Chinese Journal of Tissue Engineering Research ›› 2018, Vol. 22 ›› Issue (3): 450-455.doi: 10.3969/j.issn.2095-4344.0046
Previous Articles Next Articles
Lumbar intervertebral disc degeneration assessed by the nine-point system with X-ray
Zhao Yin, Zhou Sheng-yuan, Yuan Bo, Xu Guo-feng, Xu Zheng, Lv Bi-tao, Jia Lian-shun, Chen Xiong-sheng
- Department of Spine Surgery, Shanghai Changzheng Hospital, the Second Military Medical University, Shanghai 200003, China
-
Online:2018-01-28Published:2018-01-28 -
Contact:Chen Xiong-sheng, M.D., Chief physician, Department of Spine Surgery, Shanghai Changzheng Hospital, the Second Military Medical University, Shanghai 200003, China -
About author:Zhao Yin, Studying for doctorate, Physician, Department of Spine Surgery, Shanghai Changzheng Hospital, the Second Military Medical University, Shanghai 200003, China -
Supported by:the Experimental Animal Project of Shanghai Science and Technology Commission, No. 15140903800
CLC Number:
Cite this article
Zhao Yin, Zhou Sheng-yuan, Yuan Bo, Xu Guo-feng, Xu Zheng, Lv Bi-tao, Jia Lian-shun, Chen Xiong-sheng. Lumbar intervertebral disc degeneration assessed by the nine-point system with X-ray[J]. Chinese Journal of Tissue Engineering Research, 2018, 22(3): 450-455.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
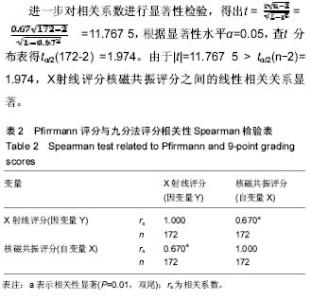
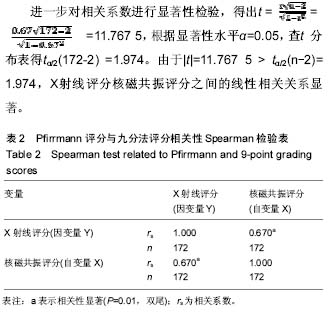
2.1 影像学退变评估结果 172例腰椎间盘退变的核磁共振和X射线评分均不符合正态分布,结果如下: 核磁共振评分:1分2例,2分8例,3分55例,4分84例,5分23例(图4);X射线评分:0分2例,1分6例,2分21例,3分43例,4分40例,5分26例,6分16例,7分8例,8分7例,9分3例(图5)。 2.2 两组评分相关性检验 核磁共振与X射线评分相关性的Spearman秩和检验统计学数据见表2:腰椎间盘退变基于核磁共振的评分(自变量X)和基于X射线的评分(因变量Y)之间存在正相关,且自变量X和因变量Y的相关系数rs=0.670(P < 0.01),介于0.5-0.8之间,属显著正相关。"
| [1] Yu LP, Qian WW, Yin GY, et al. MRI assessment of lumbar intervertebral disc degeneration with lumbar degenerative disease using the Pfirrmann grading systems. PLoS One. 2012;7(12):e48074.[2] Peter G, Katherine D, Michael R, et al. Assessment of intervertebral disc degeneration based on quantitative MRI analysis: an in vivo study. Spine. 2014;39(6):e369-378.[3] Desai MJ, Hargens LM, Breitenfeldt MD, et al. The rate of magnetic resonance imaging in patients with spinal cord stimulation.Spine (Phila Pa 1976). 2015; 40(9): E531-E537.[4] Arnbak B, Jensen RK, Manniche C, et al. Identification of subgroups of inflammatory and degenerative MRI findings in the spine and sacroiliac joints: a latent class analysis of 1037 patients with persistent low back pain.Arthritis Res Ther. 2016; 18: 237.[5] Pfirrmann CW, Metzdorf A, Zanetti M, et al. Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine. 2001;26(17):1873-1878.[6] Muriuki MG, Havey RM, Voronov LI, et al. Effects of motion segment level, Pfirrmann intervertebral disc degeneration grade and gender on lumbar spine kinematics. J Orthop Res. 2016;34(8):1389-1398.[7] Weber U, Pfirrmann CWA, Kissling RO, et al. Whole body MR imaging in ankylosing spondylitis: a descriptive pilot study in patients with suspected early and active confirmed ankylosing spondylitis.BMC Musculoskelet Disord. 2007;8:20.[8] Urrutia J, Besa P, Campos M, et al. The Pfirrmann classification of lumbar intervertebral disc degeneration: an independent inter- and intra-observer agreement assessment. Eur Spine J. 2016;25(9):2728-2733.[9] Leite MS, Luciano RP, Martins DE, et al. Correlation between Pfirrmann and Modic classifications in the degeneration of lumbar intervertebral disc. Coluna/Columna. 2010;9(4): 401-406.[10] Bergknut N, Auriemma E, Wijsman S, et al. Evaluation of intervertebral disk degeneration in chondrodystrophic and nonchondrodystrophic dogs by use of Pfirrmann grading of images obtained with low-field magnetic resonance imaging. Am J Vet Res. 2011;72(7):893-898.[11] Wei W, Jin H, Deyong L, et al. Multimodal quantitative magnetic resonance imaging for lumbar intervertebral disc degeneration. Exp Ther Med. 2017;14(3):2078-2084.[12] Smith GW, Robinson RA. The treatment of certain cervical-spine disorders by anterior removal of the intervertebral disc and interbody fusion. J Bone Joint Surg Am. 1958;40(3):607-624.[13] Oglesby M1, Fineberg SJ, Patel AA, et al. Epidemiological trends in cervical spine surgery for degenerative diseases between 2002 and 2009. Spine. 2013;38(14):1226-1232.[14] Baldwin A, Mesfin A. Adjacent segment disease 44 years following posterior spinal fusion for congenital lumbar kyphosis. Spine Deform. 2017;5(6):435-439.[15] Dong L, Xu Z, Chen X, et al. The change of adjacent segment after cervical disc arthroplasty compared with anterior cervical discectomy and fusion: a meta-analysis of randomized controlled trials. Spine J. 2017;17(10):1549-1558.[16] 姜允琦,李熙雷,董健.腰椎融合术后邻椎病发生的危险因素[J].中华医学杂志. 2012;92(29):2078-2080.[17] Sears WR, Sergides IG, Kazemi N, et al. Incidence and prevalence of surgery at segments adjacent to a previous posterior lumbar arthrodesis. Spine J. 2011;11(1):11-20.[18] Cho KS, Kang SG, Yoo DS, et al. Risk factors and surgical treatment for symptomatic adjacent segment degeneration after lumbar spine fusion. J Korean Neurosurg Soc. 2009; 46(5):425-430.[19] Lee CS, Hwang CJ, Lee SW, et al. Risk factors for adjacent segment disease after lumbar fusion. Eur Spine J. 2009; 18(11):1637-1643.[20] Hilibrand AS, Robbins M. Adjacent segment degeneration and adjacent segment disease: the consequences of spinal fusion? Spine J. 2004;4(6 Suppl):190-194.[21] Benneker LM, Heini PF, Anderson SE, et al. Correlation of radiographic and MRI parameters to morphological and biochemical assessment of intervertebral disc degeneration. Eur Spine J. 2005;14(1):27-35.[22] Walraevens J, Liu B, Meersschaert J, et al. Qualitative and quantitative assessment of degeneration of cervical intervertebral discs and facet joints. Eur Spine J. 2009; 18(3):358-369.[23] 于斌,王以朋,邱贵兴.腰椎间盘退变的MRI分级评价方法研究进展[J].中国骨与关节外科杂志. 2010;3(5):410-413.[24] Schneiderman G, Flannigan B, Kingston S, et al.Magnetic resonance imaging in the diagnosis of disc degeneration: correlation with discography. Spine. 1987;12:276-281.[25] Luoma K, Vehmas T, Riihimäki H, etal. Disc height and signal intensity of the nucleus pulposus on magnetic resonance imaging as indicators of lumbar disc degeneration. Spine. 2001;26(6):680-686.[26] Videman T, Nummi P, Battié MC, et al. Digital assessment of MRI for lumbar disc desiccation. A comparison of digital versus subjective assessments and digital intensity profiles versus discogram and macroanatomic findings. Spine.1994; 19(2):192-198.[27] Thompson JP, Pearce RH, Schechter MT, et al. Preliminary evaluation of a scheme for grading the gross morphology of the human intervertebral disc. Spine.1990;15(5):411-415.[28] Griffith JF, Wang YX, Antonio GE, et al. Modified Pfirrmann grading system for lumbar intervertebral disc degeneration. Spine. 2007;32(24):e708-712.[29] Edmondston SJ, Song S, Bricknell RV, et al. MRI evaluation of lumbar spine flexion and extension in asymptomatic individuals. Man Ther. 2000;5(3):158-164.[30] Campana S, Charpail E, De Guise JA, et al. Relationships between viscoelastic properties of lumbar intervertebral disc and degeneration grade assessed by MRI. J Mech Behav Biomed Mater. 2011;4(4):593-599.[31] Niinimäki J, Korkiakoski A, Ojala O, et al. Association between visual degeneration of intervertebral discs and the apparent diffusion coefficient. Magn Reson Imaging. 2009;27(5): 641-647.[32] Zuo J, Saadat E, Romero A, et al. Assessment of intervertebral disc degeneration with magnetic resonance single-voxel spectroscopy. Magn Reson Med. 2009;62(5): 1140-1146.[33] Xiao L, Ni C, Shi J, et al. Analysis of correlation between vertebral endplate change and lumbar disc degeneration. Med Sci Monit. 2017;23:4932-4938.[34] Hausmann ON,Böni T,Pfirrmann CWA, et al. Preoperative radiological and electrophysiological evaluation in 100 adolescent idiopathic scoliosis patients.Eur Spine J. 2003; 12(5): 501-506.[35] Young KJ. Gimme that old time religion: the influence of the healthcare belief system of chiropractic’s early leaders on the development of x-ray imaging in the profession.Chiropr Man Therap. 2014; 22: 36.[36] Tannor AY. Lumbar spine X-ray as a standard investigation for all low back pain in Ghana: is it evidence based? Ghana Med J. 2017; 51(1): 24-29.[37] Peterfy CG, DiCarlo JC, Olech E, et al. Evaluating joint-space narrowing and cartilage loss in rheumatoid arthritis by using MRI.Arthritis Res Ther. 2012;14(3): R131. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [3] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [4] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [5] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [6] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [7] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [8] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [9] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [10] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [11] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [12] | Wang Hao, Chen Mingxue, Li Junkang, Luo Xujiang, Peng Liqing, Li Huo, Huang Bo, Tian Guangzhao, Liu Shuyun, Sui Xiang, Huang Jingxiang, Guo Quanyi, Lu Xiaobo. Decellularized porcine skin matrix for tissue-engineered meniscus scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3473-3478. |
| [13] | Mo Jianling, He Shaoru, Feng Bowen, Jian Minqiao, Zhang Xiaohui, Liu Caisheng, Liang Yijing, Liu Yumei, Chen Liang, Zhou Haiyu, Liu Yanhui. Forming prevascularized cell sheets and the expression of angiogenesis-related factors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3479-3486. |
| [14] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| [15] | Liu Liyong, Zhou Lei. Research and development status and development trend of hydrogel in tissue engineering based on patent information [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3527-3533. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||