Chinese Journal of Tissue Engineering Research ›› 2022, Vol. 26 ›› Issue (17): 2775-2781.doi: 10.12307/2022.550
Previous Articles Next Articles
Sequence of prevention for anterior cruciate ligament injury: screening, intervention and assessment
Yuan Haoxiang, Xu Jing, Zeng Jinshu, Chen Hao, Yan Yelei, Chen Jiahao, Liu Qingshan, Xu Fei
- School of Physical Education and Health, Hangzhou Normal University, Hangzhou 311122, Zhejiang Province, China
-
Received:2021-04-27Revised:2021-04-28Accepted:2021-05-27Online:2022-06-18Published:2021-12-27 -
Contact:Liu Qingshan, MD, Associate professor, School of Physical Education and Health, Hangzhou Normal University, Hangzhou 311122, Zhejiang Province, China Xu Fei, MD, Associate professor, School of Physical Education and Health, Hangzhou Normal University, Hangzhou 311122, Zhejiang Province, China -
About author:Yuan Haoxiang, Master candidate, School of Physical Education and Health, Hangzhou Normal University, Hangzhou 311122, Zhejiang Province, China Xu Jing, Master candidate, School of Physical Education and Health, Hangzhou Normal University, Hangzhou 311122, Zhejiang Province, China Yuan Haoxiang and Xu Jing contributed equally to this work. -
Supported by:the Natural Science Foundation of Zhejiang Province (General Project), No. LY18C110002 (to XF)
CLC Number:
Cite this article
Yuan Haoxiang, Xu Jing, Zeng Jinshu, Chen Hao, Yan Yelei, Chen Jiahao, Liu Qingshan, Xu Fei. Sequence of prevention for anterior cruciate ligament injury: screening, intervention and assessment[J]. Chinese Journal of Tissue Engineering Research, 2022, 26(17): 2775-2781.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
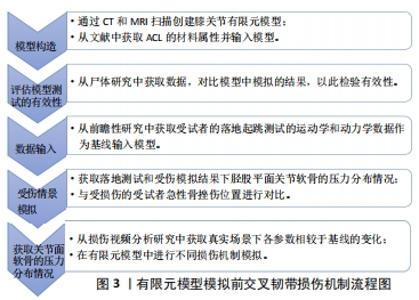

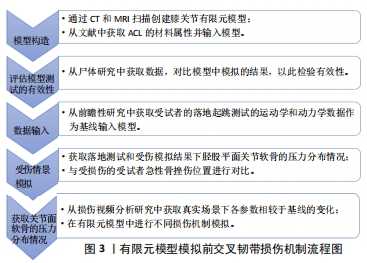
2.1 前交叉韧带损伤机制的研究 非接触性前交叉韧带损伤可能发生在最初触地的30-100 ms内,且有超过70%前交叉韧带损伤发生在运动者完成跳起、落地或侧切过程中单腿支撑改变方向的运动场景之中[12-13]。大量研究运用了各种方法试图还原或模拟损伤发生时施加在膝关节的力的位置与方向,以明确前交叉韧带损伤的内在机制,包括体内(运动者访谈法、关节镜或影像学检查法、视频分析法和实验室场景测试法等)、体外(尸体模拟研究法等)及计算机模拟研究。有团队提出一种新的研究范式(In SIM),能够弥补传统研究方法中的一些不足,但现阶段尚未广泛运用于损伤机制研究。该方法首先通过MRI、CT扫描数据在计算机中建立膝关节有限元模型并用尸体研究数据进行效度检验,以受试者在前瞻性落地测试研究中数据作为基线,见图3。"


在计算机中对受试者损伤视频研究中不同损伤机制进行模拟并获取胫股平面关节软骨的压力分布对比,最后与影像学观察到的急性期关节面挫伤类型比较验证,结果表明女性运动者在膝关节“外翻塌陷”的机制下,表现出胫骨外展伴随向前平移的同时或内旋或外旋,多个运动面的过度负载导致前交叉韧带损伤[14-15]。尽管这种将实验室场景测试数据、尸体实验数据和计算机有限元模型结合分析损伤机制的方法具有诸多优点,但未能充分考虑到模型中关节软组织材料属性的个体差异,故可能会影响关节动力学的模拟参数结果[16]。建议未来有限元模型中加入更多类型场地测试(侧切、急停跳和落地起跳等)数据作为基线,建立具有个体解剖学特征的膝关节模型,模拟或预测损伤的内在机制和危险因素时更加有效。 2.2 病因学分析"
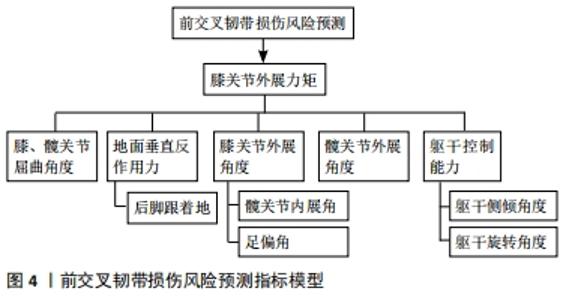
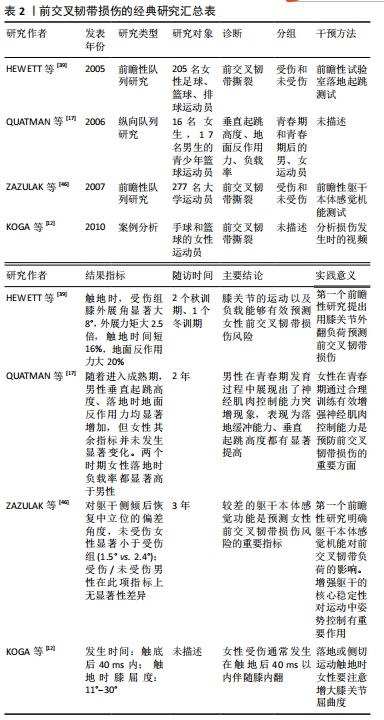
2.2.1 神经肌肉与生物力学因素 女性运动者前交叉韧带损伤率是男性的2-6倍,其中进入青春期后(16-18岁)性别差异达到最大[3]。男性进入青春期后力量、爆发力和协调性都自然地发生适应性增强,迎来了神经肌肉发展突增期,垂直跳跃高度、落地时的缓冲能力都显著增强[17],但女性未观察到明显变化。这提示青春期女性发育过程中运动系统可能无法满足身高体质量迅速增长而产生更大负荷的要求,出现神经肌肉控制能力不足现象[18],增加了前交叉韧带损伤风险。 不同性别膝关节处屈肌与伸肌的协同收缩模式也有较大差异。有研究对比了不同角速度的等速测试中男女腘绳肌与股四头肌力矩比(hamstring quadriceps ratio,H/Q),结果男性膝关节以较高角速度运动时H/Q显著增加,提示男性可能是通过增强腘绳肌收缩克服胫骨前移的惯性作用,提高膝关节的动态稳定性,但女性H/Q无显著变化[19]。另一项研究对女性运动者在不同高度进行落地起跳测试,发现随高度增加,股四头肌激活显著增强但腘绳肌未有明显变化[20],表明女性承受较大落地负荷时倾向于采用增强股四头肌激活的控制模式,在矢状面上对前交叉韧带产生较大负载。在侧切运动测试中,男性在变向触地时以股内侧肌激活为主,而女性则采用增强股外侧肌激活的策略[21],并且由于内侧腘绳肌激活较弱,加大了女性膝关节在额状面上的外展角度,这种膝关节控制肌群协同收缩模式的差异部分解释了女性更易出现“外翻塌陷”姿势的原因。另一方面,青春发育过程中男性髋关节标准化后的外展力矩增加显著,但女性未表现类似特点且成年后外展力矩峰值比男性更低[22-23]。女性较弱的髋关节外展肌力会增大膝关节外展角度,因此落地时更易出现错误的下肢姿势。青春发育过程中,不同性别髋关节与膝关节处的神经肌肉募集方式差异形成的原因目前尚不清楚。 2.2.2 激素 前交叉韧带上存在性别相关的激素受体,包括雌激素、睾酮和松弛素等,这些激素能够影响骨、肌肉和胶原蛋白的生理特性[24]。有研究对女性的月经周期进行观察,发现在卵泡的形成期和排卵期,激素的周期性波动可能会影响前交叉韧带的力学特性、降低关节松弛度和减小肌力[25-26],而排卵前期是前交叉韧带损伤风险最高的阶段[27]。值得注意的是,以往研究表明正常月经周期与相对稳定激素水平(口服避孕药)的女性相比,在高风险运动中对膝关节或髋关节负荷并无显著性差异[28-29],因此不同的受伤率更可能是由于力量、神经肌肉协调性或韧带的力学特性等方面的差异所引起的。目前,与女性月经周期相关的激素对前交叉韧带损伤风险的继发影响以及如何改变这些影响的方案尚不清楚。 2.2.3 伤病史 研究表明前交叉韧带重建后运动者二次损伤率约为15%,其中25岁以下运动者风险更高(23%)[30],这提示前交叉韧带再次受伤风险存在明显的年龄差异,但对于其内在机制研究尚不深入。而女性运动者下肢同侧、对侧发生二次损伤的风险分别是男性的4倍和6倍[31],提示女性二次损伤风险不仅远高于男性,并且健侧肢的风险更大。这可能是由于伤后运动者更倾向于健侧肢承重,产生负荷过载,表现出下肢负荷不对称现象。这种异常运动模式在前交叉韧带重建后两年仍可能持续存在[32-33]。综上所述,姿势控制能力、膝关节稳定性以及下肢不对称是运动者前交叉韧带二次损伤的重要潜在风险。 2.2.4 遗传 现阶段,大多数研究认为与Ⅰ,Ⅴ和Ⅶ型胶原蛋白(COL1A1,COL5A1和COL12A1)以及基质金属蛋白酶(MMP10,MMP1,MMP3和MMP12)合成有关的基因可能是前交叉韧带损伤的潜在因素[34-35]。但有研究检验了与胶原蛋白合成相关的6个点突变后,发现结果与上述观点并不一致[36],另一项病例对照研究对全基因组测序后也未发现与前交叉韧带损伤显著相关的点突变[37],这说明尽管前交叉韧带损伤可能存在基因易感性并且遗传度达到了较高的69%[38],但因其临床意义尚不明确且研究中有诸多试验伦理学方面的制约,想要针对个体特点基因编辑的预防策略现阶段并不可行。未来的研究中建议增加前瞻性研究的样本量并纳入更多高质量的同质性数据,进一步探究遗传因素与前交叉韧带损伤的关系。 2.3 前交叉韧带损伤的预测与筛查 2.3.1 风险预测指标 近20年,有多项研究对超过3 000例运动者的下肢生物力学特征和神经肌肉控制能力进行测量并跟踪调查,以探究前交叉韧带损伤与各风险因素之间的联系,见图4。"
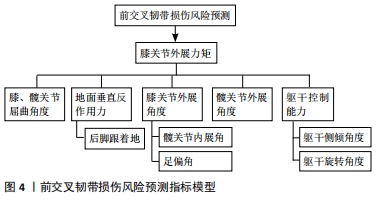

一项经典的前瞻性研究表明,女性膝关节外展力矩在预测前交叉韧带损伤时表现出较高的敏感性78%和特异性73%,并且它与膝关节外展角度和垂直地面反作用力有显著相关性[39]。在侧切运动中,膝关节屈曲角度较小且以足跟触地的运动者发生前交叉韧带损伤的概率显著高于控制组[40],尽管后足触地模式相对前足触地的运动者产生的膝关节外翻力矩和地面反作用力更大[41-42],但目前仍缺乏作为损伤预测指标的直接证据。现阶段普遍认为膝关节外展力矩是预测前交叉韧带损伤的重要指标,大多数筛查工具也围绕评估或预测膝关节外展力矩展开设计。有一项横断面研究提出髋关节外展角度峰值能够作为独立预测膝关节外展力矩的显著性指标[43],这表明女性运动者在侧切运动中更易表现出较大膝关节外展角度的机制可能是通过增大髋关节冠状面运动实现的。 此外,运动者膝关节的外展力矩不仅会受到躯干和髋关节冠状面运动幅度的间接影响[44],足偏角也可能会影响膝关节外展角度从而改变外展力矩[45]。有研究指出在外力作用后,运动者依靠其本体感觉重新恢复躯干原位置时,出现的偏差角度每增大1°,膝关节韧带及半月板损伤的概率就增加3.3倍[46],因此在高危风险运动中躯干侧倾角度能辅助预测前交叉韧带损伤。值得注意的是,在以往认知中,使上半身保持竖直能够在减速过程中增加肌肉的离心收缩做功,被认为是有效吸收负荷的减速策略。研究表明侧切运动中髋关节屈曲力矩、躯干前屈对膝关节外展力矩表现出较好的预测能力[43, 47]。但目前使用髋关节屈曲角度作为预测膝关节外展负荷指标的证据尚不充分,未来需要对这一特征参数与膝关节的外展力矩的关系进一步探究,这对于开发简易筛查、评估工具具有重要意义。 2.3.2 筛查工具 开发评估工具来识别前交叉韧带损伤高风险的运动者将有助于临床医生筛选出从干预中获益最多的人群。现阶段,大多数研究人员在进行高风险运动者人群筛查时常采用实验室场景测试,即利用三维捕捉系统、测力台和肌电对运动者侧切、落地起跳和急停跳等运动中个体生物力学特征进行测量,随后评估触地时膝关节外翻力矩、外展角度等前交叉韧带损伤的重要预测因子,但由于实验室设备较为昂贵且后期处理数据耗时耗力,不便在场地测试中大规模应用。有团队开发了一套便捷且低成本的筛查工具,它能够快速开展测试,对识别膝关节外展力矩异常的人群具有较高的敏感性(73%)和特异性(70%)[48]。这套评测工具由体重秤、标准量尺、摄像机、Image J软件和等速测力计共同组成,分别对胫骨长度、膝关节外翻运动位移、膝关节屈曲活动度、体质量以及Q/H值进行测量后,运用回归诺模图(Nomogram)对运动者前交叉韧带损伤风险进行量化评分,在预测个体的膝关节外展力矩时准确率超过了75%。然而,该工具无法评估运动者在其他特定运动场景中的受伤风险,并且未能将激素、伤病史、神经肌肉控制能力纳入评估体系。未来可能需要从损伤的病因学出发,构建更加细致的筛查流程。目前来看,将其纳入损伤预防程序能够帮助专业人员有效识别、分类高风险运动者,对制定针对性干预训练计划具有重要意义。目前关于前交叉韧带损伤诊断的研究,见表2。"


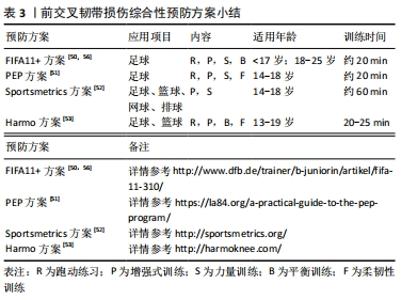
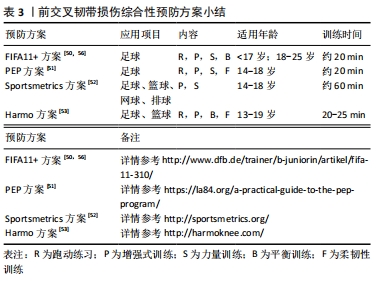
这些训练计划通常由力量训练、灵敏性训练、增强式训练、跑动练习、平衡训练以及柔韧性训练共同构成。从应用形式上看,综合性预防方案大多以热身训练的方式嵌入比赛期,时长为20-60 min,有些训练方案分级设置内容,以适应不同竞技水平和处于不同训练周期的运动者。有研究已经证实了以上综合性预防方案能够有效减小特定年龄段、运动项目运动者的伤病发生率,但目前其作用机制的研究证据尚不充足。 对于不同个体运动者,在高风险运动场景下表现出的风险因素也可能是不同的。因此,在设计干预训练计划时,应首先明确个体在运动中所暴露出来的神经肌肉控制能力缺陷的具体内容,其次再根据不同项目特点、个体特点调整相应训练方法的比例,有效改善运动者的高风险因素。尽管已有一些研究讨论了不同干预训练方式对改善高风险运动中运动者神经肌肉控制能力以及生物力学特征的效果,但结果还存在一些矛盾。在一项探究落地任务中预防训练对运动者下肢生物力学因素影响的系统综述中指出,大部分包含增强式训练为主的干预方案能够有效降低膝关节触地时屈度、减小膝关节外展力矩,但垂直地面反作用力和相关风险指标并无显著变化[54],而在侧切运动测试中,平衡训练和技巧优化训练被认为是减小膝关节负荷的有效策略[55],在此过程中要求教练员不断运用语言、视频等形式的反馈信息,及时纠正运动者的错误动作。提示教练员需要依据不同高风险运动场景在专项中比例设计训练内容,帮助建立正确的动作模式。另外,在探究前交叉韧带损伤风险的研究设计中建议加入急停跳、侧切等测试任务并综合评定不同训练方式对损伤预防的作用。未来需要纳入大样本量、包含合理对照组的前瞻性研究,在理解不同训练方式改善运动者风险因素内在机制的基础上,设计针对不同运动项目、人群的特定训练方案,继续探究不同训练方式对降低前交叉韧带损伤率效果的有效性。 对于神经肌肉训练能够有效减小前交叉韧带损伤风险的最佳干预训练周期以及是否应需要将干预训练独立安排在赛季期之外依旧存在争议。一项Meta分析表明,神经肌肉训练与前交叉韧带损伤率存在剂量效应关系 [57]。有研究对运动者进行4周的神经肌肉训练,但在侧切运动中,受试者触地时膝关节屈度、地面反作用力均未发生显著变化[58],多数研究通常设置6周的干预训练周期。然而,MYER等[59]设置了7周的干预训练,运动者的膝关节外展角度虽然有所降低,但并没有回到与对照组一致的水平。建议未来在设计干预实验时应纳入控制组,并且理想的神经肌肉训练周期至少需要持续6-8周。另有证据表明,在赛季期内加入预防训练内容,无法有效降低女性前交叉韧带受伤风险[60]。一方面可能是由于运动者赛季期内大部分训练时间都致力于提升运动表现,对预防训练内容安排的比例不够;另一方面可能由于训练周期较短且针对性不强,无法对运动者产生有效刺激,故效果不佳。因此,未来教练员应提高对预防训练的重视程度,并将其融入赛季前和赛季中的训练计划,更有助于降低前交叉韧带损伤风险。 2.4.2 干预时机的选择 青春期前或青春期早期是降低女性运动者前交叉韧带损伤风险的关键阶段。在此时期,综合性的神经肌肉训练不仅能够发展青少年的健康适能和运动技能水平[61],还可能会诱导女性运动者“神经肌肉控制突增”现象[62-63]。在以往研究中,出于对青少年身体长期发展的考虑,加入力量训练的最佳年龄尚不确定。大多数初高中女生因为缺乏场地器械等客观原因和不重视等主观因素,参与力量训练的比例也远小于男生。然而,力量训练是神经肌肉综合训练的基础,只要抗阻训练是在专业人员指导下采取符合相应年龄的技术练习并严格遵循安全指南,就能够保证训练安全有效地实施,这对预防损伤具有重要意义[64]。现阶段对于青春期前后引入神经肌肉综合训练的最佳干预时间尚未清晰界定,但建议教练员尽早在训练中融入符合运动者年龄特点的神经肌肉训练,重视力量训练在青少年训练中的正确应用。 2.4.3 评估干预措施有效性的工具 为了对神经肌肉训练计划实施的有效性做出客观判断并提供反馈,需要一款准确且能有效评估运动者高危风险的评估工具。目前,临床上常用星形平衡测试、功能性跳跃测试、Biodex Stabilometer测试[65]、等速测力仪等工具对运动者下肢肌力、动态稳定性、单侧下肢姿势控制能力和下肢不对称性进行评估。尽管此类测试能一定程度反映下肢运动机能,但在神经肌肉训练过程中,需要对前交叉韧带损伤特定风险因素的改善效果作出相应评估时,大多就无法满足了。前文介绍的一款筛查工具可以脱离实验室环境对膝关节外展力矩作出较准确预测,可用于落地起跳测试中前交叉韧带损伤高风险因素的排查。而在运动训练实践中,教练员需要经常对运动者的练习效果进行即时或阶段性评估以提供针对性指导,就需要一款简单易行的评估工具。而目前常用的简易定性评估量表大多应用于下肢损伤的康复领域,未能全面引入前交叉韧带损伤预防进程之中。“落地危险评分系统”(Landing Error Scoring System,LESS)、“抱膝跳评估” (Tuck Jump Assessment,TJA)和“QASLS评分系统”(Qualitative Analysis of Single Leg Loading)能够帮助教练员快速筛查高风险人群和评估干预训练效果[66-68],见表4。"
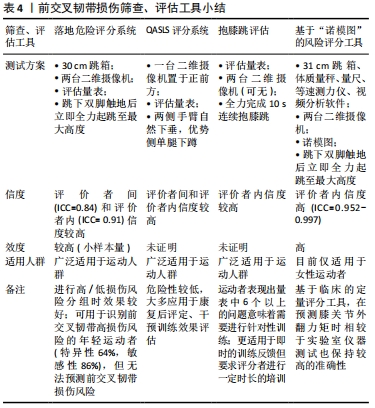


LESS评分系统是3者中惟一初步被证明过效度的工具,它能够对落地起跳时下肢出现的错误姿势分级评分,内容上也较为全面,目前应用相对广泛;“抱膝跳评估”工具允许教练员独自对个体前交叉韧带损伤风险进行评估(评分者内信度:0.84),分别从膝关节与髋关节的运动、触地时双脚位置以及连续跳跃的落地技术3个方面进行综合评估,故更适用于训练中即时的评估反馈,优化运动者的落地技巧;QASLS通过视频分析受试者在单腿下蹲时身体各部分的表现,以一种危险性较小且信度满足临床同类标准的方式对单侧膝关节负荷作出判断。但是,此3款工具对于预防前交叉韧带损伤的效度尚未进行大样本量的前瞻性研究。未来应结合前交叉韧带损伤机制,开发出更多能在特定测试场景中(如侧切运动和急停起跳等)评估下肢高风险因素的临床评估工具,并且还需要重新评估它们预测损伤风险的信效度。"

| [1] KAEDING CC, LÉGER-ST-JEAN B, MAGNUSSEN RA. Epidemiology and diagnosis of anterior cruciate ligament injuries. Clin Sports Med. 2017;36(1):1-8. [2] RENSTRÖM PA. Eight clinical conundrums relating to anterior cruciate ligament (ACL) injury in sport: recent evidence and a personal reflection. Br J Sports Med. 2013;47(6):367-372. [3] MUSAHL V, KARLSSON J. Anterior cruciate ligament tear. N Engl J Med. 2019; 380(24):2341-2348. [4] CUMPS E, VERHAGEN E, ANNEMANS L, et al. Injury rate and socioeconomic costs resulting from sports injuries in Flanders: data derived from sports insurance statistics 2003. Br J Sports Med. 2008;42(9):767-772. [5] LIEN-IVERSEN T, MORGAN DB, JENSEN C, et al. Does surgery reduce knee osteoarthritis, meniscal injury and subsequent complications compared with non-surgery after ACL rupture with at least 10 years follow-up? A systematic review and meta-analysis. Br J Sports Med. 2020;54(10):592-598. [6] LAI CCH, ARDERN CL, FELLER JA, et al. Eighty-three per cent of elite athletes return to preinjury sport after anterior cruciate ligament reconstruction: a systematic review with meta-analysis of return to sport rates, graft rupture rates and performance outcomes. Br J Sports Med. 2018;52(2):128-138. [7] MOHTADI NG, CHAN DS. Return to sport-specific performance after primary anterior cruciate ligament reconstruction: a systematic review. Am J Sports Med. 2018;46(13):3307-3316. [8] LOHMANDER LS, ENGLUND PM, DAHL LL, et al. The long-term consequence of anterior cruciate ligament and meniscus injuries: osteoarthritis. Am J Sports Med. 2007;35(10):1756-1769. [9] WANG LJ, ZENG N, YAN ZP, et al. Post-traumatic osteoarthritis following ACL injury. Arthritis Res Ther. 2020;22(1):57. [10] VAN MECHELEN W, HLOBIL H, KEMPER HC. Incidence, severity, aetiology and prevention of sports injuries. A review of concepts. Sports Med, 1992;14(2):82-99. [11] MEEUWISSE WH, TYREMAN H, HAGEL B, et al. A dynamic model of etiology in sport injury: the recursive nature of risk and causation. Clin J Sport Med. 2007; 17(3):215-219. [12] KOGA H, NAKAMAE A, SHIMA Y, et al. Mechanisms for noncontact anterior cruciate ligament injuries: knee joint kinematics in 10 injury situations from female team handball and basketball. Am J Sports Med. 2010;38(11):2218-25. [13] JOHNSTON JT, MANDELBAUM BR, SCHUB D, et al. Video analysis of anterior cruciate ligament tears in professional american football athletes. Am J Sports Med. 2018;46(4):862-868. [14] QUATMAN CE, KIAPOUR A, MYER GD, et al. Cartilage pressure distributions provide a footprint to define female anterior cruciate ligament injury mechanisms. Am J Sports Med. 2011;39(8):1706-1713. [15] KIAPOUR AM, DEMETROPOULOS CK, KIAPOUR A, et al. Strain response of the anterior cruciate ligament to uniplanar and multiplanar loads during simulated landings: implications for injury mechanism. Am J Sports Med. 2016;44(8):2087-2096. [16] KIAPOUR A, KIAPOUR AM, KAUL V, et al. Finite element model of the knee for investigation of injury mechanisms: development and validation. J Biomech Eng. 2014;136(1):011002. [17] QUATMAN CE, FORD KR, MYER GD, et al. Maturation leads to gender differences in landing force and vertical jump performance: a longitudinal study. Am J Sports Med. 2006;34(5):806-813. [18] DISTEFANO LJ, MARTINEZ JC, CROWLEY E, et al. Maturation and sex differences in neuromuscular characteristics of youth athletes. J Strength Cond Res. 2015; 29(9):2465-2473. [19] HEWETT TE, MYER GD, ZAZULAK BT. Hamstrings to quadriceps peak torque ratios diverge between sexes with increasing isokinetic angular velocity. J Sci Med Sport. 2008;11(5):452-459. [20] FORD KR, MYER GD, SCHMITT LC, et al. Preferential quadriceps activation in female athletes with incremental increases in landing intensity. J Appl Biomech. 2011;27(3):215-222. [21] BEAULIEU ML, LAMONTAGNE M, XU L. Lower limb muscle activity and kinematics of an unanticipated cutting manoeuvre: a gender comparison. Knee Surg Sports Traumatol Arthrosc. 2009;17(8):968-976. [22] BRENT JL, MYER GD, FORD KR, et al. The effect of sex and age on isokinetic hip-abduction torques. J Sport Rehabil. 2013;22(1):41-46. [23] SUGIMOTO D, MATTACOLA CG, MULLINEAUX DR, et al. Comparison of isokinetic hip abduction and adduction peak torques and ratio between sexes. Clin J Sport Med. 2014;24(5):422-428. [24] RENSTROM P, LJUNGQVIST A, ARENDT E, et al. Non-contact ACL injuries in female athletes: an International Olympic Committee current concepts statement. Br J Sports Med. 2008;42(6):394-412. [25] HERZBERG SD, MOTU’APUAKA ML, Lambert W, et al. The effect of menstrual cycle and contraceptives on acl injuries and laxity: a systematic review and meta-analysis. Orthop J Sports Med. 2017;5(7):2325967117718781. [26] WEIDAUER L, ZWART MB, CLAPPER J, et al. Neuromuscular performance changes throughout the menstrual cycle in physically active females. J Musculoskelet Neuronal Interact. 2020;20(3):314-324. [27] BALACHANDAR V, MARCINIAK JL, WALL O, et al. Effects of the menstrual cycle on lower-limb biomechanics, neuromuscular control, and anterior cruciate ligament injury risk: a systematic review. Muscles Ligaments Tendons J. 2017;7(1):136-146. [28] CHAUDHARI AM, LINDENFELD TN, ANDRIACCHI TP, et al. Knee and hip loading patterns at different phases in the menstrual cycle: implications for the gender difference in anterior cruciate ligament injury rates. Am J Sports Med. 2007;35(5): 793-800. [29] LEGERLOTZ K, BEY M E, GÖTZ S, et al. Constant performance in balance and proprioception tests across the menstrual cycle - a pilot study in well trained female ice hockey players on hormonal contraception. Health Sci Rep. 2018;1(1):e18. [30] WIGGINS AJ, GRANDHI RK, SCHNEIDER DK, et al. Risk of secondary injury in younger athletes after anterior cruciate ligament reconstruction: a systematic review and meta-analysis. Am J Sports Med. 2016;44(7):1861-1876. [31] PATERNO MV, WEED AM, HEWETT TE. A between sex comparison of anterior-posterior knee laxity after anterior cruciate ligament reconstruction with patellar tendon or hamstrings autograft: a systematic review. Sports Med. 2012;42(2):135-152. [32] PATERNO MV, SCHMITT LC, FORD KR, et al. Effects of sex on compensatory landing strategies upon return to sport after anterior cruciate ligament reconstruction. J Orthop Sports Phys Ther. 2011;41(8):553-559. [33] PATERNO MV, FORD KR, MYER GD, et al. Limb asymmetries in landing and jumping 2 years following anterior cruciate ligament reconstruction. Clin J Sport Med. 2007;17(4):258-262. [34] KAYNAK M, NIJMAN F, VAN MEURS J, et al. Genetic Variants and Anterior Cruciate Ligament Rupture: A Systematic Review. Sports Med. 2017;47(8):1637-1650. [35] LULIŃSKA E, GIBBON A, KACZMARCZYK M, et al. Matrix Metalloproteinase Genes (MMP1, MMP10, MMP12) on Chromosome 11q22 and the Risk of Non-Contact Anterior Cruciate Ligament Ruptures. Genes (Basel). 2020;11(7):766. [36] SIVERTSEN EA, HAUG KBF, KRISTIANSLUND EK, et al. No association between risk of anterior cruciate ligament rupture and selected candidate collagen gene variants in female elite athletes from high-risk team sports. Am J Sports Med. 2019;47(1):52-58. [37] KIM SK, ROOS TR, ROOS AK, et al. Genome-wide association screens for Achilles tendon and ACL tears and tendinopathy. PLoS One. 2017;12(3):e0170422. [38] MAGNUSSON K, TURKIEWICZ A, HUGHES V, et al. High genetic contribution to anterior cruciate ligament rupture: heritability ~69. Br J Sports Med. 2021;55(7):385-389. [39] HEWETT TE, MYER GD, FORD KR, et al. Biomechanical measures of neuromuscular control and valgus loading of the knee predict anterior cruciate ligament injury risk in female athletes: a prospective study. Am J Sports Med. 2005;33(4):492-501. [40] MONTGOMERY C, BLACKBURN J, WITHERS D, et al. Mechanisms of ACL injury in professional rugby union: a systematic video analysis of 36 cases. Br J Sports Med. 2018;52(15):994-1001. [41] DONNELLY CJ, CHINNASEE C, WEIR G, et al. Joint dynamics of rear- and fore-foot unplanned sidestepping. J Sci Med Sport. 2017;20(1):32-37. [42] DAVID S, KOMNIK I, PETERS M, et al. Identification and risk estimation of movement strategies during cutting maneuvers. J Sci Med Sport. 2017;20(12):1075-1080. [43] WEIR G, ALDERSON J, SMAILES N, et al. A reliable video-based ACL injury screening tool for female team sport athletes. Int J Sports Med. 2019;40(3):191-199. [44] KRISTIANSLUND E, FAUL O, BAHR R, et al. Sidestep cutting technique and knee abduction loading: implications for ACL prevention exercises. Br J Sports Med. 2014;48(9):779-783. [45] SIGWARD SM, POWERS CM. Loading characteristics of females exhibiting excessive valgus moments during cutting. Clin Biomech (Bristol, Avon). 2007;22(7):827-833. [46] ZAZULAK BT, HEWETT TE, REEVES NP, et al. The effects of core proprioception on knee injury: a prospective biomechanical-epidemiological study. Am J Sports Med. 2007;35(3):368-373. [47] MCBURNIE A, DOS’ SANTOS T, JONES PA. Biomechanical associates of performance and knee joint loads during a 70–90° cutting maneuver in sub-elite soccer players. J Strength Cond Res. 2019. doi: 10.1519/JSC.0000000000003252. [48] MYER GD, BRENT JL, FORD KR, et al. Real-time assessment and neuromuscular training feedback techniques to prevent ACL injury in female athletes. Strength Cond J. 2011;33(3):21-35. [49] DARGO L, ROBINSON K J, GAMES KE. Prevention of knee and anterior cruciate ligament injuries through the use of neuromuscular and proprioceptive training: an evidence-based review. J Athl Train. 2017;52(12):1171-1172. [50] SILVERS-GRANELLI HJ, BIZZINI M, ARUNDALE A, et al. Does the FIFA 11+ injury prevention program reduce the incidence of ACL injury in male soccer players? Clin Orthop Relat Res. 2017;475(10):2447-2455. [51] MANDELBAUM BR, SILVERS HJ, WATANABE DS, et al. Effectiveness of a neuromuscular and proprioceptive training program in preventing anterior cruciate ligament injuries in female athletes: 2-year follow-up. Am J Sports Med. 2005;33(7):1003-1010. [52] HEWETT TE, LINDENFELD TN, RICCOBENE JV, et al. The effect of neuromuscular training on the incidence of knee injury in female athletes. A prospective study. Am J Sports Med. 1999;27(6):699-706. [53] KIANI A, HELLQUIST E, AHLQVIST K, et al. Prevention of soccer-related knee injuries in teenaged girls. Arch Intern Med. 2010;170(1):43-49. [54] LOPES TJA, SIMIC M, MYER GD, et al. The effects of injury prevention programs on the biomechanics of landing tasks: a systematic review with meta-analysis. Am J Sports Med. 2018;46(6):1492-1499. [55] DOS’SANTOS T, THOMAS C, COMFORT P, et al. The effect of training interventions on change of direction biomechanics associated with increased anterior cruciate ligament loading: a scoping review. Sports Med. 2019;49(12):1837-1859. [56] SOLIGARD T, MYKLEBUST G, STEFFEN K, et al. Comprehensive warm-up programme to prevent injuries in young female footballers: cluster randomised controlled trial. BMJ. 2008;337:a2469. [57] SUGIMOTO D, MYER GD, BARBER FOSS KD, et al. Critical components of neuromuscular training to reduce ACL injury risk in female athletes: meta-regression analysis. Br J Sports Med. 2016;50(20):1259-1266. [58] YANG C, YAO W, GARRETT WE, et al. Effects of an intervention program on lower extremity biomechanics in stop-jump and side-cutting tasks. Am J Sports Med. 2018;46(12):3014-3022. [59] MYER GD, FORD KR, BRENT JL, et al. Differential neuromuscular training effects on ACL injury risk factors in”high-risk” versus “low-risk” athletes. BMC Musculoskelet Disord. 2007;8:39. [60] KLUGMAN MF, BRENT JL, MYER GD, et al. Does an in-season only neuromuscular training protocol reduce deficits quantified by the tuck jump assessment? Clin Sports Med. 2011;30(4):825-840. [61] FAIGENBAUM AD, FARRELL A, FABIANO M, et al. Effects of integrative neuromuscular training on fitness performance in children. Pediatr Exerc Sci. 2011;23(4):573-584. [62] MYER GD, FAIGENBAUM AD, FORD KR, et al. When to initiate integrative neuromuscular training to reduce sports-related injuries and enhance health in youth? Curr Sports Med Rep. 2011;10(3):155-166. [63] HOPPER AJ, HAFF EE, JOYCE C, et al. Neuromuscular training improves lower extremity biomechanics associated with knee injury during landing in 11-13 year old female netball athletes: a randomized control study. Front Physiol. 2017;8:883. [64] ZWOLSKI C, QUATMAN-YATES C, PATERNO MV. Resistance training in youth: laying the foundation for injury prevention and physical literacy. Sports Health. 2017;9(5):436-443. [65] PATERNO MV, SCHMITT LC, FORD KR, et al. Biomechanical measures during landing and postural stability predict second anterior cruciate ligament injury after anterior cruciate ligament reconstruction and return to sport. Am J Sports Med. 2010;38(10):1968-1078. [66] PADUA DA, DISTEFANO LJ, BEUTLER AI, et al. The landing error scoring system as a screening tool for an anterior cruciate ligament injury-prevention program in elite-youth soccer athletes. J Athl Train. 2015;50(6):589-595. [67] MYER GD, FORD KR, HEWETT TE. Tuck jump assessment for reducing anterior cruciate ligament injury risk. Athl Ther Today. 2008;13(5):39-44. [68] ALMANGOUSH A, HERRINGTON L, JONES R. A preliminary reliability study of a qualitative scoring system of limb alignment during single leg squat. Phys Ther Rehabil. 2014;1(1):2. |
| [1] | Feng Ziyi, Liang Shanshan, Yu Weiting, Wang Ruoyu. Culture, research and application of patient-derived tumor organoids [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 4082-4088. |
| [2] | Ni Jinghua, Luo Jia, Jiang Sen, Li Heng, Zhu Jianzhong. Application and prospect of induced pluripotent stem cells in tumor diseases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(13): 2127-2132. |
| [3] |
Li Ningxin, Yang Zhaohui.
In-depth discussion on the treatment of terrible triad of the elbow |
| [4] | Luo Hong1, Liu Fang1, Li Shunhua1, Qiu Bing1, Liu Fuyao1, Zhang Yu2, Ma Limin3. Significance of gait analysis in the diagnosis of anterior cruciate ligament injury [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(31): 4969-4973. |
| [5] | Zhuan Hang, Zheng Guoxia, Wang Yunhua. Advantages and application prospects of microfluidic chip technology in cell adhesion research [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(22): 3584-3590. |
| [6] | Yang Peng-cheng, Qi Yan, Zhang Dong-hui. Research advance, bottlenecks and challenges of microarray of micro organs [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(32): 5234-5240. |
| [7] | Hun Ting-ting, Qiu Chang-jun, Zhao Ying-tong, Zhao Feng, He Jing-wen, Sun Yan. Latest advances in high-throughput cell capture and arrangement [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(17): 2783-2788. |
| [8] | Lin Qing-keng, Yin De-hong, Liu Ju-fen, Zhang Xue-juan, Bai Ying-ying, Song Yi-jia, Pan Xing-hua, Liu-Gao Mi-yang. Exosomes from human umbilical cord mesenchymal stem cells at passage 2 and 5: a comparative study on microRNA profiles [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(17): 2686-2691. |
| [9] | Feng Rui-cheng, Lang Yan-he, Liang Yang, Wu Ying, Teng Chun-bo. Identification of marker molecules for negative screening of pancreatic stem cells [J]. Chinese Journal of Tissue Engineering Research, 2013, 17(10): 1785-1792. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||