Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (27): 4421-4428.doi: 10.3969/j.issn.2095-4344.2771
Therapeutic effects of platelet-rich plasma versus hyaluronic acid for knee osteoarthritis: a meta-analysis
Wang Yangfa1, Liu Jun1, Pan Jianke1, Gao Shihua2, Huang Junhan1, Li Huiwen1, He Xiangzhong1, Chen Haiyun1
- 1Second Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510120, Guangdong Province, China; 2Second Clinical Medical College of Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China
-
Received:2019-12-11Revised:2019-12-14Accepted:2020-01-20Online:2020-09-28Published:2020-09-10 -
Contact:Chen Haiyun, Chief physician, Second Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510120, Guangdong Province, China -
About author:Wang Yangfa, Master candidate, Second Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510120, Guangdong Province, China -
Supported by:the Project of Guangdong Provincial Department of Finance, No. [2014]157, [2018]8; the Science and Technology Research Project of Traditional Chinese Medicine of Guangdong Hospital of Traditional Chinese Medicine, No. YN2019ML08, YN2015MS15, YK2013B2N19
CLC Number:
Cite this article
Wang Yangfa, Liu Jun, Pan Jianke, Gao Shihua, Huang Junhan, Li Huiwen, He Xiangzhong, Chen Haiyun. Therapeutic effects of platelet-rich plasma versus hyaluronic acid for knee osteoarthritis: a meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(27): 4421-4428.
share this article
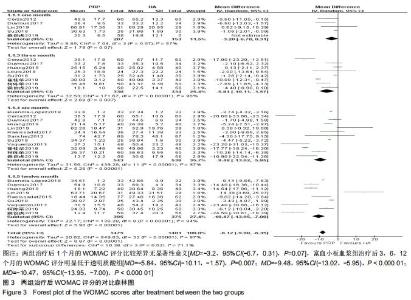
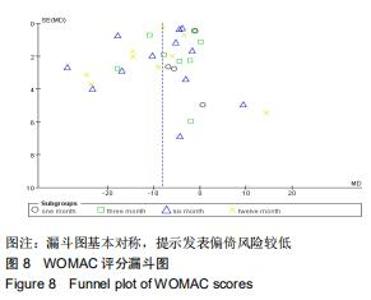
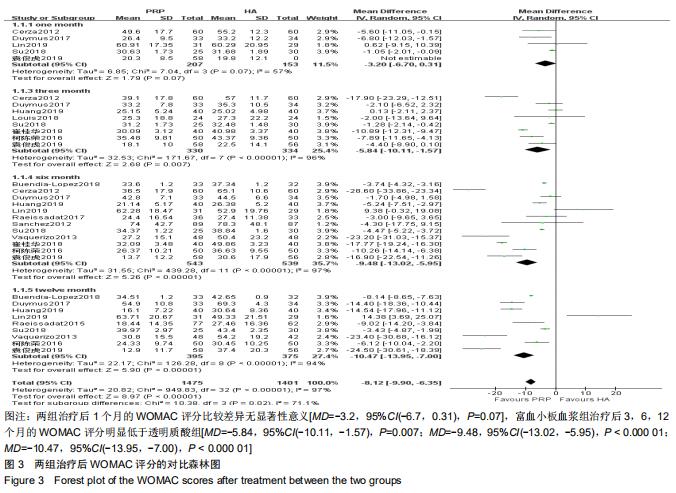
2.2.1 WOMAC评分 分别有5篇[5,11-12,14,22]、8篇[4,11-12,14,17,22-24]、12篇[4-6,9,11-12,14-16,22-24]、9篇文献报道了治疗后1,3,6,12个月的WOMAC评分[4-6,8,12,14-15,22,24]。治疗后1,3,6,12个月的WOMAC评分异质性检验均偏高(P=0.07,I2=57%;P < 0.001,I2=96%;P < 0.001,I2=97%;P < 0.001,I2=94%),故采用随机效应模型进行分析。结果显示,两组治疗后1个月的WOMAC评分比较差异无显著性意义[MD=-3.2,95%CI(-6.7,0.31),P=0.07],富血小板血浆组治疗后3,6,12个月的WOMAC评分明显低于透明质酸组[MD= -5.84,95%CI(-10.11,-1.57),P=0.007;[MD=-9.48,95%CI(-13.02,-5.95),P < 0.000 01;[MD=-10.47,95%CI(-13.95,-7.00),P < 0.000 01],见图3。 "
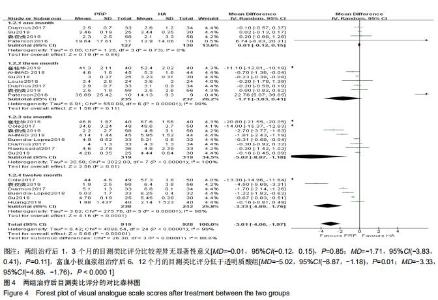
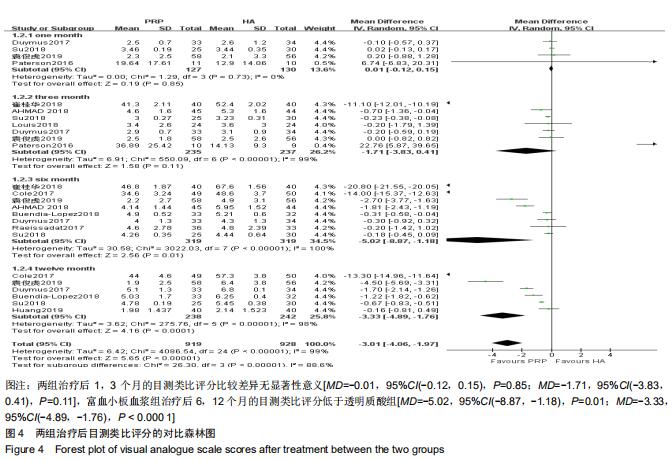
2.2.2 目测类比评分 分别有4篇[12,14,20,22]、7篇[12,14,7,20-23]、8篇[6,9,12-14,21-23]、6篇文献报道了治疗后1,3,6,12个月的目测类比评分[4,6,12-14,22],治疗后1个月的目测类比评分无明显异质性(P=0.73,I2=0%),但治疗后3,6,12个月异质性检验均偏高(P < 0.001,I2=99%;P < 0.001,I2=100%;P < 0.001,I2=98%),故采用随机效应模型进行分析。分析结果显示,两组治疗后1,3个月的目测类比评分比较差异无显著性意义[MD=-0.01,95%CI(-0.12,0.15),P=0.85;MD=-1.71,95%CI(-3.83,0.41),P=0.11],富血小板血浆组治疗后6,12个月的目测类比评分低于透明质酸组[MD=-5.02,95%CI(-8.87,-1.18),P=0.01;MD=-3.33,95%CI(-4.89,-1.76),P < 0.000 1],见图4。 "
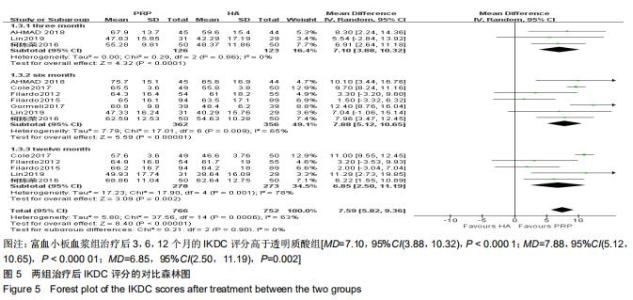
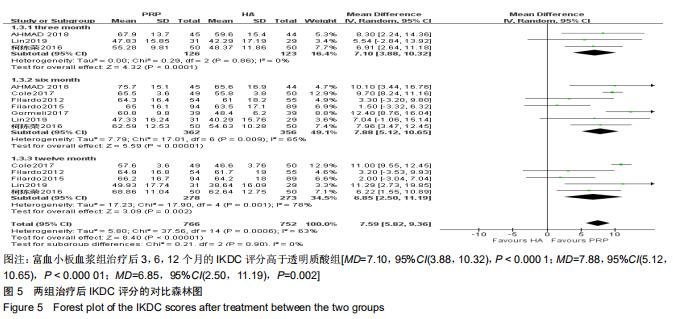
2.2.3 IKDC评分 分别有3篇[5,21,24]、7篇[5,10,13,18-19,21,24]、5篇文献报道了治疗后3,6,12个月的IKDC评 分[5,10,13,19,24]。治疗后3个月的IKDC评分无明显异质性(P=0.86,I2=0%),但治疗后6,12个月的IKDC评分异质性检验均偏高(P=0.005,I2=70%;P=0.001,I2=78%),故采用随机效应模型进行分析。分析结果显示,富血小板血浆组治疗后3,6,12个月的IKDC评分高于透明质酸组[MD=7.10,95%CI(3.88,10.32),P < 0.000 1;MD=7.88,95%CI(5.12,10.65),P < 0.000 01;MD=6.85,95%CI (2.50,11.19),P=0.002],见图5。 "
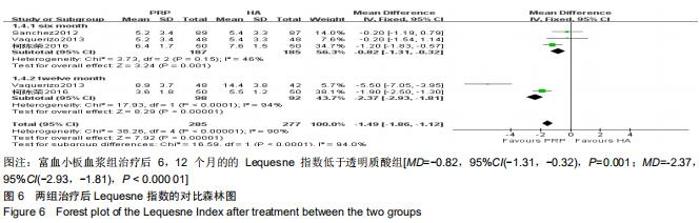
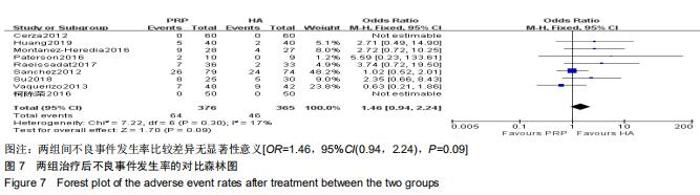
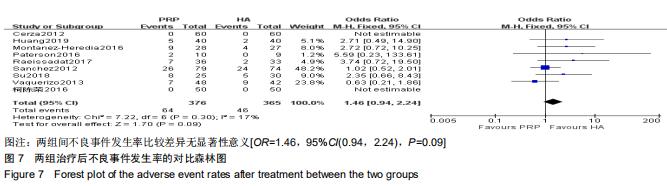
2.2.4 Lequesne指数 分别有3篇[15-16,24]、2篇文献报道了治疗后6,12个月的Lequesne指数[15,24]。治疗后6个月的Lequesne指数检验无明显异质性(P=0.15,I2=46%),治疗后12个月的异质性检验偏高(P < 0.001,I2=94%),因6个月的文献较多,故采用固定效应模型进行分析。分析结果显示,富血小板血浆组治疗后6,12个月的的Lequesne指数低于透明质酸组[MD=-0.82,95%CI(-1.31,-0.32),P=0.001;MD=-2.37,95%CI(-2.93,-1.81),P < 0.000 01],见图6。 2.2.5 不良事件 有9篇文献报道了发生的不良事 件[4,7,9,11,14-16,20,24]。检验提示各研究间无明显异质性(P=0.30,I2=17%),故采用固定效应模型进行分析。结果显示两组间不良事件的发生率相当[OR=1.46,95%CI(0.94,2.24),P=0.09],见图7。 "
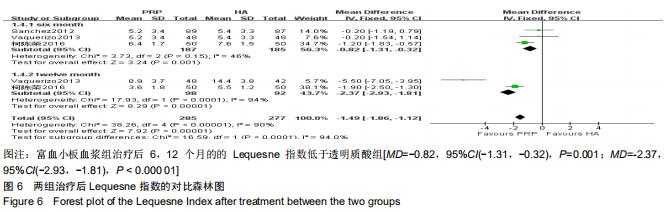

2.2.4 Lequesne指数 分别有3篇[15-16,24]、2篇文献报道了治疗后6,12个月的Lequesne指数[15,24]。治疗后6个月的Lequesne指数检验无明显异质性(P=0.15,I2=46%),治疗后12个月的异质性检验偏高(P < 0.001,I2=94%),因6个月的文献较多,故采用固定效应模型进行分析。分析结果显示,富血小板血浆组治疗后6,12个月的的Lequesne指数低于透明质酸组[MD=-0.82,95%CI(-1.31,-0.32),P=0.001;MD=-2.37,95%CI(-2.93,-1.81),P < 0.000 01],见图6。 2.2.5 不良事件 有9篇文献报道了发生的不良事 件[4,7,9,11,14-16,20,24]。检验提示各研究间无明显异质性(P=0.30,I2=17%),故采用固定效应模型进行分析。结果显示两组间不良事件的发生率相当[OR=1.46,95%CI(0.94,2.24),P=0.09],见图7。 "
|
[1] MCALINDON TE, BANNURU RR. Osteoarthritis in 2017: Latest advances in the management of knee OA.Nat Rev Rheumatol.2018;14(2):73-74.
[2] CONAGHAN PG. NSAIDs or paracetamol for short-term treatment of mild to moderate knee pain in early osteoarthritis: are they equivalent?Evid Based Med.2016;21(1):14.
[3] VAN BUUL GM, KOEVOET WL, KOPS N, et al. Platelet-rich plasma releasate inhibits inflammatory processes in osteoarthritic chondrocytes.Am J Sports Med. 2011;39(11): 2362-2370.
[4] HUANG Y, LIU X, XU X, et al. Intra-articular injections of platelet-rich plasma, hyaluronic acid or corticosteroids for knee osteoarthritis.Der Orthopäde.2019;48(3):239-247.
[5] LIN KY, YANG CC, HSU CJ, et al. Intra-articular Injection of Platelet-Rich Plasma Is Superior to Hyaluronic Acid or Saline Solution in the Treatment of Mild to Moderate Knee Osteoarthritis: A Randomized, Double-Blind, Triple-Parallel, Placebo-Controlled Clinical Trial. Arthroscopy. 2019;35(1): 106-117.
[6] BUENDIA-LOPEZ D, MEDINA-QUIROS M, FERNANDEZ-VILLACANAS MM. Clinical and radiographic comparison of a single LP-PRP injection, a single hyaluronic acid injection and daily NSAID administration with a 52-week follow-up: a randomized controlled trial.J Orthop Traumatol. 2018;19(1):3.
[7] MONTAÑEZ-HEREDIA E, IRÍZAR S, HUERTAS P, et al. Intra-Articular Injections of Platelet-Rich Plasma versus Hyaluronic Acid in the Treatment of Osteoarthritic Knee Pain: A Randomized Clinical Trial in the Context of the Spanish National Health Care System.Int J Mol Sci.2016;17(7):1064.
[8] RAEISSADAT SA, RAYEGANI SM, HASSANABADI H, et al. Knee Osteoarthritis Injection Choices: Platelet- Rich Plasma (PRP) Versus Hyaluronic Acid (A one-year randomized clinical trial).Clin Med Insights Arthritis Musculoskelet Disord. 2015;8:1-8.
[9] RAEISSADAT SA, RAYEGANI SM, AHANGAR AG, et al. Efficacy of Intra-articular Injection of a Newly Developed Plasma Rich in Growth Factor (PRGF) Versus Hyaluronic Acid on Pain and Function of Patients with Knee Osteoarthritis: A Single-Blinded Randomized Clinical Trial. Clin Med Insights Arthritis and Musculoskelet Disord. 2017; 10:1179544117733452.
[10] FILARDO G, KON E, DI MARTINO A,et al.Platelet-rich plasma vs hyaluronic acid to treat knee degenerative pathology: study design and preliminary results of a randomized controlled trial.BMC Musculoskelet Disord.2012; 13:229.
[11] CERZA F, CARNI S, CARCANGIU A, et al. Comparison Between Hyaluronic Acid and Platelet-Rich Plasma, Intra-articular Infiltration in the Treatment of Gonarthrosis. Am J Sports Med.2012;40(12):2822-2827.
[12] DUYMUS TM, MUTLU S, DERNEK B, et al. Choice of intra-articular injection in treatment of knee osteoarthritis: platelet-rich plasma, hyaluronic acid or ozone options.Knee Surg Sports Traumatol Arthrosc.2017;25(2):485-492.
[13] COLE BJ, FORTIER LA, KARAS V, et al. Hyaluronic Acid versus Platelet-Rich Plasma: Double-blind Randomized Controlled Trial Comparing Clinical Outcomes and Intra-Articular Biology for Treatment of Knee osteoarthritis.Am J Sports Med.2017;45(2):339-346.
[14] SU K, BAI Y, WANG J, et al. Comparison of hyaluronic acid and PRP intra-articular injection with combined intra-articular and intraosseous PRP injections to treat patients with knee osteoarthritis.Clin Rheumatol.2018;37(5):1341-1350.
[15] VAQUERIZO V, PLASENCIA MÁ, ARRIBAS I, et al. Comparison of Intra-Articular Injections of Plasma Rich in Growth Factors (PRGF-Endoret) Versus Durolane Hyaluronic Acid in the Treatment of Patients With Symptomatic Osteoarthritis: A Randomized Controlled Trial.Arthroscopy. 2013;29(10):1635-1643.
[16] SÁNCHEZ M, FIZ N, AZOFRA J, et al. A Randomized Clinical Trial Evaluating Plasma Rich in Growth Factors (PRGF-Endoret) Versus Hyaluronic Acid in the Short-Term Treatment of Symptomatic Knee Osteoarthritis. Arthroscopy. 2012;28(8):1070-1078.
[17] LOUIS ML, MAGALON J, JOUVE E, et al. Growth Factors Levels Determine Efficacy of Platelets Rich Plasma Injection in Knee Osteoarthritis: A Randomized Double Blind Noninferiority Trial Compared With Viscosupplementation. Arthroscopy.2018;34(5):1530-1540.
[18] GÖRMELI G, GÖRMELI CA, ATAOGLU B, et al. Multiple PRP injections are more effective than single injections and hyaluronic acid in knees with early osteoarthritis: a randomized, double-blind, placebo-controlled trial. Knee Surg Sports Traumatol. Arthroscopy.2017;25(3):958-965.
[19] FILARDO G, Di MATTEO B, Di MARTINO A, et al.Platelet-Rich Plasma Intra-articular Knee Injections Show No Superiority Versus Viscosupplementation.Am J Sports Med. 2015;43(7):1575-1582.
[20] PATERSON KL, NICHOLLS M, BENNELL KL, et al. Intra-articular injection of photo-activated platelet-rich plasma in patients with knee osteoarthritis: a double-blind, randomized controlled pilot study.BMC Musculoskelet Disord. 2016;17(1).
[21] AHMAD HS, FARRAG SE, OKASHA AE, et al. Clinical outcomes are associated with changes in ultrasonographic structural appearance after platelet-rich plasma treatment for knee osteoarthritis.Int J Rheum Dis.2018;21(5):960-966.
[22] 袁俊虎,陈扬,魏鲁青,等.富含血小板血浆与常规药物关节腔注射治疗早期膝骨关节炎的临床疗效比较[J].骨科,2019,10(1): 25-30. [23] 崔桂华.富血小板血浆与透明质酸钠治疗膝骨关节炎的效果比较[J].中国当代医药,2018,25(16):102-104.
[24] 柯陈荣,张睿,薛继鑫.富血小板血浆联合透明质酸关节腔内注射治疗膝骨关节炎疗效分析[J].中华全科医学,2016,14(11): 1810-1812.
[25] BIJLSMA JW, BERENBAUM F, LAFEBER FP. Osteoarthritis: An update with relevance for clinical practice.Lancet. 2011; 377(9783):2115-2126.
[26] WANG B, LIU W, XING D, et al. Injectable nanohydroxyapatite-chitosan-gelatin micro-scaffolds induce regeneration of knee subchondral bone lesions.Sci Rep. 2017; 7(1):16709.
[27] MCALINDON TE, BANNURU RR, SULLIVAN MC, et al. OARSI guidelines for the non-surgical management of knee osteoarthritis. Osteoarthritis Cartilage.2014;22(3):363-388.
[28] HAWKER GA, MIAN S, BEDNIS K, et al. Osteoarthritis year 2010 in review: non-pharmacologic therapy.Osteoarthritis Cartilage.2011;19(4):366-374.
[29] SÁNCHEZ M, ANITUA E, AZOFRA J, et al. Intra-articular injection of an autologous preparation rich in growth factors for the treatment of knee OA: a retrospective cohort study.Clin Exper Rheumatol.2008;26(5):910.
[30] GOBBI A,LAD D, KARNATZIKOS G. The effects of repeated intra-articular PRP injections on clinical outcomes of early osteoarthritis of the knee.Knee Surg Sports Traumatol Arthrosc. 2015;23(8):2170-2177.
[31] 王波,余楠生.膝骨关节炎阶梯治疗专家共识(2018年版)[J].中华关节外科杂志(电子版),2019,13(1):124-130.
[32] BELLAMY N. Pain assessment in osteoarthritis: Experience with the WOMAC osteoarthritis index.Semin Arthritis Rheum. 1989;18(4-supp-S2):14-17.
[33] HIGGINS LD, TAYLOR MK, PARK D, et al. Reliability and validity of the International Knee Documentation Committee (IKDC) Subjective Knee Form.Joint Bone Spine. 2007;74(6): 594-599.
[34] MANICOURT DH, AZRIA M, MINDEHOLM L, et al. Oral salmon calcitonin reduces Lequesne's algofunctional index scores and decreases urinary and serum levels of biomarkers of joint metabolism in knee osteoarthritis.Arthritis Rheumatol. 2006;54(10):3205-3211.
[35] 袁涛,席刚,韩鹏飞,等.关节腔内注射PRP与HA治疗膝关节骨性关节炎的荟萃分析[J].中国矫形外科杂志,2019,27(3):235-242.
[36] HAN YH, HUANG HT, PAN JK, et al. Comparison of platelet-rich plasma vs hyaluronic acid injections in patients with knee osteoarthritis: A protocol for a systematic review and meta-analysis.Medicine.2018;97(44):e13049.
[37] TEXTOR JA, WILLITS NH, TABLIN F. Synovial fluid growth factor and cytokine concentrations after intra-articular injection of a platelet-rich product in horses.Vet J. 2013; 198(1):217-223.
[38] GOBBI A, LAD D, KARNATZIKOS G. The effects of repeated intra-articular PRP injections on clinical outcomes of early osteoarthritis of the knee. Knee Surg Sports Traumatol Arthrosc. 2015;23(8):2170-2177.
[39] KIM SJ, KIM EK, KIM SJ, et al. Effects of bone marrow aspirate concentrate and platelet-rich plasma on patients with partial tear of the rotator cuff tendon.J Orthop Surg Res. 2018; 13(1):1.
[40] CUGAT R, CUSCÓ X, SEIJAS R, et al. Biologic Enhancement of Cartilage Repair: The Role of Platelet-Rich Plasma and Other Commercially Available Growth Factors. Arthroscopy. 2015;31(4):777-783. |
| [1] | Peng Zhihao, Feng Zongquan, Zou Yonggen, Niu Guoqing, Wu Feng. Relationship of lower limb force line and the progression of lateral compartment arthritis after unicompartmental knee arthroplasty with mobile bearing [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1368-1374. |
| [2] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [3] | Chen Jinping, Li Kui, Chen Qian, Guo Haoran, Zhang Yingbo, Wei Peng. Meta-analysis of the efficacy and safety of tranexamic acid in open spinal surgery [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1458-1464. |
| [4] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [5] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [6] | Wang Yongsheng, Wu Yang, Li Yanchun. Effect of acute high-intensity exercise on appetite hormones in adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1305-1312. |
| [7] | Jiang Hongying, Zhu Liang, Yu Xi, Huang Jing, Xiang Xiaona, Lan Zhengyan, He Hongchen. Effect of platelet-rich plasma on pressure ulcers after spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1149-1153. |
| [8] | Liu Xiangxiang, Huang Yunmei, Chen Wenlie, Lin Ruhui, Lu Xiaodong, Li Zuanfang, Xu Yaye, Huang Meiya, Li Xihai. Ultrastructural changes of the white zone cells of the meniscus in a rat model of early osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1237-1242. |
| [9] | Kong Desheng, He Jingjing, Feng Baofeng, Guo Ruiyun, Asiamah Ernest Amponsah, Lü Fei, Zhang Shuhan, Zhang Xiaolin, Ma Jun, Cui Huixian. Efficacy of mesenchymal stem cells in the spinal cord injury of large animal models: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1142-1148. |
| [10] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Intravenous, topical tranexamic acid alone or their combination in total knee arthroplasty: a meta-analysis of randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 948-956. |
| [11] | Li Yan, Wang Pei, Deng Donghuan, Yan Wei, Li Lei, Jiang Hongjiang. Electroacupuncture for pain control after total knee arthroplasty: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 957-963. |
| [12] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| [13] | Hua Haotian, Zhao Wenyu, Zhang Lei, Bai Wenbo, Wang Xinwei. Meta-analysis of clinical efficacy and safety of antibiotic artificial bone in the treatment of chronic osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 970-976. |
| [14] | Zhan Fangbiao, Cheng Jun, Zou Xinsen, Long Jie, Xie Lizhong, Deng Qianrong. Intraoperative intravenous application of tranexamic acid reduces perioperative bleeding in multilevel posterior spinal surgery: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 977-984. |
| [15] | Zhong Hehe, Sun Pengpeng, Sang Peng, Wu Shuhong, Liu Yi. Evaluation of knee stability after simulated reconstruction of the core ligament of the posterolateral complex [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 821-825. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||