Chinese Journal of Tissue Engineering Research ›› 2026, Vol. 30 ›› Issue (28): 7475-7484.doi: 10.12307/2026.818
Previous Articles Next Articles
Meta-analysis of robot-assisted walking training on lower limb motor function improvement in Parkinson's disease patients#br#
Ren Yi1, Wang Qing1, Yu Shaohong2, Qiu Zhengang1
- 1School of Rehabilitation Medicine, Shandong University of Traditional Chinese Medicine, Jinan 250355, Shandong Province, China; 2Second Affiliated Hospital of Shandong University of Traditional Chinese Medicine, Jinan 250001, Shandong Province, China
-
Received:2025-09-25Revised:2025-12-13Online:2026-10-08Published:2026-02-27 -
Contact:Qiu Zhengang, PhD, Associate professor, School of Rehabilitation Medicine, Shandong University of Traditional Chinese Medicine, Jinan 250355, Shandong Province, China -
About author:Ren Yi, MS candidate, School of Rehabilitation Medicine, Shandong University of Traditional Chinese Medicine, Jinan 250355, Shandong Province, China -
Supported by:Shandong Provincial Natural Science Foundation, No. ZR2024MH048 (to YSH); 2025 Postgraduate Quality Improvement and Innovation Project of Shandong University of Traditional Chinese Medicine, No. YJSTZCX2025077 (to RY)
CLC Number:
Cite this article
Ren Yi, Wang Qing, Yu Shaohong, Qiu Zhengang. Meta-analysis of robot-assisted walking training on lower limb motor function improvement in Parkinson's disease patients#br#[J]. Chinese Journal of Tissue Engineering Research, 2026, 30(28): 7475-7484.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
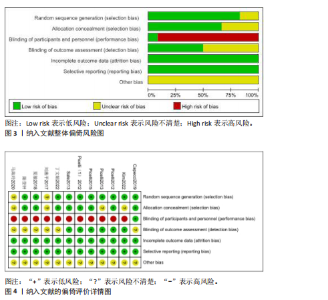

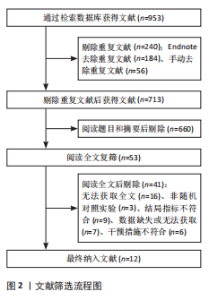
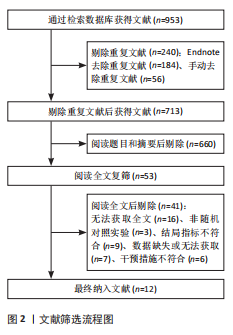
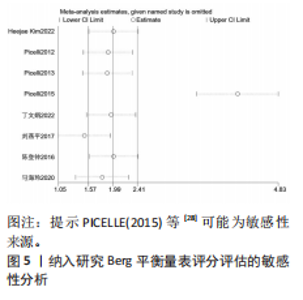
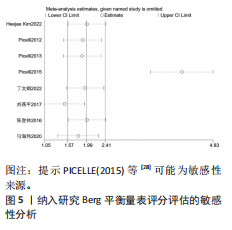
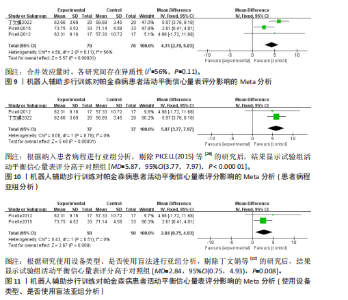
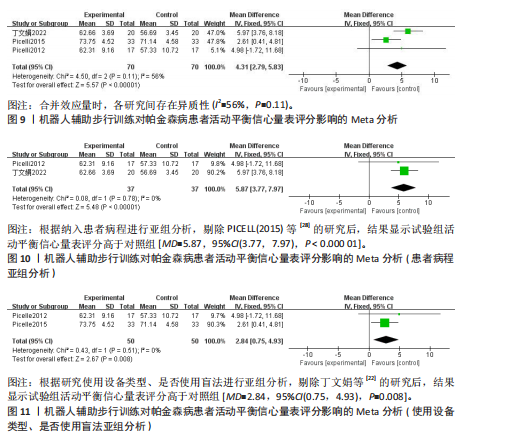
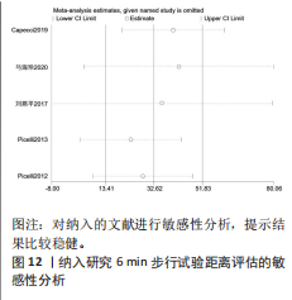
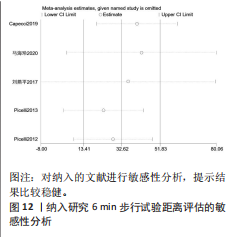
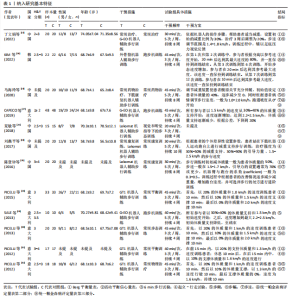
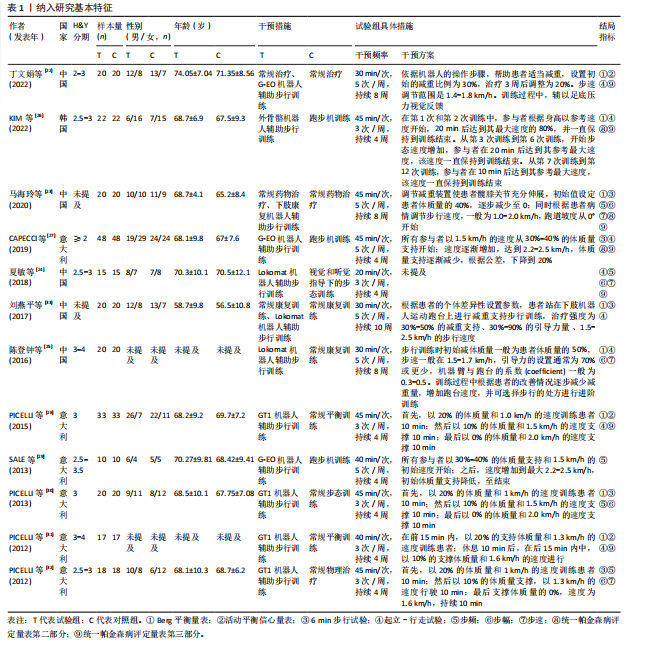
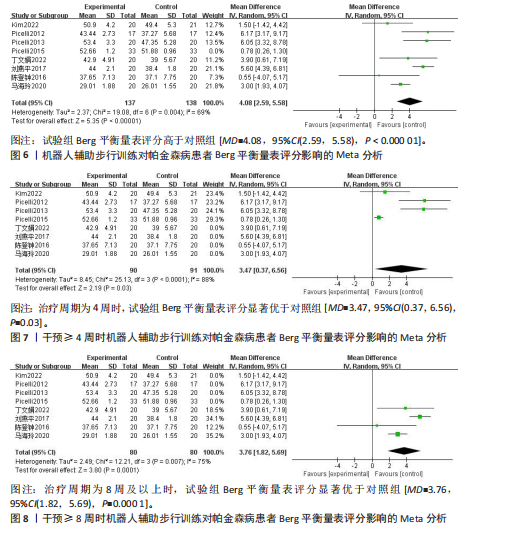
2.2 纳入文献基本特征 根据纳入标准和排除标准,共纳入12篇文献,涉及526例患者,其中试验组和对照组各263例。纳入文献的发表时间为2012-2022年,研究国家包括中国、韩国和意大利,干预周期集中在4-10周。纳入文献基本特征见表1。 2.3 纳入文献方法学质量评价 共纳入12篇研究。10项研究均报告了随机序列的产生方法(低风险)[22,24-32],2项研究仅提到随机分组(风险不清楚)[23,33];8项研究提及分配隐藏(低风 险)[22,24-26,28-29,31-32],4项研究未提及分配隐藏(风险不清楚)[23,27,30,33];1项研究对受试者施盲(低风险)[27],因干预措施的特殊性,故其余研究均判定为高风险;6项研究对评估者施盲(低风险)[26,28-32],其余6项研究均未提及是否对评估者施盲(风险不清楚)[22-25,27,33];所有研究均结果完整和无选择性报告(低风险)。纳入文献整体偏倚风险图,见图3,纳入文献偏倚评价详情图,见图4。 2.4 Meta分析结果 2.4.1 对帕金森病患者平衡功能的影响 (1)Berg平衡量表:8项研究报告了Berg平衡量表[22-23,25-26,28,30-31,33],共341例患者(试验组170例,对照组171例)。合并效应量时,异质性检验表明各研究间异质性较大(I2=91%,P < 0.000 01),对纳入的文献进行敏感性分析,提示PICELL(2015)等[28]可能为敏感性来源,见图5。剔除PICELL(2015)等[28]后,异质性降低为I2=69%,但I2 > 50%,故采用随机效应模型进行分析。结果显示,试验组Berg平衡量表评分高于对照组,具有统计学意义[MD=4.08,95%CI(2.59,5.58),P < 0.000 01],见图6。作者推测异质性可能与干预时间有关,纳入研究中干预时间大部分集中于4周,故根据干预时间进行亚组分析,结果显示异质性仍较高,因此,仅对结果进行描述性分析。亚组分析结果显示,治疗周期为4周时[26,28,30-31],试验组Berg平衡量表评分显著优于对照组,具有统计学意义[MD=3.47,95%CI(0.37,6.56),P=0.03],见图7。治疗周期为8周及以上时[22-23,25,33],试验组Berg平衡量表评分显著优于对照组,具有统计学意义[MD=3.76,95%CI(1.82,5.69),P=0.000 1],见图8。以上结果提示干预时间8周及以上机器人辅助步行训练改善帕金森病患者的Berg平衡量表评分结果更明显。 (2)活动平衡信心量表:3项研究采用活动平衡信心量表评估患者的平衡信心[22,28,31],共140例患者(试验组70例,对照组70例)。合并效应量时,各研究间存在异质性(I2=56%,P=0.11),见图9。根据纳入患者病程进行亚组分析,剔除PICELL(2015)等[28]的研究后,异质性消失(I2=0%),采用固定效应模型进行分析,结果显示试验组活动平衡信心量表评分高于对照组,具有统计学意义[MD=5.87,95%CI (3.77,7.97),P < 0.000 01],见图10。根据研究使用设备类型、是否使用盲法进行亚组分析,剔除丁文娟等[22]的研究后,异质性消失(I2=0%),采用固定效应模型进行分析,结果显示试验组活动平衡信心量表评分高于对照组,具有统计学意义[MD=2.84,95%CI(0.75,4.93),P=0.008],见图11。 2.4.2 对帕金森病患者步行能力的影响 (1)6 min步行试验:5项研究报告了6 min步行试验距离的变化[23,27,30,32-33],共252例患"
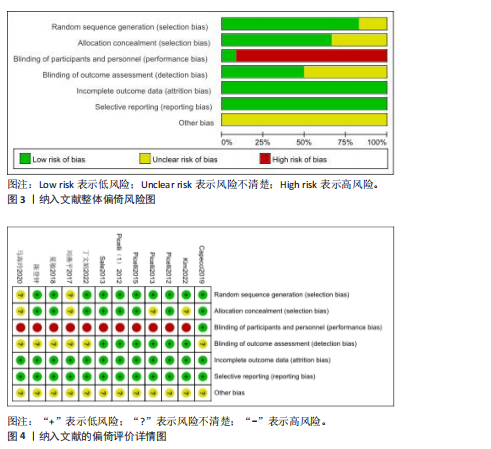
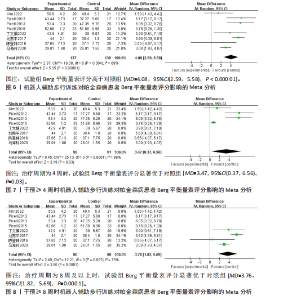
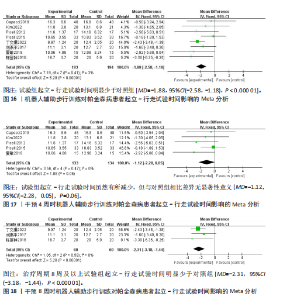
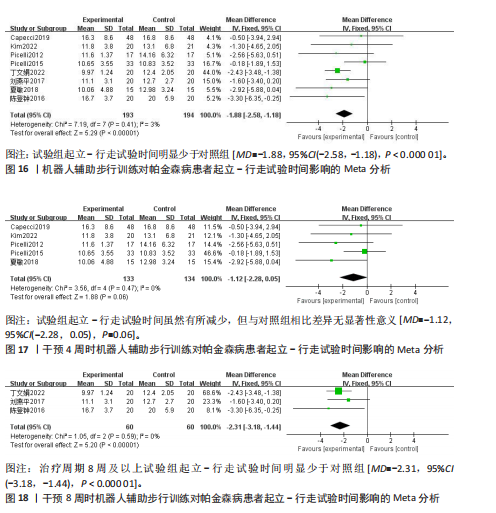
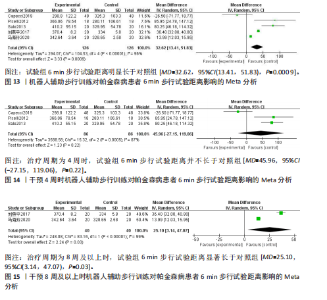
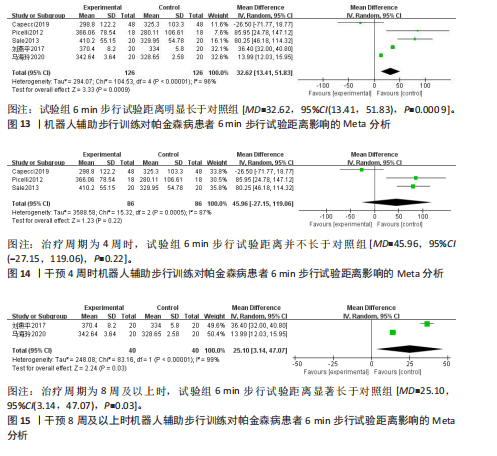
者(试验组和对照组各126例)。合并效应量时,各研究存在重度异质性(I2=96%,P < 0.000 01),对纳入的文献进行敏感性分析,提示结果比较稳健,见图12。逐一剔除单项研究进行敏感性分析,未发现明显的异质性降低,故采用随机效应模型进行分析。结果显示,试验组6 min步行试验距离明显高于对照组,具有统计学意义[MD=32.62,95%CI(13.41,51.83),P=0.000 9],见图13。为探究异质性来源,根据干预时间进行亚组分析,结果显示异质性仍较高,因此,仅对结果进行描述性分析。亚组分析结果显示,治疗周期为4周时[27,30,32],试验组6 min步行试验距离并不高于对照组[MD=45.96,95%CI(-27.15,119.06),P=0.22],见图14。治疗周期为8周及以上时[23,33],试验组6 min步行试验距离显著高于对照组,具有统计学意义[MD=25.10,95%CI(3.14,47.07),P=0.03],见图15。以上结果提示机器人辅助步行训练改善帕金森病患者的6 min步行试验距离与干预时间有关。 (2)起立-行走试验:8项研究均报告了起立-行走试验[22,24-28,32-33],共387例患者(试验组193例,对照组194例)。合并效应量时,各研究间具又较好的同质性(I2=3%,P=0.41),故采用固定效应模型进行分析。结果显示,试验组起立-行走试验时间明显少于对照组,具有统计学意义[MD=-1.88,95%CI(-2.58,-1.18),P < 0.000 01],见图16。根据干预时间进行亚组分析,结果显示,研究治疗周期为4周的试验组起立-行走试验时间虽然有所减少[24,26-28,31],但与对照组相比差异无显著性意义[MD=-1.12,95%CI(-2.28,0.05),P=0.06],见图17。治疗周期8周及以上试验组起立-行走试验明显少于对照组[22,25,33],且具有统计学意义[MD=-2.31,95%CI(-3.18,-1.44),P < 0.000 01],见图18。以上结果提示机器人辅助步行训练改善帕金森病患者的起立-行走试验与干预时间有关。 2.4.3 对帕金森病患者步态参数的影响 (1)步频:5项研究分析机器人辅助步行训练对步态参数中步频的影响[23-24,29-30,32],共166例患者(试验组83例,对照组83例)。合并效应量时,各研究间不存在异质性(I2=0%),故采用固定效应模型分析。结果显示试验组步频明显高于对照组,具有统计学意义[MD=2.98,"
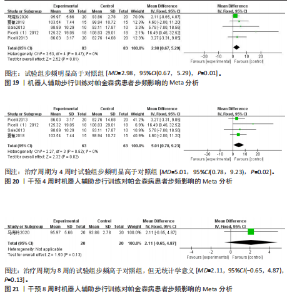
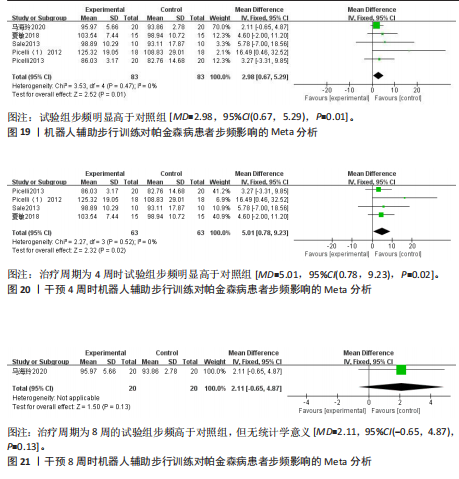
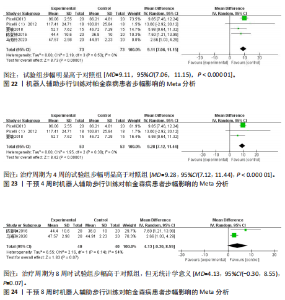
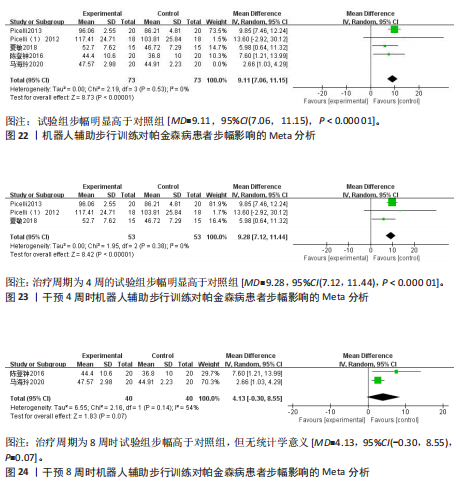
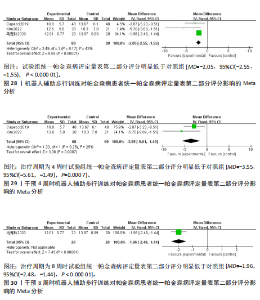
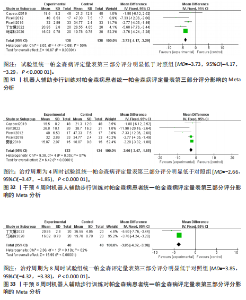
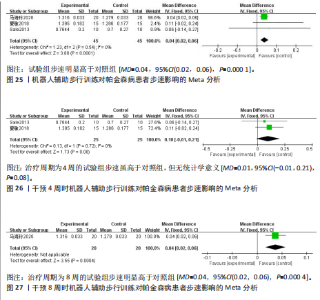
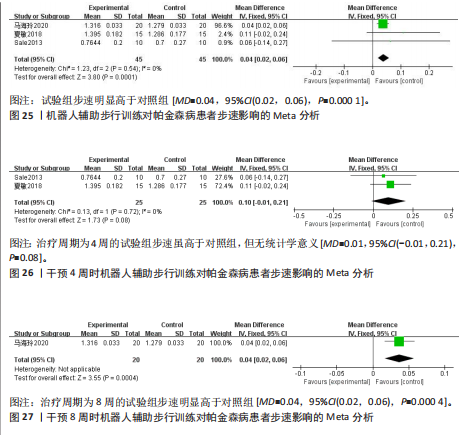
95%CI(0.67,5.29),P=0.01],见图19。根据干预时间进行亚组分析,亚组分析结果显示,治疗周期为4周时试验组步频明显高于对照组[24,29-32],且具有统计学意义[MD=5.01,95%CI(0.78,9.23),P=0.02],见图20。治疗周期为8周时试验组步频高于对照组[23],但无统计学意义[MD=2.11,95%CI(-0.65,4.87),P=0.13]。以上结果提示机器人辅助步行训练改善帕金森病患者的步频干预4周时效果最佳,见图21。 (2)步幅:5项研究分析机器人辅助步行训练对步幅的影响[23-25,30,32],共186例患者。合并效应量时,各研究间的异质性较高(I2=84%),逐一剔除单项研究进行敏感性分析,剔除马海玲等[23]的研究后,各研究间不存在异质性(I2=0%),故采用固定效应模型。试验组步幅明显高于对照组,具有统计学意义[MD=9.11,95%CI(7.06,11.15),P < 0.000 01],见图22。根据干预时间进行亚组分析,亚组分析结果显示,治疗周期为4周时试验组步幅明显高于对照组[24,30,32],且具有统计学意义[MD=9.28,95%CI(7.12,11.44),P < 0.000 01],见图23。治疗周期为8周时试验组步幅高于对照组[23,25],但无统计学意义[MD=4.13,95%CI(-0.30,8.55),P=0.07],见图24。以上结果提示机器人辅助步行训练改善帕金森病患者的步幅在干预4周时效果最佳。 (3)步速:3项研究分析机器人辅助步行训练对步速的影响[23-24,29],共90例患者。合并效应量时,各研究间具有较好的同质性(I2=0%),故采用固定模型分析。结果显示试验组步速明显高于对照组,具有统计学意义[MD=0.04,95%CI(0.02,0.06),P=0.000 1],见图25。根据干预时间进行亚组分析,亚组分析结果显示,治疗周期为4周时试验组步速虽高于对照组,且不具有统计学意义[MD=0.01,95%CI(-0.01,0.21),P=0.08],见图26。治疗周期为8周时试验组步速明显高于对照组,具有统计学意义[MD=0.04,95%CI(0.02,0.06),P=0.000 4],见图27。以上结果提示机器人辅助步行训练改善帕金森病患者的步速与干预时间有关。 2.4.4 对帕金森病患者下肢运动功能的影响 (1)统一帕金森病评定量表第二部分:机器人辅助步态训练对帕金森病患者统一帕金森病"
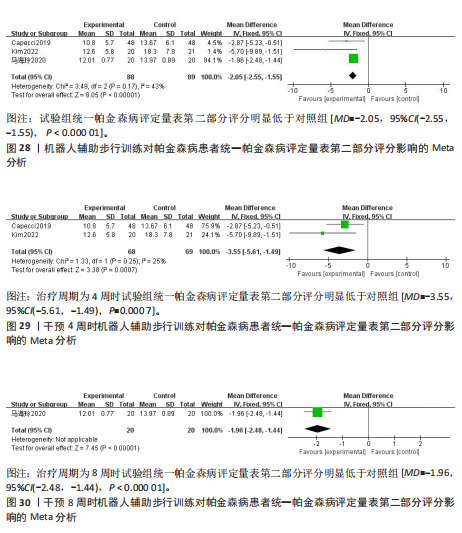
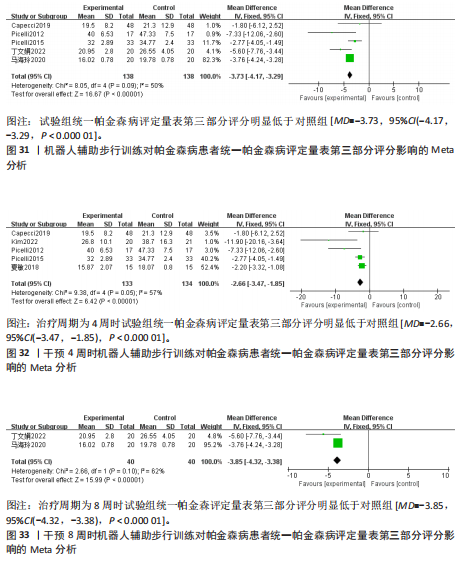
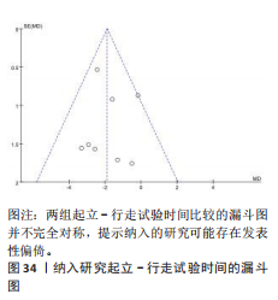
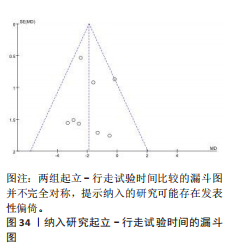
评定量表第二部分评分的影响:3项研究采用统一帕金森病评定量表第二部分评估帕金森病患者的日常生活运动功能[23,26-27],共177例患者。合并效应量时,各研究间的异质性(I2=43%)在可接受范围内,故采用固定效应模型进行分析。结果显示,试验组统一帕金森病评定量表第二部分评分明显低于对照组,具有统计学意义[MD=-2.05,95%CI(-2.55,-1.55), P < 0.000 01],见图28。根据干预时间进行亚组分析,亚组分析结果显示,治疗周期为4周[MD=-3.55,95%CI (-5.61,-1.49),P=0.000 7]与8周[MD=-1.96,95%CI(-2.48,-1.44),P < 0.000 01]的试验组统一帕金森病评定量表第二部分评分明显低于对照组,且均具有统计学意义,见图29,30。以上结果提示干预4周时机器人辅助步行训练改善统一帕金森病评定量表第二部分评分效果最佳。 (2)统一帕金森病评定量表第三部分:机器人辅助步态训练对帕金森病患者统一帕金森病评定量表第三部分的影响:7项研究采用统一帕金森病评定量表第三部分评估帕金森病患者的整体运动功能[22-24,26-28,31],共347例患者(试验组173例,对照组174例)。合并效应量时,各研究间具有中度异质性(I2=67%),敏感性分析发现,剔除KIM等[26]、夏敏等[24]的研究后,异质性降低(I2=50%,P=0.09),异质性在可接受范围内,故采用固定效应模型进行分析。结果显示:试验组统一帕金森病评定量表第三部分评分明显低于对照组,具有统计学意义[MD=-3.73,95%CI(-4.17,-3.29,P < 0.000 01],见图31。根据干预时间进行亚组分析,亚组分析结果显示,治疗周期为4周[MD=-2.66,95%CI(-3.47,-1.85),P < 0.000 01]与8周[MD=-3.85,95%CI(-4.32,-3.38),P < 0.000 01] 时试验组统一帕金森病评定量表第三部分评分明显低于对照组,且均具有统计学意义,见图32,33。以上结果提示干预4周时机器人辅助步行训练改善统一帕金森病评定量表第三部分评分与干预时间有关。 2.5 发表偏倚分析 所有结果中,关于起立-行走试验时间的文献最多,故以起立-行走试验时间为例进行漏斗图分析。结果显示试验组和对照组间起立-行走试验时间比较的漏斗图不完全对称,提示纳入的研究可能存在一定的小样本效应及发表偏倚,见图34。"
| [1] JANKOVIC J, TAN EK. Parkinson’s disease: etiopathogenesis and treatment. J Neurol Neurosurg Psychiatry. 2020;91(8):795-798. [2] HAYES MT. Parkinson’s disease and parkinsonism. Am J Med. 2019;132(7):802-807. [3] OPARA J, MAŁECKI A, MAŁECKA E, et al. Motor assessment in Parkinson’s disease. Ann Agric Environ Med. 2017;24(3):411-415. [4] CUI ML, LIU XH, LL Y, et al. Static Posture Instability as a Sensitive Biomarker for Motor Abnormalities in Pre-ataxic Spinocerebellar Ataxia Type 3 Patients. Mov Disord. 2025;40(4):642-650. [5] BALASH Y, PERETZ C, LEIBOVICH G, et al. Falls in outpatients with Parkinson’s disease: frequency, impact and identifying factors. J Neurol. 2005; 252(11):1310-1315. [6] ZHAO HY, HAN JT, HU DH, et al. A randomized controlled trial on the effect of exercise prescription based on a progressive mode in treating elderly patients with lower limb dysfunction after deep burns. Zhonghua Shao Shang Yu Chuang Mian Xiu Fu Za Zhi. 2023;39(12): 1122-1130. [7] KOHLE F, STARK C, KIVNTER HD, et al. Peripheral neuropathy, an independent risk factor for falls in the elderly, impairs stepping as a postural control mechanism: A case-cohort study. J Peripher Nerv Syst. 2024;29(4):453-463. [8] KIM SK, PARK D, YOO B, et al. Overground Robot-Assisted Gait Training for Pediatric Cerebral Palsy. Sensors (Basel). 2021;21(6):2087. [9] CHAI A. Pleiotropic neurotransmitters: neurotransmitter-receptor crosstalk regulates excitation-inhibition balance in social brain functions and pathologies. Front Neurosci. Front Neurosci. 2025;19:1552145. [10] ZENG X, QIU XC, MA YH, et al. Integration of donor mesenchymal stem cell-derived neuron-like cells into host neural network after rat spinal cord transection. Biomaterials. 2015;53:184-201. [11] HUSSAIN S, XIE SQ, LIU G. Robot assisted treadmill training: mechanisms and training strategies. Med Eng Phys. 2011;33(5):527-533. [12] CAO J, XIE SQ, DAS R, et al. Control strategies for effective robot assisted gait rehabilitation: the state of art and future prospects. Med Eng Phys. 2014;36(12):1555-1566. [13] BHARDWAJ S, KHAN AA, MUZAMMIL M. Lower limb rehabilitation robotics: The current understanding and technology. Work. 2021;69(3):775-793. [14] FANG CY, TSAI JL, LI GS, et al. Effects of Robot-Assisted Gait Training in Individuals with Spinal Cord Injury: A Meta-analysis. Biomed Res Int. 2020;2020:2102785. [15] CALAFIORE D, NEGRINI F, TOTTOLI N, et al. Efficacy of robotic exoskeleton for gait rehabilitation in patients with subacute stroke: a systematic review. Eur J Phys Rehabil Med. 2022;58(1):1-8. [16] PEREZ-DE LA CRUZ S. Use of Robotic Devices for Gait Training in Patients Diagnosed with Multiple Sclerosis: Current State of the Art. Sensors (Basel). 2022;22(7):2706. [17] YUN SJ, LEE HH, LEE WH, et al. Effect of robot-assisted gait training on gait automaticity in Parkinson disease: A prospective, open-label, single-arm, pilot study. Medicine (Baltimore). 2021;100(5):e24348. [18] GALLI M, CIMOLIN V, DE PANDIS MF, et al. Robot-assisted gait training versus treadmill training in patients with Parkinson’s disease: a kinematic evaluation with gait profile score. Funct Neurol. 2016;31(3):163-170. [19] SLADE SC, FINKELSTEIN DI, MCGINLEY JL, et al. Exercise and physical activity for people with Progressive Supranuclear Palsy: a systematic review. Clin Rehabil. 2020;34(1):23-33. [20] ALWARDAT M, ETOOM M, Al DAJAH S, et al. Effectiveness of robot-assisted gait training on motor impairments in people with Parkinson’s disease: a systematic review and meta-analysis. Int J Rehabil Res. 2018;41(4):287-296. [21] PICELLI A, CAPECCI M, FILIPPETTI M, et al. Effects of robot-assisted gait training on postural instability in Parkinson’s disease: a systematic review. Eur J Phys Rehabil Med. 2021;57(3):472-477. [22] 丁文娟,梁成盼,苏敏.下肢康复机器人对帕金森病患者平衡功能影响的研究[J]. 中国康复医学杂志,2022,37(4):494-500. [23] 马海玲,何清,吴召军,等.下肢康复机器人联合视听觉训练对帕金森病患者步态的影响[J]. 中国社区医师,2020,36(35):158-159. [24] 夏敏,詹增土,蔡国恩,等.帕金森病患者全自动下肢机器人训练前后的三维步态分析[J]. 中华神经科杂志,2018,51(7):504-509. [25] 陈登钟,苏小燕.下肢机器人步态训练对帕金森患者的疗效观察[J]. 中国医疗器械信息,2016, 22(23):50-52. [26] KIM H, KIM E, YUN SJ, et al. Robot-assisted gait training with auditory and visual cues in Parkinson’s disease: A randomized controlled trial. Ann Phys Rehabil Med. 2022;65(3):101620. [27] CAPECCI M, POURNAJAF S, GALAFATE D, et al. Clinical effects of robot-assisted gait training and treadmill training for Parkinson’s disease: a randomized controlled trial. Ann Phys Rehabil Med. 2019;62(5):303-312. [28] PICELLI A, MELOTTI C, ORIGANO F, et al. Robot-assisted gait training is not superior to balance training for improving postural instability in patients with mild to moderate Parkinson’s disease: a single-blind randomized controlled trial. Clin Rehabil. 2015;29(4):339-347. [29] SALE P, DE PANDIS MF, LE PERA D, et al. Robot-assisted walking training for individuals with Parkinson’s disease: a pilot randomized controlled trial. BMC Neurol. 2013;13:50. [30] PICELLI A, MELOTTI C, ORIGANO F, et al. Robot-assisted gait training versus equal intensity treadmill training in patients with mild to moderate Parkinson’s disease: A randomized controlled trial. Parkinsonism Relat Disord. 2013; 19(6):605-610. [31] PICELLI A, MELOTTI C, ORIGANO F, et al. Does robotic gait training improve balance in Parkinson’s disease? A randomized controlled trial. Parkinsonism Relat Disord. 2012;18(8):990-993. [32] PICELLI A, MELOTTI C, ORIGANO F, et al. Robot-Assisted Gait Training in Patients With Parkinson Disease: A Randomized Controlled Trial. Neurorehabil Neural Repair. 2012;26(4):353-361. [33] 刘燕平,陈美云. Lokomat 下肢康复机器人对改善帕金森病患者步行能力的疗效研究[J]. 中国康复,2017,32(1):30-32. [34] BLANDINI F, NAPPI G, TASSORELLI C, et al. Functional changes of the basal ganglia circuitry in Parkinson’s disease. Prog Neurobiol. 2000; 62(1):63-88. [35] MARINO G, CAMPANELLY F, NATALE G, et al. Intensive exercise ameliorates motor and cognitive symptoms in experimental Parkinson’s disease restoring striatal synaptic plasticity. Sci Adv. 2023; 9(28):eadh1403. [36] 彭瑾, 刘宇, 王晓慧. 运动因子对帕金森病运动障碍的改善作用及机制[J]. 生物化学与生物物理进展,2025,52(9):2332-2345. [37] ESQUENAZI A, PACKEL A. Robotic-assisted gait training and restoration. Am J Phys Med Rehabil. 2012;91(11 Suppl 3):S217-S227;quiz S228-S231. [38] HALPERIN O, ISRAELI-KORN S, YAKUBOVICH S, et al. Self-motion perception in Parkinson’s disease. Eur J Neurosci. 2021; 53(7):2376-2387. [39] AACH M, CRUCIGER O, SCZESNY-KAISER M, et al. Voluntary driven exoskeleton as a new tool for rehabilitation in chronic spinal cord injury: a pilot study. Spine J. 2014;14(12):2847-2853. [40] STUART S, MANCINI M. Prefrontal Cortical Activation With Open and Closed-Loop Tactile Cueing When Walking and Turning in Parkinson Disease: A Pilot Study. J Neurol Phys Ther. 2020; 44(2):121-131. [41] PTAK R, SCHNIDER A, FELLRATH J. The Dorsal Frontoparietal Network: A Core System for Emulated Action. Trends Cogn Sci. 2017;21(8):589-599. [42] HERZ DM, EICKHOFF SB, LOKKEGAARD A, et al. Functional neuroimaging of motor control in Parkinson’s disease: a meta-analysis. Hum Brain Mapp. 2014;35(7):3227-3237. [43] WESTERBERG E, MOLIN CJ, LINDBLAD I, et al. Physical exercise in myasthenia gravis is safe and improves neuromuscular parameters and physical performance-based measures: A pilot study. Muscle Nerve. 2017;56(2):207-214. [44] TOSSERAMS A, WEERDESTEYN V, BAL T, et al. Cortical Correlates of Gait Compensation Strategies in Parkinson Disease. Ann Neurol. 2022; 91(3):329-341. [45] QIAN Y, FU X, ZHANG H, et al. Comparative efficacy of 24 exercise types on postural instability in adults with Parkinson’s disease: a systematic review and network meta-analysis. BMC Geriatr. 2023;23(1):522. [46] LORENZO-GARCIA P, CAVERO-REDONDO I, TORRES-COSTOSO AI, et al. Body Weight Support Gait Training for Patients With Parkinson Disease: A Systematic Review and Meta-analyses. Arch Phys Med Rehabil. 2021;102(10):2012-2021. [47] JAKOB V, KVDERLE A, KLUGE F, et al. Validation of a Sensor-Based Gait Analysis System with a Gold-Standard Motion Capture System in Patients with Parkinson’s Disease. Sensors (Basel). 2021; 21(22):7622. [48] SIMIS M, UYGUR-KUCUKSEYMEN E, PACHECO-BARRIOS K, et al. Beta-band oscillations as a biomarker of gait recovery in spinal cord injury patients: A quantitative electroencephalography analysis. Clin Neurophysiol. 2020;131(8):1806-1814. [49] KHALILIYAN H, SHARAFATVAZIRI A, SAFAEEPOUR Z, et al. Gait and muscle activity measures after biomechanical device therapy in subjects with ankle instability: A systematic review. Foot (Edinb). 2024:59:102083. [50] YIN W, JING Z, DING J, et al. Stride-wise Adaptive Assistance Strategy for Ankle Exoskeleton Under Varying Walking Conditions. IEEE Trans Neural Syst Rehabil Eng. 2025. doi:10.1109/TNSRE.2025.3602098 [51] INKSTER LM, ENG JJ, MACINTYRE DL, et al. Leg muscle strength is reduced in Parkinson’s disease and relates to the ability to rise from a chair. Mov Disord. 2003;18(2):157-162. [52] YOKOTE A, HAYASHI Y, YANAMOTO S, et al. Leg Muscle Strength Correlates with Gait Performance in Advanced Parkinson Disease. Intern Med. 2022; 61(5):633-638. [53] 许梦圆, 陈涛, 孟徐, 等. 帕金森病运动症状量化评估的研究进展[J]. 中华神经科杂志, 2020, 53(10):845-854. |
| [1] | He Yixiang, Qiao Wanjia, Wang Wenji. Effectiveness and safety of tranexamic acid versus epsilon-aminocaproic acid in total hip and knee arthroplasties: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2361-2369. |
| [2] | Liu Jinlong, Abuduwupuer·Haibier, Bai Zhen, Su Danyang, Miao Xin, Li Fei, Yang Xiaopeng. Efficacy of different nonsurgical treatments for adolescent idiopathic scoliosis: a systematic review and network meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2370-2379. |
| [3] | Gao Feng, Zhang Jun, Yu Wenjun, Chanyu Yujing, Zhao Le, Hu Yuting, Wang Junhua, Liu Yongfu. Effects of wrist-hand orthosis on hand dysfunction in stroke patients: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2124-2131. |
| [4] | Wang Zhenze, Liu Fende, Zhang Rui, Li Wujun. Mesenchymal stem cells in treatment of arteriosclerosis obliterans of lower extremities: systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(7): 1869-1876. |
| [5] | Cao Xinyan, Yu Zifu, Leng Xiaoxuan, Gao Shiai, Chen Jinhui, Liu Xihua. Effect of repetitive transcranial magnetic stimulation and transcranial direct current stimulation on motor function and gait in children with cerebral palsy: a network meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1539-1548. |
| [6] | Zheng Yin, Wu Zhenhua, Zhang Cheng, Ruan Kexin, Gang Xiaolin, Ji Hong. Safety and efficacy of immunoadsorption therapy for rheumatoid arthritis: a network meta-analysis and systematic review [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(5): 1260-1268. |
| [7] | Chen Qiang, Wu Wenjuan, Jiang Shuhua, Huang Da. Physical exercise improves physical function in burn patients: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(5): 1269-1281. |
| [8] | Leng Xiaoxuan, Zhao Yuxin, Liu Xihua. Effects of different neuromodulatory stimulation modalities on non-motor symptoms in Parkinson’s patients: a network meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(5): 1282-1293. |
| [9] | Wen Xiaolong, Weng Xiquan, Feng Yao, Cao Wenyan, Liu Yuqian, Wang Haitao. Effects of inflammation on serum hepcidin and iron metabolism related parameters in patients with type 2 diabetes mellitus: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(5): 1294-1301. |
| [10] | Jiang Yang, Peng Hao, Song Yanping, Yao Na, Song Yueyu, Yin Xingxiao, Li Yanqi, Chen Qigang. Isometric exercise reduces resting blood pressure: a meta-analysis of moderating factors and dose effects [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(4): 975-986. |
| [11] | Li Hanyue, Li Yini, Xiang Linmei, Li Sen. Effects of resistance exercise therapy on pain and function in patients with cervical spondylotic radiculopathy: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(4): 987-996. |
| [12] | Sun Jiahe, Shi Jipeng, Zhu Tianrui, Quan Helong, Xu Hongqi. Effect of exercise intervention in elderly individuals with sarcopenia and its comorbidities: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(4): 997-1007. |
| [13] | Yang Yuanyuan, Zhou Shanshan, Cheng Xiaofei, Feng Luye, Tang Jiqin. Network meta-analysis of non-invasive brain stimulation in the treatment of lower limb motor dysfunction after stroke [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(4): 1008-1018. |
| [14] | Yang Peng, Xu Chenghan, Zhou Yingjie, Chai Xubin, Zhuo Hanjie, Li Lin, Shi Jinyu. A meta-analysis of risk factors for residual back pain after vertebral augmentation for osteoporotic vertebral compression fractures [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(3): 731-739. |
| [15] | Li Sihui, Wang Qin, Cui Shenhong, Cheng Xiaofei, Feng Ziyun, Wang Dehua, Liang Chunting, Leng Jun. A network meta-analysis of effects of non-invasive neuromodulation techniques on language function in patients with aphasia after stroke [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(28): 7485-7493. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||