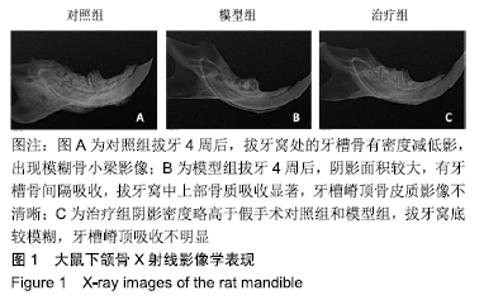
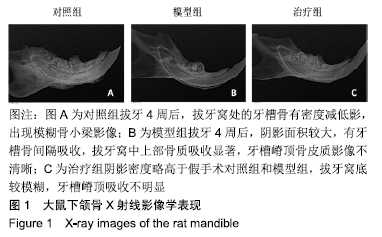
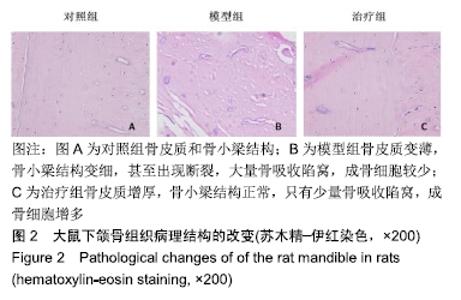
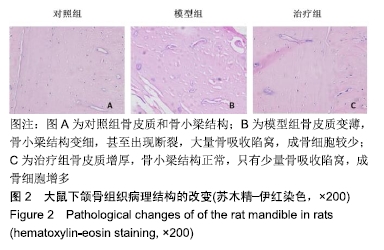
Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (17): 2686-2693.doi: 10.3969/j.issn.2095-4344.2597
Previous Articles Next Articles
Low-dose zoledronic acid regulates osteoclasts and
osteoblasts in the extraction socket of ovariectomized rats
Cheng Yuting1, Wu Chao1, Huang Xiaolin2, Li Fang1, Shi Qianhui1, Zhou Qian1, Hong Wei3, Wang Yong1, Liao Jian1
- 1Stomatological Hospital of Guizhou Medical University, Guiyang 550004, Guizhou Province, China; 2Stomatological Branch of Zhongshan People’s Hospital, Zhongshan 528403, Guangdong Province, China; 3Key Laboratory of Molecular Biology, Guizhou Medical University, Guiyang 550004, Guizhou Province, China
-
Received:2019-08-21Revised:2019-08-22Accepted:2019-09-17Online:2020-06-18Published:2020-03-28 -
Contact:Liao Jian, MD, Associate chief physician, Stomatological Hospital of Guizhou Medical University, Guiyang 550004, Guizhou Province, China -
About author:Cheng Yuting, Master candidate, Stomatological Hospital of Guizhou Medical University, Guiyang 550004, Guizhou Province, China -
Supported by:the National Natural Science Foundation of China, No. 81660179; the Science and Technology Foundation of Guizhou Province, No. [2016]1124 and [2014]2026
CLC Number:
Cite this article
Cheng Yuting, Wu Chao, Huang Xiaolin, Li Fang, Shi Qianhui, Zhou Qian, Hong Wei, Wang Yong, Liao Jian.
Low-dose zoledronic acid regulates osteoclasts and
osteoblasts in the extraction socket of ovariectomized rats
share this article

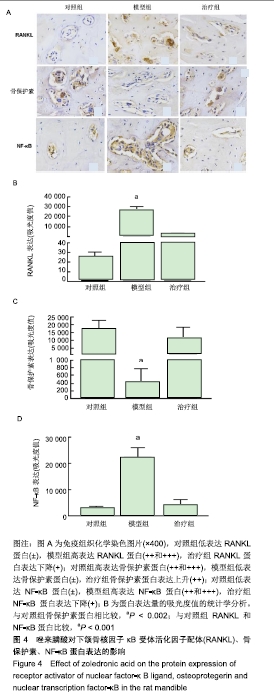
2.5 免疫组织化学染色结果 RANKL蛋白属于分泌型蛋白,主要表达于细胞浆和细胞膜上。实验中有12只正常对照组大鼠低表达RANKL蛋白(±),8只模型组大鼠高表达RANKL蛋白(++和+++),9只治疗组大鼠RANKL蛋白表达下降(+),对照组、模型组、治疗组吸光度值分别为25±5, 26 604±3 415,2 823±641,组间比较差异有显著性意义(F=212,P < 0.001),见图4A,B,与对照组相比较,模型组的骨细胞胞浆和胞膜的RANKL表达较明显,而在唑来膦酸治疗后RANKL 表达明显减少;骨保护素蛋白的阳性部位与RANKL蛋白相同,10只正常对照组大鼠高表达骨保护素蛋白(++和+++),8只模型组大鼠低表达骨保护素蛋白(±),9只大鼠用药后骨保护素蛋白表达上升(++),对照组、模型组、治疗组吸光度值分别为17 691±5 287,407±365,11 610± 6 879,组间比较差异有显著性意义(F=12.23,P < 0.002)(图4A,B),对照组的骨保护素表达与其他组相比较略为明显,模型组阳性颗粒最少,骨保护素表达量最少;NF-KB p65蛋白主要位于细胞浆和细胞核上,有11只正常对照组大鼠低表达NF-κB蛋白(±),9只模型组大鼠高表达NF-κB蛋白(++和+++),9只大鼠用药后NF-κB蛋白表达下降(+),对照组、模型组、治疗组吸光度值分别为3 175±437,22 532±3 500,4 181±2 055,组间比较差异有显著性意义(F=85.51,P < 0.001),见图4A,B,模型组表达较其他组明显,用药后的治疗组与对照组无明显差异,表达较少。 "
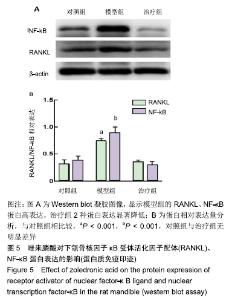
2.6 Western Blot结果 与对照组相比较,模型组的RANKL、NF-κB蛋白高表达,用药后其表达量显著降低,甚至比正常大鼠的表达量略低些,对照组、模型组、治疗组的RANKL、NF-κB与内参β-Actin的灰度比值分别为0.305 8±0.081 1,0.732 0±0.054 9,0.345 7±0.034 7,组间比较差异有显著性意义(F=46.19,P < 0.001)和 0.374 7±0.082 4,0.892 6±0.108 0,0.281 7±0.072 9,组间比较差异有显著性意义(F=41.02,P < 0.001),见图5,模型组表达较其他组明显,用药后的治疗组与对照组比较差异无显著性意义。 "

| [1] CHARATCHAIWANNA A, ROJSIRAPHISA T, AUNMEUNGTONG W, et al. Mathematical equations for dental implant stability patterns during the osseointegration period, based on previous resonance frequency analysis studies.Clin Implant Dent Relat Res.2019; 21(5): 1028-1040. [2] CHAI J, CHAU AC, CHU FC, et al.Diagnostic performance of mandibular bone density measurements in assessing osteoporotic status.Int J Oral Maxillofac Implants.2014;29(3): 667-674. [3] KULAR J, TICKNER J, CHIM SM, et al. An overview of the regulation of bone remodelling at the cellular level.Clin Biochem.2012;45(12): 863-873. [4] ODEN A, MCCLOSKEY EV, KANIS JA, et al.Burden of high fracture probability worldwide: secular increases 2010-2040.Osteoporos Int.2015;26(9): 2243-2248. [5] CAULEY JA. Osteoporosis: fracture epidemiology update 2016.Curr Opin Rheumatol.2017;29(2): 150-156. [6] THULKAR J, SINGH S, SHARMA S, et al. Preventable risk factors for osteoporosis in postmenopausal women: Systematic review and meta-analysis.J Midlife Health.2016; 7(3):108-113. [7] LU J, LIU F, LIU D, et al. Amlodipine and atorvastatin improved hypertensive cardiac hypertrophy through regulation of receptor activator of nuclear factor kappa B ligand/receptor activator of nuclear factor kappa B/ osteoprotegerin system in spontaneous hypertension rats.Exp Biol Med (Maywood).2016; 241(11): 1237-1249. [8] LIZNEVA D, YUEN T, SUN L, et al. Emerging concepts in the epidemiology, pathophysiology, and clinical care of postmenopausal osteoporosis.Matrix Biology. 2018_S0945053X18301586. [9] 白璧辉,谢兴文,李鼎鹏,等.我国近5年来骨质疏松症流行病学研究现状[J].中国骨质疏松杂志,2018,24(2):253-258. [10] SHEN Y, LI YQ, LI SP, et al. Alleviation of ovariectomy- induced osteoporosis in rats by Panax notoginseng saponins. J Nat Med.2010;64(3): 336-345. [11] KESKINRUZGAR A, BOZDAG Z, ARAS MH, et al. Histopathological Effects of Teriparatide in Medication- Related Osteonecrosis of the Jaw: An Animal Study. J Oral Maxillofac Surg. 2016;74(1):68-78. [12] ALMUBARAK H, JONES A, CHAISUPARAT R, et al. Zoledronic acid directly suppresses cell proliferation and induces apoptosis in highly tumorigenic prostate and breast cancers.J Carcinog.2011;10:2. [13] COLEMAN RE, WINTER MC, CAMERON D, et al.The effects of adding zoledronic acid to neoadjuvant chemotherapy on tumour response: exploratory evidence for direct anti-tumour activity in breast cancer. Br J Cancer. 2010;102(7):1099-1105. [14] SKERJANEC A, BERENSON J, HSU C, et al. The pharmacokinetics and pharmacodynamics of zoledronic acid in cancer patients with varying degrees of renal function.J Clin Pharmacol.2003;43(2): 154-162. [15] LI EC, DAVIS LE. Zoledronic acid: a new parenteral bisphosphonate. Clin Ther.2003;25(11): 2669-2708. [16] 吴骁伟,李少晗,曹文娟.唑来膦酸影响单个核细胞向破骨细胞分化及RANK表达的研究[J].中华全科医学,2016,14(10): 1644-1646. [17] TAI TW, SU FC, CHEN CY, et al. Activation of p38 MAPK-regulated Bcl-xL signaling increases survival against zoledronic acid-induced apoptosis in osteoclast precursors. Bone.2014;67: 166-174. [18] GREY A, BOLLAND MJ, HORNE A, et al.Duration of antiresorptive activity of zoledronate in postmenopausal women with osteopenia: a randomized, controlled multidose trial.CMAJ.2017;189(36): E1130-E1136. [19] ALSALLEEH F, KEIPPEL J, ADAMS L, et al. Bisphosphonate- associated osteonecrosis of jaw reoccurrence after methotrexate therapy: a case report.J Endod.2014;40(9): 1505-1507. [20] HAIDAR A, JØNLER M, FOLKMAR TB, et al. Bisphosphonate (zoledronic acid)-induced osteonecrosis of the jaw. Scand J Urol Nephrol.2009;43(6):442-444. [21] ZHANG Q, ATSUTA I, LIU S, et al. IL-17-mediated M1/M2 macrophage alteration contributes to pathogenesis of bisphosphonate-related osteonecrosis of the jaws.Clin Cancer Res.2013;19(12): 3176-3188. [22] CHO DC, KIM KT, JEON Y, et al.A synergistic bone sparing effect of curcumin and alendronate in ovariectomized rat.Acta Neurochir (Wien).2012;154(12): 2215-2223. [23] RISTOW O, GERNGROSS C, SCHWAIGER M, et al. Does regular zoledronic acid change the bone turnover of the jaw in men with metastatic prostate cancer: a possible clue to the pathogenesis of bisphosphonate related osteonecrosis of the jaw?.J Cancer Res Clin Oncol.2014;140(3): 487-493. [24] HUANG XL, HUANG LY, CHENG YT, et al. Zoledronic acid inhibits osteoclast differentiation and function through the regulation of NF-kappaB and JNK signalling pathways.Int J Mol Med.2019;44(2): 582-592. [25] 黄晓林,廖健,洪伟,等.破骨细胞形成过程中唑来膦酸的作用途径及机制[J].中国组织工程研究,2019,23(17):98-103. [26] ZHOU L, FENG Y, JIN Y, et al.Verbascoside promotes apoptosis by regulating HIPK2-p53 signaling in human colorectal cancer.BMC Cancer.2014;14: 747. [27] GOMEZ-DE DR, MANG-DE LRMR, ROMERO-PEREZ MJ, et al. Indications and contraindications of dental implants in medically compromised patients: update.Med Oral Patol Oral Cir Bucal.2014;19(5): e483-e489. [28] KALU DN. The ovariectomized rat model of postmenopausal bone loss. Bone Miner.1991;15(3): 175-191. [29] MCCANN RM, COLLEARY G, GEDDIS C, et al. Effect of osteoporosis on bone mineral density and fracture repair in a rat femoral fracture model.J Orthop Res.2008;26(3): 384-393. [30] LUO Y, ZHANG L, WANG WY, et al. Alendronate retards the progression of lumbar intervertebral disc degeneration in ovariectomized rats.Bone.2013;55(2): 439-448. [31] KHAJURIA DK, RAZDAN R, MAHAPATRA DR. Development, in vitro and in vivo characterization of zoledronic acid functionalized hydroxyapatite nanoparticle based formulation for treatment of osteoporosis in animal model.Eur J Pharm Sci.2015;66: 173-183. [32] YISHAKE M, YASEN M, JIANG L, et al. Effects of combined teriparatide and zoledronic acid on posterior lumbar vertebral fusion in an aged ovariectomized rat model of osteopenia.J Orthop Res.2018 Mar;36(3):937-944. [33] GAO Y, LUO E, HU J, et al. Effect of combined local treatment with zoledronic acid and basic fibroblast growth factor on implant fixation in ovariectomized rats.Bone.2009;44(2): 225-232. [34] WALTER C, AL-NAWAS B, FRICKHOFEN N, et al. Prevalence of bisphosphonate associated osteonecrosis of the jaws in multiple myeloma patients.Head Face Med.2010;6: 11. [35] QI M, HU J, LI J, et al. Effect of zoledronate acid treatment on osseointegration and fixation of implants in autologous iliac bone grafts in ovariectomized rabbits.Bone.2012;50(1): 119-127. [36] YASEN M, LI X, JIANG L, et al. Effect of zoledronic acid on spinal fusion outcomes in an ovariectomized rat model of osteoporosis.J Orthop Res.2015;33(9): 1297-1304. [37] SUNITHA VR, EMMADI P, NAMASIVAYAM A, et al. The periodontal - endodontic continuum: A review.J Conserv Dent.2008;11(2): 54-62. [38] DIKICIER S, DIKICIER E, KARACAYLI U, et al. Radiodensitometric study for evaluation of bone mineral density around dental implants after zoledronic acid treatment in ovariectomized rats.Med Oral Patol Oral Cir Bucal.2017; 22(3): e377-e382. [39] HSU PY, TSAI MT, WANG SP, et al. Cortical Bone Morphological and Trabecular Bone Microarchitectural Changes in the Mandible and Femoral Neck of Ovariectomized Rats.PLoS One.2016;11(4): e154367. [40] JOHNSTON BD, WARD WE.The ovariectomized rat as a model for studying alveolar bone loss in postmenopausal women.Biomed Res Int.2015;2015: 635023. [41] LIN TH, TAMAKI Y, PAJARINEN J, et al.Chronic inflammation in biomaterial-induced periprosthetic osteolysis: NF-kappaB as a therapeutic target.Acta Biomater.2014;10(1): 1-10. [42] KIMACHI K, KAJIYA H, NAKAYAMA S, et al. Zoledronic acid inhibits RANK expression and migration of osteoclast precursors during osteoclastogenesis. Naunyn Schmiedebergs Arch Pharmacol.2011;383(3): 297-308. [43] MARUOTTI N, CORRADO A, NEVE A, et al. Bisphosphonates: effects on osteoblast.Eur J Clin Pharmacol.2012;68(7): 1013-1018. [44] REINHOLZ GG, GETZ B, PEDERSON L, et al. Bisphosphonates directly regulate cell proliferation, differentiation, and gene expression in human osteoblasts. Cancer Res.2000;60(21): 6001-6007. |
| [1] | Tang Hui, Yao Zhihao, Luo Daowen, Peng Shuanglin, Yang Shuanglin, Wang Lang, Xiao Jingang. High fat and high sugar diet combined with streptozotocin to establish a rat model of type 2 diabetic osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1207-1211. |
| [2] | Li Zhongfeng, Chen Minghai, Fan Yinuo, Wei Qiushi, He Wei, Chen Zhenqiu. Mechanism of Yougui Yin for steroid-induced femoral head necrosis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1256-1263. |
| [3] | Hou Guangyuan, Zhang Jixue, Zhang Zhijun, Meng Xianghui, Duan Wen, Gao Weilu. Bone cement pedicle screw fixation and fusion in the treatment of degenerative spinal disease with osteoporosis: one-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 878-883. |
| [4] | Li Shibin, Lai Yu, Zhou Yi, Liao Jianzhao, Zhang Xiaoyun, Zhang Xuan. Pathogenesis of hormonal osteonecrosis of the femoral head and the target effect of related signaling pathways [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 935-941. |
| [5] | Xiao Fangjun, Chen Shudong, Luan Jiyao, Hou Yu, He Kun, Lin Dingkun. An insight into the mechanism of Salvia miltiorrhiza intervention on osteoporosis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 772-778. |
| [6] | Liu Bo, Chen Xianghe, Yang Kang, Yu Huilin, Lu Pengcheng. Mechanism of DNA methylation in exercise intervention for osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 791-797. |
| [7] | Zhong Yuanming, Wan Tong, Zhong Xifeng, Wu Zhuotan, He Bingkun, Wu Sixian. Meta-analysis of the efficacy and safety of percutaneous curved vertebroplasty and unilateral pedicle approach percutaneous vertebroplasty in the treatment of osteoporotic vertebral compression fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 456-462. |
| [8] | Nie Shaobo, Li Jiantao, Sun Jien, Zhao Zhe, Zhao Yanpeng, Zhang Licheng, Tang Peifu. Mechanical stability of medial support nail in treatment of severe osteoporotic intertrochanteric fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 329-333. |
| [9] | Zhu Yun, Chen Yu, Qiu Hao, Liu Dun, Jin Guorong, Chen Shimou, Weng Zheng. Finite element analysis for treatment of osteoporotic femoral fracture with far cortical locking screw [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3832-3837. |
| [10] | Feng Guancheng, Fang Jianming, Lü Haoran, Zhang Dongsheng, Wei Jiadong, Yu Bingbing. How does bone cement dispersion affect the early outcome of percutaneous vertebroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3450-3457. |
| [11] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| [12] | Cai Qunbin, Yang Lijuan, Li Qiumin, Chen Xinmin, Zheng Liqin, Huang Peizhen, Lin Ziling, Jiang Ziwei . Feasibility of internal fixation removal of intertrochanteric fractures in elderly patients based on fracture mechanics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3313-3318. |
| [13] | Liu Yulin, Li Guotai. Combined effects of hyperbaric oxygen, vibration training and astaxanthin on bone mineral density, glucose metabolism and oxidative stress in diabetic osteoporosis rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(20): 3117-3124. |
| [14] | Lin Haishan, Mieralimu Muertizha, Li Peng, Ma Chao, Wang Li. Correlation between skeletal muscle fiber characteristics and bone mineral density in postmenopausal women with hip fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(20): 3144-3149. |
| [15] | Chen Xinling, Wang Shenglan. Cell autophagy, pathway, regulation and its multiple correlations with pulmonary hypertension [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(2): 311-316. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||