Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (7): 1101-1108.doi: 10.3969/j.issn.2095-4344.2014.07.020
Previous Articles Next Articles
Biomechanical progress of fatigue effect on non-contact anterior cruciate ligament injury
Liu Hai-rui1, Wu Xie2, Wu Ying1
- 1School of Physical Education and Coaching, Shanghai University of Sport, Shanghai 200438, China; 2School of Kinesiology, Shanghai University of Sport, Shanghai 200438, China
-
Revised:2013-12-05Online:2014-02-12Published:2014-02-12 -
Contact:Wu Ying, M.D., Professor, Doctoral supervisor, School of Physical Education and Coaching, Shanghai University of Sport, Shanghai 200438, China -
About author:Liu Hai-rui, Studying for doctorate, School of Physical Education and Coaching, Shanghai University of Sport, Shanghai 200438, China -
Supported by:the Leading Academic Discipline Project of Shanghai Education Committee, No. J51001; Shanghai Postgraduate Education Innovation Program in 2012; New Academic Development Plan for Liberal Arts Graduate Students in Local Universities of Shanghai, No. xsxr2012034
CLC Number:
Cite this article
Liu Hai-rui, Wu Xie, Wu Ying. Biomechanical progress of fatigue effect on non-contact anterior cruciate ligament injury[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(7): 1101-1108.
share this article
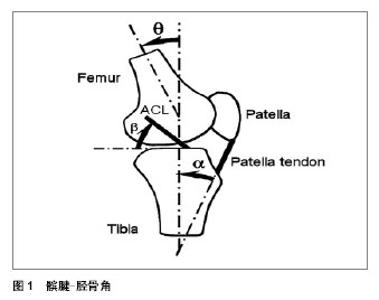
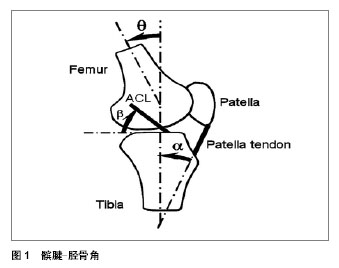
2.1 前交叉韧带损伤机制 从机械的角度看前交叉韧带损伤多发生在前交叉韧带承受过大的张力时。因此,了解人体在运动时前交叉韧带负载的机制是了解非接触性前交叉韧带损伤的重要因素。前交叉韧带损伤的机制主要发生在3个解剖面上增加的膝关节外翻角度,增加的膝关节旋内和降低的膝关节屈曲角度。 2.1.1 膝关节外翻 Berns等[11]研究发现发现较大的膝关节负荷(胫骨近端和膝关节外翻力矩的前切力)会导致前交叉韧带的紧绷。类似的研究也观察了胫骨近端的前切力和膝关节外翻,内翻,内外旋转力矩应用在前交叉韧带上的情况。一个100 N的前切力和10 N·m的膝关节内外翻和内外旋力矩被应用到尸体的膝关节上。前交叉韧带的负载被记录下来并显示膝关节从伸展的90°显示胫骨的前切力使前交叉韧带产生明显的负荷。同时,膝关节内外翻和内外旋对前交叉韧带也产生了明显的负荷,但研究显示仅是当前切力在胫骨近端时,前交叉韧带才有较为明显的负荷。这项研究进一步显示前交叉韧带的负载在前切力加上外翻或者内翻力矩时比仅有前切力时要大,同时,前交叉韧带的负载在前切力加上膝关节外旋力矩时比仅有前切力时要小。因此外翻力矩会增加前交叉韧带的负载已被以往的文献得到证实[12]。但是也有文献显示施加外翻负载后前交叉韧带张力增加并不明显,特别是在2003年,Mazzocca等[13]的研究显示副侧韧带被外翻负荷破坏后才观察到前交叉韧带张力的增加。Hewett等[14]的流行病研究显示在垂直落地-跳跃的任务中外旋的膝关节外翻力矩是预测前交叉韧带损伤的一个因素。研究跟踪了共205名高中足球、篮球和排球运动员3个赛季的比赛训练,并记录了受试者在垂直的落地-跳跃触地时,最大的膝关节屈曲和外翻角度和最大的力矩。9名受试者在3个赛季后出现前交叉韧带损伤。研究结果显示落地时前交叉韧带损伤发病者的膝关节外翻角是8°,远高于非损伤的受试者,前交叉韧带损伤者的膝关节外旋外翻力矩和反作用力分别是非受伤者的2.5倍,大约高20%。调查结果进一步揭示膝关节外翻角度,膝关节外翻力矩与前交叉韧带损伤的关系。 2.1.2 膝关节旋内 Olsen等[15]认为膝关节的外翻加上下肢较大的冲击负荷,会导致胫骨的内外旋,在这种条件下极易出现前交叉韧带损伤。Shin等[16]采用模型模拟的方式评估了外翻角度,外翻力矩,胫骨的旋转和内副侧韧带的张力对前交叉韧带损伤的影响。研究证实增加的外翻力矩和前交叉韧带的张力峰值并非永远呈线性关系。研究还显示因为骨和软组织的限制,外翻力矩增加时会导致胫骨的外旋。研究认为单纯的增大的外翻力矩会增加前交叉韧带的张力,但是并不足以造成前交叉韧带损伤,除非内副侧韧带被破坏。因为,胫骨的旋外和增加的内副侧韧带的张力会抑制前交叉韧带张力的增加。这一结论也印证了之前的研究结果:单纯的膝关节外翻角度可能会造成前交叉韧带损伤,但是更多的前交叉韧带损伤出现在胫骨的旋内(外)时,伴随的膝关节完全的伸展和较大的外翻角度和外翻力矩。膝外翻和旋外力矩是导致膝关节动态运动时外翻的主要因素,这也是现有很多前交叉韧带损伤预防训练想要避免的方面。落地时,髋关节屈曲的减小,会增大膝关节的冲击力。较为伸展的的髋关节落地角度极易导致产生较大的膝关节外展力矩。相比男性,女子运动员落地时膝关节外翻力矩较大。研究还显示前交叉韧带的负载在膝关节内翻加上内旋力矩时要比仅膝关节内翻力矩或者仅内旋力矩要大。而比较前交叉韧带的负载在膝关节外翻加上外旋力矩时比仅膝关节外翻或者外旋力矩要小。除此之外,前交叉韧带的负荷在前切力和膝关节外翻,内翻和内旋力矩在膝关节屈曲角度减小时会增大。Feagin等[17]的研究显示体质量的影响和胫骨外旋的负荷可以造成前交叉韧带的紧绷。他们在1个受试者的前交叉韧带的前内侧植入了可变磁阻变换器来独立检测胫骨前后切力,内外翻力矩和内外旋力矩来模拟体质量对膝关节负载的影响。研究结果表明前交叉韧带在胫骨近端的前切力和膝关节内旋力矩增加的情况下紧绷明显增大。同时,膝关节内外翻和外旋力矩在承受体质量的条件下对前交叉韧带的紧绷影响有限。上述研究一致表明前切力在胫骨近端对前交叉韧带负载的大小起主要的作用。同时当胫骨近端的前切力作用于膝关节时,会导致胫骨的旋内,从而可能增加前交叉韧带的负载。通过这些前交叉韧带负载机制,较小的膝关节屈曲角度,四头肌强有力的收缩或者额状面向后较大的地面反作用力都能够增加前交叉韧带的负荷。 2.1.3 膝关节屈曲角 四头肌通过髌腱在胫骨近端是主要作用于前切力的肌肉。Dargel等[18]发现四头肌的肌力在膝关节从0°-45°屈曲时能够明显的增加。Durselen等[19]发现膝关节从完全伸展至30°屈曲,四头肌能导致前交叉韧带承受较高的张力,当膝关节屈曲角度增加且超过30°时,前交叉韧带的紧绷程度开始减小。其他的研究也有类似结果(等动肌力中四头肌肌力在屈曲15°-30°时,明显的使得前交叉韧带绷紧,张力增加)。 Shoemaker等[20]的研究显示四头肌对胫骨的额状面移动和和转移前交叉韧带的张力有显著的效果。四头肌最大的张力转接发生在膝关节3°屈曲。降低的膝关节屈曲角度通过髌腱-胫骨角(patella tendon-tibia shaft angle) (图1)可以增加胫骨近端的前切力。在给定四头肌肌力的条件下,胫骨近端的前切力主要由髌 腱-胫骨角决定,定义为髌腱和胫骨纵向轴线之间的夹角。在四头肌给定的条件下,这个角度越大,胫骨的前切力也就越大。Nunley等[21]研究了这个角度和膝关节屈曲角度的关系。研究显示当髌腱-胫骨角增大时,膝关节屈曲角度减小。女性的这个角度的平均值约4°左右,大于男性。这项研究中有关髌腱-胫骨角与膝关节屈曲角度的研究结果也与Boden等[5]的研究相一致:膝关节屈曲角度的减小会导致前交叉韧带倾斜角和偏移角增大,进而导致增大前交叉韧带负载。纵轴上的前交叉韧带的合力等于cosines之后的前交叉韧带倾斜角和偏移角除以前交叉韧带的前切力。前交叉韧带倾斜角和偏移角越大,基于在前交叉韧带上的前切力,前交叉韧带的负载也就越大。Herzog等[22]研究的显示膝关节屈曲的减小导致前交叉韧带活动的直线更垂直,意味着前交叉韧带倾斜角的增加。Dargel等[18]研究还显示四头肌收缩在0°-45°明显会导致前交叉韧带的紧绷。类似的结论也出现在落地的研究中,落地或者变向时矢状面和额状面的不规则的关节角度和力矩都有可能导致非接触性的前交叉韧带损伤,特别是女子运动员。大量体内和体外的研究显示前交叉韧带张力的峰值一般出现在膝关节15°-40°屈曲时,并在超过40°以后减小至0°。计算机模拟的研究进一步显示触地后25 ms时前交叉韧带的张力峰值最大,此时膝关节接近于完全伸展。而研究也证实前交叉韧带损伤经常出现在落地减速阶段或者变向阶段[23]。也有研究认为前交叉韧带损伤一般出现在触地后(initial contact)的 50 ms左右,在这个时刻股二头肌的作用是作为对抗前交叉韧带的角色。在体实验也显示单足跳的测试中,前交叉韧带张力的峰值和垂直地面反作用力峰值出现时刻一致,这主要与触地时刻较为伸展的膝关节屈曲角度有关。"
| [1] Myer GD, Ford KR, Hewett TE. ationale and Clinical Techniques for Anterior Cruciate Ligament Injury Prevention Among Female Athletes. J Athl Train. 2004; 39(4):352-364. [2] Porter DA, Duncan M, Meyer SJ. Fifth metatarsal Jones fracture fixation with a 4.5-mm cannulated stainless steel screw in the competitive and recreational athlete: a clinical and radiographic evaluation. Am J Sports Med. 2005;33(5): 726-733.[3] Orishimo KF, Kremenic IJ. Effect of fatigue on single-leg hop landing biomechanics. J Appl Biomech. 2006;22(4): 245-254.[4] Matava MJ, Freehill AK, Grutzner S, et al. Limb dominance as a potential etiologic factor in noncontact anterior cruciate ligament tears. J Knee Surg. 2002;15(1):11-16. [5] Boden BP, Dean GS, Feagin JA Jr, et al. Mechanisms of anterior cruciate ligament injury. Orthopedics. 2000;23(6): 573-578.[6] Huston LJ, Greenfield ML, Wojtys EM. Anterior cruciate ligament injuries in the female athlete. Potential risk factors. Clin Orthop Relat Res. 2000;(372):50-63. [7] Griffin LY, Albohm MJ, Arendt EA, et al. Understanding and preventing noncontact anterior cruciate ligament injuries: a review of the Hunt Valley II meeting, January 2005. Am J Sports Med. 2006;34(9):1512-1532.[8] DeVita P, Hong D, Hamill J. Effects of asymmetric load carrying on the biomechanics of walking. J Biomech. 1991; 24(12):1119-1129.[9] Hootman JM, Dick R, Agel J. Epidemiology of collegiate injuries for 15 sports: summary and recommendations for injury prevention initiatives. J Athl Train. 2007;42(2): 311-319. [10] Lepers R, Hausswirth C, Maffiuletti N, et al. Evidence of neuromuscular fatigue after prolonged cycling exercise. Med Sci Sports Exerc. 2000;32(11):1880-1886. [11] Berns GS, Hull ML, Patterson HA. Strain in the anteromedial bundle of the anterior cruciate ligament under combination loading. J Orthop Res. 1992;10(2): 167-176. [12] Kernozek TW, Torry MR, Iwasaki M. Gender differences in lower extremity landing mechanics caused by neuromuscular fatigue. Am J Sports Med. 2008;36(3):554-565. [13] Mazzocca AD, Nissen CW, Geary M, et al. Valgus medial collateral ligament rupture causes concomitant loading and damage of the anterior cruciate ligament. Knee Surg. 2003; 16(3):148-151. [14] Hewett TE, Myer GD, Ford KR, et al. Biomechanical measures of neuromuscular control and valgus loading of the knee predict anterior cruciate ligament injury risk in female athletes: a prospective study. Am J Sports Med. 2005;33(4): 492-501.[15] Olsen OE, Myklebust G, Engebretsen L, et al. Injury mechanisms for anterior cruciate ligament injuries in team handball: a systematic video analysis. Am J Sports Med. 2004;32(4):1002-1012. [16] Shin CS, Chaudhari AM, Andriacchi TP. The effect of isolated valgus moments on ACL strain during single-leg landing: a simulation study. J Biomech. 2009;42(3):280-285. [17] Feagin JA Jr, Lambert KL. Mechanism of injury and pathology of anterior cruciate ligament injuries. Orthop Clin North Am. 1985;16(1):41-45.[18] Dargel J, Gotter M, Mader K, et al. omechanics of the anterior cruciate ligament and implications for surgical reconstruction. Strategies Trauma Limb Reconstr. 2007; 2(1):1-12. [19] Dürselen L, Claes L, Kiefer H. The influence of muscle forces and external loads on cruciate ligament strain. Am J Sports Med. 1995;23(1):129-136.[20] Shoemaker SC, Adams D, Daniel DM, et al. Quadriceps/anterior cruciate graft interaction. An in vitro study of joint kinematics and anterior cruciate ligament graft tension. Clin Orthop Relat Res. 1993;(294):379-390.[21] Nunley RM, Wright D, Renner JB, et al. Research in Sports Medicine.2003;11(3):173-185.[22] Herzog W, Read LJ. Lines of action and moment arms of the major force-carrying structures crossing the human knee joint. J Anat. 1993;182 ( Pt 2):213-230.[23] Boden BP, Sheehan FT, Torg JS, et al. Noncontact anterior cruciate ligament injuries: mechanisms and risk factors. J Am Acad Orthop Surg. 2010;18(9):520-527. [24] Kingma I, Aalbersberg S, van Dieën JH. Are hamstrings activated to counteract shear forces during isometric knee extension efforts in healthy subjects? J Electromyogr Kinesiol. 2004;14(3):307-315.[25] Gabbett TJ. Incidence of injury in amateur rugby league sevens. Br J Sports Med. 2002;36(1):23-26. [26] Hiemstra LA, Lo IK, Fowler PJ. Effect of fatigue on knee proprioception: implications for dynamic stabilization. J Orthop Sports Phys Ther. 2001;31(10):598-605.[27] Wojtys EM, Huston LJ, Schock HJ, et al. Gender differences in muscular protection of the knee in torsion in size-matched athletes. J Bone Joint Surg Am. 2003;85-A(5):782-789.[28] Henriksen M, Aaboe J, Simonsen EB, et al. Experimentally reduced hip abductor function during walking: Implications for knee joint loads. J Biomech.2009;42(9):1236-1240. [29] Buckley JP, Borg GA. Borg's scales in strength training; from theory to practice in young and older adults. Appl Physiol Nutr Metab. 2011;36(5):682-692.[30] Madigan ML, Pidcoe PE. Changes in landing biomechanics during a fatiguing landing activity. J Electromyogr Kinesiol. 2003;13(5):491-498. [31] Coventry E, O'Connor KM, Hart BA, et al. The effect of lower extremity fatigue on shock attenuation during single-leg landing. Clin Biomech (Bristol, Avon). 2006;21(10): 1090-1097. [32] Orishimo KF, Kremenic IJ. Effect of fatigue on single-leg hop landing biomechanics. J Appl Biomech. 2006;22(4): 245-254. [33] Chappell JD, Herman DC, Knight BS, et al. Effect of fatigue on knee kinetics and kinematics in stop-jump tasks. Am J Sports Med. 2005;33(7):1022-1029.[34] Pappas E, Hagins M, Sheikhzadeh A, et al. Peak biomechanical variables during bilateral drop landings: comparisons between sex (female/male) and fatigue (pre-fatigue/post-fatigue). N Am J Sports Phys Ther. 2009; 4(2):83-91. [35] Gehring D, Melnyk M, Gollhofer A. Gender and fatigue have influence on knee joint control strategies during landing. Clin Biomech (Bristol, Avon). 2009;24(1):82-87. [36] Brazen DM, Todd MK, Ambegaonkar JP, et al. The effect of fatigue on landing biomechanics in single-leg drop landings. Clin J Sport Med. 2010;20(4):286-292. [37] Webster KE, Santamaria LJ, McClelland JA, et al. Effect of fatigue on landing biomechanics after anterior cruciate ligament reconstruction surgery. Med Sci Sports Exerc. 2012; 44(5):910-916.[38] Borotikar BS, Newcomer R, Koppes R, et al. Combined effects of fatigue and decision making on female lower limb landing postures: central and peripheral contributions to ACL injury risk. in Biomech (Bristol, Avon). 2008;23(1): 81-92.[39] Sanna G, O'Connor KM. Fatigue-related changes in stance leg mechanics during sidestep cutting maneuvers. Clin Biomech (Bristol, Avon). 2008;23(7):946-954. [40] Thomas AC, McLean SG, Palmieri-Smith RM. Quadriceps and hamstrings fatigue alters hip and knee mechanics. J Appl Biomech. 2010;26(2):159-170. [41] Lucci S, Cortes N, Van Lunen B, et al. Knee and hip sagittal and transverse plane changes after two fatigue protocols. J Sci Med Sport. 2011;14(5):453-459.[42] Ortiz A, Olson SL, Etnyre B, et al. Fatigue effects on knee joint stability during two jump tasks in women. J Strength Cond Res. 2010;24(4):1019-1027. |
| [1] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [2] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [3] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Multiple problems in the selection of implants for patellar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1440-1445. |
| [4] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [5] | Zhong Hehe, Sun Pengpeng, Sang Peng, Wu Shuhong, Liu Yi. Evaluation of knee stability after simulated reconstruction of the core ligament of the posterolateral complex [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 821-825. |
| [6] | Xu Yulin, Shen Shi, Zhuo Naiqiang, Yang Huilin, Yang Chao, Li Yang, Zhao Heng, Zhao Lu. Biomechanical comparison of three different plate fixation methods for acetabular posterior column fractures in standing and sitting positions [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 826-830. |
| [7] | Cai Qunbin, Zou Xia, Hu Jiantao, Chen Xinmin, Zheng Liqin, Huang Peizhen, Lin Ziling, Jiang Ziwei. Relationship between tip-apex distance and stability of intertrochanteric femoral fractures with proximal femoral anti-rotation nail: a finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 831-836. |
| [8] | Liu Shaohua, Zhou Guanming, Chen Xicong, Xiao Keming, Cai Jian, Liu Xiaofang. Influence of anterior cruciate ligament defect on the mid-term outcome of fixed-bearing unicompartmental knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 860-865. |
| [9] | Song Chengjie, Chang Hengrui, Shi Mingxin, Meng Xianzhong. Research progress in biomechanical stability of lateral lumbar interbody fusion [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 923-928. |
| [10] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Intravenous, topical tranexamic acid alone or their combination in total knee arthroplasty: a meta-analysis of randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 948-956. |
| [11] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| [12] | Liu Xin, Yan Feihua, Hong Kunhao. Delaying cartilage degeneration by regulating the expression of aquaporins in rats with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 668-673. |
| [13] | Xie Chongxin, Zhang Lei. Comparison of knee degeneration after anterior cruciate ligament reconstruction with or without remnant preservation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 735-740. |
| [14] | Ma Ziyue, Ju Xiaochen, Zhang Lei, Sun Rongxin. Tendon-bone healing in anterior cruciate ligament reconstruction with and without remnant preservation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 582-587. |
| [15] | Nie Shaobo, Li Jiantao, Sun Jien, Zhao Zhe, Zhao Yanpeng, Zhang Licheng, Tang Peifu. Mechanical stability of medial support nail in treatment of severe osteoporotic intertrochanteric fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 329-333. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||