Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (36): 5850-5857.doi: 10.3969/j.issn.2095-4344.2914
Previous Articles Next Articles
Biomechanical study of the effect of femoral anatomy on knee arthroplasty
Li Chao, Cheng Jingbo, Feng Mingli
- Department of Orthopedics, Xuanwu Hospital, Capital Medical University, Beijing 100053, China
-
Received:2020-03-01Revised:2020-03-10Accepted:2020-04-23Online:2020-12-28Published:2020-10-27 -
Contact:Feng Mingli, MD, Chief physician, Department of Orthopedics, Xuanwu Hospital, Capital Medical University, Beijing 100053, China -
About author:Li Chao, Master candidate, Physician, Department of Orthopedics, Xuanwu Hospital, Capital Medical University, Beijing 100053, China
CLC Number:
Cite this article
Li Chao, Cheng Jingbo, Feng Mingli. Biomechanical study of the effect of femoral anatomy on knee arthroplasty[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(36): 5850-5857.
share this article
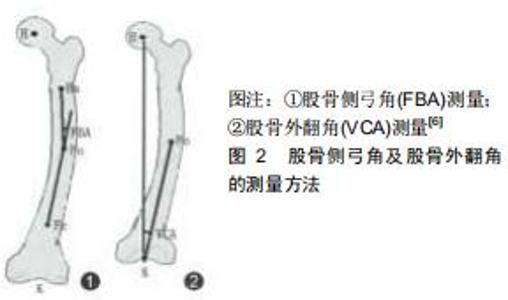
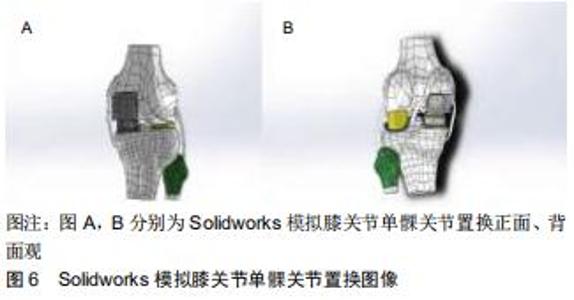
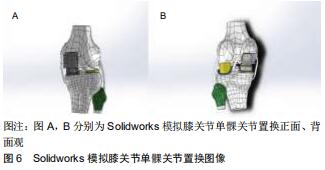
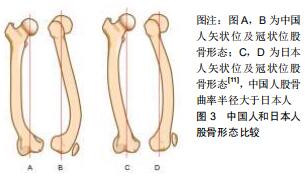
2.1 股骨形态的概述 人类股骨形态呈圆弧状弯曲状[2],可分为股骨上段、中段和远端。股骨上段髓腔存在着2个弯曲,股骨髓腔上部弯曲是朝后,下部弯曲朝前的,这说明股骨上段具有一定的弧度。在股骨中段,股骨弓向前,股骨髓腔呈开口向后的弧形,所以整个髓腔形态从侧位片上呈“S”形[3],股骨中段弯曲主要通过侧弓角度体现[4-6]。股骨侧弓角的测量方法见图2。有研究发现人类股骨侧弓角的平均值为(4.88±1.24)°[7],但不同人种之间股骨侧弓角度并不相同。有研究发现非裔美国人股骨侧弓角较亚洲人和白种人小,并且认为人种间股骨侧弓角的差异是由于股骨长度所造成的[4]。有研究发现黑色人种的股骨曲率半径大于白色人种,说明黑色人种的股骨侧弓角度要大于白色人种[8];有研究对100例股骨进行了分析,得出股骨前弓半径的平均值为108 cm,且该值与性别、年龄无关[9]。有学者通过对426例股骨CT进行研究,得出股骨的前弓半径为(971.44±211.68)mm,且男性大于女性[5]。有研究出日本人股骨曲率半径在矢状面为175 mm,冠状面为2 640 mm[10]。有研究对中国人的股骨形态经行研究后得出中国人股骨的外侧轮廓就像一根曲棍球棒的形状并且股骨曲率半径大于日本人[11],见图3。中国北方地区人群中股骨侧弓的平均值为(1.4±2.4)°,股骨外翻角为(6.5±1.3)°[12]。 "
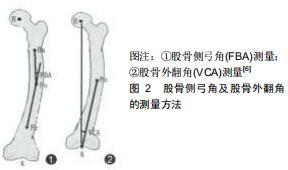
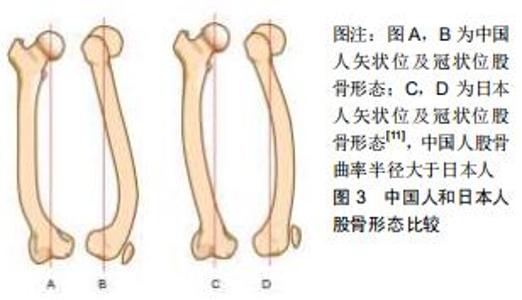
2.1 股骨形态的概述 人类股骨形态呈圆弧状弯曲状[2],可分为股骨上段、中段和远端。股骨上段髓腔存在着2个弯曲,股骨髓腔上部弯曲是朝后,下部弯曲朝前的,这说明股骨上段具有一定的弧度。在股骨中段,股骨弓向前,股骨髓腔呈开口向后的弧形,所以整个髓腔形态从侧位片上呈“S”形[3],股骨中段弯曲主要通过侧弓角度体现[4-6]。股骨侧弓角的测量方法见图2。有研究发现人类股骨侧弓角的平均值为(4.88±1.24)°[7],但不同人种之间股骨侧弓角度并不相同。有研究发现非裔美国人股骨侧弓角较亚洲人和白种人小,并且认为人种间股骨侧弓角的差异是由于股骨长度所造成的[4]。有研究发现黑色人种的股骨曲率半径大于白色人种,说明黑色人种的股骨侧弓角度要大于白色人种[8];有研究对100例股骨进行了分析,得出股骨前弓半径的平均值为108 cm,且该值与性别、年龄无关[9]。有学者通过对426例股骨CT进行研究,得出股骨的前弓半径为(971.44±211.68)mm,且男性大于女性[5]。有研究出日本人股骨曲率半径在矢状面为175 mm,冠状面为2 640 mm[10]。有研究对中国人的股骨形态经行研究后得出中国人股骨的外侧轮廓就像一根曲棍球棒的形状并且股骨曲率半径大于日本人[11],见图3。中国北方地区人群中股骨侧弓的平均值为(1.4±2.4)°,股骨外翻角为(6.5±1.3)°[12]。 "
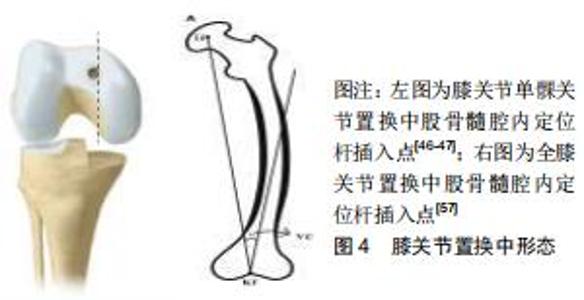
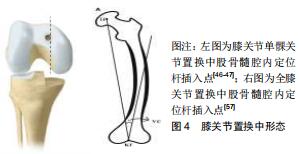
膝关节单髁置换中股骨髓内定位杆插入点的选择依据牛津微创置换操作手册:股骨髓内定位杆插入点必须在股骨髁间窝前内缘的前方1 cm处,且紧贴股骨髁间窝内壁内侧,指向髂前上棘[46-47],见图4。这样可以保证术后下肢力线<0°,因为术后下肢力线内翻>5°则会加速聚乙烯衬垫的磨损; 而过度外翻将导致外侧软骨磨损[48-49];下肢力线内翻>8°就有可能导致假体脱位或松动,甚至需进行早期翻修。牛津微创置换操作手册并未对股骨形态的不同而选择不同股骨髓内定位杆插入点经行说明,这就导致术中需要手术医师依据经验进行选择[50]。有研究对股骨髓内定位杆的位置经行研究后发现冠状位上股骨髓内导杆与股骨髓腔解剖轴线呈外侧交角,平均角度为0.96°;在矢状位上呈后方交角,平均角度为0.13°[51]。MA等[52]对20具尸体经行研究后得出在冠状面时股骨解剖轴距股骨髁间窝中心3.7 mm。蔡骏丰等[47]基于单髁关节置换的尸体骨研究得出,中国人股骨平均外翻角约5.1°,最大7.78°,最小3.78°,并且该研究认为股骨髓内定位杆插入点的理想位置应在髁间窝最高点与髁间窝内侧缘中间距髁间窝水平线前方约1.46 cm的位置。 "
|
[1] 帖小佳,郑如庚,赵梦,等.中国中老年人膝关节骨关节炎患病率的Meta分析[J].中国组织工程研究,2018,22(4):650-656.
[2] BRUNS W, BRUCE M, PRESCOTT G, et al. Temporal trends in femoral curvature and length in medieval and modern Scotland. Am J Phys Anthropol. 2002;119(3):224-230.
[3] 黄宁,魏杰,秦德安.股骨前弓角的临床意义[J].实用骨科杂志,2014,20(3): 237-239.
[4] MARATT J, SCHILLING PL, HOLCOMBE S, et al. Variation in the Femoral Bow: A Novel High-Throughput Analysis of 3922 Femurs on Cross-Sectional Imaging. J Orthop Trauma. 2013;28(1):6-9.
[5] SU XY, ZHE Z, JING-XIN Z, et al. Three-Dimensional Analysis of the Curvature of the Femoral Canal in 426 Chinese Femurs. Biomed Res Int. 2015;2015:1-8.
[6] MULLAJI AB, MARAWAR SV, MITTAL V. A comparison of coronal plane axial femoral relationships in Asian patients with varus osteoarthritic knees and healthy knees. J Arthroplasty. 2009;24(6):861-867.
[7] OCAL MK, SABANCI SS, COBANOGLU M, et al. Anterior Femoral Bow and Possible Effect on the Stifle Joint: A Comparison between Humans and Dogs. Anatomia Histol Embryol. 2017;46(Suppl 1): 391-396.
[8] TRUDELL MB. Anterior femoral curvature revisited: race assessment from the femur. J Forensic Sci. 1999;44(4):700.
[9] ZUBER K, SCHNEIDER E, EULENBERGER J, et al. Form and dimension of the bone marrow cavity of the human femur with reference to the fit of intramedullary implants. Der Unfallchirurg. 1988;91(7):314-319.
[10] ABDELAAL AH, YAMAMOTO N, HAYASHI K, et al. Radiological assessment of the femoral bowing in Japanese population. SICOT J. 2016;2:2.
[11] TANG WM, CHIU KY, KWAN MFY, et al. Sagittal bowing of the distal femur in Chinese patients who require total knee arthroplasty. J Orthop Res. 2005;23(1):41-45.
[12] 吴伟,郭万首,程立明,等.股骨侧弓角的个体差异对全膝人工关节置换后下肢力线的影响[J].中华医学杂志,2017,21(11):1764-1769.
[13] 朱志刚,金大地,罗吉伟,等.股骨远端解剖形态性别差异与假体形态设计的关系[J].中国临床解剖学杂志,2008,26(4):42-44.
[14] 李梁.国人股骨远端形态的测量及其在全膝关节置换与假体设计中的意义[D].上海:第二军医大学,2012:1-46.
[15] HUANG AB, WANG HJ, YANG B, et al. Intraoperative anthropomorphic study of anterior femoral condyles compared with sizing of femoral arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2016;24(4):1280-1285.
[16] REILLY G, YANG B, YU JK, et al. Comparative Study of Sex Differences in Distal Femur Morphology in Osteoarthritic Knees in a Chinese Population. PLoS One. 2014;9(2):e89394.
[17] HÖLLMER H. Bicompartmental versus total knee arthroplasty for medio-patellofemoral osteoarthritis: a comparison of early clinical and functional outcomes. J Knee Surg. 2013;26(6):411-416.
[18] 刘朝晖,郭万首,张启栋,等.单髁置换与全膝关节置换治疗膝关节单室骨性关节炎为主的早中期疗效比较[J].中华医学杂志,2010,90(37):2597-2600.
[19] YAU W, CHIU K, TANG W, et al. Coronal bowing of the femur and tibia in chinese: its incidence and effects on total knee arthroplasty planning. J Orthop Surg. 2007;15(1):32-36.
[20] MULLAJI AB, MARAWAR SV, MITTAL V. A comparison of coronal plane axial femoral relationships in asian patients with varus osteoarthritic knees and healthy. Knee. 2009;24(6):861-867.
[21] MERIC G, GRACITELLI GC, ARAM LJ, et al. Variability in distal femoral anatomy in patients undergoing total knee arthroplasty: measurements on 13,546 computed tomography scans. J Arthroplasty. 2015;30(10):1835-1838.
[22] MOCHIZUKI T, TANIFUJI O, KOGA Y, et al. Sex differences in femoral deformity determined using three-dimensional assessment for osteoarthritic knees. Knee Surg Sports Traumatol Arthrosc. 2017;25(2): 468-476.
[23] LU Y, ZHENG Z L, LV J, et al. Relationships between morphological changes of lower limbs and gender during medial compartment knee osteoarthritis. J Orthop Surg. 2019;11(5):835-844.
[24] NAGAMINE R, KONDO K, IKEMURA S, et al. Distal femoral cut perpendicular to the mechanical axis may induce varus instability in flexion in medial osteoarthritic knees with varus deformity in total knee arthroplasty: a pitfall of the navigation system. J Orthop Sci. 2004;9(6): 555-559.
[25] ŞAHIN N, ÖZDEMIR ST, OCAKOĞLU G, et al. Is axial shape of distal femur different in normal and osteoarthritic female patients? Joint Dis Relat Surg. 2016;27(2):68.
[26] WADA M, TATSUO H, BABA H, et al. Femoral intercondylar notch measurements in osteoarthritic knees. Rheumatology.1999;(6):6.
[27] SHEPSTONE L, ROGERS J, KIRWAN JR, et al. Shape of the intercondylar notch of the human femur: a comparison of osteoarthritic and non-osteoarthritic bones from a skeletal sample. Ann Rheum Dis. 2001;60(10):968-973.
[28] 陈加荣,李凭跃.膝关节骨性关节炎的阶梯治疗原则[J].中国骨科临床与基础研究杂志,2018,10(1):53-57.
[29] 张军,孙磊.关节镜治疗膝骨性关节炎的临床分析[J].中国矫形外科杂志, 2010,18(11):895-898.
[30] 蒋尧传,蒋就喜,唐志宏,等.膝骨性关节炎的关节镜手术治疗[J].中国骨与关节损伤杂志,2010,25(3):259-260.
[31] GUNSTON FH. Polycentric knee arthroplasty: prosthetic simulation of normal knee movement. J Bone Joint Surg Br Vol. 1971;53(2): 272-277.
[32] COVENTRY MB, FINERMAN GM, RILEY LH, et al. A New Geometric Knee for Total Knee Arthroplasty. Clin Orthop Relat Res. 1972;83(94): 157-162.
[33] 张新安,连鸿凯,刘云涛,等.单髁膝置换术与全膝关节置换术治疗膝关节内侧间室骨关节炎的近期疗效比较[J].中国临床新医学,2019,12(11): 1213-1217.
[34] EPINETTE JA, BRUNSCHWEILER B, MERTL P, et al. Unicompartmental knee arthroplasty modes of failure: wear is not the main reason for failure: a multicentre study of 418 failed knees. Orthop Traumatol Surg Res. 2012;98(6):S124-S130.
[35] MÜLLER PE, PELLENGAHR C, WITT M, et al. Influence of minimally invasive surgery on implant positioning and the functional outcome for medial unicompartmental knee arthroplasty. J Arthroplasty. 2004;19(3): 296-301.
[36] PAPAIOANNOU TA, DIGAS G, BIKOS C, et al. Femoral neck version affects medial femorotibial loading. ISRN Orthop. 2013;2013:328246.。
[37] 沙宇,韩晓峰,胡彬,等.活动平台与固定平台单髁置换后下肢力线的矫正效果比较[J].骨科临床与研究杂志,2019,4(6):329-332,364.
[38] 凌晶,章军辉,狄正林,等.移动平台单髁置换术治疗膝关节内侧间室骨性关节炎[J].中国骨与关节损伤杂志,2014,29(8):776-778.
[39] VAN DER LIST JP, ZUIDERBAAN HA, PEARLE AD. Why Do Medial Unicompartmental Knee Arthroplasties Fail Today? J Arthroplasty. 2016;31(5):1016-1021.
[40] DAI X, FANG J, JIANG L, et al. How does the inclination of the tibial component matter? A three-dimensional finite element analysis of medial mobile-bearing unicompartmental arthroplasty. Knee. 2018; 25(3):434-444.
[41] HOPKINS AR, NEW AM, RODRIGUEZ-Y-BAENA F, et al. Finite element analysis of unicompartmental knee arthroplasty. Med Eng Phys. 2010;32(1):14-21.
[42] LIOW MH, TSAI TY, DIMITRIOU D, et al. Does 3-Dimensional In Vivo Component Rotation Affect Clinical Outcomes in Unicompartmental Knee Arthroplasty? J Arthroplasty. 2016;31(10):2167-2172.
[43] 张催,陈游,张春雷,等.单髁置换术与全膝关节置换术治疗膝单间室骨性关节炎近中期疗效的对比研究[J].中华关节外科杂志(电子版),2010,4(2): 51-56.
[44] 李相伟,丁晶.Oxford单髁置换术的术后影像学评价及分析[J].中华关节外科杂志(电子版),2013,7(1):48-51.
[45] NOVOTNY J, GONZALEZ MH, AMIROUCHE FML, et al. Geometric analysis of potential error in using femoral intramedullary guides in total knee arthroplasty. J Arthroplasty. 2001;16(5):641-647.
[46] TU Y, XUE H, MA T, et al. Superior femoral component alignment can be achieved with Oxford microplasty instrumentation after minimally invasive unicompartmental knee arthroplasty. Knee Surg Sports Traumatol Arthroscopy. 2017;25(3):729-735.
[47] 蔡俊丰,马敏,罗树林,等.单髁关节置换中股骨髓内定位杆插入点的解剖学研究[J].中华关节外科杂志(电子版),2017,11(5):511-515.
[48] VASSO M, DEL REGNO C, D"AMELIO A. Minor varus alignment provides better results than neutral alignment in medial UKA. Knee. 2015;22(2):117-121.
[49] BERGER AR. Results of Unicompartmental Knee Arthroplasty at a Minimum of Ten Years of Follow-up. J Bone Joint Surg Am. 2005; 87(5):999-1006.
[50] JENNY JY, BOERI C. Unicompartmental knee prosthesis implantation with a non-image-based navigation system: rationale, technique, case-control comparative study with a conventional instrumented implantation. Knee Surg Sports Traumatol Arthrosc. 2003;11(1):40-45.
[51] 杨涛,涂意辉,薛华明,等.单髁关节置换术股骨髓内定位对股骨假体力线影响的影像学研究[J].中国修复重建外科杂志,2019,33(1):8-12.
[52] MA B, LONG W, RUDAN JF, et al. Three-dimensional analysis of alignment error in using femoral intramedullary guides in unicompartmental knee arthroplasty. J Arthroplasty. 2006;21(2): 271-278.
[53] REED SC, GOLLISH J. The accuracy of femoral intramedullary guides in total knee arthroplasty. J Arthroplasty. 1997;12(6):677-682.
[54] JEFFERY JA. Accuracy of intramedullary femoral alignment in total knee replacement: intraoperative assessment of alignment rod position. Knee. 1999;6(3):211-215.
[55] 李乐翔,薛峰,盛晓文,等.膝关节置换时股骨髓内定位对假体排列的影响[J].中国组织工程研究,2016,20(4):481-485.
[56] THIPPANNA RK, KUMAR MN. Lateralization of femoral entry point to improve the coronal alignment during total knee arthroplasty in patients with bowed femur. J Arthroplasty.2016;31(9):1943-1948.
[57] SHI X, LI H, ZHOU Z, et al. Comparison of postoperative alignment using fixed vs individual valgus correction angle in primary total knee arthroplasty with lateral bowing femur. J Arthroplasty. 2016;31(5): 976-983.
[58] MULLAJI AB, SHETTY GM, KANNA R, et al. The influence of preoperative deformity on valgus correction angle: an analysis of 503 total knee arthroplasties. J Arthroplasty. 2013;28(1):20-27.
[59] BARDAKOS N, CIL A, THOMPSON B, et al. Mechanical axis cannot be restored in total knee arthroplasty with a fixed valgus resection angle: a radiographic study. J Arthroplasty. 2007;22(6 Suppl 2):85-89.
[60] DEAKIN AH, BASANAGOUDAR PL, NUNAG P, et al. Natural distribution of the femoral mechanical–anatomical angle in an osteoarthritic population and its relevance to total knee arthroplasty. Knee. 2012;19(2):120-123.
[61] NAM D, MAHER P A, ROBLES A, et al. Variability in the relationship between the distal femoral mechanical and anatomical axes in patients undergoing primary total knee arthroplasty. J Arthroplasty. 2013;28(5): 798-801.
[62] KIM JM, HONG SH, KIM JM, et al. Femoral shaft bowing in the coronal plane has more significant effect on the coronal alignment of TKA than proximal or distal variations of femoral shape. Knee Surg Sports Traumatol Arthrosc. 2015;23(7):1936-1942.
[63] BERGER RA, RUBASH HE, SEEL MJ, et al. Determining the Rotational Alignment of the Femoral Component in Total Knee Arthroplasty Using the Epicondylar Axis. Clin Orthop. 1993;286(286): 40-47.
[64] GRIFFIN FM, INSALL JN, SCUDERI GR. The posterior condylar angle in osteoarthritic knees. J Arthroplasty. 1998;13(7):812-815.
[65] YIP DKH, ZHU YH, CHIU KY, et al. Distal rotational alignment of the Chinese femur and its relevance in total knee arthroplasty. J Arthroplasty. 2004;19(5):613-619.
[66] JANG KM, LIM HC, HAN SB, et al. Does new instrumentation improve radiologic alignment of the Oxford? medial unicompartmental knee arthroplasty? Knee. 2017;24(3):641-650.
[67] BALDWIN MA, CLARY CW, FITZPATRICK CK, et al. Dynamic finite element knee simulation for evaluation of knee replacement mechanics. J Biomech. 2012;45(3):474-483.
[68] ANDRIACCHI TP, MÜNDERMANN A, SMITH RL, et al. A Framework for the in Vivo Pathomechanics of Osteoarthritis at the Knee. Ann Biomed Eng. 2004;32(3):447-457.
[69] ASANO T, AKAGI M, NAKAMURA T. The functional flexion-extension axis of the knee corresponds to the surgical epicondylar axis: in vivo analysis using a biplanar image-matching technique. J Arthroplasty. 2005;20(8):1060-1067.
[70] RAMOS A, SIMÕES JA. Tetrahedral versus hexahedral finite elements in numerical modelling of the proximal femur. Med Eng Phys. 2006; 28(9):916-924.
[71] BALIUNAS AJ, HURWITZ DE, RYALS AB, et al. Increased knee joint loads during walking are present in subjects with knee osteoarthritis. Osteoarthritis Cartilage. 2002;10(7):573-579.
[72] LIIKAVAINIO T, BRAGGE T, HAKKARAINEN M, et al. Gait and muscle activation changes in men with knee osteoarthritis. Knee. 2010;17(1): 69-76.
[73] VERIM Ö, TAŞGETIREN S, ER MS, et al. Anatomical comparison and evaluation of human proximal femurs modeling via different devices and FEM analysis. Int J Med Robot. 2013;9(2):e19-e24.
[74] BREKELMANS WA, POORT HW, SLOOFF TJ. A new method to analyse the mechanical behaviour of skeletal parts. Acta Orthop Scand. 1972;43(5):301-317.
[75] DONAHUE T LH, HULL ML, RASHID MM, et al. A finite element model of the human knee joint for the study of tibio-femoral contact. J Biomech Eng. 2002;124(3):273-280.
[76] MEAKIN JR, SHRIVE NG, FRANK CB, et al. Finite element analysis of the meniscus: the influence of geometry and material properties on its behaviour. Knee. 2003;10(1):33-41.
[77] PÉREZ-GONZÁLEZ A, FENOLLOSA-ESTEVE C, SANCHO-BRU JL, et al. A modified elastic foundation contact model for application in 3D models of the prosthetic knee. Med Eng Phys. 2008;30(3):387-398.
[78] MOGLO KE, SHIRAZI-ADL AJK. Biomechanics of passive knee joint in drawer: load transmission in intact and ACL-deficient joints.Knee. 2003; 10(3):265-276.
[79] 白波,罗林聪,彭缣侨.有限元法在髋关节运动力学研究中的应用进展[J].国际骨科学杂志,2018,39(1):24-27. [80] 李峰,吴华.基于DICOM数据构建股骨三维有限元模型的精确力学分析[J].中国组织工程研究,2013,2017(30):5483-5489.
[81] 汪金平,杨天府,钟凤林,等.股骨生物力学特性的有限元分析[J].中华创伤骨科杂志,2005,7(10):931-934.
[82] 刘安庆,张银光,王春生,等.人股骨生物力学特性的三维有限元分析[J].西安交通大学学报(医学版),2001,22(3):242-244.
[83] VISURI T, HIETANIEMI K. Displaced stress fracture of the femoral shaft: a report of three cases. Mil Med. 1992;157(6):325-327.
[84] 杨挺,郑建河,姚子龙,等.行走中股骨生物力学特性的有限元分析[J].广东医学,2016,37(4):512-515.
[85] KWON OR, KANG KT, SON J, et al. Biomechanical comparison of fixed- and mobile-bearing for unicomparmental knee arthroplasty using finite element analysis. J Orthop Res. 2014;32(2):338-345.
[86] KO YB, GUJARATHI MR, OH KJ. Outcome of unicompartmental knee arthroplasty: a systematic review of comparative studies between fixed and mobile bearings focusing on complications. Knee Surg Relat Res. 2015;27(3):141-148.
[87] KANG KT, JUHYUN S, YONG-GON K, et al. Effect of femoral component position on biomechanical outcomes of unicompartmental knee arthroplasty. Knee. 2018;25(3):491-498.
[88] DUDLEY TE, GIOE TJ, SINNER P, et al. Registry outcomes of unicompartmental knee arthroplasty revisions. Clin Orthop Relat Res. 2008;466(7):1666-1670.
[89] HOPKINS AR, NEW AM, RODRIGUEZ-Y-BAENA F, et al. Finite element analysis of unicompartmental knee arthroplasty. Med Eng Phys. 2010;32(1):14-21.
[90] KWON OR, KANG KT, SON J, et al. Importance of joint line preservation in unicompartmental knee arthroplasty: Finite element analysis. J Orthop Res. 2017;35(2):347-352.
[91] PATRICK W, MATTHIAS W, ARND S, et al. Increase in the Tibial Slope in Unicondylar Knee Replacement: Analysis of the Effect on the Kinematics and Ligaments in a Weight-Bearing Finite Element Model. Biomed Res Int. 2018;2018:8743604.
[92] INOUE S, AKAGI M, ASADA S, et al. The valgus inclination of the tibial component increases the risk of medial tibial condylar fractures in unicompartmental knee arthroplasty. J Arthroplasty. 2016;31(9): 2025-2030.
[93] PE AE, CALVO B, MARTÍNEZ MA, et al. A three-dimensional finite element analysis of the combined behavior of ligaments and menisci in the healthy human knee joint. J Biomech. 2006;39(9):1686-1701.
[94] INNOCENTI B, BILGEN MF, LABEY L, et al. Load sharing and ligament strains in balanced, overstuffed and understuffed uka. a validated finite element analysis. J Arthroplasty. 2014;29(7): 1491-1498.
[95] VILLA T, MIGLIAVACCA F, GASTALDI D, et al. Contact stresses and fatigue life in a knee prosthesis: comparison between in vitro measurements and computational simulations. J Biomech. 2004; 37(1):45-53.
[96] BISCHOFF JE, HERTZLER JS, MASON JJ. Patellofemoral interactions in walking, stair ascent, and stair descent using a virtual patella model. J Biomech. 2009;42(11):1678-1684.
[97] LIAU JJ, CHENG CK, HUANG CH, et al. The effect of malalignment on stresses in polyethylene component of total knee prostheses-a finite element analysis. Clin Biomech (Bristol, Avon). 2002;17(2):140-146.
[98] IESAKA K, TSUMURA H, SONODA H, et al. The effects of tibial component inclination on bone stress after unicompartmental knee arthroplasty. J Biomech. 2002;35(7):969-974.
[99] SAWATARI T, TSUMURA H, IESAKA K, et al. Three-dimensional finite element analysis of unicompartmental knee arthroplasty–the influence of tibial component inclination. J Orthop Res. 2005;23(3):549-554.
[100] SIMPSON DJ, PRICE AJ, GULATI A, et al. Elevated proximal tibial strains following unicompartmental knee replacement-a possible cause of pain. Med Eng Phys. 2009;31(7):752-757.
[101] BRUNI D, IACONO F, RUSSO A, et al. Minimally invasive unicompartmental knee replacement: retrospective clinical and radiographic evaluation of 83 patients. Knee Surg Sports Traumatol Arthroscopy. 2010;18(6):710-717. [102] KIM KT, LEE S, KIM TW, et al. The influence of postoperative tibiofemoral alignment on the clinical results of unicompartmental knee arthroplasty. Knee Surg Relat Res. 2012;24(2):85-90. |
| [1] | Zhong Yizheng, Huang Peizhen, Cai Qunbin, Zheng Liqin, He Xingpeng, Dong Hang. Microstructural indexes that determine the trabecular bone maximum stress of micro-finite element models [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1313-1318. |
| [2] | Li Xiaomin, Tian Xiangdong, Tan Yetong, Zhu Guangyu, Wang Rongtian, Wang Jian, Xue Zhipeng, Ma Sheng, Hu Yuanyi, Huang Ye, Ding Tiansong. Changes of lower limb force line and knee function after high tibial osteotomy in osteoporotic medial ventricular knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1325-1329. |
| [3] | Wu Taoguang, Nie Shaobo, Chen Hua, Zhu Zhengguo, Qi Lin, Tang Peifu. Biomechanical characteristics of a new multi-dimensional cross locking plate in the treatment of subtrochanteric nonunion [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1330-1334. |
| [4] | Peng Zhixin, Yan Wengang, Wang Kun, Zhang Zhenjiang. Finite element analysis and structural optimization design of 3D printed forearm braces [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1340-1345. |
| [5] | Wu Tianliang, Tao Xiuxia, Xu Hongguang. Influence of different bone mineral densities on cage subsidence after stand-alone oblique lateral interbody fusion: three-dimensional finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1352-1358. |
| [6] | Liu Jinyu, Zhang Hanshuo, Cui Hongpeng, Pan Lingzhi, Zhao Boran, Li Fei, Ding Yu. Finite element biomechanical analysis of minimally invasive treatment of cervical spondylotic myelopathy and accurate exercise rehabilitation [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1359-1364. |
| [7] | He Yujie, Kang Zhijie, Xue Mingming, Jin Feng, Li Zhijun, Wang Xing, Xu Yangyang, Gao Mingjie, Li Jiawei, Li Xiaohe, Wang Haiyan. Finite element analysis of transarticular screw fixation of adolescent thoracic vertebra [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1365-1370. |
| [8] | Wen Xinghua, Ding Huanwen, Cheng Kai, Yan Xiaonan, Peng Yuanhao, Wang Yuning, Liu Kang, Zhang Huiwu. Three-dimensional finite element model analysis of intramedullary nailing fixation design for large femoral defects in Beagle dogs [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1371-1376. |
| [9] | Zhang Lichuang, Gao Huali, Wang Jingchao, Lin Huijun, Wu Chonggui, Ma Yinghui, Huang Yunfei, Fang Xue, Zhai Weitao. Effect of tendon manipulation with equal emphasis on muscles and bones on accelerating the functional rehabilitation of quadriceps femoris after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1383-1389. |
| [10] | Dang Yi, Du Chengyan, Yao Honglin, Yuan Nenghua, Cao Jin, Xiong Shan, Zhang Dingmei, Wang Xin. Hormonal osteonecrosis and oxidative stress [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1469-1476. |
| [11] | Sun Jiajia, Zhu Haidi, Lu Yun, Zhang Kai. Comparison of bone metabolism markers between type 2 diabetes mellitus and non-type 2 diabetes mellitus patients with hip fracture [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1156-1160. |
| [12] | Huang Linke, Wei Linhua, Jiang Jie, Liu Qian, Chen Weiwei. Effects of estrogen combined with treadmill exercise on bone mass and articular cartilage in ovariectomized mice [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1166-1171. |
| [13] | Bi Gengchao, Zhang Yanlong, Li Qiuyue, Hu Longwei, Zhang Yu. Knee joint mechanics and activation characteristics of surrounding muscles during deep jumps at different heights and distances [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1211-1218. |
| [14] | Yang Zhishan, Tang Zhenglong. YAP/TAZ, a core factor of the Hippo signaling pathway, is involved in bone formation [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1264-1271. |
| [15] | Bai Yulong, Li Zhonghai, Zhao Yantao, Xia Cencan, Shi Lei. History, current situation and prospect of tissue banks in China [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1306-1312. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||