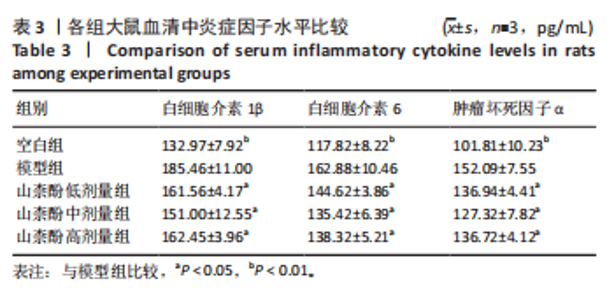
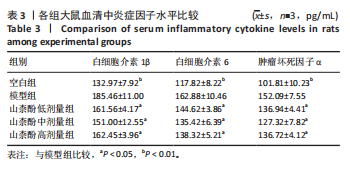
Chinese Journal of Tissue Engineering Research ›› 2026, Vol. 30 ›› Issue (29): 7529-7538.doi: 10.12307/2026.210
Previous Articles Next Articles
Mechanism by which kaempferol inhibits intervertebral disc degeneration in rats by regulating mitophagy levels
Wang Chenmoji1, Wu Yadong2, Gao Di1, Wang Hao1, Li Nianhu3
- 1First Clinical Medical College, Shandong University of Traditional Chinese Medicine, Jinan 250014, Shandong Province, China; 2Rizhao Traditional Chinese Medicine Hospital, Rizhao 276800, Shandong Province, China; 3Affiliated Hospital of Shandong University of Traditional Chinese Medicine, Jinan 250014, Shandong Province, China
-
Received:2025-06-07Revised:2025-09-15Online:2026-10-18Published:2026-03-03 -
Contact:Li Nianhu, PhD, Chief physician, Affiliated Hospital of Shandong University of Traditional Chinese Medicine, Jinan 250014, Shandong Province, China -
About author:Wang Chenmoji, MS, First Clinical Medical College, Shandong University of Traditional Chinese Medicine, Jinan 250014, Shandong Province, China -
Supported by:National Administration of Traditional Chinese Medicine - Department of Science and Technology Joint Research Program, No. GZY-KJS-SD-2023-042 (LNH); Shandong Provincial Natural Science Foundation Innovation and Development Joint Fund Program, No. ZR2021LZY006 (to WYD)
CLC Number:
Cite this article
Wang Chenmoji, Wu Yadong, Gao Di, Wang Hao, Li Nianhu. Mechanism by which kaempferol inhibits intervertebral disc degeneration in rats by regulating mitophagy levels[J]. Chinese Journal of Tissue Engineering Research, 2026, 30(29): 7529-7538.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
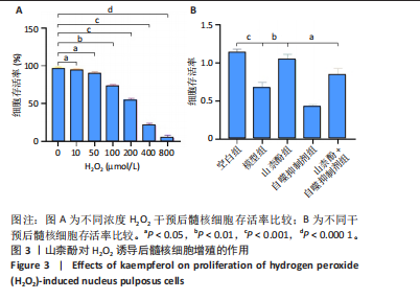
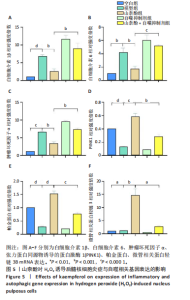
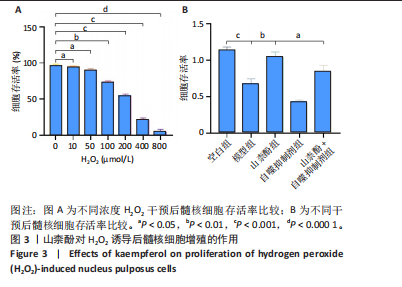
2.2 细胞实验结果 2.2.1 山柰酚对H2O2诱导后髓核细胞增殖的作用 CCK-8检测结果显示,随着H2O2浓度的升高(0-800 μmol/L 髓核细胞存活率降低,当H2O2浓度> 200 μmol/L时,髓核细胞存活率较对照组下降> 50%,见图3A,为避免细胞过度损伤,选取细胞存活率为55.32%的200 μmol/L H2O2建立髓核细胞氧化应激模型。 CCK-8检测结果显示,模型组髓核细胞存活率低于空白组、山柰酚组(P < 0.001,P < 0.01),山柰酚+自噬抑制剂组髓核细胞存活率低于山柰酚组(P < 0.05),见图3B。 2.2.2 山柰酚对H2O2诱导后髓核细胞炎症与自噬相关蛋白表达的影响 Western blot检测结果显示,与空白组比较,模型组髓核细胞内白细胞介素1β、白细胞介素6、肿瘤坏死因子α、微管相关蛋白轻链3Ⅱ/Ⅰ蛋白表达升高(P < 0.05,"
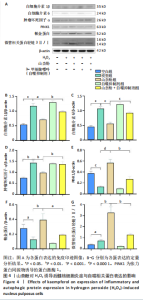
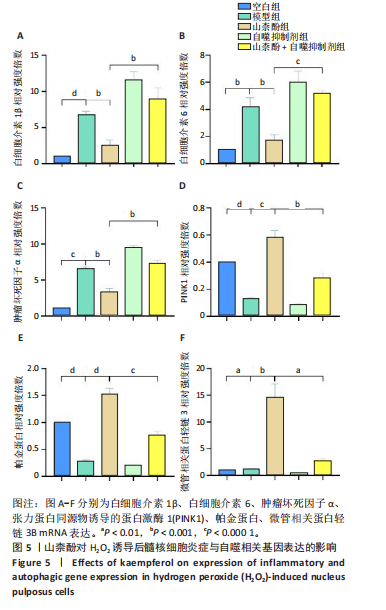
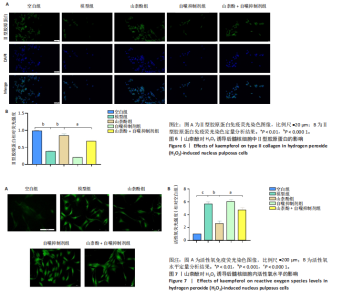
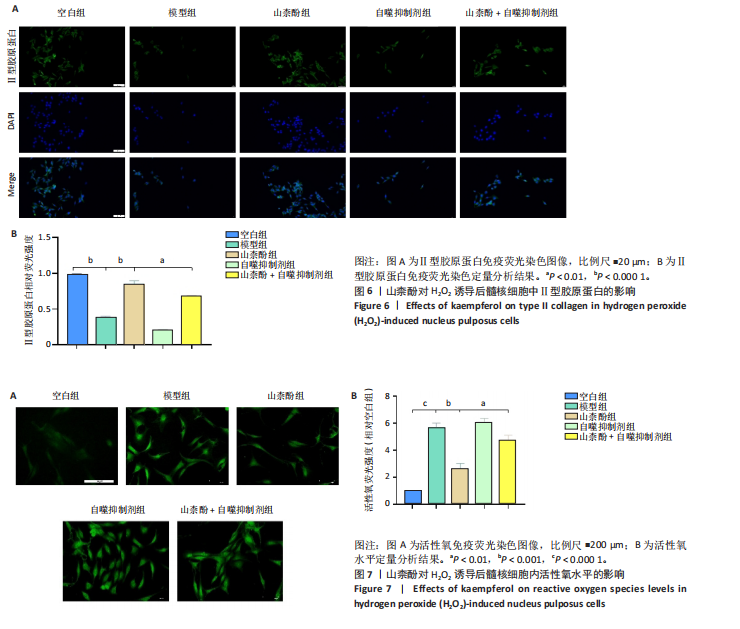
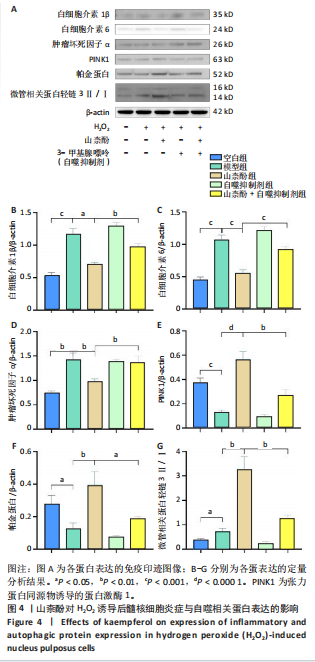
P < 0.01,P < 0.001),PINK1、帕金蛋白的蛋白表达降低(P < 0.001,P < 0.05);与模型组比较,山柰酚组内白细胞介素1β、白细胞介素6、肿瘤坏死因子α蛋白表达降低(P < 0.01,P < 0.001),微管相关蛋白轻链3Ⅱ/Ⅰ、帕金蛋白、PINK1蛋白表达升高(P < 0.01,P < 0.000 1);与山柰酚组比较,山柰酚+自噬抑制剂组髓核细胞内白细胞介素1β、白细胞介素6、肿瘤坏死因子α蛋白表达升高(P < 0.01,P < 0.001),微管相关蛋白轻链3Ⅱ/Ⅰ、帕金蛋白、PINK1蛋白表达降低(P < 0.05,P < 0.01),见图4。结果表明,在椎间盘退变过程中自噬作用可能被激活,但激活程度有限,而山柰酚可明显提高髓核细胞的自噬水平。 2.2.3 山柰酚对H2O2诱导后髓核细胞炎症与自噬相关基因表达的影响 RT-qPCR检测结果显示,与空白组比较,模型组髓核细胞内白细胞介素1β、白细胞介素6、肿瘤坏死因子α、微管相关蛋白轻链3B mRNA表达升高(P < 0.01,P < 0.000 1),帕金蛋白、PINK1 mRNA表达降低(P < 0.000 1);与模型组比较,山柰酚组髓核细胞内白细胞介素1β、白细胞介素6、肿瘤坏死因子α mRNA表达降低(P < 0.01,P < 0.001),微管相关蛋白轻链3B、帕金蛋白、PINK1 mRNA表达升高(P < 0.001,P < 0.000 1);与山柰酚组比较,山柰酚+自噬抑制剂组髓核细胞内白细胞介素1β、白细胞介素6、肿瘤坏死因子α mRNA表达升高(P < 0.01,P < 0.001),微管相关蛋白轻链3B、帕金蛋白、PINK1 mRNA表达降低(P < 0.01,P < 0.001),见图5。结果表明,氧化应激损伤抑制了线粒体自噬核心通路的活性,导致受损线粒体累积,而山柰酚可能通过激活PINK1/帕金蛋白信号轴促进受损线粒体的选择性清除,恢复线粒体稳态,同时增强自噬通量强化了线粒体质量控制能力。 2.2.4 山柰酚对H2O2诱导后髓核细胞中Ⅱ型胶原蛋白的影响 免疫荧光染色结果显示,模型组髓核细胞内Ⅱ型胶原蛋白表达低于空白组、山柰酚组(P < 0.000 1),山柰酚+自噬抑制剂组髓核细胞内Ⅱ型胶原蛋白表达低于山柰酚组(P < 0.01),见图6。结果表明,山柰酚可能通过增加Ⅱ型胶原蛋白表达间接保护髓核细胞外基质稳态。"
| [1] XU J, SHAO T, LOU J, et al. Aging, cell senescence, the pathogenesis and targeted therapies of intervertebral disc degeneration. Front Pharmacol. 2023;14:1172920. [2] CAO G, YANG S, CAO J, et al. The role of oxidative stress in intervertebral disc degeneration. Oxid Med Cell Longev. 2022;2022:2166817. [3] KAMALI A, ZIADLOU R, LANG G, et al. Small molecule-based treatment approaches for intervertebral disc degeneration: Current options and future directions. Theranostics. 2021;11(1):27-47. [4] MOHD ISA IL, TEOH SL, MOHD NOR NH, et al. Discogenic low back pain: Anatomy, pathophysiology and treatments of intervertebral disc degeneration. Int J Mol Sci. 2022;24(1):208. [5] WANG N, CHEN S, ZHANG X, et al. Global research status and hot trends in stem cells therapy for intervertebral disc degeneration: A bibliometric and clinical study analysis. Front Pharmacol. 2022;13:873177. [6] WANG M, WANG H, WANG X, et al. Identification of cellular senescence-related genes and immune cell infiltration characteristics in intervertebral disc degeneration. Front Immunol. 2024;15:1439976. [7] CHAO-YANG G, PENG C, HAI-HONG Z. Roles of NLRP3 inflammasome in intervertebral disc degeneration. Osteoarthritis Cartilage. 2021; 29(6):793-801. [8] SONG Q, ZHANG F, WANG K, et al. MiR-874-3p plays a protective role in intervertebral disc degeneration by suppressing MMP2 and MMP3. Eur J Pharmacol. 2021;895:173891. [9] SONG Y, LU S, GENG W, et al. Mitochondrial quality control in intervertebral disc degeneration. Exp Mol Med. 2021;53(7):1124-1133. [10] MARCHEV AS, DIMITROVA PA, BURNS AJ, et al. Oxidative stress and chronic inflammation in osteoarthritis: Can NRF2 counteract these partners in crime? Ann N Y Acad Sci. 2017;1401(1):114-135. [11] 刘学睿,李兴勇,唐兆鹏,等.中药复方调控氧化应激防治骨关节炎研究进展[J].中国骨质疏松杂志,2024,30(12):1820-1825. [12] LUO X, HUAN L, LIN F, et al. Ulinastatin ameliorates IL-1β-induced cell dysfunction in human nucleus pulposus cells via Nrf2/NF-κB pathway. Oxid Med Cell Longev. 2021:5558687. doi:10.1155/2021/5558687. [13] ZOU L, LEI H, SHEN J, et al. HO-1 induced autophagy protects against IL-1 β-mediated apoptosis in human nucleus pulposus cells by inhibiting NF-κB. Aging (Albany NY). 2020;12(3):2440-2452. [14] BRILLO V, CHIEREGATO L, LEANZA L, et al. Mitochondrial dynamics, ROS, and cell signaling: A blended overview. Life (Basel). 2021;11(4):332. [15] NAPOLITANO G, FASCIOLO G, VENDITTI P. Mitochondrial management of reactive oxygen species. Antioxidants (Basel). 2021;10(11):1824. [16] ONISHI M, YAMANO K, SATO M, et al. Molecular mechanisms and physiological functions of mitophagy. EMBO J. 2021;40(3):e104705. [17] BANGAR SP, CHAUDHARY V, SHARMA N, et al. Kaempferol: A flavonoid with wider biological activities and its applications. Crit Rev Food Sci Nutr. 2023;63(28):9580-9604. [18] 汪陈莫及,吴亚东,梁松林,等.基于p38 MAPK信号通路探讨山柰酚对椎间盘退变的作用机制[J].中国中药杂志,2024,49(21): 5721-5729. [19] HOSSEINI A, ALIPOUR A, BARADARAN RAHIMI V, et al. A comprehensive and mechanistic review on protective effects of kaempferol against natural and chemical toxins: Role of NF-κB inhibition and Nrf2 activation. Biofactors. 2023;49(2):322-350. [20] ALRUMAIHI F, ALMATROODI SA, ALHARBI HOA, et al. Pharmacological potential of kaempferol, a flavonoid in the management of pathogenesis via modulation of inflammation and other biological activities. Molecules. 2024;29(9):2007. [21] 崔力扬,刘尚礼,丁悦,等.大鼠腰椎间盘针刺退变模型的建立[J].中国矫形外科杂志,2007,15(13):1008-1011. [22] 王新立,刘汝银,王西彬,等.牛膝总皂苷对大鼠椎间盘髓核细胞外基质合成的影响[J].中成药,2020,42(1):69-74. [23] LIN J, ZHENG X, ZHANG Z, et al. Inhibition of LRRK2 restores parkin-mediated mitophagy and attenuates intervertebral disc degeneration. Osteoarthritis Cartilage. 2021;29(4):579-591. [24] LI S, DU J, HUANG Y, et al. From hyperglycemia to intervertebral disc damage: Exploring diabetic-induced disc degeneration. Front Immunol. 2024;15:1355503. [25] LI F, SUN X, WANG Y, et al. Development and validation of a novel nomogram to predict the risk of intervertebral disc degeneration. Mediators Inflamm. 2022:3665934. doi: 10.1155/2022/3665934. [26] CHO PG, YOON SJ, SHIN DA, et al. Finite element analysis of stress distribution and range of motion in discogenic back pain. Neurospine. 2024;21(2):536-543. [27] KAWARAI Y, JANG SH, LEE S, et al. Exercise attenuates low back pain and alters epigenetic regulation in intervertebral discs in a mouse model. Spine J. 2021;21(11):1938-1949. [28] SHU D, DAI S, WANG J, et al. Impact of running exercise on intervertebral disc: A systematic review. Sports Health. 2024;16(6): 958-970. [29] 朱少兵,张龙君,陈建良,等.腰痛病因病机述略[J].浙江中医杂志, 2012,47(7):502-503. [30] 韩涛,于杰,金哲峰,等.中药干预椎间盘退变治疗腰椎间盘突出症作用机制研究进展[J].世界中医药,2023,18(21):3042-3046. [31] 陈祁青,马东,赵继荣,等.基于网络药理学及动物实验的杜仲腰痛丸治疗腰椎间盘突出症慢性下肢痛的作用研究[J].世界科学技术-中医药现代化,2023,25(5):1702-1713. [32] 赵赫.补肾壮筋汤颗粒对腰椎间盘退变大鼠影响的实验研究[D]. 北京:北京中医药大学,2018. [33] 朱立国,张平,宋庆慧,等.补肾活血方对沙鼠增龄过程中腰椎软骨终板钙化干预作用的初步研究[J].中国骨伤,2017,30(10):926-932. [34] HERB M, SCHRAMM M. Functions of ROS in macrophages and antimicrobial immunity. Antioxidants (Basel). 2021;10(2):313. [35] KUZNETSOV AV, MARGREITER R, AUSSERLECHNER MJ, et al. The complex interplay between mitochondria, ROS and entire cellular metabolism. Antioxid. (Basel Switz.). 2022;11(10):1995. [36] HWANG HJ, KIM YK. The role of LC3B in autophagy as an RNA-binding protein. Autophagy. 2023;19(3):1028-1030. [37] WHITEN DR, COX D, SUE CM. PINK1 signalling in neurodegenerative disease. Essays Biochem. 2021;65(7):913-923. [38] TSENG MC, LIM J, CHU YC, et al. Dynamic pressure stimulation upregulates collagen II and aggrecan in nucleus pulposus cells through calcium signaling. Spine (Phila Pa 1976). 2022;47(15):1111-1119. [39] GAO T, ZHAO H, WANG L, et al. Preparation and characterisation of kaempferol composite carrier solid dispersion: evaluation of its application in preventing soybean oil spoilage. Nat Prod Res. 2024:1-8. doi:10.1080/14786419.2024.2338811. [40] CHENG H, GUO Q, ZHAO H, et al. An injectable hydrogel scaffold loaded with dual-drug/sustained-release PLGA microspheres for the regulation of macrophage polarization in the treatment of intervertebral disc degeneration.Int J Mol Sci. 2022;24(1):390. [41] SUN Y, GUO F, PENG X, et al. Metabolism of phenolics of tetrastigma hemsleyanum roots under in vitro digestion and colonic fermentation as well as their in vivo antioxidant activity in rats. Foods. 2021;10(9):2123. |
| [1] | Zhu Xiaolong, Zhang Wei, Yang Yang. Visualization analysis of research hotspots and cutting-edge information in the field of intervertebral disc regeneration and repair [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2391-2402. |
| [2] | Yang Xuetao, Zhu Menghan, Zhang Chenxi, Sun Yimin, Ye Ling. Applications and limitations of antioxidant nanomaterials in oral cavity [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2044-2053. |
| [3] |
Dong Chunyang, Zhou Tianen, Mo Mengxue, Lyu Wenquan, Gao Ming, Zhu Ruikai, Gao Zhiwei.
Action mechanism of metformin combined with Eomecon chionantha Hance dressing in treatment of deep second-degree burn wounds#br#
#br#
[J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2001-2013.
|
| [4] | Liu Anting, Lu Jiangtao, Zhang Wenjie, He Ling, Tang Zongsheng, Chen Xiaoling. Regulation of AMP-activated protein kinase by platelet lysate inhibits cadmium-induced neuronal apoptosis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(7): 1800-1807. |
| [5] | Cai Ziming, Yu Qinghe, Ma Pengfei, Zhang Xin, Zhou Longqian, Zhang Chongyang, Lin Wenping. Heme oxygenase-1 alleviates lipopolysaccharide-induced inflammatory response in nucleus pulposus mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(7): 1624-1631. |
| [6] | Yang Xiao, Bai Yuehui, Zhao Tiantian, Wang Donghao, Zhao Chen, Yuan Shuo. Cartilage degeneration in temporomandibular joint osteoarthritis: mechanisms and regenerative challenges [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(4): 926-935. |
| [7] | Wang Peng, Li Zhijun, Zhang Shaojie, Wu Yimin. Intervertebral disc rehydration after posterior lumbar dynamic internal fixation [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(3): 711-720. |
| [8] | Zhang Zhilong, Wang Haiying, Ma Fenghua, Hou Yanjie. Regulating mitochondrial dynamics balance in nucleus pulposus cells inhibits cell apoptosis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(29): 7520-7528. |
| [9] | Du Yaxin, Zhao Xiaojuan, Wu Ruixia, Dong Yizhi, Song Xinyue, Fu Hongyang, She Yitong, Zhang Jialin, Zhu Yong. Interaction between vascular-lymphatic system imbalance and immune microenvironment in intervertebral disc degeneration [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(29): 7612-7618. |
| [10] | He Long, Gao Shuang, Chen Chao, Qin Guozhong, Ran Qingsen, Wang Zhengchun, Yang Yafeng, Ren Hang, Qiu Yunkai, Yang Yang, Li Wei. A new strategy for preventing and treating orthopedic diseases by regulating ferroptosis through signaling pathways [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(29): 7619-7631. |
| [11] | Yong Qiao, Sun Xin, Wang Guoyou, Zhang Lei, Shen Huarui, Liu Huan, Guan Taiyuan. Shaoyang Shenggu Fang inhibits oxidative stress and delays cartilage aging in rats with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(28): 7251-7259. |
| [12] | You Chenyang, Jiang Chao, Che Yanjun. Synergistic imbalance in lumbar core muscles and novel targeted interventions for intervertebral disc degeneration [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(28): 7323-7331. |
| [13] | Guo Jun, Lu Zheng, Yu Jinling, Hao Yuanyuan, Liu Kaishun, Liu Xuexia, Huang Yourong. Oxidative stress and osteoporosis: a bibliometric analysis of literature from SCI core database [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(28): 7428-7436. |
| [14] | Yuan Min, Han Yu, Liu Jinhong, Zhang Jingyu, Cao Jimin, Sun Teng . Role and mechanism of ABL1 in myocardial necroptosis and cardiac ischemia/reperfusion injury [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(24): 6247-6258. |
| [15] | Zhang Xiaoxu, Tian Zhenli, Xie Tingting. Roles of pregnane X receptor in sodium arsenite-induced oxidative stress and inflammatory injury in human normal hepatocytes [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(24): 6259-6266. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||