Chinese Journal of Tissue Engineering Research ›› 2026, Vol. 30 ›› Issue (21): 5524-5533.doi: 10.12307/2026.777
Previous Articles Next Articles
Arthroscopy-assisted loop titanium plate versus clavicular hook plate for acute acromioclavicular joint dislocation: clinical efficacy and cost-effectiveness
Li Kanglin, Gao Shihua, Jiang Yongdong, Huang Ziqi, Wu Yufeng
- Zhongshan Hospital of Traditional Chinese Medicine Affiliated to Guangzhou University of Chinese Medicine, Zhongshan 528400, Guangdong Province, China
-
Accepted:2025-09-02Online:2026-07-28Published:2026-03-05 -
Contact:Wu Yufeng, MS, Master’s supervisor, Professor, Chief physician, Zhongshan Hospital of Traditional Chinese Medicine Affiliated to Guangzhou University of Chinese Medicine, Zhongshan 528400, Guangdong Province, China -
About author:Li Kanglin, Master candidate, Zhongshan Hospital of Traditional Chinese Medicine Affiliated to Guangzhou University of Chinese Medicine, Zhongshan 528400, Guangdong Province, China -
Supported by:Zhongshan City's First Batch of Social Welfare and Basic Research Projects (General Medical and Health Projects), No. 2021B1061 (to WYF)
CLC Number:
Cite this article
Li Kanglin, Gao Shihua, Jiang Yongdong, Huang Ziqi, Wu Yufeng. Arthroscopy-assisted loop titanium plate versus clavicular hook plate for acute acromioclavicular joint dislocation: clinical efficacy and cost-effectiveness[J]. Chinese Journal of Tissue Engineering Research, 2026, 30(21): 5524-5533.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
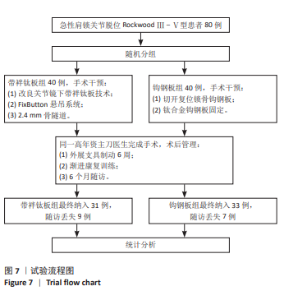
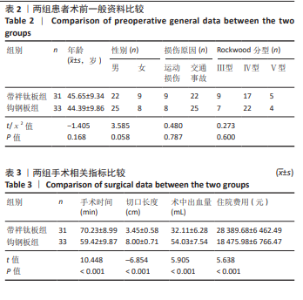
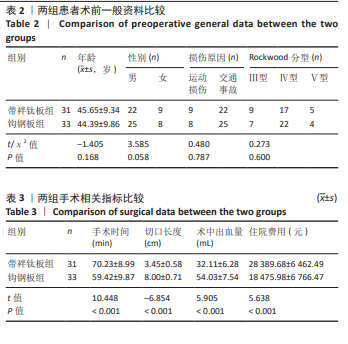
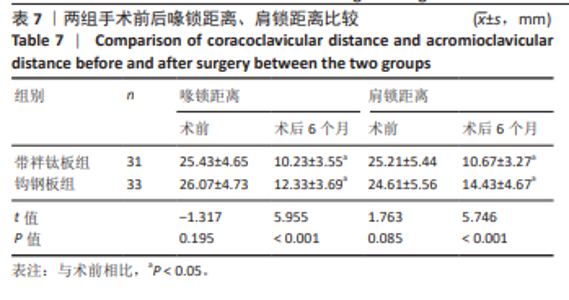
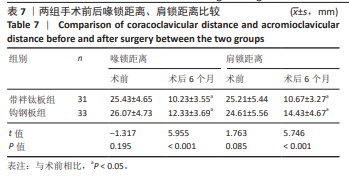
2.1 参与者数量分析 纳入急性 Ⅲ-Ⅴ型肩锁关节脱位患者80例,依据手术方式的不同分为带袢钛板组和钩钢板组,每组40 例。在研究进程中,部分患者因多种原因未能完成随访,最终进入结果分析的患者共 64 例,其中带袢钛板组31例,钩钢板组33例。 带袢钛板组脱落9例,具体原因如下:4 例患者在随访过程中失联,可能是由于患者更换联系方式后未及时告知研究团队,或因工作、生活变动等因素导致无法追踪;3例患者明确拒绝复查,因对复查流程存在抵触情绪或时间安排冲突等导致脱落;另有2例为其他原因,包括患者因严重基础疾病需优先治疗其他病症,以及因居住地变迁距离研究中心过远而放弃继续参与随访。 钩钢板组脱落7例,其中2例发生二次创伤,由于术后康复期间防护不当,导致肩部再次受损,从而影响了后续随访的进行;3例患者失联,原因与带袢钛板组失联患者类似,主要涉及联系方式变更和追踪困难;2例患者转院治疗,都因个人原因选择到其他医疗机构接受进一步诊治,进而退出了此次研究的随访。 2.2 试验流程图 见图7。"

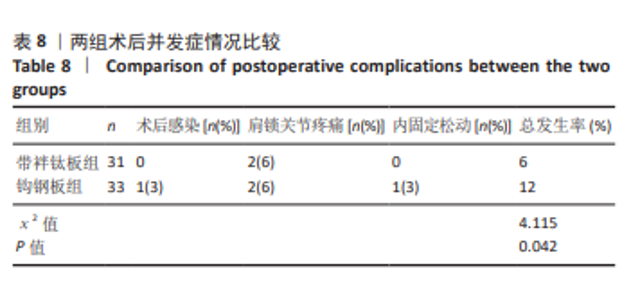
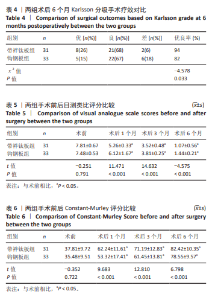
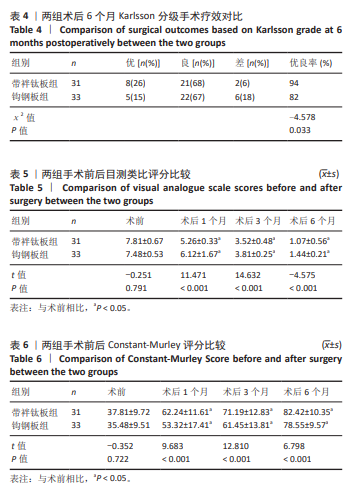
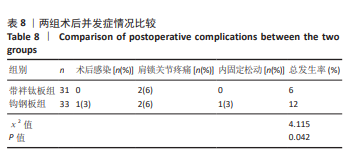
2.6 两组术后并发症情况 带袢钛板组术后感染、肩锁关节疼痛、内固定松动总发生率低于钩钢板组(P < 0.05)。对于术后感染患者,行抗生素抗感染治疗;对于肩锁关节疼痛者,予以口服止痛药,配合外敷药物、推拿、按摩、针灸、理疗等方法来缓解;对于内固定松动严重者,必要时考虑二次手术。见表8。 2.7 植入物与宿主的生物相容性 带袢钛板组术后未出现植入物周围感染、过敏反应、免疫反应及排斥反应,但发生2例原因不明的肩锁关节疼痛,经过一系列的药物理疗手段,最终患者疼痛缓解。分析疼痛原因,推测可能与术后组织修复过程中的炎症反应以及个人疼痛敏感程度有关。 锁骨钩钢板组术后出现1例植入物周围感染,但未出现明确的过敏反应、免疫或排斥反应。此外,还存在2例原因不明的肩锁关节疼痛和1例内固定松动,其中感染可能与手术创伤、术后护理相关,而非植入物本身的生物相容性问题。 综上,两种植入物在此次研究中均未表现出明显的过敏、免疫排斥等生物相容性相关不良反应。"
| [1] GU Y, ZHUANG Y. 3D printing-assisted surgery for the treatment of proximal clavicle fracture with ipsilateral acromioclavicular joint dislocation: a case description. Quant Imaging Med Surg. 2024;14(1): 1234-1240. [2] MAZZOCCA AD, ARCIERO RA, BICOS J. Evaluation and treatment of acromioclavicular joint injuries. Am J Sports Med. 2007;35(2):316-329. [3] HUANG J, HUANG D, WANG J, et al. A Modified Endoscopic Technique with Three Incisions for Rockwood Types III and V Acromioclavicular Joint Dislocation. Orthop Surg. 2023;15(2):648-654. [4] TAUBER M. Management of acute acromioclavicular joint dislocations: current concepts. Arch Orthop Trauma Surg. 2013;133(7):985-995. [5] FREGE S, LACHETA L, KARPINSKI K, et al. Influence of Tilt and Rotation on Coracoclavicular Distance Measurements and Rockwood Classification in Panorama View Radiographs in the Diagnosis of Acromioclavicular Dislocations. Orthop J Sports Med. 2025;13(4): 23259671251329344. [6] TUXUN A, KEREMU A, AILA P, et al. Combination of Clavicular Hook Plate with Coracoacromial Ligament Transposition in Treatment of Acromioclavicular Joint Dislocation. Orthop Surg. 2022;14(3):613-620. [7] TAUBER M, HOFFELNER T, LEHMANN L, et al. Prospective multicenter randomized controlled trial of surgical versus nonsurgical treatment for acute Rockwood type 3 acromioclavicular injury. Orthop J Sports Med. 2023;11(8):23259671231190411. [8] CHEN K, XU B, LAO YJ, et al. Risk factors related to the loss of reduction after acromioclavicular joint dislocation treated with the EndoButton device. Ann Transl Med. 2021;9(4):345. [9] KUMBARACI M, OZER A, BOZOGLAN M, et al. Can a coracoclavicular screw added to the clavicular hook plate reduce subacromial stress? A finite element analysis. Jt Dis Relat Surg. 2022;33(3):609-615. [10] JIANG H, TONG J, SHEN L, et al. Clinical outcomes of arthroscopy‐assisted modified triple endobutton plate fixation in rockwood type iii acute acromioclavicular joint dislocation: a retrospective study. Orthop Surg. 2022;14(10):2436-2446. [11] ELMARAGHY AW, DEVEREAUX MW, RAVICHANDIRAN K, et al. Subacromial morphometric assessment of the clavicle hook plate. Injury. 2010;41(6):613-619. [12] NADARAJAH R, MAHALUXMIVALA J, AMIN A, et al. Clavicular hook–plate: complications of retaining the implant. Injury. 2005;36(5):681-683. [13] ZHANG L, ZHOU X, QI J, et al. Modified closed-loop double-endobutton technique for repair of rockwood type III acromioclavicular dislocation. Exp Ther Med. 2018;15(1):940-948. [14] ELHALAWANY MF, ABDALLA UG, SHWITTER L, et al. Assessment of Coracoclavicular Ligament Healing on MRI After Arthroscopic TightRope Fixation for Acute Acromioclavicular Joint Dislocation. Orthop J Sports Med. 2023;11(10):23259671231185749. [15] XIE C, HONG Z, SU Y, et al. No Significant Difference Between Suture Button and Hook Plate in Treating Acute Rockwood Type III Acromioclavicular Joint Dislocation: A Systematic Review. Arthroscopy. 2025;41(7):2598-2610. [16] YU P, ZHANG Y, YE T, et al. Clinical and radiological outcomes of acute Rookwood type IIIB acromioclavicular joint dislocation: Mini-open tightrope technique versus hook plate. Injury. 2023;54 Suppl 2: S63-S69. [17] OZCAFER R, ALBAYRAK K, LAPCIN O, et al. Early clinical and radiographic results of fixation with the TightRope device for Rockwood type V acromioclavicular joint dislocation: A retrospective review of 15 patients. Acta Orthop Traumatol Turc. 2020;54(5):473-477. [18] ZHANG L, HE AN, JIN YF, et al. Novel Double Endobutton Technique Combined with Three-Dimensional Printing: A Biomechanical Study of Reconstruction in Acromioclavicular Joint Dislocation. Orthop Surg. 2020;12(5):1511-1519. [19] CHEN K, XU B, LAO YJ, et al. Risk factors related to the loss of reduction after acromioclavicular joint dislocation treated with the EndoButton device. Ann Transl Med. 2021;9(4):345. [20] SALZMANN GM, WALZ L, SCHOETTLE PB, et al. Arthroscopic anatomical reconstruction of the acromioclavicular joint. Acta Orthopaedica Belgica. 2008;74(3):397-400. [21] ROSSLENBROICH SB, SCHLIEMANN B, SCHNEIDER KN, et al. Minimally Invasive Coracoclavicular Ligament Reconstruction With a Flip-Button Technique (MINAR): Clinical and Radiological Midterm Results. Am J Sports Med. 2015;43(7):1751-1757. [22] YAN Y, LIAO M, LAI H, et al. Comparison of Effectiveness and Safety in Treating Acute Acromioclavicular Joint Dislocation with Five Different Surgical Procedures: A Systematic Review and Network Meta-Analysis. Orthop Surg. 2023;15(8):1944-1958. [23] XIE C, FAN S, CHEN L, et al. Comparative efficacy of operative versus conservative treatment for Rockwood type III acromioclavicular joint dislocation: a systematic review and meta-analysis of randomized controlled trials. BMC Musculoskelet Disord. 2024;25(1):960. [24] AKGUN D, GEBAUER H, PAKSOY A, et al. Comparison of Clinical Outcomes Between Nonoperative Treatment and Arthroscopically Assisted Stabilization in Patients With Acute Rockwood Type 5 Acromioclavicular Dislocation. Orthop J Sports Med. 2024;12(11): 23259671241289117. [25] MALEITZKE T, BARTHOD-TONNOT N, MAZIAK N, et al. Noninvasive bracing of acromioclavicular joint dislocations is not superior to early functional rehabilitation and not inferior to surgical stabilization in Rockwood type III and V injuries. J Shoulder Elbow Surg. 2025;34(5): 1236-1244. [26] VOSSEN RJM, VERSTIFT D, VAN ETTEN-JAMALUDIN FS, et al. Choice of Acromioclavicular Dislocation Treatment Should Not Be Influenced by Risk of Development of Acromioclavicular Osteoarthritis: A Systematic Review With Meta-Analysis. JBJS Rev. 2024;12(9):e24.00085. [27] LI Y, TIAN Q, LENG K, et al. Risk factors for clavicular midshaft fractures after hook plate fixation for the treatment of Neer type II clavicular fractures. J Int Med Res. 2021;49(8):3000605211035898. [28] LIU G, HU Y, YE F, et al. Clavicular hook plate for acute high-grade acromioclavicular dislocation involving Rockwood type V: clinical and radiological outcomes and complications evaluation. Int Orthop. 2022;46(10):2405-2411. [29] CHANG HM, HONG CK, SU WR, et al. Comparison of clavicular hook plate with and without coracoclavicular suture fixation for acute acromioclavicular joint dislocation. Acta Orthop Traumatol Turc. 2019; 53(6):408-413. [30] HUANG L, CAI L, FAN M, et al. Subacromial osteolysis following hook plate fixation for acromioclavicular dislocation: a systematic review and meta-analysis. J Shoulder Elbow Surg. 2024;33(9):2086-2095. [31] LEE YS, KIM DS, JUNG JW, et al. Risk factors of loss of reduction after acromioclavicular joint dislocation treated with a hook plate. J Orthop Traumatol. 2023;24(1):10. [32] PAN X, LV RY, LV MG, et al. TightRope vs Clavicular Hook Plate for Rockwood III-V Acromioclavicular Dislocations: A Meta-Analysis. Orthop Surg. 2020;12(4):1045-1052. [33] VOIGHT ML, NORMAN C, WILK KE, et al. Management of High Ankle Sprains Utilizing the Tightrope Surgical Procedure - A Novel Approach for a Rapid Return to Play. Int J Sports Phys Ther. 2024;19(5):513-521. [34] VENJAKOB AJ, SALZMANN GM, GABEL F, et al. Arthroscopically assisted 2-bundle anatomic reduction of acute acromioclavicular joint separations: 58-month findings. Am J Sports Med. 2013;41(3): 615-621. [35] ZHANG L, XIONG L, ZHOU X, et al. Computed Tomography-Based Determination of the Optimal Locations of Bone Tunnels for Coracoclavicular Ligament Reconstruction. Orthop Surg. 2022;14(10): 2692-2700. [36] QI J, FU S, PING R, et al. Biomechanical testing of three coracoclavicular ligament reconstruction techniques with a 3D printing navigation template for clavicle-coracoid drilling. Ann Transl Med. 2021;9(14): 1121. [37] ARMITAGE MS, ELKINSON I, GILES JW, et al. An anatomic, computed tomographic assessment of the coracoid process with special reference to the congruent-arc latarjet procedure. Arthroscopy. 2011;27(11): 1485-1489. [38] BELLMANN F, ECKL L, VETTER P, et al. Clavicular Tunnel Widening After Acromioclavicular Stabilization Shows Implant-Dependent Correlation With Postoperative Loss of Reduction. Arthroscopy. 2023;39(11): 2273-2280. [39] VELASQUEZ GARCIA A, FRANCO ABACHE A, INGALA MARTINI L. Clavicular tunnel widening after coracoclavicular stabilization surgery: a systematic review and meta-analysis. J Shoulder Elbow Surg. 2024; 33(3):738-755. [40] SPIEGL UJ, SMITH SD, EULER SA, et al. Biomechanical Consequences of Coracoclavicular Reconstruction Techniques on Clavicle Strength. Am J Sports Med. 2014;42(7):1724-1730. [41] LIM TK, OH WK. Intraoperative and Postoperative Complications after Arthroscopic Coracoclavicular Stabilization. Clin Orthop Surg. 2019;11(1):103-111. [42] YOO JH, MIN BC, SUNG KH, et al. Fracture of the coracoid process with acute subscapularis tear without shoulder dislocation. Indian J Orthop. 2014;48(6):625-627. [43] LI H, JIANG F, GE Y, et al. Differences in artificial ligament graft osseointegration of the anterior cruciate ligament in a sheep model: a comparison between interference screw and cortical suspensory fixation. Ann Transl Med. 2021;9(17):1370. [44] CHA Y, YOO JI, KIM JT, et al. How to Solve Anatomical Mismatch in Fixation of Acetabular Fractures Using an Anatomical Quadrilateral Surface Plate. Clin Orthop Surg. 2023;15(2):338-342. [45] ZHU W, XU L, XIE K, et al. Design and Validation of a Smile-Necklace Plate for Treating Inferior Patellar Pole Avulsion Fractures: A Review and Hypothesis. Orthop Surg. 2022;14(11):2799-2808. [46] LIU B, MA Z, LI J, et al. Experimental study of a 3D printed permanent implantable porous Ta-coated bone plate for fracture fixation. Bioact Mater. 2022;10:269-280. [47] VENJAKOB AJ, SALZMANN GM, GABEL F, et al. Arthroscopically assisted 2-bundle anatomic reduction of acute acromioclavicular joint separations: 58-month findings. Am J Sports Med. 2013;41(3): 615-621. [48] CHAUDHARY D, JAIN V, JOSHI D, et al. Arthroscopic fixation for acute acromioclavicular joint disruption using the TightRope device. J Orthop Surg (Hong Kong). 2015;23(3):309-314. [49] LI Y, CAI J, LI P, et al. Suture Button Could Result in More Functional Outcomes Improvement and Pain Relief Than Hook Plate Technique for Treating Acute Acromioclavicular Joint Dislocation: A Systematic Review of Comparative Studies. Arthroscopy. 2024;40(2):553-566. [50] LI D, ZHANG Z, WANG X. Treatment of acromioclavicular joint dislocation with looped steel plate and clavicular hook steel plate: recent therapeutic observation. J Pak Med Assoc. 2024;74(10): 1791-1795. [51] CHANG YH, CHANG SW, LIU CY, et al. Demographic characteristics and complications of open and minimally invasive surgeries for renal cell carcinoma: a population-based case-control study in Taiwan. Ther Clin Risk Manag. 2018;14:1235-1241. |
| [1] | Liu Jinlong, Abuduwupuer·Haibier, Bai Zhen, Su Danyang, Miao Xin, Li Fei, Yang Xiaopeng. Efficacy of different nonsurgical treatments for adolescent idiopathic scoliosis: a systematic review and network meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2370-2379. |
| [2] | Yang Qiongqiong, Liu Wei. Comparison of performance and clinical effects of zirconia and titanium implants [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 2063-2071. |
| [3] | Wang Zhenze, Liu Fende, Zhang Rui, Li Wujun. Mesenchymal stem cells in treatment of arteriosclerosis obliterans of lower extremities: systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(7): 1869-1876. |
| [4] | Wang Yalei, Wang Xuezhi, Zhou Tao, Shen Xinxin, Fang Ding, Chen Hongliang. Effect of sacroiliac joint ankylosis on outcomes of L5/S1 transforminal lumbar interbody fusion and lumbar sagittal parameters [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(3): 634-641. |
| [5] | Liao Guangtao, Feng Ziyu, Fu Xiaoyong, Zhao Qinglan, Chen Chao, Hong Jinsong. Subtalar arthroereisis for treatment of pediatric flexible flatfoot: relationship between radiographic indicators and clinical efficacy [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(3): 661-670. |
| [6] | Wang Shili, Luo Yuan, Qiao Li, Yang Yonghong, Zhang Yujie, Zhang Shun. Relationship between blood drug concentration and safety of vancomycin in patients with orthopedic infection determined by ultra-performance liquid chromatography-tandem mass spectrometry [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(21): 5494-5502. |
| [7] | Zhang Ping, Zhou Dafang, Chen Hui, Zhang Ying, Liu Qing, Shi Ce. Application of a modified rectangular locking device in the treatment of femoral shaft fractures with intramedullary nailing [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(21): 5510-5516. |
| [8] | Hu Yujie, Xie Ping, , Lu Weijie, Yang Kang, Deng Yaoting, Liu Mengyang. Meta-analysis of the clinical efficacy of high-intensity interval exercise and middle-intensity continuous training in patients with coronary heart disease [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(10): 2584-2593. |
| [9] | Yu Ming, Wang Wen. Posterior cruciate ligament tibial attachment point avulsion fracture: materials, implants, and internal fixation techniques in arthroscopic treatment [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(4): 872-880. |
| [10] | Liu Ning, Sun Yingjin, Huang Long, Feng Shuo, Chen Xiangyang. Optimal rotational alignment of the tibial component during Oxford unicompartmental knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(33): 7158-7164. |
| [11] | Jiang Zehua, Du Wenjun, Ren Zhishuai, Cui Haojun, Zhu Rusen. Percutaneous vertebroplasty via Kambin's triangle for treatment of osteoporotic compression fractures: evaluation of safety and effectiveness [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(33): 7181-7188. |
| [12] | Lin Qing, Liu Huan, Cheng Yongzhong, Jiang Junjie, Li Yongyao, Li Guangyao. Meta-analysis of external stent fixation and internal plate fixation for treatment of comminuted distal radius fractures [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(21): 4602-4611. |
| [13] | Cao Zhengpei, Lu Shengsheng, Zhang Jiahuan, Wang Xiaoying. Effects of silver needle comprehensive therapy on the ultrasonographic morphology of multifidus muscles in patients with lumbar disc herniation: an ultrasound morphologic assessment [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(11): 2261-2267. |
| [14] | Zhang Xiaoyun, Liu Hua, Chai Yuan, Chen Feng, Zeng Hao, Gao Zhengang, Huang Yourong. Effect of Yishen Gushu Formula on bone metabolic markers and clinical efficacyn in patients with osteoporosis of kidney deficiency and blood stasis type [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1155-1160. |
| [15] | Huang Jie, Shi Yanghua, Tan Zhen, Bo Zhandong. Free vascularized fibular grafting in treatment of femoral head osteonecrosis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(21): 3373-3379. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||