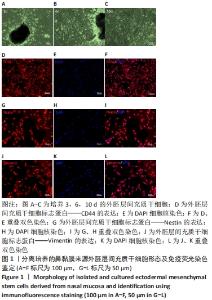
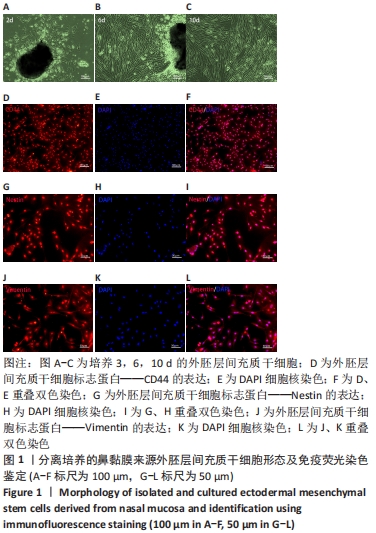
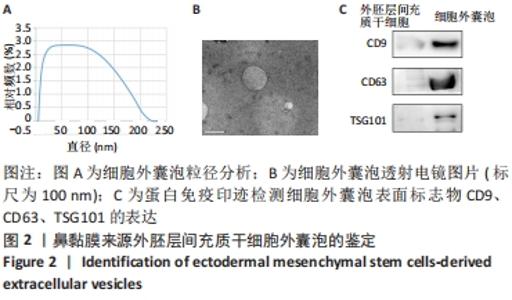
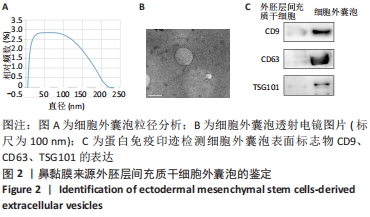
Chinese Journal of Tissue Engineering Research ›› 2022, Vol. 26 ›› Issue (30): 4840-4846.doi: 10.12307/2022.764
Previous Articles Next Articles
Transdifferentiation of rat astrocytes into neurons induced by ectodermal mesenchymal stem cells-derived extracellular vesicles
Guan Shihao1, Huang Yonghui1, Gong Aihua2, Cao Xingbing1, Sun Haitao1, Cai Chuang1
- 1Affiliated Hospital of Jiangsu University, Zhenjiang 212000, Jiangsu Province, China; 2Jiangsu University, Zhenjiang 212000, Jiangsu Province, China
-
Received:2021-08-31Accepted:2021-10-11Online:2022-10-28Published:2022-03-29 -
Contact:Huang Yonghui, Master, Chief physician, Affiliated Hospital of Jiangsu University, Zhenjiang 212000, Jiangsu Province, China -
About author:Guan Shihao, Master candidate, Affiliated Hospital of Jiangsu University, Zhenjiang 212000, Jiangsu Province, China -
Supported by:Zhenjiang Science and Technology Project, No. SH2020053 (to HYH)
CLC Number:
Cite this article
Guan Shihao, Huang Yonghui, Gong Aihua, Cao Xingbing, Sun Haitao, Cai Chuang. Transdifferentiation of rat astrocytes into neurons induced by ectodermal mesenchymal stem cells-derived extracellular vesicles[J]. Chinese Journal of Tissue Engineering Research, 2022, 26(30): 4840-4846.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
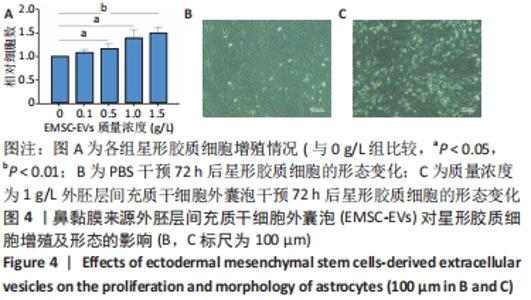
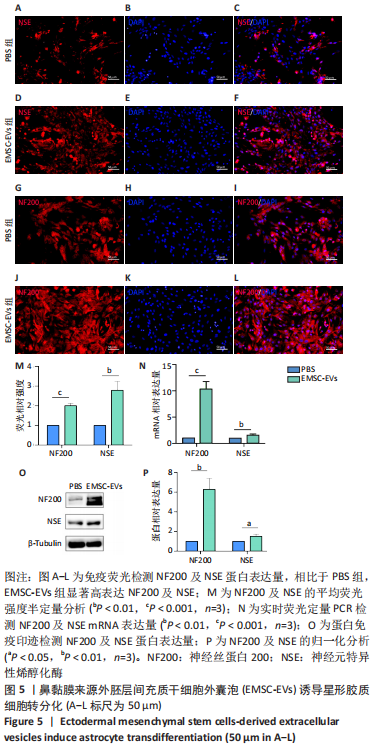
2.4 EMSC-EVs对星形胶质细胞存活率的影响 随着EMSC-EVs质量浓度的增加,星形胶质细胞数量明显增高,且呈一定浓度依赖性,1.0,1.5 g/L细胞外囊泡均能有效促进细胞增殖,参考相关文献[24],选用1 g/L EMSC-EVs进行后续实验,见图4A。 2.5 EMSC-EVs干预星形胶质细胞后形态变化以及免疫荧光检测结果 PBS组细胞呈现原有不规则星状,神经元样细胞较少,突起较短且少,见图4B,而EMSC-EVs干预72 h后可见EMSC-EVs组细胞呈现神经元样,胞体饱满呈梭形,突起增多变长,见图4C。采用免疫荧光检测EMSC-EVs干预72 h后神经元特异性蛋白表达,EMSC-EVs组显示成熟神经元表型特征神经元特异性烯醇化酶及神经丝蛋白200的表达较PBS组显著增多(P < 0.01,P < 0.001,n=3),见图5A-M。 2.6 实时荧光定量PCR及蛋白免疫印迹检测EMSC-EVs干预后细胞中神经元特异性烯醇化酶及神经丝蛋白200的表达 EMSC-EVs组较PBS组显著高表达神经元特异性烯醇化酶及神经丝蛋白200(P 均 < 0.001,n=3),见图5N-P,以上结果提示 EMSC-EVs可以诱导大鼠星形胶质细胞向神经元转分化。"

| [1] HOU B, ZHANG Y, LIANG P, et al. Inhibition of the NLRP3-inflammasome prevents cognitive deficits in experimental autoimmune encephalomyelitis mice via the alteration of astrocyte phenotype. Cell Death Dis. 2020;11(5):377. [2] MURRAY CE, GAMI-PATEL P, GKANATSIOU E, et al. The presubiculum is preserved from neurodegenerative changes in Alzheimer’s disease. Acta Neuropathol Commun. 2018;6(1):62. [3] CHEN J, HU R, GE H, et al. G-protein-coupled receptor 30-mediated antiapoptotic effect of estrogen on spinal motor neurons following injury and its underlying mechanisms. Mol Med Rep. 2015;12(2):1733-1740. [4] SARKIS GA, MANGAONKAR MD, MOGHIEB A, et al. The Application of Proteomics to Traumatic Brain and Spinal Cord Injuries. Curr Neurol Neurosci Rep. 2017;17(3):23. [5] LEE JS, HSU YH, CHIU YS, et al. Anti-IL-20 antibody improved motor function and reduced glial scar formation after traumatic spinal cord injury in rats. J Neuroinflammation. 2020;17(1):156. [6] LI P, GAO Y, LI X, et al. mRNA and miRNA expression profile reveals the role of miR-31 overexpression in neural stem cell. Sci Rep. 2020; 10(1):17537. [7] QU J, ZHANG H. Roles of Mesenchymal Stem Cells in Spinal Cord Injury. Stem Cells Int. 2017;2017:5251313. [8] TSAI MJ, LIOU DY, LIN YR, et al. Attenuating Spinal Cord Injury by Conditioned Medium from Bone Marrow Mesenchymal Stem Cells. J Clin Med. 2018;8(1):23. [9] COFANO F, BOIDO M, MONTICELLI M, et al. Mesenchymal Stem Cells for Spinal Cord Injury: Current Options, Limitations, and Future of Cell Therapy. Int J Mol Sci. 2019;20(11):2698. [10] LIAU LL, LOOI QH, CHIA WC, et al. Treatment of spinal cord injury with mesenchymal stem cells. Cell Biosci. 2020;10:112. [11] 黄佩琦,卓毅,段答,等.嗅粘膜间充质干细胞与嗅粘膜嗅鞘细胞在人鼻粘膜中分布的研究[J].湖南师范大学学报(医学版),2020, 17(5):10-14. [12] HUANG H, ZOU X, ZHONG L, et al. CRISPR/dCas9-mediated activation of multiple endogenous target genes directly converts human foreskin fibroblasts into Leydig-like cells. J Cell Mol Med. 2019;23(9):6072-6084. [13] LIANG B, LIANG JM, DING JN, et al. Dimethyloxaloylglycine-stimulated human bone marrow mesenchymal stem cell-derived exosomes enhance bone regeneration through angiogenesis by targeting the AKT/mTOR pathway. Stem Cell Res Ther. 2019;10(1):335. [14] DENG Z, WANG Y, ZHOU L, et al. High salt-induced activation and expression of inflammatory cytokines in cultured astrocytes. Cell Cycle. 2017;16(8):785-794. [15] YANG H, YAN H, LI X, et al. Inhibition of Connexin 43 and Phosphorylated NR2B in Spinal Astrocytes Attenuates Bone Cancer Pain in Mice. Front Cell Neurosci. 2018;12:129. [16] SHIGETOMI E, SAITO K, SANO F, et al. Aberrant Calcium Signals in Reactive Astrocytes: A Key Process in Neurological Disorders. Int J Mol Sci. 2019;20(4):996. [17] YU Y, YAN Y, LUO Z, et al. Effects of human umbilical cord blood CD34+ cell transplantation in neonatal hypoxic-ischemia rat model. Brain Dev. 2019;41(2):173-181. [18] HUANG Y, TAN S. Direct lineage conversion of astrocytes to induced neural stem cells or neurons. Neurosci Bull. 2015;31(3):357-367. [19] SHIH CH, LACAGNINA M, LEUER-BISCIOTTI K, et al. Astroglial-derived periostin promotes axonal regeneration after spinal cord injury. J Neurosci. 2014;34(7):2438-2443. [20] BRULET R, MATSUDA T, ZHANG L, et al. NEUROD1 Instructs Neuronal Conversion in Non-Reactive Astrocytes. Stem Cell Reports. 2017;8(6): 1506-1515. [21] ROBINSON M, FRASER I, MCKEE E, et al. Transdifferentiating Astrocytes Into Neurons Using ASCL1 Functionalized With a Novel Intracellular Protein Delivery Technology. Front Bioeng Biotechnol. 2018;6:173. [22] 凌华军,王其友,林伟文,等.骨髓间充质干细胞来源外泌体保护软骨细胞延缓骨关节炎的发生发展[J].中国组织工程研究,2021, 25(31):4964-4969. [23] ZHAO AG, SHAH K, CROMER B, et al. Mesenchymal Stem Cell-Derived Extracellular Vesicles and Their Therapeutic Potential. Stem Cells Int. 2020;2020:8825771. [24] LIU W, RONG Y, WANG J, et al. Exosome-shuttled miR-216a-5p from hypoxic preconditioned mesenchymal stem cells repair traumatic spinal cord injury by shifting microglial M1/M2 polarization. J Neuroinflammation. 2020;17(1):47. [25] KOMATSU F, FARKAS I, AKATSU H, et al. Potential neural progenitor cells in fetal liver and regenerating liver. Cytotechnology. 2008;56(3):209-217. [26] NAKANO M, FUJIMIYA M. Potential effects of mesenchymal stem cell derived extracellular vesicles and exosomal miRNAs in neurological disorders. Neural Regen Res. 2021;16(12):2359-2366. [27] 朱东京,鲜盼盼,王甜,等.间充质干细胞外泌体对海马星形胶质细胞活化的抑制作用研究[J].中华细胞与干细胞杂志(电子版), 2021,11(2):99-105. [28] RONG Y, LIU W, WANG J, et al. Neural stem cell-derived small extracellular vesicles attenuate apoptosis and neuroinflammation after traumatic spinal cord injury by activating autophagy. Cell Death Dis. 2019;10(5):340. [29] ROMANELLI P, BIELER L, SCHARLER C, et al. Extracellular Vesicles Can Deliver Anti-inflammatory and Anti-scarring Activities of Mesenchymal Stromal Cells After Spinal Cord Injury. Front Neurol. 2019;10:1225. [30] LU Y, ZHOU Y, ZHANG R, et al. Bone Mesenchymal Stem Cell-Derived Extracellular Vesicles Promote Recovery Following Spinal Cord Injury via Improvement of the Integrity of the Blood-Spinal Cord Barrier. Front Neurosci. 2019;13:209. [31] LIU FT, XU SM, XIANG ZH, et al. Molecular hydrogen suppresses reactive astrogliosis related to oxidative injury during spinal cord injury in rats. CNS Neurosci Ther. 2014;20(8):778-786. [32] YU B, YAO C, WANG Y, et al. The Landscape of Gene Expression and Molecular Regulation Following Spinal Cord Hemisection in Rats. Front Mol Neurosci. 2019;12:287. [33] YOKOYAMA A, SAKAMOTO A, KAMEDA K, et al. NG2 proteoglycan-expressing microglia as multipotent neural progenitors in normal and pathologic brains. Glia. 2006;53(7):754-768. [34] ZAREI-KHEIRABADI M, HESARAKI M, KIANI S, et al. In vivo conversion of rat astrocytes into neuronal cells through neural stem cells in injured spinal cord with a single zinc-finger transcription factor. Stem Cell Res Ther. 2019;10(1):380. [35] WANG J, RONG Y, JI C, et al. MicroRNA-421-3p-abundant small extracellular vesicles derived from M2 bone marrow-derived macrophages attenuate apoptosis and promote motor function recovery via inhibition of mTOR in spinal cord injury. J Nanobiotechnology. 2020; 18(1):72. [36] RUPPERT KA, NGUYEN TT, PRABHAKARA KS, et al. Human Mesenchymal Stromal Cell-Derived Extracellular Vesicles Modify Microglial Response and Improve Clinical Outcomes in Experimental Spinal Cord Injury. Sci Rep. 2018;8(1):480. [37] XIAO X, LI W, RONG D, et al. Human umbilical cord mesenchymal stem cells-derived extracellular vesicles facilitate the repair of spinal cord injury via the miR-29b-3p/PTEN/Akt/mTOR axis. Cell Death Discov. 2021;7(1):212. [38] DING ZB, SONG LJ, WANG Q, et al. Astrocytes: a double-edged sword in neurodegenerative diseases. Neural Regen Res. 2021;16(9):1702-1710. [39] YIN JC, ZHANG L, MA NX, et al. Chemical Conversion of Human Fetal Astrocytes into Neurons through Modulation of Multiple Signaling Pathways. Stem Cell Reports. 2019;12(3):488-501. [40] LIU S, LIU D, CHEN C, et al. MSC Transplantation Improves Osteopenia via Epigenetic Regulation of Notch Signaling in Lupus. Cell Metab. 2015; 22(4):606-618. [41] COLLETTI M, TOMAO L, GALARDI A, et al. Neuroblastoma-secreted exosomes carrying miR-375 promote osteogenic differentiation of bone-marrow mesenchymal stromal cells. J Extracell Vesicles. 2020; 9(1):1774144. |
| [1] | Wang Jing, Xiong Shan, Cao Jin, Feng Linwei, Wang Xin. Role and mechanism of interleukin-3 in bone metabolism [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1260-1265. |
| [2] | Xiao Hao, Liu Jing, Zhou Jun. Research progress of pulsed electromagnetic field in the treatment of postmenopausal osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1266-1271. |
| [3] | Tian Chuan, Zhu Xiangqing, Yang Zailing, Yan Donghai, Li Ye, Wang Yanying, Yang Yukun, He Jie, Lü Guanke, Cai Xuemin, Shu Liping, He Zhixu, Pan Xinghua. Bone marrow mesenchymal stem cells regulate ovarian aging in macaques [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 985-991. |
| [4] | Hu Wei, Xie Xingqi, Tu Guanjun. Exosomes derived from bone marrow mesenchymal stem cells improve the integrity of the blood-spinal cord barrier after spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 992-998. |
| [5] | Hou Jingying, Guo Tianzhu, Yu Menglei, Long Huibao, Wu Hao. Hypoxia preconditioning targets and downregulates miR-195 and promotes bone marrow mesenchymal stem cell survival and pro-angiogenic potential by activating MALAT1 [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1005-1011. |
| [6] | Liang Xuezhen, Yang Xi, Li Jiacheng, Luo Di, Xu Bo, Li Gang. Bushen Huoxue capsule regulates osteogenic and adipogenic differentiation of rat bone marrow mesenchymal stem cells via Hedgehog signaling pathway [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1020-1026. |
| [7] | Wen Dandan, Li Qiang, Shen Caiqi, Ji Zhe, Jin Peisheng. Nocardia rubra cell wall skeleton for extemal use improves the viability of adipogenic mesenchymal stem cells and promotes diabetes wound repair [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1038-1044. |
| [8] | Zhu Bingbing, Deng Jianghua, Chen Jingjing, Mu Xiaoling. Interleukin-8 receptor enhances the migration and adhesion of umbilical cord mesenchymal stem cells to injured endothelium [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1045-1050. |
| [9] | Fang Xiaolei, Leng Jun, Zhang Chen, Liu Huimin, Guo Wen. Systematic evaluation of different therapeutic effects of mesenchymal stem cell transplantation in the treatment of ischemic stroke [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1085-1092. |
| [10] | Guo Jia, Ding Qionghua, Liu Ze, Lü Siyi, Zhou Quancheng, Gao Yuhua, Bai Chunyu. Biological characteristics and immunoregulation of exosomes derived from mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1093-1101. |
| [11] | Kang Kunlong, Wang Xintao. Research hotspot of biological scaffold materials promoting osteogenic differentiation of bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 597-603. |
| [12] | Huang Chuanjun, Zou Yu, Zhou Xiaoting, Zhu Yangqing, Qian Wei, Zhang Wei, Liu Xing. Transplantation of umbilical cord mesenchymal stem cells encapsulated in RADA16-BDNF hydrogel promotes neurological recovery in an intracerebral hemorrhage rat model [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 510-515. |
| [13] | Wu Chengcong, Wang Fang, Wan Jianshan, Wu Zheng, Sun Rong, Huang Hefei, Qian Xuankun, Ou Hua, Ren Jing. Adenovirus-mediated bone morphogenetic protein 2 induces osteogenic differentiation of rabbit bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(30): 4757-4761. |
| [14] | Dong Yi, Shan Shuai, Liu Jialin, Han Xiangzhen, He Huiyu. Circular RNA mmu_circ_0001775 knockdown improves the osteogenic ability of mouse bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(30): 4767-4772. |
| [15] | Shen Enpu, Huang Ba, Liu Danping, Qi Hui, Wu Zhiwen, Li Beibei. Exosomes derived from melatonin-modified bone marrow mesenchymal stem cells promote osteogenesis of bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(30): 4800-4805. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||