Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (18): 2836-2841.doi: 10.3969/j.issn.2095-4344.2648
Previous Articles Next Articles
Early acute complications after total knee arthroplasty in patients with rheumatoid arthritis
Shen Rui1, Hu Chuan1, Wang Cui1, Rao Huili2, Ding Tao3, Sun Kang1, Tian Shaoqi1
- 1Department of Orthopedics, the Affiliated Hospital of Qingdao University, Qingdao 266000, Shandong Province, China; 2Department of Nursing, Sir Run Run Shaw Hospital Affiliated to Zhejiang University, Hangzhou 310016, Zhejiang Province, China; 3Department of Joint Surgery, Affiliated Hospital of Weifang Medical University, Weifang 261031, Shandong Province, China
-
Received:2019-10-26Revised:2019-10-30Accepted:2019-12-05Online:2020-06-28Published:2020-04-03 -
Contact:Tian Shaoqi, MD, Associate chief physician, Department of Orthopedics, the Affiliated Hospital of Qingdao University, Qingdao 266000, Shandong Province, China -
About author:Shen Rui, Physician, Department of Orthopedics, the Affiliated Hospital of Qingdao University, Qingdao 266000, Shandong Province, China -
Supported by:the National Natural Science Foundation of China (Youth Project), No. 81702172
CLC Number:
Cite this article
Shen Rui, Hu Chuan, Wang Cui, Rao Huili, Ding Tao, Sun Kang, Tian Shaoqi. Early acute complications after total knee arthroplasty in patients with rheumatoid arthritis[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(18): 2836-2841.
share this article
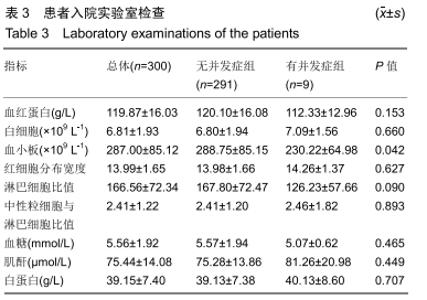
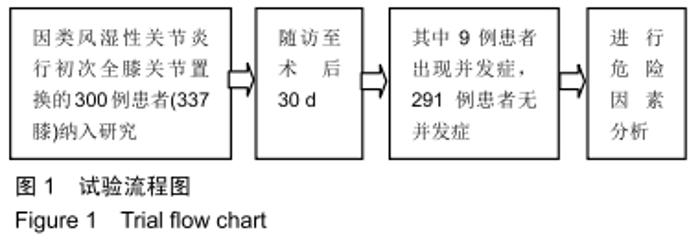
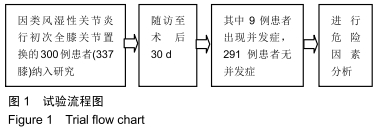
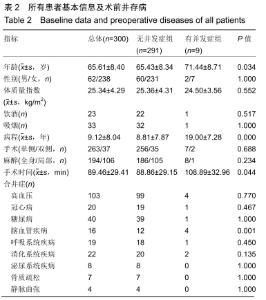
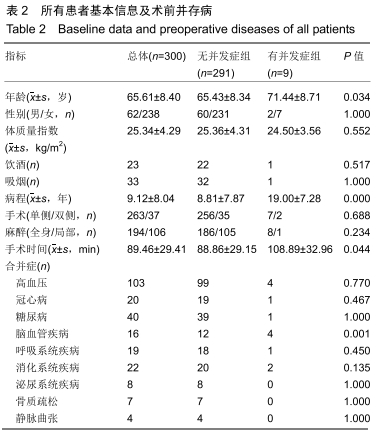
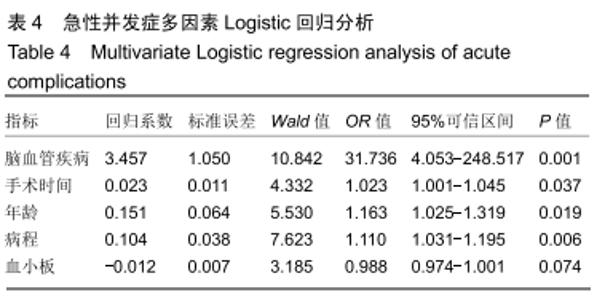
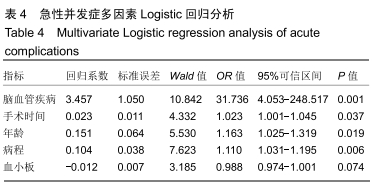
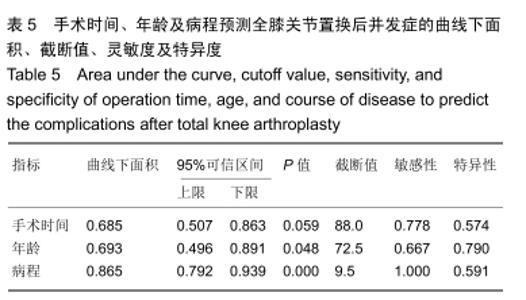
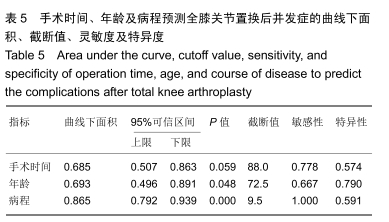
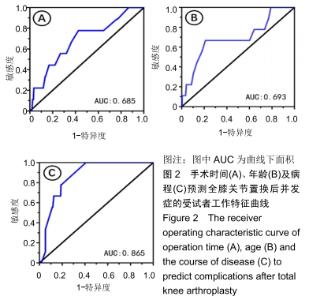
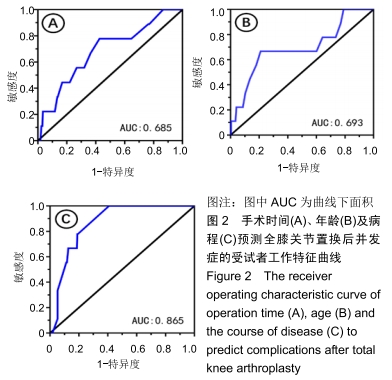
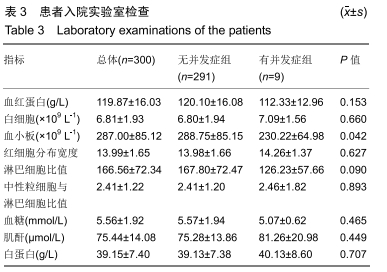
2.4 并发症发生情况 所有患者均随访至术后30 d,无失访病例。9例患者(3.3%)在术后30 d内出现急性并发症,其中2例患者发生手术切口感染(细菌培养结果均为金黄色葡萄球菌),1例患者出现急性肺栓塞,1例患者出现急性心肌梗死,1例患者发生急性胰腺炎,1例患者发生下肢深静脉血栓,1例患者发生心律失常(频发室性早搏),1例患者出现双下肢大面积瘀斑,1例患者出现呕血,所有患者经积极处理后均好转出院,30 d随访时间内无再手术患者及死亡病例。 2.5 急性并发症危险因素分析 根据患者30 d内是否出现急性并发症,将300例患者分为并发症组(9例患者)及无并发症组(291例患者)。单因素分析显示,2组患者在年龄、病程、手术时间、术前并存脑血管疾病方面的差异有显著性意义(P < 0.05),而性别、体质量指数、烟酒情况、手术情况、麻醉情况、其他内科合并症及实验室检查之间的差异无显著性意义(P > 0.05),见表2,3。 "
| [1] BLEVINS JL, CHIU YF, LYMAN S, et al. Comparison of expectations and outcomes in rheumatoid arthritis versus osteoarthritis patients undergoing total knee arthroplasty. J Arthroplasty. 2019;34(9): 1946-1952.e2. [2] YOSHIHARA H, YONEOKA D, MARGALIT A, et al. Rheumatoid arthritis patients undergoing total hip and knee arthroplasty have better in-hospital outcomes compared with non-rheumatoid arthritis patients. Clin Exp Rheumatol. 2016;34(2): 270-275. [3] CRAWFORD DA, ADAMS JB, BEREND KR, et al. Low complication rates in outpatient total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2019. [4] PATEL H, KHOURY H, GIRGENTI D, et al. Burden of surgical site infections associated with arthroplasty and the contribution of staphylococcus aureus. Surg Infect. 2016;17(1):78. [5] REEVES RA, SCHAIRER WW, JEVSEVAR DS. The national burden of periprosthetic hip fractures in the US: costs and risk factors for hospital readmission. Hip Int. 2019;29(5):550-557. [6] BOHL DD, ONDECK NT, BASQUES BA, et al. What is the timing of general health adverse events that occur after total joint arthroplasty? Clin Orthop Relat Res. 2017;475(12):2952-2959. [7] JOHNSON DJ, HARTWELL MJ, WEINER JA, et al. Which post-operative day after total joint arthroplasty are catastrophic events most likely to occur? Jarthroplasty. 2019. [8] YOO JY, O'MALLEY MJ, MATSEN KO LJ, et al. Knee arthroplasty after subchondroplasty: early results, complications, and technical challenges. J Arthroplasty, 2016;31(10): 2188-2192. [9] JOHNSON DJ, HARTWELL MJ, WEINER JA, et al. Which postoperative day after total joint arthroplasty are catastrophic events most likely to occur? J Arthroplasty. 2019;34(10):2466-2472. [10] WARREN JA, SUNDARAM K, KAMATH AF, et al. Venous thromboembolism rates did not decrease in lower extremity revision total joint arthroplasty from 2008 to 2016. J Arthroplasty. 2019;34(11): 2774-2779. [11] TANG H, LI H, ZHANG S, et al. Postoperative complications causing readmission in 30 days after total knee arthroplasty: a retrospective nested case-control study of risk factors based on propensity score matching. J Knee Surg. 2019. doi: 10.1055/s-0039-1692630. [12] HART A, KHALIL JA, CARLI A, et al. Blood transfusion in primary total hip and knee arthroplasty. Incidence, risk factors, and thirty-day complication rates. J Bone Joint Surg Am. 2014;96(23):1945-1951. [13] BOTTLE A, PARIKH S, AYLIN P, et al. Risk factors for early revision after total hip and knee arthroplasty: National observational study from a surgeon and population perspective. PloS One. 2019;14(4): e0214855-e0214855. [14] BAIER C, ADELMUND S, SCHWAB F, et al. Incidence and risk factors of surgical site infection after total knee arthroplasty: Results of a retrospective cohort study. Am J Infect Control.2019;47(10): 1270-1272. [15] TAY KS, CHER EWL, ZHANG K, et al. Comorbidities have a greater impact than age alone in the outcomes of octogenarian total knee arthroplasty. J Arthroplasty. 2017;32(11): 3373-3378. [16] VAKHARIA RM, VAKHARIA AM, EHIOROBO JO, et al. Rheumatoid arthritis increases venous thromboemboli, readmissions, and costs of care after primary total knee arthroplasty: a matched-control analysis. J Arthroplasty. 2019. pii: S0883-5403(19)31003-4. [17] CORDTZ R, ODGAARD A, KRISTENSEN LE, et al. Risk of medical complications following total hip or knee arthroplasty in patients with rheumatoid arthritis: A register-based cohort study from Denmark. Semin Arthritis Rheum. 2019. pii: S0049-0172(19)30281-1. [18] VAKHARIA AM, COHEN-LEVY WB, VAKHARIA RM, et al. Perioperative complications in patients with rheumatoid arthritis following primary total knee arthroplasty: an analysis of 102,898 patients. J Knee Surg. 2019;32(11):1075-1080. [19] CANCIENNE JM, WERNER BC, BROWNE JA. Complications of primary total knee arthroplasty among patients with rheumatoid arthritis, psoriatic arthritis, ankylosing spondylitis, and osteoarthritis. J Am Acad Orthop Surg. 2016;24(8): 567-574. [20] SINGH JA, INACIO MC, NAMBA RS, et al. Rheumatoid arthritis is associated with higher ninety-day hospital readmission rates compared to osteoarthritis after hip or knee arthroplasty: a cohort study. Arthritis Care Res (Hoboken). 2015;67(5):718-724. [21] PUGELY AJ, CALLAGHAN JJ, MARTIN CT, et al. Incidence of and risk factors for 30-day readmission following elective primary total joint arthroplasty: analysis from the ACS-NSQIP. J Arthroplasty, 2013;28(9): 1499-1504. [22] STUNDNER O, CHIU Y, SUN X, et al. Perioperative outcomes in patients with rheumatoid versus osteoarthritis for total hip arthroplasty: a population-based study. Clin Exp Rheumatol. 2013; 31(6): 889-895. [23] STUNDNER O, DANNINGER T, CHIU YL, et al. Rheumatoid arthritis vs osteoarthritis in patients receiving total knee arthroplasty: perioperative outcomes. J Arthroplasty. 2014; 29(2): 308-313. [24] RAVI B, CROXFORD R, HOLLANDS S, et al. Increased risk of complications following total joint arthroplasty in patients with rheumatoid arthritis. Arthritis Rheumatol. 2014;66(2): 254-263. [25] SIU KT, NG FY, CHAN PK, et al. Bacteriology and risk factors associated with periprosthetic joint infection after primary total knee arthroplasty: retrospective study of 2543 cases. Hong Kong Med J. 2018;24(2):152-157. [26] ALETAHA D, NEOGI T, SILMAN AJ, et al. 2010 rheumatoid arthritis classification criteria: an American College of Rheumatology/European League Against Rheumatism collaborative initiative. Arthritis Rheum. 2010;62(9):2569-2581. [27] BELMONT PJ, GOODMAN GP, WATERMAN BR, et al. Thirty-day postoperative complications and mortality following total knee arthroplasty. J Bone Joint Surg Am. 2014;96(1): 20-26. [28] DIXON W, WATSON K, LUNT M, et al. Rates of serious infection, including site-specific and bacterial intracellular infection, in rheumatoid arthritis patients receiving anti–tumor necrosis factor therapy: results from the British Society for Rheumatology Biologics Register. Arthritis Rheum. 2006;54(8):2368-2376. [29] HUNTER TM, BOYTSOV NN, ZHANG X, et al. Prevalence of rheumatoid arthritis in the United States adult population in healthcare claims databases, 2004–2014. Rheumatol Int. 2017;37(9): 1551-1557. [30] MURPHY BPD, DOWSEY MM, SPELMAN T, et al. The impact of older age on patient outcomes following primary total knee arthroplasty. Bone Joint J. 2018;100-B(11):1463-1470. [31] SEO JG, MOON YW, CHO BC, et al. Is total knee arthroplasty a viable treatment option in octogenarians with advanced osteoarthritis? Knee Surg Relat Res. 2015;27(4): 221-227. [32] ROSS D, ERKOCAK O, RASOULI MR, et al. Operative time directly correlates with blood loss and need for blood transfusion in total joint arthroplasty. Arch Bone Joint Surg. 2019;7(3): 229-234. [33] SODHI N, ANIS HK, GOLD PA, et al. Operative times can predict and are correlated with lengths-of-stay in primary total knee arthroplasty: a nationwide database study. J Arthroplasty. 2019;34(7): 1328-1332. [34] GEORGE J, MAHMOOD B, SULTAN AA, et al. How fast should a total knee arthroplasty be performed? An analysis of 140,199 surgeries. J Arthroplasty. 2018;33(8): 2616-2622. [35] WANG L, SEOK S, KIM S, et al. The risk factors of postoperative delirium after total knee arthroplasty. J Knee Surg. 2017;30(6): 600-605. [36] ZENG Y, SI H, WU Y, et al. The incidence of symptomatic in-hospital VTEs in Asian patients undergoing joint arthroplasty was low: a prospective, multicenter, 17,660-patient-enrolled cohort study. Knee Surg Sports Traumatol Arthrosc. 2019; 27(4): 1075-1082. [37] BROWN CH 4TH, FAIGLE R, KLINKER L, et al. The association of brain mri characteristics and postoperative delirium in cardiac surgery patients. Clin Ther. 2015; 37(12): 2686-2699.e2689. [38] 马利阁,尹万乐,尤笑迎.全髋关节置换术后老年患者感染发生相关因素分析[J]. 中华老年医学杂志, 2018, 37(5): 550-553. |
| [1] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [2] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [3] | Zhang Chao, Lü Xin. Heterotopic ossification after acetabular fracture fixation: risk factors, prevention and treatment progress [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1434-1439. |
| [4] | Gu Xia, Zhao Min, Wang Pingyi, Li Yimei, Li Wenhua. Relationship between hypoxia inducible factor 1 alpha and hypoxia signaling pathway [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1284-1289. |
| [5] | Zhao Min, Feng Liuxiang, Chen Yao, Gu Xia, Wang Pingyi, Li Yimei, Li Wenhua. Exosomes as a disease marker under hypoxic conditions [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1104-1108. |
| [6] | Liu Qing, Wan Bijiang. Effect of acupotomy therapy on the expression of Bcl-2/Bax in synovial tissue of collagen-induced arthritis rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 729-734. |
| [7] | Su Baotong, Wang Hanyu, Xu Yilang, Xie Yajuan, Cheng Zhian. Construction of a Nomogram prediction model for postoperative delirium after hip fracture in the elderly based on medical records from a hospital [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3844-3849. |
| [8] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| [9] | Zhang Mingyan, Liu Xiangyang, Chang Lei, Chen Jing, Shen Xiongjie, Liu Bin, Peng Shuai, Zhang Chao, Wu Huanyu, Zhu Feng, Mou Haipin . Relationship between the intraoperative endplate injury and cage retropulsion after lumbar interbody fusion [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2856-2862. |
| [10] | Shen Fu, Kuang Gaoyan, Yang Zhuo, Wen Meng, Zhu Kaimin, Yu Guizhi, Xu Wuji, Deng Bo . Immune infiltration mechanism of differential expression genes in rheumatoid arthritis and potential therapeutic prediction of Chinese herbs [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(14): 2183-2191. |
| [11] | Zhang Tengfei, Wang Kun, Zhu Yanyu, Mei Wei, Wang Qingde. Meta-analysis of risk factors associated with adjacent segment degeneration after lumbar posterior fusion [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(12): 1936-1943. |
| [12] | Zhao Yanxu, Zhang Zhao, Luo Dong, Li Manglai, Wang Jing, Fang Jie, Jiang Wen, Feng Yong, Peng Jiang, Xu Wenjing, Wang Yu, Wang Aiyuan, Zhang Minze. Risk factors for stress fracture of lower limbs and future research direction [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(9): 1422-1429. |
| [13] | Chen Jinsong, Wang Zhonghan, Chang Fei, Liu He. Tissue engineering methods for repair of articular cartilage defect under special conditions [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(8): 1272-1279. |
| [14] | Wu Zhancheng, Zhao Jing, Zhu Xiuhui, Zhang Shaoying, Gao Zhiqiang, Huo Wengang, Jiang Fubin. Treatment of rheumatoid arthritis based on the collateral disease theory [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(5): 760-765. |
| [15] | Qin Wenpin, Yang Yujie, Zhao Laihe, Shi Xiaowei, Lu Lei, Yang Hongxu, Huang Jinghui. Hemorrhage control of fluid gelatin SurgifloTM versus gelatin sponge in lumbar spine fusion surgery [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(4): 561-565. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||