Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (32): 5122-5127.doi: 10.3969/j.issn.2095-4344.2859
Previous Articles Next Articles
Vacuum sealing drainage enhances wound healing by up-regulating collagen type I/III ratio in rats
Zhao Xin1, 2, Shi Xin1, 2, Chen Bei2, Cao Yanpeng2, Chen Yaowu2, Liu Xiaoren2, He Yusheng2, He Liyun2, Li Xiying2, Liu Jun1, 2
- 1The First School of Clinical Medicine, Southern Medical University, Guangzhou 510000, Guangdong Province, China; 2Chenzhou No.1 People’s Hospital, Chenzhou 423000, Hunan Province, China
-
Received:2019-12-04Revised:2019-12-10Accepted:2020-01-17Online:2020-11-18Published:2020-09-24 -
Contact:Liu Jun, MD, Professor, Chief physician, Master’s supervisor, the First School of Clinical Medicine, Southern Medical University, Guangzhou 510000, Guangdong Province, China; Chenzhou No.1 People’s Hospital, Chenzhou 423000, Hunan Province, China -
About author:Zhao Xin, Master candidate, Physician, the First School of Clinical Medicine, Southern Medical University, Guangzhou 510000, Guangdong Province, China; Chenzhou No.1 People’s Hospital, Chenzhou 423000, Hunan Province, China. -
Supported by:the Natural Science Foundation of Hunan Province, China, No. 2017JJ2006
CLC Number:
Cite this article
Zhao Xin, Shi Xin, Chen Bei, Cao Yanpeng, Chen Yaowu, Liu Xiaoren, He Yusheng, He Liyun, Li Xiying, Liu Jun. Vacuum sealing drainage enhances wound healing by up-regulating collagen type I/III ratio in rats[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(32): 5122-5127.
share this article
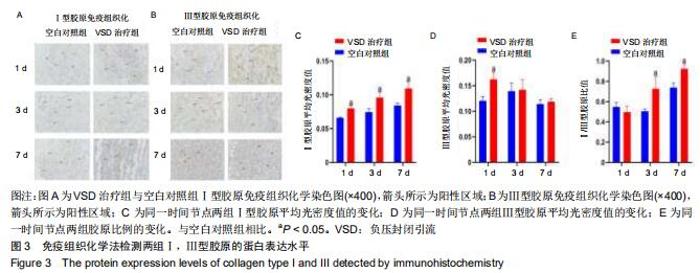
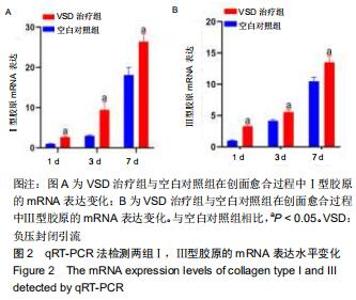
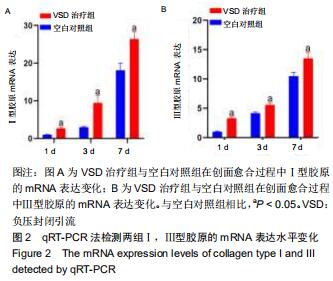
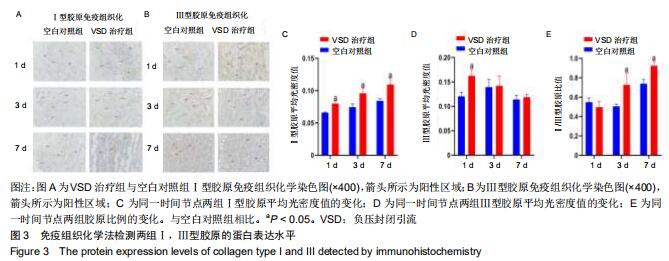
2.4 各组Ⅰ,Ⅲ型胶原的免疫组织化学检测结果 与同时间节点空白对照组相比,术后第1,3,7天负压封闭引流治疗组Ⅰ型胶原免疫组织化学的棕黄色面积明显增多,见图3A;负压封闭引流治疗组Ⅲ型胶原免疫组织化学的棕黄色面积术后第一天明显高于空白对照组,术后第3,7天棕黄色面积未见明显差异,见图3B;利用Image J软件对阳性区域进行半定量分析,负压封闭引流治疗组Ⅰ型胶原的平均光密度值在术后第1,3,7天均高于空白对照组(P < 0.05),见图3C;负压封闭引流治疗组Ⅲ型胶原的平均光密度值在术后第一天明显高于空白对照组(P < 0.05),术后第3,7天未见明显差异,见图3D;Ⅰ,Ⅲ胶原的比例在术后第1天负压封闭引流治疗组稍低于空白对照组,但无显著差异(P > 0.05),术后第3,7天负压封闭引流治疗组的Ⅰ,Ⅲ胶原比例逐渐上升且均高于空白对照组(P < 0.05),见图3E。 "
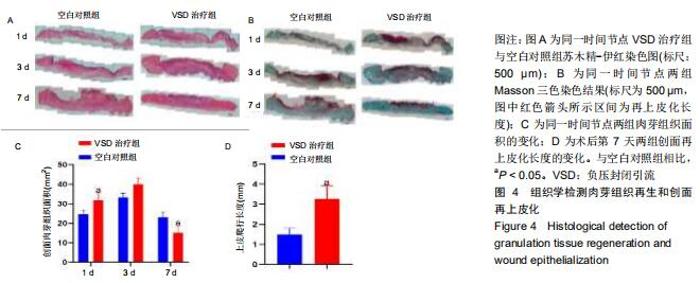
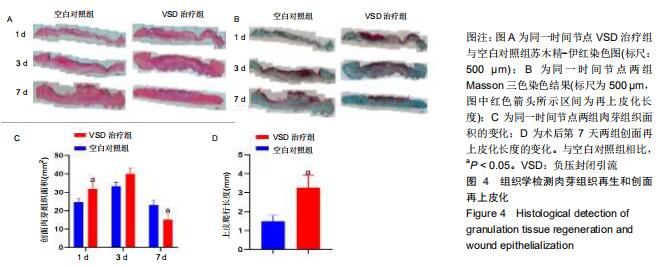
2.5 各组组织学变化 苏木精-伊红染色结果显示负压封闭引流治疗组的肉芽组织生成较多,能够早期填补创面缺损,见图4A;Massson三色染色结果可以看出负压封闭引流治疗组的创面再上皮化速度明显快于空白对照组,见图4B;术后第1天负压封闭引流治疗组的肉芽组织含量高于空白对照组(P < 0.05),术后第3天负压封闭引流治疗组的肉芽组织含量稍高于空白对照组,但无显著差异(P > 0.05),术后第7天负压封闭引流治疗组的肉芽组织含量下降且低于空白对照组(P < 0.05),见图4C;术后第7天两组进行再上皮化长度分析,负压封闭引流治疗组的再上皮化长度明高于空白对照组(P < 0.05),见图4D。 "
|
[1] BARBIERI A, SABATINI L, GRAZIOSI F, et al. Occupational safety and health risks in dock work: a narrative literature review. Med Lav. 2014; 105(6):413-434.
[2] LIU T, BAI X. Trauma care system in China. Chin J Traumatol. 2018; 21(2):80-83.
[3] RUTTER L. Identifying and managing wound infection in the community. Br J Community Nurs. 2018;23(Sup3):S6-S14.
[4] AZIZ ARA, ALSABEK MB. Diabetic foot and disaster; risk factors for amputation during the Syrian crisis. J Diabetes Complications. 2020; 34(2):107493.
[5] GAO M, NGUYEN TT, SUCKOW MA, et al. Acceleration of diabetic wound healing using a novel protease-anti-protease combination therapy. Proc Natl Acad Sci USA. 2015;112(49):15226.
[6] KONG F, FAN C, YANG Y, et al. 5-hydroxymethylfurfural-embedded poly (vinyl alcohol)/sodium alginate hybrid hydrogels accelerate wound healing. Int J Biol Macromol. 2019;138:933-949.
[7] RAJAN V, MURRAY RZ. The duplicitous nature of inflammation in wound repair. Wound Pract Res. 2008;16(3):122-129.
[8] FLEISCHMANN W, STRECKER W, BOMBELLI M, et al. Vacuum sealing as treatment of soft tissue damage in open fractures. Unfallchirurg. 1993;96(9):488-492.
[9] FREAR C C, GRIFFIN B, CUTTLE L, et al. Study of negative pressure wound therapy as an adjunct treatment for acute burns in children (SONATA in C): protocol for a randomised controlled trial. Trials. 2019; 20(1):130.
[10] HYLDIG N, VINTER CA, KRUSE M, et al. Prophylactic incisional negative pressure wound therapy reduces the risk of surgical site infection after caesarean section in obese women: a pragmatic randomised clinical trial. BJOG. 2019,126(5):628-635.
[11] MILAN PB, LOTFIBAKHSHAIESH N, JOGHATAIE MT, et al. Accelerated wound healing in a diabetic rat model using decellularized dermal matrix and human umbilical cord perivascular cells. Acta Biomater. 2016;45:234-246.
[12] 张媛,解怡洁.不同负压值在负压伤口治疗中的作用[J].医学研究生学报, 2012,25(6):661-663.
[13] MA Z, LI Z, SHOU K, et al. Negative pressure wound therapy: regulating blood flow perfusion and microvessel maturation through microvascular pericytes. Int J Mol Med. 2017;40(5):1415-1425.
[14] RIEKKI R, PARIKKA M, JUKKOLA A, et al. Increased expression of collagen types I and III in human skin as a consequence of radiotherapy. Arch Dermatol Res. 2002;294(4):178-184.
[15] LIU X, WU H, BYRNE M, et al. Type III collagen is crucial for collagen I fibrillogenesis and for normal cardiovascular development. Proc Natl Acad Sci USA. 1997;94(5):1852.
[16] HIRE JM, EVANSON JL, JOHNSON PC, et al. Variance of matrix metalloproteinase (MMP) and tissue inhibitor of metalloproteinase (TIMP) concentrations in activated, concentrated platelets from healthy male donors. J Orthop Surg Res. 2014;9:29.
[17] RAHAJENG R. The increased of MMP-9 and MMP-2 with the decreased of TIMP-1 on the uterosacral ligament after childbirth. Pan Afr Med J. 2018;30:283.
[18] BROUGHTON G, JANIS JE, ATTINGER CE. Wound healing: an overview. Plast Reconstr Surg. 2006;117(7 Suppl):1e-S-32e-S.
[19] BUSNARDO VL, BIONDO-SIMÕES MLP. Effects of low-level helium-neon laser on induced wound healing in rats. Rev Bras fisioter. 2010;14(1):45-51.
[20] BIRK D E, MAYNE R. Localization of collagen types I, III and V during tendon development. Changes in collagen types I and III are correlated with changes in fibril diameter. Eur J cell Biol. 1997;72(4): 352-361.
[21] JACOBS S, SIMHAEE DA, MARSANO A, et al. Efficacy and mechanisms of vacuum-assisted closure (VAC) therapy in promoting wound healing: a rodent model. J Plast Reconstr Aesthet Surg. 2009; 62(10):1331-1338.
[22] 王翔,杨帆,解杰,等.负压封闭引流技术干预局部氧分压的实验研究[J].中华急诊医学杂志,2018,27(11):1218-1223.
[23] ELTZSCHIG HK, ECKLE T. Ischemia and reperfusion-from mechanism to translation. Nat Med. 2011;17(11):1391-1401.
[24] BOREA PA, GESSI S, MERIGHI S, et al. Adenosine as a multi-signalling guardian angel in human diseases: when, where and how does it exert its protective effects? Trends Pharmacol Sci. 2016; 37(6):419-434.
[25] SHAIKH G, ZHANG J, PEREZ-ASO M, et al. Adenosine A(2A) receptor promotes collagen type III synthesis via β-catenin activation in human dermal fibroblasts. Br J Pharmacol. 2016;173(23): 3279-3291.
[26] 杨少玲,朱旅云,孙蕾蕾,等.创面负压治疗上调糖尿病足创面肉芽组织TGFβ1表达[J].基础医学与临床,2017,37(9):1323-1325.
[27] LU F, OGAWA R, NGUYEN DT, et al. Microdeformation of three-dimensional cultured fibroblasts induces gene expression and morphological changes. Ann Plast Surg. 2011;66(3):296-300.
[28] 胡承浩,李东宇,庞宗超,等.封闭式负压引流技术治疗糖尿病足对创面组织中TGF-β1及其受体表达的影响研究[J].中国修复重建外科杂志,2018, 32(8):1061-1065.
[29] SUTO M, MASUTOMI H, ISHIHARA K, et al. A Potato peel extract stimulates type I collagen synthesis via Akt and ERK signaling in normal human dermal fibroblasts. Biol Pharm Bull. 2019;42(9): 1510-1516.
[30] VERRECCHIA F, MAUVIEL A. TGF-β and TNF-α: antagonistic cytokines controlling type I collagen gene expression. Cell Signal. 2004;16(8):873-880.
[31] LIU X, LONG X, LIU W, et al. Type I collagen induces mesenchymal cell differentiation into myofibroblasts through YAP-induced TGF-β1 activation. Biochimie. 2018;150:110-130.
[32] MÜLLER S A, DÜRSELEN L, HEISTERBACH P, et al. Effect of a simple collagen type i sponge for achilles tendon repair in a rat model. Am J Sports Med. 2016;44(8):1998-2004.
[33] ZHAO F, CHEN F, YUAN X, et al. Decreased collagen type III synthesis in skin fibroblasts is associated with parastomal hernia following colostomy. Int J Mol Med. 2019,44(5):1609-1618.
[34] XIE S, ZHOU Y, TANG Y, et al. -Book-shaped decellularized tendon matrix scaffold combined with bone marrow mesenchymal stem cells-sheets for repair of achilles tendon defect in rabbit. J Orthop Res. 2019;37(4):887-897.
[35] SEIDEL D, LEFERING R, NEUGEBAUER EAM. Treatment of subcutaneous abdominal wound healing impairment after surgery without fascial dehiscence by vacuum assisted closure™ (SAWHI-V.A.C.®-study) versus standard conventional wound therapy: study protocol for a randomized controlled trial. Trials. 2013;14:394.
[36] GOVINDARAJU P, TODD L, SHETYE S, et al. CD44-dependent inflammation, fibrogenesis, and collagenolysis regulates extracellular matrix remodeling and tensile strength during cutaneous wound healing. Matrix Biol. 2019;75-76:314-330.
[37] SQUIER CA. The stretching of mouse skin in vivo: effect on epidermal proliferation and thickness. J Invest Dermatol. 1980;74(2):68-71. |
| [1] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [2] | Liu Fang, Shan Zhengming, Tang Yulei, Wu Xiaomin, Tian Weiqun. Effects of hemostasis and promoting wound healing of ozone sustained-release hydrogel [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3445-3449. |
| [3] | Chen Zhenyu, Zhang Xiaoning, Luo Yuxin, Liang Jianwei, Yan Chi. Evaluation of silk fibroin/curcumin composite film for promoting wound healing [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(16): 2554-2561. |
| [4] |
Zhan Long, Meng Nongqin, Nong Juan, Li Xiaofeng, Yang Yuan, Yu Xue.
Protocatechuic acid alleviates degeneration of chondrocytes |
| [5] | Cao Guolong, Tian Faming, Liu Jiayin. Lovastatin combined with insulin effects on fracture healing in rat models of bilateral ovariectomized type 2 diabetic mellitus [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(5): 673-681. |
| [6] | Li Xiao, Pan Jinbing, Ma Yun, Qian Haoyu, Zhang Quncheng, Wang Zheng. Silicone stent insertion for treating tracheobronchomalacia in adults [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(4): 549-554. |
| [7] | Li Qinwen, Liang Jie, Wang Dongmei, Shang Zhenghui. Fibrotic changes in rat dorsal root ganglion following chronic sciatic nerve compression [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(29): 4686-4691. |
| [8] | Liu Yanhua, Zhu Zhou, Wan Qianbing. A drug-loading system for electrospinning wound repair: component selection and construction strategy [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(28): 4465-4473. |
| [9] |
Geng Kang, Ding Xiaobin, Tian Xinli, Wang Xue, Yang Yuting, Yan Hong.
Electrical stimulation promotes wound healing and angiogenesis in diabetic rats [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(26): 4152-4156. |
| [10] |
Wu Zhen, Ma Wei, Zang Chenghao, Liu Kuangpin, Liu Wei, Liu Jie, Liang Yu, Li Chunyan, Chen Zhiming, Ru Jin, Fan Chuming, Yang Jinwei, Guo Jianhui, Li Liyan.
Protective effect of notoginsenoside R1 on carbon tetrachloride-induced liver fibrosis in rats [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(26): 4213-4217. |
| [11] |
Gu Yingxuan, Huang Linfeng, Hu Xiaohui, Quan Xiaoming, Kang Liangqi, Zhou Linghan, Wang Xiaojun.
Platelet-rich plasma combined with negative pressure for chronic refractory wounds: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(26): 4257-4264. |
| [12] | Liang Zhou, Wen Lichun, He Zhong, Huang Zheng, Li Kaijing, Yang Xiaoping, Liang Shihe, Pang Gexiong. Three-dimensional printing combined with virtual surgical design in the treatment of complex Pilon fractures [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(24): 3786-3791. |
| [13] | Zhong Shuxian, Shi Yuqing, Yang Yalan, Li Chun. Effect of soft silicone silver ion dressing applied in burn wounds [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(22): 3602-3608. |
| [14] | Cui Yishuang, Lai Zhenquan, Hu Zhongling, Wang Qian, Zhang Hui, Guo Baowen, Li Qijia. Effect of bone morphogenetic protein-7 combined with porous tantalum on chondrogenic differentiation and function of bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(16): 2478-2484. |
| [15] | Zhong Shuxian, Yang Yalan, Shi Yuqing, Li Chun . Meta-analysis of platelet-rich plasma in repairing burn wounds [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(14): 2291-2296. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||