghao, Zheng Taikeng, Zhou Shuyi, Mo Guoye, Zhou Tengpeng, Li Haishan, Lai Yiyi. Effects and mechanisms of isoginkgetin on osteoclastogenesis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1348-1358. |
| [5] | Li Linzhen, Jiao Hongzhuo, Chen Weinan, Zhang Mingzhe, Wang Jianlong, Zhang Juntao. Effect of icariin-containing serum on lipopolysaccharide-induced inflammatory damage in human chondrocytes [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1368-1374. |
| [6] | Pan Hongfei, Zhuang Zhenbing, Xu Baiyun, Yang Zhangyang, Lin Kairui, Zhan Bingqing, Lan Jinghan, Gao Heng, Zhang Nanbo, Lin Jiayu. Inhibitory effects of different concentrations of auranofin on M1 macrophage function and its therapeutic potential in diabetic wound healing [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1390-1397. |
| [7] | Peng Zhiwei, Chen Lei, Tong Lei. Luteolin promotes wound healing in diabetic mice: roles and mechanisms [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1398-1406. |
| [8] | Lyu Xiaofan, Huang Yi, Ding Liucheng . Mitochondrial mechanism and intervention therapy in diabetic cystopathy [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1508-1515. |
| [9] | Cao Xinyan, Yu Zifu, Leng Xiaoxuan, Gao Shiai, Chen Jinhui, Liu Xihua. Effect of repetitive transcranial magnetic stimulation and transcranial direct current stimulation on motor function and gait in children with cerebral palsy: a network meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1539-1548. |
| [10] | Guo Ying, Tian Feng, Wang Chunfang. Potential drug targets for the treatment of rheumatoid arthritis: large sample analysis from European databases [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1549-1557. |
| [11] | Huang Jie, Zeng Hao, Wang Wenchi, Lyu Zhucheng, Cui Wei. Visualization analysis of literature on the effect of lipid metabolism on osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1558-1568. |
| [12] | Sun Yajie, Zhao Xinchen, Bo Shuangling. Spatiotemporal expression of bone morphologic protein 7 in mouse kidney development [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(5): 1156-1161. |
| [13] | Li Haojing, Wang Xin, Song Chenglin, Zhang Shengnan, Chen Yunxin. Therapeutic efficacy of extracorporeal shock wave therapy in the upper trapezius muscle area combined with exercise control training in patients with chronic non-specific neck pain [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(5): 1162-1170. |
| [14] | Liu Yu, Lei Senlin, Zhou Jintao, Liu Hui, Li Xianhui. Mechanisms by which aerobic and resistance exercises improve obesity-related cognitive impairment [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(5): 1171-1183. |
| [15] | Yu Huifen, Mo Licun, Cheng Leping. The position and role of 5-hydroxytryptamine in the repair of tissue injury [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(5): 1196-1206. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||