Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (15): 2297-2302.doi: 10.3969/j.issn.2095-4344.3811
Biomechanical characteristics of a sleeve-type guided growth rod in a six-degree-of-freedom joint robot
Xue Jingbo, Zhu Bin, Li Zepeng, Wang Cheng, Ouyang Zhihua, Yan Yiguo
- Department of Spine Surgery, The First Affiliated Hospital of University of South China, Hengyang 421001, Hunan Province, China
-
Received:2020-06-28Revised:2020-07-02Accepted:2020-08-22Online:2021-05-28Published:2021-01-04 -
Contact:Yan Yiguo, MD, Chief physician, Department of Spine Surgery, The First Affiliated Hospital of University of South China, Hengyang 421001, Hunan Province, China -
About author:Xue Jingbo, MD, Associate chief physician, Department of Spine Surgery, The First Affiliated Hospital of University of South China, Hengyang 421001, Hunan Province, China -
Supported by:the Clinical Medical Technology Innovation Guidance Program Project of Hunan Province, No. 2017SK50202 (to XJB); the Scientific Research Project of Hunan Provincial Health and Family Planning Commission, No. 20180154 (to XJB)
CLC Number:
Cite this article
Xue Jingbo, Zhu Bin, Li Zepeng, Wang Cheng, Ouyang Zhihua, Yan Yiguo. Biomechanical characteristics of a sleeve-type guided growth rod in a six-degree-of-freedom joint robot [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(15): 2297-2302.
share this article
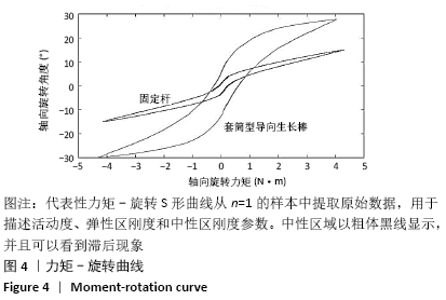
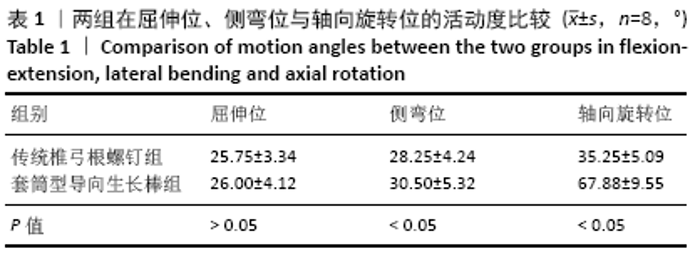
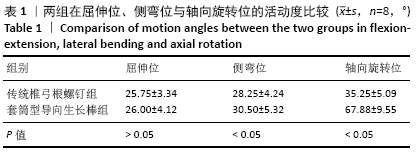
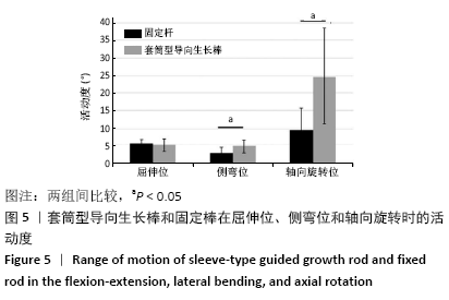
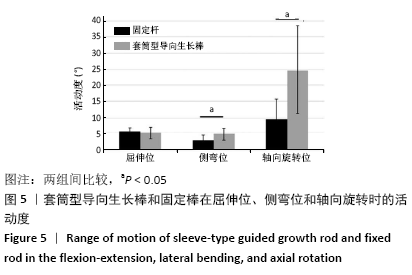
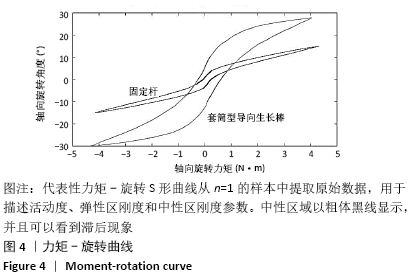
2.1 样本情况 在所有测试参数下,所有样本的检测均为非破坏性;测试完成时,未出现内植物断裂、骨折或软组织损伤等相关并发症;并且在研究结束取出内植物时未发现螺钉松动。 2.2 套筒型导向生长棒和固定棒在屈伸位、侧弯位及轴向旋转位的活动度比较 如代表性力矩-旋转曲线所示,当使用套筒型导向生长棒和固定棒进行检测时,样本都呈现出经典的S型曲线,并具有明确的中性区、弹性区和滞后现象,见图4。从这些曲线计算出来的活动度中可以看出,在所测试的3个方向运动中,套筒型导向生长棒在侧弯位和轴向旋转运动时其活动度显著增加(表1、图5),在测试前后生长棒的长度之间没有显著区别;套筒型导向生长棒在屈伸位的活动度为(26.00±4.12)°,而固定棒为(25.75±3.34)°,两者在屈伸位活动度之间的差异无显著性意义(P > 0.05);套筒型导向生长棒杆在侧弯位活动度为(30.50±5.32)°,相对于固定棒的(28.25±4.24)°,其差异有显著性意义(P < 0.05);套筒型导向生长棒杆在轴向旋转位活动度为(67.88±9.55)°,相比于固定棒的(35.25±5.09)°,其差异有显著性意义(P < 0.05)。 "
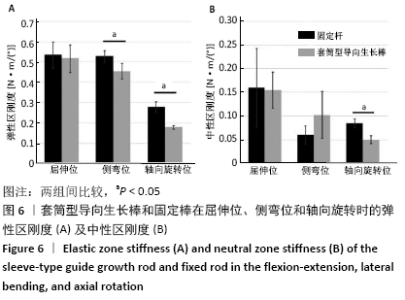
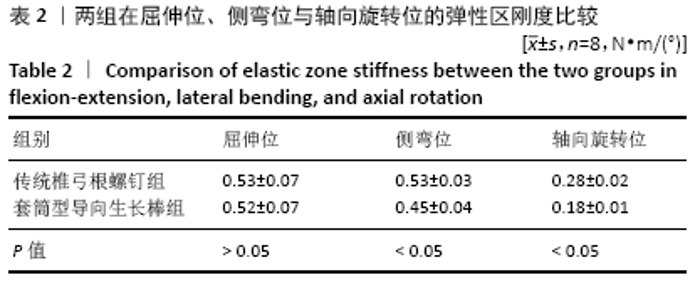
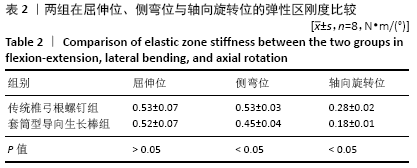
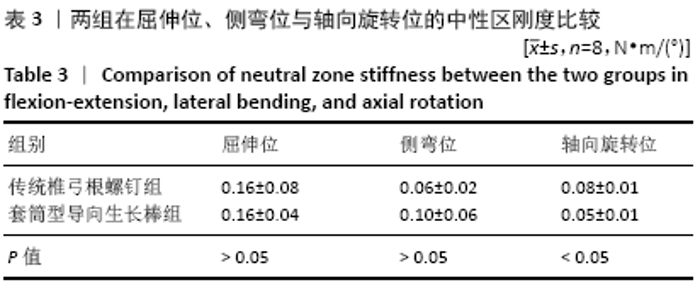
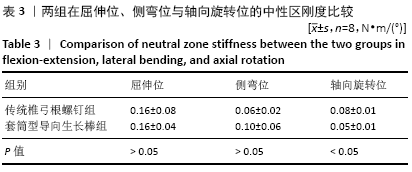
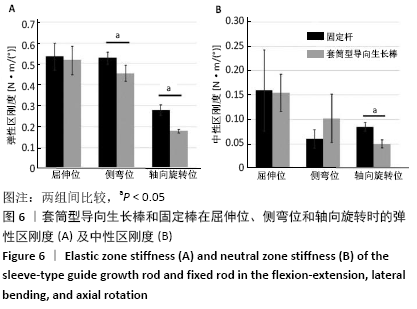
2.3 套筒型导向生长棒和固定棒在屈伸位、侧弯位及轴向旋转位的中性区、弹性区刚度比较 套筒型导向生长棒的脊柱标本在弹性区刚度较固定棒低:屈伸位时两者的弹性区刚度相比,差异无显著性意义(P=0.384);固定棒和套筒型导向生长棒在侧弯时弹性区刚度分别为(0.53±0.03) N?m/(°)和(0.45±0.04) N?m/(°),两者的差异有显著性意义(P=0.000);在轴向旋转时,固定棒的弹性区刚度为(0.28±0.02) N?m/(°),套筒型导向生长棒的弹性区刚度为(0.18±0.01) N?m/(°),两者间差异有显著性意义(P=0.002),见图6A及表2。 同样,使用套筒型导向生长棒的脊柱标本在轴向旋转位时其中性区刚度较固定棒低:屈伸位时两者的中性区刚度相比,差异无显著性意义(P=0.914);侧弯位时两者的中性区刚度相比,差异无显著性意义(P=0.207);在轴向旋转时,固定棒中性区刚度为(0.08±0.01) N?m/(°),套筒型导向生长棒的中性区刚度为(0.05±0.01) N?m/(°),两者间差异有显著性意义(P=0.003),见图6B及表3。 "
| [1] THOMETZ J, LIU XC. Serial CAD/CAM bracing: an alternative to serial casting for early onset scoliosis. J Pediatr Orthop. 2019;39:e185-e189. [2] MARUYAMA T, KOBAYASHI Y, MIURA M, et al. Effectiveness of brace treatment for adolescent idiopathic scoliosis. Scoliosis. 2015;10:S12. [3] MCMASTER MJ, MACNICOL MF. The management of progressive infantile idiopathic scoliosis. J Bone Joint Surg Br. 1979;61:36-42. [4] THOMPSON RM, HUBBARD EW, JO CH, et al. Brace Success Is Related to Curve Type in Patients with Adolescent Idiopathic Scoliosis. J Bone Joint Surg Am. 2017;99:923-928. [5] FEDORAK GT, STASIKELIS PJ, CARPENTER AM, et al. Optimization of casting in early-onset scoliosis. J Pediatr Orthop. 2019;39:e303-e307. [6] CANAVESE F, SAMBA A, DIMEGLIO A, et al. Serial elongation-derotation-flexion casting for children with early-onset scoliosis. World J Orthop. 2015;6:935-943. [7] CAMPBELL RM JR, SMITH MD, MAYES TC, et al. The effect of opening wedge thoracostomy on thoracic insufficiency syndrome associated with fused ribs and congenital scoliosis. J Bone Joint Surg Am. 2004;86: 1659-1674. [8] HARDESTY CK, HUANG RP, EL-HAWARY R, et al. Early-onset scoliosis: updated treatment techniques and results. Spine Deform. 2018;6: 467-472. [9] LIANG J, LI S, XU D, et al. Risk factors for predicting complications associated with growing rod surgery for early-onset scoliosis. Clin Neurol Neurosurg. 2015;136:15-19. [10] SUN ZJ, QIU GX, ZHAO Y, et al. Dual growing rod treatment in early onset scoliosis: the effect of repeated lengthening surgeries on thoracic growth and dimensions. Eur Spine J. 2015;24:1434-1440. [11] BESS S, AKBARNIA BA, THOMPSON GH, et al. Complications of growing-rod treatment for early-onset scoliosis: analysis of one hundred and forty patients. J Bone Joint Surg Am. 2010;92:2533-2543. [12] AKGÜL T, DIKICI F, ŞAR C, et al. Growing rod instrumentation in the treatment of early onset scoliosis. Acta Orthop Belg. 2014,80:457-463. [13] WILKINSON JT, SONGY CE, BUMPASS DB, et al. Curve modulation and apex migration using shilla growth guidance rods for early-onset scoliosis at 5-year follow-up. J Pediatr Orthop. 2017;37:e567-e574. [14] LA ROSA G, OGGIANO L, RUZZINI L. Magnetically controlled growing rods for the management of early-onset scoliosis: a preliminary report. J Pediatr Orthop. 2017;37:79-85. [15] CALDAS JC, PAIS-RIBEIRO JL, CARNEIRO SR. General anesthesia, surgery and hospitalization in children and their effects upon cognitive, academic, emotional and sociobehavioral development - a review. Paediatr Anaesth. 2004;14:910-915. [16] SANKAR WN, ACEVEDO DC, SKAGGS DL. Comparison of complications among growing spinal implants. Spine (Phila Pa 1976). 2010;35: 2091-2096. [17] KWAN K, ALANAY A, YAZICI M, et al. Unplanned Reoperations in Magnetically Controlled Growing Rod Surgery for Early Onset Scoliosis With a Minimum of Two-Year Follow-Up. Spine (Phila Pa 1976). 2017; 42:E1410-E1414. [18] LUQUE ER. Paralytic scoliosis in growing children. Clin Orthop Relat Res. 1982:202-209. [19] KESKINEN H, HELENIUS I, NNADI C, et al. Preliminary comparison of primary and conversion surgery with magnetically controlled growing rods in children with early onset scoliosis. Eur Spine J. 2016;25: 3294-3300. [20] 邓海洋,邓海洋,吴双,等. 套筒型导向生长棒对幼猪脊柱生长影响的实验研究[J]. 中华骨科杂志,2018,38(6):361-369. [21] 何斌,胡侦明,郝杰,等.后部不同结构切除对胸椎稳定性的影响[J]. 第三军医大学学报,2012,34(20):2101-2104. [22] BELL KM, HARTMAN RA, GILBERTSON LG, et al. In vitro spine testing using a robot-based testing system: comparison of displacement control and “hybrid control”. J Biomech. 2013;46:1663-1669. [23] THAWRANI DP, GLOS DL, COOMBS MT, et al. Transverse process hooks at upper instrumented vertebra provide more gradual motion transition than pedicle screws. Spine (Phila Pa 1976). 2014;39:E826-832. [24] QUICK ME, GRANT CA, ADAM CJ, et al. A biomechanical investigation of dual growing rods used for fusionless scoliosis correction. Clin Biomech(Bristol, Avon). 2015;30:33-39. [25] HARTMAN RA, BELL KM, QUAN B, et al. Needle puncture in rabbit functional spinal units alters rotational biomechanics. J Spinal Disord Tech. 2015;28:E146-153. [26] SMIT TH, VAN TUNEN MS, VAN DER VEEN AJ, et al. Quantifying intervertebral disc mechanics: a new definition of the neutral zone. BMC Musculoskelet Disord. 2011;12:38. [27] KAROL LA, JOHNSTON C, MLADENOV K, et al. Pulmonary function following early thoracic fusion in non-neuromuscular scoliosis. J Bone Joint Surg Am. 2008;90(6):1272-1281. [28] SPONSELLER PD, THOMPSON GH, AKBARNIA BA, et al. Growing rods for infantile scoliosis in Marfan syndrome. Spine(Phila Pa l976). 2009; 34(16):1711-1715. [29] LUHMANN SJ, MCCARTHY RE. A comparison of Shilla growth guidance system and growing rods in the treatment of spinal deformity in children less than 10 years of age. J Pediatr Orthop. 2017;37: e567-e574. [30] ANDRAS LM, JOINER ER, MCCARTHY RE, et al. Growing Rods Versus Shilla Growth Guidance: Better Cobb Angle Correction and T1-S1 Length Increase But More Surgeries. Spine Deform. 2015;3:246-252. [31] MCCARTHY RE, MCCULLOUGH FL. Shilla Growth Guidance for Early-Onset Scoliosis: Results After a Minimum of Five Years of Follow-up. J Bone Joint Surg Am. 2015;97:1578-1584. [32] AKBARNIA BA, PAWELEK JB, CHEUNG KM, et al. Traditional Growing Rods Versus Magnetically Controlled Growing Rods for the Surgical Treatment of Early-Onset Scoliosis: A Case-Matched 2-Year Study. Spine Deform. 2014;2:493-497. [33] ROLTON D, RICHARDS J, NNADI C. Magnetic controlled growth rods versus conventional growing rod systems in the treatment of early onset scoliosis: a cost comparison. Eur Spine J. 2015;24:1457-1461. [34] KESKINEN H, HELENIUS I, NNADI C, et al. Preliminary comparison of primary and conversion surgery with magnetically controlled growing rods in children with early onset scoliosis. Eur Spine J. 2016;25: 3294-3300. [35] WILKE HJ, WENGER K, CLAES L. Testing criteria for spinal implants: recommendations for the standardization of in vitro stability testing of spinal implants. Eur Spine J. 1998;7:148-154. [36] BOZKUS H, CRAWFORD NR, CHAMBERLAIN RH, et al. Comparative anatomy of the porcine and human thoracic spines with reference to thoracoscopic surgical techniques. Surg Endosc. 2005;19:1652-1665. [37] STRATHE AB, SØRENSEN H, DANFAER A. A new mathematical model for combining growth and energy intake in animals: the case of the growing pig. J Theor Biol. 2009;261:165-175. [38] WILKE HJ, MATHES B, MIDDERHOFF S, et al. Development of a scoliotic spine model for biomechanical in vitro studies. Clin Biomech (Bristol, Avon). 2015;30:182-187. |
| [1] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [2] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [3] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [4] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [5] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| [6] | Zhang Shangpu, Ju Xiaodong, Song Hengyi, Dong Zhi, Wang Chen, Sun Guodong. Arthroscopic suture bridge technique with suture anchor in the treatment of acromioclavicular dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1417-1422. |
| [7] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Multiple problems in the selection of implants for patellar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1440-1445. |
| [8] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [9] | Xu Yulin, Shen Shi, Zhuo Naiqiang, Yang Huilin, Yang Chao, Li Yang, Zhao Heng, Zhao Lu. Biomechanical comparison of three different plate fixation methods for acetabular posterior column fractures in standing and sitting positions [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 826-830. |
| [10] | Cai Qunbin, Zou Xia, Hu Jiantao, Chen Xinmin, Zheng Liqin, Huang Peizhen, Lin Ziling, Jiang Ziwei. Relationship between tip-apex distance and stability of intertrochanteric femoral fractures with proximal femoral anti-rotation nail: a finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 831-836. |
| [11] | Hou Guangyuan, Zhang Jixue, Zhang Zhijun, Meng Xianghui, Duan Wen, Gao Weilu. Bone cement pedicle screw fixation and fusion in the treatment of degenerative spinal disease with osteoporosis: one-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 878-883. |
| [12] | He Li, Tian Wei, Xu Song, Zhao Xiaoyu, Miao Jun, Jia Jian. Factors influencing the efficacy of lumbopelvic internal fixation in the treatment of traumatic spinopelvic dissociation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 884-889. |
| [13] | Yang Weiqiang, Ding Tong, Yang Weike, Jiang Zhengang. Combined variable stress plate internal fixation affects changes of bone histiocyte function and bone mineral density at the fractured end of goat femur [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 890-894. |
| [14] | Zhang Lei, Ma Li, Fu Shijie, Zhou Xin, Yu Lin, Guo Xiaoguang. Arthroscopic treatment of greater tuberosity avulsion fractures with anterior shoulder dislocation using the double-row suture anchor technique [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 895-900. |
| [15] | Yuan Xinping, Shao Yanbo, Wu Chao, Wang Jianling, Tong Liangcheng, Li Ying. Accuracy of target bone segments in personalized differential modeling and simulation of CT scanning parameters at fracture end [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 912-916. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||