Chinese Journal of Tissue Engineering Research ›› 2022, Vol. 26 ›› Issue (31): 4967-4974.doi: 10.12307/2022.993
Previous Articles Next Articles
Human amniotic epithelial cells regulate the proliferation, apoptosis and extracellular matrix synthesis of articular chondrocytes by activating the EGFR/ERK1 signaling axis
Wang Kang1, 2, Zhi Xiaodong1, 2, Zhang Yuqiang1, 2, Gong Chao1, 2, Wang Chenliang1, 2, Wang Wei1, 2, 3
- 1Department of Orthopedics, First Affiliated Hospital of Jinzhou Medical University, Jinzhou 121000, Liaoning Province, China; 2Liaoning Key Laboratory of Medical Tissue Engineering, Jinzhou 121000, Liaoning Province, China; 3Institute of Orthopedics, Jinzhou Medical University, Jinzhou 121000, Liaoning Province, China
-
Received:2021-07-05Accepted:2021-08-19Online:2022-11-08Published:2022-04-24 -
Contact:Wang Wei, MD, Chief physician, Professor, Department of Orthopedics, First Affiliated Hospital of Jinzhou Medical University, Jinzhou 121000, Liaoning Province, China; Liaoning Key Laboratory of Medical Tissue Engineering, Jinzhou 121000, Liaoning Province, China; Institute of Orthopedics, Jinzhou Medical University, Jinzhou 121000, Liaoning Province, China -
About author:Wang Kang, Master candidate, Department of Orthopedics, First Affiliated Hospital of Jinzhou Medical University, Jinzhou 121000, Liaoning Province, China; Liaoning Key Laboratory of Medical Tissue Engineering, Jinzhou 121000, Liaoning Province, China -
Supported by:The School-Enterprise Cooperation Fund Project of Jinzhou Medical University, No. 2020002 (to WW); Science and Technology Foundation of Liaoning Provincial Department of Science and Technology, No. 20180551216 (to ZXD)
CLC Number:
Cite this article
Wang Kang, Zhi Xiaodong, Zhang Yuqiang, Gong Chao, Wang Chenliang, Wang Wei. Human amniotic epithelial cells regulate the proliferation, apoptosis and extracellular matrix synthesis of articular chondrocytes by activating the EGFR/ERK1 signaling axis[J]. Chinese Journal of Tissue Engineering Research, 2022, 26(31): 4967-4974.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks

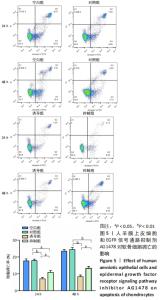
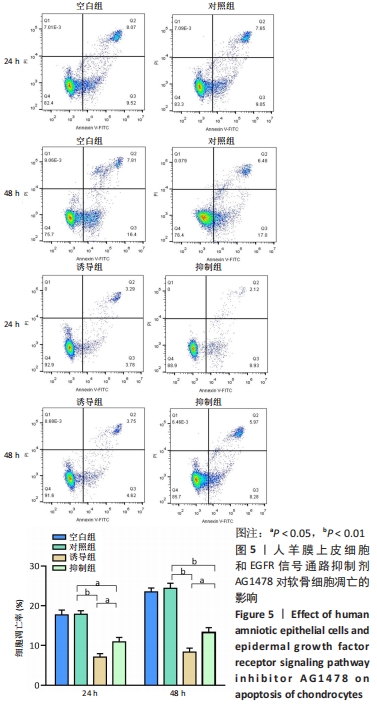
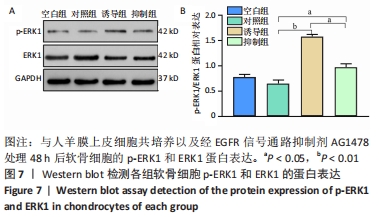
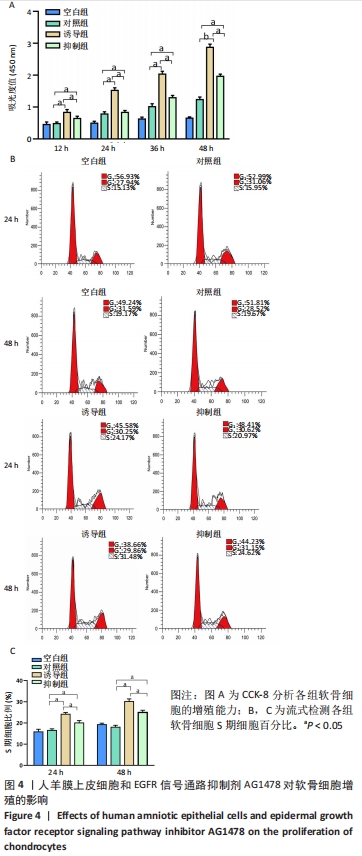
2.2 各组软骨细胞增殖能力 CCK-8实验结果表明,人羊膜上皮细胞与软骨细胞共培养可以显著增强软骨细胞的增殖活性,并且趋势是时间依赖性的;加入EGFR信号通路抑制剂AG1478后,促进作用明显减弱,差异有显著性意义(P < 0.05),见图4A。为了进一步证实人羊膜上皮细胞和AG1478对软骨细胞增殖的影响,使用流式细胞仪检测每组软骨细胞的细胞周期分布。与对照组比较,软骨细胞与人羊膜上皮细胞共培养24,48 h后可以显著增加S期细胞比例,表明人羊膜上皮细胞可以增强软骨细胞的增殖能力,差异有显著性意义(P < 0.05)。与诱导组比较,抑制组24 h和48 h的S期细胞比例明显降低,表明EGFR信号通路抑制剂可以减弱人羊膜上皮细胞促进软骨细胞增殖的作用,差异有显著性意义(P < 0.05),见图4B和4C。"
| [1] SHARMA L. Osteoarthritis of the Knee. N Engl J Med. 2021;384(1):51-59. [2] LATOURTE A, KLOPPENBURG M, RICHETTE P. Emerging pharmaceutical therapies for osteoarthritis. Nat Rev Rheumatol. 2020;16(12):673-688. [3] YUNUS MHM, NORDIN A, KAMAL H. Pathophysiological Perspective of Osteoarthritis. Medicina (Kaunas). 2020;56(11):614. [4] KATZ JN, ARANT KR, LOESER RF. Diagnosis and Treatment of Hip and Knee Osteoarthritis: A Review. JAMA. 2021;325(6):568-578. [5] MAHESHWER B, POLCE EM, PAUL K, et al. Regenerative Potential of Mesenchymal Stem Cells for the Treatment of Knee Osteoarthritis and Chondral Defects: A Systematic Review and Meta-analysis. Arthroscopy. 2021;37(1):362-378. [6] DOYLE EC, WRAGG NM, WILSON SL. Intraarticular injection of bone marrow-derived mesenchymal stem cells enhances regeneration in knee osteoarthritis. Knee Surg Sports Traumatol Arthrosc. 2020; 28(12):3827-3842. [7] MA W, LIU C, WANG S, et al. Efficacy and safety of intra-articular injection of mesenchymal stem cells in the treatment of knee osteoarthritis: A systematic review and meta-analysis. Medicine (Baltimore). 2020;99(49):e23343. [8] GUPTA A, CADY C, FAUSER AM, et al. Cell-free Stem Cell-Derived Extract Formulation for Regenerative Medicine Applications. Int J Mol Sci. 2020;21(24):9364. [9] QIU C, GE Z, CUI W, et al. Human Amniotic Epithelial Stem Cells: A Promising Seed Cell for Clinical Applications. Int J Mol Sci. 2020;21(20): 7730. [10] ZHANG Q, LAI D. Application of human amniotic epithelial cells in regenerative medicine: a systematic review. Stem Cell Res Ther. 2020; 11(1):439. [11] LIU QW, HUANG QM, WU HY, et al. Characteristics and Therapeutic Potential of Human Amnion-Derived Stem Cells. Int J Mol Sci. 2021; 22(2):970. [12] MIKI T. Stem cell characteristics and the therapeutic potential of amniotic epithelial cells. Am J Reprod Immunol. 2018;80(4):e13003. [13] MUTTINI A, BARBONI B, VALBONETTI L, et al. Amniotic Epithelial Stem Cells: Salient Features and Possible Therapeutic Role. Sports Med Arthrosc Rev. 2018;26(2):70-74. [14] LEBRETON F, LAVALLARD V, BELLOFATTO K, et al. Insulin-producing organoids engineered from islet and amniotic epithelial cells to treat diabetes. Nat Commun. 2019;10(1):4491. [15] XU H, ZHANG J, TSANG KS, et al. Therapeutic Potential of Human Amniotic Epithelial Cells on Injuries and Disorders in the Central Nervous System. Stem Cells Int. 2019;2019:5432301. [16] REN Y, CHEN Y, ZHENG X, et al. Human amniotic epithelial cells ameliorate kidney damage in ischemia-reperfusion mouse model of acute kidney injury. Stem Cell Res Ther. 2020;11(1):410. [17] SABBAH DA, HAJJO R, SWEIDAN K. Review on Epidermal Growth Factor Receptor (EGFR) Structure, Signaling Pathways, Interactions, and Recent Updates of EGFR Inhibitors. Curr Top Med Chem. 2020;20(10):815-834. [18] SCHNEIDER MR, SIBILIA M, ERBEN RG. The EGFR network in bone biology and pathology. Trends Endocrinol Metab. 2009;20(10):517-524. [19] BYRNE PO, HRISTOVA K, LEAHY DJ. EGFR forms ligand-independent oligomers that are distinct from the active state. J Biol Chem. 2020; 295(38):13353-13362. [20] APPLETON CT, USMANI SE, MORT JS, et al. Rho/ROCK and MEK/ERK activation by transforming growth factor-alpha induces articular cartilage degradation. Lab Invest. 2010;90(1):20-30. [21] 袁功武,兰生辉,刘曦明.表皮生长因子受体信号通路对骨折愈合的生物学作用[J].中国矫形外科杂志,2018,26(4):328-332. [22] 袁功武,兰生辉,曾文波,等.吉非替尼对骨折愈合中I、II及X 型胶原基因表达的影响[J].中国矫形外科杂志,2018,26(10):939-944. [23] 程潭.降钙素对大鼠膝关节骨性关节炎潜在保护作用及其机制[D].石家庄:河北医科大学,2012. [24] ALIMIRAH F, PULIDO T, VALDOVINOS A, et al. Cellular Senescence Promotes Skin Carcinogenesis through p38MAPK and p44/42MAPK Signaling. Cancer Res. 2020;80(17):3606-3619. [25] PAN L, NI H, JIN W, et al. Inhibition of ERK or Akt ameliorates intimal hyperplasia via up-regulation of Cx37 and down-regulation of Cx43 in balloon injury rat model. Cardiovasc Diagn Ther. 2020;10(4):658-666. [26] WU Q, FANG T, LANG H, et al. Comparison of the proliferation, migration and angiogenic properties of human amniotic epithelial and mesenchymal stem cells and their effects on endothelial cells. Int J Mol Med. 2017;39(4):918-926. [27] MA XF, MA XB, QIAN WJ, et al. Co-Culture of Adipose-Derived Stem Cells and Chondrocytes With Transforming Growth Factor-Beta 3 Promotes Chondrogenic Differentiation. J Craniofac Surg. 2020;31(8): 2355-2359. [28] KAWAKAMI T, KOMATSU T, YOKOYAMA K, et al. Establishment of co-culture of human induced pluripotent stem cell-derived melanocytes and keratinocytes in vitro. J Dermatol. 2021;48(1):123-125. [29] HUNTER DJ, MARCH L, CHEW M. Osteoarthritis in 2020 and beyond: a Lancet Commission. Lancet. 2020;396(10264):1711-1712. [30] KULKARNI P, MARTSON A, VIDYA R, et al. Pathophysiological landscape of osteoarthritis. Adv Clin Chem. 2021;100:37-90. [31] KALAMEGAM G, MEMIC A, BUDD E, et al. A Comprehensive Review of Stem Cells for Cartilage Regeneration in Osteoarthritis. Adv Exp Med Biol. 2018;1089:23-36. [32] DÍAZ-PRADO S, MUIÑOS-LÓPEZ E, HERMIDA-GÓMEZ T, et al. Human amniotic membrane as an alternative source of stem cells for regenerative medicine. Differentiation. 2011;81(3):162-171. [33] MANUELPILLAI U, MOODLEY Y, BORLONGAN CV, et al. Amniotic membrane and amniotic cells: potential therapeutic tools to combat tissue inflammation and fibrosis? Placenta. 2011;32 Suppl 4:S320-325. [34] LIU XY, CHEN J, ZHOU Q, et al. In vitro tissue engineering of lamellar cornea using human amniotic epithelial cells and rabbit cornea stroma. Int J Ophthalmol. 2013;6(4):425-429. [35] YANG PJ, YUAN WX, LIU J, et al. Biological characterization of human amniotic epithelial cells in a serum-free system and their safety evaluation. Acta Pharmacol Sin. 2018;39(8):1305-1316. [36] SANKAR V, MUTHUSAMY R. Role of human amniotic epithelial cell transplantation in spinal cord injury repair research. Neuroscience. 2003;118(1):11-17. [37] YUGE I, TAKUMI Y, KOYABU K, et al. Transplanted human amniotic epithelial cells express connexin 26 and Na-K-adenosine triphosphatase in the inner ear. Transplantation. 2004;77(9):1452-1454. [38] HORI J, WANG M, KAMIYA K, et al. Immunological characteristics of amniotic epithelium. Cornea. 2006;25(10 Suppl 1):S53-58. [39] MIKI T, LEHMANN T, CAI H, et al. Stem cell characteristics of amniotic epithelial cells. Stem Cells. 2005;23(10):1549-1559. [40] SCHNEIDER MR, WOLF E. The epidermal growth factor receptor ligands at a glance. J Cell Physiol. 2009;218(3):460-466. [41] ZHANG X, ZHU J, LIU F, et al. Reduced EGFR signaling enhances cartilage destruction in a mouse osteoarthritis model. Bone Res. 2014;2:14015. [42] ROMANO R, BUCCI C. Role of EGFR in the Nervous System. Cells. 2020; 9(8):1887. [43] ZHU M, QIN YC, GAO CQ, et al. l-Glutamate drives porcine intestinal epithelial renewal by increasing stem cell activity via upregulation of the EGFR-ERK-mTORC1 pathway. Food Funct. 2020;11(3):2714-2724. [44] LINDER M, HECKING M, GLITZNER E, et al. EGFR controls bone development by negatively regulating mTOR-signaling during osteoblast differentiation. Cell Death Differ. 2018;25(6):1094-1106. [45] 任科伟,范卫民,姜雪峰,等.周期性机械应力通过激活EGFR-ERK1/2信号通路促进大鼠软骨细胞增殖和细胞外基质合成[J].江苏医药,2013,39(21):2526-2528. |
| [1] | LIU Danni, SUN Guanghua, ZHOU Guijuan, LIU Hongya, ZHOU Jun, TAN Jinqu, HUANG Xiarong, PENG Ting, FENG Wei-bin, LUO Fu. Effect of electroacupuncture on apoptosis of neurons in cerebral cortex of rats with cerebral ischemia-reperfusion injury at "Shuigou" and "Baihui" points [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(在线): 1-6. |
| [2] | Zhang Haobo, Zhao Yunan, Yang Xuejun. Role and therapeutic implications of pyroptosis in intervertebral disc degeneration [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1445-1451. |
| [3] | Jin Tao, Liu Lin, Zhu Xiaoyan, Shi Yucong, Niu Jianxiong, Zhang Tongtong, Wu Shujin, Yang Qingshan. Osteoarthritis and mitochondrial abnormalities [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1452-1458. |
| [4] | Zhang Jichao, Dong Yuefu, Mou Zhifang, Zhang Zhen, Li Bingyan, Xu Xiangjun, Li Jiayi, Ren Meng, Dong Wanpeng. Finite element analysis of biomechanical changes in the osteoarthritis knee joint in different gait flexion angles [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1357-1361. |
| [5] | Wang Baojuan, Zheng Shuguang, Zhang Qi, Li Tianyang. Miao medicine fumigation can delay extracellular matrix destruction in a rabbit model of knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1180-1186. |
| [6] | Wang Jifang, Bao Zhen, Qiao Yahong. miR-206 regulates EVI1 gene expression and cell biological behavior in stem cells of small cell lung cancer [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1027-1031. |
| [7] | Wen Dandan, Li Qiang, Shen Caiqi, Ji Zhe, Jin Peisheng. Nocardia rubra cell wall skeleton for extemal use improves the viability of adipogenic mesenchymal stem cells and promotes diabetes wound repair [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1038-1044. |
| [8] | Zhu Bingbing, Deng Jianghua, Chen Jingjing, Mu Xiaoling. Interleukin-8 receptor enhances the migration and adhesion of umbilical cord mesenchymal stem cells to injured endothelium [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1045-1050. |
| [9] | Zhang Yujie, Yang Jiandong, Cai Jun, Zhu Shoulei, Tian Yuan. Mechanism by which allicin inhibits proliferation and promotes apoptosis of rat vascular endothelial cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1080-1084. |
| [10] | Zhang Jinglin, Leng Min, Zhu Boheng, Wang Hong. Mechanism and application of stem cell-derived exosomes in promoting diabetic wound healing [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1113-1118. |
| [11] | Liu Dongcheng, Zhao Jijun, Zhou Zihong, Wu Zhaofeng, Yu Yinghao, Chen Yuhao, Feng Dehong. Comparison of different reference methods for force line correction in open wedge high tibial osteotomy [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 827-831. |
| [12] | Zhou Jianguo, Liu Shiwei, Yuan Changhong, Bi Shengrong, Yang Guoping, Hu Weiquan, Liu Hui, Qian Rui. Total knee arthroplasty with posterior cruciate ligament retaining prosthesis in the treatment of knee osteoarthritis with knee valgus deformity [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 892-897. |
| [13] | He Junjun, Huang Zeling, Hong Zhenqiang. Interventional effect of Yanghe Decoction on synovial inflammation in a rabbit model of early knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 694-699. |
| [14] | Lin Xuchen, Zhu Hainian, Wang Zengshun, Qi Tengmin, Liu Limin, Suonan Angxiu. Effect of xanthohumol on inflammatory factors and articular cartilage in a mouse mode of osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 676-681. |
| [15] | Deng Shuang, Pu Rui, Chen Ziyang, Zhang Jianchao, Yuan Lingyan . Effects of exercise preconditioning on myocardial protection and apoptosis in a mouse model of myocardial remodeling due to early stress overload [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 717-723. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||