Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (24): 3918-3924.doi: 10.3969/j.issn.2095-4344.2754
Previous Articles Next Articles
Meta-analysis of independent risk factors for surgical site infection after spinal surgery
Qin Zuoheng, Li Lijun, Ni Dongkui
- Department of Orthopedics, Second Hospital of Tianjin Medical University, Tianjin 300211, China
-
Received:2019-11-20Revised:2019-11-29Accepted:2020-01-06Online:2020-08-28Published:2020-08-17 -
Contact:Ni Dongkui, Master, Associate professor, Chief physician, Department of Orthopedics, Second Hospital of Tianjin Medical University, Tianjin 300211, China -
About author:Qin Zuoheng, Master, Physician, Department of Orthopedics, Second Hospital of Tianjin Medical University, Tianjin 300211, China
CLC Number:
Cite this article
Qin Zuoheng, Li Lijun, Ni Dongkui. Meta-analysis of independent risk factors for surgical site infection after spinal surgery[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(24): 3918-3924.
share this article
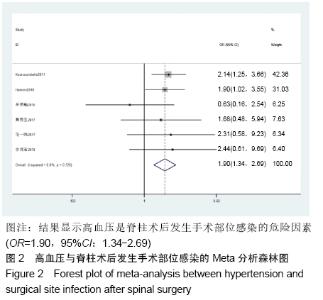
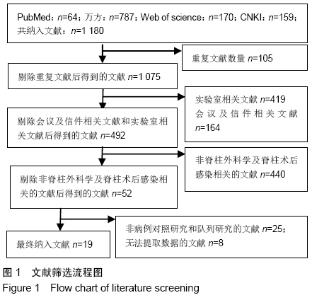
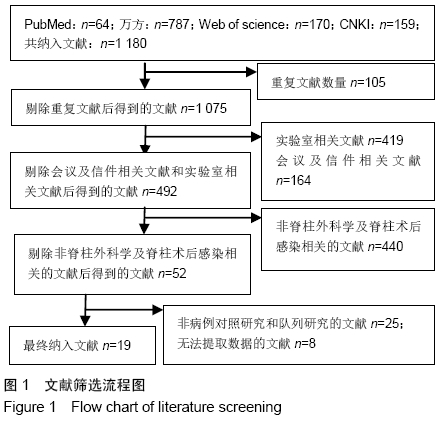
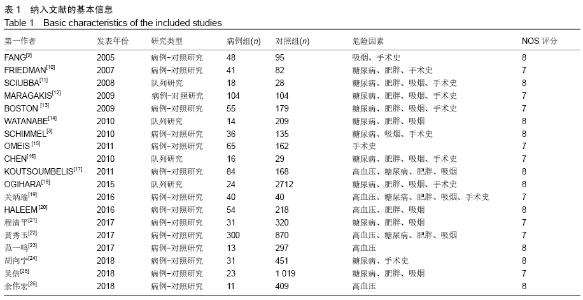
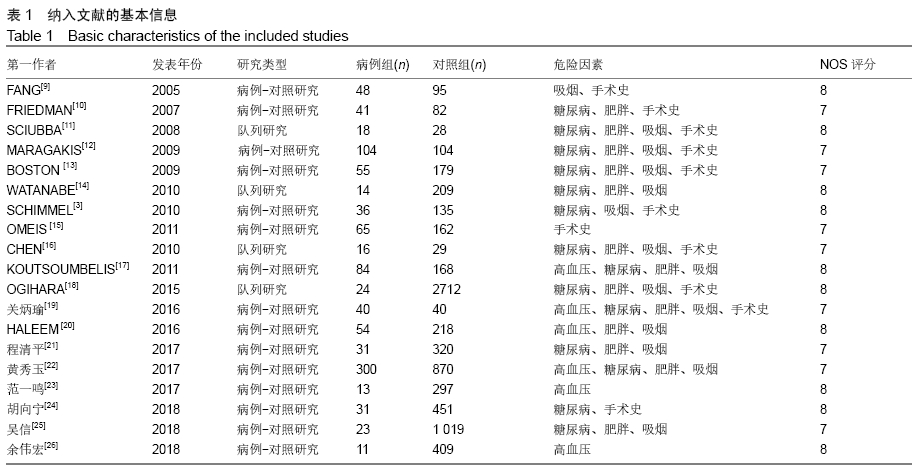
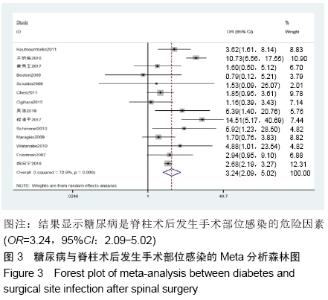
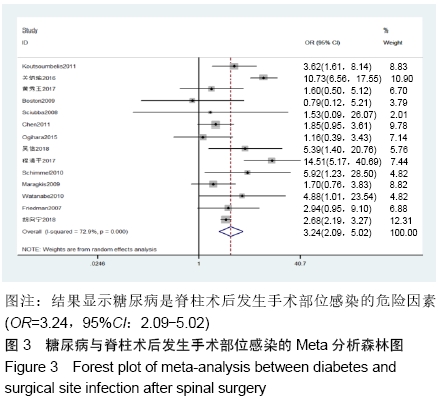
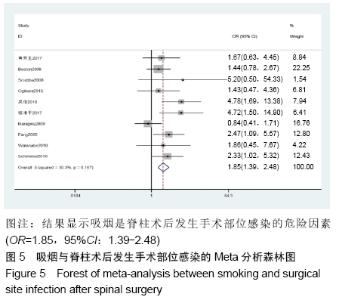
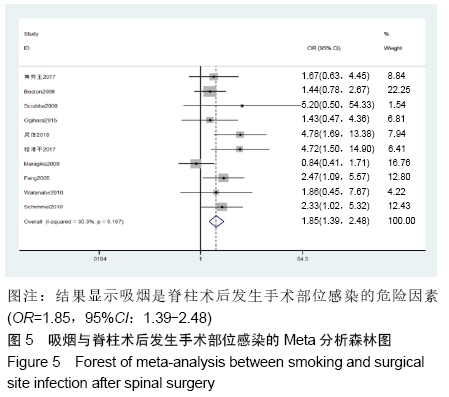
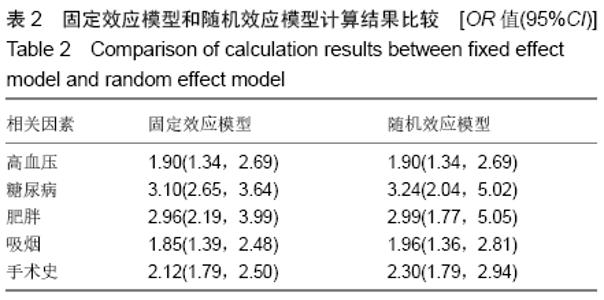
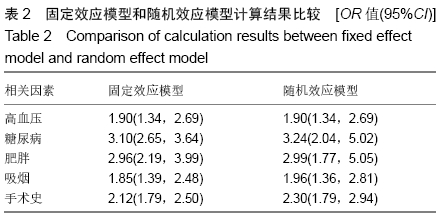
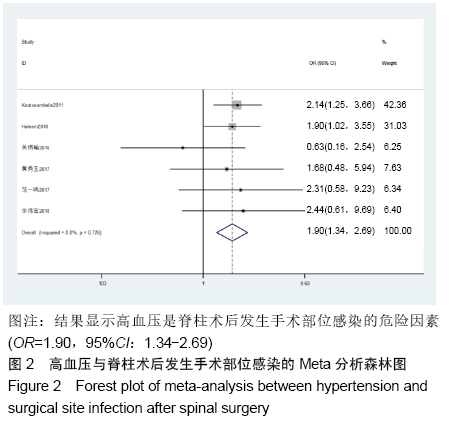
高血压[4]:在未使用降压药物的情况下,非同日3次测量诊室血压,收缩压≥140 mm Hg(1 mm Hg=0.133 kPa)和(或)舒张压≥90 mm Hg。 糖尿病[5]:①患者有糖尿病典型症状,空腹血糖≥ 7.0 mmol/L,或餐后2 h血糖≥11.1 mmol/L;②患者没有糖尿病典型症状,空腹血糖≥7.0 mmol/L或者餐后2 h血 糖≥11.1 mmol/L,应该再重复1次,仍然达到以上值,可以确诊为糖尿病患者;③患者没有糖尿病典型症状,空腹血糖≥7.0 mmol/L或者餐后2 h血糖≥11.1 mmol/L,口服葡萄糖耐量试验结果显示餐后2 h血糖≥11.1 mmol/L,可确诊为糖尿病患者。 肥胖[6]:体质量指数≥30 kg/m2。 吸烟[7]:定义为以前吸烟、现在吸烟及曾经吸烟,并且现在吸烟和以前吸烟均视为曾经吸烟。 手术史:此次研究纳入的研究对象包括既往脊柱手术史和非脊柱手术的外科手术史。 手术部位感染[8]:术后30 d内(或者置入内固定装置1年内)发生的浅表、深部或者器官的感染。浅部感染指术后30 d内发生感染,感染只涉及切口皮肤或皮下组织。深部感染指若无植入物留在原位,感染发生在术后30 d内;若植入物在原位,感染发生在1年内,并且感染可能与手术有关,深部感染涉及深部软组织。当感染涉及解剖的任何部分(如器官或空间)而非手术操作的切口感染即为器官感染。 2.2 各因素与脊柱术后发生SSI关系的Meta分析 2.2.1 高血压 共纳入6篇文献[17,19-20,22-23,26],包括病例组502例,对照组2 002例。经异质性检验(P=0.726,I2=0%),采用固定效应模型。结果显示高血压是脊柱术后发生SSI的危险因素(OR=1.90,95%CI:1.34-2.69),见图2。 "
| [1] 张淑娟. 2018年我院普外科医院感染现患率调查及因素分析[J]. 基层医学论坛,2019,23(27): 3967. [2] 王铮,曹华,徐正,等.腰椎术后切口感染病原菌及耐药性分析[J]. 中华医院感染学杂志,2019,29(5):734-736. [3] SCHIMMEL JJ, HORSTING PP, DE KLEUVER M, et al. Risk factors for deep surgical site infections after spinal fusion. Eur Spine J. 2010;19(10):1711-719. [4] 中国高血压防治指南修订委员会,高血压联盟(中国中华医学会心血管病学分会,中国医师协会高血压专业委员会,中国医疗保健国际交流促进会高血压分会,中国老年医学学会高血压分会.中国高血压防治指南(2018年修订版)[J].中国心血管杂志,2019, 24(1):24-56. [5] 中华医学会糖尿病分会.中国2型糖尿病防治指南(2017年版) [J]. 中国实用内科杂志,2018,38(4): 292-344. [6] OGDEN CL, YANOVSKI SZ, CARROLL MD, et al. The epidemiology of obesity. Gastroenterology. 2007;132(6): 2087-2102. [7] KONG L, LIU Z, MENG F, et al. Smoking and risk of surgical site infection after spinal surgery: a systematic review and meta-analysis. Surg Infect (Larchmt). 2017;18(2): 206-214. [8] MANGRAM AJ, HORAN TC, PEARSON ML, et al. Guideline for prevention of surgical site infection, 1999. Hospital Infection Control Practices Advisory Committee. Infect Control Hosp Epidemiol. 1999;20(4): 250-278; quiz 279-280. [9] FANG A, HU SS, ENDRES N, et al. Risk factors for infection after spinal surgery. Spine. 2005;30(12):1460-1465. [10] FRIEDMAN ND, SEXTON DJ, CONNELLY SM, et al. Risk factors for surgical site infection complicating laminectomy. Infect Control Hosp Epidemiol. 2007;28(9):1060-1065. [11] SCIUBBA DM, NELSON C, GOK B, et al. Evaluation of factors associated with postoperative infection following sacral tumor resection. J Neurosurg Spine. 2008;9(6): 593-599. [12] MARAGAKIS LL, COSGROVE SE, MARTINEZ EA, et al. Intraoperative fraction of inspired oxygen is a modifiable risk factor for surgical site infection after spinal surgery. Anesthesiology. 2009; 110(3):556-562. [13] BOSTON KM, BARANIUK S, O'HERON S, et al. Risk factors for spinal surgical site infection, houston, texas. Infect Control Hosp Epidemiol. 2009; 30(9): 884-889. [14] WATANABE M1, SAKAI D, MATSUYAMA D, et al. Risk factors for surgical site infection following spine surgery: efficacy of intraoperative saline irrigation. J Neurosurg Spine. 2010;12(5):540-546. [15] OMEIS IA, DHIR M, SCIUBBA DM, et al. Postoperative surgical site infections in patients undergoing spinal tumor surgery: incidence and risk factors. Spine (Philadelphia, 1976). 2011; 36(17):1410-1419. [16] CHEN KW, YANG HL, LU J, et al. Risk factors for postoperative wound infections of sacral chordoma after surgical excision. J Spinal Disord Tech. 2011;24(4):230-234. [17] KOUTSOUMBELIS S, HUGHES AP, GIRARDI FP, et al. Risk factors for postoperative infection following posterior lumbar instrumented arthrodesis. J Bone Joint Surg Am. 2011; 93A(17):1627-1633. [18] OGIHARA S, YAMAZAKI T, MARUYAMA T, et al. Prospective multicenter surveillance and risk factor analysis of deep surgical site infection after posterior thoracic and/or lumbar spinal surgery in adults. J Orthop Sci. 2015; 20(1): 71-77. [19] 关炳瑜,阿海,贺元,等.脊柱外科术后感染的影响因素分析[J]. 临床骨科杂志,2016,19(5): 547-549. [20] HALEEM A, CHIANG HY, VODELA R, et al. Risk factors for surgical site infections following adult spine operations. Infect Control Hosp Epidemiol. 2016;37(12):1458-1467. [21] 程清平,王东福,焦朋,等.腰椎间盘突出症术后椎间隙感染的治疗及危险因素分析[J].中国骨与关节损伤杂志,2017,32(1):32-35. [22] 黄秀玉.脊柱后路术后感染危险因素分析[J].中国医药导报,2017, 14(22):72-75. [23] 范一鸣,王征,王岩.腰椎后路内固定术后早期切口深部感染的相关因素分析[J].颈腰痛杂志,2017,38(4):327-330. [24] 胡向宁,周秦,穆玲娟,等.脊柱手术后发生切口感染的相关因素分析及预防措施[J].临床医学研究与实践,2018,3(20):50-51. [25] 吴信,尚显文,张皓,等.脊柱内固定术后手术部位感染的原因分析及防治措施探究[J].实用骨科杂志,2018,24(1): 10-14. [26] 余伟宏,冯永洪,王新强,等.腰椎后路术后手术切口早期感染的危险因素分析[J].海南医学,2018,29(15):2175-2177. [27] MALONE DL, GENUIT T, TRACY JK, et al. Surgical site infections: Reanalysis of risk factors. J Surg Res. 2002;103(1): 89-95. [28] NEUMAYER L, HOSOKAWA P, ITANI K, et al. Multivariable predictors of postoperative surgical site infection after general and vascular surgery: results from the patient safety in surgery study. J Am Coll Surg. 2007;204(6):1178-1187. [29] SHILLING AM, RAPHAEL J. Diabetes, hyperglycemia, and infections. Best Pract Res Clin Anaesthesiol. 2008; 22(3): 519-535. [30] VERHOFSTAD MH, HENDRIKS T. Complete prevention of impaired anastomotic healing in diabetic rats requires preoperative blood glucose control. Br J Surg. 1996;83(12): 1717-1721. [31] VAN DEN BERGHE G, WOUTERS P, WEEKERS F, et al. Intensive insulin therapy in the critically ill patients. N Eng J Med. 2001;345(19):1359-1367. [32] 黄文娟,王成,旭思哲,等.学龄期儿童高血压和肥胖发病率调查[J]. 国际儿科学杂志,2017,44(4):294-296. [33] PULL TER GUNNE AF, COHEN DB. Incidence, prevalence, and analysis of risk factors for surgical site infection following adult spinal surgery. Spine (Phila Pa 1976). 2009;34(13): 1422-1428. [34] WISSE BE. The inflammatory syndrome: the role of adipose tissue cytokines in metabolic disorders linked to obesity. J Am Soc Nephrol. 2004;15(11):2792-2800. [35] SERNÉ EH, GANS RO, TER MAATEN JC, et al. Impaired skin capillary recruitment in essential hypertension is caused by both functional and structural capillary rarefaction. Hypertension. 2001; 38(2):238-242. [36] WEBER MA, SCHIFFRIN EL, WHITE WB, et al. Clinical practice guidelines for the management of hypertension in the community: a statement by the American Society of Hypertension and the International Society of Hypertension. J Clin Hypertens (Greenwich). 2014;16(1):14-26. [37] WRIGHT JT JR, FINE LJ, LACKLAND DT, et al. Evidence supporting a systolic blood pressure goal of less than 150 mm Hg in patients aged 60 years or older: the minority view. Ann Intern Med. 2014;160(7):499-503. [38] 李军.围术期高血压管理专家共识[J].临床麻醉学杂志,2016, 32(3): 295-297. [39] 李瑶宣,李吕力.超声检测肱动脉内皮功能的研究进展[J].医学综述,2009,15(4): 585-587. [40] 陈桂英,郭来敬,廖燕华,等.吸烟与脉搏波传导速度、踝臂指数以及颈动脉硬化改变的相关性研究[J].现代中西医结合杂志,2013, 22(35): 3883-3885. [41] YAMAGUCHI Y, HAGINAKA J, MORIMOTO S, et al. Facilitated nitration and oxidation of LDL in cigarette smokers. Eur J Clin Invest. 2005;35(3):186-193. [42] MCEVOY JW, NASIR K, DEFILIPPIS AP, et al. Relationship of cigarette smoking with inflammation and subclinical vascular disease: the Multi-Ethnic Study of Atherosclerosis. Arterioscler Thromb Vasc Biol. 2015;35(4):1002-1010. [43] XING D, MA JX, MA XL, et al. A methodological, systematic review of evidence-based independent risk factors for surgical site infections after spinal surgery. Eur Spine J. 2013;22(3): 605-615 [44] OLSEN MA, MAYFIELD J, LAURYSSEN C, et al. Risk factors for surgical site infection in spinal surgery. J Neurosurg. 2003; 98(2 Suppl):149-155. [45] 吴信.脊柱内固定术后手术部位感染的原因分析及治疗措施探究[J].贵阳:贵州医科大学, 2016. [46] 刘晓芳.尼古丁依赖的药物治疗:指南与经验[J].临床药物治疗杂志, 2011, 9(6): 25-28. [47] PENG XQ, SUN CG, FEI ZG, et al. Risk factors for surgical site infection after spinal surgery: a systematic review and meta-analysis based on twenty-seven studies. World Neurosurg. 2019;123:e318-e329. [48] SEBAALY A, SHEDID D, BOUBEZ G, et al. Surgical site infection in spinal metastasis: incidence and risk factors. Spine J. 2018; 18(8): 1382-1387. [49] PESENTI S. Meta-analysis of risk factors associated with surgical site infection after spinal arthrodesis. Spine J. 2017. |
| [1] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [2] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [3] | Zhang Chao, Lü Xin. Heterotopic ossification after acetabular fracture fixation: risk factors, prevention and treatment progress [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1434-1439. |
| [4] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [5] | Chen Jinping, Li Kui, Chen Qian, Guo Haoran, Zhang Yingbo, Wei Peng. Meta-analysis of the efficacy and safety of tranexamic acid in open spinal surgery [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1458-1464. |
| [6] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [7] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [8] | Wang Yongsheng, Wu Yang, Li Yanchun. Effect of acute high-intensity exercise on appetite hormones in adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1305-1312. |
| [9] | Kong Desheng, He Jingjing, Feng Baofeng, Guo Ruiyun, Asiamah Ernest Amponsah, Lü Fei, Zhang Shuhan, Zhang Xiaolin, Ma Jun, Cui Huixian. Efficacy of mesenchymal stem cells in the spinal cord injury of large animal models: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1142-1148. |
| [10] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Intravenous, topical tranexamic acid alone or their combination in total knee arthroplasty: a meta-analysis of randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 948-956. |
| [11] | Li Yan, Wang Pei, Deng Donghuan, Yan Wei, Li Lei, Jiang Hongjiang. Electroacupuncture for pain control after total knee arthroplasty: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 957-963. |
| [12] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| [13] | Hua Haotian, Zhao Wenyu, Zhang Lei, Bai Wenbo, Wang Xinwei. Meta-analysis of clinical efficacy and safety of antibiotic artificial bone in the treatment of chronic osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 970-976. |
| [14] | Zhan Fangbiao, Cheng Jun, Zou Xinsen, Long Jie, Xie Lizhong, Deng Qianrong. Intraoperative intravenous application of tranexamic acid reduces perioperative bleeding in multilevel posterior spinal surgery: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 977-984. |
| [15] | Zhong Yuanming, Wan Tong, Zhong Xifeng, Wu Zhuotan, He Bingkun, Wu Sixian. Meta-analysis of the efficacy and safety of percutaneous curved vertebroplasty and unilateral pedicle approach percutaneous vertebroplasty in the treatment of osteoporotic vertebral compression fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 456-462. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||